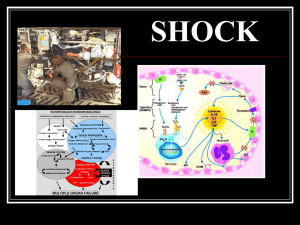
SHOCK: A CLINICAL SYNDROME
advertisement

SHOCK: Ruth M. Kolk, RN,MS,CEN Joy Borrero, RN, MSN NUR240 Overview of Shock Definition: Shock can be defined as a clinical clinical syndrome of decreased blood flow to body tissues resulting in cellular dysfunction and eventual organ failure. Tissue perfusion in shock is inadequate to supply to oxygen and nutrients to cells. Although shock begins as a cellular phenomenon, it is a dynamic process which has been described as a final pathway to death. Risk Factors MAP: a change in sympathetic tone by dilation or constriction of blood vessels will affect MAP MAP= 2D+S 3 CLASSIFICATION OF SHOCK Hypovolemic: decreased intravascular volume-dehydration or hemorrhage Cardiogenic : inability of the heart to pump blood-MI,valve disorders,dysrhythmias,arrest Distributive or vasogenic: abnormality in the vascular system that produces a maldistribution of blood volume –neurogenic anaphylactic, septic, capillary leak Obstructive –tension pneumo, pulmonary embolism, pulmonary HTN Hypovolemic shock characterized by decreased intravascular volume. Inadequate fluid volume in the intravascular compartments results in decreased blood flow and reduced tissue perfusion Excessive fluid loss Causes: internal fluid shifts external fluid loss Hypovolemia Decrease in circulating volume – hemorrhage, plasma volume loss Untreated will lead to hypovolemic shock –causes profound alteration in tissue perfusion . Cellular O2 demand exceeds available supply Stages of Hypovolemic shock 1. Initial – MAP decreased less than 10mm Hg. Compensation is effective. No visible changes 2. Compensatory –body’s primary goal is to maintain blood flow to heart & brain through vasoconstriction ( epinephrine ) & shunting to vital organs. Anaerobic metabolism occurs. Compensatory continued Decreased peripheral blood flow Tachycardia to maintain C.O. Pulse pressure narrows Initially BP may be “ normal “ Urine output decreases Early s/s of shock : thirst, restless/anxiety , AMS Shock : late signs & symptoms Progressive and Refractory Stages Tachypnea & tachycardia Weak pulse Narrow pulse pressure Flat neck veins Pale , cool ,clammy skin Hypotension Oliguria Progressive (intermediate ) Vital organs develop hypoxia Significant changes occur at cellular level which makes resuscitation difficult Cardiac dysrhythmias due to inadequate oxygenation Microclotting :DIC begins Refractory ( irreversible ) Tissue perfusion is negligible Acidosis is prevalent Cellular necrosis occurs due to lack of oxygen Massive DIC Multi system organ failure Interventions for shockGOALS? Position patient – supine vs semifowlers Large bore vascular access Oxygen Crystalloid infusions Blood transfusions Vasopressors Prevent heat loss ( warmed IV fluids) , heating blankets Cardiogenic Shock Caused by decreased cardiac output that results from impaired heart function. Impaired heart function can be classified as systolic or diastolic. Pathophysiology of Cardiogenic Shock When LV cannot propel blood forward, two problems occur: Decreased stroke with resultant declines in CO, BP & tissue perfusion. As BP decreases perfusion to coronary muscles also decreases potentiating myocardial ischemia & predisposing the patient to further muscle damage. Classic cardiogenic shock is secondary to systolic dysfunction. (the ability of the heart to pump blood forward). The left ventricle has a greater workload and metabolic demand than the right ventricle. Left ventricular dysfunction affects forward flow of blood into systemic circulation. Death of the heart (MI) places the patient at risk of developing cardiogenic shock. Necrotic heart muscle does not contract normally leading to decreased CO and inadequate tissue perfusion. This type of shock is the leading cause of in-hospital death Those at the greatest risk are patients who have lost a large portion of Left ventricular muscle mass (anterior wall) Noncoronary Causes Valvular defects, such as stenosis or regurgitation. Stenosis refers to incomplete opening of the valve (impedes blood flow ) Decreased stroke volume Decreased cardiac output cardiomyopathy Pathophysiology Cardiogenic Shock Impaired Function of LV Inadequate systolic emptying LV filling pressures Stroke volume LA pressures CO Pulmonary congestion Tissue perfusion Pulmonary capillary pressures Pulmonary Interstitial edema Intra-alveolar edema Distributive Shock Types: Neurogenic Vasogenic ( anaphylactic, septic, endotoxins) Septic