Path 4
advertisement

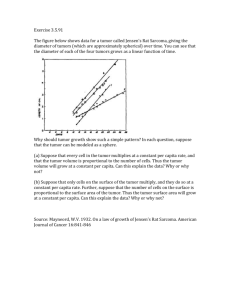
Skin Pathology Disease Cause/Risk Factors Ichthyosis Genetic (X-Linked) Acquired Symptoms Lack of normal skin shedding Steroid Sulfatase Deficiency Urticaria Edematous plaque (wheal); Pruritis Lesions disappear in 24 hours Angioedema of lips and eyelids Minimal inflammatory cell infiltrate Acute Dermatitis Erythema, Blisters, Pruritis Subacute Dermatitis Erythema, Oozing, Crusting & Pruritis (Early Scale) Chronic Dermatitis Erythema, Scaling, Pruritis Buzzwords Acquired = Paraneoplastic Other X-Linked = Due to steroid sulfatase deficiency Acquired = Part of paraneoplastic syndrome Allergic = Type I (IgE) Hypersensitivity All wheals are not urticartia Allergic Contact Dermatitis = Type IV (CMI) Hypersensitivity Drug Related Dermatitis = Eosinophils (Penicillin) Photeczematous Dermatitis = UV Light – Deep Infiltrate Atopic Dermatitis = Family History Acute Eczematous Dermatitis Erythema Multiforme Minor HSV Wheals, Target Lesions, Blisters Limited Associated with HSV Erythema Multiforme Major (Stevens Johnson Syndrome) Drugs Mycoplasma Wheals, Target Lesions, Blisters Widespread-Severe Confluent Target Lesions Target Lesions Almost always associated with drugs (Dilantin, Sulfa, etc) Minimal Lymphocyte Infiltrate Vacuolar alteration along BM Dead Keratinocytes in epidermis Erythema Multiforme Major (Toxic Epidermal Necrolysis) Drugs Mycoplasma Wheals, Target Lesions, Blisters Explosive Skin and Mucous Membrane Damage Target Lesions Like a burn Occurs within 24 hours – treated like burn Minimal Lymphocyte Infiltrate Vacuolar alteration along BM Dead Keratinocytes in epidermis Classic Psoriasis AD Arthritis Flat Silvery Plaques Nail Dystrophies (30%) Auspitz Sign = Pinpoint Bleeding Flat Plaques Munro’s Anscesses Arthritis Koebner Phenomenon Acanthosis without spongiosis Parakeratotic Scale, PMNs in epidermal layer Stratum Corneum Microabscesses (Munro’s) Guttate Psoriasis AD Arthritis Eruptive small scaly Papules Nail Dystrophies (30%) Auspitz Sign = Pinpoint Bleeding Small Scaly Papules Munro’s (Micro) Abscesses Arthritis Koebner Phenomenon Acanthosis without spongiosis Parakeratotic Scale, PMNs in epidermal layer Stratum Corneum Microabscesses (Munro’s) AD Arthritis Gerneralized Red Scaly Skin Nail Dystrophies (30%) Auspitz Sign = Pinpoint Bleeding Red Scaly Skin Munro’s (Micro) Abscesses Arthritis Koebner Phenomenon Acanthosis without spongiosis Parakeratotic Scale, PMNs in epidermal layer Stratum Corneum Microabscesses (Munro’s) Erythrodermic Psoriasis Target Lesions Minimal Lymphocyte Infiltrate Vacuolar alteration along BM Dead Keratinocytes in epidermis Skin Pathology (Contd) Disease Pustular Psoriasis Cause/Risk Factors AD Symptoms Localized = Palms & Soles, Painful Gernearlized = (Von Zumbush), Fatal Nail Dystrophies (30%) Auspitz Sign = Pinpoint Bleeding Buzzwords Other Von Zumbrush (fatal) Munro’s (Micro) Abscesses Arthritis Koebner Phenomenon Acanthosis without spongiosis Parakeratotic Scale, PMNs in epidermal layer Stratum Corneum Microabscesses (Munro’s) Koebner Phenomenon Civatte Bodies (Colloid Bodies) Wickham Stria Band like lymphocytic infiltrate in dermal-epidermal junction Saw-tooth rete ridges, Dead Keratocysts (Civatte Bodies) in DEJ Orthokeratotic Hyperkaratosis SCC may develop in mucous lesions Lichen Planus Hepatitis C? Limited &Pruritic Lesions on skin and mucous membrane Violaceous Papules with Wickham Stria Lacy, white mucous membrane lesions Localized Lupus Erythematosus Autoimmune Hyperkeratotic lesions/rash on sun exposed areas Immunoglobulin DEJ band Periappendageal and perivascular lymphocytic infiltrate Vacuolar alteration along DEJ with BMZ thickening Necrotic keratinocytes in epidermis, Mucin in dermis Immunoglobulin and complement in lesions Systemic Lupus Erythematosus Autoimmune Hyperkeratotic lesions/rash on sun exposed areas Immunoglobulin DEJ band Periappendageal and perivascular lymphocytic infiltrate Vacuolar alteration along DEJ with BMZ thickening Necrotic keratinocytes in epidermis, Mucin in dermis Immunoglobulin and complement in ALL of skin Autoimmune (Desmoglein 3 Ab) Suprabasal Blisters Mucous Membrane lesions precede skin Trunk, Face, Extremities Net Wire Fence on IF Suprabasal May be lethal Intraepidermal Blisters-Suprabasal Positive Direct Immunofluorescence (Net Wire Fence) Acantholytic keratinocytes floating in blisters Pemphigus Foliaceous Subcorneal blisters Crust more common than blisters Mucous membrane not involved Trunk, Face, Extremities Subcorneal Corn Flakes No mucous membrane Endemic (S. America) or Sporadic Intraepidermal Blisters – Subcorneal (Superficial) Positive Direct Immunofluorescence (Net Wire Fence) Acantholytic keratinocytes floating in blisters Pemphigus vegetans Hyperplastic lesions in intertriginous areas Oozing & crusting (no blisters) Often axilla or groin Pemphigus Erythematosus Localized form of P. Foliaceous Face only Pemphigus Vulgaris No blisters Warty plaques Positive Direct Immunofluorescence (Net Wire Fence) Acantholytic keratinocytes floating in blisters Intraepidermal Blisters Positive Direct Immunofluorescence (Net Wire Fence) Acantholytic keratinocytes floating in blisters Bullous Pemphigoid Autoimmune (BMZ element Ab) Sub-epidermal (tense) blisters – don’t rupture Older Patients Mucous Membrane Rare Bullous Pemphigoid antigen Sub-epidermal Mucous Membrane only involved in Mucous Membrane & Scarring Types Blisters contain eosinophils BMZ line of compliment (& less frequently immunoglobulin) Dermatitis Hepetiformis Gluten Sensitivity HLA-B8 & HLA-DR3 Grouped vesicles on erythematous base Very pruritic On extensor surfaces Celiac Disease Micro Abscesses Extensor Surfaces Micro abscesses of PMNs destroy dermal papillae Direct Immunofluorecense shows granular deposits of IgA in dermal papillae May have some bowel overlap (celiac sprue) Friction Blister High heat & moisture Subcorneal split Melanobullous Disorders (Epidermolysis bullosa) Genetic Blister with minimal frictional trauma Group of disorders: All w/ defect in elements holding skin together Skin Pathology (Contd 2) Disease Porphyria Cause/Risk Factors Genetic Acquired Symptoms Buzzwords Blistering & Scarring Milial Cyst formation in sun exposed areas Hypertrichosis of temples Hemachromatosis Group of disorders (Porphyria Cutanea Tarda most common) Uroporphyrinogen Decarboxylase Deficiency Non-inflammatory Comedones at first Papules, pustules, nodules & cysts later Significant scarring Acne Vulgaris Other Disease of Epidermal Appendages Inflammatory Disease of Sebaceous Follicles Erythema Nodosum Unknown Birth Control Pills Sarcoid Strep Infection, TB Anterior surface of legs Painful lesions Rarely drains to skin surface Erythema Induratum Unknown TB Posterior surface of legs May ulcerate More of a Panniculitis – Inflammation of fat lobules Human Papilloma Virus All body surfaces Verrucous Papules/Nodules Grow Rapidly Bleed easily Filliform epidermal projections with parakeratosis Dilated paipllary capillaries Keratohyaline granules Some koilocytes Commonly on legs and face Slightly Raised Hyperpigmented Spread by scratching Obvious koilocytosis Minimal keratinocyte proliferation Common Wart Flat Wart Really more of a septitis Plantar Wart Keratohyaline like granules Moist Wart Proliferation of keratinocytes with kocloyctosis Molluscum Contagiosum Pox Virus Bullous Impetigo Staph aureus (Group A Strep?) Actinic Keratosis UV Radiation Squamous Cell Carcinoma Actinic Keratosis Carcinogens, Ulcers, Scars, Arsenic HPV Ionizing Radiation Papules with a hair follicle opening May become large in immunosuppressed Cytoplasmic inclusions (35 microns) Spread worsened by topical steroids Sub-corneal blister with acantholytic epidermal cells, staph & PMNs Rough (sandpaper like) Red with indistinct borders Epithelial Dysplasia in lower epidermis Can become Squamous cell carcinoma May regress, but all should be treated Fleshy to erythematous with scaly nodules CIS = Bowen’s Diease; epidermis replaced by atypical keratinocytes Infiltrates to dermis; Nodular proliferation of dysplastic keratinocytes UV induced rarely metastasizes to nodes Mucous Membrane is more likely to metastasize Bowen’s Disease Skin Pathology (Contd 3) Disease Cause/Risk Factors Squamous Cell Carcinoma Actinic Keratosis Carcinogens, Ulcers, Scars, Arsenic HPV Ionizing Radiation Symptoms Fleshy to erythematous with scaly nodules Basal Cell Carcinoma Sun Exposure? Noduloulcerative = translucent telangiectasia Superficial = scaly red patch Sclerosing = scar like plaque Basal Cell Nevus Syndrome PTC gene mutation Hundreds of basal cell carcinomas Frontal losing jaw Cysts Bifid ribs Buzzwords Bowen’s Disease Other CIS = Bowen’s Diease; epidermis replaced by atypical keratinocytes Infiltrates to dermis; Nodular proliferation of dysplastic keratinocytes UV induced rarely metastasizes (if it does = to nodes) Mucous Membrane is more likely to metastasize Most common cancer, rarely metastasizes (if it does = blood) 1) Noduloulcerative = basaloid cells in fibromucinous