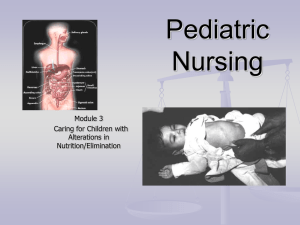
Cleft Palate
advertisement

GASTROINTESTINAL Common GI disorders in Children • Obesity • Anorexia Nervosa • Bulimia • Cleft lip/Cleft palate • GER • Pyloric Stenosis • Intussusception • Hirschprung’s Disease • Celiac disease • Giardiasis • Pin worm • Diarrhea EATING DISORDERS Overweight and Obesity • Many reasons the increase in overweight children in the US. • Calories consumed is not the issue • Lack of exercise is believed to be the main cause: • convenience of driving • unsafe neighborhoods • Television viewing and screen time accompanied by ingestion of high-calorie foods Childhood Obesity • Both immediate and long term side effects • Low Self-esteem • Can be a precursor of • hyperlipidemia, • sleep apnea • gall stones • orthopedic problems • HTN • DM Nursing Consideration • Identify risk and prevent new cases of overweight children • How much screen time per day? • TV, computer in bedroom? • Video games (unless Wii-fit or Kinect) • I-pods, I-pads, Smart phone? • Genetic factors and common lifestyles are also a risk • Overweight parents Nursing Considerations • Identify overweight children and support to establish healthy lifestyles • Screen time should be limited to 2 hours a day • Family exercise 30-60 minutes a day • Healthy snacking • Avoid ‘supersizing’ fast food portions • Limit eating out • Teach MyPyramid Nursing Considerations • Add fiber to prolong stomach emptying time • Teach methods to manage stress • Set short term, reachable goals (5lbs. over 1 month, not 50 for the year) • For school age obese children, formal weight loss programs are available Nursing Considerations • Teach children how to prepare food within developmental limits • Parental education plays a very important part in success. Anorexia Nervosa • A potentially life-threatening type of disordered eating • 95% of cases are girls age 12-18 • A voluntary refusal to eat b/c of an intense fear of gaining weight leads to: • Preoccupation with food and body weight • Excessive weight loss Causes of Anorexia Nervosa • Cultural overemphasis on thinness • May have existing “Perfectionist” personality • Possible biological cause • Life stress or loss • Conflict in the family • the child is not encouraged to be independent, and never develops autonomy…feelings of loss of control, poor self esteem Anorexia Nervosa • Poor self-esteem leads to a pronounced disturbed body image • Excessive dieting leads to a feeling of control over body Symptoms • Lengthy and vigorous exercise(up to 4 hours daily) to prevent weight gain. • Laxatives or diuretics to induce weight loss. • Intense and irrational fear of becoming obese (although underweight) • Fear does not decrease as weight is lost • Perceive food as revolting • Refuse to eat or vomit immediately after eating Symptoms • Girls can find support of anorexia on internet • Share information on weight loss techniques • View anorexia as beautiful Physical Characteristics • Excessive weight loss (25% less than normal body • • • • • • • • • weight) Hypokalemia Dysthymias Dependent edema Hypotension Hypothermia Bradycardia Lanugo formation Amenorrhea Can lead to death Treatment Goals • Address the physiologic problems associated with malnutrition • Local Hospital 2-3 days admission • Enteral feedings or TPN • replace lost fluid, protein, and nutrients • Address the behavioral and cognitive components of the disorder • Specialized Treatment Center-long term Long Term Out-Patient Treatment • Establish realistic goals • Build rapport, trusting relationship • Need to gain weight to reach 90-95 lbs. • 3 lbs per week, only weigh once a week. • Individual, group, and family therapy • Need continued follow-up, 2-3 years of counseling to be sure that self-image is being maintained Bulimia Binge eating followed by depression and activities to control weight gain • Also occurs primarily in adolescent females • Food is eaten secretly, high in calories • Abdominal pain from overfull stomach • Vomit to relieve the pain • Laxatives and diuretics • Affects older adolescents, college age Cause of Bulimia • Adolescent may be unable to express feelings • Has an existing low self esteem or depression • Lacks impulse control • Poor body image • Purging leads to increased sense of control and decreased anxiety Symptoms • Easily concealed • Usually average body weight • Physical Findings depend on amount of purging • Electrolyte imbalances • Tooth erosion, gum recession • Esophagitis • Abdominal distension Treatment • Hospitalization is usually not needed • Focus is on changing behavior • Treating depression • Teaching to recognize connections between emotional states and stress and the impulse to binge or purge STRUCTURAL DISORDERS Cleft lip/Cleft palate • Cleft Lip: failure of maxillary and median nasal processes to fuse • Cleft Palate: midline fissure of palate • Cause is believed to be multifactorial environmental and genetic • Apparent at birth => severe emotional reaction by parents Unilateral Cleft Lip Cleft Lip: Immediate nursing challenges birth until surgery Keep upright during feeding Cannot use a normal nipple (can’t generate suction) Use large soft nipple with large hole or a “gravity flow” nipple (deposits formula in mouth) Needs breaks during feedings Cleft Palate: Immediate nursing challenges birth until surgery Nipple must be positioned so that it is compressed by infant’s tongue and existing palate Swallow excessive air, burp frequently Immediate nursing challenges Emphasize positive aspects of child Hold infant close (modeling behavior), infant is special Explanation of immediate and longrange problems assoc. with CL/CP Surgical Repair • Cleft Lip age 6-12 wks • Z-plasty: staggered suture line minimizes scar tissue formation • May need more than one operation • Cleft Palate 12-18 months Post-operatively: Cleft Lip Repair • # 1 Priority-Protect operative site! • Logan Bar: thin arched metal device taped or butterflied to cheeks, protects suture line from tension & trauma • Arms restrained at elbows x 2 weeks Post-operatively: Cleft Lip Repair Clear liquids first => formula Breck feeder (syringe with rubber tubing), prevents infant from sucking on tubing until lip heals Meticulous care to suture line, carefully cleanse after feeding by gently wiping with saline Position on side or back Breck Feeder Post-operatively: Cleft Palate Repair • Can lie on abdomen • Fluids from a cup • Still needs restraint at elbow • No: pacifiers, tongue depressors, thermometers, straws, spoons • Blended diet => soft (no food harder than mashed potatoes) Cleft lip/palate & repair Pre-repair Post-repair Prognosis: good, BUT • Speech impairment • Improper tooth alignment • Varying degree of hearing loss • Improper drainage of middle ear => recurrent otitis media • Therefore upper respiratory infections need prompt treatment Gastroesophageal Reflux (GER) • LE sphincter & lower portion of esophagus are lax • Regurgitation of gastric contents into esophagus • Usually begins 1 week after birth • Regurgitation immediately after feeding Gastroesophageal Reflux Treatment • Upright position for feeding & 1h after feeding • Formula thickened with rice cereal or special formula • Enfamil AR (contains added rice) • Semi-elemental formula (Pregestimil, Nutramigen, Alimentum) • Zantac or Prilosec (decrease irritation) Pyloric Stenosis hypertrophied muscle of the pylorus is grossly enlarged leads to delayed stomach emptying Symptoms • Begins a few weeks after birth • regurgitation, occasional non-projectile vomiting 4-6 weeks after birth • progresses to projectile vomiting (3-4 feet) shortly after feeding Symptoms • Emesis contains stale milk, sour smell, no bile • Chronic hunger • Visible gastric peristalsis moves from left to right across the epigastrium • Dehydration, lethargic, weight loss Treatment • Pylorotomy • longitudinal incision through muscle fibers of the pyloris • Incision is in the periumbical area Pyloric Stenosis Post-op • High risk for infection-location of incision • Small, frequent feedings • “Down’s Regimen • NPO x 4 hrs, then Glucose and H2O q 2-3 hrs, then ½ strength formula/breast milk q 2-3 hrs, then full strength • Burp well to prevent air in stomach • Position right side Intussusception • Telescoping of one portion of the