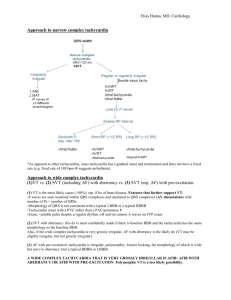
JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 ª 2022 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION PUBLISHED BY ELSEVIER ORIGINAL RESEARCH VENTRICULAR ARRHYTHMIAS - ELECTROCARDIOGRAPHY Simplified Integrated Clinical and Electrocardiographic Algorithm for Differentiation of Wide QRS Complex Tachycardia The Basel Algorithm Federico Moccetti, MD,a,b,c Mrinal Yadava, MD,b Yllka Latifi, MD,b,d Ivo Strebel, PHD,a Nikola Pavlovic, MD, PHD,a,e Sven Knecht, DSC,a Babken Asatryan, MD, PHD,f Beat Schaer, MD,a Michael Kühne, MD,a Charles A. Henrikson, MD,b Frank-Peter Stephan, MD,a Stefan Osswald, MD,a Christian Sticherling, MD,a Tobias Reichlin, MDa,f ABSTRACT BACKGROUND Prompt differential diagnosis of wide QRS complex tachycardia (WCT) is crucial to patient management. However, distinguishing ventricular tachycardia (VT) from supraventricular tachycardia (SVT) with wide QRS complexes remains problematic, especially for nonelectrophysiologists. OBJECTIVES This study aimed to develop a simple-to-use algorithm with integration of clinical and electrocardiographic (ECG) parameters for the differential diagnosis of WCT. METHODS The 12-lead ECGs of 206 monomorphic WCTs (153 VT, 53 SVT) with electrophysiology-confirmed diagnoses were analyzed. In the novel Basel algorithm, VT was diagnosed in the presence of at least 2 of the following criteria: 1) clinical high risk features; 2) lead II time to first peak >40 ms; and 3) lead aVR time to first peak >40 ms. The algorithm was externally validated in 203 consecutive WCT cases (151 VT, 52 SVT). Its’ diagnostic performance and clinical applicability were compared with those of the Brugada and Vereckei algorithms. RESULTS The Basel algorithm showed a sensitivity, specificity, and accuracy of 92%, 89%, and 91%, respectively, in the derivation cohort and 93%, 90%, and 93%, respectively, in the validation cohort. There were no significant differences in the performance characteristics between the 3 algorithms. The evaluation of the clinical applicability of the Basel algorithm showed similar diagnostic accuracy compared with the Brugada algorithm (80% vs 81%; P ¼ 1.00), but superiority compared with the Vereckei algorithm (72%; P ¼ 0.03). The Basel algorithm, however, enabled a faster diagnosis (median 36 seconds vs 105 seconds for the Brugada algorithm [P ¼ 0.002] and 50 seconds for the Vereckei algorithm [P ¼ 0.02]). CONCLUSIONS The novel Basel algorithm based on simple clinical and ECG criteria allows for a rapid and accurate differential diagnosis of WCT. (J Am Coll Cardiol EP 2022;8:831–839) © 2022 by the American College of Cardiology Foundation. From the aDivision of Cardiology, Department of Medicine, University Hospital Basel, University of Basel, Basel, Switzerland; b Knight Cardiovascular Institute, Oregon Health and Science University, Portland, Oregon, USA; cHeart Center Lucerne, Luzerner Kantonsspital, Lucerne, Switzerland; dCardiology Spital Uster, Uster, Switzerland; eCardiology, Klinicki Bolnicki Centar Sestre Milosrdnice, Zagreb, Croatia; and the fDepartment of Cardiology, Inselspital, Bern University Hospital, University of Bern, Bern, Switzerland. The authors attest they are in compliance with human studies committees and animal welfare regulations of the authors’ institutions and Food and Drug Administration guidelines, including patient consent where appropriate. For more information, visit the Author Center. Manuscript received October 18, 2021; revised manuscript received March 22, 2022, accepted March 28, 2022. ISSN 2405-500X/$36.00 https://doi.org/10.1016/j.jacep.2022.03.017 832 Moccetti et al JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT A ABBREVIATIONS AND ACRONYMS ECG = electrocardiography wide tachycardia patients undergoing EP studies for regular WCT at the (WCT) on the surface electrocardio- Knight Cardiovascular Institute of the Oregon Health gram (ECG) prompts a complex dif- and Science University, Portland, Oregon, were ferential EP = electrophysiology SVT = supraventricular tachycardia VT = ventricular tachycardia WCT = wide QRS complex QRS diagnosis complex of arrhythmias with The study was performed in accordance with the potentially lethal, requiring different treat- principles of the Declaration of Helsinki. The study ment strategies.1,2 While WCT is a manifesta- protocol tion of ventricular tachycardia (VT) in around committees. 