Investigations • Innovation • Clinical Application
Optimizing Neurotherapy and Emerging Paradigm
for
Alzheimer’s Disease
The Current Foundation Role of Cholinergic Stimulation
of Alzheimer’s Disease—Focus on Evidence-Based
Management of Moderate and Severe AD
Program Chairman
MURRAY A. RASKIND, MD
Professor and Vice-Chairman
Department of Psychiatry and Behavioral Sciences
University of Washington School of Medicine
Director of the University of Washington Alzheimer’s Disease Research Center
Director of the VA Northwest Network Mental Illness
Research, Education and Clinical Center (MIRECC)
Program Faculty
Program Chairman
MURRAY A. RASKIND, MD
Professor and Vice-Chairman
Department of Psychiatry and Behavioral
Sciences
University of Washington School of
Medicine
Director of the University of Washington
Alzheimer’s Disease Research Center
Director of the VA Northwest Network
Mental Illness
Research, Education and Clinical Center
Seattle, WA
SANDRA E. BLACK, MD, FRCPC
Brill Chair in Neurology
University of Toronto, Sunnybrook
Health Sciences Centre
Toronto, Ontario Canada
JAMES E. GALVIN, MD, MPH
Professor of Neurology and Psychiatry
Director of Clinical Operations
Center of Excellence on Brain Aging
Director Pearl Barlow Center for
Memory Evaluation and Treatment
New York University Langone School of
Medicine
New York, NY
SERGE GAUTHIER, MD
Director of the Alzheimer’s Disease
Research Unit
McGill Centre for Studies in Aging
Professor of Neurology and Neurosurgery,
Psychiatry and Medicine
McGill University
Montreal, Quebec Canada
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Advances in Alzheimer’s Disease
Diagnostics and Therapeutics:
A Clinician’s Perspective
Program Chairman
MURRAY A. RASKIND, MD
Professor and Vice-Chairman
Department of Psychiatry and Behavioral Sciences
University of Washington School of Medicine
Director of the University of Washington Alzheimer’s Disease Research Center
Director of the VA Northwest Network Mental Illness
Research, Education and Clinical Center (MIRECC)
Questions
►
How can biomarkers help us diagnose AD and
estimate treatment response?
►
Do “disease modifying” anti-beta-amyloid (Aβ)
therapeutics modify AD progression?
►
Are cholinesterases “simply” symptomatic
drugs?
►
Can we find rational pharmacotherapies for
AD agitation/aggression?
Keeping Expectations Modest
►
If your primary goal is cure, switch to
ophthalmology or orthopedics.
►
Maintain quality of life and function
and relieving distress are important
accomplishments.
►
Slowing disease progression is a
primary goal.
Why Biomarkers?
►
Earlier diagnosis.
►
More precise monitor of the effect of
anti-amyloid therapeutics.
►
However, cognitive testing may still
be most sensitive measure of disease
progression.
AD Biomarkers
►
PET imaging of brain beta-amyloid protein in
aggregated form.
►
Cerebrospinal fluid Aβ and tau concentrations.
“Promise Seen for Detection
of Alzheimer’s”
Headline – New York Times June 23, 2010
This front page article discusses the development
and potential of PET Aβ imaging
Beta Amyloid PET Imaging Ligands
[11C] Pittsburgh Compound B (PIB)
Currently available, but short half-life
(20 minutes), requires close
proximity to cyclotron.
[18F] –AV-45
Approaching availability. Longer
half-life (10 minutes), enhances
availability.
Alzheimer’s Disease
Neuroimaging Initiative (ADNI)
►
PIB distinguishes AD from MCI from normals.
►
PIB highly correlated with CSF Aβ42.
►
But PIB and CSF Aβ42 not significantly
correlated with MMSE cognitive measure.
►
In 17 normal, 50 MCI, and 13 AD one-year
follow-up subjects: small, nonsignificant
changes in Aβ load.
►
However, some individuals had apparently
meaningful Aβ load increases.
Jagust WJ et al, Alzheimer’s and Dementia 6:221-229, 2010.
A Treatment Relevance Question
►
Does a drug that reduces [C-11] PIBmeasured Aβ load slow cognitive
decline?
►
If so, do beneficial cognitive effects
reflect Aβ load reductions?
The “Anti-Amyloid Antibody” Approach to
the Treatment of Alzheimer’s Disease
►
Transgenic AD mice show marked
reduction in amyloid plaque
deposition when actively immunized
against beta amyloid.
►
Active beta amyloid immunization in
humans produced apparent reduction
of amyloid plaque density; but no
clear cognitive benefits. 6% incidence
of meningo-encephalitis.
Would Passive Monoclonal Anti-Amyloid Antibody
Approaches be More Effective and Less Toxic?
Bapineuzumab: N terminus-directed beta amyloid
monoclonal antibody in clinical trials.
Primary efficacy outcomes in Phase 2 trial not significant.
Significant effect on ADAS-Cog in completers.
Signal for efficacy in E4 negative subjects.
Solanezumab: Mid domain-directed beta amyloid
monoclonal antibody in clinical trials.
No human trial results available.
Antibody design targets soluble beta amyloid.
Estimated Mean Change from Baseline on
ADAS-COG
ADAS-COG mITT
ADAS-COG Completers
2
2
0
Placebo
Bapineuzumab
0
-2
-2
-4
-4
-6
-6
-8
-8
-10
-12
Rx difference at week 78 = 2.3
P=0.078
0
11
24
37
50
63
Salloway S, et al. Neurology 2009; 73:2061-2070
-10
78
-12
Rx difference at week 78 = 4.3
P=0.003
0
11
24
37
50
63
78
Bapineuzumab Decreases
11C-PIB
Aβ Load
►
28 AD patients assigned to bapineuzumab
(n=20) or placebo (n=8).
►
Treatment with bapineuzumab for 78 weeks
reduced cortical 11C-PIB amyloid load
compared to baseline and placebo.
►
But, in this small subsample, effects on clinical
endpoints were disappointing and did not
appear related to effects on Aβ binding.
Estimated mean change from
baseline in mean C-PiB
Estimated Change from Baseline in
Mean C-PiB PET
0.4
Placebo
Bapineuzumab
0.3
0.2
0.1
0
-0.1
-0.2
Baseline
20
45
Week
Rinne JO , et al. Lancet Neurol 2010;9:363-72.
78
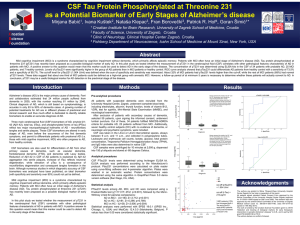
Potential Utility of CSF Biomarkers
A, Total Tau, and Phosphorylated Tau in Alzheimer’s Disease
►
Improving diagnostic accuracy.
►
Predictive value.
►
Monitoring treatment:
●
●
●
Alzheimer’s disease (AD)
Mild cognitive impairment (MCI)
Primary prevention
Neurochemical Changes in
Alzheimer’s Disease
phospho-tau
Neurofibrillary tangles
tau
Axonal damage
oxidation? isoprostanes
inflammation??
Amyloid
A42
A deposition/metabolism/clearance?
A42 is the Initiator and Main Culprit in Amyloid
Deposition, and Implicated in AD Pathogenesis
►
►
►
►
►
A42 is the initial amyloid
species deposited in brain.
A42 exceeds A40 in
amyloid deposits.
Toxicity and amyloid fibril
formation: A42>A 40.
in trisomy 21 and almost
all APP mutations.
