Chapter 24
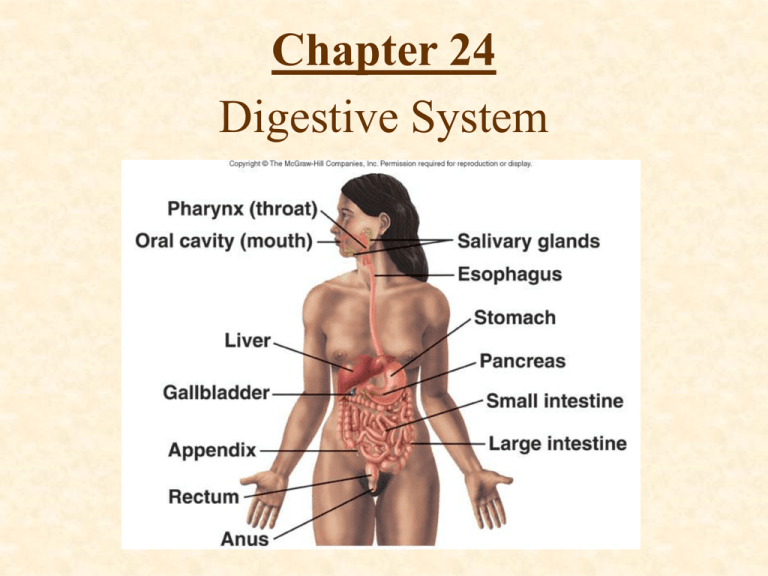
Digestive System
Digestive System Anatomy
• Digestive tract
– Alimentary tract or canal
– GI tract
• Accessory organs
– Primarily glands
• Regions
–
–
–
–
–
–
–
Mouth or oral cavity
Pharynx
Esophagus
Stomach
Small intestine
Large intestine
Anus
The function of digestive system:
Mechanically breakdown the food stuff and
enzymatically digest them.
Absorb necessary nutrients including ions.
Lubrication, emulsification, mixing, transport Deglutition, bolus, peristalisis, etc.
Release of wastes from the body
Functions
• Ingestion: Introduction of food into stomach
• Mastication: Chewing
• Propulsion
– Deglutition: Swallowing
– Peristalsis: Moves material through digestive tract
Functions
•
•
•
•
•
Mixing: Segmental contraction that occurs in small intestine
Secretion: Lubricate, liquefy, digest
Digestion: Mechanical and chemical
Absorption: Movement from tract into circulation or lymph
Elimination: Waste products removed from body
Digestive Tract Histology
Digestive System Regulation
• Nervous regulation
– Involves enteric
nervous system
• Types of neurons:
sensory, motor,
interneurons
– Coordinates peristalsis
and regulates local
reflexes
• Chemical regulation
– Production of hormones
• Gastrin, secretin
– Production of paracrine
chemicals
• Histamine
• Help local reflexes in
ENS control digestive
environments as pH
levels
Oral Cavity
• Mouth or oral cavity
– Vestibule: Space between
lips or cheeks and alveolar
processes
– Oral cavity proper
• Lips (labia) and cheeks
• Palate: Oral cavity roof
– Hard and soft
• Palatine tonsils
• Tongue: Involved in
speech, taste, mastication,
swallowing
Salivary Glands
• Produce saliva
– Prevents bacterial
infection
– Lubrication
– Contains salivary
amylase
• Breaks down starch
• Three pairs
– Parotid: Largest
– Submandibular
– Sublingual: Smallest
a.
Functions of the oral cavity
In addition to chewing, or mastication in the oral cavity its enzyme contributes the
initial stage of digestion.
The salivary glands release salivary amylase, which digests starch into glucose and
the other polysaccharides to disaccharides. (Fig. 24-7 and Fig. 24.9)
Note that humans do not digest cellulose, since they do not have cellulase.
In addition, saliva contains lysozyme and immunoglobulin A to fight against bacteria.
Mucous release from the other glands in the oral cavity contains mucin, a
proteoglycan, that contributes lubrication of the mouth.
The salivary glands stimulation is primarily through the parasympathetic nerve.
Higher centers of the brain also affect the activity of the salivary glands.