80% of cases,2 other potential causes of WCT tachycardia retrospectively identified. prognoses ranging from utterly benign to include pre-excited supraventricular tachycardia (SVT), SVT with abnormal intraventricular conduction, ventricular-paced rhythm, and drug- and electrolyte-induced QRS widening.3,4 Rapid recognition of the underlying cause of the WCT is of critical importance for timely initiation of the appropriate treatment, 5 because delayed diagnosis or inappropriate management in patients with VT may have deleterious consequences. 6-8 Therefore, a simplified, was approved by the local ethics ECG ANALYSIS. The 12-lead ECGs were analyzed by 2 of the authors (F.M. and M.Y.) blinded to the EP diagnosis at a sweep speed of 25 mm/s. As in previous studies assessing the accuracy of ECG algorithms, the 12-lead ECGs of the tachycardias acquired during the EP studies were assessed.10,12 The criterion standard diagnosis of VT vs SVT was the one obtained during the EP study. All ECGs from the derivation and validation cohorts were assessed according to: 1) the novel simplified integrated ECG algorithm (“the Basel algorithmic, and practical approach to WCTs is crucial algorithm”); 2) the Brugada algorithm; 10 and 3) the for all clinicians responsible for ECG interpretation, Vereckei algorithm. 12 Interobserver agreement for the whether in emergency medicine, cardiology, or primary care.9 measurements in lead II and aVR were assessed in the validation cohort. SEE PAGE 840 DERIVATION OF THE BASEL ALGORITHM. The per- Over the past 3 decades, several criteria and algo- formance of several ECG candidate criteria was tested rithms have been proposed to distinguish VT from in the derivation cohort and the 2 with the highest SVT with abnormal intraventricular conduction.10-17 area under the receiver operating characteristic (ROC) Among them the Brugada algorithm and Vereckei curve for the diagnosis of VT (lead II time to first algorithm are the most commonly used. Despite peak, lead aVR time to first peak) were chosen. the Accordingly, the proposed Basel algorithm is based on high sensitivity (SN) and specificity (SP) reported in original cohorts, their use in the clinical 3 criteria (Figure 1, Central Illustration): 1) clinical high setting has consistently showed low reproducibility risk feature; 2) lead II time to first peak >40 ms; and 3) (Supplemental Table 1).18-23 Furthermore, these WCT lead aVR time to first peak >40 ms. VT was diagnosed algorithms are rather complex, involving multiple if at least 2 of those 3 criteria were met. If 0 or 1 cri- sequential steps and requiring evaluation of WCT terion was positive, the diagnosis was SVT. Examples morphology, and are difficult to recall in an emer- of ECGs with WCT demonstrating successful and un- gency setting. These factors render the everyday use successful diagnoses of VT and of SVT are shown in of WCT algorithms challenging, particularly for non- Figure 2. electrophysiologist (non-EP) practitioners. The clinical high risk feature criterion is considered To address these remaining challenges in the dif- to be met if the patient has a history of myocardial ferential diagnosis of WCT we aimed to develop a infarction, a history of congestive heart failure with user-friendly algorithm based on clinical and ECG left parameters to facilitate a rapid and accurate diagnosis implanted implantable cardioverter-defibrillator or ventricular ejection fraction #35% (or an in patients presenting with monomorphic regular cardiac resynchronization therapy–defibrillator). The WCT. lead II and lead aVR time to first peak criterion is considered to be positive if the time from the begin- METHODS PATIENT POPULATIONS AND STUDY DESIGN. For the derivation cohort, consecutive patients undergo- ning of the QRS to the first change in polarity, ie, the first positive or negative deflection (or “peak”), is >40 ms. This can be expressed as a QRS complex beginning with an