Selectively in presenilin
mutations.
What Does Decreased CSF A42 Mean?
►
In Tg 2576 (APP-Swedish mutation) mice,
decreases in CSF A42 parallel increases in brain
A421.
►
In humans, inverse relation between in vivo
brain amyloid load (PIB binding) and CSF A42,
even in cognitively normal subjects2.
1Kawarabayashi
2Fagan
et al., J Neurosci 21:372-381, 2001.
et al., Ann Neurol 59:512-519, 2006.
Inverse Relation Between in vivo Amyloid
Imaging Load and CSF A42 in Humans
CSF Aß42 (pg/mL)
1000
750
500
250
0
0.0
0.5
Mean Cortical PIB Binding
(Binding Potential)
Fagan AM, et al., Ann Neurol 59:512-519, 2006.
1.0
CSF Total Tau in the Diagnosis of AD
CSF total tau is measured by a sensitive ELISA.
► Meta-analysis of AD versus controls:1
►
●
►
35 studies, 2315 AD; 1126 controls
In all studies, CSF T-tau in AD > normal controls
●
●
●
●
1Sunderland
2-3 fold increase in AD
Effect size = 1.31 (95% CI 1.23-1.39)
No correlation with age, dementia duration or
severity
Increases slightly with aging in normals
T, et al., JAMA 289:2094-2103, 2003.
Summary of CSF Biomarkers
►
CSF A42 is decreased and CSF tau
increased in 75-85% of patients with AD.
►
Changes in CSF A42 and tau are present,
but are less marked, in MCI than AD.
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Use of CSF Biomarkers for
Preclinical Diagnosis:
Where Do We Stand
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
CSF Tau: A42 Ratio for
Increased Risk of Mild
Cognitive Impairment:
A Follow-up Study
Li G, et al., Neurology 69:631-639, 2007.
Methods
►
Subjects:
●
●
●
●
►
129 controls aged 21-100
12 MCI
21 probable AD
12 other neurodegenerative disease
CSF collected between 0900-1100 hours
after overnight fast.
Li G, et al., Neurology 69:631-639, 2007.
Subject Characteristics and CSF
Biomarker Concentrations
Controls
< 65 yr
Controls
≥ 65 yr
MCI
AD
Other
81
48
12
21
12
M:F
41:40
22:26
8:4
10:11
7:5
Age
40 ± 15*
(21 – 64)
73 ± 7
(65 – 100)
71 ± 13
(49 – 82)
69±9
(52 – 87)
63 ± 11
18
14
50
72
---
RBC/l
7 ± 22
(0 – 176)
10 ± 28
(0 – 163)
10 ± 21
(0 – 58)
14 ± 39
(0 – 180)
8 ± 18
(0 – 83)
CSF A42
(pg/ml)
313 ± 14
386 ± 34
245 ± 41
225 ± 27*
332 ± 35
CSF tau
(pg/ml)
487 ± 24*
784 ± 49
1117 ±
115
1535 ±
131
769 ± 111
CSF P-tau181
(pg/ml)
97 ± 16*
248 ± 33
676 ± 125
936 ± 120
---
n
% APOE*4+
Li G, et al., Neurology 69:631-639, 2007.
High CSF T/A42 Ratio and
Conversion to MCI in 42 month F/U
►
Conversion to MCI over 42-months of followup in:
●
●
●
4/17 persons with high CSF T/A42 ratio
0/26 persons with normal CSF T/A42 ratio
Logrank test for survival curve, p<0.05
Li G, et al., Neurology 69:631-639, 2007.
Implications of High CSF T/A42 Ratio
►
The high CSF T/A42 subgroup of controls had
significantly increased risk of conversion to
MCI during 42 months of follow-up.
►
Suggests that high CSF T/A42 individuals had
“latent” AD at time of CSF collection.
Li G, et al., Neurology 69:631-639, 2007.
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Cross-sectional Lifespan
Study Suggests CSF A42
Concentration is Altered in
APOE*4 Carriers.
Peskind ER, et al., Arch Neurol 63:936-939, 2006.
CSF A42 and A40 in 184 Normal
Controls Aged 21-88
Peskind ER, et al., Arch Neurol 63:936-939, 2006.
A Sobering Finding
►
CSF A42 findings consistent with acceleration
by the APOE*4 allele of pathogenic A42
deposition starting in later middle life in
persons with normal cognition.
Peskind ER, et al., Arch Neurol 63:936-939, 2006.
Cholinesterase Inhibitor Clinical Experience and
Clinical Trials Support Reduction of AD Progression
►
Persistent treatment slows clinical progression.
►
Delayed start design: persons first on placebo
than switched to a cholinesterase inhibitor do not
“catch up.”
►
Increasingly divergent clinical status in long-term
trials favoring cholinesterase inhibitors.
►
Sounds like disease modification to me.
Persistent Treatment with Cholinesterase Inhibitors
and/or Memantine Slows Progression of AD
►
641 AD patients followed at Baylor College of
Medicine for over 20 years.
►
Persistent treatment with donepezil, other
cholinesterase inhibitors, and memantine
slowed AD progression assessed by multiple
cognitive, functional and global measures.
Rountree SD, et al. Alzheimers Res Ther 1(2):7, 2009
Galantamine Shows Sustained
Cognitive Benefits in AD Over 12 months
(including a delayed start time)
-4
Double-blind
Open-extension
in ADAS-Cog from baseline
Mean ( SE) change
-3
-2
-1
*# *p < 0.05 vs placebo/ Galantamine 24 mg/day
# not significantly different from baseline
0
1
2
3
4
Galantamine 24 mg/day
Placebo/ Galantamine 24 mg/day
5
6
7
Baseline
Data from historical placebo group
3
6
Raskind M et al., Neurology 54:2261–8, 2000
9
12
Mean change from baseline
± SE in ADAS-Cog/11
Long-term Data: Change from
Baseline in ADAS-Cog/11 scores
Clinical
Improvement
-4
0
4
8
12
16
20
24
Baseline 3
Placebo comparison
Estimation of decline – Stern Equation
Clinical
Decline
Galantamine 24–32 / 24 mg
6
9
12
18
24
Months of Treatment
Raskind MA et al. Arch Neurology 61:252-246, 2004.
30
36
Donepezil Significantly Better Compared to
Calculated Change by Stern Equation over 3 Years
Wallin AK, et al. Dement Geriatr Disord 2007:23:150-160
36-Month Galantamine Trial
►
Does a greater rate of cognitive decline
in “dropouts” than 36 month
“completers” explain results?
►
No! Rate of decline prior to galantamine
discontinuation in “dropouts” was the
same as in “completers.”
We Compared Slopes of ADAS-cog Decline
Between Dropouts and Completers
Change from baseline in ADAS-Cog/11
-1
0
1
2
3
4
5
6
7
8
9
Galantamine patients who completed treatment
Galantamine patients who discontinued
10
11
0
10
20
Time (months)
Raskind MA, et al., Arch Neurol 61:252-256, 2004.
30
40
If ChEIs Delay Disease Progression,
What are the Candidate Mechanisms?
►
Nicotinic cholinergic stimulation in vitro:
●
►
Muscarinic cholinergic stimulation in vitro:
●
●
1Arias
Protects against A-induced neuronal
death1
Inhibits A production from amyloid
precursor protein (APP)2
Reduces phosphorylation of tau2
E et al., Neuropharmacology 46:103-114, 2004.
A et al., J Mol Neurosci 20:349-356, 2003.
