All - Austin Community College
advertisement

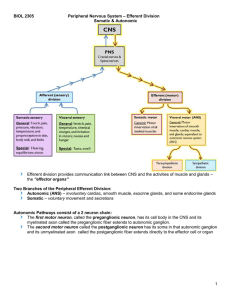
BIO2305 PNS – Efferent Division Somatic & Autonomic Efferent Pathways • Heavily myelinated axons of the somatic motor neurons extend from the CNS to the effector (lacks ganglia) • Pathways in the ANS are a two-neuron chain –The preganglionic (first) neuron has a lightly myelinated axon. The ganglionic (second) unmyelinated neuron extends to an effector organ via the postganglionic axon Autonomic Pathways consist of a 2 neuron chain: • The first motor neuron, called the preganglionic neuron, has its cell body in the CNS and its myelinated axon called the preganglionic fiber extends to autonomic ganglion. • The second motor neuron called the postganglionic neuron has its soma in that autonomic ganglion and its unmyelinated axon called the postganglionic fiber extends directly to the effector cell or organ 1 Efferent division provides communication link between CNS and the activities of muscle and glands – the effector organs Two branches of the peripheral efferent division Autonomic – involuntary cardiac, smooth muscle, exocrine and some endocrine glands Aomatic – voluntary movement and secretions Comparison of Somatic and Autonomic Systems Efferent Reflex Pathways 2 Autonomic branch Autonomic Nervous System • The ANS operates without conscious control; it is primarily regulated by the hypothalamus and the medulla oblongata with input from the limbic system and other regions of the cerebrum. • The afferent component of the ANS consists of general visceral sensory neurons. Interoreceptors such as chemoreceptors (CO2 levels) and mechanoreceptors (degree of stretch of organs and vessels) • Afferent signals are not consciously recognized unless intense enough to cause pain or nausea from damaged viscera, fullness of bladder, angina pectoris (inadequate blood flow to heart) • The efferent component consists of the autonomic motor neurons that excite or inhibit visceral activities of effector tissues; cardiac muscle, smooth muscle, glands • Efferent responses include automatic activities beyond conscious control dilation/constriction of pupils, accommodation of lens, dilation of blood vessels, heartbeat, GI tract movement, glandular secretions. Synapses in Autonomic Nerves • Varicosities • NT released to ECF • No cleft • Impact • Large area • Slow acting • Long duration 3 Efferent Pathways: Motor & Autonomic Autonomic Nervous System: Sympathetic & Parasympathetic • Regulation of the “internal” environment generally outside of our conscious control: “autonomous” • Innervates organs that are not usually under voluntary control - glands, smooth/cardiac muscle • Efferent (motor) systems “visceromotor” - effectors are part of visceral organs and blood vessels • Involve 2 neurons that synapse in a peripheral ganglion • Presynaptic neuron is myelinated and postsynaptic neuron is unmyelinated • Autonomic nerves release NT that may be stimulatory or inhibitory ANS • Autonomic nerve pathway • Extends from CNS to an innervated organ • Two-neuron chain • Preganglionic fiber (synapses with cell body of second neuron) • Postganglionic fiber (innervates effector organ) 4 Divisions of the ANS: Sympathetic & Parasympathetic • Both have preganglionic neurons that originate in CNS. • Both have postganglionic neurons that originate outside of the CNS in ganglia. Anatomical Differences between the Sympathetic and Parasympathetic Divisions PNS • Fibers originate from cranial and sacral areas of CNS • Preganglionic fibers are longer • Very short postganglionic fibers • Preganglionic fibers release acetylcholine (Ach) • Postganglionic fibers release acetylcholine SNS • • • • • Fibers originate in thoracic and lumbar regions of spinal cord Most preganglionic fibers are short Long postganglionic fibers Preganglionic fibers release acetylcholine (Ach) Most postganglionic fibers release noradrenaline (norepinephrine) 5 Neurochemistry of the ANS • All preganglionic fibers release acetylcholine (=cholinergic) • Postganglionic PARASYMPATHETIC fibers release acetylcholine(=cholinergic) • Postganglionic SYMPATHETIC