GMEC Minutes 1-22
advertisement
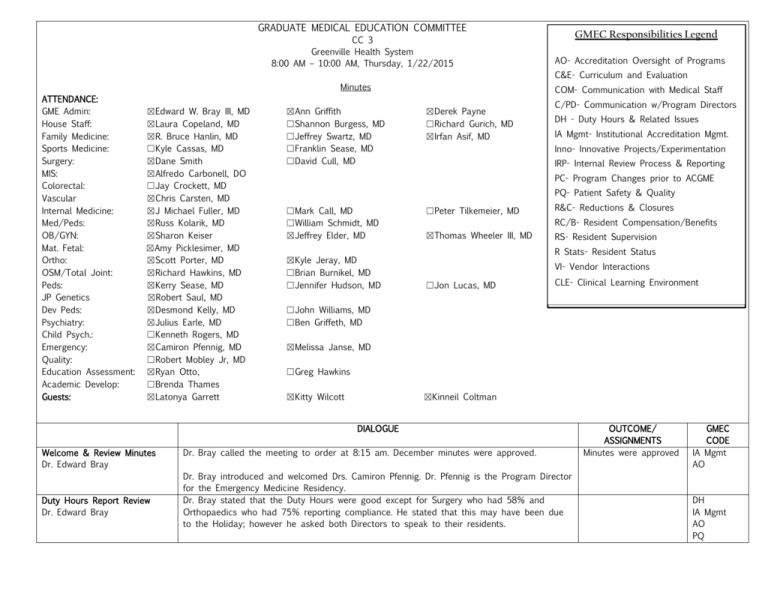

GRADUATE MEDICAL EDUCATION COMMITTEE CC 3 Greenville Health System 8:00 AM – 10:00 AM, Thursday, 1/22/2015 GMEC Responsibilities Legend AO- Accreditation Oversight of Programs C&E- Curriculum and Evaluation Minutes ATTENDANCE: GME Admin: House Staff: Family Medicine: Sports Medicine: Surgery: MIS: Colorectal: Vascular Internal Medicine: Med/Peds: OB/GYN: Mat. Fetal: Ortho: OSM/Total Joint: Peds: JP Genetics Dev Peds: Psychiatry: Child Psych.: Emergency: Quality: Education Assessment: Academic Develop: Guests: ☒Edward W. Bray III, MD ☒Laura Copeland, MD ☒R. Bruce Hanlin, MD ☐Kyle Cassas, MD ☒Dane Smith ☒Alfredo Carbonell, DO ☐Jay Crockett, MD ☒Chris Carsten, MD ☒J Michael Fuller, MD ☒Russ Kolarik, MD ☒Sharon Keiser ☒Amy Picklesimer, MD ☒Scott Porter, MD ☒Richard Hawkins, MD ☒Kerry Sease, MD ☒Robert Saul, MD ☒Desmond Kelly, MD ☒Julius Earle, MD ☐Kenneth Rogers, MD ☒Camiron Pfennig, MD ☐Robert Mobley Jr, MD ☒Ryan Otto, ☐Brenda Thames ☒Latonya Garrett ☒Ann Griffith ☐Shannon Burgess, MD ☐Jeffrey Swartz, MD ☐Franklin Sease, MD ☐David Cull, MD COM- Communication with Medical Staff ☒Derek Payne ☐Richard Gurich, MD ☒Irfan Asif, MD C/PD- Communication w/Program Directors DH - Duty Hours & Related Issues IA Mgmt- Institutional Accreditation Mgmt. Inno- Innovative Projects/Experimentation IRP- Internal Review Process & Reporting PC- Program Changes prior to ACGME PQ- Patient Safety & Quality ☐Mark Call, MD ☐William Schmidt, MD ☒Jeffrey Elder, MD ☒Kyle Jeray, MD ☐Brian Burnikel, MD ☐Jennifer Hudson, MD ☐Peter Tilkemeier, MD R&C- Reductions & Closures RC/B- Resident Compensation/Benefits ☒Thomas Wheeler III, MD RS- Resident Supervision R Stats- Resident Status VI- Vendor Interactions ☐Jon Lucas, MD CLE- Clinical Learning Environment ☐John Williams, MD ☐Ben Griffeth, MD ☒Melissa Janse, MD ☐Greg Hawkins ☒Kitty Wilcott ☒Kinneil Coltman DIALOGUE Welcome & Review Minutes Dr. Edward Bray Duty Hours Report Review Dr. Edward Bray Dr. Bray called the meeting to order at 8:15 am. December minutes were approved. Dr. Bray introduced and welcomed Drs. Camiron Pfennig. Dr. Pfennig is the Program Director for the Emergency Medicine Residency. Dr. Bray stated that the Duty Hours were good except for Surgery who had 58% and Orthopaedics who had 75% reporting compliance. He stated that this may have been due to the Holiday; however he asked both Directors to speak to their residents. OUTCOME/ ASSIGNMENTS Minutes were approved GMEC CODE IA Mgmt AO DH IA Mgmt AO PQ House Senate Report Dr. Laura Copeland ACGME Communications Dr. Edward Bray Resident Salary Approval Edward Bray, MD Kitty Wilcott Dr. Copeland stated that the Business in Medicine financial workshop and disability insurance policy information was well received by the House Staff. Dr. Copeland reported that there is a big gap in what residents perceive and what the GHS institution perceives regarding patient safety issues. She spoke specifically about the number of lost orders or lost and deleted labs. She would like to obtain a description of circumstances and identify the scope of circumstances regarding these areas. Dr. Copeland asked the program directors to encourage residents to document any complaints regarding this issue. Dr. Kerry Sease asked if they are to be using event reporting shouldn’t this information be captured that way? Dr. Copeland answers that she is not discouraging the use of event reporting system, but she doesn’t think that investigations are taking place especially with orders. Dr. Scott Porter stated having residents use event reporting system and another tracking method would cause redundancy. Dr. Sharon Keiser stated someone that works with event reporting system needs to present to GMEC so this issue can be communicated. Dr. Bray stated that a representative from the events reporting system will need to attend the House Staff Senate Meeting to discuss this issue. Dr. Russ Kolarik stated that he does not receive any reports after something is submitted in events reporting system. He would like for them to come back