Off Site Anesthesia - UM Anesthesiology
advertisement

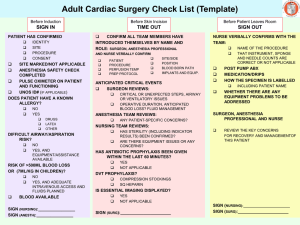
Off-site Anesthesia: New Challenges Pattricia S Klarr, M.D. University of Michigan What is the largest thing an endoscopist can remove from an anesthetized patient? …A Surgeon! Goals and Objectives -compare providing anesthesia in the endoscopy suite vs the operating room -review procedure types and anesthetic considerations -discuss evolution of anesthetic presence and effect of cost and efficiency -discuss impact of technology on the future Introduction NORA: Non Operating Room Anesthesia Also known as “Remote, offsite” Challenges 1. Not working with surgeons and operating room personnel 2. Lack of understanding of respective processes 3. Team building 4. Equipment needs/space requirements If the relationship of surgeons with anesthesia is a marriage without love… Then working with gastroenterologists is kind of like this…… ….but it doesn’t have to be. How did we get here? Vast majority of endoscopic procedures can be done with (nurse) sedation What has evolved is improvement of technology and acuity of patients NORA Rotation “…doing 5 straight days of the MPU is a bit much. It’s not that the hours are bad, it’s just that the pace and workflow down here can be pretty frustrating, and after a couple of days of it, I feel like I need to go back to an OR or I may lose my mind.” NORA GI anesthesia is like regular anesthesia because: • Standardized monitoring • Preprocedure evaluation and preparation It’s different because… • Access to specialized equipment is limited • Less support from nearby anesthetic colleagues Other challenges -inefficient scheduling -lack of access to medical records-open access patients -equipment upkeep/stocking of supplies -poor physical lay out -tech and nursing unfamiliar with anesthesia procedures -unfamiliarity with procedures/proceduralists Conditions where anesthesia support is indicated Uncooperative/combative patient Severe GERD ASA>3 OSA, morbid obesity Known/suspected difficult intubation Known difficult to sedate Chronic pain patients Anesthesia support for: Prolonged, difficult or painful procedures Abnormal body habitus making positioning difficult Extremes of ages Common Endoscopic Procedures -Colonoscopy -Esophagogastroduodenoscopy (EGD) -Endoscopic Ultrasonography (EUS) -Endoscopic Retrograde Cholangiopancreatography (ERCP) -Double balloon enteroscopy (DBE) -Endoscopic Mucosal Resection (EMR) 1. Mostly done with light to moderate sedation 2. Deep sedation indicated with 1. Uncooperative patient 2. Tolerant to pain/antianxiety medication 3. ASA>3 3. Anesthetic choices include midazolam/fentanyl and or propofol EGD 1. Moderate to deep sedation 2. Consider intubation with severe reflux, aspiration risk EUS 1. Ultrasound probe larger 2. May require deep sedation to general anesthesia -better yield with FNA with deeper anesthetic ERCP 1. Weigh risk versus benefits of deep sedation and intubating patient. 2. Patients are prone 3. GERD is common comorbidity Double Balloon Endoscopy 1. General anesthesia for oral entry 2. Improves visualization of entire GI tract. Endoscopic Mucosal Resection Removes mucosal lesions while preserving the submucosa and deeper layers. -diagnosis and treatment of superficial lesions, precancerous such as Barrett's -can be curative early superficial cancers of GI tract Deep vs. General Anesthesia Risks Associated with GI Endoscopy -Hemodynamic instability -elderly with limited cardiac reserve -dehydrated after prep -vagal response to GI distention -Aspiration risk -Airway access -shared airway Closed Claims NORA Findings 24 NORA Claims from 1990-2001 -half were from GI Suite -most were MAC -7of the 9 respiratory NORA events were GI 4 of the 7 were during ERCP Respiratory Events -half respiratory events deemed preventable with better monitoring -respiratory complications associated with -nonvigilance -inappropriate anesthetic choice -untrained staff -poor documentation Further Findings Inadequate oxygenation/ventilation was most common damaging event -oversedation -lack of monitoring specifically 