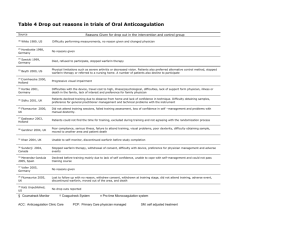
Management of Anticoagulation Therapy in the Perioperative Period

Management of Anticoagulation
Therapy in the
Peri-operative Period
J. Christian Barrett, MD
Assistant Professor, Division of Hematology-Oncology
Virginia Commonwealth University
Management of Anticoagulation
Therapy Peri-operatively
• What are the issues?
– Risk of thrombosis vs.
bleeding
• Variable indications for the therapy
• Variable procedural risks
– Reversal of Therapy
• Lack of conclusive evidence
HEMORRHAGE
•Major bleeding
•9-13% fatal
•Rarely disabling
Weighing the Risks
THROMBOSIS
•Venous
•5-10% fatal
•<5% disabling
•Arterial
•20-40% fatal
•20-50% disabling
Case #1
• 70 year old male with a history of atrial fibrillation and CHF (EF 30%) on chronic warfarin therapy with a therapeutic INR of
2.4
• Going for a routine screening colonoscopy
• Asks what he should do with his warfarin for the procedure.
Thrombotic Risk:
Non-Valvular Heart Disease
• Non-valvular Atrial Fibrillation
– 4.5% per year risk of arterial thromboembolism (range
1-20% based on individual risk factors)
– Warfarin reduces risk by 66%
• Left Ventricular Dysfunction
– 18% increase stroke risk for every 5% decrease in LV
EF
– Warfarin reduces risk by 81%
– Aspirin reduces risk by 56%
Archives Internal Medicine 1994;154:1449
Colonoscopy Risk?
• American Society for Gastrointestinal Endoscopy
Guidelines…
– Low-risk procedures
• EGD, Flex sig, and colonoscopy with/without biopsy
• EUS and push enteroscopy
• ERCP and biliary stent placement without sphincterotomy
– High-risk procedures
• Gastric (4%) or colonoscopic (1%-2.5%) polypectomy
• Laser ablation and coagulation (<6%)
• Endoscopic sphincterotomy (2.5%-5%)
• EUS-guided biopsy
• Percutaneous gastrostomy
• Stricture dilation
ASGE Guideline
• Recommendation for low risk procedure: No adjustments in anticoagulation need be made irrespective of the underlying condition.
• Recommendation for high risk procedure:
Warfarin should be discontinued 3-5 days before the scheduled procedure.
– In patients, with high risk conditions, bridging with heparin or LMWH may be individualized.
– If to resume after procedure, heparin may resume 2-6 hours after procedure and warfarin that night.*
*extra caution if s/p sphincterotomy where major hemorrhage risk is 10%-15% if reinstituted within first 3 days (or if s/p large sessile polyp removal where caution in order up to 2 weeks.)
Polypectomy Risk
• Retrospective review of 6617 colorectal polypectomies in 3138 consecutive patients
– Delayed hemorrhage defined as bloody feces reported on >2 occasions
• 37 patients (1.2%) or 38 polypectomies (0.57%)
• At second endoscopy, 15 patients had stopped and 22 patients required endoscopic hemostasis.
