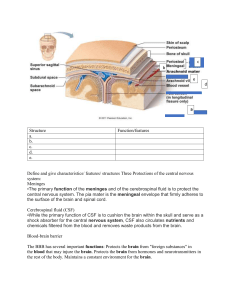
Pediatric Pharmacology Population Pharmacokinetics of Nusinersen in the Cerebral Spinal Fluid and Plasma of Pediatric Patients With Spinal Muscular Atrophy Following Intrathecal Administrations The Journal of Clinical Pharmacology 2017, 00(0) 1–11 C 2017, The American College of Clinical Pharmacology DOI: 10.1002/jcph.884 Kenneth T. Luu, PhD1 , Daniel A. Norris, PhD1 , Rudy Gunawan, PhD1 , Scott Henry, PhD2 , Richard Geary, PhD3 , and Yanfeng Wang, PhD1 Abstract Nusinersen is an antisense oligonucleotide intended for the treatment of spinal muscular atrophy. The pharmacokinetics of nusinersen, following intrathecal administrations, in the cerebrospinal fluid (CSF) and plasma of 72 pediatric patients (3 months to 17 years) with spinal muscular atrophy across 5 clinical trials was analyzed via population-based modeling. With sparse data in the CSF and profile data in the plasma, a linear 4-compartment model simultaneously described the time-concentration profiles in both matrices. The typical population parameters were: Qp = 0.572 L/h, QCSF = 0.069 L/h, CLp = 2.50 L/h, CLCSF = 0.133 L/hr, VCSF = 0.441 L, Vp = 32.0 L, Vsystemic_tissue = 429 L, and VCNS_tissue = 258 L. A full covariate modeling approach identified baseline body weight to be a statistically and clinically relevant covariate on VCSF , Vp , and CLp . The model predicted that the CSF volume of distribution increased steadily with age from 0 to 2 years but became relatively steady for children >2 years. Simulations from the final model showed that age-based dosing in children under 2 years ensured a more comparable exposure (peak concentration and area under the concentration-time curve) across subjects in the population relative to a fixed dosing scheme. However, because no dose-limiting toxicity has been reported in any of the trials, a fixed-dose scheme (12 mg across all age groups) was recommended. The median terminal half-life of nusinersen in the CSF was determined from the model to be 163 days, which supported infrequent dosing, once every 4 to 6 months in pediatric patients with spinal muscular atrophy. Keywords nusinersen, cerebral spinal fluid, intrathecal administration, spinal muscular atrophy, Spinraza, population pharmacokinetics Spinal muscular atrophy (SMA) is an autosomal recessive neuromuscular disease characterized by degeneration of the motor neurons in the anterior horn of the spinal cord, resulting in atrophy of the voluntary muscles of the limbs and trunk. SMA is a debilitating disease, rendering patients unable to walk, eat, or breathe in its most severe form. SMA has an incidence of 1:6000 to 1:10,000 live births; it is the most common monogenetic cause of infant mortality and a major cause of childhood morbidity due to weakness.1 SMA is caused by loss of survival motor neuron (SMN) protein due to a homozygous recessive deletion or mutation in the SMN1 gene on chromosome 5q11-q13.2 Humans have a duplication of the chromosome region where SMN1 is found, resulting in a nearly identical copy of the gene, SMN2. In SMN2, a C-to-T nucleotide substitution in exon 7 results in an alternative splicing event such that the majority of transcripts produced (90%) lack exon 7, and a defective truncated protein (often referred to as 7) is produced.3 Low levels of SMN protein result in the degeneration of spinal motor neurons and cause muscle weakness that is followed by symmetric limb paralysis, respiratory failure, and death.1,4,5 Nusinersen is a uniformly modified 2 -O-(2-methoxyethyl) antisense oligonucleotide in development for SMA. These so-called “uniformly modified” antisense oligonucleotides can interfere with RNA function and metabolism (e.g., translation into protein, splicing, polyadenylation).6 Nusinersen corrects a splicing defect in the SMN2 pre-mRNA, rather than to promote degradation of a targeted mRNA as is a typical case for antisense oligonucleotides. It is designed to bind to a specific sequence in the intron 1 Pharmacokinetics and Clinical Pharmacology, Ionis Pharmaceuticals, Carlsbad, CA, USA 2 Nonclinical Development, Ionis Pharmaceuticals, Carlsbad, CA, USA 3 Clinical Development, Ionis Pharmaceuticals, Carlsbad, CA, USA Submitted for publication 25 October 2016; accepted 31 January 2017. Corresponding Author: Kenneth Luu, PhD, Ionis Pharmaceuticals, 2855 Gazelle Ct, Carlsbad, CA 92010 Email: kenneth.t.luu@gmail.com 2 downstream of exon 7 of the SMN2 pre-mRNA transcript, thus promoting the increase in inclusion of exon 7 in SMN2 mRNA.7 The result is increased production of full-length SMN protein, equivalent to SMN protein produced by the SMN1 gene. Because the number of SMN2 gene copies and resulting amount of SMN protein is correlated with disease severity and age of onset, a therapeutic approach predicted to benefit SMA patients is to increase the levels of full-length SMN2 pre-mRNA by restoring the splicing pattern that gives rise to full-length SMN2 mRNA. The clinical experience with nusinersen includes clinical trials in infants with genetically diagnosed and presymptomatic SMA, infants with “infantile-onset SMA” (most likely to develop type I SMA), and in children and adolescents with “later-onset SMA” (most likely to develop type II or type III SMA). The clinical pharmacokinetics (PK) of nusinersen