stroma 2) Superficial = Buds of basaloid cells in dermal epidermal junction 3)Sclerosing = strands of basaloid cells in fibrous stroma Merkel Cell Carcinoma Similar to BCC under microscope Cutaneous neuroendocrine carcinoma Melanoma Assymetric Border Notching Color Irregularity Diameter > 6 mm Pagetoid Growth – Radial, larger cells, buckshot scatter Lentiginous Growth – Radial, singly & nests, dermal-epidermal jxn Vertical Growht – Metastatic, grows into dermis Dermatofibrosarcoma Protuberans Nodule or plaque Storiform pattern Infiltrates fat Poor margins, CD34 + Destructive but rarely Metastatic Histiocytosis X (Langerhans Histiocytosis) (Letterer-Siwe Disease) Similar to seborrheic dermatitis w/ hemangiomas Cutaneous T Cell Lymphoma (Mycosis Fungoides) Red Scaly Patches, Plaques or nodules Pruritic With or without leukemia Sezary Syndrome Erythriderma + Leukemia Vitiligo Melanocyte loss or damage Patchy Hypopigmentation May become generalized Albinism Genetic (lack tyrosinose) Inability to produce pigment Freckle (Ephelis) Tan-brown macules Darker in summer/lighter in winter Birbeck Granules Several patterns exist, but all have histiocytes present Also eosinophils and lymphocytes Cells contain Birbeck Granules, S-100 + & CD1a + Due to clonal proliferation of CD4 cells (Sezary-Lutzner Cells) Cell Clusters = Pautrier micro-abscesses Hyperpigmentation of rete No proliferation of melanocytes Skin Pathology (Contd 4) Disease Cause/Risk Factors Symptoms Buzzwords Melasma Facial & neck (mask like) hyperpigmentation Mask of Prenancy Seborrheic Keratosis Benign keratinocyte proliferation in elderly Rough (warty); Most common on trunk Fleshy colored (brown to black) “Stuck on look” Dermatosis Papulosa Nigra Tiny dark popular seborrheic keratoses On Mongoloid or Negroid populations Acanthosis Nigricans Obese young to middle age Hyperinsulinism/Type II DM Predisposition Folded skin (not thickened) Seen on extensor surfaces (hard to see on neck) Other Epidermal = hyperpigmented basal layer keratinocytes Dermal = incontinent melanin pigment in papillary dermis Occurs in pregnancy Proliferation of basaloid keratinocytes (may be more squamoid) Often hyperkeratotic Cystic foci of lamellated keratin Leser Trelat Sign = rapid occurrence fue to internal malignancy Fibroepithelial Polyp (Skin Tag or Acrochordon) (Squamous Papilloma) Acanthosis Nigrans? Diabetes? Epithelioid Cysts Acne? (Epidermoid) Injury? (Epidermal Inclusion) Dome shaped nodule Poral opening Fixed to epidermis Wall and cyst keratin look like normal skin 90% of all cutaneous cysts Most from follicular infundibulum Trichilemmal (Pilar) Cysts Genetic (AD-multiple in women) Dome shaped papule Fixed to epidermis - No pore Firmer than epidermoid cyst Mainly on scalp Lining like middle of hair follicle Pink homogenous keratin About 10% of cysts Dermoid Cysts Most common cyst on face of infant (Rare) Lined like epidermoid cysts Hair follicle elements (sebaceous glands) in wall Occur in developmental fusion planes Steatocystoma Oily Center Wall lined by sebaceous glands Usually on trunk (teens or older) Keratocanthoma Rapidly growing module with keratin filled crater Self healing Squamous Cell Carcinoma Appendage Tumor Flesh colored papules and nodules Nevocellular Nevi (Melanocytic Nevi) UV Light Exposure Thick Seborrheic Keratosis like epithelium or fibrous core Lentigo Simplex (1-2mm) Junctional Nevus (2-3mm) = Distal Extremities Compound Nevus (3-5mm) = Body Intradermal Nevus (3-5mm, flesh colored) = Face Benign Tumor of Melanocytes; Develop before age 40 Junctional = ↑ # melanocytes at rete ridges Compound = clusters at rete & crests, sheets & strands at dermis Intradermal = junctional disappears leaving dermal component Skin Pathology (Contd 5) Disease Dysplastic Nevi Cause/Risk Factors Genetic (AD) Sporadic (benign) Hyperlipidemia? Buzzwords Other Aberrant Differentiation of common nevi Junctional or compound Lentiginous proliferation singly/in nests w/ lateral bridging Concentric & Lamellar Fibrosis; Patchy lymphatic infiltrate Trunk or proximal extremities Larger than common nevi & border irregularity +/- Cytologic atypia Firm Dermal Papule; Indents when pressed Reddish tan to black; Multiple Usually on women’s legs Assymptomatic Benign Fibrous Histiocytoma (Dermatofibroma) Xanthoma Symptoms Dimple Sign Women’s Legs Circumscribed proliferation of spindled fibroblasts Trap collagen bundles at periphery; Foamy macrophages; CD34May not be a true neoplasm Not neoplasms, but collections of foamy macrophages Tuberous & Tendinous = yellow nodules Plane = yellow streaks in skin folds (palmar areas) Xanthelasma = yellow plaques on eyelids (not from Hyperlipidemia) Flesh colored to yellow papules On butt, posterior thighs, knees & elbows Cherry Angioma 2-3mm hemangiomas in adults No internal disease implications Strawberry Angioma Rapidly growing In infants Usually involutes If multiple, internal lesions are likely Mastocytoma Few lesions Urticate, blister when rubbed (Darier Sign) Involutes after months to years Urticaria pigmentosa Slightly smaller than mastocytomas & numerous Rubbing →histamine release (diarrhea & ↑ HR) Histamine release from mast cell granules Diffuse Intracutaneous Mastocytosis Diffusely infiltrated with mast cells Diffuse edema causes “pigskin look” Concern for Mast Cell Leukemia & Internal Organ Involvement Telangiectasia Macularis Eruptiva Perstons No Darrier sign Tan macules with telangiectasias Mainly on trunk Disease of middle age Darier Sign Middle Age Localized dermal nodule of mast cell infiltration Minimal Increase in mast cells around dermal vessels Cells stain melachromatically with several stains Soft Tissue Pathology Disease Cause/Risk Factors Symptoms Buzzwords Lipoma (BenignFatty Tumor) On back, shoulders, abdomen & extremities Slow growing, freely mobile, painless Painless Most common soft tissue tumor in adults; More common in ♂ Liposarcoma (Malignant Fatty Tumor) Proximal extremities & retroperitoneum Slow growing, deep seeded mass Lipoblast is diagnostic Mets (esp to lungs) & recurrence are common Lipoblast T(12:16) Chicker Wire Most common sarcoma in adults; More common in ♂ 5 Types: Well differentiated, Myxoid, Round Cell (rare, very aggressive), Dedifferentiated, Pleomorphic (Bizarre giant cells) Myxoid = chicken wire; Round Cell & Pleomorphic = bad prognosis Rapid growth Cell culture appearance Men = Women Nodular fasciitis (Benign Fibrous Tumor) Trauma? Volar aspect of forearm; Grows rapidly & tender Cell Culture Appearance with hemorrhage Dupuytren’s Conracture Palmar Fibromatosis (Borderline Fibrous Tumor) Alcoholism Diabetes Epilepsy Volar surface of hand Self-limited or Progressive; Doesn’t metastasize Estrogen Sensitive Other Increasing frequency with age More common in men Peyronie’s Disease Penile Fibromatosis (Borderline Fibrous Tumor) Penile Fibromatosis Self-limited or Progressive; Doesn’t metastasize Estrogen Sensitive Extra-Abdominal Fibromatosis (Borderline Fibrous Tumor) Shoulder & Chest Wall Self-limited or Progressive; Doesn’t metastasize Estrogen Sensitive Women More common in women Treat with radiation or Tamoxifen Infiltrative with 50% recurrence Women Childbirth Women of childbearing age following childbirth 25% Recurrance Herringbone Usually 30-55 yo males 39-54% survival with recurrence > 50% & mets > 25% Mets to lung, vertebral body & skull Frequent mitoses, pleomorphism & necrosis Abdominal Fibromatosis (Borderline Fibrous Tumor) Childbirth? Abdominal Wall Self-limited or Progressive; Doesn’t metastasize Estrogen Sensitive Intra-Abdominal Fibromatosis (Borderline Fibrous Tumor) FAP (Gardner’s Syndrome) Mesentery or Pelvic Wall Self-limited or Progressive; Doesn’t metastasize Estrogen Sensitive Retroperitoneal Fibromatosis (Borderline Fibrous Tumor) Compress aorta or ureters Self-limited or Progressive; Doesn’t metastasize Estrogen Sensitive Fibrosarcoma (Malignant Fibrous Tumor) Retroperitoneum or lower extremities Slow growing & painless; Hypoglycemia Fasiculated growth of spindle cells Fibrous Histiocytoma (Benign Fibrohistiocytic Tumor) Extremities, Solitary, Slow growing nodule Can look like Basal Cell Carcinoma Early to mid adult life Cured by excision; Deep lesions may recur Intradermal or SubQ proliferation of bland spindle cells Doesn’t invade epidermis, may cause hyperplasia Dermatofibrosarcoma protuberans (Borderline Fibrohistiocytic Tumor) Trunk & Proximal Extremities Soriform or cartwheel pattern? Slow growing followed by rapid progression Locally aggressive with 50% recurrence May rarely metastasize Diffusely infiltrates dermis & subcutis; can invade epidermis Malignant Fibrous Histiocytoma (Malignant Fibrohistiocytic Tumor) Lower extremity Most common sarcoma of late adult life Storiform: Cartwheel w/spindle histiocytes & giant cells Myxoid: Tumor cells & inflammatory cells around vessels Giant Cell: Histiocytes, Fibroblasts & Osteocyte like cells Inflammatory: Only in retroperitoneum (histiocytes & inflammatory) Soft Tissue Pathology (contd) Disease Cause/Risk Factors Symptoms Buzzwords Other Myxoid