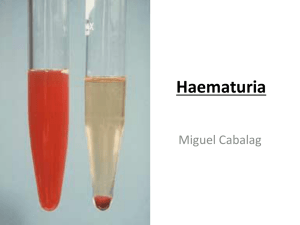
Post-mortem Toxicology
advertisement

Post-mortem Toxicology DR A J JEFFERY MBChB MD FRCPath (Forensic) MFFLM HOME OFFICE REGISTERED FORENSIC PATHOLOGIST Areas to Cover Why take toxicology What samples How to take them What does the toxicologist do with the samples? How to interpret the results – general considerations Alcohol Drugs of abuse Toxicology in other causes of death Other specimens Case examples WHY TAKE TOXICOLOGY ? Why take toxicology ? To ascertain if the deceased was under the influence of alcohol or drugs of abuse at the time of their death. RTAs / Accidental deaths / suicides To confirm or refute overdose / poisoning To confirm presence / levels of therapeutic drugs. Eg epilepsy / antidepressants WHAT SAMPLES ARE APPROPRIATE ? Samples Blood Blood Urine Urine (plain) (preserved) (plain) (preserved) (peripheral) (peripheral) Fluoride – inhibits further alcohol production but won’t undo the damage already done. Vitreous Stomach Contents Tissues Liver Skeletal muscle (mid R lobe) (eg psoas) (if embalmed buttock) OBTAINING THE BLOOD SAMPLE Femoral Vein Sampling Vein NOT artery Before evisceration Before urine sampling Ideal = tie off / clamp, then sample by wide-bore needle below Routine = clean catch Ideal = don’t milk the leg Routine = required to gain sufficient sample Problem: MINIMAL FEMORAL BLOOD Insufficient Femoral Blood Take what ever you can in preserved tubes Subclavian = reasonable alternative Could take free-lying chest blood etc for screening for the general presence of drugs Make sure you say where each sample has come from Obtain an alternative specimen OBTAINING THE URINE SAMPLE Urine Sampling Needle and syringe or Open dome of bladder and aspirate with syringe alone Presence of a catheter may be important toxicologically as the urine may contain artefactually high lignocaine due to catheter lubricant gel Vitreous WHAT DO THE TOXICOLOGISTS DO WITH THE SAMPLE ? Analysis Screening (GC / Immunoassay) What classes of drug are present Confirmation (GCMS) Specific drugs found by breaking them down & looking at the breakdown products. Quantification Technique may vary dependent on the nature of the drug being analysed. HOW TO INTERPRET THE RESULTS General Considerations Accuracy of reference ranges Re-distribution – site matters! Individual variation (e.g. renal disease) Decomposition Tolerance Accuracy of reference ranges Interpretation of absolute drug levels / Reference ranges Based on individual reports Variable from lab to lab due to varying techniques Need to consider the previous list General Considerations Re-distribution – site matters! Individual variation (renal disease) Decomposition Tolerance Redistribution Discovered with digoxin Most drugs that undergo redistribution do so because of their relative lipid solubility. Due to Loss of cell integrity Diffusion GI tract – to adjacent structures Through conduits – lymph Diffusion from bladder Natural Disease Depends or route of administration 1st pass / second pass metabolism Absorption With or without meal GI surgery Elimination / Clearance Renal impairment Liver impairment Decomposition Significant redistribution Some drug levels increase Alcohol production by bacterial action Others degrade If there is a degree of decomposition make sure you write it on the tox request Tolerance Increasing doses required over time to achieve same effects. What is lethal to a naïve user may have no effect at all in a chronic user. First dose deaths People walking around and working with enough drugs on board to kill an elephant! Prison release deaths Alcohol Deaths due to Alcohol What alcohol related causes of death do you know? How might you classify them? Which specific toxicological causes do you know? Alcohol Acute alcohol toxicity Ketoacidosis Alcohol in combination with other drugs Problems with Interpretation of Alcohol Redistribution Dealing with decomposition Back calculations Acute alcohol toxicity How does it cause death? >30 = higher skills Death – respiratory 30 – 50 = deterioration in depression due to action on brainstem UK legal driving limit? Driving