has been evaluated in a number of trials (see Methods), measuring drug levels in both the cerebrospinal fluid (CSF) and the plasma. Unlike in the plasma, however, where serial sampling was performed, the sparse sampling in the CSF did not allow for the calculation of basic PK parameters in the CSF compartment such as volume of distribution and clearance with reasonable confidence. The objective of this work was to develop a population PK model that simultaneously describes the PK of nusinersen in the CSF and plasma, with the goal of generating interpretable PK parameters—and their interindividual variability—in both matrices. Methods Each of the above studies was approved by the respective local institution review board. Written informed consent and assent (if applicable) were obtained before any evaluations were conducted for eligibility. These trials were conducted in compliance with the Declaration of Helsinki, the International Conference on Harmonisation Good Clinical Practice guidelines, and local regulatory requirements. The study designs for the above studies are listed below (specific blood and CSF PK sampling times for each study are shown in Table S1 of the supplemental section). Study Design Data from 5 clinical studies were pooled for analysis (Protocols ISIS 396443-CS1, ISIS 396443-CS2, ISIS 396443-CS3A, ISIS 396443-CS10, and ISIS 396443CS12). In these 5 studies limited PK samples were obtained in the CSF, and serial PK samples were obtained in the blood of SMA patients. Study ISIS 396443-CS1 was an open-label singledose safety, tolerability, and dose-range-finding clinical trial (n = 24) in patients aged 2 to 14 years with SMA. A The Journal of Clinical Pharmacology / Vol 00 No 0 2017 brief PK summary from this study has been reported by Chiriboga et al.8 Patients were randomized at baseline to 1 of 4 independent treatment arms and received a single intrathecal dose of 1, 3, 6, or 9 mg. CSF samples were collected predose, at dose administration, and 7 days after dosing in the 1-, 3-, and 6-mg dose cohorts. In the 9-mg dose cohort, CSF samples were collected postdose on day 8 or day 29 (5 patients at each time point). Serial blood samples were collected on day 1 with additional blood samples collected on days 2, 8, and 29. Patients randomized to cohort 1 (1 mg) and completing study procedures were eligible to enroll in study ISIS 396443-CS2, and patients randomized to cohorts 2 to 4 (3, 6, and 9 mg) and completing study procedures were eligible to enroll in study ISIS 396443CS10. Study ISIS 396443-CS2 was an open-label multipledose safety, tolerability, and dose-range-finding clinical trial (n = 32) in patients aged 2 to 14 years with SMA. Patients were randomized at baseline to 1 of 4 independent treatment arms and received 2 (9-mg cohort only) or 3 intrathecal doses of 3, 6, 9, or 12 mg on days 1, 29 (3-, 6-, and 12-mg cohorts only), and 85. Six patients who participated in study ISIS 396443CS1 were eligible for and enrolled in study ISIS 396443CS2; 3 in cohort 1 (3 mg), and 3 in cohort 2 (6 mg). CSF samples were collected predose before each dose administration. Intensive blood profile samples were collected on days 1, 29 (3-, 6-, and 12-mg cohorts only), and 85 with additional blood samples collected on days 2, 8, 36, 86, and 92. Study ISIS 396443-CS10 was an open-label singledose safety and tolerability clinical trial (n = 16) in patients aged 2 to 14 years with SMA. Patients were randomized at baseline to 1 of 2 independent treatment arms and received a single intrathecal dose of 6 or 9 mg on day 1. All patients who enrolled in study ISIS 396443-CS10 participated in study ISIS 396443-CS1. CSF samples were collected predose on day 1. Blood samples were collected on days 1 (limited profile), 8, 85, and 169. Study ISIS 396443-CS3A is an ongoing open-label multiple-dose safety, tolerability, and PK clinical trial (n = 20) in patients aged >21 days to 7 months at the time of screening with infantile-onset SMA. Patients were randomized at baseline to 1 of 2 independent treatment arms and received 3 intrathecal doses of 6 or 12 mg during a “loading” dosing phase on days 1, 15, and 85. All patients received multiple 12-mg intrathecal doses every 4 months during a “maintenance” dosing phase beginning on day 253. CSF samples were collected predose before each dose administration. Blood samples were collected on days 1 (limited profile), 2, 15, 85 (predose and 4 hours postdose), and 92, followed by predose collections prior to each dose 3 Luu et al during the “maintenance” dosing phase beginning on day 253. Study ISIS 396443-CS12 is an ongoing open-label multiple-dose safety, tolerability, and PK clinical trial (n = 43) in patients aged 2 to 14 years with SMA. Patients received multiple intrathecal doses of 12 mg on days 1, 169, 351, and 533. All patients who enrolled in and completed study ISIS 396443-CS12 participated in either study ISIS 396443-CS2 or ISIS 396443-CS10. CSF samples were collected predose on all dosing days. Blood samples were collected on days 1 (limited profile), 85, 169, 351, and 533. Dose Scheme The intended age-based dose scheme applied in the later nusinersen trials were determined based on the age-to-CSF volume relationship equation reported by Matsuzawa et al.9 In this reference, Matsuzawa et al performed 