w/ Round & Spindle cells Rhabdomyoblast (eosinophillic tadpole cell) Head, Neck, GU Tract & Retroperitoneum Most common soft tissue tumor of kids Most common type of rhabdomyosarcoma Metrs to bone marrow (20%) Treat with surgery, radiation & Chemo Botryoid Malignant Rhabdomyosarcoma (Skeletal Muscle Tumor) Myxoid below epithelium Rhabdomyoblast (eosinophillic tadpole cell) GU tumor of young girls Nasopharynx, Bladder, Vagina, Bile Duct Variant of embryonal arising in hollow vscera “Bunch of Grapes” Metrs to bone marrow (20%) Treat with surgery, radiation & Chemo Alveolar Malignant Rhabdomyosarcoma (Skeletal Muscle Tumor) Extremities Rhabdomyoblast (eosinophillic tadpole cell) Round to oval cells with loss of cohesion Pleomorphic Malignant Rhabdomyosarcoma (Skeletal Muscle Tumor) Large, bizarre, multinucleate cells Extremities Few Rhabdomyoblasts Uncommon Appears in older patients Metrs to bone marrow (20%) Treat with surgery, radiation & Chemo Multiple & Painful Pilar arrector, genitalia, blood vessel, soft tissue & organ origin Solitary lesions cured by excision Smooth Muscle Tumor of Undetermined Malignant Potential STUMP (Intermediate) Bland spindle cells with elongated nuclei Atypia & Mitoses rare Hemorrhage & necrosis Uterine leiomyoma (fibroid) most common Leiomyosarcoma (Malignant SM tumor) Non-Specific: Weight loss, mass, N&V Elongate spindle cells with cigar nuclei Frequent mitoses & atypia Necrosis & Hemorrhage Females More common in females Arise from retroperitoneum or abdominal cavity Retroperitoneum: 29% 5 year survival Deep soft tissue: 64% 5 year survival Synovial Sarcoma (Malignant Synovial Tumor) Large joints (esp. knee) Palpable mass & pain; Focal calcification Biphasic: spindle fasicles & Cuboidal glands Almost herring-bone; Epithelial Antigen (EMA) t(X:18) Focal Calcification EMA & Cytokeratin Most common in adolescents & young adults t(X:18) Aggressive & recurrence: 28-36%; Mets: 50% May not arise from synovium! Tumor must arrive “fresh” Hemangioma (Benign Vascular Tumor) Looks like malformation/hamartoma Capillary, cavernous Embryonal Malignant Rhabdomyosarcoma (Skeletal Muscle Tumor) Leiomyoma (Beinign Smooth Muscle Tumor) Genetic? (AD) Girls t(2:13) & t(1:13) t(2:13) & t(1:13) Aggressive Metrs to bone marrow (20%) Treat with surgery, radiation & Chemo Infants & Children Hemangiopericytoma Benign & Malignant Angiosarcoma & Hemangiosarcoma (Malignant Vascular Tumor) Hepatic: Arsenic, PVC, Thorotrast Lymphan Kaposi’s Sarcoma Transplant AIDS-HSV8 European: Chronic Variable Clinical Course Ashkanazi Jews: Indolent Africans: Fatal Breast Pathology Disease Cause/Risk Factors Symptoms Buzzwords Other Acute Mastitis Nursing Cracks or Fissures in nipple Inflammation of duct, lobules or both Most Common Inflammation Acute Mastitis is most common Insipissation of secretions Chronic periductal inflammation Duct dilation with inflammatory cells Plugged ducts Older Women Duct Ectasia Mostly 5th and 67th decades Poorly defined ropy area Subareolar Abscess (Periductal Mastitis) Smoking? Painful red subareolar mass Recurrent with scarring Fat Necrosis Trauma Surgery Radiation Seatbelts, Underwire bras Hemorrhagic or grey-white necrotic area Signs of inflammation/repair Non-Proliferative Fibrocystic Change Syndrome Hormones? Single or multiple painful lumps; Calcification Changes in size with menstruation Brown to blue w/ Semi-transparent fluid Proliferative (without atypia) Fibrocystic Change Syndrome (Epithelial Hyperplasia) Hormones? Single or multiple painful lumps; Calcification Changes in size with menstruation Ductal & Lobular Hyperplasia Most common condition of female breast, no clinical significance 20-59 yo; Fibroadenomatosis: many small areas like fibroadenomas Risk of breast cancer = 1.5-2X that of non-proliferative change Proliferative (with atypia) Fibrocystic Change Syndrome (Epithelial Hyperplasia) Hormones? Single or multiple painful lumps; Calcification Changes in size with menstruation Ductal Hyperplasia & Atypia Lobular Hyperplasia (proliferation <1/2 acini) Most common condition of female breast, no clinical significance 20-59 yo; Fibroadenomatosis: many small areas like fibroadenomas Risk of breast cancer = 5X that of non-proliferative change 10X risk if family history Sclerosing Adenosis Hormones? Single or multiple painful lumps; Calcification Changes in size with menstruation Intralobular fibrosis (radial scar) & necrosis Small distorted acini Central Scar/Surround Ducts Most common condition of female breast, no clinical significance 20-59 yo; Fibroadenomatosis: many small areas like fibroadenomas Firm & confused with cancer Risk of breast cancer = 1.5-2X that of non-proliferative change Fibroadenoma Circumscribed, variable size; Calcification Myxoid to Hyalinized glands & stroma Most Common Benign Tumor Most common benign tumor of breast; young women Slight increased risk of cancer (esp w/ proliferative change) Phyllodes Tumor (Cystosarcoma Phylooides) Stroma more cellular than fibroadenoma Mitotic activity Highly Cellular Rare tumor resembling fibroadenoma May become malignant Tends to recur locally Smoking Trauma Best seen by FNA May mimic carcinoma Granulomatous Mastitis Silicone Reaction Most Common Overall Most common condition of female breast, no clinical significance 20-59 yo; Fibroadenomatosis: many small areas like fibroadenomas Epithelial lining with + change Fibrosis & Adenosis (↑ acinar units) Breast Pathology (contd) Disease Cause/Risk Factors Intraductal Papilloma Symptoms Buzzwords Other Papillary Polypoid growth in major duct Nipple discharge, bleeding, nipple changesa Subareolar nodule Bleeding! Discharge If solitary, not associated with cancer If Multiple, 1.5-2X risk of cancer Hard to distinguish from papillary carcinoma Intraductal Carcinoma Estrogen Excess BRCA1 & 2 P53 Geography & Diet Spreads throughout ducts; Can be multifocal Comedocarcinoma: high grade w/ necrosis Noncomedo: variable grades Infiltrating Duct Carcinoma Estrogen Excess P53 Geography & Diet BRCA1 (Medullary type) most common form hard with variable morphology Ductal Carcinoma In Situ (With Microinvasion) Estrogen Excess BRCA1 & 2 P53 Geography & Diet Rarely palpable Presents with calcification Lobular Carcinoma in Situ Estrogen Excess BRCA1 & 2 P53 Geography & Diet Non-invassive Monomorphic cells fill lobules Multifocal or bilateral Often Bilateral 9X risk of ductal or lobular invasive cancer Incidental finding Lobular Carcinoma Estrogen Excess BRCA1 & 2 P53 Geography & Diet Infiltrating “Indian File” Pattern Poorly circumscribed Often Bilateral Hard to detect Paget’s Disease of the Breast Estrogen Excess BRCA1 & 2 P53 Geography & Diet Tumor cells in Squamous epithelium of nipple Red and ulcerated nipple May be non-palpable Gynecomastia ↑ Estrogens or Gonadotropins Drugs (pot, HT meds, H2 blockers) Liver Disease Abnormal Overgrowth of ducts & surround tissue Non-Invasive; 1/3 of mammogram detected cacncers (increasing) Noncomedo: cribriform, solid, papillary, micropapillary Medullary = Good Prognosis Mucinous = Cells in Pools Medullary: pleomorphic sheets with lymph infiltrade, good prognosis Mucinous(Colloid): soft with pools of mucin, good prognosis Tubular: well differentiated & small, very good prognosis Papillary: rare but good prognosis Not progressive, but a risk for cancer Always associated with underlying carcinoma May be invasive or in-situ Ovary Pathology Disease Serous Cystadenoma (Surface Epithelial Ovarian Tumor) Cause/Risk Factors Symptoms Buzzwords Ciliated epithelium (Fallopian tube) Peg Cells Unilocular or Paucilocular cyst Cuboidal/Columnar Other Most common ovarian tumor, frequently bilateral Borderline Serous Tumor (Surface Epithelial Ovarian Tumor) Ciliated epithelium (Fallopian tube) Atypia; Cuboidal/Columnar Psammoma bodies No stromal invastion Psammoma Bodies Complex Papillary Growth Pattern Prognosis related to peritoneal implants Serous Cystadenocarcinoma (Surface Epithelial Ovarian Tumor) Ciliated epithelium (Fallopian tube) Atypia; Cuboidal/Columnar Psammoma bodies Stromal invastion Stromal Invasion Psammoma Bodies Commonest Malignant Tumor Complex Papillary Growth Pattern (Serous Papillary) Prognosis related to peritoneal implants Mucinous Cystadenoma (Surface Epithelial Ovarian Tumor) Intestinal or endocervical epithelium; large Mucinous Columnar Borderline Mucinous Tumor (Surface Epithelial Ovarian Tumor) Intestinal or endocervical epithelium; large Glandular & Papillary growth Atypia; Stratification of cells Mucinous Columnar Mucinous Cystadenocarcinoma (Surface Epithelial Ovarian Tumor) Intestinal or endocervical epithelium; large Very complex Looks like colonic adenoma with Dysplasia/CIS Mucinous Columnar Endometrioid Adenofibroma (Surface Epithelial Ovarian Tumor) Endometrial gland epithelium Squamous metaplasia Non-mucinous columnar Rare Borderline Endometrioid Tumor (Surface Epithelial Ovarian Tumor) Endometrial gland epithelium Squamous metaplasia Non-mucinous columnar Rare Endometrioid Adenocarcinoma (Surface Epithelial Ovarian Tumor) Endometrial gland