Chapter 20
advertisement

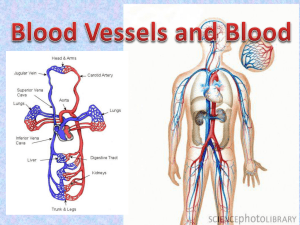
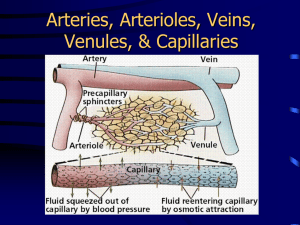
Chapter 20 Lecture Outline See PowerPoint Image Slides for all figures and tables pre-inserted into PowerPoint without notes. 20-1 Copyright (c) The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Blood Vessels and Circulation • • • • • • General anatomy of blood vessels Blood pressure, resistance and flow Capillary exchange Venous return and circulatory shock Special circulatory routes Anatomy of – pulmonary circuit – systemic arteries and veins 20-2 Anatomy of Blood Vessels • Arteries carry blood away from heart • Veins carry blood back to heart • Capillaries connect smallest arteries to veins 20-3 Vessel Wall • Tunica interna (intima) – smooth inner layer that repels blood cells and platelets – simple squamous endothelium overlying a basement membrane and layer of fibrous tissue • Tunica media – middle layer – usually thickest; smooth muscle, collagen, some elastic – smooth muscle for vasomotion • Tunica externa (tunica adventitia) – outermost layer – loose connective tissue with vasa vasorum 20-4 Large Vessels 20-5 Arteries • Conducting (elastic) arteries - largest – pulmonary, aorta and common carotid – tunica media consists of perforated sheets of elastic tissue, alternating with thin layers of smooth muscle, collagen and elastic fibers – expand during systole, recoil during diastole; lessens fluctuations in BP • Distributing (muscular) arteries – distributes blood to specific organs; femoral and splenic – smooth muscle layers constitute 3/4 of wall thickness 20-6 Medium Vessels 20-7 Arteries and Metarterioles • Resistance (small) arteries – arterioles control amount of blood to various organs • Metarterioles – short vessels connect arterioles to capillaries – muscle cells form a precapillary sphincter about entrance to capillary 20-8 Small Vessels 20-9 Arterial Sense Organs • Major arteries above heart • Carotid sinuses – in walls of internal carotid artery – monitors BP – signaling brainstem • HR and vessels dilate • Carotid bodies – oval bodies near carotids – monitor blood chemistry • adjust respiratory rate to stabilize pH, CO2, and O2 • Aortic bodies – in walls of aorta – same function as carotid bodies 20-10 Capillaries • Thoroughfare channel - metarteriole continues through capillary bed to venule • Precapillary sphincters control which beds are well perfused – only 1/4 of the capillaries are open at a given time 20-11 Control of Capillary Bed Perfusion 20-12 Control of Capillary Bed Perfusion 20-13 Types of Capillaries • Continuous - occur in most tissues – endothelial cells have tight junctions with intercellular clefts (allow passage of solutes) • Fenestrated - kidneys, small intestine – organs that require rapid absorption or filtration – filtration pores – spanned by very thin glycoprotein layer - allows passage of only small molecules • Sinusoids - liver, bone marrow, spleen – irregular blood-filled spaces; some have extra large fenestrations, allow proteins and blood cells to enter 20-14 Fenestrated Capillary 20-15 Sinusoid in Liver 20-16 Veins • Veins – – – – lower blood pressure: 10mmHg with little fluctuation thinner walls, less muscular and elastic tissue expand easily, have high capacitance valves aid skeletal muscles in upward blood flow • Venules – postcapillary venules more porous than capillaries – muscular venules have tunica media • Venous sinuses – veins with thin walls, large lumens, no smooth muscle 20-17 Blood Distribution, Resting Adult 20-18 Circulatory Routes • Most common route – heart arteries arterioles capillaries venules veins • Portal system – blood flows through two consecutive capillary networks before returning to heart • hypothalamus - anterior pituitary • found in kidneys • between intestines - liver 20-19 Anastomoses • Point where 2 blood vessels merge • Arteriovenous shunt – artery flows directly into vein • Venous anastomosis – most common, blockage less serious – alternate drainage of organs • Arterial anastomosis – collateral circulation (coronary) 20-20 Principles of Blood Flow • Blood flow: amount of blood flowing through a tissue in a given time (ml/min) • Perfusion: rate of blood flow per given mass of tissue (ml/min/g) • Important for delivery of nutrients and oxygen, and removal of metabolic wastes • Hemodynamics – physical principles of blood flow based on pressure and resistance • F P/R, (F = flow, P = difference in pressure, R = resistance to flow) 20-21 Blood Pressure • • • • • • Force that blood exerts against a vessel wall Measured at brachial artery of arm Systolic pressure: BP during ventricular systole Diastolic pressure: BP during ventricular diastole Normal value, young adult: 120/75 mm Hg Pulse pressure: systolic - diastolic – important measure of stress exerted on small arteries • Mean arterial pressure (MAP): – measurements taken at intervals of cardiac cycle, best estimate: diastolic pressure + (1/3 of pulse pressure) – varies with gravity: standing; 62 - head, 180 - ankle 20-22 BP Changes With Distance 20-23 Blood Pressure • Importance of arterial elasticity – expansion and recoil maintains steady flow of blood throughout cardiac cycle, smoothes out pressure fluctuations and stress on small arteries • BP rises with age: arteries less distensible • BP determined by cardiac output, blood volume and peripheral resistance 20-24 Abnormalities of Blood Pressure • Hypertension – chronic resting BP > 140/90 – consequences • can weaken small arteries and cause aneurysms • Hypotension – chronic low resting BP – caused by blood loss, dehydration, anemia 20-25 Peripheral Resistance • Blood viscosity - by RBC’s and albumin – viscosity with anemia, hypoproteinemia – viscosity with polycythemia , dehydration • Vessel length – pressure and flow with distance (friction) • Vessel radius - very powerful influence over flow – most adjustable variable, controls resistance quickly – vasomotion: change in vessel radius • vasoconstriction, vasodilation 20-26 Peripheral Resistance • Vessel radius (cont.) – laminar flow - flows in layers, faster in center – blood flow (F) proportional to the fourth power of radius (r), F r4 • arterioles can constrict to 1/3 of fully relaxed radius – if r = 3 mm, F = (34) = 81 mm/sec; if r = 1 mm, F = 1mm/sec – 3X in radius results in 81X in flow 20-27 Flow at Different Points • From aorta to capillaries, flow for 3 reasons – greater distance, more friction to flow – smaller radii of arterioles and capillaries – farther from heart, greater total cross sectional area • From capillaries to vena cava, flow again – large amount of blood forced into smaller channels – never regains velocity of large arteries 20-28 Regulation of BP and Flow • Local control • Neural control • Hormonal control 20-29 Local Control of BP and Flow • Metabolic theory of autoregulation – tissue inadequately perfused, wastes accumulate = vasodilation • Vasoactive chemicals – substances that stimulate vasomotion; histamine, bradykinin • Reactive hyperemia – blood supply cut off then restored • Angiogenesis - growth of new vessels – regrowth of uterine lining, around obstructions, exercise, malignant tumors – controlled by growth factors and inhibitors 20-30 Neural Control of BP and Flow • Vasomotor center of medulla oblongata: – sympathetic control stimulates most vessels to constrict, but dilates vessels in skeletal and cardiac muscle – integrates three autonomic reflexes • baroreflexes • chemoreflexes • medullary ischemic reflex 20-31 Neural Control: Baroreflex • Changes in BP detected by stretch receptors (baroreceptors), in large arteries above heart – aortic arch – aortic sinuses (behind aortic valve cusps) – carotid sinus (base of each internal carotid artery) • Autonomic negative feedback response – baroreceptors send constant signals to brainstem – BP causes rate of