intestine into another • Most common site is the ileocecal valve • Inflammation, edema, ischemia, peritonitis & shock • Unknown why occurs, viral infection? Symptoms • Affects children (3mos to 5 years, usually occurs in first year of life) • Sudden acute abdominal pain q 15minutes • Vomiting (contains bile) • Lethargy • Tender, distended abdomen • Stools contain blood and mucus (“currant jelly”) Management • nonsurgical hydrostatic reduction (barium enema) • force is exerted by flowing barium via enema to push bowel back into place • surgery if unsuccessful • if positive bowel sounds (oral feedings) • watch for passage of normal brown stool MOTILITY DISORDERS Hirschprung’s Disease • Absence of nerve cells to the muscle portion of part of the bowel • Congenital abnormality Symptoms • Symptoms vary according to severity of aganglionic bowel • Severe-symptoms present in newborn • Mild-may not be detected until childhood Newborns • Failure to pass meconium • Spitting up, poor feeding • Bile-stained vomit • Abdominal distention Infancy • Failure to thrive • Abdominal distention • Constipation and may have episodes of vomiting and explosive, watery diarrhea with fever Childhood • Chronic constipation • May alternate with diarrhea • Ribbon-like stools • Abdominal distention • Poorly nourished, anemic Diagnosis • Barium enema, x-ray • Biopsy of intestine (will show lack of nerve enervation) Treatment • Bowel repair at 12-18 months • Surgery to remove the agaglionic portion of the bowel, 2 parts • Temporary colostomy Post Op • NG tube, IV, Foley • Abdominal distention • Assess bowel status • Assess stoma • Small, frequent feedings Closure of Colostomy • Perineal area is not accustomed to contact with stool. • Provide meticulous skin care, breakdown is very likely. • Teach parents • change diapers frequently • clean the perineal area carefully • apply a protective barrier at each diaper change. MALABSORPTION DISORDERS Celiac disease • Malabsorption syndrome • Inability to digest gluten leads to toxic levels that damage mucosal cells of small intestine Signs and Symptoms • Usually noticed at 9-18 months of age • Impaired fat absorption (Steatorrhea) • Behavioral changes (irritability, apathy) • Impaired absorption of nutrients (malnutrition, abdominal distention, anemia, anorexia, muscle wasting) Celiac Crisis • Acute, severe, profuse watery diarrhea and vomiting • May be precipitated by: infections, prolonged fluid and electrolyte depletion, emotional distress • Corn and rice are the dietary substitutes • Avoid oats, barley, rye, wheat Nursing Considerations • Supporting the parents in maintaining a gluten-free diet for the child for life even when symptom free • Watch for hidden sources of gluten • Assist in maintaining diet in school • Discontinuation of the diet • risk for growth retardation • Risk of gastrointestinal cancers INFECTIONS Intestinal parasites • Occur most frequently in tropical regions. • Outbreaks take place where: • Water is not treated • Food is incorrectly prepared • People live in crowded conditions with poor sanitation • Camping • Pets • Sandboxes Most Common Parasites in Children • Giardiasis • Pinworms Giardiasis • Transmitted hand-to-mouth • Cysts are ingested • Passed into the duodenum where they begin actively feeding. • excreted in the stool. Giardiasis Infants & young children: • Diarrhea, vomiting, anorexia, poor weight gain Children • Abdominal cramps, intermittent loose stools (malodorous, watery, pale, greasy), constipation Treatment Flagyl x 7 days) Pin Worms • Eggs float in air (easily inhaled) • Worms move on skin and mucous membranes cause intense itching • As child scratches eggs are deposited under fingernails • Hand to mouth activity leads to continual reinfection • Can live on toilet seats, doorknobs, bed linen, underwear, food Symptoms • Intense rectal itching • Nonspecific symptoms of irritability, poor sleep, bed-wetting, distractibility • Tape test loop of transparent tape pressed to perianal area for microscopic exam • Treated with (Vermox) mebendazole Intestinal parasites Provide preventative education • good hygiene and health