epithelium Squamous metaplasia Non-mucinous columnar 20% of ovarian cancers 15% coexist with endometriosis 15-30% associated with carcinoma of endometrium 40% bilateral Clear Cell Adenocarcinoma (Surface Epithelial Ovarian Tumor) Endometrial pg Hobnail morphology Glycogen Rich Hobnail Poor Prognosis Considered a variant of endometrioid High grade, aggressive, rarely survive 5 years 40% bilateral Brenner Tumor (Surface Epithelial Ovarian Tumor) Bladder epithelium Mesothelial, Cuboidal, Stratified Unilateral Benign Most common transitional cell tumor Benign; May be associated with mucinous tumor 90% unilateral Borderline Brenner Tumor (Surface Epithelial Ovarian Tumor) Bladder epithelium Mesothelial, Cuboidal, Stratified Most common type of mucinous tumor May resemble adenoma of colon Malignant Ascites Pseudomyxoma peritonei (malignant mucinous ascites) Rare Ovary Pathology (contd) Disease Cause/Risk Factors Symptoms Buzzwords Other Transitional Cell Carcinoma (Surface Epithelial Ovarian Tumor) Bladder epithelium Mesothelial, Cuboidal, Stratified Granulosa Cell Tumor (Sex Cord-Stromal Tumor) Estrogenic (post menopausal bleeding) Coffee Bean Nuclei Microfollicles (Call-Exner Bodies) Coffee Bean Call-Exner Follicles Estrogen Usually post-menopausal; Risk of endometrial carcinoma Unilateral; May present with rupture (hemoperitoneum) Malignant but indolent course in 5-25% Intraabdominal recurrences after 10-20 years Thecoma-Fibroma (Sex Cord-Stromal Tumor) Estrogenic (uterine bleeding) Solid tumor of plump spindle cells Cytoplasmic lipid droplets Benign Unilateral Oil-Red-O Positive Estrogen Mixed granulose-theca tumor Risk for endometrial carcinoma Sertoli-Leydig Androblastoma (Sex Cord-Stromal Tumor) Tubules & Cords of sertoli & leydig cells Resemble immature testis 50% androgenic & virilizing Crystals Virilizing Stage I: well differentiated – benign All poorly differentiated or > Stage II: malignant Dysgerminoma (Germ Cell Tumor) Sheets of large primitive germ cells Stroma contains lymphocytes Some giant cells HCG Like Seminoma Endodermal Sinus Tumor (Germ Cell Tumor) Schiller-Duval Bodies Hyaline Globules AFP & AAT Schiller-Duval Bodies Choriocarcinoma (Germ Cell Tumor) Malignant syncitiotrophoblast capping malignant cytotrophoblast Rare in ovary, usually with other germ cell tumors Benign Cystic Teratoma (Dermoid) (Mature Teratoma) Peutz-Jeghers Pregnancy Rare HCG & HPL Skin with hair, sebaceous glands, muscle, bone, cartilage, neural tissue Infants-Children Radiosensitivity: good results Tumor Markers: HCG Usually in children Embryonal Yolk Sac Differentiation Tumor Markers: AFP & AAT Related to pregnancy in younger patients Must be distinguished from origin:uterine, tubular or ovarian Tumor Markers: HCG, HPL May spread to solid organs (unusual for most ovarian cancer) Derived from endoderm, ectoderm or mesoderm Most common ovarian tumor in 2nd-3rd decade Monodermal (Specialized) (Mature Teratoma) ex. Thyroid (Struma ovarii) Immature (Malignant) Teratoma CEA Can become Squamous Cell Ca Composed of fetal or embryonic tissue Behavior & Prognosis depends on grade (I-III) Malignant Degeneration of Mature Teratoma in older women Tumor Marker: CEA Embryonal Carcinoma AFP HCG HPL Rare in ovary (not rare in testis) Primitive, anaplastic tumor Tumor Markers: AFP, HCG, HPL in some Metastatic Carcinoma Krukenberg (GI) Usually from GI or breast Krukenberg tumor = bilateral mets (signet ring) from GI Tumor may stimulate stromal hyperplasia w/ ↑ E2 & AUB Ovary Pathology (contd 2) Disease Cause/Risk Factors Symptoms Buzzwords Follicular Cyst (Functional Cyst) Granulosa Cells secrete fluid high in Estrogen Estrogen Size < 5 cm Origin is follicles undergoing atresia Luteinized Follicular Cyst: stromal lining becomes luteinized Corpus Luteum Cyst (Functional Cyst) Fluid high in progesterone Lipid turns gelatinous; hemorrhagic Progesterone Follicle post-ovulation has delayed resolution of cavity Fibroblastic layer of CT with shell of luteinized theca Non-functional Cyst Predominantly serous Smooth Lined by Cuboidal “Simple Cyst” Inclusion of coelomic epithelium Para-Ovarian Similar to paratubal Chocolate Cyst Polycystic Ovary Disease Other Darkly Colored Obesity, 2 Amenorrhea, Hirsutism Anovulatory & Dismenorrhea; Infertility Bilateral ovarian enlargement, ↑ LH & E2, ↓ FSH Cysts w/ luteinized theca interna & fibrotic cortex Estrogen Obesity Amenorrhea Hirsutism Not a true cyst Chronic Anovulatory Syndrome (Stein Levinthal is a variant) 3.5-7% of women (3rd decade) Due to increased Estrogen Menometrorrhagia, Endometrial Hyperplasia & Adenocarcinoma Uterus Pathology Disease Cause/Risk Factors Symptoms Buzzwords Other Acute Endometritis Strep/Staph Post-Partum Post-Abortion Acute Inflammation + Necrosis Birth or Abortion Usually an ascending infection Chronic Endometritis PID Retained POC IUD Actinomyces/TB Plasma Cells Endometrial glands & stroma in myometrium Menorrhagia, Colicky dysmenorrheal, Dyspareunia & Pelvic Pain Adenomyosis Endometriosis Regurgitation? Metaplastic? Vascular or Lymphatic Dissemination Endometrial glands & stroma outside uterus Ovaries>Ligaments>Rectovaginal Septum> Pelvic Peritoneum>Scars Dysfunctional Uterine Bleeding No Corpus Luteum Production ↑ Estrogen Endometrial Hyperplasia Prolonged Estrogen stimulation Abnormal Uterine Bleeding Endometrial Polyp Hyperplasias? Tamoxifen Benign Proliferation of endometrial glands Abnormal Uterine Bleeding Infertility Causes Infertility, dysmenorrheal & Pelvic Pain Affects women in 3rd & 4th decade More common at beginning of menstrual life Excess Estrogen: Endocrine, Tumor, Obesity, Malnutrition Endocrine dependent – affects mitotic index Profuse bleeding, pain, impaired fertility Sharply circumscribed mass in myometrium Mitotic Index < 20, No necrosis, No/Mild atypia Leiomyoma (Fibroid) Endometrium in Myometrium Uterine Elnargement Simple Hyperplasia: Lowest risk for carcinoma Complex Hyperplasia: Less than 5% risk for carcinoma Atypical Hyperplasia: 25% associated with development of cancer Whorling Bundles Common (1 in 4 women); Esp common in black women Whorling bundles of smooth muscle Subtypes: Mitotically active, Cellular, Atypical, Myxoid, Neurilemoma-like & lipoleiomyoma Adenocarcinoma (Endometrial Carcinoma) Obesity, DM, ↑BP, Nulliparity, E2 Therapy, Anovulatory Cycles Atypical Hyperplasia Early Menarche/Late menopause Irregular bleeding Malignant glands Most common invasive GYN cancer 75% in post menopausal women Adenoacanthoma (Endometrial Carcinoma) Obesity, DM, ↑BP, Nulliparity, E2 Therapy, Anovulatory Cycles Atypical Hyperplasia Early Menarche/Late menopause Irregular bleeding Malignant glands, Benign Epithelium Younger women, related to hormones, better prognosis Adenosquamous Carcinoma (Endometrial Carcinoma) Obesity, DM, ↑BP, Nulliparity, E2 Therapy, Anovulatory Cycles Atypical Hyperplasia Early Menarche/Late menopause Irregular bleeding Malignant glands & Squamous epithelium Same or Worse prognosis than adenoacanthoma Clear Cell Carcinoma Grade III? Poor Prognosis Poor Prognosis Occur in older women without history of Estrogen Therapy Uterus Pathology (contd) Disease Papillary Serous Carcinoma Cause/Risk Factors Symptoms Buzzwords Grade III? Poor Prognosis Mucinous Carcinoma Other Poor Prognosis Occur in older women without history of Estrogen Therapy Occur in older women without history of Estrogen Therapy Grade I Endometrial Carcinoma Well Differentiated Easily Recognized Glandular Pattern Grade II Endometrial Carcinoma Moderately Differentiated Tumor in glands/solid sheets Grade III Endometrial Carcinoma Poorly Differentiated Mostly solid sheets Ex. Papillary Serous or Clear Cell Carcinoma Stage IA/B Endometrial Carcinoma Confined to Corpus Length of uterine cavity < 8 cm (A) Length of uterine cavity > 8 cm (B) 90% 5 year survival Stage II Endometrial Carcinoma Involves corpus & cervix 30-50% 5 year survival Stage III Endometrial Carcinoma Outside uterus but not outside true pelvis < 20% 5 year survival Stage IV Endometrial Carcinoma Outside true pelvis Involves mucosa of bladder ot rectum < 20% 5 year survival Malignant Mixed Mesodermal Tumors (MMMT) Malignant glands & stroma No necrosis? Poor Prognosis Postmenopausal women; Poor prognosis From stromal cells of mullerian mesoderm Homologous (tissue of origin native to uterus) Heterologous (Tissue of origin is foreign to uterus) Leiomyosarcoma Any Mitotic Index, coagulative necrosis, atypia Uterine Enlargement Most common uterine sarcoma; 40-60 yo From myometrium (malignant smooth muscle) Recur & Metastasize (hematogenously) Poor prognosis w/ 40% 5-year survival Endometrial Stromal Sarcoma Margin between tumor & myometrium Stromal Nodule (benign counterpart) Best prognosis From endometrial stromal cells; Mean age < 50 yo High grade: indistinct borders; Low grade: pushing borders 5 year survival is 50% Endolymphatic stromal myosis: penetrates lymph (50% recur) Fallopian Tube Pathology Disease Cause/Risk Factors Symptoms Buzzwords Usually unilateral Unicornuate uterus Aplasia Hypoplasia Other DES (a