3-dimensional magnetic resonance imaging in healthy children aged 1 month to 10 years and examined the CSF along with other brain regions. The CSF volume data from this study were best fitted to a model in which CSF volume (mL) = 149.88 + 13.90 × [ln(age [months]/100) + 0.7596]. From this equation, the applied age-based dose schemes were determined, with each dose intending to provide consistent exposure across the age groups: 9.6 mg (0-3 months), 10.3 mg (3-6 months), 10.8 mg (6-12 months), 11.3 mg (1224 months), and 12 mg (>24 months). Based on this scheme, infants less than 2 years received an age-based dosing, as listed, and children >2 years received a fixed 12-mg dose. Of note is that this dosing scheme was not made based on PK or PK/PD results and, thus, was considered purely experimental. Dose escalation during the development of this program was based primarily on safety monitoring starting at 1 mg in the first trial. However, the escalations were made with the desire to achieve the preclinical efficacious CSF concentrations seen in monkeys. Bioanalytical Assays A noncompetitive hybridization nuclease-based enzyme-linked immunosorbent assay (ELISA) method or an electrochemiluminescence (ECL) method was used to quantify intact nusinersen in human CSF and plasma. The ELISA method was used to quantify intact nusinersen in CSF and plasma for study ISIS 396443-CS1 only. The ECL method was used to quantify intact nusinersen in CSF and plasma for studies ISIS 396443-CS2, ISIS 396443-CS10, ISIS 396443-CS3A, and ISIS 396443-CS12. The sensitivities of the ELISA (1.5 ng/mL) and ECL (0.05 ng/mL) assays were sufficient to characterize the disposition of nusinersen well below levels associated with pharmacologic activity. For the ELISA method, the quantitation range for a sample is 1.5 ng/mL to 150 ng/mL from lower limit of quantification to upper limit of quantification, respectively. For the ECL method, the quantitation range for a sample is 0.05000 ng/mL to 10.00 ng/mL (from lower to upper limit of quantification). Samples with concentrations previously observed or expected to be above the upper limit of quantification were diluted within the range using a suitable volume of blank matrix prior to analysis. Calibration standards were within 25% of the theoretical concentration at the lower limit of quantification and within 20% of the theoretical concentration for all other levels, except for the anchor point, which had no precision criteria. The criteria for quality controls were within 20% of the theoretical value if the precision of each replicate was within 20%. During validation of either assay, the intra-assay and interassay precisions were 20%, and accuracies were within ±20% of the theoretical value for each QC level. Cross-validation of the 2 methods confirmed suitability of transition from ELISA to ECL. Analyses for CSF and plasma concentrations using ELISA and ECL were conducted with fully validated methods, and samples were analyzed under United States Food and Drug Administration Good Laboratory Practice guidelines. Modeling Methodology NONMEM 7.2 (Icon, Ellicott City, Maryland) was used for all model estimation. First-order conditional estimation interaction was used for the base model as well as the final model. Perl speaks NONMEM (PsN; Uppsala Universitet, Uppsala, Sweden) 4.2.0, Xpose 4.0.4, R 3.3.1 (with the installation and implementation of the following library packages: ggplot2, lattice, gridExtra, GGally, and plyr) were used for postprocessing and plotting results. The prediction-corrected visual predictive check (pcVPC) with parameter uncertainty was conducted using PsN.10 The intersubject variability in the structural PK parameters was modeled using multiplicative exponential random effects of the form: θ i = θ · eηi (1) where θ is the typical individual (population mean) value of the PK parameter and ηi denotes the interindividual variability (IIV) accounting for the i-th individual’s deviation from the typical value having 0 mean and variance ω2 . Interoccasion variability (IOV) was deemed to be important, especially because of the intrathecal route of administration, sampling procedure, and infrequent dosing intervals (4-6 months), and was also evaluated as an additional level of random effect on 4 The Journal of Clinical Pharmacology / Vol 00 No 0 2017 CSF clearance. The relationship was expressed as follows: Pi = TVPex p (I O V ) (2) where I O V = κ1i ·OCC1 +κ2i ·OCC2 + . . . + κni ·OCCn (3) Pi is the parameter of interest, TVP is the typical value of the parameter, OCCn (occasion) has the value of 1 for the nth occasion, otherwise 0, for each individual. κ 1 . . . n -values are random variables assumed to be normally distributed around 0 with identical variance denoted by π 2 P .11 Four occasions were defined in this analysis: each dose event was assigned a unique occasion starting with 1 for the first dose, 2 for the second dose, and 3 for the third dose. For the fourth and additional doses, the occasions were assigned to 4. Goodness of fit was determined based on diagnostic plots and precision of the parameter estimates. Hypothesis testing to discriminate among alternative hierarchic structural models was performed using the likelihood ratio test. When alternative models were compared, the difference in the