r- or R-wave >40 ms, or beginning ing electrophysiological (EP) studies for regular WCT with a q-, Q-, or QS-wave >40 ms. at the University Hospital of Basel, Switzerland, from EVALUATION OF THE CLINICAL APPLICABILITY OF January 2010 to December 2014 were retrospectively THE NOVEL BASEL ALGORITHM. To evaluate the identified. For the validation cohort, consecutive “real-world” clinical applicability of the novel Moccetti et al JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT F I G U R E 1 Graphical Representation of the Novel Basel Algorithm CHF ¼ congestive heart failure; CRT ¼ cardiac resynchronization therapy; ICD ¼ implantable cardioverter-defibrillator; LVEF ¼ left ventricular ejection fraction; SVT¼ supraventricular tachycardia; VT¼ ventricular tachycardia. algorithm, a total of 8 physicians (2 EPs, 2 general DATA cardiologists, 2 cardiology fellows, and 2 internal article cannot be shared publicly owing to privacy of AVAILABILITY. The medicine residents) analyzed a random subset of 50 the individuals that were investigated in the study. WCT ECGs (25 VTs and 25 SVTs) at a sweep speed of The data will be shared on reasonable request to the 25 mm/s. Each of them analyzed the 50 ECGs indi- corresponding author provided that it in accordance vidually, blinded to the criterion standard diagnosis. with the institutional ethical guidelines as well as The ECG analysis was performed at 6 different time regulations and legislation. data underlying this points (with at least 2 weeks interval in between) according to 5 existing algorithms (Brugada, Vereckei, Pava, Jastrzebski, and Chen) 10,13-16 and the novel RESULTS Basel algorithm. The time to diagnosis was recorded BASELINE CHARACTERISTICS OF THE PATIENTS. In for every ECG assessed. the derivation cohort, a total of 206 WCT episodes STATISTICAL ANALYSIS. Continuous variables are presented as median (IQR) and compared with the use of the Mann-Whitney U test. Chi-square tests were used to compare categoric variables. To assess the algorithm performance, SN, SP, positive predictive value, negative predictive value, and diagnostic ac- (153 VT, 53 SVT) were recorded in 124 patients. In the validation cohort, 203 WCT episodes (151 VT, 52 SVT) were recorded in 112 patients. Baseline characteristics of the patients and the ECG characteristics of the 2 cohorts are presented in Tables 1 and 2. The underlying arrhythmias in the groups of SVTs and VTs are curacy were calculated from 2 2 cross-tables. presented in Table 3. McNemar’s test was used to compare the perfor- DERIVATION mance of the Basel algorithm with those of the Bru- analysis of several candidate criteria in the derivation gada and Vereckei algorithms. OF THE NOVEL ALGORITHM. After Interobserver cohort, time to first peak in lead II and lead aVR agreement for measurements performed in lead II showed the best performance characteristics (area and aVR were assessed with the use of correlation under the ROC curve: 0.91 for both). ROC derived coefficients and Bland-Altman plots in the validation optimal cutoffs were 51 ms for lead II time to peak and cohort. 46 ms for lead aVR time to peak (Supplemental For the clinical validation, SN, SP, positive pre- Table 2). For the algorithm, a cutoff of 40 ms was dictive value, negative predictive value, diagnostic chosen to facilitate user-friendly application in clin- accuracy, and average time to diagnosis using the 3 ical practice. algorithms were compared by means of Tukey’s multiple comparisons test. Observer agreement (Supplemental Figure 1) showed good correlation for lead II and aVR (r 2 ¼ 0.94 A P value <0.05 was considered to be statistically and r2 ¼0.92, respectively). Bland-Altman plots significant. The statistical analyses were performed showed a small bias (0.4 ms and 0.8 ms for lead II with the use of SPSS version 24.0 (IBM), Prism and aVR, respectively) and narrow 95% limits of Graphpad version 8.2.1 (Graphpad Software), and R (R agreement (14.8 and 14.0 ms for lead II, 17.0 and Foundation for Statistical Computing. 15.4 ms for lead aVR). 