2Fisher
Mechanisms of Neuroprotective Effects of
Nicotine and Acetylcholinesterase Inhibitors
Role of Alpha-4 and Alpha-7 Receptors in Neuroprotection
►
An excellent review
►
Highlights:
●
●
Stimulation of nicotinic receptors (particularly
alpha-7) by nicotine or galantamine or
donepezil prevents glutamate neurotoxicity.
These effects of cholinesterase inhibitors
appear independent of their inhibition of
cholinesterase activity.
Akaike A, et al. J Mol Neurosci 40:211-216, 2010
Loss of Alpha-7 Nicotinic Receptors Enhances
Beta-amyloid Oligomer Accumulation in a
Mouse Model of Alzheimer’s Disease
►
“Alzheimer’s” transgenic mice with deletion of
the alpha-7 nicotinic receptor have increased:
●
●
●
Learning and memory deficits
Hippocampal and cholinergic
neurodegeneration
Soluble oligomer (neurotoxic) beta-amyloid
Hernandez CM, et al. J Neuroscience 30:2442-2453, 2010.
Disruptive Agitation: What is it?
Distressing behaviors that often cluster together
•
•
•
•
•
Irritability
Anger outbursts, aggression
Sleep disruption
Pressured pacing and restlessness
Uncooperativeness with necessary care
Major cause of long-term care placement.
Commonly Used Psychotropic Medications
for Disruptive Agitation in AD
►
Antipsychotics: haloperidol, risperidone,
olanzapine, aripiprazole, quetiapine. All show
modest efficacy in some placebo-controlled trials.
●
●
●
Frequent non-responders
Adverse effects: pseudoparkinsonism, sedation
Increased risk of stroke and death caused FDA to issue “Black
Box Warning.”
All antipsychotics are antagonists of the Alpha-1
Adrenoreceptor: Does this contribute to efficacy
for agitation?
The Brain Noradrenergic System
► The
noradrenergic system is the brain
“adrenaline” system for attention and
arousal.
► Excessive
noradrenergic reactivity
produces anxiety and agitation.
► Does
excessive noradrenergic activity
contribute to agitation in AD?
Noradrenergic System Pathology in
Alzheimer’s Disease
►
Despite loss of noradrenergic locus
coeruleus neurons there is:
●
●
●
●
1Elrod
Increased cerebrospinal fluid (CSF)
norepinephrine (NE) in AD1
Increased agitation response to NE in AD2
Compensatory upregulation of surviving LC
neurons3
Increased alpha-1 adrenoreceptors in locus
ceruleus target areas4
et al., Am J Psychiatry 154:25-30, 1997.
et al., Arch Gen Psychiatry, 1995.
3Szot, et al., J Neuroscience, 2006.
4Szot, et al., J Neuroscience, 2007.
2Peskind,
CSF norepinephrine (pg/ml)
CSF Norepinephrine:
Effects of Aging and AD
500
*significantly higher than young subjects
**significantly higher than all other subject groups
**
400
*
300
*
200
100
0
Young
(n=54)
Old
(n=42)
Elrod et al., Am J Psychiatry 154:25-30, 1997.4
Mild-Moderate Advanced
AD (n=49)
AD (n=25)
Postsynaptic Adrenergic Receptor
Antagonists in AD
►
Would reducing brain responsiveness to
NE by blocking adrenergic receptors
reduce agitation in AD?
►
Alpha-1 receptor antagonist: prazosin.
●
●
Long lasting benefits in posttraumatic
stress disorder
Would prazosin be helpful in AD?
Raskind MA, et al., Am J Psychiatry 160:371-373, 2003.
Prazosin as a Novel Pharmacologic
Approach to Agitation in AD
►
Prazosin is an alpha-1 receptor antagonist.
● Only one that crosses from the blood into
the brain
►
Inexpensive, generic, used for BPH and
hypertension by millions of older persons for
decades.
►
Clinically effective for AD agitation in open
label pilot study.
Placebo-Controlled Trial of Prazosin
for Disruptive Agitation in Dementia
►
Twenty-one persons (mean age 80 years) with
DSM-IV dementia (possible or probable AD)
and frequent disruptive agitation.
►
Randomized to prazosin (n = 10) or placebo (n
= 11) for 8 weeks.
►
Prazosin dose range 2-6 mg/day (mean dose
5.6 ± 1.2 mg/day).
►
Primary outcome measures: BPRS, NPI, CGIC.
Placebo-Controlled Trial of Prazosin for
Disruptive Agitation in Dementia: NPI
Wang L, et al., Am J Geriatr Psych 17:744-75, 2009.
Where Are We Now?
►
AD biomarkers will be increasingly valuable,
but do not under-estimate the importance of a
careful history and longitudinal cognitive/
functional assessment.
►
The primacy of Aβ in AD pathogenesis and
therapeutics remains in question.
►
Improving treatments for behavioral
disturbances in AD will have major impacts on
patients and caregiver quality of life and health
care costs.
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Pathophysiology of AD:
Foundation Role of Cholinergic
Dysregulation and Emerging Perspectives
on the Pathobiology of AD
JAMES E. GALVIN, MD, MPH
Professor of Neurology and Psychiatry
Director of Clinical Operations
Center of Excellence on Brain Aging
Director Pearl Barlow Center for Memory Evaluation and Treatment
New York University Langone School of Medicine
New York, NY
Objectives
►
Pathophysiology of AD
►
Beta-amlyoid hypothesis
►
Cholinergic Hypothesis
►
Clinical and therapeutic implications of
Cholinergic hypothesis
►
Intersection of cholinergic and
amyloid-based pathobiology
►
Approaches to therapy
►
Implications for multi-modal therapies
for AD
Pathophysiology of AD
►
Neuropathologic hallmarks of AD
● Senile plaques – Amyloid b-protein (Ab)
● Neurofibrillary tangle – tau protein
►
Largely a sporadic, late-life cause of dementia,
early-onset and familial forms exist
● Mutations in APP, PS-1 and PS-2
● Mutations increase production of Ab
►
Late-onset disease is associated with presence
of the e4 allele of Apolipoprotein E
● More than 40 other genes have been
associated with AD
Amyloid Hypothesis
►
First proposed in 1991
►
Initiating molecule in AD, ultimately
leading to AD
►
Mutations in familial AD encode
substrate (APP) and enzyme
(Presenilin) for A production
►
Infusions of A cause neuronal
degeneration and cognitive deficits
►
Harmful form of A is small, diffusable
aggregates or oligomers
Pakasi and Kalman 2008, Hardy and Allsop 1991, Kowall et al 1991, McDonald et al 1994, Dahlgren et al 2002
A is Derived After Cleavage of APP
sAPP
Plaque
sAPPa
APP
Ab
a
g
p3
g
A
Lumen/
Extracellular
Cytosol
AICD
C99
C83
AICD
(-stub)
(a-stub)
(A50-Cter)
APP = amyloid precursor protein; sAPP = soluble form of APP; AICD = APP intracellular domain
Acetylcholine
►
ACh activity known since turn of 20th century
●
Nobel prize to Henry Dales and Otto Loewi
►
Synthesized de novo by the brain
►
Two types of receptors
●
●
►
Muscaric
Nicotinic
In the CNS, largely produced in collection of
neurons in basal forebrain and pons with widerange projections
Cholinergic Projections
From: Cooper, Roth and Bloom, Biochemical Basis of Neuropharmacology, 7th Ed, 1996
Cholinergic Hypothesis
►
►
Dysfunction of cholinergic system contributes to
memory decline
Drachman and Leavitt (1974)
●
●
●
►
Link between cholinergic dysfunction and memory
impairment
Scopolamine in young adults caused impairment
Corroborated by primate, canine and rodent studies
Reduced choline acetyl transferase (ChAT) activity in
cortex, hippocampus and amygdala of AD patients
●
●
Activity correlated with level of cognitive impairment
Selective loss of cholinergic cells in basal forebrain
Davies and Maloney, 1976, Perry et al 1978, Wilcock et al 1982, Whitehouse et al 1981.
