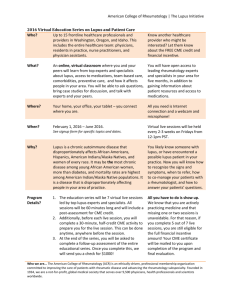
Activation of the signaling cascade in response to T lymphocytes and prostanoids in cutaneous lupus
advertisement

www.najms.org North American Journal of Medical Sciences 2011 May, Volume 3. No. 5. Case Report OPEN ACCESS Activation of the signaling cascade in response to T lymphocyte receptor stimulation and prostanoids in a case of cutaneous lupus Ana Maria Abreu-Velez, M.D. Ph.D.1, Graham Smith, Jr., M.D. 2, Michael S. Howard, M.D.1 1 Georgia Dermatopathology Associates, Atlanta, Georgia, USA. Diagnostic and Medical Clinic/Dermatology, Mobile, Alabama, USA. 2 Citation: Abreu-Velez AM, Smith G, Howard MS. Activation of the signaling cascade in response to T lymphocyte receptor stimulation and prostanoids in a case of cutaneous lupus. North Am J Med Sci 2011; 3: 251-254. Doi: 10.4297/najms.2011.3251 Availability: www.najms.org ISSN: 1947 – 2714 Abstract Context: Discoid lupus erythematosus is a chronic inflammatory skin disorder presenting with scarring lesions that occur predominately on sun exposed areas of the face and scalp. Case Report: A 22-year-old male was evaluated after presenting with reddish-purple, atrophic and erythematous plaques on the scalp, with loss of hair within the plaques. Biopsies for hematoxylin and eosin examination, direct immunofluorescence and immunohistochemistry analysis were performed. The hematoxylin and eosin staining demonstrated classic features of cutaneous lupus. Direct immunofluorescence revealed strong deposits of immunoglobulins IgG and IgM, fibrinogen and Complement/C3, present in 1) a shaggy pattern at the epidermal basement membrane zone, and 2) focal pericytoplasmic and perinuclear staining within epidermal keratynocytes. Immunohistochemisty staining revealed strongly positive staining with antibodies to cyclooxygenase-2, Zeta-chain-associated protein kinase 70, and HLA-DPDQDR in areas where the inflammatory infiltrate was predominant, as well as around dermal blood vessels and within the dermal extracellular matrix. Conclusions: Noting the autoimmune nature of lupus and its strong inflammatory component, we present a patient with active discoid lupus erythematosus and strong expression of Zeta-chain-associated protein kinase 70, cyclo-oxygenase-2, and HLA-DPDQDR in the inflammatory areas. We suggest that these molecules may play a significant role in the immune response of discoid cutaneous lupus, possibly including 1) the biosynthesis of the prostanoids and 2) activation of the signaling cascade in response to T-lymphocyte receptor stimulation. Keywords: Zap 70, COX-2, HLA-DPDQDR, discoid lupus erythematosus, autoantibodies, prostanoids. Correspondence to: Ana Maria Abreu-Velez, MD., PhD., Georgia Dermatopathology Associates, 1534 North Decatur Rd. NE; Suite 206, Atlanta, GA 30307-1000, USA. Tel.: (404) 371-0077, Fax: (404) 371-1900, Email: abreuvelez@yahoo.com. erythematosus, lupus erythematosus tumidus, lupus profundus, neonatal lupus erythematosus, chilblain lupus erythematosus, drug-induced lupus erythematosus, systemic lupus erythematosus, and hypertrophic LE, among others [1, 2]. Multiple models have been suggested for the pathogenesis of DLE. Ultraviolet radiation is thought to increase local mediators of inflammation, and stimulate local cytokine release. The cytokine release could in turn modify selectins, adhesion molecules, chemokines and prostanoids [3]. In addition, it has been suggested that the cytokines help to recruit and activate T lymphocytes, Introduction In the classic presentation of discoid lupus erythematosus (DLE), erythematous, scaly patches and plaques develop which leave postinflammatory pigmentary changes and white scars [1, 2]. The disease lesions may be localized or widespread. DLE predominantly affects the cheeks, nose and ears, but sometimes involves the upper back, frontal neck, and dorsal hands. LE is classified as an autoimmune disease, as it is associated with antibodies directed against components of cell nuclei. [1, 2]. There are multiple types of cutaneous LE, including DLE, subacute lupus 251 www.najms.org North American Journal of Medical Sciences 2011 May, Volume 3. No. 5. classic dendritic cells, and plasmocytoid dendritic cells [3]. Based on these factors, we investigated the possible presence of selected molecules in the skin biopsies of a patient affected by DLE. staining of stratum spinosum keratinocytes); IgM (-); IgE (-); complement/C1q (+, linear at the BMZ); complement/C3 (++, mild staining on dermal vascular walls); albumin (+++, pericytoplasmic and perinuclear staining of stratum spinosum keratinocytes, and mild linear staining along the BMZ) and fibrinogen (+++, linear pattern along the BMZ) (Figure 1). Case Report A 22-year-old African American male presented with reddish-purple atrophic plaques and erythematous patches on the scalp, with lesional hair loss. The clinical lesions were consistent with a presentation of discoid lupus erythematosus (DLE). He denied systemic symptoms of arthralgia, arthropathy, myalgia, fatigue, Raynaud's phenomenon and gastrointestinal complaints. Lesions were present on the head, mainly on the cheeks, but also on the trunk.. Laboratory data revealed a normal complete blood count, and a normal erythrocyte sedimentation rate. Serum electrolytes, blood urea nitrogen, creatinine, and liver function tests, as well as urinalysis and chest radiograms were within normal limits. The antiphospholipid, anti-Smith, anti-double stranded DNA, anti-histone, anti-ribonuclease-sensitive antigen, extractable nuclear antigen, small nuclear antigen, ribonucleoproteins, U1, U2, anti-SS-A and anti-SS-B antibodies were all negative. Complement was normal. Biopsies of the lesions were performed, with subsequent hematoxylin and eosin (H&E) staining, multicolor direct immunofluorescence (DIF) and immunohistochemistry (IHC); these techniques were performed as previously described [4-7]. Selected IHC antibodies included 1) Zeta-chain-associated protein kinase 70 (ZAP-70), which plays a critical role in the initiation of T-lymphocyte signaling, and 2) prostaglandin-endoperoxide synthase 2, also known as cyclo-oxygenase-2 (COX-2). Immunohistochemistry staining (IHC) The IHC staining revealed strong positivities to HLA-DPDQDR and ZAP-70 in most of the dermal inflammatory infiltrate, primarily around dermal blood vessels and within the extracellular matrix. The antibody to COX-2 was also overexpressed around the dermal vessels, and within the dermal extracellular matrix in focal areas surrounding inflammatory cells (Figure 1). To our surprise, the antibodies for linker for activation of T cells (LAT), CD34, BAX and CD35 displayed normal staining patterns, vis-à-vis their respective negative controls. We focused our studies on 1) several molecules involved in triggering the signaling cascade in response to T-cell receptor stimulation, 2) molecules expressed on antigen-presenting cells and 3) enzymes that play a role in biosynthesis of prostanoids. Hematoxylin and eosin staining (H&E) Examination of the H&E tissue sections demonstrated mild epidermal hyperkeratosis with focal follicular plugging. A mild interface infiltrate of lymphocytes, histiocytes and plasma cells was noted. Rouleaux of erythrocytes were noted in multiple superficial dermal blood vessels (Figure 1). Within the dermis, a superficial and deep, perivascular and periadnexal infiltrate of lymphocytes, histiocytes and plasma cells were observed. Neutrophils and eosinophils were rare, and dermal mucin was not appreciated (Figure 1). The histologic features were consisted with discoid lupus erythematosus (DLE). Fig. 1 a. H&E section demonstrating prominent follicular plugging (blue arrow).b. Erythrocytes sludging in dermal blood vessels and forming linear stacks of erythrocytes called rouleaux (blue arrows). c. Same as b, at higher magnification. d. Positive PAS staining along the BMZ (basement membrane zone) (blue arrow). e. DIF showing positive staining along the epidermal BMZ utilizing FITC conjugated anti-human fibrinogen (yellow arrow); the white arrow highlights cytoplasmic and perinuclear Direct immunofluorescence staining (DIF) DIF displayed positive (+++) deposits of FITC conjugated IgG, present as pericytoplasmic and perinuclear staining within the stratum spinosum of the keratinocytes, and in a linear pattern along the basement membrane zone (BMZ). Additional antibody staining supported a diagnosis of discoid lupus, i.e., IgA (+, pericytoplasmic and perinuclear 252 www.najms.org North American Journal of Medical Sciences 2011 May, Volume 3. No. 5. reactivity within epidermal keratinocytes. F. DIF showing positive epidermal staining with FITC conjugated anti-IgG (yellow staining; dark blue arrow). Epidermal keratinocyte nuclei are conterstained with Dapi (light blue). g, DIF showing positive staining along the epidermal BMZ utilizing