833 Moccetti et al 834 JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT C E NT R AL IL L U STR AT IO N Simplified Integrated Clinical and Electrocardiographic Algorithm for Differentiation of Wide QRS Complex Tachycardia Derivation, 206 ECGs Validation, 203 ECGs I II V1 V2 Novel Simplified Algorithm for the Differential Diagnosis of WCT Structural Heart Disease Lead II Time to First Peak >40 ms + + Lead aVR Time to First Peak >40 ms Structural Heart Disease: - Myocardial Infarction (history) - CHF (LVEF <35%) - Device (ICD, CRT) 120 ms 0 or 1 criteria fulfilled → SVT ≥2 criteria fulfilled → VT III V3 Comparison of Algorithm Performance 100% aVR V4 90% 80% aVL 70% V5 60% 50% Sensitivity aVF V6 Specificity Accuracy Basel-Algorithm Derivation / Validation Brugada-Algorithm Derivation / Validation Vereckei-Algorithm Derivation / Validation Clinical Validation Diagnostic Accuracy Time to Diagnosis P = 1.0 P = 0.002 P = 0.02 P = 0.003 P = 0.02 Seconds % P = 0.03 100 90 80 70 60 50 40 30 Brugada Vereckei Novel 160 140 120 100 80 60 40 20 0 Brugada Vereckei EP Attending Cardiology Attending Cardiology Fellow Internal Medicine Resident Novel Moccetti F, et al. J Am Coll Cardiol EP. 2022;8(7):831–839. CHF ¼ congestive heart failure; CRT ¼ cardiac resynchronization therapy; ECG ¼ electrocardiogram; EP ¼ electrophysiology; ICD ¼ implantable cardioverterdefibrillator; LVEF ¼ left ventricular ejection fraction; SVT ¼ supraventricular tachycardia; VT ¼ ventricular tachycardia; WCT ¼ wide QRS complex tachycardia. Moccetti et al JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT F I G U R E 2 Examples of Electrocardiograms With Wide QRS Complex Tachycardia Demonstrating Successful and Unsuccessful Diagnoses of VT and SVT (A) Ventricular tachycardia (VT) with a focus in the left ventricular outflow tract correctly classified as VT with the Basel algorithm (time to first peak >40 ms in leads II and aVR). (B) Fascicular VT incorrectly classified with the Basel algorithm (time to first peak <40 ms in leads II and aVR). (C) Typical atrial flutter with 1:1 atrioventricular conduction and right bundle branch block aberrancy correctly classified as supraventricular tachycardia (SVT) with the Basel algorithm (time to first peak <40 ms in leads II and aVR). (D) SVT incorrectly classified as VT with the Basel algorithm (time to first peak >40 ms in leads II and aVR). PERFORMANCE OF THE NOVEL ALGORITHM IN THE performance of each criterion, are presented in DERIVATION AND THE VALIDATION COHORT. The Table 4. The novel algorithm reached SN and SP of, diagnostic performance of the Brugada algorithm, the respectively, 91.5% and 88.7% in the derivation Vereckei algorithm and the novel Basel algorithm in cohort and 93.3% and 90.4% in the validation cohort. the derivation and the validation cohort, including This was similar to the Brugada and Vereckei T A B L E 1 Patient Characteristics Derivation Cohort All (N ¼ 124) VT (n ¼ 74) SVT (n ¼ 50) 65 (50-74) 64 (50-72) Male 82 (69) Structural heart disease Age, y LVEF, % Validation Cohort P Value All (N ¼ 112) VT (n ¼ 64) SVT (n ¼ 48) P Value 68 (51-77) 0.46 61 (42-69) 61 (42-70) 58 (34-69) 0.23 51 (69) 31 (69) 0.45 64 (57) 49 (77) 30 (63) 0.14 65 (55) 51 (69) 14 (31) <0.05 56 (50) 49 (52) 7 (15) <0.05 50 (34-60) 40 (27-55) 56 (50-60) <0.001 45 (30-60) 30 (25-55) 60 (51-63) <0.001 <0.001 Antiarrhythmic drugs Any 97 (78) 60 (81) 37 (74) 0.38 72 (64) 53 (83) 18 (38) Class I 4 (3.2) 1 (1.4) 3 (6) 0.30 19 (17) 16 (25) 3 (6) 0.01 Class II 89 (72) 54 (73) 35 (70) 0.84 69 (62) 50 (78) 13 (27) <0.001 Class III 37 (30) 27 (37) 10 (20) 0.07 31 (28) 29 (45) 2 (4.2) <0.001 Class IV 4 (3.2) 1 (1.4) 3 (6) 0.30 0 0 0 1.00 Values are median (IQR) or n (%). LVEF ¼ left ventricular ejection fraction; SVT ¼ supraventricular tachycardia; VT¼ ventricular tachycardia. 