Pharynx and Esophagus
• Esophagus
• Pharynx
– Nasopharynx
– Oropharynx: Transmits
food normally
– Laryngopharynx:
Transmits food
normally
– Transports food from
pharynx to stomach
– Passes through
esophageal hiatus
(opening) of diaphragm
and ends at stomach
• Hiatal hernia
– Sphincters
• Upper
• Lower
Deglutition (Swallowing)
• Three phases
– Voluntary
• Bolus of food moved by tongue from oral cavity to
pharynx
– Pharyngeal
Reflex: Upper esophageal sphincter relaxes, elevated
pharynx opens the esophagus, food pushed into
esophagus
– Esophageal
• Reflex: Epiglottis is tipped posteriorly, larynx
elevated to prevent food from passing into larynx
Fig. 24-11 The
swallowing
process
Stomach Anatomy
• Openings
– Gastroesophageal: To
esophagus
– Pyloric: To duodenum
• Regions
–
–
–
–
Cardiac
Fundus
Body
Pyloric
Stomach Histology
• Layers
– Serosa or visceral
peritoneum: Outermost
– Muscularis: Three layers
• Outer longitudinal
• Middle circular
• Inner oblique
– Submucosa
– Mucosa
Stomach Histology
• Rugae: Folds in
stomach when empty
• Gastric pits: Openings
for gastric glands
– Contain cells
• Surface mucous: Mucus
• Mucous neck: Mucus
• Parietal: Hydrochloric
acid and intrinsic factor
• Chief: Pepsinogen
• Endocrine: Regulatory
hormones
i.
Secretions in the stomach (Fig. 24-13)
The mixture in the stomach is called chyme.
Stomach secretes mucus, hydrochloric acid, gastrin, intrinsic factor,
and pepsinogen, a precursor to protease pepsin.
Alkaline mucus secreted from the mucus cells protects the epithelial
cells from the acidic chyme and pepsin.
Parietal cells in the gastric glands secrete intrinsic factor and
concentrated HCl. Intrinsic factor is a vitamin B12 binding
glycoprotein for better absorption of B12.
Chief cells within the gastric glands secrete pepsinogen, which will
be activated to pepsin by HCl.
i.
Low pH in the stomach
Relatively high concentration of HCl released in the stomach has
the following functions
(a) The value of pH in the stomach is 1 - 3.
(b) Most of bacteria are killed at this pH. But not all! Pylori
(c) Inactivate amylase, thus no further
digestion of carbohydrates.
(d) Many proteins are denatured.
(e) Pepsin, now activated at this pH, can digest these
proteins
Fig. 24-14
Secretion
of HCl
i.
Secretion of H+
Release of H+ from parietal cell into the stomach
starts with consumption of CO2 from blood. (Fig.
24-14) Note the names of players in this process:
CA, ATP requiring proton/potassium exchange
pump, bicarbonate/chloride shift, movements of
potassium, bicarbonate and chloride ions.
i.
Regulation of stomach secretion
2 - 3 L of gastric secretion/day.
Up to 700 ml/meal depending on the types of
meals.
Both neuronal and hormonal regulations are
possible. For details study Fig. 24-15.
Phases of Gastric Secretion
Fig. 24-15a
Fig. 24-15b
Fig. 24-15c
Movements in Stomach
Small Intestine
• Site of greatest amount of
digestion and absorption
• Divisions
– Duodenum
– Jejunum
– Ileum: Peyer’s patches or
lymph nodules
• Modifications
– Circular folds or plicae
circulares, villi, lacteal,
microvilli
• Cells of mucosa
– Absorptive, goblet, granular,
endocrine
Small Intestine Secretions
• Mucus
– Protects against digestive enzymes and stomach acids
• Digestive enzymes
– Disaccharidases: Break down disaccharides to
monosaccharides
– Peptidases: Hydrolyze peptide bonds
– Nucleases: Break down nucleic acids
• Duodenal glands
– Stimulated by vagus nerve, secretin, chemical or tactile
irritation of duodenal mucosa
The primary center for digestion and adsorption. In
three parts: duodenum, jejunum and ileum making up
to 6 meters (Fig. 24-16)
In fact, the digestive function in the small intestine
follows the food stuff being digested by pancreatic juice
to relatively smaller molecules.
Observe the anatomy and histology of the intestinal wall
to find intestinal glands, capillary networks in the villi,
lacteal, goblet cells, etc. (Fig. 24-17)
i.
Secretions in the small intestine (Fig. 24-16, 17)
Duodenal glands and Goblet cells release mucus.
The final stage of break down to small molecules so that they may be
absorbed through villi.