Neuropathological Signaling:
Cholinergic Hypothesis
Presynaptic
Neuron
Acetyl
CoA
+
Choline
Glial Cell
Choline
ChAT
BuChE
ACh
Synaptic Cleft
Postsynaptic
Neuron
ACh
AChE
Choline
+
Acetate
AChE
Cholinergic Receptor
ACh = acetylcholine; AChE = acetylcholinesterase; BuChE = butyrylcholinesterase;
ChAT = choline acetyltransferase; CoA = coenzyme A.
Adapted from Adem A. Acta Neurol Scand. 1992;85(suppl 139):69-74.
BuChE
Cholinergic Hypothesis
►
Basal forebrain and rostral brainstem
cholinergic pathways converge to serve
important functional rolls in awareness,
attention, working memory and mnemonic
processes
►
Loss of cholinergic function contributes to
cognitive decline associated with AD
Perry et al 1999, Bartus 2000,
Cholinergic Receptors and AD
►
Two classes
●
Nicotinic ionic channels
• Responsible for fast transmission
• Reduction in a4 nAChR in AD
• Up-regulation of a7 nAChR in AD compared with MCI and
controls
– a7 receptors down-regulated in DLB
• Possible compensatory response to maintain basal
forebrain-cortical cholinergic activity
• a7 nAChR interacts with APP and A peptides which
●
could lead to aberrant function
Muscarinic G protein-coupled receptors
• Preserved during progression of AD
• In triple transgenic mice, M1 agonists improved cognitive
and reduced A and tau pathology
• Hypothesis: activation of TACE/ADAM17, decreased
BACE1 levels and/or inhibition of GSK3
Mufson et al 2009, Nagele et al 2002, Counts et al, 2007, Caccamo et al 2006
Role of Cholinergic Deficits in
Behavioral Symptoms of AD
►
Temporal and frontal lobe dysfunction implicated in
psychosis of AD
►
Regional cholinergic deficits—apathy and
indifference
►
Cholinergic-monoaminergic imbalance hypothesized
in mood disorders
►
Cholinesterase inhibitors (ChEIs) have shown
behavioral benefits in several clinical trials
Lanari A, et al 2006; Cummings JL. 2000
Clinical and Therapeutic Implications
of Cholinergic hypothesis
►
Recent functional MRI study demonstrated MCI treated with
donepezil demonstrated increased frontal cortex activation
relative to untreated control
●
►
AChE does not show decline until late stages of disease
●
►
Only mild losses in MCI and mild AD
Vesicular Ach transporter is not severely altered in AD
●
●
►
Correlated with task performance
Cholinergic neurons appear then to shrink and become
dysfunctional rather than degenerate early in disease
Suggest cholinergic neurons may be viable, however dysfunctional
early in disease and thus amenable to manipulations
Changes in neurotrophic gene expression may provide targets of
intervention for dysregulation of cholinergic neurons
● NGF (trk) receptors down-regulation may be a molecular marker
for transition from MCI to frank AD
Saykin et al, 2004, Bierer et al 1995, Rinne et al, 2003, Gilmor et al, 1999, Rinne et al 1987, Mufson et al, 2009
Challenges to Cholinergic Hypothesis
►
Studies of post-mortem tissue
●
●
►
►
Since neither ChAT nor AChE are rate-limiting cholinergic enzymes,
they are unlikely to accurately reflect cholinergic function in a living
patient
Other factors may be involved
●
●
●
►
Levels of AChE and ChAT are not reduced in very mild AD
Levels of ChAT may be upregulated in MCI and very mild AD
Alterations in high-affinity choline transport (rate-limiting step)
Deficits in nicotinic and muscarinic receptors
Dysfunctional neurotrophic support
Neurochemical analyses of autopsy tissue maybe unreliable
●
●
Dependent on length of agonal state and post-mortem interval
More recent in vivo imaging studies support amyloid hypothesis
• 11C N-methylpiperidine-4-yl proprianate (AChE activity)
• Nicotine-based ligands
• Non-selective muscarinic ligands
• 123I Benzovesamacol (vesicular Ach transporter)
Terry and Buccafusco 2003, Slotkin 1990, Auld et al 2002, Kuhl et al 1999, Norberg 2001, Zubieta et al 2001, Kuhl et al 1996
Recent Developments
►
Extension of studies to early, prodromal stages
●
●
●
Religious Orders Study
Very mild cases did not show decreases in ChAT but
actually increases
Immunochemistry of brain with very mild AD/MCI
• ChAT or vesicular ACh transporter not reduced
• Markers of NGF receptors markedly reduced
• Possible that other pre- or post-synaptic mechanisms
may be compromised
• Perhaps down-regulation of retrograde transmission of
NGF from hippocampus/frontal cortex to basal forebrain
• Altered neurotrophic receptors may mark early stage of
disease with initial increases in ChAT activity
• Decreased connectivity between hippocampus and
entorhinal cortex
Davis et al, 1999, Dekosky et al, 2002, Gilmor et al, 2000, Mufson et al, 2002, Terry et al, 2003, Counts and Mufson, 2005,
Ikonomovic et al, 2003, Kordower et al, 2001
Interactions Between Amyloid and
Cholinergic Hypotheses
►
Regulation of A by stimulation of muscarinic or nicotinic receptors
●
●
Partial M1 agonists increase aAPPs, decrease A and decrease tau
phosphorylation
Nicotine may increase downstream synthesis of neurotropins
►
Cholinergic deficits could be secondary to amyloid toxicity
►
Bidirectional interaction between cholinergic function and processing
of amyloid precursor protein
●
●
●
High affinitity a7 receptors can serve as high affinity binding sites for
A peptides
Amyloid peptides inhibit uptake of choline and decrease endogenous
Ach release without exhibiting effects on ChAT activity
A block functional interaction between nicotinic agonists and receptors
on hippocampal neurons
Court et al, 1998, Muller et al 1997, Genis et al 1999, Jonnala et al 2002, Roberson et al, 1997, Wang et al
2000, Pakaski and Kalman, 2008, Liu 2001
Interactions Between Ab and ACh
►
Toxicity of A on the cholinergic system
●
●
●
●
●
●
►
Ach synthesis and release reduced by solubilized Ab
Loss of cholinergic fibers without loss of cholinergic neurons
Reduction of binding to vesicular Ach transporter
Inhibition of fast axonal transport
A 42 binds with higher affinity to a7 nAChR than A 40
A 42 reduced downstream events in mAChR signal transduction
Cholinergic system and APP processing via a-secretase
●
●
●
mAChR
a7nAChR agonists
AChEI
Auld et al 1998, Boncristiano et al 2002, Ikeda et al 2000, Kasa et al 2000, Qi et al 2005, Kelly et al 1996, Buxbaum et al
1992, Zimmerman et al 2004
Mechanisms of AChE Inhibitors on the
Release of sAPPα
AchE
inhibitor
Change
Tacrine
Metrifonate
Cholinergic
mechanism
Other mechanism
Reference
Decrease −
?