NONMEM objective function was approximately χ 2 distributed with n degrees of freedom, where n was the difference in number of parameters between the hierarchic models. A decrease of 6.64 in the value of the objective function was considered significant under the likelihood ratio test (n = 1, P < .01). The full covariate model approach was used.12 As opposed to stepwise covariate modeling, the full covariate model approach emphasized parameter estimation rather than stepwise hypothesis testing.12 This method initially built a stable and structurally sound base model using the standard goodness-of-fit diagnostics. Then, extensive graphical evaluation was utilized to assess the correlation between each covariate and each η as well as evaluating potential relationship between each covariate and each model parameter. The final model was then constructed, and point estimates and parameter precision were evaluated for all base model parameters and covariate model parameters. The performance of the final model was evaluated by conducting a visual predictive check (VPC). Simulations were performed using the subjects’ characteristics and the dosing and sampling history from the original data set using PsN. From these simulations, concentration-time data were summarized using median and 2.5th and 97.5th percentiles. Because the diagnostic value of a VPC can be hampered by binning across a large variability in dose and/or influential covariates, the pcVPC was used. The pcVPC offers a solution to these problems while retaining the visual interpretation of the traditional VPC.10 In a pcVPC, the variability originating from binning across independent variables is eliminated by normalizing the observed and simulated dependent variable based on the typical population prediction for the median independent variable in the bin. Because the observed data from the CSF were very sparse, limiting the ability to calculate the CSF terminal half-life for the individual patients in the dataset, the approach was taken to calculate this parameter based on the model-derived individual post hoc estimates of the microconstants. The CSF portion of the structural model was set up to be identical to a traditional 2-compartment model, and the CSF β half-life was calculated based on the following formula13 : Beta H L = ln2 0.5(k12 +k21 +k10 − (k12 +k21 +k10 )2 − 4k21 k10 ) (4) Simulations Population simulations were performed using the final model to test if the age-based dose scheme (see Dose Scheme section) implemented in the trials was valid. In these simulations a data set of 1000 virtual subjects with normal distribution in age ranging from 0.1 month to 17 years with a mean age of 5 years (these statistics were based on the modeled data set) was created; each subject was randomly assigned to an age value based on this distribution. SMA patients tend to have low body mass index despite increased fat mass and overweight.14 Thus, SMA patients are not expected to have normal age-weight correlations, and the Center for Disease Control age-weight chart was not used. The body weight was then assigned to the subjects according to their assigned age using the age–body weight relationship determined from the original data set. This age–body weight relationship was modeled by a piecewise relationship (pivoted among 0, 1, and 6 years of age). The fitting was implemented using the R function: lm(formula=BWTbs(AGE, df=NULL, knots=c(0,1,6)), data=d1) under the “splines” library package. Once the age–body weight relationship was determined, the body weight was calculated based on the subject’s assigned age. The simulation outputs were exported to WINNONLIN for determining area under the concentration-time curve (AUCinf ) and peak concentration (Cmax ). Box plots of AUCinf and Cmax were presented by age (with intersubject variability and residual variability included but not IOV). 5 Luu et al Table 1. Subject Demographic Based on the Pooled Data Set Used in the Analysis Number of Subjects (N) Age, y, Median (Range) Male Female Weight, kg, Median (Range) All 72a 5 (0.10 to 17) 37 35 15.2 (5.1 to 83) CS1 24 6 (2 to 12) 9 15 18.6 (10.3 to 52.1) CS2 32 5 (2 to 15) 19 13 21.5 (10.8 to 83.1) CS10 16 6 (2 to 11) 5 11 18.4 (10.3 to 52.1) CS3A 20 0.425 (0.10 to 0.57) 12 8 6.58 (5.07 to 9.25) CS12 43 7 (3 to 17) 22 21 16.9 (10.3 to 83.1) Study Race White 62, Black 4, Asian 3, Other 3 White 19, Black 1, Asian 2, Other 2 White 28, Black 2, Asian 1, Other 1 White 13, Black 1, Asian 1, Other 1 White 16, Black 1, Asian 1, Other 2 White 39, Black 1, Asian 2, Other 1 CSF Data Points Plasma Data Points 279 1181 15 105 53 458 16 118 89 183 100 293 a Note that many subjects continued on from one study to another; thus, the total number of unique subjects in all of the studies is less than the sum of the numbers of subjects in each study. Figure 1. Diagram of the structural model. CLp represents plasma clearance; CLCSF , CSF clearance; QCSF and Qp , the intercompartmental clearances within the CSF and plasma, respectively; VCSF , VCNS_tissue , Vp , and Vsystemic_tissue , apparent volumes in the CSF, CNS tissue, plasma, and systemic tissue compartment, respectively. Results Table 1 lists the demographics and the data points used in the model. In brief, the model included 72 subjects (37 males and 35 