A 21-year-old woman presenting with rapid mental status change
advertisement

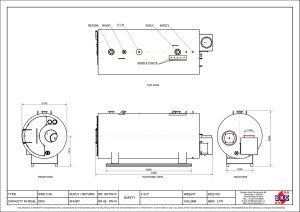
A 21-year-old woman presenting with rapid mental status change leading to coma. MRI, sagittal T1-weighted image, showing hyperintense thrombus within the posterior half of the superior sagittal sinus (SSS) (arrows) and straight sinus (arrowheads). MRV, sagittal reconstruction, confirming the obliteration of the SSS and the partial occlusion of the straight sinus. Note the presence of engorged parasagittal veins trying to act as collateral pathways for the occluded SSS (arrowheads). MRI, coronal T1-weighted image post gadolinium administration. The thrombus is seen as an intraluminal defect within the sinus. Note again engorged parasagittal venous channels serving as collateral pathways (arrowheads). DSA, selective SSS venogram, lateral projection, obtained during endovascular therapy. The tip of the catheter has been advanced proximally to the thrombosed segment. The venogram documents the patent portion of the sinus, with drainage essentially directed towards the pterygoid plexus via the sphenoparietal sinus (arrowhead). The parasagittal collateral veins are seen as well. The flattening of the posterior aspect of both eyes (arrowheads) associated with papilledema from increased intracranial pressure with pseudotumor cerebri. Note, increased subarachnoid space surrounding the orbital portions of both optic nerves. Table. Shunting Study (Author, Year) (McGirt, Woodworth et al. 2004) N 42 Shunt Type 79LP+ 36 VP Headache Papilledema Vision Relief Resolution Improvement 40 (95) NA NA VP Shunts Complications* FU (Mo) VP Shunt16(44) Overdrainage 3(8) 24 Distal catheter migration 1(3) LP Shunt Overdrainage 13(16) Distal catheter migration 4(5) Infection 3(4) Back Pain 4(5) (Abubaker, Ali et al. 2011) 25 10 VP +15 LP LP 11/13 (85) VP 9/10 (90) 6/7 LP Shunt VP Shunt 60% Visual Acuity Improved LP Shunt 30% 6/6(100%) Visual Field Improved 48 10/10(100%) VP Shunt Acuity Improvement 4/4(100%) Visual Field Improvement 4/4(100%) (Tulipan, Lavin et al. 1998) 7 VP only 6/7 (89) 5/7 complete resolution NA 0 (0) LP Shunt LP Shunt 2/7 resolving (Tarnaris, Toma et al. 2011) 29 29 Primary shunts Shunts 25 LP + 5VP (Primary shunts) LP VA 17/25 (71) Improve 10(42) VP 3/5(60) No Change/ Worst Complications 6(24) Revision 10(40) 14(58) VP Shunt VP Shunt 9 Improve 2(40) Complications 1(11) No Change/ Worst Revision 2(22) 3(60) (Bynke, Zemack et al. 2004) 17 VP Only 16/16 VA improved (100) Improved 3 eyes, Unchanged 26 eyes Non-significant changes 5eyes. Proximal Malpositioning 1(6) Distal Malfunction 6(35) Infection 2(17) Visual fields Normal 11 eyes, Improved 11 eyes Unchanged 12 eyes. (Rosenberg, Corbett et al. 1993) 37 (Johnston, Besser et al. 36 73 LP +9 Ventricular Shunt Failure LP (11%) VP (14%) 32/32 37 /37 (100) LP Shunt 78 1988) (100%) eyes Obstruction 18(49) Infection 4(11) Overdrainage11 (29) Sciatica 1(3) VP Shunt Obstruction 4(80) Over-drainage 1(20)