FITC conjugated anti-human fibrinogen (yellow arrow); the white arrow highlights BMZ reactivity, and the yellow arrow shows vascular reactivity h. DIF showing positive staining with FITC conjugated vomplement/C3 against superficial dermal blood vessels (yellow staining; dark blue arrow). i. IHC demonstrating positive staining against COX-2 in the dermal inflammatory infiltrate, and also in the dermal extracellular matrix (brown staining; blue arrows). j. IHC highlighting positive staining against HLA-DPDQDR in the dermal inflammatory infiltrate (brown staining; blue arrow). k and l, IHCs showing positive staining against ZAP-70 in the dermal inflammatory infiltrate(brown staining; blue arrows). expressed in T cells and natural killer cells, but is also detectable in mast cells and basophils [9, 10]. ZAP-70 is further expressed in normal pre-B lymphocytes, but not in mature B lymphocytes [10, 11]. It has been previously demonstrated that T cells from SLE patients exhibit defective functions of CD4 (+) T cells; these T cells can in turn be responsible for improper activation of B cells, and resultant antibody biosynthesis against host antigens. Other authors found that ZAP-70 protein content in SLE CD4 (+) T cells may be reciprocally correlated with SLE disease activity [9, 11]. In our patient, we also found positive staining for prostaglandin-endoperoxide synthase 2, also known as cyclo-oxygenase 2 (COX-2). The COX-2 molecule represents a key enzyme in biosynthesis of the prostanoids (prostaglandins, prostacyclins and thromboxanes). COX-2 acts both as a dioxygenase, and a peroxidase. Overall, the cyclo-oxygenase (COX) enzymes, COX-1 and COX-2, play critical roles in the biosynthesis of prostaglandins from arachidonic acid [11]. Thus, are two isozymes of COX: a constitutive COX-1 and an inducible COX-2, which differ in their regulation of expression and tissue distribution. The human COX-1 protein is constituitively expressed in most tissues, and functions in the maintenance of tissue homeostasis. Human COX-2 shows 86-89% amino acid sequence identity with mouse, rat, sheep, bovine, horse and rabbit COX-2 proteins, respectively. Human COX-2 is expressed in a limited number of cell types and regulated by specific stimulatory events, suggesting that it contributes to prostanoid biosynthesis involved in inflammation and mitogenesis [3]. Human COX-2 is encoded by the PTGS2 gene. Moreover, nonsteroidal anti-inflammatory drugs are effective in decreasing the inflammatory response, by blocking both COX isoenzymes [12]. In addition, previous authors have investigated the role of COX isozymes in the functioning of cell types involved in the lupus autoimmune response. These authors examined the therapeutic effect of COX-2 inhibitors in mice prone to spontaneously developing SLE [12, 13]. In their results, treatment with COX-2 inhibitors resulted in 1) decreased autoantibody production and 2) inhibition of the T cell response to the major lupus autoantigen, nucleosome, and its pathophysiologic presentation by antigen-presenting cells. Surprisingly, a significant increase in survival occurred only in mice receiving intermittent therapy with the lowest dose of celecoxib [12, 13]. The authors concluded that the major players in the lupus pathogenic autoimmune response, namely, hyperactive T cells, B cells, dendritic cells, and macrophages, depend on an increased expression and activity of COX-2 in target organs. Discussion DLE is an autoimmune disease. The presence of ZAP-70, HLA-DPDQDR and COX-2 in skin biopsies from patients affected by this disease has never been reported in the medical literature [1, 2]. Of interest, our staining results for another cell signaling molecule, the linker for activation of T cells (LAT) were negative. LAT is a transmembrane adaptor protein that plays an essential role in T cell receptor (TCR) signal transduction pathways. LAT is phosphorylated on multiple tyrosine residues upon TCR engagement, recruits several important signaling proteins to the cell membrane, and functions as a scaffold for the assembly of numerous signaling complexes. In this study we confirmed the diagnosis of DLE by H&E staining, and established the typical BMZ lupus band by DIF. In addition, we demonstrated pericytoplasmic and perinuclear reactivity within epidermal keratinocytes with selected antibodies. The primary function of the HLA-DP, DQ and DR molecules is to present antigenic