contraceptive) DES Rare Accessory orifices more common (failed tubal ligation) Duplication Acute Salpingitis (PID) 1º STD(Gonococcus-60%,Chlamydia) 2º Invasion due to local organisms (Strep, Staph, Coliforms, Anaerobes, post D&C/abortion, postpartum, IUD) Subacute Salpingitis (PID) Granulomatous TB Mycoplasma Viral Chronic Salpingitis (PID) Chlamydia? Mycoplasma? May be assymptomatic Open conduit/tubal damage by prior infection makes it succeptable Mural scarring with adhesions and occlusions Complication: Tubo-ovarian abscess (TOA), pyosalpinx, hydrosalpinx, infertility, ectopic pregnancy Ectopic Pregnancy PID Endometriosis Gestation outside endometrial cavity Pelvic/Abdominal Pain; Missed Menses ↑ HCG, Absent uterine gestational sac, mass 95% tubal, 2% maternal mortality Complications: Rupture, pregnancy loss, hemoperitoneum Fallopian Tube Cysts Para/Mesonephric remnants Trauma Surgery Fimbrial (hydatids of Morgagni), Ligamentous, Tubal Body Fallopian Tube Neoplasms Suppurative Infection of fallopian tube Pelvic Pain, Fever, Mucopurulent Discharge Chandelier Sign Mimics appendicitis Mimics Appendicitis Chandelier Sign Hydatids of Morgagni Repeat Infections cause scarring Complication: Sepsis (Arthritis, Meningitis Endocarditis, Peritonitis) Hydrosalpinx (healed acute) Common; < 4 cm in size Rare: Leiomyoma, Adenomatoid Tumor, Nerve sheath tumor Malignant: 1º Rare, 95% serous papillary adenocarcinoma from serous epithelium (poor prognosis) Mets: common; from GU, GI, pancreas & breast Placenta Pathology Disease Cause/Risk Factors Symptoms Buzzwords Other Succenturiate Lobe (Accessory Lobe) Vessel Rupture during delivery→Fetal blood loss Retention of lobe→postpartum bleeding/infection Bipartite Two equal lobes Placenta previa Placenta over cervical os Bleeding Associated with placenta acreta Placenta acreta Abnormally adherent to myometrium Placenta increta Villi grow into myometrium Complications: failure of separation, postpartum bleeding, rupture Placenta percreta Villi grow through uterine wall Complications: failure of separation, postpartum bleeding, rupture Velamentous Insertion Vessel compression or thrombosis Rupture during delivery→Fetal blood loss Single Uterine Artery Fetal Malformations Increased risk of fetal mortality Meconium Stain Pigmented macrophages in amnion/chorion Pigmented macrophages May be related to intrauterine fetal distress Large amounts can cause intrauterine asphyxia Amnion nodosum Amnion studded with nodules of cellular debris “Epithelial Plaques” with oligohydramnios cellular debris Associated with oligohydramnios (renal agenesis & immature lungs) Amniotic Band Syndrome Strings of amnion entangle limbs or digits Infarction Pregnancy-induced Hypertension Arterial supply unsupported across fetal membranes No Decidua Due to lack of deciduas Must be removed Complications: failure of separation, postpartum bleeding, rupture Difficult to distinguish from some chromosome abnormalities Interruption of blood supply from uterine arteries to placenta Placenta Pathology (contd) Disease Cause/Risk Factors Symptoms Abruptio placentae Pre-eclampsia Cocaine/Crack Abdominal Trauma Decreased blood to baby & increased pressure Low SES? Prolonged Rupture of Membranes Group B Strep (most common) Gram – Enterics, Staph, Anaerobes, Mycoplasma, Viruses, Candida Inflammation of membranes, chorionic plate, Cord(funisitis) & fetus; Evidence of aspiration Most common type of placental infection May result in abortion, stillbirth, malformations or neonatal infection High frequency of negative cultures Hematogenous Infection (transplacental) (T)oxoplasmosis (O)ther (R)ubella (C)ytomegalovirus (H)erpes Fever, Encephalitis, Chorioretinitis, Hepatosplenomegaly, Pneumonitis, Myocarditis, Hemolytic Anemia, Skin Lesions, Retardation Cataracts, Heart & Bone defects May result in abortion, stillbirth, malformations or neonatal infection Etiologic agent usually unknown Most parasitic, viral & a few bacterial infections enter via placenta Changes involve villi! Toxemia of Pregnancy Placental Ischemia (trophoblast failure) Vasoconstriction (Angiotensin, etc) DIC (Thromobxane) Small placenta Many large infarcts Retroplacental hematoma Organ Damage (liver, kidney, brain) Pre-eclampsia: Hypertension, Edema, Proteinuria (6% of pregnancy) Eclampsia: Seizures & Coma Treatment: Bedrest, diet, BP drugs, induction of delivery Dizygous Pregnancy Hereditary Release & Fertilization of 2 ova Dichorionic & Diamniotic + Fused Placenta Ascending (transcervical) Infection Acute Chorioamnionitis Buzzwords Other Premature seperation of placenta Partial or complete Usually occurs late Monozygous Pregnancy Single fertilized ovum Monochorionic/Diamniotic or Monochorioinic/Monoamniotic Vascular Anastomoses Occur with all monochorionic placentas Complete Hydatidaform Mole Gestational Trophoblastic Disease) 1st trimester bleeding, Hyperthyroidism Toxemia (25%), Hyperemesis gravidarum Hydropic villi, 46XX/Y (solely paternal) ↑ Uterus, trophoblastic proliferation & atypia Partial Hydatidaform Mole Gestational Trophoblastic Disease) Missed abortion, 69 XXX/Y, Embryo present ↓ uterus 18-20 weeks Treatment: D&C, follow HCG, physical exam, CXR Persistant GTD Either Metastatic or non-metastatic Risks: Initial HCG >100K, Uterus > 16 weeks, Ovaries > 6 cn, age > 50, Hyperthyroidism, Pre-eclampsia, DIC, pulmonary insufficiency & hyperemesis Non-metastatic & Good Prognosis: single chemotherapy 100% remit Unbalanced A→V shunt results in twin-twin transfusion syndrome 70% fatality ↑HCG Solely Paternal High risk of Permanent GTD Most common form of persistant or Metastatic GTD following mole Hydropic villi invade myometrium & metastasize to lung & vagina Risk of uterine perforation & hemorrhage Invasive Mole Choriocarcinoma Placental Site Trophoblastic Tumor 16-18 weeks High risk of persistant GTD Treatment: D&C, follow HCG, physical exam, CXR Pregnancy Hydatidaform mole Spontaneous abortion Ectopic pregnancy or teratoma Malignant neoplasm of trophoblast Persistantly elevated or rising HCG Abnormal Uterine Bleeding Symptoms related to mets Proliferation of intermediate trophoblast Abnormal uterine bleeding & enlargement HCG low, HPL high Mimics pregancy Most Serious HCG Hemorrhagic, necrotic nodules; no villi Made of plexiform masses of cytotrophoblast & syncitiotrophoblast Aggressive (invade blood vessels) Responsive to chemotherapy HPL Nodular mass of intermediate trophoblast Infiltrates endometrium & myometrium Resembles implantation site 90& benign, don’t to chemotherapy; hysterectomy is preferred Cervical & Vulvar Pathology Disease Cause/Risk Factors Symptoms Cervical Carcinoma HPV; Early age at first intercourse Many sexual partners; Immune Status High risk male partners; Inflammation Tobacco, Low Folate, OCPs; p53 Unexplained bleeding (esp. post coitus) Eye, mouth, larynx, tracheobronchial tree, esophagus, bladder, anus, genital tract lesions Koilocytosis, Multinucleate, Hyperkeratosis Human Papilloma Virus Condyloma acuminatum (HPV Lesion) HPV Verrucous lesion Multiple Perineal, Perianal, Vulva, Vagina or Cervix Flat Lesions (HPV Lesion) HPV Cervix Squamous Metaplasia HPV Replacement of glandular epithelium by Squamous Buzzwords Other E6 & E7 (from HPV) interact with p53 & RB genes Koilocytosis Infection always precedes cancer, but not sufficient to cause it Most women exposed to HPV at some time; Most regress Persistant infection is necessary for development of cancer HPV 16, 18, 31 & 45: high risk, integrate into DNA Usually just on Cervix Not Premalignant Not Premalignant Protective Low-Grade Squamous Intraepithelial Lesion (LSIL) Dysplasia in lower 1/3 of epithelium Same as Cervical Intraepithelial Neoplasia (CIN1) HPV cytologic change Treatment: Colposcopy High Grade Squamous Intraepithelial Lesion (HSIL) Dysplasia in lower 2/3 of epithelium (CIN 2) Dysplasia in most of epithelium (CIN 3) Dysplasia throughout epithelium (CIS) Basement membrane intact CIN 3 = Only most superficial layer is spared Treatment: Colposcopy, Biopsy, Endocervical Sampling Cone biopsy is done for persistant unexplained abnormality Atypical Squamous Cells Changes suggestive of SIL ASC of Undetermined Significance: HPV Triage or Colposcopy ASC can’t exclude HSIL: Colposcopy More difficult & harder to diagnose Treatment: Colposcopy & endocervical sampling; Endometrial sampling on women > 35 Atypical Endocervical cells: Cone biopsy Atypical Glandular Cells Microinvasive (Invasive Cervical Cancer) Squamous Cell Carcinoma (Invasive Cervical Cancer) Small Cell Carcinoma (Invasive Cervical Cancer) Invasive no more than 3 mm (IA1) or 3-5 mm (IA2) beneath BM Horizontal spread < 7mm No vascular space invasion Most Common Most common type (80%) 1) Large Cell nonkeratinizing (most common) 2) Large cell keratinizing Cervical & Vulvar Pathology (contd) Disease Cause/Risk Factors Symptoms Adenocarcinoma (Invasive Cervical Cancer) Buzzwords Other Increasing Incidence Increasing Incidence; HPV 18 most common Harder to detect (lower sensitivity on PAP) Adenosquamous Carcinoma (Invasive Cervical Cancer) Lichen