Case Study- Fetal demise

Case Study: Stillbirth risk factors lead to fetal demise
Background:
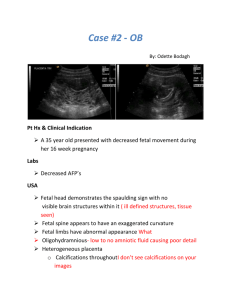
T.T. (primigravida, 39weeks) was admitted to XX Hospital on xx/20/xxxx with complaints of spontaneous ruptures of membranes. Ultrasound technicians noted no fetal heart tones, but the patient’s family insisted that the baby continued to move and kick. A Caesarean section was performed on the same day. A full term, fetal demise female child with Apgar 0, 0 was delivered via a total breech extraction.
Action:
Trivent’s gynecologist organized a medical chronology and medical opinion by reviewing T.T.’s medical records, focusing on why there was a delay in planning the C-section. Our physicians noted that there was a deviation from the standard of care that led to fetal demise. Since the patient had multiple risk factors that could have contributed to a stillbirth, intervention should have occurred earlier.
Conclusion:
The most common risk factors associated with stillbirth are: non-Hispanic black race, nulli-parity
(no previous births), advanced maternal age, and obesity.
Hypertension and diabetes, both risk factors for stillbirth , are two of the most common medical conditions that occur along with pregnancy.
Failure to do a timely intervention was a deviation in the standard of care, as this could have prevented the fetal demise. Failure to attempt vaginal delivery after the fetal demise was also a deviation in the standard of care.