Acquisition and Implementation
advertisement

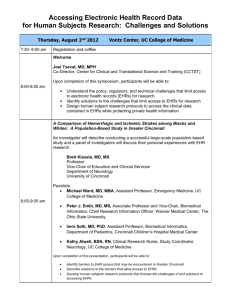
System acquisition refers to the process that occurs from the time the decision is made to select a new system until the time a contract has been negotiated and signed. System implementation begins once the organization has acquired the system and continues through the early stages following the go-live date Support & Evaluation Planning & Analysis Implementation Design Panning & Analysis Examine current systems and problems to identify opportunities for improvement (independent of technology) If new IS is needed, what are the information needs of the users and what are the functional requirements? Design In-house, outside developer? Or purchase from a vendor or contract with an Application Service Provider (ASP) “the cloud” All the alternatives are considered, cost-benefit is done and a system is selected Implementation Support & Evaluation Workflow and process analyses Installing new system Training, converting data Longest phase in the life cycle The first two states are referred to as the acquisition process the second two implementation Health care executive team should Engage in strategic information systems planning Identify goals and strategies and how IT will be employed to aid the organization in achieving them Establish IT priorities Gain budgetary approval and institutional support Establish Project Steering Committee Primary function is to plan, organize, coordinate, and manage all aspects of the acquisition process. Project manager Is critical Often clinicians with training in informatics Chief medical informatics officers or nursing informatics officers Size of the committee Define Project Objectives and Scope of Analysis What does the committee expect to achieve? What process will be used to ensure success? How will milestones be acknowledged? How will committee communicate progress? What resources are needed? Screen the Marketplace and review Vendor Profiles Determine System Goals The system goals should be aligned with the strategic goals of the organization and should serve as measures of success throughout the system acquisition process. Determine and Prioritize System Requirements Focus groups/interviews/written surveys/product demonstrations Software Technical infrastructure Training and support Develop and Distribute RFP or RFI RFP tend to be highly detailed and are costly and time consuming to develop RFI is considerably shorter Some may send RFI and then RFP to screened vendors Explore Other Acquisition Options Contract with an ASP On a subscription basis to deliver an application and provide the support. Buy vs. lease Benefits Requires less IT staff Fewer up-front costs and less capital Rapid deployment Disadvantages Off the shelf Technical support will not be site specific Data ownership, security and privacy worries Explore Other Acquisition Options Evaluate Vendor Proposals Contract with a system developer or build in-house Develop evaluation criteria Vendor demonstrations Make Site visits/check references Conduct Cost-Benefit Analysis Prepare Summary Report and Recommendations Conduct Contract Negotiations Organize the Implementation Team and Identify a Champion May contain some of the members of the selection team, but also others System champion is someone who is well respected in the organization, sees the new system as necessary to the organization and is passionate about implementing it. EG: Physician (system champion), nurse manager, lab manager, radiology director, CIO, IT analysis, business manager Determine Project Scope and Expectations Should be consistent with the system goals established in the system selection process Establish and Institute a Project Plan Major tasks and milestones Estimated duration of each task Dependencies among tasks Resources and budget Individuals responsible for completing each task Target dates Measures for evaluating completion and success Workflow and Process Analysis Analyze current process and procedures Identify opportunities for improvement Identify sources of data Determine location and number of workstations Redesign physical location as needed Involving users at this stage is critical System installation Determine system configuration Order and install hardware Upgrade or implement IT infrastructure Install software and interfaces Test, rest, and test again Staff training and procedure manuals How much training? Do different groups have different training needs? Who should conduct the training? When should the training occur? What intervals of training are ideal? What training format is best (classroom, one-on-one, small group, computer-based?) What is the role of the vendor? Who in the organization will manage or oversee the training? How is it documented? What criteria and methods will be used to monitor training and ensured that staff are adequately trained? Will staff be tested? Conversion Communications Data should be complete, accurate, and current before being converted Testing Establish communication mechanisms for identifying and addressing problems and concerns Communicate regularly with various constituent groups Preparation for Go-Live Date Select date when patient volume is relatively low Ensure sufficient staff are on hand Set up mechanism for reporting and correcting problems and issues Review and effect process reengineering Create an appropriate environment Expectations are defined, met and managed CFO – financial return CMO – physician’s time/quality of care Nursing staff – workload, patient satisfaction IT staff – help desk calls Do not underestimate user resistance One of the biggest managerial challenges Allocate sufficient resources Provide adequate training Manage unintended consequences More work or new work Workflow (workarounds) System demands Opportunity cost of time Communication Emotions New kinds of errors Upcoding Juxtaposition errors Power shifts Dependence on the system (what happens when the system is down?) American College of Physicians and AmericanEHR Partners The following are 10 mistakes that physicians commonly make with EHRs: Thinking a site visit to a practice that is using the same EHR product isn't worth the effort. 2. Signing an unvetted contract with a vendor. 3. Neglecting to perform a workflow analysis before implementing EHRs. 4. Undertraining other physicians and staff on EHR use. 5. Refusing to purchase a laboratory or device interface. 6. Entering too much data into the EHR. 7. Doing EHR-related work staffers should be doing. 8. Using shortcuts and workarounds while using EHRs. 9. Creating "shadow" paper documents and believing they are more accurate than EHR information. 10. Accepting inefficiency as the new status quo. 1.