limit 80 mg/100ml Less than 20 mg/100ml generally considered insignificant. driving 50 – 100 = inhibitions / laughter 100 – 150 = slurring, insteadiness, poss nausea 150 – 200 = obvious drunkenness, nausea staggering 200 – 300 = stupor, vomiting, coma 300 + = stupor, coma, aspiration & Alcohol – fatal level or not? LD 50 = 400 mg/100ml Alcohol has symbiotic relationship with other drugs. e.g. < 200mg/100ml can be fatal if opioids are taken. > 200mg/100ml can ½ the fatal dose of opioids > 100mg/100ml may enhance heroin toxicity Ethyl glucuronide (minor breakdown product) in urine if imbibed within 5 days of death. What is ketoacidosis? Can you explain why this happens? Ketoacidosis Brain can utilise ketone bodies when glucose is unavailable – fasting / starvation Ketone bodies, formed by the breakdown of fatty acids and the de-amination of amino acids. Ketoacidosis is an extreme and uncontrolled form of ketosis, which is a normal response to prolonged fasting. In ketoacidosis, the body fails to adequately regulate ketone production causing such a severe accumulation of keto acids that the pH of the blood is substantially decreased. Alcoholic ketoacidosis Metabolic acidosis Malnutrition Binge drinking superimposed on chronic alcohol abuse Ketoacidosis Ketones: Acetone (can be produced pm) <0.5 mg/100ml Beta hydroxybutyrate (less likely to be raised artefactually) <0.5 mmol/L 1.26 – 47.2 mmol/L (assoc with fatalities) Causes Alcoholic ketoacidosis Diabetic ketoacidosis Alcoholic vs Diabetic How might you differentiate? Urine glucose HbA1c 4 - 6.1% Calculations AVOID ! Clearance 10 – 25 mg/dl/hr ( about a unit an hour) In 10 hours you can clear ~ 100-200 mg/dl Alcoholics can clear 30 – 40 mg/dl/hr (due to training!) Widmark equation Used by some to predict amount of alcohol consumed Decomposition 70 – 190 mg/100ml reported as artefact Consider pm findings Look for other substances produced pm Use vitreous and urine as supportive evidence These are relatively protected from redistribution Normal ratios (if in equilibrium) Urine : Blood 1.23 : 1 Vitreous : Blood 1 : 0.81 Drugs of Abuse OPIOID AGONISTS SYMPATHOMIMETICS Opioid agonists Opioid agonists Analgesia / euphoria / dysphoria Respiratory depression miosis Morphine and other opioids Morphine Heroin (diamorphine) – IV, smoked, sniffed Methadone (green liquid – oral or IV) Pethidine, buprenorphine ** CNS depression ** Findings History / scene / paraphernalia External iv sites Foam at nose / mouth Limited & non specific Pulmonary congestion and oedema Stomach contents – methadone is usu green! Morphine / Heroin Heroin / diamorphine – synthetic morphine derivative Powerful opioid analgesic Metabolised almost immediately (10 – 15 mins) to 6 monoacetyl morphine 6MAM and then within 24 hours to morphine. Presence of 6MAM is consistent with use within 12-24 hours Ie recent intake / top up injections Acute alcohol intoxication potentiates the effects Total morphine : Free Morphine Gives some idea of time since administration Eg in IV admin 15 mins post admin 60 mins 4 9 Therapeutic Free morphine 10 – 100ng/ml : : 1 1 Lethal_______ 50 – 4000 ng/ml Heroin A contaminate of street heroin is acetylcodeine Hence may have +ve codeine levels Most heroin deaths occur several hours after taking the drug Sleepy / snoring May have time to metabolise drug despite irreversible respiratory depression Methadone Therapeutic 75 – 1100 ng/ml Toxic 200 – 2000 ng/ml Lethal 400 – 2000 ng/ml Significant overlap Tolerance becomes very important Interpretation requires knowledge of drug history Long & variable T ½ Methadone Breakdown product – EDDP This is inactive Titration is important Many deaths occur during first few weeks of treatment Can cause respiratory depression at therapeutic doses Lipophilic so undergoes significant redistribution Even peripheral samples can be 2x in and 3x in Opioids Tolerance = V V important consideration Eg. Prison release Palliative care Nb worth remembering that 10% of codeine will breakdown to become morphine. Free Codeine Therapeutic Lethal_______ 30 – 340ng/ml >1600 ng/ml Sympathomimetics Sympathomimetics Incr activity