Lahiri et al. (1994); Lahiri et al. (1996)
Increase +
?
(Pakaski et al., 2000) and (Pakaski et al.,
2001); Racchi et al. (2001)
Ambenonium Increase +
?
Pakaski et al. (2001)
Ganstigmine Increase +
?
Mazzucchelli et al. (2003)
Ladostigil
Increase +
Donepezil
Increase +
Phenserine
Decrease −
Galantamine Increase +
Pakaski and Kalman 2008
MAP-kinase or tyrosin
Yogev-Falach et al. (2002)
kinase-dependent pathway
Enhancing trafficking and
Zimmermann et al. (2004)
activity of ADAM 10
Inhibition of APP mRNA
Lahiri et al. (2000); Shaw et al. (2001)
translation
?
Lenzken et al. (2007)
Linking Ab and ACh
Pakaski and Kalman 2008
Discrimination Between Disease
Modification and Symptomatic Benefit
Withdrawal design
Randomized
phase
Placebo
phase
Active
Disease-modifying
effect
Placebo
Performance
Performance
Randomized
phase
Staggered-start design
Placebo
phase
Active
Placebo
Symptomatic
effect
Symptomatic
effect
Disease-modifying
effect
Time
Time
Is There Evidence of DiseaseModifying Effects?
►
From clinical trials, functional imaging and basic
science studies, anti-cholinesterase drugs may:
●
●
●
●
►
Reduce circulating A
Alter APP processing
Prevent A deposition in cholinergic projection sites
Promote non-amyloidogenic APP processing
If changes in cholinergic transmission alters APP
processing, appropriate cholimimetic
therapeutics might provide both symptomatic
benefit and modify AD pathogenesis
Lopez et al 2002, Krishman et al 2003, Francis et al 2005, Nordberg 2006, Inestrosa et al 1996, Rogers et al 2000
Amyloid-Based Approaches
Barten and Albright 2008
Immunization Reduces Ab burden
Holmes et al 2008
Immunization Does not rRduce
Disease Burden
Time to severe dementia
Holmes et al 2008
Time to death
Neurotransmitter-Based Approaches
Barten and Albright 2008
Model of Multi-Modal Approach
Performance
Mild
Moderate
Severe
Disease-modifying
Rx
Combining
Symptomatic and
Disease-modifying RX
Symptomatic Rx
Time
Summary
►
Ab as the likely culprit leading to AD is a logical
target for anti-AD therapies but to date, Phase
III trials have not been successful
►
Ach provides targets for symptomatic benefit
●
●
Dysfunction/degeneration of the cholinergic projection
neurons is a later stage event in AD
Dysregulation of the cholinergic system is an early event
Mufson et al 2009,Davis et al 1999, DeKosky et al 2002, Mufson et al 200, Mufson et al 2002
Summary (cont.)
►
There is a bidirectional relationship between the
amyloid and cholinergic hypotheses
►
Disease-modifying therapies will likely be more
effective when used earlier in disease process
●
►
Clear need for improve detection of AD at earliest, even
preclinical stages
Multi-modal approaches offer the best potential
to provide treatment throughout the spectrum of
disease
Mufson et al 2009,Davis et al 1999, DeKosky et al 2002, Mufson et al 200, Mufson et al 2002
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Evidence-based Role of
Cholinesterase Inhibition
Across the Severity
Spectrum in AD
SANDRA E. BLACK, MD, FRCPC
Brill Chair in Neurology
University of Toronto, Sunnybrook
Health Sciences Centre
Toronto, Ontario Canada
Learning Objectives
►
Review evidence for cholinesterase inhibitors
as cognitive enhancers in mild-moderate
Alzheimer’s Disease
►
Summarize evidence for utility in earlier and
later stages of AD
►
Consider evidence for longer term use
See Canadian Consensus on Dementia Diagnosis and Treatment:
Hogan et al, CMAJ 2008; Alzheimer’s and Dementia special issue 2007
The Cholinergic Deficit in AD
– Progressive loss of
cholinergic neurons
– Progressive decrease in
available ACh
N. basalis Meynert
– Impairment in ADL,
behavior and cognition
Cortex
Hippocampus
Bartus et al., 1982; Cummings and Back, 1998, Perry et al., 1978
Cholinesterase Inhibitors:
Mechanisms of Action
Presynaptic
nerve terminal
ACh
N = nicotinic
M = muscarinic
ACh = acetylcholine
Astrocyte
BuChE
N receptor
Galantamine
M receptor
Donepezil
Rivastigmine
Galantamine
Acetylcholinesterase
Rivastigmine
ACh
Butyrylcholinesterase
Postsynaptic
nerve
terminal
Increased availability of ACh at synapse (AChE and BuChE inhibition)
Efficacy-Cognitive Improvement
benefit
Rogers, 1998b
no benefit
Rosler, 1999
Wilcock, 2000
heterogeneous
Rockwood,
2001
Wilkinson, 2001
Meta-analytic
difference
30%
20%
10%
0%
-10%
10% [4%, 17%] of patients show significant benefit over placebo
Lanctot et al, CMAJ, 2003
Efficacy Clinical Global Impression
Rogers, 1998a
Rogers, 1998b
Burns, 1999
Rosler, 1999
Raskind, 2000
Wilcock, 2000
Rockwood, 2001
Wilkinson, 2001
Meta-analytic difference
30%
20%
benefit
no benefit
Homogeneous
10%
0%
-10%
9% [6%, 12%] of patients show significant benefit over placebo
Lanctot et al, CMAJ, 2003
Number Needed to Treat for Benefit
►
Numbers needed to treat to benefit
●
●
●
7 (CI95%: 6, 9) for stabilization or better
12 (CI95%: 9, 16) for minimal
improvement or better
42 (CI95%: 26, 114) for marked
improvement
►NNT for clinically benefit are low.
►Homogeneous-all 3 ChEI similar
Lanctot et al, CMAJ, 2003
Tolerability
14
Caveat
ChEI placebo diff
12
Galantamine
above
recommended
doses,
heterogeneity
10
8
6
donepezil
rivastigmine
galantamine
4
2
0
DO
8% [5,11]
Lanctot et al CMAJ, 2003
AE
DO d/t AE
8% [5,12]
7% [3,10]
Safety
► Number needed to harm (ie to cause AE in 1
patient) = 12
(Lanctot et al CMAJ 2003 )
► Recent study of community-dwelling dementia
patients using healthcare database in Ontario,
Canada (2002-4)
► 19,803 treated with cholinesterase inhibitors vs
61,499 not on CHEI’s
●
●
●
●
Syncope 31.5 vs 18.6/1000
Bradycardia 6.9 vs 4-4/1000
Pacemaker needed 4.7 vs 3.3/1000
Hip fracture 22.4 vs 19.8/1000
Gill et al Arch Int Med 2009
HR 1.76
HR 1.69
HR 1.49
HR 1.18
Limitations of Drug Trials to Date
►
►
Benefits in cognition, behavior and function have been for 6 monthsonly a few 1-year placebo-controlled studies
Longer term benefits derived from open label extensions, limited by
large dropouts and bias from self-selection
►
Most clinical trials have been pharma-sponsored without independent
analyses, except for AD 2000
►
Differential treatment effects on specific cognitive domains are not
known as they have not been studied; the tools used may not have
sampled the most sensitive domains
►
Placebo trials may no longer be feasible or ethical
►
Recent review of RCTs highlight methodological flaws (e.g., no
corrections for multiple comparisons, LOCF method) and questions
utility of drugs in clinical practice
Kaduszkiewicz et al., BMJ, 2005
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Use in Early and Later
Disease Stages
Natural History of AD: early
30
25
Loss of functional
independence
20
MMSE
Early
Cognitive symptoms
Mild-moderate
Behavioural problems
15
10
Nursing home placement
5
Severe
Death
0
1
2
3
4
5
6
7
8
Years
Feldman H and Gracon S in: Clinical Diagnosis and Management of Alzheimer’s Disease 1998.
