40k doc - UCLA.edu
advertisement

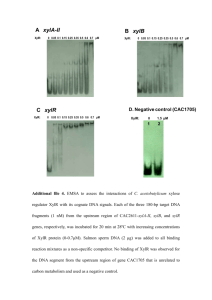
David Blanco, PhD CHS A2-087G MIMG C106 Mycobacteria Tuberculosis (TB), caused by the bacterium Mycobacterium tuberculosis, is the world’s leading cause of death in adults by a single infectious agent. In 1995, >3 million people died from tuberculosis and it is estimated that one third of the world’s human population is currently infected with M. tuberculosis. The incidence of TB continues to increase in developing countries and, after a century of decline in developed countries, it is now increasing in developed countries as well. The largest factor contributing to spread of TB in the US in recent years has been AIDS, because immunodeficiency greatly increases the conversion of asymptomatic to symptomatic disease. Symptomatic disease results in the spread of infection. The most frightening contribution to increased incidence is the emergence of multiple drug resistant strains of Mycobacteria. Tuberculosis is caused by members of the Mycobacterium tuberculosis complex which includes Mycobacterium tuberculosis, Mycobacterium bovis, Mycobacterium africanum, and Mycobacterium microtii. Mycobacteria are aerobic, non-sporeforming bacilli with unique staining characteristics. They are gram positive like in their structure but stain characteristically with a special stain using carbol-fuchsin. While Gram negative and positive bacteria decolorize with acid-alcohol after carbol-fuchsin staining, Mycobacteria are resistant to acidalcohol destaining and are thus referred to as “acid fast”. The name “acid fast bacilli” or “AFB” is nearly synonymous with Mycobacteria. Mycobacteria are extremely slow growing – both in vitro and in vivo. Doubling times can be from 12 to 24 hours, depending on the strain. In Mycobacteria research laboratories, this has resulted in significant limitations and slow progress. In vivo, this is a major contributing factor in increased incidence: prolonged doubling times translates to long duration drug therapy and in turn results in poor patient compliance with these medications. Decreased compliance contributes to increased disease (and hence spread) and also to increased incidence of drug resistant strains. Basic biology of Mycobacterial infection. Tuberculosis is a prototype of infections that require cellular immune response (CMI) for their control. Like diseases caused by the related species, Mycobacterium leprae, the outcome of M. tuberculosis infection is dramatically influenced by the nature of the host immune response. Key stages in the disease process are: 1. M. tuberculosis enters the lungs in aerosol droplets. It’s taken up by alveolar macrophages. Activated macrophages can kill M. tuberculosis but if the bacteria enter resting macrophages they can survive, multiply and spread to other resting macrophages. Like Salmonella, M. tuberculosis is able to prevent phagosome-lysosome fusion. 2. Initial growth in alveolar macrophages results in the formation of small necrotic lesions with a solid, caseous centers in which M tuberculosis growth is probably restricted. An effective T cell response is essential for protection. Cytotoxic T lymphocytes (CTLs) are required to release intracellular bacteria from host cells so that they can be killed by activated macrophages. Helper T cells are also required to recruit and activate additional macrophages. 3. For the majority of people infected with M. tuberculosis, bacteria are either cleared by the action of T cells before symptoms even develop, or bacteria become enclosed within a caseous lesion and remain dormant for months or even years. In this dormant state, the bacteria become surrounded by lymphocytes, macrophages, Langhan’s giant cells and fibroblasts. Langhan’s giant cells are macrophages that have surrounded the M. tuberculosis and fused to form one very large cell with many peripherally located nuclei. This organization of cells is called a “granuloma” and contributes to the formation of hard tubercles (hence the name). This is a successful tissue reaction with respect to the containment of infection, healing with eventual fibrosis, encapsulation, and scar formation. 4. In response to factors that compromise the immune system, such as malnutrition, alcoholism, drug abuse, and AIDS, reactivation can occur. The solid, caseous foci progress to liquefied capsules in which the M. tuberculosis multiply. The liquefied lesions, along with the bacteria, are discharged throughout the bronchial tree producing a tuberculous cavity. In these lesions, bacterial numbers are 5 to 6 logs higher than in noncavity lesions. Coughing leads to delivery of M. tuberculosis into the air in respiratory droplets. Treatment and Control. Vaccination: BCG (bacilli Calmette-Guerin; attenuated strain of M. bovis) has been used in many countries; its efficacy has not been conclusively proven. It is not used in the US because BCG vaccination causes conversion of the commonly used diagnostic skin test (to positive). PPD (purified protein derivative) skin test: In the US, this skin test is often the first evidence of exposure, positive skin test is followed by chest X-ray and prophylactic drug therapy that usually is prescribed for 6 months to 1 year. Multiple drug therapy: isoniazid, rifampin, pyrazinamide, and ethambutol for 6 to 12 months. Drug resistant strains: MDR (multiple drug resistant) strains have been associated with outbreaks of disease characterized by rapid progression and high mortality (up to 75%!). Genetic approaches to understanding Mycobacterial pathogenesis. Development of genetic tools: M. smegmatis (a non-pathogenic species of Mycobacteria that grows much faster and easier in the laboratory than M. tuberculosis); shuttle plasmids (to transfer DNA into and out of Mycobacteria and for manipulations in vitro and in E. coli); transformation protocols; mycobacteriophage L5; and reporter genes (xylE, phoA). Isolation of avirulent and attenuated strains: Spontaneous mutants, transposon mutants. Complementation of attenuated strains with DNA from virulent strains: (Collins et al., 1995. PNAS 92:8036-8040) Collins et al. made use of an integrating cosmid shuttle vector, pYUB178, to clone a gene that conferred virulence upon an avirulent M. bovis strain. M. bovis WAg200 is virulent in a guinea pig model system: lesions in the spleens, livers, kidneys, and lungs can be