Document 13959447
advertisement

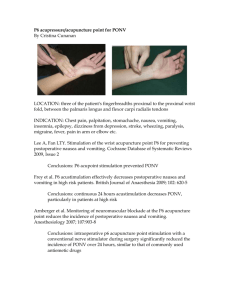
Contemporary OB/GYN April, 2000 Management of nausea and vomiting in pregnancy: alternative therapies. Author/s: Ronald A. Chez Years ago, I used to prescribe Bendectin as often as I did prenatal vitamin pills. Now, I half-heartedly prescribe other medications for "morning sickness" since they don't really seem to work. And for a large dose of humility, about twice a month, when I admit someone for hyperemesis, I struggle to write pseudo-intelligent orders without all that much rhyme or reason. Worse, I have several teleological explanations for why pregnant women suffer from nausea and vomiting, none of which is scientifically proved. One impressive thing about complementary and alternative medicine is that it can be a fallback when my training doesn't seem to help ameliorate my patient's nausea plus or minus vomiting. Although this treatment, in general, is not much more successful than traditional methods, it does provide patients with another option. It also buys me tincture of time until that magic week 12, 13, 14, or even 16 when the symptoms subside for most women. What follows is the second of two interviews with clinicians who are real authorities on nausea and vomiting. Last month, Jennifer R. Niebyl, MD, discussed traditional therapy. In this issue, Patricia Murphy, CNM, DrPh, OB/GYN Nurse Practitioner, discusses alternative therapies. Although it initially appears that they have different approaches to therapy, both share a focus on providing comprehensive, supportive, and individualized care until they find something that works for a particular patient. Chez: Dr. Murphy, you recently published a review of the literature on the use of alternative therapies for nausea and vomiting in pregnancy. [1] How do you define alternative therapy? Murphy: Basically I consider the term to apply to anything that is an alternative to standard treatments and conventional medicine, which include pharmaceutical prescriptions and dietary advice. Alternative therapies for nausea and vomiting include herbal medicines and other forms of treatment, such as acupuncture and homeopathy. Chez: One of the focuses of your review was efficacy. Please relate your general considerations and your conclusions in that area. Murphy: I was concerned about the abundance of recommendations with very little other than anecdotal support for their effectiveness in alleviating the symptoms of nausea and vomiting. As I looked further, it became clear that there were very, very few clinical trials that actually compared alternative remedies in terms of their outcomes. Part of the difficulty in doing research and assessment in this area is the fact that many women use multiple remedies for relief, nausea and vomiting itself is difficult to measure in terms of outcomes, and it is very difficult to develop an appropriate placebo for many of the alternatives. Finally the condition itself is self-limiting and it tends to get better over time, with or without treatment. Acupuncture and acupressure Chez: The NIH Consensus Development Conference on Acupuncture in 1997 included positive comments on the use of acupuncture or acupressure for postoperative nausea and vomiting, chemotherapy-induced nausea and vomiting, nausea of pregnancy, and postoperative dental pain. [2] Your review focused on that particular modality. Do you differentiate between acupuncture and acupressure? Murphy: In terms of the studies that have been done for nausea and vomiting of pregnancy yes, I do differentiate between the two. Many people think of acupuncture as placing needles into specific acupuncture points. But in fact, most of the studies on this modality for treatment of nausea and vomiting in pregnancy have looked at acupressure, a noninvasive method that places pressure over acupuncture points but does not use needles. Acupressure can be done manually by the woman simply applying pressure over the points herself, or with the use of wrist bands that are designed to be continuously to put pressure over these same acupressure points. Is there more than one point for nausea? If so, where are these points located and what are their names? Murphy: There may be several points that are used for relief of nausea and vomiting, but the one that has been studied for the condition in pregnancy is the P6 point, also called the Neiguan pressure point (Figure 1). It is on the volar surface of the forearm, about three fingerbreadths from the distal wrist crease and between the two tendons. Chez: How many reports did you analyze as part of your review? Murphy: I looked at a number of reports, from both controlled and uncontrolled trials. I