females) having 279 CSF and 1181 plasma concentration data points. The base and full structural model are diagrammed in Figure 1. The model consisted of a total of 4 compartments, with 2 compartments representing the CNS (a CSF compartment and a CNS tissue compartment) and 2 compartments representing the plasma and peripheral tissue. The model was defined in terms of the following parameters: CLp represents the plasma clearance, CLCSF represents the CSF clearance, QCSF and Qp represent the intercompartmental clearances within the CSF and plasma, respectively, and VCSF , Vp , Vsystemic_tissue and VCNS_tissue represent the modelestimated apparent volume of distribution in the CSF, plasma, systemic tissue, and CNS tissue, respectively. All clearance rate constants in the model were assumed to be linear. Parameters of the base model and final model are shown in Table 2. Overall, the base model estimated the parameters with reasonable precision as shown. Diagnostic plots of the base model are shown in Figure 2, indicating reasonable goodness of fit. For the base model, the random effects associated with the IIVs were assigned to CLp , CLCSF , VCSF , and Vp ; their estimated IIVs were 58.5, 24.8, 104, and 63.2%, respectively. Interoccasion variability was estimated to be 38.1%. Baseline body weight (BWT), baseline age, baseline body surface area, and baseline height were found to be highly collinear to each other. Thus, covariate testing was not performed on all of these variables. Because BWT was considered most physiologically relevant, it was selected to be tested for covariate effect. In the final model, a power model was used to relate BWT to VCSF 6 The Journal of Clinical Pharmacology / Vol 00 No 0 2017 Table 2. Parameters of the Base Model and Final Modela Base Model Parameter Definition Typical Value (%RSE) Unit %IIV η Shrinkage (%) Typical Value (%RSE) Unit %IIV η Shrinkage (%) 0.572 (11.3) L/h NE NA 0.568 (11.7) L/h NE NA 0.069 (18.1) L/h NE NA 0.0712 (19.5) L/h NE NA 2.50 (11.2) 0.133 (8.87) 0.441 (21.7) L/h L/h L 58.5 24.8 104 1.78 19.4 15.2 2.36 (5.04) 0.136 (9.12) 0.433 (21.7) L/h L/h L 29.5 24.4 88.1 7.25 20.7 18.0 32.0 (21.7) L 63.2 3.66 29.0 (11.4) L 39.0 10.0 429 (19.2) L NE NA 418 (20.9) L NE NA 258 (17.1) L NE NA 263 (18.9) L NE NA NA NA NA None 38.1 NA 4.51 NA NA 0.689 (12.2) NA None 38.1 NA 5.21 NA NA None NA NA 0.596 (52.3) None NA NA NA None NA NA 0.047 (21.7) None NA NA 0.493 (2.39) None NA 6.94 ( shrinkage) 0.494 (2.45) None NA 6.81 ( shrinkage) Qp Intercompartmental clearance between the plasma and the systemic tissue compartments Intercompartmental QCSF clearance between the CSF fluid and the CNS tissue compartments Plasma clearance CLp CSF clearance CLCSF Volume of distribution in VCSF the CSF Volume of distribution in Vp the plasma Volume of distribution of Vsystemic_tissue the systemic tissue compartment VCNS_tissue Volume of distribution of the CNS tissue compartment IOV Interoccasion variability BWT on CLp Covariate effect of the baseline body weight (BWT) on CLp BWT on VCSF Covariate effect of the baseline body weight (BWT) onVCSF BWT on Vp Covariate effect of the baseline body weight (BWT) on Vp (Proportional) Residual error (proportional structure) a Final Model %IIV indicates intersubject variability (%); IOV, interoccasion variability; NA, not applicable; NE, not estimated or fixed to 0; %RSE, relative standard error (%). and CLP , and a linear model was used to relate BWT to Vp as defined in the following equations: Vcs f (i) =Vcs f e eta(i) BW Ti M BW T θ V cs f , (5) V p(i) =V p eeta(i) [1+ V p(i) (BW T − M BW T )], C L p(i) = C L p eeta(i) BW Ti M BW T θC L p , (6) (7) where VCSF(i) is the individual specific value of CSF volume, VCSF is the population value of CSV volume, θ VCSF is the estimated power coefficient scaling VCSF(i) and VCSF based on body weight (BWTi ), Vp(i) is the individual specific value of plasma volume, θ Vp(i) is the linear parameter scaling BWT to Vp(i) , MBWT is the median body weight based on the data. CLp(i) is the individual plasma volume, CLp is the population volume, and θ CLp is the estimated power coefficient scaling CLp(i) and CLp based on BWT. A summary of model performance of the base model relative to the full model is presented in Table 2. The final model resulted in a –89-point change in OFV compared to the base model. Incorporating BWT into the final model reduced the IIVs by –29, –0.4, –16, and –24 for CLp , CLCSF , VCSF , and Vp , respectively, confirming that BWT was a meaningful covariate. Diagnostic plots of the base model are shown in Figure 2. The diagnostic plots of the final model are shown in Figure 3, indicating reasonable goodness of fit. The pcVPC plots of the final model are shown in the supplementary Figure S1. Separate diagnostic plots for plasma and CSF are shown in supplementary Figures S2 and S3, respectively. There appeared to be a clear trend in the population model-predicted–vs– dependent variable plot for the CSF data, indicating that additional sources of variability had not been accounted for by the model. 