Sclerosus (Vulvar Dystrophy) Grossly white & scaly plaque Discomfort & Pruritis Thinned epithelium with atrophy & fibrosis Squamous Cell Hyperplasia (Vulvar Dystrophy) Epithelial Thickening & Hyperkeratosis Grossly white & scaly plaque Discomfort & Pruritis White Plaque - Thickening Dyskeratosis, Atypia, Disturbed maturation Abnormal mitoses, No invasion Bowen’s Disease (CIS-VIN) Vulvar Intraepithelial Neoplasia HPV Vulvar Dystrophy Cervical & Vaginal Carcinoma Squamous Carcinoma of Vulva Keratinizing White Plaque - Thinning Elderly Collagen Layer Common in elderly Younger Women VIN I-III: Mild severe dysplasia (similar to cervix) CIS (or VIN III): Also known as Bowen’s Disease Mets to inguinal nodes Malignant Melanoma of Vulva Paget’s Disease of Vulva Intraepithelial or invasive Nabothian Cyst Inflammation Squamous Metaplasia (over glands) Cystically dilated endocervical glands Mucous filled cysts plugged by Squamous epithelium Endocervical Polyps Inflammation May cause bleeding Inflammation & Metaplasia Common Vulva, Vagina & Cervix Multinucleate cells with viral inclusions Risk to newborn babies Herpes Simplex II Yeast Infection Candida albicans Diabetes, Pregnancy, OCPs Cervical & Vulvar Pathology (contd 2) Disease Trichomonas vaginalis Chlamydia trachomatis Bacterial Infection Cause/Risk Factors Symptoms Buzzwords Other Small, pear or oval shaped with small nucleus Most Common Very frequent May spread to other gyn organs Cocci = abnormal Rods = normal Male GU Pathology Disease Cause/Risk Factors Symptoms Vesico-Ureteral Reflux Short intra-vesical portion of ureter Bladder Enlargement Abnormal Patency of Valve Incompetent Vesico-Ureteral Valve Regurgitation of urine into distal ureter Infection (pyelonephritis); Hydronephrosis; Chronic Renal Failure (Reflux Nephropathy) Non-Infectious Cystitis Cytotoxic Drugs (Cyclophosphamide) Ionizing Radiation Idiopathic (Interstitial Cystitis) Frequency, Lower Abdominal Pain, Dysuria, Hematuria, Urgency; No exudate/ulceration Inflammation, edema, hyperemia, hemorrhage Inflammatory cells on mucosa in lamina propria Infectious Cystitis Young ♀ (short urethra,hormonal, etc) Elderly ♂ (obstruction, catheters) Urinary Tract Abnormalities Diabetics Frequency, Lower Abdominal Pain, Dysuria, Hematuria, Urgency Calculi (Nephrolithiasis) Stasis (Obstruction, Diverticuli) Infection, Foreign Body, Metabolic Disease Urothelial Carcinoma Smoking, Industrial Dyes Analgesics, Cyclophosphamide Schistosoma haematobium Bladder>Renal Pelvis>Ureter>Urethra Papillary, Sessile, Flat (CIS) Painless Hematuria Increasing Incidence, Decreasing Mortality; Males>Females Urothelial in origin; Radiation Therapy is useless TCC (most) Squamous & Adenocarcinoma (rare); Mets to lymph Flat CIS tends to progress; Muscularis Propria Invasion is critical Acute Bacterial Prostatitis Pyogenic bacteria Intraprostatic Reflux of Urine Catheter, Biopsy, Hematogenous Diffuse suppurative inflammation Fever, Chils & Dysuria Necrotizing Inflammation with PMNs Microabscesses centering on glands and ducts Chronic Bacterial Prostatitis Pyogenic bacteria Intraprostatic Reflux of Urine Catheter, Biopsy, Hematogenous Indolent or Recurring Infection Insidious onset, recurring infection Dysuria, Perineal/Low Back Pain Antibiotics penetrate prostate poorly Lymphoplasmacytic infiltrate in stroma with macrophages Lymphocytes in stroma with age Chronic Abacterial Prostatitis Unknown Chlamydia/Mycoplasma Low Back Pain Absense of pyuria Presence of 10 PMNs/HPF Buzzwords No exudate/ulceration Cyclophosphamide Other Chronic: Thickening of wall with plasma cells from vessel damage Fungal & TB = granulomatous Hemorrhagic Cystitis: Cyclophosphamide Complications: Pyelonephritis, VUR, Calculi, CRF & fistulas Caused by: Bacteria (Coliforms, TB), Fungi (Candida, Torulopsis), Parasites (Schisto), Viruses (Adeno), Chlamydia & Mycoplasma Hemorrhagic Cystitis: bacterial & adeno infxn Arise in urinary bladder or renal pelvis, lodge at outflow narrowing Cpmplications: Hydronephrosis, Infection, Chronic Renal Failure Hard to distinguish from chronic bacterial prostatitis Granulomatous Prostatitis Non-infectious Induration of prostate (resembles cancer) Rare Due to immune response to secretions from prior bacterial infxn, massage, biopsy or instrumentation Palisading granulomas Nodular Hyperplasia (BPH) DHT Estrogens (Estradiol?) Proliferation of stroma & glands in mid-prostate Obstructed urinary tract (hesitancy & frequency) Lack prominent nucleoli Have prominent double layered lining No malignant potential; Disease of the elderly Nodules in transitional zone: yellow-pink, soft, milky exudate Nodules in periurethral zone: firm & rubbery Bladder Distended, ↑ Resid. Volume, Infection, Incontinence, VUR Prostatic Adenocarcinoma Age, Race, Family Hx Hormonal Diet 90% asymptomatic at diagnosis Back pain from vertebral mets Crystal Inclusions; High Free PSA No basal layer; Prominent nucleoli Most common cancer in males/2nd most common cancer death Peripheral>>Central>Transitional Grading is prognostic; Staging determines treatment Yellow, rubbery indurated nodules Prostatic Intra-epithelial Neoplasia Intraglandular malignant cells Basal Layer present No basal layer Precursor lesion to prostatic carcinoma Male GU Pathology (contd) Disease Cause/Risk Factors Cryptorchidism Symptoms Buzzwords Undescended Testicle Other Predisposes to infertility & testicular tumors Inflammation of Epididymis UTI Gonorrhea Chlamydia Congenital Defects/Obstruction Initially an acute inflammation with PMNs & edema, later abscess If chronic can cuse scarring and infertlility Inflammation of Testis UTI Syphilis Congenital Defects/Obstruction Less common than inflammation of epididymis Initially an acute inflammation with PMNs & edema, later abscess If chronic can cuse scarring and infertlility Torsion Violent movement Trauma Twisting of spermatic cord Cuts of f veins/arteries Vascular engorgement & veinous infarction Assymptomatic or painless enlargement Primitive germ cells with stromal lymphocytes Syncitial Giant Cells (produce HCG) Seminoma (Pure Germ Cell Tumor) Best Prognosis HCG – no AFP Most common Pure GCT Best prognosis Older patients (30s) Older age group (60s) Benign unless associated with a sarcoma Spermatocytic Seminoma Choriocarcinoma Hemorrhage & Necrosis HCG Aggressive - Metastatic HCG Embryonal Carcinoma Abortive gland formation Mixed GCT Hemorrhagic Yolk Sac Tumor (Endodermal Sinuys Tumor) Lace-Like Pattern AFP Yonger Patients AFP Embryonic-Placental line tumor Proliferation of primitive placental cells Most aggressive Rare in pure form Embryonal Line Anaplastic cohesive nest of cells Frequent component of mixed GCT Embryonal-Allantoic Line Most common tumor of infancts & children Good prognosis in children Usually associated with embryonal carcinoma in adults Embryonal-Somatic Line Cystic & Sclerotic Foci Components of all three germ layers In children: Pure & Benign; In adults: mixed & malignant Teratoma Hydrocele Neighboring infections/tumors Idiopathic Accumuation of serous fluid in tunica vaginalis Hematocele Trauma Torsion Bleeding Disorders Blood within tunica vaginalis Male GU Pathology (contd 2) Disease Cause/Risk Factors Trauma>? Lymphatic Obstruction Hypospadias Malformationo of urethral groove & canal Opening on ventral surface Epispadias Malformationo of urethral groove & canal Opening on dorsal surface Phimosis Prepucial orifice is too small to allow retraction Secondary infections/carcinoma Balanoposthitis Non-specific inflammation of shaft & foreskin HPV Benign tumorous growth Pedunculated Papillary growth Arund prepuce & coronal sulcus Koilocytic change & raisinoid nucleus Carcinoma in Situ HPV (16,17,etc) Squamous Malignancy confined to epithelium Full thickness Dysplasia High mitotic index Invasive Squamous Carcinoma Poor Hygeine; Lack of circumcision HPV infection Smegma Infiltrating nests of Squamous epithelia Atypia & mitotic figures Keratin pearls Bleeding & infection Verrucous Squamous Carcinoma Other Cystic accumulation of semen in spermatic cord Chylocele Condyloma acuminatum Buzzwords Dilated veins within spermatic cord Painful Varicocele Spermatocele Symptoms Opening may be constricted & cause obstruction/UTI Ejaculation may be hampered & cause infertility Forcible retraction may cause urethral constriction/urine retention Villous branching projections with fibrovascular cores Lined by Squamous epithelium with hyperkeratosis Squamous cells reveal perinuclear vacuolization Bowen’s Disease Bowen’s Disease: white/opaque plaques of shaft Erythroplasia of Queyrat: red velvety plaques on glans/prepuce Bowenoid Papulosis: multiple pigmented papules on younger pts Bowenoid = not progressive Papillary, Exophytic or verrucous (condyloma-like) Slow progression with local mets to inguinal nodes Special type of Squamous carcinoma Broad bulbous pushing margins with underlying tissue Good prognosis Although locally invasive, rarely metastasizes Bone & Joint Pathology Disease Osteoarthritis Rheumatoid Arthritis Cause/Risk Factors Symptoms Buzzwords