focused mostly on seven controlled trials in my literature review. All of them varied in terms of study design and measurement of outcomes. Treatment was administered for different periods of time and the approaches to control groups varied. Six of the seven studies found a pronounced, beneficial response to acupressure with improvement in nausea and vomiting in pregnancy. Some of these studies used manual acupressure, whereas others involved use of a commercial wristband. The largest study of acupressure, however, which was done in Canada, found no effect at all. [3] So the evidence might best be characterized as equivocal when looking at the controlled trials as a whole. Chez: Was there a difference in the efficacy related to nausea versus that related to vomiting per se? Murphy: Some of the studies looked primarily at nausea and others looked at vomiting. There were variations in the responses. Some showed efficacy for nausea, but not for vomiting. Chez: How cost-effective and acceptable is acupressure? Murphy: Regarding clinical value, my assessment is that it definitely does work for a number of women. In terms of cost-effectiveness, manual or even wristband acupressure is extremely cheap. It can be taught as a manual technique, or the wristbands can be bought at low cost. It may very well provide a moderate degree of relief. I didn't find any controlled clinical trials of acupuncture for nausea and vomiting in pregnancy, although I know there is one ongoing in Australia. The difference with acupuncture is an increase in both financial and temporal costs because the woman would need to find a qualified acupuncturist and probably make a number of visits in order to have her symptoms alleviated. Chez: Have you had any experience with the Relief Band device recently put on the market? It's a prescription item that is placed very close to the P6 point. It is battery operated and provides continuous sensory afferent, electric stimulation with the intensity of the impulse controlled by the patient. Murphy: I am familiar with the device, although I don't have any clinical experience with it. Relief Band is relatively new in the market and most of the women I care for are in a lower-income bracket and can't afford to purchase the device. I believe it was used in the study by Evans that is included in my review. [4] In a review of acupuncture for treatment of nausea and vomiting, Vickers identified P6 as the key point used in the Evans study. Chez: The only article I found on use of Relief Band was a report that involved only 27 patients. [6] Perhaps more information is forthcoming. Hypnotherapy Moving to another modality, what about hypnosis or hypnotherapy? Did you find any randomized trials of that treatment, and if so, what is your impression? Murphy: Although there were a number of case reports and case series on hypnotherapy in the literature, I didn't find any controlled clinical trials of the treatment. Most of the articles involved severely ill women, many of whom did show some benefit. My concerns were that in the absence of controlled trials, it was difficult to assess whether hypnotherapy was beneficial above and beyond the emotional support and the passage of time during the course of therapy. Practically speaking, the concerns faced by an obstetrician/gynecologist who wants to prescribe hypnotherapy for a patient are the need to find a qualified practitioner and the cost to the woman to travel to and from the therapist's office. Chez: When I was in training many years ago, there was a strong belief that nausea and vomiting in pregnancy had a psychiatric derivation or at least involved somatization of the psyche on the patient's part. Is there any reason to believe that some variant of behavior modification, such as group therapy, counseling, or even reading patient education booklets, has any value at all in this area? Murphy: Again, there are some case reports and case series in the literature that have looked at modalities like stimulus control, imagery, relaxation training, and behavioral modification in the management of nausea and vomiting in pregnancy. Like the studies on hypnotherapy, case series are difficult to evaluate as to their efficacy in the absence of a control group. In reading a number of these studies, however, it seemed to me that clinicians essentially already use many of these treatments. For example, stimulus control, or avoidance of obnoxious smells and cooking, often is recommended to pregnant patients with nausea. To be more formal, referral to a therapist for behavior modification courses and group support may be of help to some women. But again, we need to consider the cost to the patient in terms of