9
Proportion Free of Dementia (%)
Conversion of Normal and MCI Subjects
to Dementia (AD Cooperative Study)
100
90
80
70
60
50
40
30
20
10
0
0.0
Normals
MCI
45%
0.5
1.0
1.5
2.0
2.5
Follow-up Time (Years)
3.0
3.5
Retrospective analysis of 687 subjects with MCI Mean age 72.2 yrs
DeKosky ST. J Am Geriatr Soc, 2003; Adapted from Grundman M et al, Abstract in Neurology, 1996.
ADCS: MCI Study Design
Objectives
►
To determine whether daily doses of vitamin E or donepezil given over
a 3-year period can:
1) delay or prevent the onset of AD in people who have MCI
2) slow the decline of symptoms
Design:
3-year, randomized, double-blind, placebo-controlled,
parallel group study
►
60 sites in the US and 9 sites in Canada
►
Patients were randomized to receive donepezil 10 mg/day, vitamin E
1,000 IU b.i.d., or placebo
Subjects: 769 patients with MCI
Outcome measures:
►
►
Primary:
Secondary:
Conversion to AD
MMSE, ADAS-cog, CDR, CDR-SB, ADCS, GDS,
Neuropsychological battery
Petersen et al. N Engl J Med, 2005
Survival Analysis: Donepezil vs. Placebo
6 mo
1 yr
18 mo
Probability of not
converting to AD
1.0
0.9
0.8
0.7
0.6
Donepezil
Placebo
p<0.001
0.5
p<0.009
p<0.035
0.4
0
200
400
600
800
Time on MCI study (days)
Petersen RC et al. N Engl J Med, 2005
1,000
1,200
Summary of MCI Studies
►
NIH MCI study with donepezil failed statistical significance
on primary endpoint, but decline delayed by up to 12
months, and was slower in APOE e4 participants
(Petersen et al NEJM 2005)
►
Recent 48 wk study of donepezil in 821 aMCI patients
likewise found nsd in 1o and 2o outcomes, though patients
felt better subjectively (Doody et al Neurol 2009)
►
Other MCI trials with galantamine (Winblad et al Neurol 2008)
rivastigmine (Feldman et al Lancet Neurol 2007) also did not
delay conversion
►
More deaths noted with galantamine 1.4% vs 0.3% in
placebo MCI subjects leading to product label warning
See Raschetti et al Cochrane Review PLoS Med 2007
Safety and Tolerability of Donepezil
(10mg/d) in aMCI
Study Design
• Safety and tolerability of donepezil (10mg) was evaluated in 145 aMCI patients as
an open label 28-week extension study after a 48-week RCT of 821 aMCI
Key Results
• 57.4% in the donepezil/donepezil group and 62.3% in the placebo/donepezil group
experienced an AE
• Most frequent treatment related AEs were diarrhea, muscle spasms, insomnia, and
nausea (more common early on & mild-moderate in severity)
• 22.1% in the placebo/donepezil group discontinued donepezil due to an AE
compared with 10.3% in the donepezil/donepezil group
Conclusions
• Donepezil in aMCI appeared to be safe, but patients with AD seem to tolerate it
better than patients with MCI
Doody, et al., Am J of AD & Other Dem. 2010
Higher Rate of Progression to AD in Patients
with aMCI and Depressive Symptoms
Study Design
• 756 aMCI from the three year NIH study drug trial of donepezil and vitamin
E
• Depressive symptoms assessed at baseline using the Beck Depression
Inventory (BDI)
Key Results
• On regression analysis higher BDI scores were associated with progression to AD
• Depressive subjects: proportion progressing to AD was lower in donepezil group
than combined vitamin E and placebo groups at 1.7 years, 2.2 years, and marginally
lower at 2.7 years
• Nondepressive subjects: no difference between the three treatment groups
Conclusions
• Depressive symptoms may be predictive of progression from aMCI to AD
• Treatment with donepezil delayed progression to AD in depressive
subjects with aMCI
Lu, et al., Neurology 2009
Survival
Lu, et al., Neurology 2009
Natural History of AD:
Moderate to severe stage
30
Early
Cognitive symptoms
25
Loss of functional
independence
MMSE
20
Mild-moderate
15
Behavioural problems
10
Nursing home placement
5
Severe
Death
0
1
2
3
4
5
6
7
8
9
Years
Feldman H and Gracon S in: Clinical Diagnosis and Management of Alzheimer’s Disease 1998.
Donepezil vs Placebo in Nursing Home Study in
Severe AD (MMSE 1-10): Cognition (SIB)
6
Mean Change From Baseline
in SIB Score
p=0.003*
SIB
p=0.008*
p=0.008†
Clinical
improvement
4
2
Baseline
0
-2
Donepezil
Placebo
-4
Clinical
decline
-6
0
3
6
ITT LOCF
Months
Winblad et al. Lancet, 2006.
*OC analysis; †LOCF analysis.
Mean Change From Baseline
in ADCS-ADL
Functional Abilities Also
Showed Less Decline
4
Donepezil
Placebo
3
Clinical
Improvement
2
1
P = 0.086*
P = 0.031*
P = 0.029†
Baseline
0
-1
-2
-3
Clinical
Decline
-4
0
3
6
Months
*OC analysis; †LOCF analysis.
Winblad et al Lancet, 2006
ITT LOCF
SIB scores: LS mean change from
baseline (SE)
Less Cognitive Decline in Community
Dwelling Severe AD (MMSE1-12)
8
6
p =0 .0001
4
Clinical
improvement
2
0
-2
d
Clinical
decline
-4
Donepezil 10mg/d
Placebo
-6
-8
0
8
16
Study week
Black et al Neur 2007
24
ITT LOCF
Cholinesterase Inhibitor Use in
Other Dementias
►
Level 1 evidence for different compounds
according to studies undertaken
●
●
●
●
Donepezil in vascular dementia
Rivastigmine in parkinson/diffuse lewy body
dementia
Galantamine in mixed vascular dementia
(Memantine also shows efficacy in moderate to
severe AD)
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Use of Higher Doses,
New Formulations
Once Daily Formulations
Galantamine
extended release
8mg od –16mg od– 24mg od
Rivastigmine patch
4.6-mg od –9.5mg od
GI tolerability better than oral
formulation
(eg nausea: oral 23 vs patch 7%
vs placebo 5%)
Skin sensitivity (erythema, edema,
pruritus, pain)
Winblad et al. Int J Geri Psych. 2007
Recent caution due to additive dose effects
if patch not removed daily before new one applied
Safety & Tolerability of Higher Dose
Donepezil (20mg)
Purpose
• To evaluate the safety and tolerability of donepezil at doses of 15 and 20mg/day
Study Design
• A 24-week, randomized, double-blind, placebo controlled, pilot study
• 31 patients (male and female) aged 50-86 years
•All patients had been treated with 10mg/day donepezil for 12-30 months prior to
enrollment
• Primary outcome measures:
• Tolerability (discontinuations, dose modifications, and adverse events)
• Safety (monitored by adverse events, physical examinations, clinical lab tests,
and ECGs)
• Secondary outcome measures:
• Psychometric measures: ADAS-Cog, MMSE, CIBIC+,
pharmacokinetic/pharmacodynamic parameters
Doody, et al., Drugs Aging 2008
Safety & Tolerability of higher dose
Donepezil (20mg)
Key Results
•Higher-dose group:
•15 of 16 patients tolerated the maximum 20 mg/day dose by week 24
• Standard-dose group:
•14 of 15 patients tolerated donepezil 10 mg/day plus placebo 10 mg/day by
the end of the study
• Adverse events possibly related to treatment were reported by 3 patients in the
standard-dose group and 6 patients in the higher-dose group
• No difference between groups on psychometric measures
Conclusions
• Doses of 15 and 20 mg/day of donepezil appeared to be safe and well tolerated
• May justify larger clinical trials for the safety and efficacy of donepezil at higher
doses in patients with AD.
