PATH3205 lab report – asthma
advertisement

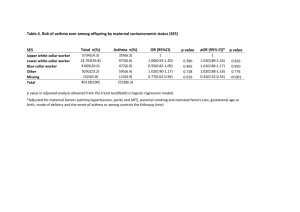
PATH3205 Topic C: Asthma Research Laboratory z3460307 Introduction Asthma can be described as a chronic airway inflammatory disorder, with episodes of acute inflammation, often referred to as ‘exacerbations’ (Global Initiative for Asthma, 2015). An exact method of diagnosing asthma, and its underlying aetiology however, remains elusive. Of immediate concern are these asthma exacerbations, which in terms of costs is the most significant contributor to direct health-care expenditure (Dougherty & Fahy, 2009). Asthma incidence and exacerbation has been generally agreed to be higher in metropolitan areas (Gem, 2010), however other recent studies have failed to find significantly higher asthma risk and incidence in metropolitan areas (Keet et al. 2015). Thus we need to determine exactly what it is, in the environment that exacerbates asthma. A few studies (Tecer, Alagha, Karaca, Tuncel & Eldes, 2008; Lin, Chen, Burnett, Villeneuve & Krewski, 2002) have explored the effects of particulate matter of various sizes, including those <10µm aerodynamic diameter (PM10) as is used in this experiment, and found a positive correlation between concentration of ambient particulate matter and incidence of asthma exacerbations, measured by number of hospitalisations. This experiment parallels that outlined in the method of “Ambient particulate matter induces an exacerbation of airway inflammation in experimental asthma: role of interleukin-33” by Shadie, Herbert & Kumar, 2014. We hypothesised and found that ambient particulate matter exacerbates airway inflammation in asthma. More specifically, that ambient (PM10) particulate matter induces acute exacerbation of airway inflammation in the BALB/c asthma mouse model. Furthermore, we suspected and found evidence to support that Interleukin-33 (IL-33) is a key player in PM10 induced asthma exacerbation development, as was suggested in previous studies (Oboki, Nakae, Matsumoto & Saito, 2011), in the decreased level of inflammation of antiIL-33 antibody treated, chronically challenged mice in comparison to the non-treated mice. The aim of this experiment is to determine whether Sydney’s ambient (PM10) particulate pollutants can drive acute inflammation of airways in asthma, as measured 1 PATH3205 Topic C: Asthma Research Laboratory z3460307 by the level of TNF-alpha expressed and histologically assessed inflammation. That is, the number of eosinophils, a hallmark of asthmatic airway inflammation (Oboki et al., 2011). The administration of anti-IL-33 antibodies was also performed here, to determine the effect on level of inflammation induced, as asthma exacerbation. Materials and Methods The BALB/c mouse model for asthma was used, which was a previously described, effective model of asthma (Temelkovski, Hogan, Shepherd, Foster & Kumar, 1998). The weanling mice were systemically sensitized to ovalbumin, as was done in Herbert et al., 2012. The features of chronic asthma were induced by challenging the mice with aerosolized OVA over 4 weeks. Four experimental groups (eight mice each), were utilized: naïve mice, chronically challenged, chronically challenged + Sydney PM10, and chronically challenged + Sydney PM10 +IL-33 neutralising antibody. The Sydney PM10 particulate matter was intranasally administered. Inflammation was assessed histologically and in terms of TNF-alpha levels in bronchoalveolar lavage (BAL) fluid, measured using ELISA. Results Histologically, it was found that the presence of eosinophils were not elevated in chronically challenged only mice. In those who were chronically challenged, and treated with Sydney PM10, number of eosinophils were significantly elevated, consistent with asthma exacerbation. In the group of mice, chronically challenged, treated with Sydney PM10 and also treated with anti-IL-33 antibodies, eosinophil infiltration was not as high as in those without anti-IL-33 antibodies. Quantitatively, we found that TNF-alpha levels in the chronic challenged mice were slightly elevated (~122pg/ml) compared to the naïve mice (~108pg/ml). The chronic challenged mice treated with Sydney PM10 exhibited much higher levels (~468pg/ml), and those also treated with anti-IL-33 antibodies exhibited slightly lower levels at (~275pg/ml) (see Figure 1). 