File - SOUTHERN MEDICAL UNIVERSITY
advertisement

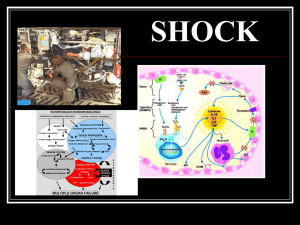
Shock is a condition of profound haemodynamic and metabolic disturbance characterised by failure of the circulatory system to maintain an appropriate blood supply to the microcirculation, with consequent inadequate perfusion of vital organs. OR inadequate tissue perfusion Etiology / classification • Loss of blood or fluid • Trauma • Infection • Anaphylaxis • Heart failure • Strong stimulation of nervous system Effective perfusion depends on • Sufficient blood volume • Normal vasoconstriction / dilation • Normal function of heart pump 3 stages • Ischemic hypoxia • Stagnant hypoxia • Refractory shock Ischemic hypoxia • Altered microcirculation and tissue perfusion – Arteriolar and pre-capillary sphincter constriction, AV shunt • Underlying mechanisms - varied Compensatory mechanisms • Increased heart rate / contractility • Renin Angiotensin system • Arteriole constriction • Venous constriction – auto blood transfusion • Reduced pressure in capillaries – auto fluid transfusion • Redistribution of blood flow Early shock (non-progressive) activation of renin-alodsterone-angiotensin system ADH secretion - conservation of fluid by kidneys catecholamine secretion - tachycardia - peripheral vasoconstriction (except for shock caused by abnormal vasodilatation) cold limbs limited urine output Significance Reversible compensatory stage Stagnant hypoxia stage • Altered microcirculation and tissue perfusion • Decompensated stage – Vessel dilatation – Blood flow is true capillary – Stasis of blood Mechanisms of stasis • Hypoxia – anaerobic glycolysis – low pH – blunts vasomotor response to catecholamines – peripheral pooling of blood 1. Acidosis 2. Local accumulation of metabolic products:histamine,adenosine, K,kinin etc 3. Altered blood flow:↑ viscosity blood,↓.Perfusion pressure →RBC & platelet aggregation.↑adhesion molecules →WBC adhesion and FR production and lysosomal enzymes →endothelial damage 4. Endotoxins bind TLR → ↑IL-1/TNF 5. Effect of humoral factors: histamine, NO cause vasodil’n. Endorphin nulls constriction response by inhibiting vasomotor centr. TXA 2 .→ platelet aggregationTNF, IL-1 .→ WBC adhesion BP falls patient is confused blood diverted to heart and brain urine output falls systemic acidosis Refractory Stage • Cardiac depression • Failure of vasoconstriction responses • Damage of vessels • Deficiency of oxygen and nutrients • DIC, MODS Irreversible shock lysosomal enzymes released from damaged cells skin = cyanosed kidneys = necrosis of tubular epithelium gut = necrosis of tubular epithelium (causes sepsis) lung = necrosis of alveolar epithelium liver = necrosis of centrilobular cells brain = necrosis of neurons, coma heart = myocardial necrosis death due to multiple organ failure Multiple Organ Dysfunction Syndrome (MODS) Presence of altered organ function in an acutely ill patient such that homeostasis cannot be maintained without intervention Cellular and molecular mechanisms • Alteration of cell metabolism – Acidosis – Lack of ATP • Cell injury / apoptosis • Humoral factors – Vasoactive amines – Endothelium derived vasoactive mediators – Regulated peptides • Catecholamines:prolonged vasoconstricn →tissue ischemia & hypoxia • Histamine and 5 HT: arteriole & venule relaxation. • ↑capillary permeability→plasma exudation, viscous blood. • Nitric Oxide: activates guanylate cyclasein smooth muscle to form cyclic GMP • Endothelin: increased levels in hypoxia, ischemia, platelet aggregation and adrenalin. • Also induce intracellular Ca overload and direct toxicity to myocardium Regulated peptides • Angiotensin • Vasopressin • Kinin: bradkykinin from kininogen by action of kallikrein.dilation of arteriole and venule, increase microvascular permeability and promote tissue edema • Endogenous opiod peptide:Endorphins blunts constriction response by inhibiting vasomotor center. Inappropriate inflammatory response • Vascular endothelial damage • Permeability – edema • Impaired