of adrenaline and serotonin Adrenalin Hypertension Tachycardia Mydriasis Serotonin Excitement Hyperthermia Stimulants Cocaine Amphetamine Ecstasy Other methamphetamines Associated with subarchnoid haemorrhage 80% of these assoc with aneurysms Intracerebral haemorrhage Associated with AVMs & hypertension Findings Hearts of stimulant users tend to be heavier than controls Fibrosis Contraction band necrosis Accelerated atherosclerosis Non specific pulmonary changes Crack cocaine smokers – prominent anthracosis esp in alveolar macrophages & emphysematous changes. Cocaine Naturally occurring plant alkaloid stimulant Snorted, smoked, cutaneous, injected Nb always consider in sudden death in the same way that you might consider HOCM. Breakdown Products Benzoylecgonine Inactive Methylecgonine Cocaethylene As active as cocaine itself & indicative of alcohol consumption at the same time Cocaine Toxicity Less than 50 ng/ml cocaine is considered not to produce measurable physiological effects T ½ can be as little as 40 mins Benzoylecgonine – 1-4 days in urine Toxic >900 ng/ml Lethal >1000 ng/ml Benzoylecgonine Lethal - >1000 ng/ml * Cocaine But lethal nature not dose related Long term effects: Cardiovascular damage – incr ischaemic event / Coronary Art thrombosis coronary artery spasm contraction band necrosis fibrosis / sudden arrhytmia myocarditis/cardiomyop/valvular/aortic dissection/hypertensive crisis Non cardiac - Cerebral infarction / intracerebral haemorrhage So death can be attributed to cocaine even if not found in blood. Cocaine can decrease rapidly in unpreserved blood samples stored at room temperature. Cocaine, death & Excited delirium Excited delirium Hyperthermia Mental & physiological arousal Excited, erratic & sometimes bizarre, violent behaviour May have florid psychosis May exhibit extra-ordinary strength Tends to result in sudden respiratory arrest Blood cocaine and benzoylecgonine may be low but there is usually concentration of benzoylecgonine within the brain indicating long term use Marked decease in D2 receptors in hypothalamus in psychotic cocaine abusers. D2 receptors play a role in temperature regulation Amphetamine Prevalence second only to cannabis Synthetic stimulant Effects similar to cocaine Stimulate release of catecholamines, particularly adrenaline Tolerance & dependence develop Absorbed by GIT, clinical effects commence within 20 minutes, last 4-6 hours. Amphetamine Toxic >500 ng/ml amphetamine >1800 ng/ml methamphetamine Lethal Usu > 1000 ng/ml amphetamine But can be seen if >50ong/ml Usu > 10 000 ng/ml methamphetamine Different Forms Amphetamine (Benzedrine, uppers, 'A', speed, whizz, cranks, wake-up, sulph, hearts) Dextroamphetamine (Dexedrine, dex, dexy, dexies) Methamphetamine (ICE, crystal, glass, meth) Methylenedioxyamphetamine (MDA, EVE) 3 ,4, Methylenedioxymethamphetamine (MDMA, ADAM, Ecstasy, 'E', doves, Dennis) Amphetamine Alcohol can potentiate effects on the heart. Rare toxic effects: Coma Cerebral vasculitis Cerebral haemorrhage Rhabdomyolysis D.I.C. Renal dysfunction Cardiac – long term users Accelerated coronary atherosclerosis Microvascular disease MDMA / Ecstasy Amphetamine-like drugs 3,4-methylenedioxymethamphetamine Serotinergic and noradrenergic effects • Hyperthermic effects Liquid ecstasy – GHB Gamma hydroxybutyrate Other Benzodiazepines Diazepam – 20 – 4000 ng/ml Nordiazepam – 20 – 1800 ng/ml Need in the order of thousands to consider fatal. Cannabis Cannabinoids THC – tetrahydrocannabinol Delta 9 THC carboxylic acid Rapidly distributed into tissues Blood levels drop >90% within 2 hours of intake THC can only be found within 4-12 hours post intake >2 ng/ml suggestive of recent intake THC metabolites remain in Blood – up to ~ 5 days Urine – up to ~ 12-36 days Volatile substance abuse - VSA Adhesives, aerosols, petrols, paint stripper, nail varnish remover ….. amongst others Increased risk taking behaviour Accidental suffocation CNS depression Deaths thought to be due to cardiac arrhythmias Sensitisation of myocardium to effects of adrenaline Deaths often seen in association with physical exertion Blood sample must be in a