to GMEC and address this issue. Dr. Copeland states that she was told that the residents should be following up to ensure orders and labs are done. She states that this is not practical with the work load. Dr. Bray said that this was a major issue in the CLER report and we will have a citation if no improvements are made. Dr. Bray relayed to the group that ACGME had continued the full accreditation of Orthopaedics (Dr. Scott Porter) and Orthopaedic Sports Medicine (Dr. Richard Hawkins). Dr. Porter also stated that were approved for an increase of 1 compliment. Dr. Bray reported that ACGME are beginning a new system and they are contacting each program with regard to the process. Someone from the Events Reporting System will present at GMEC and to the House Senate Meetings. Kitty Wilcott reported that after comparison of resident salaries and discussion with Dr. Bray, there is recommendation for raises for PGYI, PGYII and PGYIII.. Ms. Wilcott stated that according to the national compensation rates from AHEC that GHS salaries are lower than average. As a result, a 1.35% pay increase is proposed as of last GMEC meeting. The Program Directors asked for additional benefit comparison information which they did receive and has been posted on GMEC SharePoint. GMEC voted to approve the proposed salary increase of 2% for the first 3 PGY years then 1% following that. GMEC voted to approve the proposed salary increase. No one opposed the increase. IA Mgmt AO IA Mgmt AO IA Mgmt AO C/PD RC/B 2 Academic Council Update Derek Payne CLER Moment: Quality Interactions Demo Kinneil Coltman Derek Payne reported that the Physician Assistant Program for North Greenville has been put on hold until 2020. The nursing program with Clemson is scheduled to start in the Fall 2015. Mr. Payne stated that Clemson Advisory Board was being established and will include the partnering institutions and community members. He reported the first meeting will take place Feb. 3rd. Mr. Payne spoke regarding the financials submitted for expansions and states that a budget will be compiled in March. Ms. Kinneil Coltman, Chief Executive Diversity Officer, discussed a new computer based training (CBT) option for residents and interns that would provide realistic evidencebased case experience in diversity and cross cultural care. Ms. Coltman facilitated a demonstration of the CBT with the assistance of Dr. Joseph Betancourt of Harvard Medical School and Massachusetts General Hospital. Ms. Coltman explained that unlike other CBTs this training is totally interactive where the resident can propose different care options and receive evidence-based guidance regarding their proposal of care. IA Mgmt C/PD Com C&E Ms. Coltman will gather more information regarding the proposed as well as other CBT or programs offered for this quality requirement. C&E C/PD PQ CLE Dr. Betancourt is the Director, The Disparities Solutions Center, Massachusetts General Hospital and the Co-Founder of Quality Interactions, Inc. Dr. Betancourt explains that Quality Interactions has developed technology-based educational e-learning programs. He added that this set of learning programs that have been utilized in over 130,000 trainings across the country. In explanation, he described that the program provides targeted training through interactive exercises where residents learn the key principles that include mistrust and communication styles, language and interpreters, health literacy, health beliefs, and cross-cultural negotiation. The program provides situational examples of communication, religious beliefs, social and cultural background issues that patients and residents have that may create barriers to receiving high quality care. Dr. Beckencourt presented several of the slides within the on-line training. + Ann Griffith asked what level of resident does the training target? Dr. Betancourt answered by explaining the many differing varying courses that are offered for prelims up to 3rd year residents. Dr. Bray emphasized that this is a quality requirement of CLER that will be implemented. Dr. Kerry Sease asked if this