travel, time, and money to access these therapies. Dietary remedies Chez: Ginger products are part of the folk medicine lore for nausea. Some practitioners advise patients to drink ginger ale or nonalcoholic ginger beer and eat pickled ginger, ginger preserves, or candied ginger. Are there any reports about ginger in the literature? Murphy: I did find one study that looked at hospitalized women with hyperemesis gravidarum and used a total dose of approximately 1 g of ginger per day, compared with a lactose placebo. [7] The treatment group showed significant improvement, with significant reduction in symptoms. It is interesting because ginger is an herb used traditionally across cultures for nausea and vomiting of many types. There have been other studies that show it is effective in treating nausea and vomiting associated with chemotherapy and motion sickness. Chez: Should I have any hesitancy in recommending ginger? I am asking the question because there are reports of its theoretical effect on thromboxane synthetase activity, testerone-receptor binding, and sex steroid differentiation of the fetal brain. [8] It strikes me, however, that there never has been interdiction of ginger in any of the literature from the FDA or the US Pharmacopeia, and as you say, in a number of cultures, ginger is part of the daily diet. What do you think? Murphy: I am familiar with the hypothesis that was raised about ginger possibly having adverse effects on the fetus. It is also of interest to note that the German Commission E monographs express a caution about the use of ginger in pregnancy. Some of that may be dose related. Some of the contraindications about ginger come from Chinese medicine, where it is viewed with caution in pregnancy but used at higher doses than in the Fischer-Rasmussen study and typically found in food sources in this country. [7] According to a newsletter on the medical use of herbs, ginger doses in Chinese medicine may range from 3 to 12 g per day. [9] In contrast, the Fischer-Rasmussen study used about 1 g per day. The amounts typically found in food also are low For example, a cup of ginger tea may contain about 250 mg, a heavily spiced dish may have 500 mg of ginger, and an 8-ounce glass of ginger ale or beer may have up to 1 g. [9] The concerns about possible fetal damage are hypothetical, and there are no studies in the litera ture that either support or refute this theory. Chez: What advice do you give patients about making ginger tea? Murphy: First, I suggest that they buy ginger tea bags, which are a form of preparation that is familiar to and easy for most women. For those who are more interested in the whole concept of using botanical remedies, I might recommend making tea by grating fresh ginger root into boiling water. Eating candied or crystallized ginger is a pleasant way for some women to try using this remedy Chez: What about other teas? There are teas available that are made from raspberries, peppermint, spearmint, fennel, anise, and chamomile. Are there any clinical studies on these teas or do you have any contradictory information on their safety in pregnancy? Murphy: No. Unfortunately, I found no clinical studies for any of the multiple types of herbs that are used in teas. Commonly used herbal teas, in preparations such as home brewed teas and not medicinal tinctures, are probably fine because they would be essentially food sources of the herb. There is no scientific evidence of efficacy. Homeopathy Chez: Homeopathy would be another potential remedy. It would seem to me that Nux Vomica, Pulsatilla, or Ipecac as homeopathic preparations might be appropriate for someone who already had nausea and was vomiting. Again, considering the small number of molecules in any of these substances, is safety an issue and, more pertinent, is there any reason to believe they may work? Murphy: I am also fascinated by the concept of using homeopathic treatments simply because of the apparent lack of potential harm, given the small number of molecules. One of the issues with homeopathy though, is that the treatment is highly individualized, and although there are a number of homeopathic treatments for nausea and vomiting, according to homeopathic theory, only one treatment would be appropriate for a particular person. It makes it difficult to do studies of this topic, although such studies would be of great interest. A patient scenario Chez: Let's talk now about how you would handle a particular patient. This scenario involves a woman who is 7 weeks' pregnant and nauseated to the point that she is missing work; she vomits at least once a day What general instructions would you give this patient? Murphy: Like most clinicians, I