Acid/Base

Acid/Base Conference
11/3/09
Saleem Bharmal
Case
HPI: 43 y/o AAF with PMHx of SLE, ESRD from lupus nephritis on HD, interstitial lung disease on 4L home O2 at baseline who was admitted for confusion and hypercapnic respiratory failure after several days of increased cough and SOB. On day of admission patient went to her scheduled outpatient dialysis where she states she “felt sick” She completed dialysis but no ultrafiltration was removed.
She was sent to the ED from dialysis and was found be confused and have a
PaCO2 in the 120s. She was started on non-invasive ventilation with improvement of mental status and admitted to the ICU.
PMHX:
• SLE
• ESRD from lupus nephritis, kidney transplant 2002 s/p rejection in 2004
• Interstitial lung disease felt secondary to both lupus and several round of Cytoxan to treat her lupus
• History of LGIB; partial bowel resection for bleeding AVM
Case
Outpt Meds: Plaquenil, Renagel, Ferrous Sulfate, VitD
Admission Physical Exam:
• T 99 BP 110/70 P 100 RR 26 O2Sat 100% bipap 20/5 60% FiO2
• Pt is noted to be obese, comfortable on Bipap. No JVD. Lungs noted to have dry crackles ¾ up lung fields bilaterally. Tachycardic, regular with 2/6 murmur at LUSB.
AVF on right arm with no edema in the extremities.
Admission Labs:
WBC 8.8 /Hgb 12.7 / Hct 44.8 / plts 171
Na 140 / K 3.4 / Cl 99 / HCO3 34 / BUN 13 / Cre 4.1 / gluc 92 / Ca 8.7
CXR: Lung inspiratory volume is low. Known background of pulmonary fibrosis.
Superimposed infectious process of pulmonary venous congestion in not excluded
Case
Admission ABGs:
Pt initially placed on 1.0 NRB when arrived to ER satting 100%; then switched to bipap 10/5/0.60
8/24 10:25 - 7.11/116/53/37
8/24 11:22 - 7.17/103/163/37
8/24 12:52 - 7.19/99/305/38
Bipap changed to 20/5/0.40
8/24 16:30 - 7.25/84/108/37
Case
• Given CXR findings and concern for possible pulmonary congestion patient underwent UF for 2.5hrs with 3L fluid removal
• 8/25: There was little improvement with UF and patient remained on bipap
ABG: 7.18/95/74/35 Na 139 / K 3.8 / Cl 99 / HCO3 30 / BUN 22 / Cre 5.8
• 8/26: Pt had bipap removed for 1 hour and then developed progressive respiratory acidosis so placed back on bipap.
ABG: 7.22/82/184/33 serum HCO3: 30
• 8/26: Pt underwent HD using low bicarb bath (30 mEq/L)
• 8/27: Pt continued to require bipap as developed worsening hypercapneic respiratory failure with nasal canula. Started on antibiotics.
ABG: 7.15/70/102/24.8
• 8/27: Pt given 1 amp NaHCO3 followed by 1300mg NaHCO3 tid
• 8/28: Remained on bipap; pt started on steroids
ABG 7.17/81/151/30 serum HCO3 27
• 8/28: HD with low HCO3 bath (30 mEq/L) to avoid worsening respiratory acidosis
Case
• Discussion whether patient should be on low or high bicarb bath?
• Argument for high bicarbonate bath to optimize metabolic compensation for respiratory acidosis
• Argument for low bicarbonate bath is possible worsening of respiratory acidosis in setting of high flux HD and poor ventilation
• What is the evidence that HD can worsen respiratory acidosis?
Bicarbonate / Carbon Dioxide Buffer
System
HA + NaHCO
3
NaA + H
2
CO
3
H
2
O + CO
2
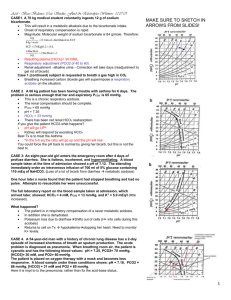
• Examined the change in CO
2 generation and ventilation with high flux hemodialysis and bicarbonate buffer
• Recruited 7 clinically stable hemodialysis patients without any underlying respiratory illness
• Dialysis was performed using Gambro high efficiency dialyzer with 38mEq/L bicarbonate bath
• Ventilation, expired gas collections, and arterialized blood (from AVF) samples were obtained every 30 minutes. Beginning 2 hours before and ending 4 hours after completion of dialysis.
VE – MINUTE VENTILATION
VCO2 – CO2 EXCRETION
VO2 – O2 CONSUMPTION
pH
HCO3 pO2 pCO2
pH
HCO3 pCO2
Authors’ Conclusions
• Combination of bicarbonate dialysate and high efficiency HD generated substantial quantities of CO2 gas which then stimulated respiration as evidenced by a 13% increase in minute ventilation and CO2 production
• Rise in VCO2 is primarily due to bicarbonate metabolism and subsequent CO2 generation, not transfer of dissolved CO2 from the dialysate
• Adequate ventilatory capacity is imperative to excrete the excess CO2 generated during high efficiency bicarbonate hemodialysis
• 26 stable chronic hemodialysis patients undergoing chronic hemodialysis were studied
• Patients were divided in three groups (A, B, and C)
• In group A , “arterial” (a) and “venous” (v) samples were withdrawn before dialysis, after circulation of the blood with the dialysate in the by-pass mode, and after high-flux
HD . In group B, (a) and (v) samples were withdrawn before dialysis, after (“isolatedclosed” ultrafiltration), and after high-flux HD. In group C, withdrawal before hemodialysis , and after high-flux HD was initiated.
• FLX-18 hemodialyzers were used
• Dialysate bicarbonate bath = 36 mEq/L
• Parameters measured were pH, pO2, pCO2, andHCO3
• Although there was an increase in postdialyzer HCO3 in all 3 groups there was also a significant increment of pCO2 in all 3 groups after 5 minutes of high-flux HD
• Case report describing obese patient with respiratory failure from CHF, pleural effusions and restrictive lung disease managed on BIPAP
• Patient initially dialyzed with low bicarb bath 25mEq/L which was associated with increase in metabolic acidosis
• Second HD was done with 30mEq/L bath and this was associated with intradialytic exacerbation of hypercapnia with pCO2 rising from 49mmHg to 67mmHg
Case
• Patient was able to come off bipap 8/29 and initially her pCO2 remained elevated at 69-78mmHg
• She continued to improve on antibiotics and steroids and returned to her baseline of pCO2 55-58mmHg.
• She continued to be dialyzed with bicarbonate bath of
40mEq/L with no episodes of worsening respiratory failure.
• It was noted that her pCO2 did rise during/after dialysis with 40mEq/L HCO3 bath but she was asymptomatic.