Stevens Johnson Syndrome - Wellington Intensive Care Unit
advertisement
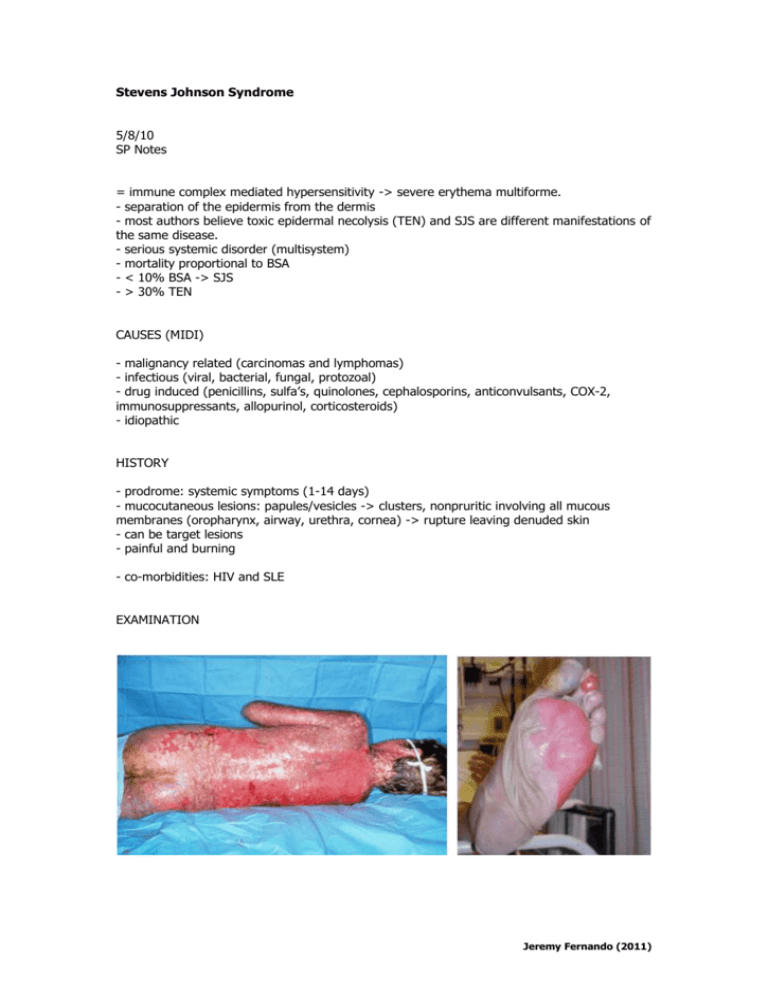
Stevens Johnson Syndrome 5/8/10 SP Notes = immune complex mediated hypersensitivity -> severe erythema multiforme. - separation of the epidermis from the dermis - most authors believe toxic epidermal necolysis (TEN) and SJS are different manifestations of the same disease. - serious systemic disorder (multisystem) - mortality proportional to BSA - < 10% BSA -> SJS - > 30% TEN CAUSES (MIDI) - malignancy related (carcinomas and lymphomas) - infectious (viral, bacterial, fungal, protozoal) - drug induced (penicillins, sulfa’s, quinolones, cephalosporins, anticonvulsants, COX-2, immunosuppressants, allopurinol, corticosteroids) - idiopathic HISTORY - prodrome: systemic symptoms (1-14 days) - mucocutaneous lesions: papules/vesicles -> clusters, nonpruritic involving all mucous membranes (oropharynx, airway, urethra, cornea) -> rupture leaving denuded skin - can be target lesions - painful and burning - co-morbidities: HIV and SLE EXAMINATION Jeremy Fernando (2011) INVESTIGATIONS - standard investigations involved in resuscitation skin biopsy: subepidermal bullae, epidermal necrosis, perivascular lymphocytic infiltration skin and blood cutures bronchoscopy – airway involvement endoscopy – GI involvement MANAGEMENT - determined by the severity of the syndrome Resuscitate A - may need to be intubated c/o mucosal involvement B – protective lung ventilation (can develop pulmonary complications: secretions, sloughing of bronchial epithelim, BOOP) C - fluid resuscitation similar to burn patient, large volumes proportional to BSA involved, will have a hyperdynamic circulation with vasodilatory shock (managed with careful fluids and inotropic support), monitor end-organ function -> urine output >1mL/kg/hr D - multimodal analgesia required -> may have to intubated and ventilated for analgesia E - keep warm and isolated if possible to decrease risk of superinfection, humified environment, warm OT Treatment Specific - stop offending agent identify and treat underlying disease and secondary infection (antibiotics) burns dressings early consultation with dermatologist antibiotics for documented invasive superinfection avoid antibiotics that may exacerbate conditions (silver sulphadizine -> sulpha based) IgG and steroids – controversial (EuroSCAR study) consider plasma exchange General - careful management of fluid-balance and electrolyte abnormalities required - nutrition - thromboprophylaxis Disposition - management in a burns unit if large TBSA involvement - keep family informed - consult dermatology and plastic surgery early Jeremy Fernando (2011)