fibers release norepinephrine(=adrenergic) • Exceptions: • Adrenal medullary chromaffin cells secrete epinephrine • Sympathetic nerves innervating sweat glands secrete acetylcholine • Sympathetic nerves innervating blood vessels in skeletal muscle secrete acetylcholine • Sympathetic nerves innervating renal blood vessels secrete dopamine Functional Differences • Sympathetic - “fight or flight” • Catabolic (expend energy) • Excites body in emergency or threatening situations • Release of norepinephrine (NT) from postganglionic fibers and epinephrine (NT) from adrenal medulla. • Mass activation prepares for intense activity. • Heart rate (HR) increases. • Bronchioles dilate. • Blood [glucose] increases. • Parasympathetic - “feed & breed”, “rest & digest” • Maintain homeostasis • Concerned with keeping body energy use as low as possible, and SLUDD (salivation, lacrimation, urination digestion, defecation) • Normally not activated as a whole, stimulation of separate parasympathetic nerves. • Release ACh as NT. • Relaxing effects: • Decreases HR. • Dilates visceral blood vessels. • Increases digestive activity. • Dual innervation of many organs — having a brake and an accelerator provides more control Autonomic Pathways 6 Synaptic Organization Adrenal Glands • Adrenal medulla secretes epinephrine (Epi) and norepinephrine (NE) when stimulated by the sympathetic nervous system. • Modified sympathetic ganglion, derived from same embryonic tissue that forms postganglionic sympathetic neurons. • Sympathoadrenal system: • mass activation of the sympathetic nervous system. • Innervated by preganglionic sympathetic fibers. • Stimulation of preganglionic fiber prompts secretion of hormones into blood • About 20% of hormone release is norepinephrine • About 80% of hormone released is epinephrine (adrenaline) 7 Adrenergic and Cholinergic NTs • ACh is NT for all preganglionic fibers of both sympathetic and parasympathetic nervous systems. • Transmission at these synapses is termed cholinergic: • ACh is NT released by most postganglionic parasympathetic fibers at synapse with effector. • Axons of postganglionic neurons have numerous varicosities along the axon that contain NT. • • • • NT released by most postganglionic sympathetic nerve fibers is NE. Epi, released by the adrenal medulla is synthesized from the same precursor as NE. Transmission at these synapses is called adrenergic Collectively called catecholamines. 8 Responses to Cholinergic Stimulation • All somatic motor neurons, all preganglionic and most postganglionic parasympathetic neurons are cholinergic. • Release ACh as NT. • Somatic motor neurons and all preganglionic autonomic neurons are excitatory. • Postganglionic axons, may be excitatory or inhibitory. • Muscarinic receptors: • Found on smooth, cardiac muscle and glands • ACh binds to receptor. • Requires the mediation of G-proteins. • Nicotinic receptors (ligand-gated): • Found on the postganglionic cell bodies in all autonomic ganglia • ACh binds to 2 nicotinic receptor binding sites. • Opens a Na+/K+ channel. • Always excitatory. Responses to Adrenergic Stimulation • Has both excitatory and inhibitory effects • All act through G-proteins • Alpha adrenergic responses due to Ca2+ • A1 : excitatory constricts smooth muscles • A2 : inhibitory decreases contraction of smooth muscle • Beta adrenergic responses due to cAMP • B1 : excitatory increases HR and force of contraction • B2 : inhibitory relaxes bronchial smooth muscles 9 Responses to Adrenergic Stimulation Organs with Dual Innervation • Most visceral organs receive dual innervation (innervation by both sympathetic and parasympathetic fibers). • Antagonistic effects: • Sympathetic and parasympathetic fibers innervate the same cells. • Actions counteract each other, ex. Heart rate • Complementary - sympathetic and parasympathetic stimulation produces similar effects ex. salivary gland secretion • Cooperative - Sympathetic and parasympathetic stimulation produce different effects that work together to produce desired effect ex. • Parasympathetic fibers penile erection • Sympathetic fibers ejaculation 10 