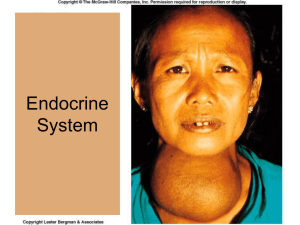
Endocrine dysfunction
(Hormone imbalances)
in Diamond Blackfan Anemia
Dr Amit Lahoti
Dr Phyllis Speiser
Cohen Children’s Medical Center of New York
North Shore LIJ Hospital System
Diamond Blackfan Anemia (DBA)
is a rare condition.
Really!!!
DBA
5-7 per 1,000,000 live births
Beta
thalassemia
Sickle-cell disease
1 per 100,000 live births
1 per 500 AfricanAmerican live births
Role of a registry
For rare conditions, clear guidelines on how to
manage the disease or its complications often
not available.
A registry provides a unique opportunity to do
systematic research.
Until more research data are available, doctors
use best practices learned from other somewhat
similar conditions.
Treatment course of DBA
BMT recipients
Pros and cons of DBA treatments
Pros
Corticosteroids
Chronic Transfusions
Bone marrow
transplant
No risk of iron
overload
First line treatment for
severe anemia under 1y
Can lead to resolution
of anemia
Can improve quality of
life
Cons
Risk of low bone
density
Frequent hospital visits
for transfusions
Risk of Graft versus
Host Disease (GVHD),
and infection
Excess weight gain &
impaired growth
Endocrine complications
of iron overload
Risk of graft rejection
Increased risk of
diabetes (at high
doses)
Side-effects of
immunosuppressive
drugs & radiation
Where do hormones come from and what do they do?
Risk of
Hormone disorders
in patients with DBA:
Is it real?
*Unpublished data presented at Pediatric Endocrine society meeting at Washington DC, 2013
You or some one sitting next to you
may have a similar story….
• At 6 months: Diagnosed with DBA
– Monthly transfusions started.
• Subsequently developed Iron overload
– Chelation therapy with Desferal started
• At 14.5 years, 7/2004: went to ER for frequent urination,
excessive thirst and 15 lb weight loss. Blood glucose
markedly elevated. Diagnosed with Diabetes mellitus,
– Insulin therapy started
• Two months later, 9/2004: Thyroid function tests show
Thyroid gland failure.
– Thyroid hormone started
In the next year…
• At 15 years, 12/2004: Teen non-compliant with insulin
regimen & diet. Poor blood glucose control, stunted
growth, despite normal GH levels. Diagnosed Growth
hormone resistance.
– Growth hormone therapy started
• At 15.75 years, 10/2005: Delayed puberty with evidence
of Pituitary failure.
– Testosterone therapy started.
• At 16.5 years, 5/2006: Multiple seizures related to low
blood glucose despite not being compliant with insulin
regime. Diagnosed with Adrenal insufficiency
– Hydrocortisone therapy started.
And as time went by…
• Two months later, 7/2006: Complaints of frequent
urination at night. Diagnosed Diabetes insipidus.
– DDAVP treatment started.
• At 17.5 years, 8/2007: Evidence of Diabetic kidney
damage.
– Enalapril treatment started.
• At 18 years, 2/2008: Growth hormone therapy stopped.
Adult height: 5 feet.
Hormone problems can start in
childhood!
You are never “too young” to be tested.
Early diagnosis can avoid later problems.
Questions?
What are these conditions?
How common are these?
Are you at risk?
How can you be tested for these?
How are they treated?
Hypogonadism
What is it?
Absent or delayed puberty
Hypogonadism
What is Delayed Puberty?
• In girls, no breast development by 13 years, or
no periods by 15 years or by 2 years after
breast development.
• In boys, no testicular enlargement by 14 years
Hypogonadism
How
common?
How to
diagnose?
How to
treat?
• With iron overload: 30-50%
• After BMT:
Females- ovarian malfunction in ~100%
Males- testicular dysfunction in 0-40%
Blood sampling for pituitary pubertyregulating hormones (LH and FSH) and
sex hormones (Testosterone or Estradiol).
Bone age x-ray of hand.
Males: Testosterone injections or skin gel.
Females: Estrogen oral or skin gel.
Hypothyroidism
What is it?
Insufficient thyroid hormone
Hypothyroidism
Feeling cold
out of ordinary
Not growing well
Or, no symptoms at all!!! ( especially in early stages)
Hypothyroidism
How
common?
How to
diagnose?
How to
treat?
• Patients with iron overload: 2-20 %
• Patients on steroids and after BMT:
Less common, frequency unknown
By measuring blood levels of:
Thyroid stimulating hormone (TSH); and
Total and free Thyroid hormone (T4)
Once a day thyroid hormone (tablets)
Adrenal insufficiency
What is it?
Not enough adrenal hormones
Stress hormone (cortisol)
Salt retaining hormone (Aldosterone)
Male hormones
Adrenal insufficiency
Dark color of nonsun- exposed areas
Low BP and dizziness
Extreme tiredness
Nausea, vomiting,
abdominal pain,
diarrhea, constipation
Muscle
weakness
Symptoms may be missed or attributed to anemia or missed!
Adrenal insufficiency
How
common?
Patients on steroids: considered to have
adrenal insufficiency
Patients with iron overload: biochemical
adrenal insufficiency (often partial): 18-45%
How to
diagnose?
