THE HEMOLYTIC DISORDFRS:
advertisement

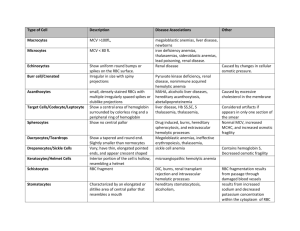
THE HEMOLYTIC DISORDFRS: GENERAL CONSIDERATIONS Hemolytic anemias are anemias that result from an increased rate of red cell destruction. The term hemolytic anemia, or better still hemolytic disorders, is limited to those conditions in which the rate of red cell destruction is accelerated and the ability of the bone marrow to respond to the stimulus of anemia is unimpaired. Under maximal stimulation, the normal marrow is capable of undergoing hyperplasia until its production rate is increased about six-to eight-fold. With optimal marrow compensation, it is theoretically possible for the survival of red cells in the circulation to decrease from the normal 120 days to as little as 15 to 20 days without anemia developing. Such an increase in both destruction and production of erythrocytes can produce a compensated hemolytic state without anemia being present usually known as compensated hemolytic disease. On the other hand, when red cell survival becomes so short that anemia develops in spite of a vigorous erythropoietic response, the term hemolytic anemia is appropriate. Classification 1. Clinical forms----acute and chronic 2. Site of hemolysis---intravascular and extravascular 3. Pathogenetic classification---inherited and acquired Since the intravascular hemolytic disorders are accompanied by unique manifestations, such as hemoglobinemia, hemoglobinuria, and hemosiderinuzia, the classification is easily made and often serves to limit the diagnostic possibilities. Hemolytic anemias characterized by predominantly intravascular red cell destruction: 1. Paroxysmal nocturnal hemoglobinuria 2. Disorders associated with erythrocyte fragmentation 3. Certain immunohemolytic anemias a. Transfusion reactions resulting from ABO isoantibodies b. paroxysmal cold hemoglobinuria c. Some instances of idiopathic autoimmune hemolytic anemia 4. Those associated with certain infections. Black water fever in faloiparum malaria. 5. Those caused by certain chemical agents a. Introvenous administration of distilled water b. Snake and spider venoms c. Arsine poisoning d. Acute drug reactions in association with glucose-6-phosphate dehydrogenase deficiency 6. Thermal injury. Since most hemolytic diseases are characterized by extravascular red cell destruction, detection of this mode of hemolysis still leaves one with a large number of diagnostic possibilities, Hemolytic disorders also may be divided into inherited and acquired varieties. Excessive destruction of erythrocytes may occur either because of an intrinsic defect in the cell itself or because of the action of extrinsic agents on normally constructed cells. As a general rule, the intrinsic defects are inherited and the extrinsic ones are acquired. Hemolytic Disorders I. Inherited hemolytic disorders . A. Defects in the erythrocyte membrane B. Deficiency of erythrocyte glycolytic enzymes C. Defects in globin structure and synthesis II. Acquired hemolytic anemias A. Immunohemolytic anemias 1. Transfusion of incompatible blood 2. Hemolytic disease of the newborn 3. Autoimmune hemolytic anemia due to warm-reactive antibodies a. ldiopathic b. "Secondary" (1). Virus and mycoplasma infections (2). Lymphosarcoma, chronic lymphocytic leukemia (3). Other malignant diseases (4). Immune-deficiency states (5). Systemic lupus erythematosus and other “autoimmune” disorders C. Drug-induced B. Traumatic and microangiopathic hemolytic anemias 1. Prosthetic valves and other cardiac abnormalities 2. Hemolytic-uremic syndrome 3. Thrombotic thrombocytopenic purpura 4. Disseminated intravascular coagulation 5. Associated with immunologic phenomena (graft rejection, immune complex disease, etc.) C. Chemical, physical and biologic factors 1. drugs and chemicals----Aniline, Sulfonamides, Copper 2. Burns 3. infectious agents----malaria, toxoplasmosis 4. biologic toxin----Venoms D. Hypersplenism Pathogenesis: The increased rate of red cell destruction may happen at intravascular or extravascular spaces. Extravascular hemolysis is the red cell destruction within the macrophage cell at spleen and liver. Intravascular hemolysis happens at the site within the circulation and the hemoglobin is released to the plasma directly. Extravascular hemolysis: 1. The spleen is capable of tapping and destroying and removing abnormal red blood cells which have IgG or complement at the cell membrane. 