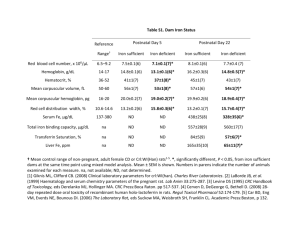
The Consequences of Iron Toxicity Tomado de www.medscape.com
advertisement

The Consequences of Iron Toxicity Tomado de www.medscape.com Unmanaged Iron Toxicity Causes Cumulative Toxicity and Progressive, Life-Threatening Organ Damage Unmanaged chronic iron overload causes progressive damage to the liver, heart, and endocrine glands, and may eventually lead to premature death.1-9 Furthermore, nonspecific early symptoms (such as abdominal discomfort and fatigue) may delay diagnosis until severe damage to heart or liver tissues produces clinically apparent symptoms.2,10 Therefore at-risk patients (such as those who have received multiple blood transfusions) should be screened for iron toxicity. Clinical Sequelae of Iron Toxicity. Transfusional iron overload can lead to life-altering conditions and premature mortality.1-9 Patients can be asymptomatic as iron is invading and accumulating in their organs.2,10 The Impact of Iron Toxicity on Survival The impact of iron toxicity on survival is significant. Severe iron overload is associated with premature death.11 Among patients with sickle cell disease (SCD), iron overload is among the most frequent findings at death. Iron overload is associated with the development of cirrhosis and cardiac disease, which are also leading findings at death in SCD.8 Iron Overload Was a Leading Finding at Death in Patients with SCD, Who Died at an Average Age of 36 Years8 *Including endocarditis. † Other than endocarditis and cor pulmonale. Above is a proportional mortality study that looked at the circumstances of death in 141 adults with sickle cell disease, who died over a 25-year period. Iron overload was a leading finding at death in patients with sickle cell disease, who died at an average age of 36 years.8 Iron Buildup in the Body There is no physiologic mechanism for removing excess iron.12 Regardless of disease state or the number of years between transfusions, once the bodys natural ability to store iron is exceeded, transfusional excess iron will build up in the body and may lead to serious health consequences.1,12 When iron is bound to transferrin, ferritin, or other iron transport and storage proteins, it cannot participate in oxidative reactions, and therefore cannot cause cellular damage.13 In iron overloaded patients, the capacity of these proteins to neutralize the damaging effects of iron is exceeded. Excess iron binds weakly to various other low-molecularweight proteins in the plasma and cells, and in this form propagates cellular damage by peroxidation of organelles such as mitochondria and lysosomes.13,14 Download the Iron Overload Brochure and have an important resource on the clinical consequences of iron toxicity. Cardiac Complications Cardiac iron accumulation usually occurs after organs such as the liver and spleen have become saturated with iron. Cardiac function may not change significantly until iron levels reach a critical value or duration, after which systolic function rapidly deteriorates and refractory heart failure occurs.14,15 Once cardiac dysfunction is detected, the prognosis is poor without intervention, but can be improved if appropriate therapy is given to address the iron overload.7,16 Iron overload cardiomyopathy is an old disease that has become increasingly common.14 Currently, it is thought that iron overload cardiomyopathy is caused by the direct effect of non–transferrin-bound iron (NTBI) on myocytes, rather than by interstitial iron infiltration.14 NTBI is toxic to cardiac myocytes in extremely low concentrations.14 Diastolic dysfunction is a result of myocardial damage due to iron overload.14 Conduction defects are also linked to excess iron deposition in the bundle of His and the Purkinje system.17,18 The incidence of cardiac disease for those with transfusion-dependent anemias is of great concern. The most useful noninvasive diagnostic techniques for hemosiderotic cardiomyopathy are left ventricular ejection fraction (LVEF) studies performed with radionuclide ventriculography (in adults) or echocardiography (in children). The lower the myocardial MRI T2* value, the higher the risk of cardiac dysfunction; T2* values <20 ms are associated with a progressive and significant decline in LVEF.19 It was once thought that liver and cardiac iron levels were directly correlated;20 