7 Luu et al Figure 2. Diagnostic plots of the base model fit. DV indicates dependent variable (concentration); PRED, population model prediction; IPRED, individual prediction; red line, line of identity or line through 0; blue line, trend line; gray shade, 95% confidence interval of the trend line. Figure 3. Diagnostic plots of the final model fit. DV indicates dependent variable (concentration); PRED, population model prediction; IPRED, individual prediction; red line, line of identity or line through 0; blue line, trend line; gray shade, 95% confidence interval of the trend line. The median β half-life of nusinersen in the CSF was 163 days as calculated from the post-hoc estimates of each individual’s PK parameters using equation 4. The CSF half-life did not change with age (Table 3). Results of the population simulations are shown in Figure 4. For the fixed-dose scenario (all patients received 12-mg dose), neonates and infants up to 3 months tended to be overexposed in terms of AUCinf and Cmax . However, the protocol-based dosing (agebased up to 2 years and fixed dose >2 years) ensured a more consistent AUCinf and Cmax . The simulated median profiles of nusinersen following a single dose in all 4 compartments are shown in Figure 5. Nusinersen had a steep distribution phase followed by a prolonged elimination phase in the CSF. CSF and CNS tissues were quickly equilibrated, followed by plasma uptake and then systemic tissue uptake. Discussion SMA is one of the most common genetic causes of infant death.15 Clinical trial results of nusinersen administered intrathecally showed good safety and tolerability profiles and promising clinical outcomes.8 In a phase 2 open-label study, patients with type I 8 The Journal of Clinical Pharmacology / Vol 00 No 0 2017 Table 3. Model-Derived CSF Terminal Half-Life Values by Age Groups Terminal Elimination Half-Life Age Group N Mean (Days) SD Median (Days) Range (Days) All (0.1 to 15 years) 0 to 3 months 3 to 6 months 6 to 12 months 1 to 2 years 2 to 6 years >6 years 72 5 8 7 9 22 21 172 169 166 180 180 169 173 32.7 18.7 22.0 28.3 40.0 31.0 40.1 163 159 165 171 172 163 160 123 to 310 155 to 199 135 to 196 145 to 224 147 to 289 123 to 247 139 to 310 SD, standard deviation. Figure 4. Population simulations (n = 1000 virtual subjects) showing AUCinf (A and B) and Cmax (C and D) relative to age following either a fixed dose (A and C, 12 mg single dose for all virtual subjects, n = 1000) or a protocol-based (single dose, dose level based on age) dose adjustment (C and D, age-adjusted for subjects 2 years, 12 mg for subjects >2 years as implemented in the protocols). For each box in the plot, thick middle line is the median, lower and upper edges are first quartile and third quartile, respectively, and whiskers are minimum (lower whisker) and maximum (upper whisker). SMA who were treated with nusinersen demonstrated significant (P = .01) improvements in motor function scores, incremental achievement of motor milestones such as head control, rolling, sitting, and improvements in neuromuscular electrophysiology compared to baseline and published natural history data.16 In this article we report a population PK model for intrathecally dosed nusinersen describing the pooled time-concentration data from 5 clinical trials in the CSF and plasma of pediatric patients with SMA. With sparse data in the CSF, the population PK model enabled the estimation of PK parameters in the CSF by integrating the CSF PK data with rich plasma PK data. The PK of nusinersen in the CSF and plasma were best described, simultaneously, by a 4-compartment model with 2 compartments representing the CSF and CNS 9 Luu et al Figure 5. Simulated median PK profiles of nusinersen in the CSF, CNS tissue, plasma, and systemic tissue following a single 12-mg fixed dose. tissue and 2 compartments representing the plasma and peripheral tissue. CSF formation in adults has been traditionally reported to be 500-600 mL/d with a turnover rate of about 4 times per day.17 Recent imaging data, however, indicated that CSF turnover rate could be much faster than traditionally reported: 140 times a day, with fluxes of more than 22 mL/min.18 CSF turnover in infants is thought to be higher than that in children and adults.19 Nevertheless, nusinersen has a CSF half-life much beyond the human CSF turnover rate and was predicted by our model to be 163 days. This halflife value was in agreement with the values calculated from monkeys, where more CSF PK sampling took place, which were reported to be >100 days.20 The extended half-life was most likely due to distribution from CSF to the CNS tissue compartment and slow equilibration back to the CSF before it was cleared into the systemic circulation. The inclusion of the CNS tissue compartment in the model was also supported by measurable brain concentration data obtained from monkeys following an intrathecal dosing at clinically relevant doses (unpublished data). Post hoc CSF halflife values for all 72 subjects included in the population PK modeling indicated that the CSF half-life of nusinersen was not age (or body-weight) dependent. Covariate testing resulted in the BWT being a clinically relevant covariate on the VCSF . In the evaluation of the covariate effect of BWT on CSF exposures, population simulations were performed to investigate whether covariate-adjusted dosing was warranted. In these simulations we tested whether (1) fixed dosing was feasible with nusinersen across all age groups and (2) the age-adjusted dosing for the youngest patients (2 