requirement could be completed prior to attending Orientation? Ms. Coltman responded yes. GHS could monitor whether the training was done but hopes this training is more longitudinal and something continued as they progress as residents. Dr. Dane Smith asked about the cost or subscription to this CBT? Ms. Coltman stated there is costs by the participant but she willing to add partial expense to her budget. She also stated that there is some negotiating room with the charges of $11,000$12,000. Ms. Coltman continued to say that the training program is set up almost in an a la carte manner so we could say we only want to budget 2 hours of training because there are many levels of training to choose from. Dr. Smith added the program appeared to be well prepared and highly versatile. 3 CLER Moment: Quality Interactions Demo-Cont’d. Kinneil Coltman GME Expansion Reviews Edward Bray, MD Dr. Richard Hawkins stated that there was not a lot of information or supporting randomized measured studies to show the effectiveness of this program. Ms. Coltman stated that there is a book named “Unequal Treatment” which is a research study completed that looked thoroughly at this program. Dr. Dane Smith stated that there is not a study with true metrics available to meet the requirement. Ms. Coltman reiterated that this is her specialty field and in her opinion this is the best tool available. Dr. Scott Porter wants to ensure that this isn’t just the easiest thing to do to meet this requirement but something effective. Ms. Coltman stated that the cross cultural complaints that she receives are real and training of some sort is needed. Dr. Irfan Asif informed the group of another program used by Northwestern that could also be reviewed. Dr. Desmond Kelly asked that the vote to approve the usage of this CBT be tabled until next month to receive more information or other program options could be reviewed. Dr. Bray stated that a preliminary approval was needed by GMEC for all expansion programs. Programs then would be reviewed by Academic Council (AC) and Resource Council (RC) and sent back to GMEC for final approval. Dr. Bray introduced Dr. Robert Saul who has been appointed as the Program Director for Joint Pediatric Genetic Fellowship. Dr. Robert Saul stated that he has been with GHS for 2years and before that worked at the Genetic Center at Greenwood serving as Program Director from 1989 until 2013. He explained Joint Pediatric Genetic Fellowship is a 4-year program with 1 resident per year enrollment. Once completed the Resident would be eligible for joint certification in Pediatrics and Genomics. The genetic program at Greenwood is national and internationally recognized and this joint program will be 1 of only 16 programs in the country. He further explains that this will be a positive gain financially for the institution because it uses 1 categorical spot for Pediatrics that is already approved in their budget and Greenwood Genetic Center (verbal agreement only to date) would pay for half of that spot. Dr. Desmond Kelly asked what happens if the spot is not used. Dr. Kerry Sease explained that the categorical spot would be a flex spot so if no Genetic applicants applied then it would be filled in Pediatrics. GMEC scored the Residency as a 10 for Motivation and 0 for Barriers. GMEC voted by a show of hands to recommend this Residency. Dr. Bray introduced Dr. Amy Picklesimer who has been appointed as the Program Director for Maternal Fetal Fellowship. Dr. Amy Picklesimer stated that this will be a 3 year/ 1 fellow per year fellowship sub-specialty of the OB/Gyn Program. She adds that the Maternal-Fetal Medicine (MFM) Fellowship is not accredited by ACGME but by the American Board of Obstetrics and Gynecology (ABOG). MFM Fellowship will be 50% research and 50% clinical to create research scholars. The financial piece of it will be generated by the fellows by night calls which will cover about half the cost. There is a demand for staff to cover multiple requests to replace faculty time even at satellite locations. Voting to approve deferred until February GMEC