however, their relationship has proven to be more complex. The mechanisms of iron uptake and clearance differ in heart and liver tissue, resulting in differing iron transport kinetics. Iron transport is not well understood.21 Patients may develop cardiac dysfunction despite low liver iron levels. Some data suggest a critical liver iron concentration (LIC) above which high myocardial iron levels are present.20 In one longitudinal study of patients with β-thalassemia receiving chelation therapy, an LIC >15 mg/g dry weight was shown to be suggestive of increased risk of cardiac disease and early death.20 Similarly, the maintenance of serum ferritin levels below 2500 mcg/L has been associated with improved cardiac disease-free survival.7 As a marker of iron toxicity, serum ferritin levels can predict the chances that at-risk patients will develop cardiac disease. Persistently High Serum Ferritin Levels Substantially Increased the Risk of Cardiac Disease in Patients with β-Thalassemia7 This clinical study tracked cardiac disease-free survival in patients with thalassemia over a period of 15 years, using serum ferritin as an indicator of iron burden.7 Cardiac disease-free survival was achieved in only 18% of patients with high iron burden over this time period. However, cardiac disease-free survival in the patient group that adequately controlled serum ferritin levels was 91% during the 15-year follow-up. Hepatic Complications The liver is the major site of iron storage, and as such it is susceptible to damage from iron overload. At the cellular level, mitochondria swell and their membranes rupture, resulting in cell death.22 Two main clinical sequelae of excess iron deposition in the liver are fibrosis/cirrhosis and hepatocellular carcinoma.23 In patients receiving regular transfusions, serious liver damage can occur within 2 years of the first transfusion,23 and liver cirrhosis can develop if the excess iron is not removed. Studies have shown a correlation between the development of liver fibrosis and high liver iron24 and serum ferritin20 levels. The study evaluating liver iron found that the fibrosis score was higher in patients with greater baseline liver iron levels, as well as in those patients who were hepatitis C positive. Hepatic iron burden can be assessed noninvasively through regular monitoring of serum ferritin levels. Cirrhosis is more prevalent in those with serum ferritin >1000 mcg/L than in those below this level.25 Damage to Other Major Organs Skeletomuscular Damage Osteoporosis is common among patients with thalassemia26 Other troubling musculoskeletal problems include severe muscle cramps and disabling myalgia. Muscle biopsy often reveals iron deposits in the myocytes27 Compromised Immune Function Patients with iron overload appear to have increased susceptibility to infections, often with unusual microorganisms28-30 This apparent immune compromise may result from the abnormally high transferrin saturations seen in patients with iron overload Transferrin has been shown in vitro to have bacteriostatic properties31; high saturations may compromise this property Skin Pigmentation Cutaneous iron deposition induces melanin production, causing a characteristic bronze pigmentation in fair-skinned people Exposure to ultraviolet light acts synergistically with this process, and as a result many people with iron toxicity tan very easily, although these effects are variable Fair-skinned people seldom develop hyperpigmentation even with a large iron burden, while people of moderate baseline pigmentation often develop a striking almond-colored hue For more information on the relationship between iron toxicity and damage to organs and glands, visit irontoxicity.com/hcp/consequences.jsp 1. Porter J. Pathophysiology of iron overload. Hematol Oncol Clin North Am. 2005;19(suppl 1):7-12. 2. Cabantchik ZI, Breuer W, Zanninelli G, Cianciulli P. LPI-labile plasma iron in iron overload. Best Pract Res Clin Haematol. 2005;18:277-287. 3. Kushner JP, Porter JP, Olivieri NF. Secondary iron overload. Hematology (Am Soc Hematol Educ Program). 2001:47-61. 4. Gabutti V, Piga A. Results of long-term iron-chelating therapy. Acta Haematol. 1996;95:26-36. 5. Telfer PT, Prestcott E, Holden S, Walker M, Hoffbrand AV, Wonke B. Hepatic iron concentration combined with long-term monitoring of serum ferritin to predict complications of iron overload in thalassaemia major. Br J Haematol. 