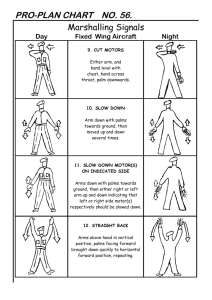
Table 2.3 The 5-min neuro exam
advertisement

Table 2.3 The 5-min neuro exam Feature evaluated How to check General health General appraisal of overall assessment appearance Vital signs What to look for and questions to ask Does the patient look acutely ill? Abnormal vital signs (e.g., elevated temperature, hypotension, tachycardia) often suggest systemic illness General neuro assessment Observe the patient walking, if they are able to do so. Also observe sitting/lying posture in patients who are unable to get out of bed For patients who are able to walk: does the patient move symmetrically, with similar movements of the arms and legs on both sides of the body? Does the patient walk with her feet close together, turn easily, and walk in a straight line OR do you see signs of imbalance? For patients observed when sitting: do they easily sit upright or do they tend to lean or fall to one side? Do they hold their arms and legs in a similar posture and move them symmetrically while sitting? Cognitive assessment This should be performed as part of the history Was the patient able to complete paperwork during their intake, showing an ability to read, write, and manipulate a pen? Can the patient speak fluently with good use of language? Can the patient tell a coherent story? Does the patient answer your questions well OR is she confused, disoriented, lethargic, or easily distracted? Eye grounds/ fundoscopic evaluation Fundoscopic examination Look for papilledema to suggest increased intracranial pressure. Vascular constriction or nicking or the presence of hemorrhages or yellowish exudates suggests hypertension. Venous pulsations, when present, are a sign of normal intracranial pressure; venous pulsations may be absent when pressure is normal or abnormal Cranial nerve assessment Cranial nerve testing can be mainly performed during history taking. Check visual fields by asking the patient to look at your nose while you wiggle fingers held with your arms held out at the side and placed about equal distance between you and the patient Watch the patient’s eye and facial movements for symmetry while the patient is talking to you. Assuming you don’t have a problem with your visual fields, both you and the patients should be similarly able to see fingers wiggling on both sides during visual field testing (continued) Feature evaluated How to check What to look for and questions to ask Extremity testing Observe the patient’s resting Patients who equally position and move for strength posture and casual moveboth arms and legs will usually have a and sensation ments during history taking. normal motor screening examination. Test muscles in both the If you see differences during casual proximal and distal arm and observation, spend more time leg on both sides for carefully testing strength and reflexes. strength. Tap reflexes at the Look for evidence of symmetrical elbows and knees. Stroke the responses to both motor and sensory bottom of the foot for a testing. An up going toe on Babinski Babinski response. testing may suggest an upper motor Lightly stroke both sides with neuron (e.g., brain or spinal cord) your fingers and an open lesion and the need for additional safety pin to test sensation. testing. Watch patients as they reach for and manipulate items in their environment to notice fine motor skills and coordination