02 sat monitor and capnography -Reviewers judged care as substandard in 54% of cases and preventable with better monitoring in 32% of cases Lessons Learned/Recommendations Standard monitors for all anesthesia locations Capnography and pulse oximitry can prevent respiratory complications Supplemental oxygen may disguise hypoventilation if capnogram not used. Safety Rules in Anesthesia! -Reliable -standardization of care -minimum monitoring standards capnography/pulse oximitry Reliability -continuous learning -just and fair culture individuals are appreciated and accountable -enthusiasm for teamwork -debriefing -support of leadership -effective flow of information Have anesthesia machine… Will Travel OK, we’re needed. We are safe and reliable. They are going to love us in the endoscopy suite now, right? Propofol Increase in colonoscopy for cancer screening Propofol sedation in many ways superior to fentanyl / midazolam rapid turn over = more volume Very safe for use in moderate sedation Pesky FDA Warning Label “For general anesthesia or MAC sedation, (propofol) should be administered only by persons trained in the administration of general anesthesia and not involved in the conduct of the surgical/diagnostic procedure. “ “Much of this debate, during a time of increasing health care costs and decreasing physician reimbursements, seems to reflect economic rather than clinical concerns” Douglas K Rex in The science and politics of propofol, Am J. Gastroenterology 2004 GASTROENTEROLOGY VIEW “(T)his is purely a move by gastroenterologists related to reimbursement. It’s not for improved patient safety; it’s not for improved patient outcomes”. Gervirtz, MD, MPH, Gastroendonews, May 2005 ANESTHESIA RESPONSE Revenue from Endoscopy Gastroenterologist Douglas Rex, M.D “Trained Registered Nurses/endoscopy teams can administer propofol safely for endoscopy” Gastroenterology 2005 Oral Surgeon Weighs In -passing an ACLS course every 2 years doesn’t make you skilled to handle BMV an unconscious patient in laryngospasm -Joel Weaver, DDS, PhD Anesthesia Progress, Summer 2006 Endoscopist-directed Administration of Propofol: A Worldwide Safety Experience Douglas K Rex, et al* Findings: In almost 650,000 cases of endoscopist directed propofol sedation cases worldwide, there were only 15 major complications: 11 need for intubation 4 deaths 0 permanent neurological injuries Conclusion Paraphrasing: 1. Endoscopist directed propofol administration is safe. 2. Anesthesia providers have higher costs relative to potential benefits Oh, by the way… -one of the limitations of the paper was “the reliability of the data depended on the self-reporting by the individual participating centers…” -and about the co-author, John A. Walker, his conflict disclosure includes this: CEO of Dr. NAPS From the Internet Dr. NAPS Inc. is a company that educates and trains RNs and physicians in the safe use of Propofol for procedural sedation. We will assist you in integrating the use of NAPS (nurse administered Propofol sedation) into your practice setting efficiently and effectively. John Walker, CEO* Gastroenterology Wants In Position statement: nonanesthesiologist administratration of propofol for GI endoscopy: “…with adequate training, physician-supervised nurse administration of propofol can be done safely and effectively” joint statement of AASLD, ACG, AGA, and ASGE 2009 The fight over propofol: Michael Jackson death June 2009 CMS guidelines 2010..propofol is only indicated for general anesthesia, MAC and for the sedations of the mechanically-ventilated patients. -Anesthesia Department is responsible for oversite FDA deny ACG request 8/10 -arguments not compelling -supports CMS requirement for anesthesia training if use propofol FDA-restriction Off label use of propfol opened up liability issues for gastroenterologists bye-bye Dr NAPS European instruction still available Dr. Cohen responds: “I believe the vast majority of endoscopists target moderate sedation, not deep. Therefore, FDA’s concerns about the risk of deep sedation and general anesthesia are unwarranted.” Cote study Predictors of