Meeting Ms. Coltman will provide links to Ms. Griffith to the on-line training for the Program Directors to review further and search for additional evidence or research that has been done regarding outcomes. IA Mgmt AO C&E GMEC scored and voted to recommend Maternal Fetal Fellowship and Joint Pediatric Genetic Residency to Academic Council IA Mgmt AO PC 4 GME Expansion ReviewsCont’d. Edward Bray, MD Dr. Desmond Kelly questioned if ABOG would be ok with the night call work to generate funding? Dr. Picklesimer answered that this is the practice all over the country. Dr. Bray stated that this is a wash with no additional budget needs. Dr. Picklesimer stated that she was very liberal with budget forecasting including $20,000 expenditure for research. GMEC scored the Fellowship as a 10 for Motivation and 0 for Barriers. GMEC voted by a show of hands to recommend the Fellowship. GMEC also voted for final approval for the Emergency Medicine Residency as it has been approved by the AC and RC. Dr. Bray stated that Emergency Medicine had already been recommended by GMEC last year. Mr. Derek Payne stated that the Resource Council has now passed funding that was previously repudiated. Dr. Porter asked why the complement changed from 6 to 10 as previously discussed. Dr. Dane Smith stated that the optimal complement would be 14 so they are starting with 10 per year. Dr. Melissa Janse also added that if the residency started with a relatively small number that it would appear that the program may not be supported by the institution primarily. There is support for this number because we have the largest ER in the state. Dr. Pfennig added that if we start with a number too low it really goes against establishing ourselves as a teaching/ academic community especially if faculty only has a resident every now and then. GMEC voted to approve Emergency Medicine Residency. Dates to Remember Dr. Edward Bray Match Deadline: Jan. 31 11:59 pm Quota Change/Rank Order List Feb. 25 Dr. Bray stated that Program Directors must attend to any correspondence from the NRMP and ACGME as they are very important. ACGME Annual Meeting: Feb 26- March 1, 2015 Drs. Porter and Pfennig and Ms. Griffith will be attending the National ACGME Meeting. C/PD AO IA Mgmt AHME Institute National Meeting: May 13-15, 2015 February: Program Director Sharing: Roadmap to Milestone Tracking and Spider Diagram Reporting – Kerry Sease, MD Other Business Dr. Edward Bray Dr. Kyle Jeray reported that 1 resident due to bad decision-making had been reported to the State Board. Dr. Jeray states that the resident has apologized and they are waiting to hear from the State regarding decisions made of his misjudgement. Resident Status Reports R Stats IA Mgmt AO C/PD Dr. Kerry Sease stated that 1 resident has received written remediation after having verbal warnings for tardiness and professional issues. Dr. Sease added that explanation regarding another occurrence will result in probation. Dr. Alfredo Carbonell stated that he has a fellow that is also receiving 8 week remediation for technical improvement. 5 Other Business-Cont’d. Dr. Edward Bray Dr. Bray reminded Program Directors that documentation is imperative to cover legal recourse with remediation and probation. Dr. Irfan Asif requested a motion to vote for approval of Dr. Irfan Asif to take over as Interim Program Director replacing Dr. Robert Hanlin in the Family Medicine Residency. The vote was approved, no one opposed. Dr. Asif requested a motion to vote for approval for Dr. Vincent Green to take over as Interim Program Director replacing Dr. Kyle Casass in FM Sports Medicine Fellowship. Dr. Asif added that Dr. Green has been a Program Director for over 12 years at Laurens Hospital. The vote was approved, no one opposed. Adjourn Dr. Edward Bray There being no further business, the meeting adjourned at 9:50 AM. Next Meeting: 2/26/2015; 8:00 AM in CC3. GMEC voted and approved Dr. Asif as Interim Program Director for Family Medicine Residency and Dr. Green as Interim Program Director for FM Sports Medicine Fellowship. IA Mgmt AO C/PD PC AO IA Mgmt C/PD 6