• Only 1 patient required blood transfusion
– Anticoagulation use was prohibited for 7 days postprocedure per the protocol
Watabe H et al. Gastointest Edosc 2006;64:73-78
Polypectomy Risk
• Multivariate analysis
– Polyp-related factors
• Polyp size >1 cm (OR 4.5 with 95% CI 2.0-10.3)
– Patient-related factors
• Hypertension control (OR 5.6 with 95% CI 1.8-17.2)
– Associated with a longer interval of recognition of bleeding
Polypectomy on Anticoagulation
• Retrospective review of 1657 consecutive patients with colonoscopic polypectomy
– Immediate hemorrhage defined as bleeding sufficient to require endoscopic interventions judged by the endoscopist
• 32 patients (1.9%)
• 31/32 were classified as MILD (drop<4 g/dL and no blood)
– Delayed hemorrhage defined as rectal bleeding within
30 days of procedure of sufficient severity to require hospitalization for management
• 5 patients (0.3%)—all transfused
• Did not report warfarin use specifically among this subgroup
Hui AJ et. Gastrointest Endosc 2004;59:44-48
Polypectomy on Anticoagulation
• Among those with bleeding …
– No difference seen related to anti-platelet agent use
– Warfarin use was significantly associated with risk of hemorrhage (p<0.001)
• 4 patients (10.8%) among the 37 with hemorrhage
– Median INR 1.41 [range 1.09-2.86]
• 13 patients (0.8%) among the 1620 without hemorrhage
– Median INR 1.38 [range 1.08-1.84]
Polypectomy on Anticoagulation
• Retrospective review of 21 patients undergoing 41 colonoscopic polypectomies
– Held warfarin evening before procedure only
• Median INR 2.0 [range 1.4-4.9]
– Polypectomy with prophylactic clips if <1 cm
• No concomitant anti-platelet agent use
• No immediate hemorrhage (all <10 mL)
• No delayed hemorrhage reported at follow-up (3-8 weeks)
Friedland and Soetikno. Gastrointest Endosc 2006;64:98-100
Cataract Surgery on
Anticoagulation
• Reviewed medication use among 19,282 cataract surgeries on a RCT
– 4588 patients used aspirin (23.8%)
• 13.8% advised to stop use before the procedure
• 22.5% actually did so
– 752 patients used warfarin (3.9%)
• 10.5% advised to stop use before the procedure
• 28.3% actually did so
Katz J et al. Ophthalmology 2003;110:1784-1788
Cataract Surgery on
Anticoagulation
• Among the aspirin users …
– No difference seen in ocular hemorrhage events
• 0.56% among those with no routine use
• 0.59% among those who continued aspirin
– Increased incidence of medical events seen …
• Myocardial Infarction
– 0.84% among those with no routine use
– 4.16% among those who continued aspirin
• TIA
– 0% among those with no routine use
– 1.19% among those who continued aspirin
Cataract Surgery on
Anticoagulation
• Among the warfarin users …
– No difference seen in ocular hemorrhage events
• 0.55% among those with no routine use
• 0% among those who continued warfarin
– Increased incidence of medical events seen …
• Myocardial Infarction
– 1.43% among those with no routine use
– 5.7% among those who continued aspirin
Recommendation
• Minor procedure: Should be able to proceed without any adjustments in anticoagulation perioperatively
– If endoscopist unwilling, hold warfarin for 3-4 days before procedure and resume warfarin same day without use of heparin
– If polyp found, second procedure could be scheduled off warfarin
• Though some data suggests may be safe to proceed at initial procedure if <1cm, small numbers and unconfirmed.
Case #2
• 44 year old female with a St Jude (bileaflet) mitral valve on warfarin with an INR of 2.9
(goal 2.5-3.5)
• Is scheduled to have a laparoscopic cholecystectomy
• Asks what she should do with her anticoagulation therapy for the surgery.
Thrombotic Risk:
Valvular Heart Disease
• 4% per year risk of major* arterial thromboembolism with a mechanical valve
– plus 1.8% per year risk of valve thrombosis
• 2.2% per year with antiplatelet therapy
– plus 1.6% per year risk of valve thrombosis
• 1% per year with warfarin
• 0.8% per year with an aortic valve
• 1.3% per year with a mitral valve
– plus 0.2% per year risk of valve thrombosis
* major=death, neurologic deficit or requiring surgery
Cannegieter SC et al. Circulation 1994;89(2):635-41
ESC Guidelines
• Recommendation for low risk procedure: No adjustments in anticoagulation need be made.
• Recommendation for high risk procedure:
Warfarin should be discontinued 3-4 days before the scheduled procedure.
– In patients, with high risk factors for thrombosis, bridging with heparin* is recommended stopping 4 hours before the procedure.
– After procedure, heparin* may resume within 6-12 hours after procedure and warfarin as soon as possible.
*
LMWH is not included in the ESC guidelines
High Risk Factors
• Mechanical valve in the mitral position
• High risk prostheses
– Starr Edward, Lillehei Kaster, Omniscience
• Atrial fibrillation
• LVEF < 30%
• Prior thromboembolism
• Hypercoagulable state
• Surgery for malignancy or infection
Bridging with Heparin
• Refers to the use of therapeutic doses of
UFH or LMWH to cover the interval when warfarin dosing is subtherapeutic
• LMWH has been demonstrated to be costeffective in cost models compared with
UFH
• Data is limited
Bridging Heparin:
Preoperative Planning
• UFH
– Start 36-60 hours after last warfarin dose
– Stop 6 hours before surgery
• LMWH
– Once or twice daily dosing starting 36 hours after last warfarin dose
– Stop before surgery…
• >18 hours with twice daily dosing
• >30 hours with once daily dosing
Heparin Bridging
Postoperative Planning
Additional factors to consider …
1.
