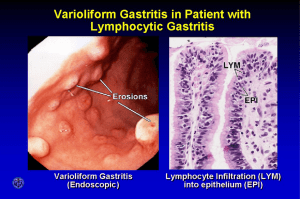
Gastritis and Peptic Ulcer Disease (PUD)
Acute and Chronic Gastritis
Etiology and Pathophysiology
o Gastritis is inflammation of the gastric lining, or mucosa, of the stomach
Can be chronic or acute, w/ some symptoms being localized to area and
some being diffuse
Gastritis occurs because of a breakdown in the gastric mucosal
barrier, which normally protects the stomach from the corrosion of
hydrochloric acid and pepsin.
Tissue edema occurs w/ disruption of capillary walls and plasma can leak
into gastric lumen
Hemorrhage may occur w/ corrosion of gastric lining
Causes of gastritis: variety of factors including certain drugs, foods,
microorganisms, and pathophysiologic conditions
o Factors broken down:
Drugs:
Corticosteroids: inhibit prostaglandins (gastric mucosal
protectant), increasing risk of gastritis
NSAIDS: can erode stomach lining
Dietary factors:
Alcohol
Spicy, irritating foods
Caffeine
Microorganisms:
H. Pylori
Salmonella organisms
Staphylococcus organisms
Pathophysiological conditions:
Burns
Large hiatal hernia
Physiologic stress
Reflux of bile and pancreatic secretions
Renal failure (uremia)
Sepsis
Shock
Other:
Smoking cigarettes
Endoscopic procedures
NG Tube
Psychologic stress
Radiation exposure
Peptic Ulcer Disease Pathophysiology
Is erosion of the stomach’s lining (gastric mucosa, submucosa, and/or muscularis)
resulting from digestive action of HCl and pepsin
o When mucosa becomes damaged histamine is released, further secretion of
HCl and pepsin
Can be acute or chronic ulcers:
o Acute: associated with superficial erosion and minimal inflammation
Resolves quickly when cause is identified and removed
o Chronic: ulcer of long duration, eroding through the muscular wall w/ the
formation of fibrous tissue
Continuously present for many months or intermittently throughout a
person’s lifetime
More common than acute ulcers
(PEPTIC)
Gastritis and Peptic Ulcer Disease: Clinical Manifestations
Treatment of Gastritis
Peptic Ulcer Disease: medical care
Conservative treatment of PUD consists of adequate rest, drug therapy, lifestyle changes
(smoking cessation and dietary management), and long-term follow-up care. The aim of
treatment is to decrease gastric acidity and enhance mucosal defense mechanisms.
Acute exacerbations w/o complications treatment:
o NPO (to include regular mouth care)
o NG suction with intermittent not constant suction
o Adequate rest promotes ulcer healing
o IV fluid replacement
o Drug therapy
o PPIs
o H2-receptor blockers
o Antibiotics for H. pylori infection
o Cytoprotective drugs
o Antacids
o Anticholinergics (used rarely)
Acute exacerbations w/ complications treatment:
o Hemorrhage: frequent vital signs, lab values (possible blood transfusions),
maintain NG patency,
o Perforation: notify healthcare provider immediately, frequent vital signs (q 15
min), NPO, maintain IV rate or increase, antibiotic therapy, ready the patient for
possible OR
o Gastric Outlet Obstruction: NG suction with regular irrigation to maintain
patency, IV fluids
o Stomach lavage (possible)
Education for PUD and Gastritis
SUMMARY:
 0
0