oxygen utilization Metabolic derangements • Decreased oxygen consumption • Enhanced glycolysis • Increased catabolism of fat • Negative nitrogen balance Water, electrolyte and acid base disturbance • Na – K pump dysfunction – increased intracellular sodium and water • Anaerobic metabolism, impaired renal excretion – acidosis • Initial hyperventilation in compensatory stage – respiratory alkalosis • Shock lung in late stage – respiratory acidosis Types of Shock Hypovolemic shock • Acute loss of 15-20% circulating blood volume • Loss of blood, plasma or fluid, internal hemorrhage, redistribution • Usually complicated by acute renal failure and endotoxemia Cardiogenic shock • myocardial infarction including complications of myocardial infarction (eg acute mitral regurgitation, VSD, free wall rupture, LV aneurysm) • end-stage cardiomyopathy • myocarditis • LV outflow obstruction (HOCM, aortic stenosis) • LV inflow obstruction (mitral stenosis, LA myxoma) • sequela of cardiopulmonary bypass Cardiogenic shock • Compensatory mechanisms such as salt & water retention and peripheral vasoconstriction tend to exacerbate LV dysfunction. • Also decreased perfusion pressure, especially in the presence of multi-vessel coronary disease leads to further depression of myocardial contractility. Septic Shock Spread and expansion of an initially localised infection into the bloodstream 70% - endotoxin producing gram-ve bacilli Escherichia coli, Klebsiella, Enterobacter, Proteus Pseudomonas aeruginosa - associated with antibiotic therapy and burn wounds; has very high mortality rate. "Bacteroides fragilis" - most common cause of anaerobic septicemias • Cytokines TNF/IL-1 , stress hormones: glucagon, GH, glucocorticoids, and catecholamines →gluconeogenesis. • Pro inflamatory cytokines suppress insulin release and also cause insulin resistance in liver and other tissues. • Hyperglycemia decreases neutrofil function →supressing bactericidal activity and cuase incr. adhesion molecule expression on endothelial cells. Though sepsis →initial rise in glucocorticoid production , frequently followed by adrenal insufficiency probably due to adrenal necrosis • Immune suppression: hypeinflammatory state also activate counter regulatory immunosuppressive mechanisms. TH2 cytokines increase , lymphocyte apoptosis, imunosuppressive effect of apoptotic cells. • MODS: systemic hypotension, interstitial edema, small vessel thrombosis, decrease delivery of O2 and nutrients to tissues. Signs & Symptoms similar to hypovolaemic shock except in the first stages: • Pyrexia and fever, or hyperthermia, due to overwhelming bacterial infection. • Vasodilation and increased cardiac output due to sepsis. Anaphylactic shock • Antigen antibody reaction – release of histamine by mast cells • Venous dilatation • Arteriole dilatation • Increased capillary permeability Signs & Symptoms • Blood vessels dilate, producing red, blotchy skin • Face and neck may swell • Localised edema, especially around the face. • Weak and rapid pulse. • Breathlessness and cough due to narrowing of airways and swelling of the throat. Neurogenic shock • Decreased sympathetic control of blood vessel tone – Brain / spinal cord injury – Deep general anaesthesia Prevention and treatment • Hemodynamic monitoring • Basic life support • Cardiopulmonary resuscitation • Airway maintenance • Intravenous access Improve microcirculation • Volume replacement • Acidosis correction • Vasoactive drugs application • Treatment of DIC Block humoral factors • TNF a monoclonal antibody • Diphenhydramine • Glucocorticoids Cell Protection • Membrane stabilizer, energy mixture and free radical scavenger • Myocyte protection by nicorandil, glucose/insulin/potassium infusions, direct inhibition of Na/H exchanger Organ Protection • General treatment • Eliminating free radicals, stabilizing lysosome and supplying nutrition • Diuresis and dialysis for shock kidney • Oxygen therapy and improving ventilation for shock lung • Reducing pre-load and after-load for heart failure