835 836 Moccetti et al JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT T A B L E 2 ECG Characteristics of Wide QRS Complex Tachycardias in the Derivation and Validation Groups Derivation Cohort Validation Cohort All (N ¼ 206) VT (n ¼ 153) SVT (n ¼ 53) P Value All (N ¼ 203) VT (n ¼ 151) SVT (n ¼ 52) Cycle length, ms 380 (312-440) 376 (312-440) P Value 400 (314-440) 0.30 405 (322-469) 402 (312-464) 413 (331-492) Heart rate, beats/min 158 (136-192) 0.38 160 (136-192) 150 (137-191) 0.30 149 (127-186) 160 (129-191) 155 (122-185) QRS duration, ms 0.38 160 (140-188) 172 (152-196) 140 (135-144) <0.001 165 (149-196) 182 (157-202) 155 (138-154) <0.001 RBBB 116 (58) 88 (58) 28 (58) <0.06 114 (56) 84 (56) 30 (59) 0.87 LBBB 84 (42) 64 (42) 20 (42) <0.07 89 (44) 67 (44) 22 (41) 0.11 Values are median (IQR) or n (%). LBBB ¼ left bundle branch block; RBBB ¼ right bundle branch block; other abbreviations as in Table 1. algorithms, in the derivation, validation, and overall [IQR: 58%-73%]; P ¼ 0.03), and no differences were cohorts (Supplemental Table 3). The diagnostic per- found between the Basel algorithm and the other al- formance of each step/criterion of the Brugada, Ver- gorithms (Figure 3, Central Illustration). eckei, and novel Basel algorithm in both the Average time to diagnosis was significantly shorter derivation and the validation cohorts are presented in using the Basel algorithm (median 38 [IQR: 2947] Supplemental Table 4. seconds) compared with the Brugada algorithm (me- EVALUATION OF THE CLINICAL APPLICABILITY OF THE NOVEL ALGORITHM. The SN and SP of the cli- nicians’ interpretation are shown in Figure 3. SP was higher with the use of the Basel algorithm vs the Vereckei algorithm (median 80% [IQR: 72%-86%] vs dian 106 [IQR: 76-135] seconds; P ¼ 0.002) and Vereckei algorithms (median 48 [IQR: 43-59] seconds; P ¼ 0.02). No differences were found between the Basel algorithm and the other algorithms (Figure 3, Central Illustration). median 58% [IQR: 46%-72%]; P ¼ 0.007), but no other ALGORITHM PERFORMANCE IN SPECIAL SITUATIONS. We differences were observed between the Basel algo- tested the performance of the Basel algorithm in 3 rithm and the other algorithms. clinically challenging albeit rare scenarios: fascicular The Basel algorithm showed a higher diagnostic ventricular tachycardia (n ¼ 3), antidromic atrioven- accuracy (median 81% [IQR: 76.5%-83.5%]) compared tricular re-entrant tachycardia (n ¼ 1), and Mahaim- with the Vereckei algorithm (median 72% [IQR: 65%- fiber tachycardia (n ¼ 3). Similar to the Brugada and 76%]; P ¼ 0.002) and the Chen algorithm (median 72% Vereckei algorithms, the performance of the novel Basel algorithm was poor in these tachycardias (Supplemental Table 5). T A B L E 3 Underlying Causes of SVT and VT Derivation Cohort Validation Cohort (n ¼ 53) (n ¼ 52) Atrial flutter 22 (42) 21 (40) AVNRT 17 (34) 18 (35) AVRT 4 (8) 3 (6) Atrial tachycardia 8 (15) 8 (15) validated a novel, simple, reproducible, sensitive, Mahaim 2 (4) 1 (2) and specific algorithm based on clinical and ECG pa- Antidromic AVRT 0 (0) 1 (2) rameters to discriminate VT from SVT in patients with (n ¼ 153) (n ¼ 151) regular monomorphic WCT. Compared with the cur- Ischemic 93 (63) 65 (43) rent standard of care,10,13 the proposed Basel algo- DCM 32 (21) 49 (32) Other 28 (18) 37 (25) ARVC 5 (3) 4 (3) RVOT 9 (6) 3 (2) offering a simplified approach based on clear-cut 2 (1) 1 (0.7) easy-to-use criteria and by avoiding measurements 1 (0.7) 1 (0.7) of complex and morphology-based parameters that SVT VT Fascicular HCM DISCUSSION By analyzing data from 2 large cohorts of patients with EP-confirmed diagnosis, we developed and rithm provides similarly high diagnostic accuracy and performance characteristics while at the same time are difficult to assess in the emergency setting (eg, V i / Values are n (%). ARVC ¼ arrhythmogenic right ventricular cardiomyopathy; AVNRT ¼ atrioventricular non-reentrant tachycardia; AVRT ¼ atrioventricular re-entrant tachycardia; DCM ¼ dilated cardiomyopathy; HCM ¼ hypertrophic cardiomyopathy; RVOT ¼ right ventricular outflow tract; other abbreviations as in Table 1. V t).23 Since a common shortcoming for the Brugada and Vereckei algorithms is their lower accuracy in the “real-world” setting compared with the performance described in original publications (Supplemental Moccetti et al JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT Table 1), 10-12,18,19,23 we sought to further validate the Basel algorithm in a clinical setting. When applied by T A B L E 4 Diagnostic Performance Characteristics of the Brugada, 10 Vereckei, 12 and Basel Algorithms clinicians with different training/background, in