signals to rise, inhibits vasomotor center, sympathetic tone, vasodilation causes BP – BP causes rate of signals to drop, excites vasomotor center, sympathetic tone, vasoconstriction and BP 20-32 Baroreflex Negative Feedback Response 20-33 Neural Control: Chemoreflex • Chemoreceptors in aortic bodies and carotid bodies – located in aortic arch, subclavian arteries, external carotid arteries • Autonomic response to changes in blood chemistry – pH, O2, CO2 – primary role: adjust respiration – secondary role: vasomotion • hypoxemia, hypercapnia and acidosis stimulate chemoreceptors, instruct vasomotor center to cause vasoconstriction, BP, lung perfusion and gas exchange 20-34 Other Inputs to Vasomotor Center • Medullary ischemic reflex – inadequate perfusion of brainstem • cardiac and vasomotor centers send sympathetic signals to heart and blood vessels • cardiac output and causes widespread vasoconstriction • BP • Other brain centers – stress, anger, arousal can also BP 20-35 Hormonal Control of BP and Flow • Angiotensinogen (prohormone produced by liver) Renin (kidney enzyme released by low BP) • Angiotensin I ACE (angiotensin-converting enzyme in lungs) ACE inhibitors block this enzyme lowering BP • Angiotensin II – very potent vasoconstrictor 20-36 Hormonal Control of BP and Flow • Aldosterone – promotes Na+ and water retention by kidneys – increases blood volume and pressure • Atrial natriuretic factor ( urinary sodium excretion) – generalized vasodilation • ADH (water retention) – pathologically high concentrations, vasoconstriction • Epinephrine and norepinephrine effects – most blood vessels • binds to -adrenergic receptors, vasoconstriction – skeletal and cardiac muscle blood vessels • binds to -adrenergic receptors, vasodilation 20-37 Routing of Blood Flow • Localized vasoconstriction – pressure downstream drops, pressure upstream rises – enables routing blood to different organs as needed • Arterioles - most control over peripheral resistance – located on proximal side of capillary beds – most numerous – more muscular by diameter 20-38 Blood Flow in Response to Needs • Arterioles shift blood flow with changing priorities 20-39 Blood Flow Comparison • During exercise – perfusion of lungs, myocardium and skeletal muscles perfusion of kidneys and digestive tract 20-40 Capillary Exchange • Only occurs across capillary walls between blood and surrounding tissues • 3 routes across endothelial cells – intercellular clefts – fenestrations – through cytoplasm • Mechanisms involved – diffusion, transcytosis, filtration and reabsorption 20-41 Capillary Exchange - Diffusion • Most important mechanism • Lipid soluble substances – steroid hormones, O2 and CO2 diffuse easily • Insoluble substances – glucose and electrolytes must pass through channels, fenestrations or intercellular clefts • Large particles - proteins, held back 20-42 Capillary Exchange - Transcytosis • Pinocytosis - transport vesicles across cell exocytosis • Important for fatty acids, albumin and some hormones (insulin) 20-43 Capillary Exchange Filtration and Reabsorption • Opposing forces – blood (hydrostatic) pressure drives fluid out of capillary • high on arterial end of capillary, low on venous end – colloid osmotic pressure (COP) draws fluid into capillary • results from plasma proteins (albumin)- more in blood • oncotic pressure = net COP (blood COP - tissue COP) • Hydrostatic pressure – physical force exerted against a surface by a liquid, (BP is an example) 20-44 Capillary Filtration and Reabsorption • Capillary filtration at arterial end • Capillary reabsorption at venous end • Variations – location (glomeruli- devoted to filtration alveolar cap.