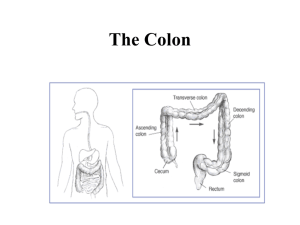
Inflammatory Bowel Diseases
advertisement

Inflammatory Bowel Diseases Dr. Nematollah Ahangar Assistant Prof. of Pharmacology Definition • Two idiopathic forms • ulcerative colitis: – mucosal inflammatory condition – confined to the rectum and colon • Crohn’s disease: – transmural inflammation of GI mucosa – may occur in any part of the GI tract • The etiologies: unknown, but may have a common pathogenetic mechanism PATHOPHYSIOLOGY • combination of infectious, genetic, and immunologic causes • Microflora of the GI tract may provide a trigger to activate inflammation • Crohn’s disease may involve a T lymphocyte disorder that arises in genetically susceptible individuals • Smoking appears to be protective for ulcerative colitis but associated with increased frequency of Crohn’s disease Ulcerative colitis and Crohn’s disease differ in two general respects: anatomic sites and depth of involvement within the bowel wall fibrosis and strictures or, alternatively, fistula formation in CD Comparisons • CD: marked infiltration of lymphocytes and macrophages, granuloma formation, and submucosal fibrosis • UC: lymphocytic and neutrophilic infiltrates • CD: interleukin-12 (IL-12), interferon-γ, and tumor necrosis factor-a (TNF-α), and T-helper 1 (TH1) • UC: T-helper 2 Aminosalicylates • • • • Sulfasalazine Olsalazine Balsalazide Various forms of mesalamine Mesalamine Compounds • To deliver it to different segments of the small or large bowel • Pentasa • Asacol • Rowasa • Canasa Pharmacokinetics & Pharmacodynamics • 5-ASA is readily absorbed from the small intestine • Absorption of 5-ASA from the colon is extremely low • 10% of sulfasalazine and less than 1% of balsalazide are absorbed • Sulfapyridine is absorbed from the colon • Mechanisms Clinical Uses • Induce and maintain remission in ulcerative colitis • considered to be the first-line agents for treatment of mild to moderate active ulcerative colitis • Efficacy in Crohn's disease is unproven • Effectiveness : depends in part on achieving high drug concentration at the site of active disease • suppositories or enemas are useful in patients with ulcerative colitis or Crohn's disease confined to the rectum (proctitis) Adverse Effects • Sulfasalazine: systemic effects of the sulfapyridine molecule • Individual differences of sulfasalazine AEs • nausea, gastrointestinal upset, headaches, arthralgias, myalgias, bone marrow suppression, and malaise • Hypersensitivity to sulfapyridine • Oligospermia • Impairs folate absorption and processing • Dietary supplementation with 1 mg/d folic acid is recommended Adverse Effects • Other aminosalicylate formulations are well tolerated • Olsalazine :a secretory diarrhea in 10% of patients • Rare cases of interstitial nephritis • Rarely cause worsening of colitis Corticosteroids • have been widely used for the treatment of ulcerative colitis and Crohn’s disease • For moderate to severe disease • Prednisolone is most commonly used • once-daily dosing • 40–60 mg/d • After 1–2 weeks, the dosage is tapered to minimize development of adverse effects • In severely ill patients, the drugs are usually administered intravenously • Hydrocortisone enemas, foam, or suppositories (15–30% of the administered dosage is still absorbed) • Budesonide controlled-release formulation Ulcerative Colitis • • • • • • First line mild to moderate colitis is oral sulfasalazine or an oral mesalamine derivative or topical mesalamine or steroids for distal disease Prednisone up to 1 mg/kg/day or 40 to 60 mg daily • Steroids and sulfasalazine appear to be equally efficacious • Choice of formulation • Transdermal nicotine improved symptoms of patients with mild to moderate active ulcerative colitis Severe or Intractable Disease • Requiring hospitalization • parenteral steroids and surgical procedures • Colectomy • Continuous IV infusion of cyclosporine (4 mg/kg/day) is recommended for patients with acute severe ulcerative colitis refractory to steroids Maintenance of Remission • The major agents: sulfasalazine (2g/day) and the mesalamine derivatives • Steroids do not have a role in the maintenance of remission • Azathioprine is effective in preventing relapse of ulcerative colitis for periods exceeding 4 years Crohn’s Disease • The goal of treatment for active Crohn’s disease is to achieve remission • sulfasalazine, mesalamine derivatives, or steroids, azathioprine, mercaptopurine, methotrexate, infliximab, and metronidazole • Steroids are frequently used • Metronidazole (given orally up to 20 mg/kg/day) in some patients with colonic or ileocolonic involvement • Combination of metronidazole with ciprofloxacin Other drugs • Cyclosporine: not recommended except for patients with symptomatic and severe perianal or cutaneous fistulas • Methotrexate: given as a weekly injection of 5 to 25 mg Anti- TNFs • • • • • Infliximab, adalimumab, and certolizumab Infliximab: IV adalimumab, and certolizumab: SC Injections: weekly For the acute and chronic treatment of patients with moderate to severe Crohn's disease • Infliximab: also for UC • The median time to clinical response is 2 weeks Adverse Effects • in up to 6% of patients • infection due to suppression of the TH1 inflammatory response • Antibodies to the antibody • Acute adverse infusion reactions • myalgia, arthralgia, jaw tightness, fever, rash, urticaria, and edema • Lymphoma Anti-Integrin Therapy • Natalizumab • humanized IgG4 monoclonal antibody targeted against the α4 subunit of integrins • significant efficacy for a subset of patients with moderate to severe Crohn's disease And multiple sclerosis • 300 mg every 4 weeks by intravenous infusion • 50% of patients respond to initial therapy with natalizumab • infusion reactions and a small risk of opportunistic infections • multifocal leukoencephalopathy due to reactivation of a human polyomavirus