Other Age Mechanical Trauma Weight Bearing Joints Hip, Knees, Lumbar & Cervical, PIP/DIP fingers Pain, Stiffness, ↓ ROM Osteophytes & Cysts PIP/DIP Most Common Progressive Erosion/Remodeling of Bone & Cartilage Autoimmune Juvenile Rheumatoid Arthritis Chronic Systemic Inflammatory Disease of Joints Women>Men, Younger age of onset IgM to IgG (RF) Skin (Nodules), Vessels, Heart, Lungs, Etc Proliferative, non-suppurative synovitis; Joint ankylosis Metacarpophalangeal Systemic Polyarthritis, Rheumatoid Factor Fibrinoid Necrosis with inflammatory collar Nodules on extensor surface/viscera Pain, Stiffness, Swelling, MCP Joints Rx: NSAIDS, Analgesics, DMARDS, Immunosuppresion, anti-TNF Systemic Presentation precedes Joints Fever, Hepatic & Lymph Node Enlargement Seronegative for RF ANA Large Joints Fewer Joints than RA Called “Still’s Disease” in adults Ankylosing Spondyloarthritis (Marie-Strumpell Disease) (Seronegative Spondyloarthopathy) HLA-B27 Infection Axial Joints (Sacroiliac) Low Back Pain; Bamboo Spine Aortic Insufficiency Lung Fibrosis & Uveitis Adolescent Boys Reactive Arthritis (Reiter Syndrome) (Seronegative Spondyloarthopathy) HLA-B27 Infection (GI & GU Bacteria) Arthritis, Urethritis & Conjunctivitis Arthritis waxes & wanes Enteropathic Arthritis Bowel Infection HLA-B27 Abruptly appearing arthritis Knees & Ankles Arthritis lasts ~ 1 year Psoriatic Arthritis Sausage Digits Iritis & Conjunctivitis Less Severe & More Remitting 5% of Psoriatic Population Acute Arthritis: PMNs in synovium Chronic Tophaceous: Fibrotic synovium & cartilage destruction Gouty Nephropathy: uric acid stones in renal interstitium Rx: NSAIDS, allopurinol, colchicine Gout Primary Secondary (Malignancy or Metabolic) Familial, Male, Age, Purines, Alcohol Obesity, Thiazides, Lead, ↑ BP Hyperuricemia Tophi (urate crystals & inflammatory cells) Secondary Pyelonephritis Bone erosion & loss of joint space Chondrocalcinosis (Pseudogout) Age Sporadic (trauma) Heriditary (8q) Hyperparathyroid Calcium Pyrophosphate Inflammtory infiltrate (PMNs) causes damage Staph, Strep, Gonococci, H. influenzae, Gram - rods Fever, Pain, Swelling ↑ WBC, ESR, CRP Sudden swollen, painful w/ ↓ ROM Usually a single joint Corticosteroid Arthopathy Hemochromatosis/Hemosiderosis (Pigmentary Arthropathy) Bacterial Arthritis H. influenzae in children Staph in older children/adults Gonococcus in young adults Bone & Joint Pathology (contd) Disease Cause/Risk Factors Symptoms Tuberculous Arthritis TB Usually weight bearing joints Synovium grows as pannus Viral Arthritis Parvo B19 Rubella HCV HIV Variable Lyme Disease Borrelia burgdorferi Symptoms within weeks to years of disease onset Usually one or two large joints Buzzwords Other Hematogenous from viscera or adjacent osteomyelitis Ganglion Small cyst near joint capsule or tendon sheath Wrist Synovial-like Fluid Cystic or myxoid degeneration of connective tissue Synovial Cyst Herniation of synovium through capsule Baker’s Cyst in RA Pigmented Villonodular Synovitis Giant Cell Tumor of Tendon Sheath Pain, locking, recurrent swelling Benign proliferation of joints, tendon sheats, bursa Most common mesenchymal neoplasm of hand Synovial Sarcoma Large joints (knee) Palpable mass & pain in 50% t(x:18) Focal calcification Less than 10% are intraarticular More common in adolescent males Mets in 50%; Aggressive in 1/3 Biphasic: Spindle Cells in Fascicles, Columnar/Cuboidal in glands Pathologic Fracture: Diseased Bone Compund Fracture: Broken Skin Stress Fracture: Repetative Minimal Injury Comminuted Fracture: Bone Fragmented Most common bone disorder Hematoma, Fibrosis, Callus, Woven Bone, Remodeling Bone Fractures Jagged edges Lacks nuclei Necrotic Bone Osteoporosis Adolescents Age Genetics ↓Vit D, Calcium, Estrogen Decreased bone mass, Fracture, Pain Vertebral Column, Femoral Neck, Wrist Osteomalacia/Rickets Vitamin D Deficiency Defective Mineralization Osteopenia Fractures Renal Osteodystrophy Skeletal Changes Chronic Renal Disease Loss of transverse trabeculae ↑ Osteoclast, ↓Osteoblast activity Rx: SERMs, Diphosphonates, Calcitonin ↑ Serum: Alk Phos & PTH ↓ Urine: Ca ↓ Serum: Ca, P, Vit D ↑ Urine: P Phosphate Retention, Hypocalcemia, abnormal Vit D metabolism Metabolic Acidosis, Aluminum Deposition Bone & Joint Pathology (contd 2) Disease Cause/Risk Factors Symptoms Buzzwords Osteitis Deformans (Paget’s) Viral? (Paramyxo, Measles) Abnormal Remodeling of Bone Mosaic Pattern & Cement Lines PAIN! – due to nerve compression High cardiac output Mosaic Pattern & Cement Lines Osteomyelitis Pyogenic, TB, Viral, Dungal Parasitic Trauma or Hematogenous spread Immunosuppression & DM Fever, Malaise, Pain, ↑ WBC, ESR, CRP Acute purulent inflammation & necrosis Repair by fibrosis & new bone Squamous Cell Carcinoma in sinus tract Bacterial Osteomyelitis Staph (all ages); Gram- (drug abusers) H influenze/Group B Strep (neonates) Salmonella (Sickle Cell) Group G Strep (alcoholics, diabetics) Mostly polyostotic Pelvis, Long Bones, Spine, Skull; Older Males Phases: Osteolytic, Mixed, Osteosclerotic Acute or Chronic Not HIV/AIDS Metaphysis common Sequestrum (old necrotic) Involucrum (new bone sleeve) Salmonella = Sickle Cell Tuberculous Osteomyelitis TB Chronic-Occult (from lung or viscera) Monostic (usually spine) Inguinal Mass (iliopsoas or psoas abscess) Pain, fever, malaise, weight loss Avascular Necrosis (Septic or Idiopathic Osteonecrosis) Corticosteroid, Alcohol, Radiation Hemoglobinopathies, Coagulopathy Vasculitis, Pancreatitis, Caisson Disease, Gaucher’s Disease Femoral Head Pain & Secere secondary osteoarthitis Chronic Corticosteroids Osteochondroma Heriditary? Exophytic, Painless Metaphysis of long bones Pedunculated or broad base Cartilage Cap, Echondral ossification Painless Pott’s Disease = TB in spine Malignancy rare Most common neoplasm of cartilage Children, Adolescents, Young adults Malignancy rare Multiple Chondromatosis = Ollier Disease Hands & Feet Radiolucent nodules of cartilage Echondroma-Echondromatosis Other Osteoid Osteoma Nocturnal Pain – responds to Asprin/NSAIDs Appendicular – arms & legs Nocturnal Pain Benign tumor of children & young adults Radiolucent osteid nidus surrounded by dense reactive bone Osteoblastoma Like osteoid osteoma Usually in vertebrae Adults Larger mass in adults Malignant potential; Recurs Finrous Dysplasia of Bone Bone replaced by fibrous tissue/woven bone Painless Limb Distortion & Fracture No osteolblasts No osteoblasts Usually monostotic (ribs, skull, long bones) Adolescents McCune-Albright Syndrome Café-au-lait spots Endocrinopathy Polyostotic Metastatic Breast, Prostate, Lung, Thyroid Kidney Multifocal (Thyroid & Kidney solitary) Pain, Fracture, ↑ Calcium & Alk Phos Spine, Pelvis, Ribs, Skull, Humerus, Femur Lytic or blastic (prostate): most mixed Rare Most Common Myelophthisis = marrow infiltration Bone & Joint Pathology (contd 3) Disease Cause/Risk Factors Symptoms Buzzwords Other Pain, Mass, ↑ Alk Phos Mets to lungs Metaphysis, periosteum long bones (knee) Most common primary bone forming tumor Young or elderly Malignant bone & osteoid Treatment: Surgery & Chemotherapy Chondrosarcoma Pain, Mass, Slow Growing Wide Distrubution: Pelvis, Shoulder, Ribs, Legs Mets to lungs Older patients with osteosarcoma Malignancy hard to assess Ewing’s Sarcoma Mass, pain, fever, ↑ WBC, ESR, anemia Small Round Blue Cell Tumor Anemia Multiple Myeloma Spine, Ribs, Pelvis, Skull Monoclonal Gammopathy (M Protein) Pain, Lysis, Fracture, Anemia, ↑ Calcium Fever, Weight Loss, Amyloid M-Protein Bone Resorption (Osteitis fibrosa cytica) Cortical Bone Brown Tumor Brown Tumor Von Recklinghausen’s Osteosarcoma Hyperparathyroidism Hypoparathyroidism Rb P53 Paget’s, Infarcts, Radiation Adenoma, Hyperplasia Hypocalcemia Children (most with translocation) Medullary cafvity of femur & pelvis Lytic destruction & periosteal reaction Treatment: chemo, radiation, surgery Widespread prolideration of plasma cells ↑ Serum: Ca, Alk Phos, PTH, Vit D ↑ Urine: Ca & P ↓ Serum P ↑ Serum: P ↓ Urine: Ca & P ↓ Serum: Ca, PTH, Vit D No Change: Alk Phos Genetic Pathology Disease Cause/Risk Factors Symptoms Buzzwords Down Syndrome Trisomy 21 (47, XX, +21) Mosaicism (46,XX/47,XX+21) Unbalanced Translocation Flattened back of head & facial profile, upslanted eyes, epicanthal folds, flat nasal bridge, Small ears, protruding tongue, short neck, single palmar crease, short stature, gap between toes Palmar Crease Protruding Tongue Upslanted Eyes Trisomy 18 Trisomy 18 (47,XX,+18) Mosaicism (46,XX/47,XX+18) Low Birth Weight, Failure to Thrive Hypertonia, Weak Cry, Poor Suck, Apnea Microcephaly, Low set ears, overlapping fingers Rocker Bottom Feet Rocker Bottom Feet Low Birth Weight Trisomy 13 Trisomy 21 (47, XX, +13) Mosaicism (46,XX/47,XX+13) Unbalanced Translocation Normal Birth Weight, Failure to Thrive Holoprosencephaly, Hypotonia, apnea, Seizures, Hearing Loss, Microcephaly, Close eyes, Cleft Lip/Palate, Polydactyly Turner Syndrome 45X; 46X,i(X)(q10); 46Xdel(X)(p) 46Xdel(X)(q); 46Xr(X) 45X/46XX; 45X/46XY Short at birth, webbed neck, lymphedema over