Doody, et al., Drugs Aging 2008
High Dose (23mg/d) vs Standard 10mg Dose
Donepezil in Moderate to Severe Stage AD
Purpose
►
To determine effectiveness, safety and tolerability of 23 mg vs
10mg donepezil in mod-severe AD already on 10 mg donepezil
Design
►
1467 patients (465 US) in 209 sites randomized to 23mg
(n=972) vs 10mg (n= 479)
►
MMSE: 76%: 0-16; 34%: 17-20
►
Approx 36% also on memantine (75% in US)
Results
►
Discontinuation higher for 23 mg vs 10mg:
●
30% (18% for AE’s vs 18% (8% for AE’s)
Effectiveness analysis:Cognition
Severe Impairment Battery
Less decline from baseline on SIB
P<0.001
Farlow et al. Clinical Therapeutics 2010.
MMSE
Frequency Distribution of CIBIC
Scores at Week 24
No difference in ADL scores
Adverse Events: 23 vs 10
Nausea %
11.8 vs 3.4
Vomiting %
9.3 vs 2.5
Diarrhea %
8.3 vs 5.3
Anorexia %
SAE %
Farlow et al. Clinical Therapeutics2010.
8.6 vs 9.6
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Is There Any Evidence for
Longer Term Use of
Cholinesterase Inhibitors?
Rivastigmine-Placebo Group Does not Catch
Up to Treated Group
6–12 mg/day rivastigmine
Placebo
Proj. placebo
ADAS-Cog mean change
from baseline
2
1–4 mg/day rivastigmine
Dose optimization with
rivastigmine (6-12 mg/day)
*
0
*
–2
*
*
*
*
*
–4
–6
*
*
All patients
restarted on rivastigmine
–8
0
10
Messina et al., 2000
20
26
30
Study week
40
50
B352 patients in Study B353 (OC) at week 52
*p<0.05 vs projected placebo
Mean Change in ADAS-Cog Score from Baseline:
Open Label Galantamine Over 4 Years
Mean change from baseline
(±SE) in ADAS-Cog/11
–4
0
4
8
12
16
12-month placebo
20
Expected decline in untreated
patients of 6–9 points/year
24
Galantamine 24–32/24 mg
28
Baseline 3
6
9
12
(n) (322) (309) (310) (233) (298)
24
36
48
(228)
(140)
(103)
Time (months)
Database and from Raskind et al Arch Neurol 2004.
1-year Preservation of Function Study
with Donepezil
Design
►
1-year, randomized, placebo-controlled, double-blind
Subjects
►
431 patients with mild-to-moderate AD
►
Aged 49-94, mean MMSE 17.1
Primary Outcome
►
Time to clinically evident functional decline’, defined by:
●
Decline in 1 basic ADL present at baseline
●
Decline of 20% of the instrumental ADL present at baseline
●
Increase 1 point from baseline in global CDR score (Clinical
Dementia Rating scale)
Mohs et al. Neurology. 2001
Time to Clinically Evident
Functional Decline*
1
Kaplan-Meier survival estimates
Probability of survival
0.9
The probability of survival (maintaining
functional ability) at 48 weeks was:
51% for donepezil
35% for placebo
0.8
0.7
0.6
0.5
0.4
Donepezil 10 mg/day
Placebo
0.3
0.2
Survival curve comparison:
p=0.002 (log-rank test)
p=0.005 (Wilcoxon test)
0.1
0
0
6
12
18
24
30
36
42
48
54
Duration of treatment (weeks)
*As judged by investigator, ITT population
Mohs et al. Neurology. 2001
Longer-Term Effects: Non-Pharmaceutical
Sponsored Study
Two-year, double blind, RCT in AD of donepezil
versus placebo in a family practice setting in the
UK sponsored by local health authority (AD2000)
Small improvements shown but not considered
clinically significant since no delay in NHP, loss
of milestones or decrease in caregiver costs
(AD 2000, Courtney et al., Lancet, 2004)
Issues:
a) Large dropout (40% 1-year, 77% 2-year)
b) Not clear if samples used for analyses
were matched after run in; also used washout
c) 51% of total sample had CVD
Other Studies Suggesting Symptomatic
Stabilization over Longer Periods
►
Potential for symptom stabilization – 50% of
patients with no change or improvement on SIB
after 1 year, and 35% after 2 years in head to
head trial of rivastigmine and donepezil1
►
Compared with placebo or untreated populations,2–
7 ChE-I therapy may delay cognitive and functional
decline and the progression of neuropsychiatric
symptoms by up to a year
1Bullock
R et al. CMRO 2005
et al. Alzheimer Dis Assoc Disord 1997
3 Feldman et al. Neurology 2001
4Winblad et al. Neurology 2001;
5Klatte et al. Alzheimer Dis Assoc Disord 2003
6Small et al Int J Clin Pract 2005
7Aisen et al. JAMA 2003
2Schmitt
Patients on ChEI’s Had Less Decline in
Multiple Cognitive Domains over 1 Year
Less decline in:
•
•
•
•
Overall cognition
Naming
Visuospatial and
visuoconstructive skills
Executive functions
Dementia Rating Scale
125
120
Mean DRS scores
N= 65 in each of treated vs
untreated group, wellmatched on age, edcuation,
severity, comorbidities, vasc
risk factors and medications
untreated
treated
115
110
105
100
95
90
baseline
follow-up
p<0.0001
Effect size
Behl et al Dem Ger Cog Dis 2006
d = 0.7
Patients on ChEI’s Continued to Show Less Decline
on Select Cognitive Domains at Two Years
Verbal Memory
Mean CVLT acquisition
Treated patients
showed less decline
on:
• Overall cognition
• Memory
• Naming
• Executive functions
30
25
untreated
treated
20
15
10
5
0
baseline follow-up1 follow-up2
p=0.007
ES: d1 =0.8; d2 = 0.4
Behl et al Dem Ger Cog Dis 2006
Patients on ChEI’s also showed less decline in functional
abilities over 2 years, especially in initiation (DAD)
Instrumental
80
70
60
50
40
untreated
30
treated
20
10
0
baseline
follow-up1
follow-up2
Basic
80
mean basic ADLs initiation
Mean overall DAD initiation
90
Mean Instrumental initiation scores
Overall DAD
70
60
50
40
untreated
30
treated
20
10
0
baseline
follow-up1
follow-up2
120
100
80
60
untreated
40
treated
20
0
baseline
follow-up1
follow-up2
Pyear1=0.036; Pyear2=0.001
Pyear1=0.04; Pyear2=0.001
Pyear1=0.08 ; Pyear2=0.001
ES 1= 0.5;
ES 1 =0.6; ES 2= 0.9
ES 1= 0.4;
ES 2= 0.8
Behl et al, Int Psychoger 2008
ES 2 = 0.7
Also Planning and Organization
Basic
Overall DAD
120
mean basic ADLs planning
Mean overall DAD planning
90
80
70
60
50
40
untreated
30
treated
20
10
100
80
60
untreated
40
treated
20
0
0
baseline
follow-up1
follow-up2
Pyear1= 0.038;
Pyear2=0.006
ES 1=0.8;
ES 2 =1.0
Behl et al, Int Psychoger 2008
baseline
follow-up1
Pyear1=0.039; Pyear2=0.001
ES 1 = 0.7;
ES = 1.0
follow-up2
Does Persistent Use of Antidementia Drugs Slow
Clinical Progression of AD over 20 Years?
