Patient Held Record
advertisement

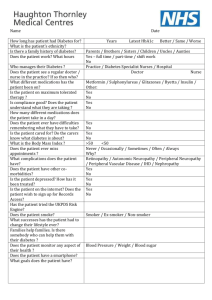
Patient Held Record Diabetes Patient Name Diabetes Health Record This record will help you receive the best care for your diabetes, provide vital information if you are taken ill and provide you with information about your diabetes. Please complete all the relevant details on this record filling it in as and when you meet with Health Care Professionals. You should bring it with you to all your appointments and ask the person that you see to fill it in also. You can use the section at the back to make your own notes. This Record includes: 1. Patient Held Records – a rationale 2. Personal details & telephone contact numbers 3. Medical details: diabetes history and other past medical history 4. Explanatory notes & glossary of terms 5. Medication charts; diabetes medications and others 6. When you are unwell: treatment of emergencies & illness 7. Checklist for education 8. Personal care plans / targets 9. Diabetes Review Record (check-ups) 10. Personal notes 11. What to expect 1. Patient Held Records – a rationale Standard 3 of the Diabetes National Service Framework (DNSF) 2001 (to view this document see Resources on the right hand side of this page), states that all individuals with Diabetes should receive a service supporting successful self-management of Diabetes, encouraging a partnership in decision making to achieve end goals. There should be an agreed, shared, plan of care. There is widespread recognition that people with Diabetes should be involved with their care. It is the patient and their families that experience the consequences of both disease and treatment. Recognising this highlights the need for education and care that not only provides expertise but also embraces psychosocial challenges. Self-management programmes and education programmes such as DAFNE (link to DAFNE http://www.diabetes.org.uk/good_practice/education/examples/education1.htm http://www.dafne.uk.com/) and the Expert Patient Programme (link to expert patient http://www.dh.gov.uk/AboutUs/MinistersAndDepartmentLeaders/ChiefMedicalOfficer/Whats New/CMOAtLarge/CMOPastVisits/fs/en?CONTENT_ID=4102506&chk=QkH8rQ) have in the last few years fuelled the belief that considerable benefits can be gained from empowering the individual with Diabetes to make key decisions about their care. The DNSF delivery strategy 2002 refers to the concept of individuals carrying with them a personal record of care that includes treatment regimens and test results as a step on from the pilot projects under way to meet the NHS Plan commitment that people receive copies of clinical correspondence. Up to date records will facilitate continuity of care between the individual themselves and the numerous and varied Health Care Professionals with whom they come into contact. There is a subtle difference between a Patient Held Records and Care Plan; the former being a systematic means of capturing ongoing information about a persons treatment needs and the latter a mutually agreed process with goals for improving an individuals diabetes and in turn well being. The DNSF Delivery Strategy links the two, believing the ideal personal diabetes record should include An agreed care plan Setting management plans between reviews to foster understanding and ownership of the set goals Identification of health, social and education needs, who is responsible for them and how they will be met Identity of a named contact Diabetes UK has been asked to provide templates for Patient Held Records (to visit see Resources on the right hand side of this page. It is felt that whilst there are general principles that should always be applied and included, individual areas should adapt these to take account of their local needs. 