Sepsis-Induced Distributive Shock Neurogenic Shock Massive vasodilatation secondary to loss of sympathetic tone. Cause is usually spinal cord injury or head injury Rare and usually transitory Neurogenic Pathophysiology Massive Vasodilatation Venous Dilation Venous return Ventricular filling Arterial Dilation Peripheral vascular resistance Stroke volume CO Blood Pressure Tissue Perfusion Anaphylactic Shock Characterized by massive dilatation and increased capillary permeability. Potentially life threatening. Causes: Antigen – Antibody Reaction Anaphylactic Shock Patho Antibody Antigen Antibody Reaction Histamine Release of Vasoactive Mediators Massive Vasodilatation Veins Venous return CO Arteries SVR Blood Pressure Tissue Perfusion Prosglandin Serotonin Capillary Refill Septic Shock Severe overwhelming infection. It develops as a result of invasion of foreign microorganisms and subsequent over- activity & dysfunction of body’s defense system. Septic shock & its sequelue are described as part of a clinical continuum. Septic Shock Continuum At one end of the continuum is infection. Presence of microorganisms stimulate the body to activate the inflammatory response. As inflammatory response becomes more widespread, SIR (Systemic Inflammatory Response) develops. Sepsis can then progress to severe sepsis, in which the inflammatory response, initiated to help the body, begins to have harmful effects. Imbalance between coagulation & fibrinolysis Pathophysiology of sepsis Severe sepsis, organ dysfunction hypoperfusion begins Hypotension despite adequate fluid resuscitation Lactic acidosis MODS Most common cause of ICU death NCLEX time In planning an in-service for a group of health care providers employed in an assisted-living facility, the nurse identifies which of the following as risk factors for sepsis? (Choose all that apply. A.Cardiomyopathy B.Low serum albumin level C.History of anaphylaxis D.Prolonged use of corticosteroids E.Age older than 85 F.Chemotherapy treatment for cancer NCLEX TIME The nurse monitors the client for which clinical manifestation as a compensatory mechanism to the initial stage of shock? A.Vascular vasodilation B.Increased heart rate C.Decreased mean arterial pressure D.Elevated body temperature NCLEX Time The nurse recognizes the client with which disorder is at greatest risk for hypovolemic shock? A.Myopathies B.Sepsis C.Pericarditis D.Burns NCLEX TIME The nurse understands that the rationale for the administration of positive inotropic medications to the client in shock is to : A.Increase heart rate B.Increase cardiac contractility C.Increase cellular metabolism D.Increase oxygen consumption Critical Thinking Challenge Your client is a 33-year-old woman who is returned to your outpatient unit after having a surgical tubal ligation by colposcopy. After moving her from the stretcher to her bed, you take her vital signs. Her pulse is 110 and thready, blood pressure is 90/72, respiratory rate is 28, and pulse oximetry is 89%. When you shake her shoulder, she opens her eyes but does not answer any questions. What should you do first? What other assessment data should you obtain? Given the type of surgery, where would you expect bleeding to occur and what manifestations would you expect to find? She still has an IV in her left hand infusing dextrose 5% in 0.45% saline. The postsurgical orders indicate that it should be removed when she is stable. Should you remove it now? Why or why not? NCLEX Time Which blood product is indicated for the client with hypovolemic shock secondary to large blood loss? A.Packed red blood cells B.Fresh frozen plasma C.Platelets D.Whole blood NCLEX Time Which clinical finding does the nurse look for in the client responding effectively to treatment for the initial stage of shock? A.Increased urine output B.Increased heart rate C.Decreased bowel sounds D.Decreased blood pressure NCLEX Time Which of the following clinical manifestations would indicate a worsening in the condition of a client in the late stage of septic shock? A.Warm, flushed skin B.Bleeding, oozing from intravenous sites C.Increasing body temperature D.Urine output of 20 mL/hr Your client who had tubal ligation by colposcopy has no external bleeding, but her abdomen is enlarging and you observe skin discoloration on her lower back. Is O2 an appropriate tx for her? Should you apply pressure to the abd area? Why or why not? What type(s) of IV fluid would be indicated for her? Why?