Absorptive cells release digestive enzymes, such as aminopeptidase,
peptidase, enterokinase (trypsinogen activator), amylase, sucrase,
maltase, isomaltase, lactase and lipase.
These enzymes are bound to the membranes of the absorptive cell
Microville.
Many other digestive enzymes are supplied from the pancreas.
i.
Movement in the small intestine
Segmental contraction for mixing and peristaltic
contractions for propelling are observed.
The contractions move at rate of 1 cm/min, thus taking 3
- 5 hours for chyme to move from the pylorus to the
ileocecal junction.
ii.
Absorption from the small intestine
Out of about 9 L of water enters the digestive system,
the small intestine absorbs about 8 - 8.5L by osmosis.
Duodenum and Pancreas
Duodenum Anatomy and
Histology
Pancreas
• Anatomy
– Endocrine
• Pancreatic islets
produce insulin and
glucagon
– Exocrine
• Acini produce digestive
enzymes
– Regions: Head, body,
tail
• Secretions
– Pancreatic juice
(exocrine)
•
•
•
•
•
•
Trypsin
Chymotrypsin
Carboxypeptidase
Pancreatic amylase
Pancreatic lipases
Enzymes that reduce
DNA and ribonucleic
acid
a.
Functions of the pancreas
The gross anatomy and cytology of the pancreas is shown
in (Fig. 24-18). The pancreas has both endocrine and
exocrine cells.
Endocrine: Pancreatic islet contact to blood stream.
Alpha cells – glucagons
Beta cells – insulin
Exocrine: Acini cells open to ducts and secrete enzymes
Bicarbonate Ion Production
i.
Pancreatic juice to adjust pH.
The columnar epithelial cells of the pancreas contains
bicarbonate ions, which will be released into the
intralobular duct of the pancreas. The bicarbonate ion
neutralize the acidic chyme and stops pepsin activity,
while make it possible for the pancreatic enzymes to
remain active in the small intestine. (Fig. 24.22 of
Seeley)
i.
Pancreatic enzymes
The acinar cells of the pancreas produce pancreatic
enzymes.
Many proteolytic enzymes are released in the form of
precursors.
They include, trypsinogen , chymotrypsinogen, and
procarboxypeptidase and are activated by other
enzymes, such as enterokinase.
Amylase, lipases are also present.
i.
Control of pancreatic secretion
By both hormonal and neuronal means. (Fig. 24-22 and
Fig. 24.23 of Seeley)
Also study Table 24-1.
Fig. 24-22
Hormone
action
Pancreatic Secretion Control
Liver
• Lobes
– Major: Left and right
– Minor: Caudate and
quadrate
• Ducts
– Common hepatic
– Cystic
• From gallbladder
– Common bile
• Joins pancreatic duct at
hepatopancreatic ampulla
Functions of the Liver
• Bile production
– Salts emulsify fats, contain pigments as bilirubin
• Storage
– Glycogen, fat, vitamins, copper and iron
• Nutrient interconversion
• Detoxification
– Hepatocytes remove ammonia and convert to urea
• Phagocytosis
– Kupffer cells phagocytize worn-out and dying red and white blood cells,
some bacteria
• Synthesis
– Albumins, fibrinogen, globulins, heparin, clotting factors
a.
i.
Liver functions
Anatomy and histology: (Fig. 24.19)
Bile production
600 - 1000 ml/day
No digestive enzymes
Dilute and neutralize stomach acid and emulsify fats.
The pH of chyme is raised so that pancreatic enzymes can function.
Contains bilirubin from broken down hemoglobin.
Cholesterol, fast, fat-soluble hormone and lecithin are found.
The blood and bile flow: (Fig. 24.20)
Stimulates bile secretion - secretin from duodenum, by parasympathetic
vegas nerve, increased blood flow in the liver, etc. (Fig. 24.21)
Blood and Bile Flow
ii.
Storage
Liver cells extract sugar from the blood and store as
glycogen. Fats, vitamins, copper and iron are also stored
for a short while
Thus hepatocytes can control blood sugar level..
.
iii.
Nutrient interconversion
Proteins to carbohydrates to fats etc., and back.
Further transformation of the nutrients. Hydroxylation of
vitamin D.
i.
Detoxification
Conversion of toxic substances to acceptable substance. For
example ammonia is converted to urea for elimination through the
kidney as urine.
ii.