- devoted to absorption) – activity or trauma ( filtration) 20-45 Causes of Edema • Capillary filtration ( capillary BP or permeability) – poor venous return • congestive heart failure - pulmonary edema • insufficient muscular activity – kidney failure (water retention, hypertension) – histamine makes capillaries more permeable • Capillary reabsorption – hypoproteinemia (oncotic pressure blood albumin) cirrhosis, famine, burns, kidney disease • Obstructed lymphatic drainage 20-46 Consequences of Edema • Tissue necrosis – oxygen delivery and waste removal impaired • Pulmonary edema – suffocation • Cerebral edema – headaches, nausea, seizures and coma • Circulatory shock – excess fluid in tissue spaces causes low blood volume and low BP 20-47 Mechanisms of Venous Return • Pressure gradient – 7-13 mm Hg venous pressure towards heart • venules (12-18 mm Hg) to central venous pressure (~5 mm Hg) • Gravity drains blood from head and neck • Skeletal muscle pump in the limbs • Thoracic pump – inhalation - thoracic cavity expands (pressure ) abdominal pressure , forcing blood upward – central venous pressure fluctuates • 2mmHg- inhalation, 6mmHg-exhalation • blood flows faster with inhalation • Cardiac suction of expanding atrial space 20-48 Skeletal Muscle Pump 20-49 Venous Return and Physical Activity • Exercise venous return in many ways – heart beats faster, harder - CO and BP – vessels of skeletal muscles, lungs and heart dilate flow – respiratory rate action of thoracic pump – skeletal muscle pump • Venous pooling occurs with inactivity – venous pressure not enough force blood upward – with prolonged standing, CO may be low enough to cause dizziness or syncope • prevented by tensing leg muscles, activate skeletal m. pump – jet pilots wear pressure suits 20-50 Circulatory Shock • Any state where cardiac output insufficient to meet metabolic needs – cardiogenic shock - inadequate pumping of heart (MI) – low venous return (LVR) shock - 3 principle forms 1. hypovolemic shock - most common – loss of blood volume: trauma, burns, dehydration 2. obstructed venous return shock – tumor or aneurysm 3. venous pooling (vascular) shock – next slide 20-51 LVR Shock • Venous pooling (vascular) shock – long periods of standing, sitting or widespread vasodilation – neurogenic shock - loss of vasomotor tone, vasodilation • causes from emotional shock to brainstem injury • Septic shock – bacterial toxins trigger vasodilation and capillary permeability • Anaphylactic shock – severe immune reaction to antigen, histamine release, generalized vasodilation, capillary permeability 20-52 Responses to Circulatory Shock • Compensated shock • Decompensated shock 20-53 Compensated shock • Homeostatic mechanisms bring about recovery • BP triggers baroreflex and production of angiotensin II, both stimulate vasoconstriction • If person faints and falls to horizontal position, gravity restores blood flow to brain; quicker if feet are raised 20-54 Decompensated shock • Life threatening positive feedback loops occur – CO myocardial ischemia and infarction CO – slow circulation disseminated intravascular coagulation slow circulation – ischemia and acidosis of brainstem vasomotor tone, vasodilation CO ischemia and acidosis of brainstem 20-55 Special Circulatory Routes- Brain • Total perfusion kept constant – seconds of deprivation causes loss of consciousness – 4-5 minutes causes irreversible brain damage – flow can be shifted from one active region to another • Responds to changes in BP and chemistry – cerebral arteries: dilate as BP , constrict as BP rises – main chemical stimulus: pH • CO2 + H2O H2 CO3 H+ + (HCO3)• hypercapnia (CO2 ) in brain, pH , triggers vasodilation • hypocapnia, pH, vasoconstriction – occurs with hyperventilation, may lead to ischemia, dizziness and sometimes syncope 20-56 TIA’s and CVA’s • TIA’s - transient ischemic attacks – dizziness, loss of vision, weakness, paralysis, headache or aphasia; lasts from a moment to a few hours, often early warning of impending stroke • CVA - cerebral vascular accident (stroke) – brain infarction caused by ischemia • atherosclerosis, thrombosis, ruptured aneurysm – effects range from unnoticeable to fatal • blindness, paralysis, loss of sensation, loss of speech common – recovery depends on surrounding neurons, collateral circulation 20-57 Special Circulatory Routes Skeletal Muscle • Highly variable flow • At rest – arterioles constrict, total flow about 1L/min • During exercise – arterioles dilate in response to epinephrine and sympathetic nerves – precapillary sphincters dilate due to lactic acid, CO2 – blood flow can increase 20 fold • Muscular contraction impedes flow – isometric contraction causes fatigue faster than isotonic 20-58 Special Circulatory Routes Lungs • Low pulmonary blood pressure – flow slower, more time for gas exchange – capillary fluid absorption • oncotic pressure overrides hydrostatic pressure • Unique response to hypoxia – pulmonary arteries constrict, redirects flow to better ventilated region 20-59 Pulmonary Circulation • Pulmonary trunk to pulmonary arteries to lungs – lobar branches for each lobe (3 right, 2 left) • Pulmonary veins return to left atrium – increased O2 and reduced CO2 levels 20-60 Pulmonary Capillaries Near Alveoli • Basketlike capillary beds surround alveoli • Exchange of gases with air at alveoli 20-61 Major Systemic Arteries • Supplies oxygen and nutrients to all organs 20-62 Major Branches of Aorta • Ascending aorta – right and left coronary arteries supply heart • Aortic arch – brachiocephalic • right common carotid supplying right side of head • right subclavian supplying right shoulder and upper limb – left common carotid supplying left side of head – left subclavian supplying shoulder and upper limb • Descending aorta – thoracic aorta above diaphragm – abdominal aorta below diaphragm 20-63 Major Branches of the Aorta 20-64 Arteries of the Head and Neck • Common carotid to internal and external carotids – external carotid supplies most external head structures 20-65 Arterial Supply of Brain • Paired vertebral aa. combine to form basilar artery on pons • Circle of Willis on base of brain formed from anastomosis of basilar and internal carotid aa • Supplies brain, internal ear and orbital structures – anterior, middle and posterior cerebral – superior, anterior and posterior cerebellar 20-66 Arteries of the Upper Limb • Subclavian passes between clavicle and 1st rib • Vessel changes names as passes to different regions – subclavian to axillary to brachial to radial and ulnar – brachial used for BP and radial artery for pulse 20-67 Arteries of the Thorax • Thoracic aorta supplies viscera and body wall – bronchial, esophageal and mediastinal branches – posterior intercostal and phrenic arteries • Internal thoracic, anterior intercostal and pericardiophrenic arise from subclavian artery 20-68 Major Branches of Abdominal Aorta 20-69 Celiac Trunk Branches • Branches of celiac trunk supply upper abdominal viscera -- stomach, spleen, liver and 20-70 pancreas Mesenteric Arteries 20-71 Arteries of the Lower Limb • Branches to the lower limb arise from external iliac branch of the common iliac artery 20-72 Arterial Pressure Points • Some major arteries close to surface -- allows palpation for pulse and serve as pressure points to reduce arterial bleeding 20-73 Major Systemic Veins • Deep veins run parallel to arteries while superficial veins have many anastomoses 20-74 Deep Veins of Head and Neck • Large, thin-walled dural sinuses form in between layers of dura mater (drain brain to internal 20-75 jugular vein) Superficial Veins of Head and Neck • Branches of internal and external jugular veins drain the external structures of the head 20-76 • Upper limb is drained by subclavian vein Superficial and Deep Veins of Upper Limb 20-77 Inferior Vena Cava and Branches • Notice absence of veins draining the viscera --20-78 stomach, spleen, pancreas and intestines Veins of Hepatic Portal System • Drains blood from viscera (stomach, spleen and intestines) to liver so that nutrients are absorbed 20-79 Superficial and Deep Veins of Lower Limb 20-80