a head-to-head comparison against the Brugada, Vereckei, and 3 other previously published algorithms,14-16 the novel Basel algorithm showed a Sensitivity Specificity PPV NPV Diagnostic Accuracy Derivation cohort (n ¼ 206) Brugada 92.8 90.6 96.6 81.4 92.2 diagnostic performance similar to that of the Brugada Vereckei 96.7 86.8 95.5 90.2 94.2 algorithm and higher than that of the Vereckei algo- Basel 90.8 91.5 88.7 95.9 78.3 rithm, while requiring significantly shorter time for Criterion I (clinical) 73.9 69.8 87.6 48.1 72.8 diagnosis. This difference in time was most pro- Criterion II (lead II) 86.9 94.3 97.8 71.4 88.8 Criterion III (lead aVR) 79.1 92.5 96.8 60.5 82.5 nounced when applied by cardiology fellows and internal medicine residents. Such performance Validation cohort (n ¼ 203) Brugada 93.3 88.5 95.9 82.1 92.1 characteristics indicate that the low complexity and Vereckei 91.3 84.6 94.5 77.2 89.6 high accuracy of the Basel algorithm make it highly Basel 92.6 93.3 90.4 96.6 82.5 applicable in clinical practice and particularly useful Criterion I (clinical) 84.7 80.8 92.7 64.4 83.7 for physicians in training to ensure timely diagnosis Criterion II (lead II) 89.3 84.6 94.4 73.3 88.1 of WCT. Similar to the lead aVR (Vereckei) algorithm13 and Criterion III (lead aVR) 86.0 96.1 98.5 70.0 88.6 the R-wave peak time (RWPT) algorithm,14 the Basel Values are %. NPV ¼ negative predictive value; PPV ¼ positive predictive value. algorithm is based on the analysis of the electrical vector in the frontal plane only. However, the aforementioned algorithms operate based on only 1 lead (leads aVR or II), with the diagnosis of WCT primarily CLINICAL IMPLICATIONS. The Basel WCT algorithm determined by R-wave parameters. Alongside clinical can be used for a quick and accurate differential parameters highly sensitive for VT, the Basel algo- diagnosis of WCT by EP and non-EP practitioners. Of rithm offers an integrated yet simplified and accurate note, the focus on leads aVR and II in the Basel al- version of 2 ECG criteria from the 2 aforementioned gorithm make it potentially suitable for the use in algorithms: RWPT >40 ms in lead aVR, which is the emergency settings and for incorporation in Holter second step of the Vereckei algorithm, 13 and a posi- tive or negative RWPT $50 ms in lead II, the criterion 14 and telemetry analysis software that include information on only limb leads. The theory behind STUDY LIMITATIONS. The findings of this study both criteria is that SVT with bundle branch block should be viewed in the light of a few potential limi- results in rapid initial activation of the ventricular tations. 1) The derivation and validation cohorts myocardium owing to impulse conductance through comprised patients from tertiary EP centers, so referral the His-Purkinje system (steeper QRS in both aVR and bias cannot be excluded. 2) All patients included in this II leads), with a delayed muscle-to-muscle spread of study had EP-confirmed diagnoses. While this meth- activation, resulting in widening of the terminal QRS. odology allows having a criterion standard for diag- In contrast, during VT, initial ventricular activation is nosing the mechanism of WCT, a selection bias might through muscle-to-muscle spread of the impulse, be present because not all patients with WCT undergo which is slower than terminal activation mediated an EP study. 3) Both cohorts contained a relatively low through the His-Purkinje system after the impulse number of cases with preexcitation-related tachy- reaches the conduction system. This results in cardia. Although pre-excited SVTs are a rare cause of steeper terminal QRS. WCT,13 the Basel algorithm needs to be further studied behind the RWPT algorithm. It should be recognized that identifying the initia- in those cases. 4) For some of the patients, more than 1 tion, peak, and termination of the QRS complex might VT ECG was included. These were, however, ECGs from at times be challenging for any given single lead, different VTs with different ECG morphologies. 