complications during endoscopy: -male gender -high BMI -ASA score of 3 or higher -overall, deep sedation with propofol is safe for advanced endoscopic cases Cote The vast majority of MAC cases (87.3%) could be considered slipping into a state of general anesthesia. Metzner and Domino 2010 Many studies aren’t blinded are biased and have conflict of interest -reliable studies are hampered by low incidence of severe adverse events, are expensive and difficult to perform NORA Near Miss Causes Anesthesiology News, March, 2013 Ootaki Paper 2012 -retrospective analysis of 371 patients -compared yield of EUS-FNA of solid pancreatic masses 73% vs. 83% diagnostic with GA -believe better patient cooperation attributed to improvement -cost impact? Ootaki, et al, Anesthesiology 2012: 117:1044-50 Technology to the Rescue? From GI private practitioners “FDA approval of (Sedasys) does not make patient care “dummy-proof” or safest for a given patient, because in the event of a misadventure, a “rescue expert’ is not immediately available to assist. It is ludicrous to assume that (training or new technology) will render community gastroenterologist as competent as anesthesia professionals” From the Oct. 9, 2013 Wall Street Journal: “Robots vs. Anesthesiologists” J&J's New Sedation Machine Promises Cheaper Colonoscopies; Doctors Fight Back By Jonathan D. Rockoff Anesthesiologists, who are among the highest-paid physicians, have long fought people in health care who target their specialty to curb costs. Now the doctors are confronting a different kind of foe: machines. A new system called Sedasys, made by Johnson & Johnson, would automate the sedation of many patients undergoing colon-cancer screenings ….. Sedation Machine Promises Cheaper Colonoscopies …… would automate (the) sedation …That could take anesthesiologists out of the room, eliminating a big source of income for the doctors. More than $1 billion is spent each year sedating... Sedasys and ASA Slide presentation and Panel discussion At 2013 Annual Meeting in San Francisco Log into ASA member website for access-video “Is Sedasys a Disruptive Device” Ad hoc committee finalized recommendations for Sedasys on 1/22/14 If all else fails… Video produced by Dr. Douglas Rex What We Know -endoscopy is a very low risk -Propopfol has high patient satisfaction -general anesthesia can improve diagnostic outcomes -the literature is full of biased studies What We Don’t know -Safety outcomes NAPs vs Anesthesia -Replacing providers with machines is cost-effective But as long as these stories exist: Propofol kills Michael Jackson 3 year old dies in dental office Our jobs are safe! Summary -compared providing anesthesia in the endoscopy suite vs the operating room -reviewed procedure types and anesthetic considerations -discussed evolution of anesthetic presence and effect of cost and efficiency -discussed impact of technology on the future References 1. 2. 3. 4. 5. 6. 7. 8. Rex DK, Heuss LT, Walker JA, Qi R. Trained registered nurses/endoscopy teams can administer propofol safely for endoscopy. Gastroenterology 2005; 129(5):1384-1391. Weaver JM. The great debate on nurse-administered propofol sedation (NAPS) – Where should we stand? Anesthesia Progress, Summer 2006; 53(2):31-33. Rex DK, et al. Endoscopist-directed administration of propofol: A worldwide safety experience. Gastroenterology, 2009; 137(4):1229-1237. Cote GA, et al. Incidence of sedation-related complications with propofol use during advanced endoscopic procedures. Clinical Gastroenterology and Hepatology, 2010; 8(2):137-142. Metzner J, Domino KB. Risks of anesthesia or sedation outside the operating room: the role of the anesthesia care provider. Curr Opin Anaesthesiol. 2010; 23(4):523-31. Ootaki C et al. Does general anesthesia increase the diagnostic yield of endoscopic ultrasound-guided fine needle aspiration of pancreatic masses? Anesthesiology. 201; 117(5):1044-50. Rex DK. The Science and politics of propofol. Am J Gastroenterol, 2004; 99(11):2080-3. Gervirtz. Nurse-administered propofol regularly puts patients at risk. Gastroendonews, 2005, May. Questions?