glass tube with a foil top filled to the top. Tie off whole lung and place within a nylon bag. Head space ‘New’ Drugs Mephadrone ‘Cream’ Toxicology IN OTHER CAUSES OF DEATH Fire deaths Carboxyhaemoglobin Normal <10% Toxic 15 – 35% Lethal >48% Cyanide Normal < 0.1mg/L Develops within the potted blood sample if not preserved Carbon Monoxide In an individual breathing air T ½ = 4 hours Breathing O2 in Hospital T ½ = 60 minutes Therefore always consider survival time. Therapeutic Drugs Anti-depressants Anti-convulsants Overdose Aspirin Therapeutic Hyper ventilation Resp Alkalosis Enhanced BBB transfer Met Acidosis Body Compensates Toxic 20 – 100mg/l Stimulation of Resp Centres >150 mg/l Lethal >500 mg/l NB those on reg Rx (eg arthritis – 3g/day) – 44- 330mg/L T ½ up to 36 hours in massive OD Findings Pm Blood stained gastric content / frank haematemesis Rarely skin petechiae Mucosal gastric erosions Malaena if survival sufficiently long Petechiae through other organs due to anticoagulant effect esp parietal pleura and epicardium Paracetamol Therapeutic Toxic 10 – 20 mg/l >150 mg/l Lethal >160 mg/l Other samples of interest IMMUNOLOGY – ANAPHYLAXIS BIOCHEMISTRY – DIABETES Immunology - Anaphylaxis Secure ante-mortem samples Needs to be peripheral as mast cell rich organs can release tryptase after death. Serum (plain tube – spun down) Mast cell tryptase ( = more specific) Specific IgE Make sure you give details of any suspected cause Available for venoms, foods, medicines, contrast agents, latex……. Mast cell tryptase T ½ during life is ~ 2 hours so may be unhelpful if they have been resuscitated and have survived and die later ( usu from cerebral anoxia) Antemortem!!! Tryptase is a sensitive marker for mast cell activation High levels will be found post severe anaphylaxis Levels are not raised in local allergic reaction eg rhinitis Can be raised in pure asthma deaths but not of the same order of magnitude Slight increases can be seen in non-anaphylactic mast cell degranulation – EG opioids for chest pain Trauma – disruption of mast cell rich tissues Unless grossly elevated – interpret with caution In presence of suggestive history and absence of pm findings it may provide confirmatory evidence. Normal Levels: IgE MCT MCT can be produced pm 0 – 122 kU/L 2-14 mg/L Biochemistry - Diabetes Vitreous is best for biochem as most blood is already haemolysed Glucose drops significantly after death Bacterial metabolism Drops even in vitreous So low glucose ≠ hypoglycaemia It is not possible to diagnose hypoglycaemia accurately at pm. A high vitreous glucose virtually rules out hypoglycaemia as one can assume it was the same or higher in the antemortem period unless peri-mortem dextrose admin HbA1c – heparinised sample Insulin If endogenous the body has to cleave C peptide from pro-insulin to make active insulin. If exogenous the insulin is already cleaved and so they will have no C peptide. Case Examples Case 1 60 yr old male, in house fire, extensive burns, no suspicious injuries, no soot in airways or stomach. Ranges Norm Tox Leth CO = 40% <10% 15-35% >50% Cyanide = 0.5 mg/L <0.1mg/L Paracetamol 6mg/l 10-20mg/l >150mg/l >160mg/l Codeine 56ng/ml 30-340ng/ml >1600ng/ml Morphine (free) <5ng/ml 10-100ng/ml 50-4000ng/ml Case 2 30 year old female found on floor with green fluid trailing from corner of mouth Ethanol Blood 181 mg/100mls Urine 244 mg/100ml Ethylglucuronide present in urine Acetone negative Methanol negative Isopropanol negative What effect might you expect? What caveat would you include? Is this likely to by PM alcohol production? Ranges: Normal Toxic Lethal Methadone 75-1100ng/ml 413 ng/ml EDDP = 276 ng/ml 200-2000ng/ml 400-2000ng/ml Amphetamine 471 ng/ml >500ng/ml >1000ng/ml Diazepam 21 ng/ml Nordiaz = 73ng/ml >5000ng/ml >30 000ng/ml Cause of Death?? 