ch 19 introduction
advertisement

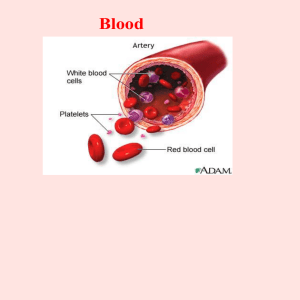
Introduction 1. The cardiovascular system consists of the blood, heart, and blood vessels. 2. Blood is a liquid connective tissue that consists of cells and cell fragments surrounded by a liquid extracellular matrix (blood plasma). 19.1 Functions and Properties of Blood 1. Blood transports oxygen, carbon dioxide, nutrients, wastes, and hormones. 2. It helps regulate pH, body temperature, and water content of cells. 3. It provides protection through clotting and by combating toxins and microbes through certain phagocytic white blood cells or specialized blood plasma proteins. 4. Physical characteristics of blood include a viscosity greater than that of water; a temperature of 38°C (100.4°F); and a pH of 7.35–7.45. 5. Blood constitutes about 8% of body weight, and its volume is 4–6 liters in adults. 6. Blood is about 55% blood plasma and 45% formed elements. 7. The hematocrit is the percentage of total blood volume occupied by red blood cells. 8. Blood plasma consists of 91.5% water and 8.5% solutes. Principal solutes include proteins (albumins, globulins, fibrinogen), nutrients, vitamins, hormones, respiratory gases, electrolytes, and waste products. 9. The formed elements in blood include red blood cells (erythrocytes), white blood cells (leukocytes), and platelets. 19.2 Formation of Blood Cells 1. Hemopoiesis is the formation of blood cells from hemopoietic stem cells in red bone marrow. 2. Myeloid stem cells form RBCs, platelets, granulocytes, and monocytes. Lymphoid stem cells give rise to lymphocytes. 3. Several hemopoietic growth factors stimulate differentiation and proliferation of the various blood cells. 19.3 Red Blood Cells 1. Mature RBCs are biconcave discs that lack nuclei and contain hemoglobin. 2. The function of the hemoglobin in red blood cells is to transport oxygen and some carbon dioxide. 3. RBCs live about 120 days. A healthy male has about 5.4 million RBCs/μL of blood; a healthy female has about 4.8 million/μL. 4. After phagocytosis of aged RBCs by macrophages, hemoglobin is recycled. 5. RBC formation, called erythropoiesis, occurs in adult red bone marrow of certain bones. It is stimulated by hypoxia, which stimulates the release of erythropoietin by the kidneys. 6. A reticulocyte count is a diagnostic test that indicates the rate of erythropoiesis. 19.4 White Blood Cells 1. WBCs are nucleated cells. The two principal types are granulocytes (neutrophils, eosinophils, and basophils) and agranulocytes (lymphocytes and monocytes). 2. The general function of WBCs is to combat inflammation and infection. Neutrophils and macrophages (which develop from monocytes) do so through phagocytosis. 3. Eosinophils combat the effects of histamine in allergic reactions, phagocytize antigen–antibody complexes, and combat parasitic worms. Basophils liberate heparin, histamine, and serotonin in allergic reactions that intensify the inflammatory response. 4. B lymphocytes, in response to the presence of foreign substances called antigens, differentiate into plasma cells that produce antibodies. Antibodies attach to the antigens and render them harmless. This antigen–antibody response combats infection and provides immunity. T lymphocytes destroy foreign invaders directly. Natural killer cells attack infectious microbes and tumor cells. 5. Except for lymphocytes, which may live for years, WBCs usually live for only a few hours or a few days. Normal blood contains 5000–10,000 WBCs/μL. 19.5 Platelets 1. Platelets (thrombocytes) are disc‐shaped cell fragments that splinter from megakaryocytes. Normal blood contains 150,000–400,000 platelets/μL. 2. Platelets help stop blood loss from damaged blood vessels by forming a platelet plug. 19.6 Stem Cell Transplants from Bone Marrow and Cord Blood 1. Bone marrow transplants involve removal of red bone marrow as a source of stem cells from the iliac crest. 2. In a cord‐blood transplant, stem cells from the placenta are removed from the umbilical cord. 3. Cord‐blood transplants have several advantages over bone marrow transplants. 19.7 Hemostasis Hemostasis refers to the stoppage of bleeding. It involves vascular spasm, platelet plug formation, and blood clotting (coagulation). In vascular spasm, the smooth muscle of a blood vessel wall contracts, which slows blood loss. 4. Platelet plug formation involves the aggregation of platelets to stop bleeding. 5. A clot is a network of insoluble protein fibers (fibrin) in which formed elements of blood are trapped. 6. The chemicals involved in clotting are known as clotting (coagulation) factors. 7. Blood clotting involves a cascade of reactions that may be divided into three stages: formation of prothrombinase, conversion of prothrombin into thrombin, and conversion of soluble fibrinogen into insoluble fibrin. 8. Clotting is initiated by the interplay of the extrinsic and intrinsic pathways of blood clotting. 9. Normal coagulation requires vitamin K and is followed by clot retraction (tightening of the clot) and ultimately fibrinolysis (dissolution of the clot). 10. Clotting in an unbroken blood vessel is called thrombosis. A thrombus that moves from its site of origin is called an embolus. 1. 2. 3. 19.8 Blood Groups and Blood Types 1. ABO and Rh blood groups are genetically determined and based on antigen–antibody responses. 2. In the ABO blood group, the presence or absence of A and B antigens on the surface of RBCs determines blood type. 3. In the Rh system, individuals whose RBCs have Rh antigens are classified as ; those who lack the antigen are . 4. Hemolytic disease of the newborn (HDN) can occur when an mother is pregnant with an fetus. 5. Before blood is transfused, a recipient's blood is typed and then either cross‐matched to potential donor blood or screened for the presence of antibodies.