2. The abnormality of cell membrane, or the existence of Heinz body within the red cell will decrease the physical deformation of the red cell. Those red cells can not pass through the microcirculation of the spleen, and will be destroyed by the macrophage cell. Intravascular hemolysis: 1.During the red cells are destroyed, hemoglobin is released into the plasma, and combined with heptoglobin become a large molecular substance, which can not filter through the kidney. The level of plasma heptoglobin is then increased during intravascular hemolysis. 2.The hemoglobin is capable to degradation and produce heme. Heme can combine with hemopexin, so plasma hemopexin is decreased during massive hemolysis. 3.lf the hemoglobin is exhausted during hemolysis, the free hemoglobin (M.W.66000) can pass through the kidney (Hemoglobinuria). The iron of the hemoglobin(Ferritin and hemosiderin) are deposited at the epithelial cell of renal tubule. The epithelial cell can excrete it in urine. and it is called hemosideinuria what the Rous test is positive. Extravascular hemolysis ↓ Mono-macrophage system ↓ Biliverdin ↓ Bilirubin ↓ (Liver) ↓ (intestine) ↓ Urobilinogen (stool) ↓(plasma) (kidney) ↓ (plasma) ↓ Urine ↓ Urobilinogen Intravascular hemolysis Plasma free hemoglobin Heptoglobin-hemoglobin (heptoglobin↓) Hemopexin-heme (hemopexin ↓) Methemoalbumin (kidney) (Urine) hemosiderin (Rous test +) methemoglobin hemoglobin (occult blood +) Clinical Manifestations The clinical manifestations of hemolytic anemia depend upon the red cell destroy speed, degree and site. Acute hemolysis Chronic hemolysis (intravascular) (extravascular) Onset quickly slowly Fever high low or no Aching back renal area no Splenmegaly no yes Jaundice slight frequent Hemoglobinuria + Hemosiderinuria +(chronic) Renal failure + Gallstone + Laboratory Manifestation is and Diagnosis: Laboratory findings in hemolytic anemia can be divided into three groups: (1).those related to the increase in erythrocyte destruction. (2).those related to the compensatory increase in the rate of erythropoiesis, and (3).those found only in particular varieties of hemolytic anemia and therefore useful in differential diagnosis. The diagnosis of hemolytic anemia can be divided into two steps: 1 .Is it a case of hemolytic anemia? 2.What kind of hemolytic anemia is it? Is it a case of hemolytic anemia ? 1.Laboratory findings of accelerated red cell destruction (1).Erythrocyte survival----erythrocyte life span is decreased (2).Catabolism of heme is increased----bilirubin production rate is increased. Serum unconjugated bilirubin and urobilinogen excretion rates are increased (3).Serum lactate dehydrogonase activity is increased. (4).Signs of intravascular hemolysis ----hemoglobinemia ----absence of heptoglobin ----hemoglobinuria ----hemosiderinuria ----methemalbuminemia ----reduced serum hemopexin 2.Laboratory findings of accelerated erythropoiesis (1).Blood ----reticulocytosis ----sometimes leukocytosis and thrombocytosis, but when crises of hemolysis is happened, both leukocyte and platelet will decrease. (2).Bone marrow----erythroid hyperplasia (3).Ferrokinetic ----increase plasma iron turnover ----increase erythrocyte iron turnover What kind of hemolytic anemia is it? (l).Those with coombs positive hemolytic anemia----AIHA, Idiopathic Secondary---SLE, lymph proliferative disorders (2).Those with coombs negative and specific morphologic abnormalities red cell ----spherocyte (spherocytosis) ----elliptocyte (elliptocytosis) ----Target cell (thalassemia) ----helmet cell (machanical hemolysis) ----sickle cell (after specific test)----(sickle cell anemia) (3).Those with non-specific morphologic abnormalities and a negative reaction to coombs test ----Ham’s test, sucrose test (PNH) ----Isopropanol test or heat denaturation test (unstable hemoglobin disease) ---Methemoglobin deoxidation test, ascorbate ZHONGLu