Blood measurements of:
8 AM cortisol level,
Plasma renin activity, aldosterone,
Androstenedione and DHEAS levels
How to
treat?
Hydrocortisone: to replace stress hormone.
May only be needed during periods of stress.
Fludrocortisone: salt-retaining hormone.
Question #1
• Which of the following is NOT a part of the
endocrine system?
a)
b)
c)
d)
Thyroid
Pituitary
Appendix
Adrenals
Question #2
• This gland is sometimes called the master
gland, though it is only about the size of a pea
a)
b)
c)
d)
Thyroid
Pituitary
Pineal
Hypothalamus
Question #3
• Which of the following is the largest endocrine
gland in the body:
a)
b)
c)
d)
Thyroid
Parathyroid
Pancreas
Adrenal
Diabetes mellitus
What is it?
Not enough insulin hormone
Diabetes mellitus
• Both iron overload and glucocorticoids lead to:
↓in insulin secretion; and
↓ in insulin sensitivity
Diabetes mellitus
How
common?
• With Iron overload: 9-14%
• On Chronic glucocorticoids: dose
dependent. May be reversible.
• BMT: depends on pre-transplant factors.
How to
diagnose?
• Fasting blood glucose
• Fructosamine level (HbA1c may not be
reliable if on transfusions)
• Oral glucose tolerance test
How to
treat?
• Diet changes,
• Insulin therapy and/or
• Oral medications
Growth Problems
For patients <18 years age:
• How many of you are shown your/ your child’s
growth chart during the visit with the
pediatrician or hematologist?
• How many of you have asked to see your/ your
child’s growth chart during these visits?
Growth chart is an important tool to detect poor
growth or short stature at an early age!!!
Growth problems
Anemia and ?DBA itself
Iron overload
Short
stature
Low Growth hormone
Absent/
Abnormal
puberty
Hypothyroidism
Glucocorticoids
Multiple causes of poor growth in DBA patients
Growth problems
How
common?
• DBA itself: Reported short stature ~30%
• Effect on growth due to iron overload or
steroids alone is hard to quantify in
DBA due to this.
• BMT: may improve growth.
How to
diagnose?
• Regular growth monitoring for early
detection
• Laboratory testing to rule out specific
endocrine causes.
How to
treat?
• Specific to the cause.
• However, final height may still be low for
mid-parental height.
Bone disorders
How?
Bone disorders
Hypogonadism
Iron overload
Weak
bones
? Low Growth hormone
Low Vitamin D
& parathyroid
gland failure
Diabetes mellitus
Glucocorticoids
Multiple causes of poor bone density in DBA patients
Bone disorders
How
common?
• With Iron overload: upto 50%
• On Chronic glucocorticoids: Dose and
duration dependent.
• After Bone marrow transplant: Not known
• Test for other endocrine problems
• Blood levels of Calcium, parathyroid
hormone and vitamin D
• Bone mineral density scan
How to
diagnose?
How to
treat?
•
•
•
•
Treat any co-existing hormone problem
Vitamin D supplements: Adequate level?
Other medications: Bisphosphonates
Newer drugs being developed.
Importance of Screening
• Vague symptoms may also be seen with anemia itself.
• Often no/minimal symptoms in early stages.
14%
impaired glucose
tolerance
1.5%
Diabetes mellitus
84.5%: normal
Diabetes screening in non- diabetic otherwise
asymptomatic beta thalassemia patients
Importance of Chelation
Impaired
glucose
tolerance
(IGT)
Normal
glucose
tolerance
Insulin
dependent
diabetes
mellitus
Intensive chelation in patients with IGT can improve beta-cell
function, improve blood glucose values.
Less effective in patients who have developed DM and in
improving insulin resistance.
Treatable nature of most of these
conditions!That’s what I love about
endocrinology!!!
• Timely diagnosis & treatment can prevent
morbidity and possible mortality associated
with some endocrine conditions.
- Versus possible long-term adverse effects of an
untreated endocrine problem.
What do we need to do?
• The only published reports about hormone
problems in DBA patients are in form of case
reports or case series with few patients.
• Collect more information about endocrine
problems in DBA patients like you.
Vs
About our research study
SPECIFIC AIMS:
1. To study the effects of iron overload on various endocrine
glands in DBA patients receiving transfusions.
2. To estimate how common are these hormone
abnormalities in the DBA population and correlate it with
measures of iron overload.
3. To recommend a possible method to screen the at-risk
DBA patients for endocrine dysfunctions at regular
intervals.
4. To compare the presence of endocrine dysfunction in
chronic transfusion dependent DBA population with DBA
patients not on chronic transfusions and beta thalassemia
major patients on chronic blood transfusions.
About our research study
Eligibility Criteria:
Inclusion criteria:
Age 1-39 years; and
Diagnosed with DBA and enrolled in DBA
Registry (DBAR), or
Diagnosed with beta thalassemia major and
followed at NSLIJ pediatric hematology division.
Exclusion criteria:
Pregnant; or
Having received a bone marrow transplant
About our research study
• Participation involves a standard endocrine evaluation.
• This includes blood tests that can be ordered and drawn at
your primary institution. The participation consent asks for
permission for us to receive the endocrine evaluation results.
Our goal is 75 DBA patients and 25 thalassemia patients
total for the study.
THANK YOU IN ADVANCE FOR YOUR PARTICIPATION!!!
THANKS FOR LISTENING!!!