5) particularly for aVR13; thus, integration of 2 limb leads Neither our approach nor the available algorithms are in the Basel algorithm will likely help in determining perfect. Given the rapid implementation of techno- the time to first peak in either of the leads, when logic advances in clinical care, development of an measurements in single leads are difficult. Further automated application that uses a complex WCT dif- prospective studies comparing the Basel algorithm ferential algorithm, with incorporation of the Basel with other proposed criteria are needed to determine and or other WCT algorithm, might enable a more ac- the validity of our criteria in distinguishing between curate and quicker differential diagnosis of WCT in the VT and SVT with wide QRS complexes. near future. 837 838 Moccetti et al JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT F I G U R E 3 Clinical Validation of the Basel Algorithm Comparison of sensitivity, specificity, diagnostic accuracy, and average time for electrocardiographic analysis of the Basel algorithm with the Vereckei,13 Brugada,10 Jastrzebski,15 Pava,14 and Chen16 algorithms based on a subset of the derivation cohort and stratified by the observers’ specialties. EP ¼ electrophysiology; IM ¼ internal medicine. CONCLUSIONS reached in a shorter time, particularly when applied by physicians in training. We constructed an easy-to-use and accurate algo- FUNDING SUPPORT AND AUTHOR DISCLOSURES rithm to distinguish VT from SVT with aberrant conduction with the use of a 6-lead limb ECG. The Basel Dr Schaer has received personal fees from Medtronic. Dr Kühne has algorithm consists of 3 criteria and had a performance received grants from the Swiss National Science Foundation, the Swiss similar to that of the established Brugada and Ver- Heart Foundation, Daiichi-Sankyo, Bayer, Pfizer BMS, and Boston Scientific; and has received personal fees from Bayer, Boehringer eckei algorithms in both derivation and validation Ingelheim, Pfizer BMS, Daiichi-Sankyo, Medtronic, Biotronik, Boston cohorts. When applied by physicians with different Scientific, and Johnson & Johnson, all outside the submitted work. Dr training levels and backgrounds, the novel algorithm showed a high accuracy similar to the Brugada and Vereckei algorithms while allowing a diagnosis to be Henrikson has received fellowship support from Abbott, Boston Scientific, and Medtronic; and has served as chair of the clinical endpoints committee for Biotronik. Dr Sticherling has received grants from Biosense-Webster; and has received lecture fees from Abbott, Moccetti et al JACC: CLINICAL ELECTROPHYSIOLOGY VOL. 8, NO. 7, 2022 JULY 2022:831–839 Basel Algorithm for Diagnosis of SVT/VT Medtronic, Biosense-Webster, Boston Scientific, Microport, and Biotronik. Dr Reichlin has received speaker/consulting honoraria or travel PERSPECTIVES support from Abbott/SJM, AstraZeneca, Brahms, Bayer, BiosenseWebster, Biotronik, Boston-Scientific, Daiichi-Sankyo, Medtronic, Pfizer BMS, and Roche, all for work outside the submitted study; and has received support for his institution’s fellowship program from COMPETENCY IN MEDICAL KNOWLEDGE: The novel algorithm can be used for rapid and accurate differential diag- Abbott/SJM, Biosense-Webster, Biotronik, Boston-Scientific, and nosis of wide QRS complex tachycardias by physicians with Medtronic for work outside the submitted study. All other authors have different backgrounds and training levels. reported that they have no relationships relevant to the contents of this paper to disclose. ADDRESS FOR CORRESPONDENCE: Prof Tobias Reichlin, Department of Cardiology, Inselspital, Bern University Hospital, University of Bern, Freiburgstrasse 10, CH-3010 Bern, Switzerland. E-mail: tobias. TRANSLATIONAL OUTLOOK :The development of automated applications using combinations of complex algorithms might further improve the differential diagnosis of wide QRS complex tachycardias. reichlin@insel.ch. REFERENCES 1. Akhtar M, Shenasa M, Jazayeri M, Caceres J, Tchou PJ. Wide QRS complex tachycardia. Reappraisal of a common clinical problem. Ann Intern Med. 1988;109:905–912. 10. Brugada P, Brugada J, Mont L, Smeets J, Andries EW. A new approach to the differential diagnosis of a regular tachycardia with a wide QRS complex. Circulation. 