2000;110:971-977. 6. Schafer AI, Cheron RG, Dluhy R, et al. Clinical consequences of acquired transfusional iron overload in adults. N Engl J Med. 1981;304:319-324. 7. Olivieri NF, Nathan DG, MacMillan JH, et al. Survival in medically-treated patients with homozygous β-thalassemia. N Engl J Med. 1994;331:574-578. 8. Darbari DS, Kple-Faget P, Kwagyan J, Rana S, Gordeuk VR, Castro O. Circumstances of death in adult sickle cell disease patients. Am J Hematol. 2006;81:858-863. 9. Leitch HA, Goodman TA, Wong KK, Vickars LM, Galbraith PF, Leger CS. Improved survival in patients with myelodysplastic syndrome (MDS) receiving iron chelation therapy [abstract]. Blood (ASH Annual Meeting Abstracts). 2006;108:Abstract 249. 10. Abetz L, Baladi J-F, Jones P, Rofail D. The impact of iron overload and its treatment on quality of life: results from a literature review. Health Qual Life Outcomes. 2006;4:73. 11. Karnon J, Zeuner D, Brown J, Ades AE, Wonke B, Modell B. Lifetime treatment costs of beta-thalassaemia major. Clin Lab Haematol. 1999;21:377385. 12. Andrews NC. Disorders of iron metabolism. N Engl J Med. 1999;341:19861995. 13. Wang WC, Ahmed N, Hanna M. Non-transferrin-bound iron in long-term transfusion in children with congenital anemias. J Pediatr. 1986;108:552-557. 14. Liu P, Olivieri N. Iron overload cardiomyopathies: new insights into an old disease. Cardiovasc Drugs Ther. 1994;8:101-110. 15. Jaeger M, Aul C, Sohngen D, et al. Secondary hemochromatosis in polytransfused patients with myelodysplastic syndromes. Beitr Infusionsther. 1992;30:464-468. 16. Brittenham GM, Griffith PM, Nienhuis AW, et al. Efficacy of deferoxamine in preventing complications of iron overload in patients with thalassemia major. N Engl J Med. 1994;331:567-573. 17. Buja LM, Roberts WC. Iron in the heart. Etiology and clinical significance. Am J Med. 1971;51:209-221. 18. Schwartz KA, Li Z, Schwartz DE, et al. Earliest cardiac toxicity induced by iron overload selectively inhibits electrical conduction. J Appl Physiol. 2002;93(2):746-751. 19. Anderson LJ, Holden S, Davis B, et al. Cardiovascular T2-star (T2*) magnetic resonance for the early diagnosis of myocardial iron overload. Eur Heart J. 2001;22:2171-2179. 20. Berdoukas V, Bohane T, Tobias V, et al. Liver iron concentration and fibrosis in a cohort of transfusion-dependent patients on long-term desferrioxamine therapy. Hematol J. 2005;5:572-578. 21. Oudit GY, Trivieri MG, Khaper N, Liu PP, Backx PH. Role of L-type Ca2+ channels in iron transport and iron-overload cardiomyopathy. J Mol Med. 2006;84:349-364. 22. Thakerngpol K, Fucharoen S, Boonyaphipat P, et al. Liver injury due to iron overload in thalassemia: histopathologic and ultrastructural studies. Biometals. 1996;9:177-183. 23. Conte D, Piperno A, Mandelli C, et al. Clinical, biochemical and histological features of primary haemochromatosis: a report of 67 cases. Liver. 1986;6:310315. 24. Tsukamoto H, Horne W, Kamimura S, et al. Experimental liver cirrhosis induced by alcohol and iron. J Clin Invest. 1995;96:620-630. 25. Morrison ED, Brandhagen DJ, Phatak PD, et al. Serum ferritin level predicts advanced hepatic fibrosis among U.S. patients with phenotypic hemochromatosis. Ann Intern Med. 2003;138:627-633. 26. Christenson RA, Pootrakul P, Burnell JM, et al. Patients with thalassemia develop osteoporosis, osteomalacia, and hypoparathyroidism, all of which are corrected by transfusion. Birth Defects Orig Artic Ser. 1987;23(5A):409-416. 27. Vallat JM, Loubet R, Leboutet MJ, et al. Hemosiderin deposition in muscle. Report of three cases. Acta Neuropathol (Berl). 1978;42:153-156. 28. Abbott M, Galloway A, Cunningham JL. Haemochromatosis presenting with a double Yersinia infection. J Infect. 1986;13:143-145. 29. Brennan RO, Crain BJ, Proctor AM, et al. Cunninghamella: a newly recognized cause of rhinocerebral mucormycosis. Am J Clin Pathol. 1983;80:98-102. 30. Bullen JJ, Spalding PB, Ward CG, et al. Hemochromatosis, iron and septicemia caused by Vibrio vulnificus. Arch Intern Med. 1991;151:1606-1609. 31. Reiter B, Brock JH, Steel ED. Inhibition of Escherichia coli by bovine colostrum and post-colostral milk. II. The bacteriostatic effect of lactoferrin on a serum susceptible and serum resistant strain of E. coli. Immunology. 1975;28:83-95.