Dual Antagonistic Innervation Organs without Dual Innervation • Regulation achieved by increasing or decreasing firing rate • Adrenal medulla, arrector pili muscle, sweat glands, and most blood vessels receive only sympathetic innervation Sympathetic vs Parasympathetic 11 Levels of ANS Control • The hypothalamus is the main integration center of ANS activity • Subconscious cerebral input via limbic lobe connections influences hypothalamic function • Other controls come from the cerebral cortex, the reticular formation, and the spinal cord Levels of Autonomic Control 12 Regulation of the ANS by CNS • Prefontal association cortex and limbic system -Responsible for visceral responses that are characteristic of emotional states and behavior • Hypothalamus – sympathetic response to anger or fear is brought on by hypothalamus through medulla • Medulla: • Most directly controls activity of autonomic system • Location of centers for control of cardiovascular pulmonary, urinary, reproductive and digestive systems. • Some autonomic reflexes integrated at spinal cord (urination, erection) Somatic Motor Controls Skeletal Muscles • Body movement • Appendages • Locomotion • Single neuron • CNS origin • Myelinated • Terminus • Branches • Neuromuscular junction Somatic Efferent • Consists of the axons of motor neurons which originate in the spinal cord and terminate on skeletal muscle • Acetylcholine released from a motor neuron stimulates muscle contraction • Motor neurons are the final common pathway by which various regions of the CNS exert control over skeletal muscle activity • The areas of the CNS that influence skeletal muscle activity by acting through the motor neurons are the spinal cord, motor regions of the cortex, basal nuclei, cerebellum, and brain stem Nerve Stimulus • Skeletal muscles are stimulated by motor neurons of the somatic nervous system • Axons of these neurons travel in nerves to muscle cells • Axons of motor neurons branch repeatedly as they enter muscles • Each axonal ending forms a neuromuscular junction with a muscle fiber 13 Neuromuscular Junction Neuromuscular Junction • When a nerve impulse reaches the neuromuscular junction: • Voltage-regulated calcium channels in the axon membrane open and allow Ca2+ to enter the axon • Ca2+ inside the axon terminal causes some of the synaptic vesicles to fuse with the axon membrane and release ACh into the synaptic cleft (exocytosis) • ACh diffuses across the synaptic cleft and attaches to ACh receptors on the sarcolemma • Binding of ACh to receptors on the sarcolemma initiates an action potential in the muscle • ACh is quickly destroyed by acetylcholinesterase 14 Motor Unit: Neuromuscular Functional Unit • A motor neuron and all the muscle fibers it supplies is called a Motor Unit • A single motor unit may contain from 2 to 2000 muscle fibers • Each muscle has at least one motor nerve that may contain hundreds of motor neuron axons. • Axons branch into terminals, each forming a neuromuscular junction with a single muscle fiber 15 Motor Unit • The number of muscle fibers per motor unit can vary from a few to several hundred • Muscles that control fine movements (fingers, eyes) have small motor units • Large weight-bearing muscles (thighs, hips) have large motor units • Muscle fibers in a single motor unit are spread throughout the muscle. As a result, stimulation of a single motor unit causes weak contraction of the entire muscle End Plate Potential • A local depolarization that creates and spreads an action potential across the sarcolemma, stronger than an EPSP due to more NT, greater surface area of membrane, greater number of receptors Summary • Autonomic branches: sympathetic and parasympathetic • Regulate glands, smooth & cardiac muscles • Team with endocrine to regulate homeostasis • Are regulated by hypothalamus, pons & medulla • Have pathways with 2 neurons and a ganglion • Use varicosities to release NTs • Have diverse receptors: tonic & antagonistic regulation • Efferent motor neurons control skeletal muscles • Single long myelinated neuron from CNS • Neuromuscular junction structure & mechanism 16