Post-operative risk of thrombosis (venous not arterial risk increased)
2.
Post-operative bleeding risk*
• UFH
– No load and not greater than 18 u/kg/hr starting
~12 hours post-op
– 1 st PTT 12hours after start infusion
• LMWH
– Start ~24 hours after surgery
• If thrombosis risk is high can consider starting prophylactic dosing within
12 hours and “step up” the next day
*If the operative bleeding risk is moderate or high, consider prophylactic dosing instead of full bridging doses.
Recommendation
• High risk of arterial thrombosis with a minor surgical bleeding risk
– Stop the warfarin 5 days before the surgery
– Start therapeutic dose LMWH with the AM dose 3 days before surgery
– Stop LMWH after the AM dose day before surgery
– Resume therapeutic dose LMWH the next day along with the warfarin at prior steady state dose
– Stop LMWH once INR >2 on 2 consecutive days
Case #3
• 59 year-old female with a history of …
– DVT following her 2 nd pregnancy at age 35 treated
– DVT with PTE at age 55 years at which time noted to be heterozygous for FVL
– On chronic anticoagulation since the 2 nd event with an INR 2.6
• Scheduled for a right-sided hemicolectomy
(non-malignant indication)
Thrombotic Risk:
Venous Thomboembolism
• Risk reduces with longer duration of warfarin
– 50% risk of recurrence within three months without anticoagulation
• 40% risk during the first month
• 10% risk during the next two months
– 5% after three months of anticoagulation
• 10-15% per year risk of recurrence among those with history of recurrent venous thrombosis without continued anticoagulation
Venous Thrombosis
• Pre-operatively
– Time from prior venous event
– Time of surgery
– Mobility of the patient
• Post-operatively
– Time from prior venous event
– Operative risk of thrombosis
– Operative risk of hemorrhage
Venous Thrombosis
• Pre-operative recommendation
– Stop warfarin 4-5 days before the surgery with no bridging or prophylactic dosing of heparin
• Post-operatively recommendation
– Prophylactic dose LMWH and steady state dose of warfarin starting 12-24 hours after surgery if hemostasis achieved and continued until warfarin is therapeutic
Case #4
• 38 year-old male discharged 8 days ago following a DVT returns off LMWH on warfarin with an INR of 3.2 with a gun shot wound requiring emergent exploratory surgery of the abdomen. Surgeons are lining up the OR and asking for recommendations.
Warfarin Reversal
• Warfarin Discontinuation
• Vitamin K
• Fresh Frozen Plasma
• Recombinant VIIa
Warfarin Discontinuation
• Wide variability—especially among elderly
• Generalizations to achieve INR <1.2 at surgery if steady state …
– INR 2-3 hold 4 doses preoperatively
– INR 3-4 hold 5 doses preoperatively
White RH et al. Annals of Internal Medicine 1995;122:40-42
Vitamin K
• Subcutaneous administration inferior to oral or IV which appear equivalent
• IV associated with a risk of hypotension and/or anaphylaxis
• Effects seen starting 12-24 hours after administration
Fresh Frozen Plasma
• Can be infused rapidly if patient can tolerate volume
• Cheaper and more widely/rapidly available at many centers than rVIIa
• Calculate dose to achieve prothrombin complex level of 40% normal plasma
– If subtherapeutic INR, 10mL/kg (3 units in 70 kg pt)
– If therapeutic INR, 25mL/kg (7 units in 70 kg pt)
– If supratherapeutic INR, 35mL/kg (10 units in 70 kg pt)
Recombinant Factor VIIa
• Warfarin reversal—not approved indication
• Candidates for consideration
– Life-threatening bleed with INR > 2.0 (+ INR >1.5 though Vit K / FFP preferable)
– Emergent surgery unable to be delayed 24+ hours
• Other factors to consider
– Fibrinogen > 120 mg/dL
– MI/angina/stroke ongoing or within prior 4 weeks
– Active DVT or other thrombotic disorder
• Optimal dose is uncertain
Recommendations
• Because of the emergent nature of surgery
– Hold warfarin
– Give dose of vitamin K (5-10mg orally or slow IV)
– Fresh frozen plasma 25-35 mL/kg or
Recombinant factor VIIa 10-20 mcg/kg (rounded to nearest full vial dose)
– IVC filter placed intraoperatively