1991;83:1649–1659. medicine residents to distinguish between ventricular tachycardia and supraventricular tachycardia with aberrancy. J Cardiol. 2012;59:307– 312. 2. Steinman RT, Herrera C, Schuger CD, Lehmann MH. Wide QRS tachycardia in the conscious adult. Ventricular tachycardia is the 11. Lau EW, Pathamanathan RK, Ng GA, Cooper J, Skehan JD, Griffith MJ. The Bayesian approach improves the electrocardiographic diagnosis of 20. Isenhour JL, Craig S, Gibbs M, Littmann L, Rose G, Risch R. Wide-complex tachycardia: continued evaluation of diagnostic criteria. Acad most frequent cause. JAMA. 1989;261:1013–1016. broad complex tachycardia. Pacing Clin Electrophysiol. 2000;23:1519–1526. Emerg Med. 2000;7:769–773. 12. Vereckei A, Duray G, Szenasi G, Altemose GT, Miller JM. Application of a new algorithm in the differential diagnosis of wide QRS complex tachycardia. Eur Heart J. 2007;28:589–600. Comparison of the “real-life” diagnostic value of two recently published electrocardiogram methods for the differential diagnosis of wide QRS complex tachycardias. Acad Emerg Med. 2013;20:1121–1130. 3. Page RL, Joglar JA, Caldwell MA, et al. 2015 ACC/AHA/HRS guideline for the management of adult patients with supraventricular tachycardia: a report of the American College of Cardiology/ American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol. 2016;67(16):1575– 1623. 4. Al-Khatib SM, Stevenson WG, Ackerman MJ, et al. 2017 AHA/ACC/HRS guideline for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol. 2018;72(14):e91–e220. 5. Alzand BS, Crijns HJ. Diagnostic criteria of broad QRS complex tachycardia: decades of evolution. Europace. 2011;13:465–472. 6. Stewart RB, Bardy GH, Greene HL. Wide complex tachycardia: misdiagnosis and outcome after emergent therapy. Ann Intern Med. 1986;104: 766–771. 7. Pelleg A, Pennock RS, Kutalek SP. Proarrhythmic effects of adenosine: one decade of clinical data. Am J Ther. 2002;9:141–147. 8. Buxton AE, Marchlinski FE, Doherty JU, Flores B, Josephson ME. Hazards of intravenous verapamil for sustained ventricular tachycardia. Am J Cardiol. 1987;59:1107–1110. 9. Garner JB, Miller JM. Wide complex tachycardia—ventricular tachycardia or not ventricular tachycardia, that remains the question. Arrhythm Electrophysiol Rev. 2013;2:23–29. 13. Vereckei A, Duray G, Szenasi G, Altemose GT, Miller JM. New algorithm using only lead aVR for differential diagnosis of wide QRS complex tachycardia. Heart Rhythm. 2008;5:89–98. 14. Pava LF, Perafan P, Badiel M, et al. R-Wave peak time at DII: a new criterion for differentiating between wide complex QRS tachycardias. Heart Rhythm. 2010;7:922–926. 15. Jastrzebski M, Sasaki K, Kukla P, Fijorek K, Stec S, Czarnecka D. The ventricular tachycardia score: a novel approach to electrocardiographic diagnosis of ventricular tachycardia. Europace. 2016;18:578–584. 16. Chen Q, Xu J, Gianni C, et al. Simple electrocardiographic criteria for rapid identification of wide QRS complex tachycardia: the new limb lead algorithm. Heart Rhythm. 2020;17:431–438. 21. Szelényi ZDG, Katona G, Fritúz G, et al. 22. Herbert MEVS, Morgan MT, Cameron P, Dziukas L. Failure to agree on the electrocardiographic diagnosis of ventricular tachycardia. Ann Emerg Med. 1996;27:35–38. 23. Kaiser E, Darrieux FC, Barbosa SA, et al. Differential diagnosis of wide QRS tachycardias: comparison of two electrocardiographic algorithms. Europace. 2015;17:1422–1427. KEY WORDS ECG, cardiac arrhythmia, wide QRS complex tachycardia, ventricular tachycardia, supraventricular tachycardia, sudden cardiac death, algorithm 17. Pachon M, Arias MA, Salvador-Montanes O, et al. A scoring algorithm for the accurate differential diagnosis of regular wide QRS complex tachycardia. Pacing Clin Electrophysiol. 2019;42: 625–633. 18. Jastrzebski M, Kukla P, Czarnecka D, Kawecka-Jaszcz K. Comparison of five electrocardiographic methods for differentiation of wide QRS-complex tachycardias. Europace. 2012;14: 1165–1171. 19. Baxi RP, Hart KW, Vereckei A, et al. Vereckei criteria as a diagnostic tool amongst emergency A PP END IX For supplemental tables and a figure, please see the online version of this paper. Go to http://www.jacc.org/cme-moc to take the CME/MOC/ECME quiz for this article. 839