2 PATH3205 Topic C: Asthma Research Laboratory z3460307 Concentration of TNF-alpha (pg/ml) TNF-alpha in bronchoalveolar lavage fluid from mice Naïve mice 600 500 Chronic challenged mice 400 300 Chronic challenged plus SydPM10 mice 200 Chronic challenged plus SydPM10 + anti-IL-33 antibody mice 100 0 Mice Groups Figure 1 – Concentration of TNF-alpha in bronchoalveolar lavage fluid for experimental groups, as measured using ELISA. From the data used to construct Figure 1, the difference between the naïve and chronic challenged plus Sydney PM10 mice is not significant (p>0.05). The difference between the naïve and chronic challenged plus Sydney PM10 mice ± anti-IL-33 antibody are both significant (P<0.0001). Similarly, the difference between the chronic challenged mice and the chronic challenged plus Sydney PM10 mice ± anti-IL-33 antibody are both significant (P<0.0001). Finally the difference between the chronic challenged plus Sydney PM10 mice and the chronic challenged plus Sydney PM10 + anti-IL-33 antibody is also significant (P<0.0001). (Significance calculated using unpaired t-test) Thus results of this experiment demonstrate a significant difference in inflammation levels between the naïve/chronic challenged mice and the chronic challenged plus Sydney PM10 mice ± anti-IL-33 antibody mice, as well as between the chronic challenged plus Sydney PM10 mice, and the chronic challenged mice plus Sydney PM10 + anti-IL-33 antibody mice. 3 PATH3205 Topic C: Asthma Research Laboratory z3460307 Discussion In this report, we determined that Sydney’s ambient (PM10) particulate matter can drive acute inflammation of airways in asthma, as measured by the level of TNF-alpha expressed and histologically assessed inflammation. The difference in TNF-alpha levels in BAL, between the chronically challenged mice and the chronically challenged mice treated with Sydney PM10 were found to be statistically significant, as consistent with the asthma exacerbation. To better quantify the effect of the treatments investigated in this experiment, more control groups would be desirable. In particular, groups of naïve mice given intranasal Sydney PM10 (50 µg/ml) ± anti-IL-33 antibody treated, naïve anti-IL-33 treated and chronically challenged, anti-IL-33 treated mice. These would allow factoring in of the treatment’s baseline effects, thus pinpointing with a greater degree of certainty the source of TNF-alpha level differences. The administration of anti-IL-33 antibodies performed here, had a suppressive effect on the level of inflammation induced (decreased concentration of TNF-alpha), as can be seen in Figure 1. This suggests that IL-33 indeed plays a key role in inducing acute asthma exacerbation as its deficiency resulted in decreased levels of TNF-alpha expression. As such, the supposition that IL-33 neutralisation may be a useful treatment option for asthma exacerbation, is supported by this experiment. Other recent studies such as those by Oboki, et al., 2011, Lee et al., 2014, and Gallelli, Busceti, Vatrella, Maselli & Pelaia, 2013, likewise has delineated that IL-33 levels are elevated in asthma exacerbation, and indicating its potential for a future asthma exacerbation treatment target. Further study needs to be done to verify the potential of anti-IL-33 antibodies as treatment. The exploration of drug interactions, systemic effects in humans, and effectiveness in the real world needs to be investigated. In conclusion, in the controlled setting of a mouse asthma model, we have shown ambient particulate matter can induce inflammation of the airway, similar to asthma exacerbation, with IL-33 playing a key role as a mediator of inflammation. 