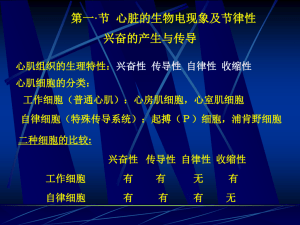
Conducting system of heart
advertisement

Elongated, branching cells containing 1-2 centrally located nuclei Contains actin and myosin myofilaments Intercalated disks: specialized cell-cell contacts. Cardiac Muscle Cell membranes interdigitate Desmosomes hold cells together Gap junctions allow action potentials to move from one cell to the next. Electrically, cardiac muscle of the atria and of the ventricles behaves as single unit • Mitochondria comprise 30% of volume of the cell vs. 2% in skeletal The Action Potential in Skeletal and Cardiac Muscle Figure 20.15 Cardiac Muscle Contraction Heart muscle: Is stimulated by nerves and is self-excitable (automaticity) Contracts as a unit; no motor units Has a long (250 ms) absolute refractory period Cardiac muscle contraction is similar to skeletal muscle contraction, i.e., sliding-filaments Conductive System of Heart Conduction System of the Heart SA node: sinoatrial node. The pacemaker. Specialized cardiac muscle cells. Generate spontaneous action potentials (autorhythmic tissue). Action potentials pass to atrial muscle cells and to the AV node AV node: atrioventricular node. Action potentials conducted more slowly here than in any other part of system. Ensures ventricles receive signal to contract after atria have contracted AV bundle: passes through hole in cardiac skeleton to reach interventricular septum Right and left bundle branches: extend beneath endocardium to apices of right and left ventricles Purkinje fibers: Large diameter cardiac muscle cells with few myofibrils. Many gap junctions. Conduct action potential to ventricular muscle cells (myocardium) Autorhythmic cells: Initiate action potentials Have unstable resting potentials called pacemaker potentials Use calcium influx (rather than sodium) for rising phase of the action potential Sequence of Excitation Sinoatrial (SA) node generates impulses about 75 times/minute Atrioventricular (AV) node delays the impulse approximately 0.1 second Impulse passes from atria to ventricles via the atrioventricular bundle (bundle of His) to the Purkinje fibers and finally to the myocardial fibers Impulse Conduction through the Heart Pacemaker and Action Potentials of the Heart Pacemaker potentials Rhythmically discharging cells have a membrane potential that, after each impulse, declines to the firing level. Thus, this Prepotential pacemaker potential triggers the next impulse At the peak of each impulse, IK begins and brings about repolarization. IK then declines, and a channel that can pass both Na+ and K+ is activated. Because this channel is activated following hyperpolarization, it is referred to as an “h” channel; however, because of its unusual (funny) activation this has also been dubbed an “f” channel As I h increases,the membrane begins to depolarize, forming the first part of the prepotential. Ca2+ channels then open These are of two types in the heart, the T(for transient)channels and the L(for longlasting)channels. The action potentials in the SA and AV nodes are largely due to Ca2+ , with no contribution by Na+ influx. Consequently, there is no sharp, rapid depolarizing spike before the plateau,as there is in other parts of the conduction system and the atrial and ventricular fibers In addition, prepotentials are normally prominent only in the SA and AV nodes. However, “latent pacemakers” are present in other portions of the conduction system that can take over when the SA and AV nodes are depressed or conduction from them is blocked. Atrial and ventricular muscle fibers do not have prepotentials, and they discharge spontaneously only when injured or abnormal Depolarization of SA Node SA node - no stable resting membrane potential Pacemaker potential gradual depolarization from -60 mV, slow influx of Na+ Action potential occurs at threshold of -40 mV depolarizing phase to 0 mV fast Ca2+ channels open, (Ca2+ in) repolarizing phase K+ channels open, (K+ out) at -60 mV K+ channels close, pacemaker potential starts over Each depolarization creates one heartbeat SA node at rest fires at 0.8 sec, about 75 bpm SA nodal fibers continuous with atrial fibers Three Inter-nodal Pathways Anterior: Bachmen Middle: Wenckebach Posterior: Thorel Contain fibers similar to purkinji fibers With rapid conduction Av nodal delay Depolarization initiated in the SA node spreads radially through the atria, then converges on the AV node. Atrial depolarization is complete in about 0.1 s. Because conduction in the AV node is slow (Table 30– 1), a delay of about 0.1 s(AV nodal delay)occurs before excitation spreads to the ventricles The slow conduction in transitional nodal and penetrating A-V bundle fibers which is caused by lesser number of gap junctions between the cells in conducting pathways result in great resistance to conduction of excitatory ions from one fiber to next. Rapid transmission in ventricular purkenji system at a velocity of 1.5 – 4 m/s. Rapid transmission in purkenji system is caused by high level of permeability of gap junction between the cells. One way conduction through A-V bundle. The A-V bundle passes downward in ventricular septum from 5 -15 mm dividing into left and right bundle branches. Left bundle branch gives of anterior fascicle and posterior fascicle Purkenji fibers penetrate the ventricular muscle Velocity of transmission in ventricular m uscle 0.3- 0.5 m/s. Ectopic Pace Makers SA node functions as pace maker of heart because its rate of discharge is 70-80 times per minute AV node discharges at 40 – 60 per minute Purkenji system discharge at 15 – 40 per minute. ectopic pace makers if any part of the heart devalops rhythmical discharge that is more rapid than SA node AV node or purkenji fibers some times become ectopic pace maker Atrial and ventricular muscle devalops excessive excitability to and become the pace maker The blockage of transmission from the SA node to other parts of heart may result in ectopic focci. Stokes Adams syndrome An Electrocardiogram




![Cardio Review 4 Quince [CAPT],Joan,Juliet](http://s2.studylib.net/store/data/005719604_1-e21fbd83f7c61c5668353826e4debbb3-300x300.png)