2. Personal details & telephone contact numbers Name Address Phone Number Home: Work: Mobile: Date of Birth NHS Number Ethnic Origin Religion Interpreter Phone Language Spoken Emergency Contact Name Relationship to you GP Name GP Surgery GP Phone: (day) (out of hours) Community Pharmacist Phone Diabetes Nurse Name Phone Chiropodist Name Phone Dietician Name Phone Hospital Diabetes Specialist Phone Hospital Number Phone 3. Medical details: diabetes history & other past medical history Type of Diabetes Date of Diagnosis Weight at Diagnosis HbA1c at Diagnosis Symptoms at diagnosis Family History: include diabetes, blood pressure, heart disease, stroke or high cholesterol and who it affected if known Initial Treatment Your Past Medical History - Note especially any high blood pressure, high cholesterol levels, angina, heart attack or heart surgery, and stroke or similar event: 4. Explanatory Notes & Glossary of Terms This is your Personal Diabetes Health Record; it is your record of important information about your diabetes care. Taking this record and the information collected in it to all appointments will help to improve communication between yourself and the healthcare professionals looking after you. Please take your record with you to all appointments including: Your GP The hospital diabetes clinic The eye clinic Your optician The diabetes nurse The dietician Your chiropodist/podiatrist The hospital accident and emergency department; ask someone to bring it in for you if you have to be admitted to hospital » The District Nurse To the Health Care Professional in completing this record please: Be concise Discuss the entry to be made with the individual before completing Date and sign every entry Entries only to be made in black ink Make your entries legible (many people will be using the information contained here) Telephone Help Lines In addition to your local GP, Practice Nurse and Diabetes Specialist Nurse the following Numbers may be helpful to you: NHS Direct 0845 4647 Diabetes UK Careline 020 7424 1030 (Lines are open Monday to Friday 9am-5pm) Novo Nordisk 0845 6005055 1730-2300 mon-fri and 0830-2300 weekends and bank holidays Sanofi Aventis 0845 606 6887 24hours a day 7 Days Lilly Customer care 01256 315999 Your insulin manufacturer may have a helpline service; ask your Health Care Professional about it and fill the details in below: Insulin Company Helpline Blood Glucose Monitor; the manufacturer of your blood glucose monitor may offer after care services. Ask your health care professional about it and fill in the details below Manufacturer Care Services Glossary of Terms and Tests Blood glucose/sugar level - the amount of glucose (sugar) in the blood. Blood pressure (BP) - the pressure level within the arteries, which indicates how hard the heart is working to pump the blood round the body. Body mass index (BMI) - a measure of how overweight or underweight you are. It is calculated by Weight (kg) divided by Height (m2). A BMI of 20-25 is considered normal, 2530 overweight and over 30 is very overweight. If overweight, loosing weight will help you control your diabetes (benefits include improved blood glucose levels, a lowered blood pressure, lower cholesterol and other fat levels, reduced risk of stroke and heart attack, improves energy levels and well-being). Waist circumference measurement Waist Size Categorisation Sex Healthy Increased risk High risk Male 69 – 94 cm 94 – 101 cm More than 27 – 37 in 37 – 39 in 101 cm 40 in 61 – 80 cm 80 – 87 cm More than 24 – 32 in 32 – 34 in 87 cm 35 in Female This measurement is preferable to BMI. Cataracts - cloudiness and thickening of the lens of the eye. Cholesterol - a type of fat in the blood. Too much cholesterol in the blood may increase your risk of developing heart disease. (see Resources on the right side of this page for) Foot pulses and sensation - checks made on the blood supply and amount of feeling in the feet. HbA1 (or HbA1c ) - a blood test which indicates the average level of your blood glucose during the past three months. Known also as Glycated Haemoglobin. The result is written as a percentage with the average target being 7% (see Resources for). HDL - high density lipoprotein, often referred to as good cholesterol, it carries cholesterol away from the arteries. High levels of these can protect people from heart disease and stroke. Hyperglycaemia - high blood glucose level. Hypoglycaemia - low blood glucose level. Normal blood glucose/sugar level is between 4 – 7 mmol/l Hyperlipidemia - another name for high cholesterol or triglyceride levels. LDL - low density lipoproteins, known as bad cholesterol, too much LDL in the blood can cause it to collect on the artery lining, leading to narrowing and hardening. Microalbuminuria - a test for very tiny amounts of protein in the urine. Protein - urine is checked for the presence of protein with test strips to test for damage to the kidneys. Protein can also be found when there is an infection in the urine. Retinopathy - damage to the back of the eye (retina). Triglyceride (TG) - a type of fat in the blood. Urea and Creatinine - blood tests to check for kidney damage. Visual acuity - an eye test which involves reading a letter chart. ACR – this is a special measurement of urine which checks for kidney damage. 