years) according to the dose scheme implemented in the protocols was justified. These results indicated that fixed dosing led to higher exposure in young patients (0-3 months) in terms of Cmax and AUCinf . The protocol age-based dosing scheme ensured a more comparable exposure across all age groups (Figure 4). Based on these covariate-exposure relationships, however, a more simplified dosing scheme than the protocol scheme might be feasible. For example, agebased dosing may be applied only for patients 0-3 months rather than 0-24 months. Alternatively, because no dose-limiting toxicity has been reported in any of the trials, a fixed-dose scheme could be recommended despite the inconsistent exposure across the age groups. The PK profiles of nusinersen in the plasma following intrathecal dosing was biphasic, which was commonly described by a 2-compartment model following a systemic (subcutaneous) administration.21,22 Although the influence on plasma Vp and CLp appeared to be clinically relevant (parameter-covariate plots not shown), the covariate-adjusted dosing for nusinersen was considered based only on CSF PK rather than plasma PK because the CNS is the site of action. In addition, the SMN target for nusinersen is located in the CNS, not in the circulation or peripheral tissue. The sparseness of the CSF data limited our ability to test for more refined mechanism(s) of distribution of nusinersen in the spinal cord and in the brain. The aim of our top-down approach was to develop a parsimonious model using the available data, not intending 10 to capture the complex physiology of the CNS space. For example, temporal and spatial distribution within the spinal cord, brain, and other CNS tissues were not accounted for. Others have developed multicompartment distribution models and computational models to describe drug distribution in the CSF for intrathecally dosed drugs.23,24 Thus, the physiologically relevant kinetics of nusinersen could be better accounted for with more relevant data. In addition, the model assumed the transport from the CSF to the plasma compartment to be the predominant mechanism of CSF clearance and that possible elimination due to other mechanisms (ie, potential metabolism within the CNS tissues, including brain) were assumed to be relatively insignificant. Attempts at including additional elimination rate constants were unsuccessful due to the sparseness of the CSF data. SMA disease severity or type has not been shown to affect CSF volume or turnover rate. In addition, impairment of organs involved in the uptake and clearance of ASOs (eg, liver and kidney) has not been associated with the disease state in humans. Thus, we did not consider the disease state to be a mechanistically relevant covariate and did not include it in the covariate testing. The CNS tissue, particularly the brain tissue, is the intended site of action, where SMN neurons are degenerated in SMA patients. Although we separated the CSF from the CNS tissue as distinct compartments in our model, there are, as structured by the model, transfer kinetics between the 2 compartments. At steady state, we expect the CSF concentration to be proportional to the CNS tissue concentration. The assumption of the structural model, however, can be supported with additional data, such as brain tissue data, which are difficult to collect in the clinical setting but could be performed in rare cases by biopsy or with postmortem sampling. Because the model was meant to be descriptive rather than fully mechanistic, it has inherent limitations. Thus, the parameters of this model should be carefully interpreted. First, for example, the CSF volume estimated from the model should be considered an apparent volume of distribution rather than an actual physiological volume. The final model estimated the typical CSF volume to be 433 mL, whereas the physiological volume of the CSF is reported to be about 150 mL in humans.25 Second, due to the sparse sampling in the CSF (with no distinct distribution profile), we limited the model to include a single transport rate constant from CSF to plasma but no transport rate constant from the plasma to the CSF. Thus, CSF reabsorption of drug is not accounted for by the model. Third, the CNS compartment is a lumped compartment consisting possibly of the spinal cord tissue, subarachnoid The Journal of Clinical Pharmacology / Vol 00 No 0 2017 space, and brain tissue. Thus, this compartment should not be interpreted solely to mean the brain compartment. Last, we did not explore between-trial variability, which can be important, especially because, in our trials, many patients transition from 1 trial to the next. We, however, did test for IOV and found it to be important, as shown in the results. Although betweentrial variability and IOV are different, we feel that IOV, in some regards, indirectly accounts for some of the variability associated with the between-trial variability. Conclusions The PK of nusinersen in the cerebral spinal fluid and plasma of 72 infants and children with SMA across 5 clinical trials was analyzed via population-based modeling. The CSF and plasma PK of nusinersen were simultaneously described by a 4-compartment model. The only relevant covariate explaining variability in the PK of nusinersen was body weight (and thus, age, because