habits. • appropriate sanitation practices I • wash hands after diaper changes, toilet use • deposit soiled diaper in closed receptacle Acute Gastroenteritis (Diarrhea) • Reabsorption of too little water • Produces diarrhea • Can lead to fluid and electrolyte alterations. • Inflammation of the stomach and intestines • Caused by viral, bacterial, or parasitic infections, or a chronic problem. • Rotavirus is the leading cause Symptoms Mild • A few loose stools each day without evidence of illness Moderate • Several loose or watery stools daily • Normal or elevated temp • Vomiting • Irritability • No signs of dehydration Diarrhea Severe • Numerous to continuous stools • Flat affect, lethargic • Irritability • Weak cry • Increased temperature (103-104) • Pulse & respirations weak & rapid Severe • Depressed fontanels • Sunken eyes, no tears • Poor skin turgor • Pale, cold skin • Urine output decreased • Increased specific gravity • 5-15% body weight loss • Metabolic acidosis Mild to moderate is managed at home • Assess fluid & electrolyte balance • Rehydration • Maintenance of fluid therapy • Reintroduction of adequate diet (BRAT) Bananas, Rice, Applesauce, Toast/Tea Oral rehydration therapy: (Pedialyte) Severe: requires hospitalization • Prevent spread to other patients/personnel • Admission weight and daily weight • IV replacement therapy Accurate I&O • Count frequency of bedding & clothing changes • Weigh diapers (1g = 1ml of fluid) • Monitor specific gravity of urine Nursing Interventions • Rest GI tract (NPO) • Assess skin turgor, mucous membranes, fontanel, sensory alterations • Maintain skin integrity • Stool samples • No rectal temps PRACTICE QUESTIONS! The nurse has completed discharge teaching on the dietary regimen of a child with celiac disease. The nurse recognized that client education has been successful when the mother states that the child must comply with the gluten-free diet: 1. 2. 3. 4. Throughout life Until the child achieved developmental milestones Only until symptoms resolved Until child reaches adolescence An 18-month child with a history of cleft lip and palate has been admitted for palate surgery. The nurse would provide which explanation about why a toothbrush should not be used immediately after surgery? 1. 2. 3. 4. The toothbrush would frighten the child The child no longer has deciduous teeth The suture line could be interrupted The child will be NPO While gathering admission data on a 2 year old child, the nurse notes all the following abnormal findings. Which finding is related to a diagnosis of Hirschsprung’s disease? (Select all that apply) 1. Bile-stained vomit 2. Decreased urine output 3. Poor weight gain since birth 4. Intermittent sharp pain 5. Alternating constipation and diarrhea A 6-week-old infant is brought to the pediatrician’s office with a history of frequent vomiting after feeding and failure to gain weight. The diagnosis of GER is made and discharge instructions are planned. The nurse should include to teach the parents to: 1. 2. 3. 4. Dilute the formula Delay burping Change to soy formula Position the baby 30-45 degree angle after feeding A child who underwent cleft palate repair has just returned form surgery with elbow restraints in place. The parents question why their child must have the restraints. The nurse would give which of the following as the best explanation to the parents? 1. 2. 3. 4. “This device is frequently used postoperatively to protect the IV site” “The restraints will help us maintain proper body alignment” “Elbow restraints are used postoperatively to keep the child’s hand away form the surgical site” “The restraints help maintain the child’s NPO status” The nurse is caring for an infant vomiting secondary to pyloric stenosis. The mother questions why the vomitus of this child’s looks different from that of her other children when they are ill. The nurse would best explain that the emesis of an infant with pyloric stenosis does not contain bile b/c: 1. 2. 3. 4. The GI system is still immature in newborns and infants The obstruction is above the bile duct The emesis is from passive regurgitation The bile duct is obstructed