4 PATH3205 Topic C: Asthma Research Laboratory z3460307 Reference: Dougherty, R., & Fahy, J. (2009). Acute exacerbations of asthma: epidemiology, biology and the exacerbation-prone phenotype. Clinical & Experimental Allergy, 39(2), 193-202. doi:10.1111/j.1365-2222.2008.03157.x Gallelli, L., Busceti, M., Vatrella, A., Maselli, R., & Pelaia, G. (2013). Update on Anticytokine Treatment for Asthma. Biomedical Research International, 2013, 110. doi:10.1155/2013/104315 Global Initiative for Asthma. (2015). Pocket Guide for Asthma Management and Prevention (for adults and children older than 5 years) (p. 5). Global Initiative for Asthma. Retrieved from http://www.ginasthma.org/local/uploads/files/GINA_Pocket_2015.pdf Keet, C., McCormack, M., Pollack, C., Peng, R., McGowan, E., & Matsui, E. (2015). Neighborhood poverty, urban residence, race/ethnicity, and asthma: Rethinking the inner-city asthma epidemic. Journal Of Allergy And Clinical Immunology, 135(3), 655-662. doi:10.1016/j.jaci.2014.11.022 Lee, H., Rhee, C., Kang, J., Byun, J., Choi, J., & Kim, S. et al. (2014). Blockade of IL-33/ST2 ameliorates airway inflammation in a murine model of allergic asthma. Experimental Lung Research, 40(2), 66-76. doi:10.3109/01902148.2013.870261 Lin, M., Chen, Y., Burnett, R., Villeneuve, P., & Krewski, D. (2002). The Influence of Ambient Coarse Particulate Matter on Asthma Hospitalization in Children: Case-Crossover and Time-Series Analyses. Environmental Health Perspectives, 110(6), 575-581. doi:10.1289/ehp.02110575 Oboki, K., Nakae, S., Matsumoto, K., & Saito, H. (2011). IL-33 and Airway Inflammation. Allergy, Asthma and Immunology Research, 3(2), 81. doi:10.4168/aair.2011.3.2.81 Shadie, A., Herbert, C., & Kumar, R. (2014). Ambient particulate matter induces an exacerbation of airway inflammation in experimental asthma: role of 5 PATH3205 Topic C: Asthma Research Laboratory z3460307 interleukin-33. Clinical and Experimental Immunology, 177(2), 491-499. doi:10.1111/cei.12348 Tecer, L., Alagha, O., Karaca, F., Tuncel, G., & Eldes, N. (2008). Particulate Matter (PM 2.5 , PM 10-2.5 , and PM 10) and Children's Hospital Admissions for Asthma and Respiratory Diseases: A Bidirectional Case-Crossover Study. Journal Of Toxicology And Environmental Health, Part A, 71(8), 512-520. doi:10.1080/15287390801907459 Temelkovski, J., Hogan, S., Shepherd, D., Foster, P., & Kumar, R. (1998). An improved murine model of asthma: selective airway inflammation, epithelial lesions and increased methacholine responsiveness following chronic exposure to aerosolised allergen. Thorax, 53(10), 849-856. doi:10.1136/thx.53.10.849 6 PATH3205 Topic C: Asthma Research Laboratory z3460307 Reflection Aside from the obvious learning of new knowledge, overall, I was glad we were given the opportunity to both learn from and speak to a variety of researchers from different areas of medical science. Given that I intend on doing honours next year, I feel that this course has provided me with valuable insight into the common laboratory techniques employed, a number of different research areas and potential supervisors, as well as encouraging the development of independent and critical thinking skills. Regarding the asthma topic, I felt that the research laboratory was particularly valuable. Prior to doing it, I was not specifically interested in asthma despite its prevalence in our society. Afterwards, having seen and better understood the difficulties faced in research of this disease, asthma seems a more captivating disease, full of variables and potential. I especially appreciated the way this lab was conducted, with a more group-oriented, conversational brainstorm approach to the question: “Can exposure to particulate pollutants drive exacerbations of asthma?” with some guidance from the tutors. It was interesting the way different groups of students all thought of different methods of investigating the same research question. I felt the lab in this way, more effectively nurtured our critical thinking skills and encouraged us to think on our own. All in all, I did not particularly feel that this course developed my teamwork skills as much as it facilitated its maintenance. However, with the group presentation, I know it necessitated my further developing my presentation skills with the seemingly mammoth task of a 10minute presentation. Prior to this, speeches extended to an average of a mere 5 minutes. I felt the more scientific style and question/answer format, also shaped us to be better prepared for the style of honours and beyond. 7