Phagocytosis
Hepatic phagocytic cells (Kupffer cells) phagocyte old RBC,
WBC, bacteria, etc.
iii.
Synthesis
Many blood proteins are synthesized in the liver. Albumin,
fibrinogen, globulin, heparin, clotting factors, etc.
Duct System
Gallbladder
• Bile is stored and concentrated
• Stimulated by cholecystokinin and vegal
stimulation
• Dumps into small intestine
• Production of gallstones possible
– Drastic dieting with rapid weight loss
a. Functions of the gallbladder
The gallbladder stores and concentrates bile
produced by the liver.
After a meal, it releases choleostokinin from the
duodenum and stimulates releases of bile into the
small intestine. (Fig. 24-21)
Fig. 24-21 The Gallbladder
Secretin and cholecystokinin:
Inhibit gastric secretions in the stomach,
Stimulate secretion and release of bile of the
gallbladder
Stimulate release of bicarbonate ion and
digestive enzymes from the pancreas
Large Intestine
• Extends from ileocecal junction to anus
• Consists of cecum, colon, rectum, anal canal
• Movements sluggish (18-24 hours)
Fig. 24-24 Histology of the large intestine
Large Intestine
• Cecum
– Blind sac, vermiform appendix attached
• Colon
– Ascending, transverse, descending, sigmoid
• Rectum
– Straight muscular tube
• Anal canal
– Internal anal sphincter (smooth muscle)
– External anal sphincter (skeletal muscle)
– Hemorrhoids: Vein enlargement or inflammation
a. Functions of the large intestine (Fig. 24.25)
Slow sluggish movement in the colon taking 18 - 24
hours. Water and salts are absorbed and
microorganisms help in the formation of feces. 1500
ml of chyme entering the colon end up only 80 - 150
ml of feces.
Secretions of Large Intestine
• Mucus provides protection
– Parasympathetic stimulation increases rate of
goblet cell secretion
• Pumps
– Exchange of bicarbonate ions for chloride ions
– Exchange of sodium ions for hydrogen ions
• Bacterial actions produce gases called flatus
Histology of Large Intestine
Movement in Large Intestine
• Mass movements
– Common after meals
• Local reflexes in enteric plexus
– Gastrocolic: Initiated by stomach
– Duodenocolic: Initiated by duodenum
• Defecation reflex
– Distension of the rectal wall by feces
• Defecation
– Usually accompanied by voluntary movements to expel feces
through abdominal cavity pressure caused by inspiration
Fig. 24-25 The
defecation reflex
Digestion, Absorption, Transport
• Digestion
– Breakdown of food molecules for absorption into
circulation
• Mechanical: Breaks large food particles to small
• Chemical: Breaking of covalent bonds by digestive
enzymes
• Absorption and transport
– Molecules are moved out of digestive tract and
into circulation for distribution throughout body
Carbohydrates
• Consist of starches, glycogen, sucrose, lactose, glucose, fructose
• Polysaccharides broken down to monosaccharides
• Monosaccharides taken up by active transport or facilitated diffusion
and carried to liver
• Glucose is transported to cells requiring energy
– Insulin influences rate of transport
Lipids
• Include triglycerides, phospholipids, steroids, fat-soluble
vitamins
• Emulsification breaks down large lipid droplets to small
Lipoproteins
• Types
– Chylomicrons
• Enter lymph
– VLDL
– LDL
• Transports cholesterol
to cells
– HDL
• Transports cholesterol
from cells to liver
Cholesterol over 200 mg/100 ml blood risks
coronary heart disease (CHD).
Other risk factors are: hypertension, diabetes
mellitus, cigarette smoking, low plasma high
density lipids (HDL),
Obesity – low HDL
Exercise – high HDL and decreased LDL
Ingestion of fatty acids – increased plasma
cholesterol, higher LDH, lower HDL
Proteins
• Pepsin breaks proteins into smaller polypeptide chains
• Proteolytic enzymes produce small peptide chains
– Dipeptides, tripeptides, amino acids
Water and Ions
• Water
– Can move in either
direction across wall of
small intestine
depending on osmotic
gradients
• Ions
– Sodium, potassium,
calcium, magnesium,
phosphate are actively
transported
Effects of Aging
• Decrease in mucus layer, connective tissue,
muscles and secretions
• Increased susceptibility to infections and
toxic agents
– Ulcerations and cancers