detected 12 weeks after subcutaneous injection of 1 X 106 cfu. M. bovis strain ATCC35721 is avirulent – it does not cause lesions in guinea pigs even after subcutaneous injection of >107 cfu. The hypothesis was that the lack of virulence in ATC35721 was due to the loss or inactivation of one or more virulence genes. Since these two strains are so closely related, the authors reasoned that they might be able to identify the missing or inactive gene by complementation using DNA from the virulent WAg200 strain. PYUB178 has several useful features: attP and int are from mycobaceriophage L5. L5 is similar to bacteriophage in that it inserts into a specific site in the bacterial chromosome, called attB, and insertion into this site (via homologous recombination) requires a bacteriophage encoded protein, integrase, encoded by the int gene. oriE is an origin of replication that functions in E. coli allowing for manipulation (cloning) and propagation of the plasmid in E. coli. (Since the plasmid does not contain an ori that functions in Mycobacteria it is a suicide plasmid, i.e., it must integrate into the chromosome in order to be maintained). aph encodes kanamycin resistance for selection. A cos site allows the plasmid to be packaged into and therefore very large fragments of DNA can be cloned for tranduction into E. coli. The unique BcII site can be used to clone fragments that have been digested with BamHI, BgIII, or Sau3A. Construction and characterization of a M. bovis WAg200 DNA library in pYUB178. WAg200 (virulent Mycobacteria) genomic DNA was digested with Sau3A (limited digestion to generate large DNA fragments), separated by agarose gel electrophoresis, and DNA fragments of 30-50 kb were isolated. These fragments were ligated into the BcII-digested site of PYUB178, packaged into phage heads, and transduced into E. coli. Cosmid DNA was then prepared and electroporated into M. bovis ATCC35721. Cointegrates were selected using kanamycin resistance. ~4000 Kmr M. bovis ATCC35721 cointegrates were obtained. To determine the diversity of the clones, 12 random cointegrates were analyzed by Southern blot. The probe used in the southern blots was the Sspl-Dral fragment from pYUB178 that contains the BcII cloning site. There is one PstI site between the Dral site and the int gene on the plasmid and there is another PstI site on the Mycobacterial chromosome adjacent to the attB site. If genomic DNA from cointegrate strains is digested with PstI and probed with the SspI-Dral fragment from pYUB178 either one or two DNA bands should be detected; 1) if there are no PstI sites within the DNA fragment cloned into the BcII site in pYUB178, one large DNA fragment will be detected, 2) if there is one or more PstI sites within the DNA inserted in the BcII site, two DNA fragments will be detected, each one containing one end of the inserted DNA. (If there are two PstI sites within the inserted DNA, the “internal” fragment will not be detected in this Southern blot). Southern blot analysis showed that all 12 of the randomly selected cointegrates produced a different hybridization pattern, indicating the integrated cosmids contained different DNA fragments inserted into the BcII sites. The library, therefore is diverse with respect to cloned DNA fragments from WAg200.. Selection of virulent cointegrate strains using a guinea pig model. Three guinea pigs were inoculated subcutaneously with 107 cfu of pooled cointegrates and then sacrificed 12 weeks later. Spleens, livers, kidneys, and lungs were examined for tuberculous lesions. All three guinea pigs inoculated with the pooled cointegrate strains had macroscopic lesion in their spleens while control guinea pigs (inoculated with ATCC35721) had no lesions. The Mycobacteria isolated from the spleen lesions were examined genetically: Southern blot analysis showed that 11 of 14 (80%) of the clones recovered from the lesions now produced the same pattern when digested with PstI and probed with the same probe (SspI-DraI) used before to assess the diversity of the library. This result indicates that a predominant clone was selected in vivo. Cloning the complementing locus. Because there is a NotI site between oriE and attP, and no NotI sites between that one and BcII site on pYUB178, at least part of the DNA contained on the complementing cointegrated plasmid could be recovered. DNA from the “virulent” cointegrate was digested with NotI, ligated, transformed into E. coli, and transformants were selected using kanamycin. This plasmid contains at least some of the WAg200 DNA that conferred upon ATCC35721 the ability to form lesions in guinea pigs. Since this plasmid probably does not contain all of the WAg200 DNA present in the cosmid that was integrated in ATCC35721 which conferred virulence, and may not even contain the fragment of DNA necessary for virulence, the WAg200 DNA fragment recovered from the chromosome was used to probe the original library in E. coli to search for “full length” clones. 48 of the clones in the library hybridized to the fragment. All contained a 2.3 kb MluI fragement. Confirmation that the locus confers virulence on ATCC35721. To determine if the 2.3 kb MluI fragment was sufficient to confer virulence on ATCC35721, it was cloned into pYUB178, integrated into the chromosome of ATCC35721, and the cointegrated strain was inoculated into guinea pigs. The results of this experiment showed that macroscopic lesions were detected in spleens within 8 weeks post-inoculation. DNA sequence analysis of the complementing locus. The nucleotide sequence of the 2.3 kb MluI fragment was determined and shown to have the potential to encode a sigma factor. Sigma factors are small proteins that provide specificity to RNA polymerase by functioning as highly specific DNA binding proteins. The gene was named rpoV (for virulence). Comparison of the nucleotide sequence of rpoV from WAg200 and ATCC35721 revealed a signal nucleotide difference resulting in an Arg to His substitution at position 522 of the protein’s amino acid sequence. This signal amino acid substitution apparently renders the RpoV protein in ATCC35721 non-functional – or at least insufficiently functional with respect to virulence regulated genes. The hypothesis is the RpoV sigma factor directs RNA polymerase to the promoters of virulence related genes and without RpoV, virulence genes are not expressed.