peptides, mostly of an exogenous nature, to T lymphocytes. HLA molecules are associated with a variety of autoimmune and non-autoimmune diseases, and aid in restricting the antibody response to certain antigens. HLA-DP, DQ and DR molecules are expressed on antigen-presenting cells such as B lymphocytes, monocytes and dendritic cells, but can also be detected on cytototoxic/suppressor T lymphocytes and activated granulocytes. HLA class II expression can also be induced on cells and tissues such as fibroblasts and endothelial cells as a result of activation by certain cytokines such as γ-interferon, tumor necrosis factor and interleukin-10 [3]. We have also demonstrated that HLA-DPDQDR is highly expressed in tumid lupus [3, 4]. As shown in this study, other authors have found that in Japanese patients affected by DLE and systemic lupus erythematosus (SLE), the HLA-DRB1*1501 carrier phenotype has a statistically significant association with these disorders [8]. We conclude that in our patient with active DLE, strong expressions of ZAP-70, COX-2 and HLA-DPDQDR are present in the inflammatory areas. These markers could play significant roles in this autoimmune disorder, specifically in the maintenance and regulation of specific stimulatory events affecting the biosynthesis of prostanoids involved in inflammation and mitogenesis. We also tested for the presence of ZAP-70, a tyrosine kinase of the Syk family. The ZAP-70 protein plays a critical role in triggering the signaling cascade in response to T-cell receptor stimulation [8-10]. ZAP-70 is primarily 253 www.najms.org North American Journal of Medical Sciences 2011 May, Volume 3. No. 5. Further studies are warranted to investigate these possibilities, and also to assess the therapeutic efficacy of ZAP-70 and COX-2 inhibitors in lupus erythematosus. 8. Acknowledgments The authors thanks Jonathan S. Jones HT (ASCP) for his excellent technical work. All work was performed with funds from Georgia Dermatopathology Associates (GDA). 9. References 1. 2. 3. 4. 5. 6. 7. Walling HW, Sontheimer RD. Cutaneous lupus erythematosus: issues in diagnosis and treatment. Am J Clin Dermatol 2009;10:365-381. Sepehr A, Wenson S, Tahan SR. Histopathologic manifestations of systemic diseases: the example of cutaneous lupus erythematosus. J Cutan Pathol 2010; 37: 112-124. Pathophysiology of Cutaneous Lupus Erythematosus. In: Daniel Jeffrey Wallace, Bevra Hahn, Edmund L Dubois eds. Dubois lupus erythematosus. Seventh ed. Baltimore, MD. Lippincott Williams & Wilkins. 2006: 566-567. Abreu Velez AM, Howard MS, Loebl A. Autoreactivity to sweat and sebaceous glands and skin homing T cells in lupus profundus. Clin Immunol 2009;132: 420-424. Abreu Velez AM, Smith JG Jr, Howard MS. Vimentin compartamentalization in discoid lupus. North Am J Med Sci. 2010; 2: 106-110. Abreu Velez AM, Girard JG, Howard MS. J. Antigen presenting cells in a patient with hair loss of and systemic lupus erythematosus. North Am J Med Sci 2009;1: 205-210. Abreu Velez AM, Smith JG Jr, Howard MS. 10. 11. 12. 13. 254 Cutaneous lupus erythematosus with autoantibodies colocalizing with glial fibrillary acidic protein. N Dermatol Online 2011; 2: 8-11. Furukawa F, Yamamoto Y, Kanazawa N, Muto M. Race differences in immunogenetic features and photosensitivity of cutaneous lupus erythematosus from the aspect of Japanese studies. Ann N Y Acad Sci 2009;1173: 5552-5556. Januchowski R, Wudarski M, Chwalińska-Sadowska H, Jagodzinski PP. Prevalence of ZAP-70, LAT, SLP-76, and DNA methyltransferase 1 expression in CD4+ T cells of patients with systemic lupus erythematosus. Clin Rheumatol 2008;27: 21-27. Crespo M, Villamor N, Giné E, et al. ZAP-70 expression in normal pro/pre B cells, mature B cells, and in B cell acute lymphoblastic leukemia. Clin Cancer Res 2006;12: 726-734. Goda S, Quale AC, Woods ML, Felthauser A, Shimizu Y. Control of TCR-mediated activation of beta 1 integrins by the ZAP-70 tyrosine kinase interdomain B region and the linker for activation of T cells adapter protein. J Immunol 2004.172: 5379-5387. Zhang L, Bertucci AM, Smith KA, Xu L, Datta SK Hyperexpression of cyclooxygenase 2 in the lupus immune system and effect of cyclooxygenase 2 inhibitor diet therapy in a murine model of systemic lupus erythematosus. Arthritis Rheum 2007; 56: 4132-4141. Bingham S, Beswick PJ, Blum DE, et al. The role of the cylooxygenase pathway in nociception and pain. Semin. Cell Dev Biol 2006; 17: 544–554.