start out with the essential reassurance that the situation will get better over time. I assess what the patient is already doing so that I don't reiterate advice that has not worked for her yet. I may uncover some things that she is doing that she should not be, such as borrowing a friend's motion sickness patch. The first step is usually common sense diet advice and stimulus control, in terms of avoiding the things that make her nauseated. I would encourage the patient to eat whatever she is able to eat. Although we do stress good nutrition in pregnancy, at this point, I think keeping hydrated and fed is more important than what the woman eats. I emphasize rest because I think fatigue makes the problem worse in a lot of women. I try to assess what is done in the patient's family and her culture for nausea and vomiting, because I prefer to find remedies that are familiar to her and perhaps psychologically comforting. Beyond that, I offer a grab bag of advice. As I present each recommendation to a patient, I try to make an assessment as to whether she seems interested or whether it's something she would not consider. My advice includes things like acupressure, adding some Vitamin [B.sub.6] to her remedies, some ginger tea, some of the herbal teas. I may suggest a syrup like Emetrol and I will sometimes discuss "home-made Bendectin" (a combination of over-the-counter Unisom and pyridoxine). If these don't work, I will discuss the benefits and risks of pharmaceutical antinausea alternatives that might help, and try to get a sense if the idea of medication is acceptable to the patient or not. I try to work in a stepwise fashion, assessing at each point whether she is getting better. Chez: Once in awhile, a patient will tell me that potato chips do the trick for her nausea, or dill pickles. Others tell me that fireball candies work. Are we dealing with a true "pharmacologic", effect, or are we dealing with patients who just have cravings and that is why they are nauseated? Murphy: I don't know. I often share with patients that the only thing that got me through the first trimester of my first pregnancy was drinking flat cola. I go on to explain that this was probably because when we were children, my parents gave us Coca-Cola syrup for nausea. So this remedy was both familiar and psychologically comforting for me. Sometimes a woman's cravings are related to a folk remedy used by her family. I may also tell a patient about my friend who made it through her first trimester on a diet of spicy, red-hot chicken wings because that seemed to help her. The point is that some things work for some people, and we just need to find what will work for the patient. Focusing on food that has a different taste- whether it's very salty very spicy or very hot- really does seem to help some people. To be honest, though, the thought of it makes me ill! Chez: Thank you. Dr. Chez is Professor of Obstetrics and Gynecology, College of Medicine, and Professor of Community and Family Health, College of Public Health, University of South Florida, Miami, Fla. Dr. Murphy is Associate Research Scientist, Department of Obstetrics and Gynecology and Center for Complementary and Alternative Medicine Research in Women's Health, Columbia University College of Physicians and Surgeons, New York, N.Y. REFERENCES (1.) Murphy PA. Alternative therapies for nausea and vomiting of pregnancy. Obstet Gynecol, 1998;91:149-155. (2.) NIH Consensus. Statement on Acupuncture. November 1997. http://odp.nih.gov/consensus/statements. (3.) O'Brien B, Relyea, MJ, Taerum T. Efficacy of P6 acupressure in the treatment of nausea and vomiting during pregnancy. Am J Obstet Gynecol. 1996;1 74:708-715. (4.) Evans AT, Samuels SN, Marshall C, et al. Suppression of pregnancy Induced nausea and vomiting with sensory afferent stimulation. J Reprod Med. 1993:38:603606. (5.) Vickers AJ. Can acupuncture have specific effects on health? A systematic review of acupuncture antimesis trials. JR Soc Med. 1996;89:303-311. (6.) Evans AT, Samuels SN, Marshall C, et al. Suppression of pregnancy induced nausea and vomiting with sensory afferent stimulation. J. Reprod Med. 1993:38:603606. (7.) Fischer-Rasmussen W, Kjaer SK, Dahi C, et al. Ginger treatment of hypermesis gravidarum. Eur / Obstet Gynecol Reprod Biol. 1990:38:19-24. (8.) Backon J. Ginger: inhibition of thromboxane synthetase and stimulation of prostacyclin: relevance for medicine and psychiatry. Med Hypotheses. 1986:20:271278. (9.) Bergner P. Is ginger safe during pregnancy? Medical Herbalism. 1991 3(3):7.

![Questionnaire used in the study Demographics GENDER: M [ ] F](http://s3.studylib.net/store/data/006712173_1-21c851410b04058d524e1b79e54e32b0-300x300.png)