5. Medication charts; diabetes medications and others Your Allergies Name of Diabetes Medication Date Prescribed Strength Amount (how much and at what time of day) What is it for? Insulin Delivery Device Needles Used Type of Glucose Monitoring Monitoring Device Used: Strips Used Lancets Used Finger Pricker Used Blood Urine Date & Reason Treatment Stopped Names of other Medications Date Prescribed Strength How often do you What is it for take it 6. When you are unwell: treatment of emergencies & illness Hypoglycaemia (‘hypo’) occurs when the blood glucose level is too low (below 4 mmol/l)(see Resources on the right hand side of this page for patient information leaflets on Hypoglycaemia). This should not affect you if you manage your diabetes with diet alone. There can be a number of causes: A meal or snack is missed Too much insulin has been taken Unexpected / excessive activity or exercise Alcohol Hot weather It can come on suddenly and in a person who is not unwell. Symptoms vary for each individual but may include; sweating, shaking, irritability, confusion, feeling faint. Stop what you are doing and take sugar or a sugary drink immediately e.g. glucose tablets, lucozade or other non-diet drink. Follow that short acting carbohydrate with some longer acting carbohydrate e.g. sandwich, milk and 2 rich tea biscuits or your next meal if due. Hypergylcaemia- high blood glucose levels (above 7 mmol/l). Coma can occur at high levels (higher than 15mmol/l) although this is rare. Hyperglycaemia can build up gradually over days or even weeks but can also become a serious problem more quickly in some. Monitor blood glucose levels frequently; every two to four hours. Ask someone to help if you are unable to so yourself. It is important NOT to stop taking your tablets or insulin; when unwell our bodies react by raising blood glucose levels worsening diabetes control. Drink plenty of unsweetened fluids. If you cannot eat, try to take in some carbohydrate consider soups, milk drinks, ice cream, ordinary squash, try small amounts little and often. Check for ketones in your urine or blood 7. Checklist for Education Sessions Below is a list of topics that you may need to know about. Some are very important; the nurse or doctor should discuss them with you regularly. Some may not be relevant to you. If you are unsure, please ask. Topic What is diabetes? Diet Tablets Physical Activity Insulin & injection technique Hypoglycaemia Hyperglycaemia Illness Blood testing Urine testing Foot care Importance of eye checks Smoking Alcohol Complications of Diabetes Driving/insurance Travel Sexual health Planning pregnancy Diabetes UK Free prescriptions Dates Discussed 8. Personal Care Targets and Care Plans This is a plan agreed between you the person with diabetes and the Health Care Professional giving dietary, physical activity, weight and self-management targets, including suggested frequency of check-ups etc. Dietary Goals Comments (with dates) Physical Activity Goals Comments (with dates) Care Plans Date Problem / Target Actions / to do Evaluation 9. Diabetes Review Record (check-ups) Date 3 - monthly Review control Weight / BMI / waist circumference Blood pressure Lying or sitting Standing Foot examination General condition Pulses Sensation Urine tests Glucose Protein Microalbuminuria Blood tests Glucose level HbA1c Total cholesterol HDL LDL Triglyceride Eye examination Fundoscopy Visual acuity Retinal photograph 6 - monthly 9 - monthly Annual Date of next visit 10. Personal Notes and Queries Use this section to note anything about your diabetes that you would like to discuss. 11. What Diabetes Care to Expect Research has shown that people with diabetes get fewer complications, and may live longer, if they have regular check-ups, even if they do not feel ill in any way. You should agree with your doctor how often these checks should be, but at the very least, you should make sure someone examines the back of your eyes once a year. For more details, see the leaflet, ‘What diabetes care to expect’ available free from Diabetes UK. To order this leaflet call freephone 0800 585 088. This Patient Held Record is adapted from Diabetes UK