Study Design
• 641 probable AD patients were followed for 20 years in a single centre
• Cumulative drug exposure was expressed as a persistency index (PI) reflecting total
years of drug use divided by total years of disease symptoms
• Measures: annual change in slope of neuropsychological and functional tests as
predicted by follow up time, PI, and the interaction between these variables
Key Results
• PI was associated with significantly slower rates of decline on MMSE, Physical SelfMaintenance Scale (PSMS), IADL, CDR-SB
• Results suggest that PI (cumulative drug exposure) slowed ADAS-Cog decline for
3.3 years, with effect then lost
Conclusions
• Persistent drug treatment had a positive impact on AD progression in terms of
cognitive, functional, and global outcome measures
• Positive treatment effects extended to those at more advanced stages of disease
Rountree, et al., Alzheimer’s Res. & Ther. 2009
Conclusions
►
Cholinesterase inhibitors have modest symptomatic benefits
in cognition, function, and behavior in mild-moderate AD
and remain the only proven therapy for these disease
stages after 20 years. They may be associated with increase
risk of syncope and falls
►
Their benefits are also seen in more advanced stages, but
are not evident in MCI though some MCI subgroups may be
more responsive
►
Duration of benefits may go beyond the 6 months used in
the pivotal trials but Level 1 evidence for this is scarce and
ethically difficult to obtain
►
Cognitive benefits are likely selective to the processes most
affected by acetylcholine (attention/executive, initiation and
social engagement)
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Translating Advances in
Biomarker-based Detection
into Clinical Practice
Implications for Current Therapies and Beyond
SERGE GAUTHIER, MD
Director of the Alzheimer’s Disease Research Unit
McGill Centre for Studies in Aging
Professor of Neurology and Neurosurgery, Psychiatry and Medicine
McGill University
Montreal, Quebec Canada
Outline
► Case histories of persons at risk
► Case history of person with MCI
► Case histories of persons with AD
► Conclusions
Young Person with
Strong Family History of AD
►
Age: 40
►
Cognitive symptoms: none
►
Family history of AD: mother d55,
sister d53
►
Biomarkers: genetic (PS, APP);
neuro-imaging (FDG-PET)
►
Current Rx: enroll in DIAN
►
Future Rx: anti-amyloid
FDG-PET IN AD
Middle-age Person with Concern About
Family History of AD
►
Age: 50
►
Cognitive symptoms: none
►
Family history of AD: mother d85
►
Biomarkers: genetic (apoE); neuroimaging (MRI)
►
Current Rx: assess risk using mid-life
risk score
►
Future Rx: enhance protective factors
CAIDE Dementia Risk Score
CAIDE Dementia Risk Score
< 47 years
47-53 years
>53 years
0
3
4
≥10 years
7-9 years
0-6 years
0
2
3
Women
Men
0
1
140 mm Hg
> 140 mm Hg
0
2
BMI
30 kg/m2
> 30 kg/m2
0
2
Total cholesterol
6.5 mmol/l
> 6.5 mmol/l
0
2
Physical activity
Active
Inactive
0
1
Age
Formal education
Sex
Systolic BP
Kivipelto et al.,
Lancet Neurol
2006
Probability of Dementia in Late-life According to the
Risk Score Category in Middle Age
The overall occurrence of dementia 4.4%
SCORE
All /Demented, n
% Risk (95% CI)
0-5
401 / 4
1.0 (0.0-2.0)
6-7
270 / 5
1.9 (0.2-3.5)
8-9
312 / 13
4.2 (1.9-6.4)
10-11
245 / 18
7.4 (4.1-10.6)
12-15
122 / 20
16.4 (9.7-23.1)
Kivipelto et al., Lancet Neurology 2006
Older Person with Concern About
Family History of AD
►
Age: 76
►
Cognitive symptoms: none
►
Family history of AD: mother d93
►
Biomarkers: genetic (apoE); neuroimaging (MRI)
►
Current Rx: assess risk using late-life
dementia risk index
►
Future Rx: enhance protective factors,
reduce risk factors
The Late-Life Dementia Risk Index
Barnes DE, et al. Neurology 2009;73;173-179;
Outline
► Case histories of persons at risk
► Case history of person with MCI
► Case histories of persons with AD
► Conclusions
Older Person with MCI
►
Age: 70
►
Cognitive symptoms: mild
►
Family history of AD: mother d87
►
Biomarkers: genetic (apoE);
CSF (ß42, total tau, phospho tau);
neuro-imaging (MRI, FDG-PET)
►
Current Rx: follow over time
►
Future Rx: anti-amyloid
Dubois et al., Lancet Neurology 2007
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Dubois et al., Lancet Neurology 2007
Optimizing Neurotherapy and Emerging Paradigms for
Alzheimer's Disease
Dubois et al., Lancet Neurology 2007
Slope Analyses According to
AD CSF Profile at Baseline
Visser PJ, et al. Lancet Neurol 2009; 8: 619–27
Outline
► Case histories of persons at risk
► Case history of person with MCI
► Case histories of persons with AD
► Conclusions
Older Person with Mild AD
►
Age: 75
►
Cognitive symptoms: mild dementia
►
Family history of AD: none
►
Biomarkers: neuro-imaging (MRI)
►
Current Rx: ChEI
►
Future Rx: anti-amyloid
Older Person with AD and
High Tau Levels in CSF
►
Age: 75
►
Cognitive symptoms: early dementia
►
Family history of AD: none
►
Biomarkers: Neuro-imagimg (MRI);
CSF low ß42, very high phospho tau
►
Current Rx: ChEI
►
Future Rx: anti-amyloid and anti-tau
Distribution of CSF total tau, phosphorylated tau (Ptau), and ß-amyloid 1-42 (Aß42) levels
Wallin AK, et al. Neurology 2010;74;1531-1537
Five-Year Survival in the Three Clusters
Wallin AK, et al. Neurology 2010;74;1531-1537
Pathology by Clinical Status
Proximate to Death
Schneider JA, et al. Ann Neurol 2009;66:200–208
Outline
► Case histories of persons at risk
► Case history of person with MCI
► Case histories of persons with AD
► Conclusions
Biomarkers for the Diagnosis and
Management of AD
► Assessment of risk is possible using mid-life
and late-life risk profiles, including apoE
genotyping
► Earlier diagnosis of AD is now possible using
neuro-imaging and CSF analysis
► Better selection of disease-modifying
treatments may be possible using CSF analysis
and neuro-imaging, knowing the relative
weight of each pathological component