20-4000ng/ml 20-1800ng/ml Case 3 Chronic alcoholic found dead at home, head injury consistent with fall to the ground. Ethanol 16 mg/100mls 72 mg/100mls 25 mg/100mls 145 mg/100mls Supports ante-mortem consumption Acetone Blood Urine Vitreous Stom Cont Blood Urine Vitreous 3mg/100mls 9mg/100mls 4mg/100mls Methanol & Isopropanol 2mg/100mls of each in Blood, urine and vitreous Ketone But Can be produced pm What else do you want to know? Urine Glucose – negative Vitreous glucose – unrecordable Urine Ketones – present Blood Betahydroxybutyrate 2.3 mmol/L (<0.5 mmol/L) more specific than acetone HbA1c – 12.1% (4.0 – 6.1%) Urine ethyl glucuronide - present Diabetes – reconsider urine alcohol Case 4 Decomposed @ home on sofa with drug paraphenalia around LIVER Homogenate Ethanol Methanol 0.88 mg/g Not detected Not detected Isopropanol Not detected Acetone General drug screen by gas chromatography – mass spectrometry (GC-MS) Liver homogenate: Morphine, cocaine metabolites, flupenthixol and metabolites, paracetamol, chlorpromazine metabolites and cotinine detected detected Liver Tissue Homogenate Quantitative Analysis by Gas chromatography – Mass spectrometry (GC-MS) Cocaine = <0.02 ug/g Benzoylecgonine = 0.28 ug/g Methylecgonine = 0.26 ug/g Cocaethylene = 0.42 ug/g Morphine (free) = 1.05 ug/g Morphine (total) = 1.50 ug/g Was it worth doing if the concentrations mean nothing? COMMENTS The external examination showed an advanced state of decomposition with no evidence of injury to suggest involvement of another individual. Within the limits imposed by the degradation of the tissues, the internal examination showed no apparent pathology which could have caused or contributed to death. Interpretation of toxicological results is complicated in cases where the individual has been dead for some time. Drug levels are altered after death by diffusion of the substances throughout the body (post-mortem redistribution) and certain substances are produced or degraded in the post-mortem period. As such, it would be unreliable to draw conclusions from the drug concentrations themselves. However cocaine and morphine are not produced endogenously by the body and so their presence indicates that cocaine and morphine (possibly heroin) were taken by the deceased. Alcohol can be produced by the body after death but the presence of cocaethylene would suggest that alcohol and cocaine were used concurrently. The exact levels of the fore-mentioned drugs within the body at the time of death cannot be determined with any accuracy. However, we feel that their presence, along with the drug paraphernalia noted in the vicinity of the body and the absence of identifiable natural disease is significant. Based on the above information, we are of the opinion that, on the balance of probabilities, death was in keeping with polydrug toxicity. The information given within this report represents our understanding of the views, opinions and circumstances of this case based on the information that we have received to date, either in writing (all forms) or by oral communication. We recognise that in part this may reproduce or rely upon witness statements, oral communications or hearsay evidence of second parties and that the information given to us by others may or may not be factually correct at the time of our consideration. We reserve the right to reconsider any aspect of this report should further factual information arise that contradicts the information provided at the time of the postmortem examination, upon which we have based our interpretations. Cause of Death Ia. In keeping with polydrug toxicity Confounding Factors Considerations Ask Yourself Arterial vs venous variation Where was it from? Continuing gastric residue absorption Redistribution Post-mortem production or degradation Tolerance Limited reference range data Vitreous / blood / urine Site Was it appropriately preserved Is there decomposition? Is it a drug prone to redistribtution / pm production Do you know about their drug taking / drinking habits In Practice Seek a drug history from coroner’s officer Always give the toxicologists as much info as you have If you are looking for a specific substance – tell them as it might not be on their routine screen Appropriate specimens / appropriate site If tox is important talk to coroner’s officer about accessing ante-mortem bloods. Resources http://www.dundee.ac.uk/forensicmedicine/ C. Baselt, Disposition of Toxic Drugs & Chemicals in Man.