dorsum of hands/feet Shield Chest, Pigmented nevi, Minimal breasts ↑ FSH & LH, ↓ E2; Infertility 47, XXX XXX Tall ↑ risk for chromosome abnormalities in offspring Slightly lower IQ – need special education Behavior Problems Kleinfelter Syndrome 47, XXY Mosaicism Small testes, Infertility Tall stature, long legs, Behavior Problems Gynecomastia; Lower IQ – special ed Low DHT, High FSH & E2 47, XYY XYY Tall, cystic acne, large teeth ↑ risk for chromosome abnormalities in offspring ↑Distractability ↓ Impulse Control Fragile X Syndrome Fra X (q27.3) Full Mutation = > 200 CGG repeats Large Head, Large Ears, Strong Jaw, High Palate Lax Eustachian Tubes, Hyperflexible Joints Mitral Prolapse, Macroorchidism ADHD, Repetitive Speech, Autistic-like Inherited Mental Retardation Most Common Inherited Cause of Mental Retardation Less severe in females Sherman Paradox: Assymptomatic carriers have problems w/ age Neurofibromatosis Type I (Von Recklinghausen Disease) NF-1 Neurofibromas with button-hole effect Pigmented Skin Lesions (Café au-lait) Lisch Nodules (iris hamartomas) Button-hole effect NF-1 = tumor suppressor gene Marfan’s Syndrome FBN1 Skeletal Changes Ocular Changes (ectopia lentis) Cardiovascular Changes (Mitral Valve Prolapse) Defective fibrillin Tay-Sachs Disease (Sphingolipidosis) Hexosaminidase A Deficiency (Splice site or frameshift mutation) GM2 Ganglioside Accumulation Motor/Mental Deterioration - Death at age 2-3 Cherry Red spots on macula Neurons have lisosomes filled with gangliosides -1,40Glucosidase Deficiency Glycogen Accumulation Cardiomegaly Hepatomegaly (mild) Muscle hypotonia Pompe Disease Type 2 (Glycogenosis) Polydactyly Other VSD, ASD & AV Canal; Duodenal Atresia, Leukemia, Hypothyroidism, Poor immunity, Hearing loss, Strabismus, Myopia, Mosaicism = Milder VSD, ASD, Polyvalvular Dysplasia, Esophageal Atresia, Imperforate Anus, Cryptorchidism High mortality ASD,VSD,PDA, Dextrocardia, Omphalocele, Intestinal Malrotation Cystic Kidneys, Scalp Defects & Hemangiomas Common; 99% of 45X spontaneously abort; 45X/46XY = risk for gonadoblastoma Coarctation of aorta, bicuspid aortic valve, aortic stenosis Hypertension, Hypothyroidism, DM No tendency for criminal behavior Genetic Pathology (contd) Disease Cause/Risk Factors Symptoms Buzzwords Gaucher Disease (Sulfatidosis) Glucocerebrosidase Deficiency Glucocerebroside Accumulation Type I: Splenomegaly & Bone Type II: Infants (early death) Type III: Juveniles, CNS Most Common Metachromatic Leukodystrophy (Sulfatidosis) Arylsulfatase A Deficiency Sulfatide Accumulation Motor defecits (death in 10 years) Demyelination causes gliosis MPS I (Hurler Syndrome) (Mucopolysaccharidosis) a-L-iduronidase Deficiency Heparan & Dermatan Sulfate Accumulation Skeletal Deformities & Corneal Clouding Mental Retardation, Joint Stiffness, HSmegaly Umbilical Herniation, Heart Problems Corneal Clouding MPS II (Hunter Syndrome) (Mucopolysaccharidosis) a-L-iduronidase Deficiency No corneal clouding X-Linked Milder X-Linked I-Cell Disease (ML-II) (Mucolipidosis) N-acetylglucosamine-1-P-transferase Hurler-like ↑ Hexosaminidase B & Iduronate Sulfatase Inclusion bodies in fibroblasts Von Gierke Disease Glucose-6-Phosphatase Deficiency Glycogen Accumulation Hypoglycemia, Hepatomegaly Hyperlipidemia, Hyperuricemia Hepatic Glycogen Storage Disease McArdle Disease Glucose-6-Phosphatase Deficiency Muscle Cramps after exercise Failure to raise lactate levels Muscle Glycogen Storage Disease Lesch-Nyhan Syndrome (X-Linked Recessive) HGPRT Deficiency CNS Problems – Mental Retardation Self Mutilating Hyperuricemia, Gout, Renal Stones Orange Sand in diaper Xeroderma Pigmentosum Defective Nucleotide Excision Repair XPA, XPB, XPC, XPD, XPE, XPF, XPG Also XPV (DNA Synthesis) Hypo/Hyperpigmentation of the Skin Neurological Abnormalities ↑ BCC, SCC & Melanoma & internal cancer Clouding of cornea, atrophy of eyelid Cockayne Syndrome Transcription Coupled Repair Defect CSA or CSB Sunlight Sensitivity, Progeria, Growth Failure Neurological Defects, Dental Defects, Cataracts Typical Facies & Dwarfed Long arms & Legs, Sunken Eyes XP/CS Defective Excision Repair & Transcription XPB, XPD or XPG Sun Sensitivity of XP Growth Abnormalities of CS HNPCC Inheritance of Colon Tumors hMSH2, hMSH3, hMSH6 (mutS) hMLH1, hPMS1, hPMS2 (mutL) Microsatellite Instability-Mismatch Repair Defect Spontaneous Mutations Endometrial, Gastric, UT, Ovarian & Colon Tumors Other Most Common Lysosome Storage Disease Problem in macrophages Treatment: Enzyme replacement, Bone Marrow Transplant Late infantile form is most common type Detected with dyes Self Mutilation Orange Sand Normal at birth, rapid deterioration at 6 mos 6-10 year life expectancy without BM transplant Remove all teeth UV Light Induced Pyrimidine DImers cause damage Skin cancer within first decade Autosomal Recessive No cancer Growth Abnormalities Typical Facies No cancer predisposition Early Death (12 years) Autosomal Recessive Sunlight sensitivity due to defective excision repair XPB & XPD are part of Transcription Factor TFIIH Autosomal Recessive AD Autosomal Dominant – early loss of remainig good allele Cancer Genetics Pathology Disease Cause/Risk Factors Symptoms Buzzwords Other Sis Protooncogene Encodes PDGF Inappropriately expressed by Carcinomas causing cell growth HER2/neu Encodes EGF Receptor Overexpressed in Breast & Ovarian Cancer (Can be treated with Herceptin) Ret Oncogene c-abl Oncogene Constiutively signals in Thyroid Carcinoma in absence of GF Encodes a Tyrosine Kinase Abnormal cell localization in CML t(9:22) A fusion gene with bcr/c-abl Required for signal transduction by growth factor receptors Mutated at codons 12 & 13 Most mutated oncogenes Ras Oncogene NF1 A GTPase activating Protein (GAP) (turns of Ras) Missing in melanoma and Neurofibromatosis APC Regulates -Catenin (cell contact signaling) Defective in colorectal cancer & benign intestinal polyps In Familial Intestinal Polyposis C-Myc A transcription factor Placed next to immunoglobulin heacy chain in Burkitt’s Lymphoma T(8:14) L-Myc A transcription factor In Lung Tumors N-myc A transcription factor In Neuroblastomas Rb Master regulatory protein Controls entry into cell cycle Unphosphrylated form binds (inactivates) E2F transcription factor Phosphorylated by Cyclin/CDK; Controlled by CDK Inhibitors Inactivated in Retinoblastoma, Osteosarcoma & by HPV E7 protein Bcl-1 Cyclin D1 gene Overexpression causes Rb inactivation Inactivated in Mantle Cell Lymphoma by t(11:14) Cancer Genetics Pathology (contd) Disease hMSH1, hMSH2 Caspases 3,6 & 7 Cause/Risk Factors Symptoms DNA Repair genes Buzzwords Other Defective in Heriditary Nonpolyposis Colorectal Cancer (Rapid cancer progression) Cause apoptosis Fas A death receptor in the extrinsic apoptosis pathway Tumor Necrosis Factor A death receptor in the extrinsic apoptosis pathway Bcl A pro-apoptotic protein in the intrinsic apoptosis pathway Opens mitochondrial membrane pores Cytochrome C A pro-apoptotic molecule in the intrinsic apoptosis pathway Released from mitochondria Activates Apaf-1 Apaf-1 A pro-apoptotic molecule in the intrinsic apoptosis pathway Activates initiator caspases to cleave effector caspases Translpant Pathology Disease Cause/Risk Factors Symptoms Buzzwords Other Immediate (seconds to minutes) Clot formation and occlusion Rare Due to preformed HLA antibodies directed against HLA class I Results from pregnancies, transfusions or previous transplants Activated complement attracts PMNs and damages endothelium Acute Rejection Weeks to months Most common type of rejection Cellular: Mediated by cytotoxic T cells Humoral: Antibodies made against HLA Type I antigens Treatment: Immunosuppression or Plasmapheresis Chronic Rejection Lungs: Obliterative Bronchilitis Liver: Bile Duct Disappearance Kidney: Scarring All patients have chronic rejection, but few get organ failure Damage primarily against arteries Circumferential intimal fibrosis & lumen narrowing Graft Versus Host Disease Fibrosis of skin Cholestasis of liver Strictures in GI Infection Caused by Contaminating Donr Lymphocytes Balanced required: Too few donor T cells = no engraft Hyperacute Rejection Usually occurs < 6 months after transplant First month = endogenous flora After first month = opportunistic flora Infection Cytomegalovirus Lung: Interstitial Pneumonia Liver: Acute Hepatitis GI: Esophagitis, Gastritis, Diarrhea Most common viral infection in transplant patients Cellular enlargement, basophilic intranuclear inclusions, halo, eosinophilic cytoplasmic inclusions Aspergillus Branching septate hyphae Silver Stain Blood Vessel Occlusion Most commonly in neutropenic BM transplant patients Hard to treat Squamous Cell Carcinoma Herpes Simplex Virus I Skin and Lip Squamous Cell Carcinoma HPV Cervix Kaposi’s Sarcoma HHV 8 Post Transplant Lymphoproliferative Disorders EBV OKT3 Highest incidence in Lung & Heart B Lymphocyte Infection Plasmacytic Hyperplasia: Polycolonal; Oropharync & Lymph Polymorphic B Cell: Monoclonal; Lymph or Extradnodal Lymphoma & Multiple Myeloma: Monoclonal (malignant)