the 2 variables were highly collinear in this population), which influences the VCSF , Vp , and CLp but not CLCSF . Simulations indicated that our agebased dosing scheme ensured more comparable median exposure in terms of Cmax and AUC relative to a fixed dosing regimen for all patients. However, because no dose-limiting toxicity has been reported in any of the trials, a fixed-dose scheme (12 mg across all age groups) was recommended. Sex and race did not likely explain variability in the PK of nusinersen. The long terminal half-life of nusinersen supported infrequent dosing, eg, once every 4 or 6 months in pediatric patients with SMA. Disclosure All authors are employees and stockholders of Ionis Pharmaceuticals, Inc. References 1. D’Amico A, Mercuri E, Tiziano FD, Bertini E. Spinal muscular atrophy. Orphanet J Rare Dis. 2011;6:71. 2. van der Steege G, Cobben JM, Osinga J, Scheffer H, van Ommen GJ, Buys CH. A sublocus of the multicopy microsatellite marker CMS1 maps proximal to spinal muscular atrophy (SMA) as shown by recombinant analysis. Hum Genet. 1995;96(5):589–591. 3. Ahmad S, Bhatia K, Kannan A, Gangwani L. Molecular mechanisms of neurodegeneration in spinal muscular atrophy. J Exp Neurosci. 2016;10:39–49. 4. Dubowitz V. Very severe spinal muscular atrophy (SMA type 0): an expanding clinical phenotype. Eur J Paediatr Neurol. 1999;3(2):49–51. 5. Crawford TO, Pardo CA. The neurobiology of childhood spinal muscular atrophy. Neurobiol Dis. 1996;3(2):97–110. 6. Bogdanik LP, Osborne MA, Davis C, et al. Systemic, postsymptomatic antisense oligonucleotide rescues motor unit maturation delay in a new mouse model for type II/III spinal muscular atrophy. Proc Natl Acad Sci USA. 2015;112(43):E5863–E5872. 11 Luu et al 7. Hua Y, Sahashi K, Hung G, et al. Antisense correction of SMN2 splicing in the CNS rescues necrosis in a type III SMA mouse model. Genes Dev. 2010;24(15):1634–1644. 8. Chiriboga CA, Swoboda KJ, Darras BT, et al. Results from a phase 1 study of nusinersen (ISIS-SMN(Rx)) in children with spinal muscular atrophy. Neurology. 2016;86(10):890– 897. 9. Matsuzawa J, Matsui M, Konishi T, et al. Age-related volumetric changes of brain gray and white matter in healthy infants and children. Cereb Cortex. 2001;11(4):335–342. 10. Bergstrand M, Hooker AC, Wallin JE, Karlsson MO. Predictioncorrected visual predictive checks for diagnosing nonlinear mixed-effects models. AAPS J. 2011;13(2):143–151. 11. Karlsson MO, Sheiner LB. The importance of modeling interoccasion variability in population pharmacokinetic analyses. J Pharmacokinet Biopharm. 1993;21(6):735–750. 12. Gastonguay M. A full model estimation approach for covariate effects: inference based on clinical importance and estimation precision [abstract]. AAPS J. 2004;6. 13. Gabrielsson JW, Weiner D. Pharmacokinetic and Pharmacodynamic Data Analysis, 3rd ed. Stockholm: Swedish Pharmaceutical Press; 2000: 82. 14. Sproule DM, Montes J, Montgomery M, et al. Increased fat mass and high incidence of overweight despite low body mass index in patients with spinal muscular atrophy. Neuromusc Disord. 2009;19(6):391–396. 15. Moultrie RR, Kish-Doto J, Peay H, Lewis MA. A review on spinal muscular atrophy: awareness, knowledge, and attitudes. J Genet Couns. 2016. 16. Finkel R, Chiriboga, CA, Vjsar, J, et al. Interim results of a phase 2 clinical study of nusinersen (ISIS-SMNRx) in patients with infantile-onset spinal muscular atrophy (AAN 2016, Poster P5.004). Poster presented at: 68th Annual American Academy of Neurology. 17. Artru AA. Spinal Cerebral Fluid Chemistry and Physiology. New York: Elsevier; 1999: 216. 18. Brinker T, Stopa E, Morrison J, Klinge P. A new look at cerebrospinal fluid circulation. Fluids Barriers CNS. 2014;11:10. 19. Bissonnette B. Pediatric Anesthesia. Shelton, CT: PMPH-USA; 2014: 455. 20. Rigo F, Chun SJ, Norris DA, et al. Pharmacology of a central nervous system delivered 2’-O-methoxyethyl-modified survival of motor neuron splicing oligonucleotide in mice and nonhuman primates. J Pharmacol Exp Ther. 2014;350(1):46–55. 21. Shimizu R, Kitade M, Kobayashi T, Hori S, Watanabe A. Pharmacokinetic-pharmacodynamic modeling for reduction of hepatic apolipoprotein B mRNA and plasma total cholesterol after administration of antisense oligonucleotide in mice. J Pharmacokinet Pharmacodyn. 2015;42(1):67–77. 22. Geary RS, Norris D, Yu R, Bennett CF. Pharmacokinetics, biodistribution and cell uptake of antisense oligonucleotides. Adv Drug Deliv Rev. 2015;87:46–51. 23. Kuttler A, Dimke T, Kern S, Helmlinger G, Stanski D, Finelli LA. Understanding pharmacokinetics using realistic computational models of fluid dynamics: biosimulation of drug distribution within the CSF space for intrathecal drugs. J Pharmacokinet Pharmacodyn. 2010;37(6):629–644. 24. Ummenhofer WC, Arends RH, Shen DD, Bernards CM. Comparative spinal distribution and clearance kinetics of intrathecally administered morphine, fentanyl, alfentanil, and sufentanil. Anesthesiology. 2000;92(3):739–753. 25. Johanson CE, Duncan JA 3rd, Klinge PM, Brinker T, Stopa EG, Silverberg GD. Multiplicity of cerebrospinal fluid functions: new challenges in health and disease. Cerebrospinal Fluid Res. 2008;5:10. Supporting Information Additional Supporting Information may be found in the online version of this article at the publisher’s website.