Macule
flat, distinct, discolored area of skin. It usually does not include a change in skin texture or thickness.
Papules
solid or cystic raised spot on the skin that is less than 1 centimeter (cm) wide. It is a type of skin lesion
Annular
ring shaped
pruritus
itching
Vesicle, pustule
fluid filled
scaling
loss of outer layer
plaques
uraised red patches covered with a whitish buildup of dead skins cells called scale
Types of infections of the skin
Bacterial- caused by strep A & B hemolytic streptococcus
Fungal
Viral
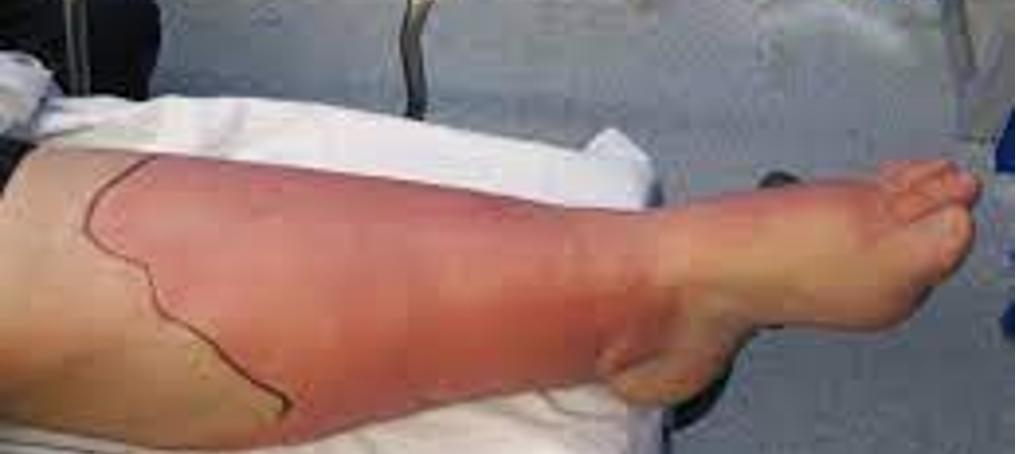
Scalded skin syndrome
Folliculitis
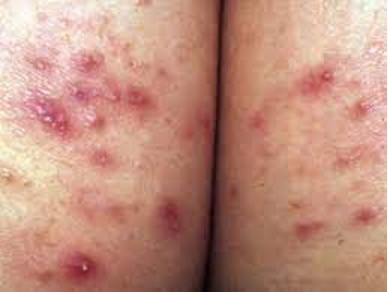
inflammation of follicule
Impetigo
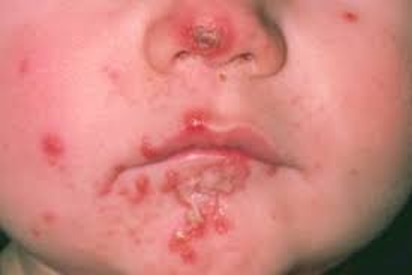
Highly contagious
-red sores that form around nose and mouth. The sores rupture and ooze then form yellow-brown crust
Antibiotics
Tinea capitis (Fungal)
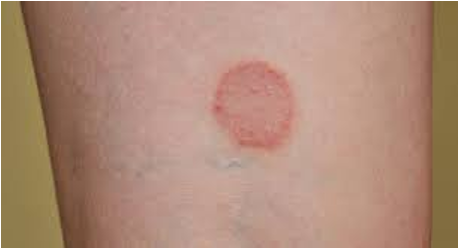
ring worm
-affecting scalp
Tinea cruris
Jock itch
-affecting groin
Tinea pedis
athletes foot
-affecting feet
tinea corporis
affecting any other parts of the body
Tinea versicolor
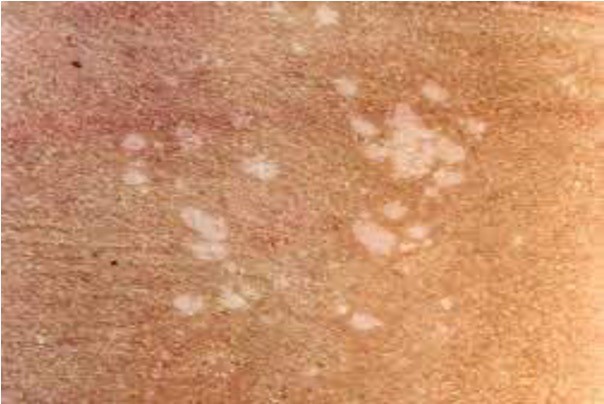
presents differently; hypopigmentation lesions on upper body
Acute hypersensitivity reactions (inflammatory)
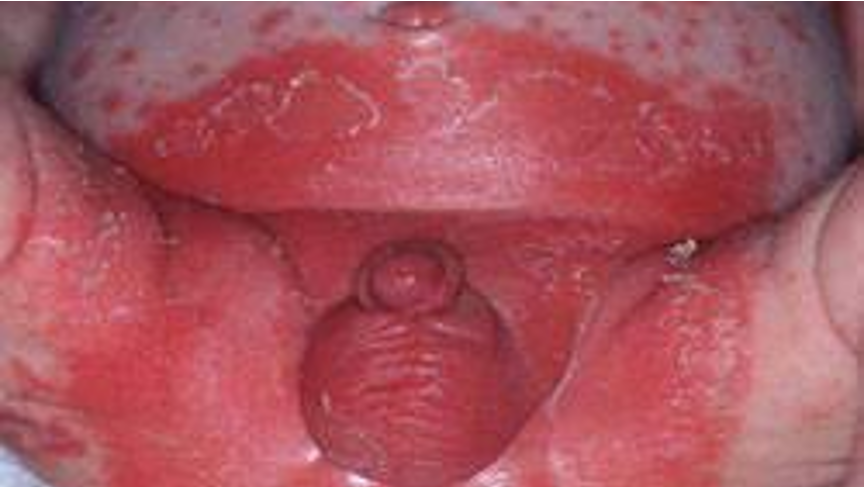
-diaper dermatitis- diaper rash
-contact dermatitis- response to antigenic substance exposure
-erythema multiforme- acute, self limiting hypersensitivity reaction; usually in response to viral infection or medication
-Uriticaria- hives; antigen-antibody response of histamine release from mast cells
Chronic hypersensitivity disorder
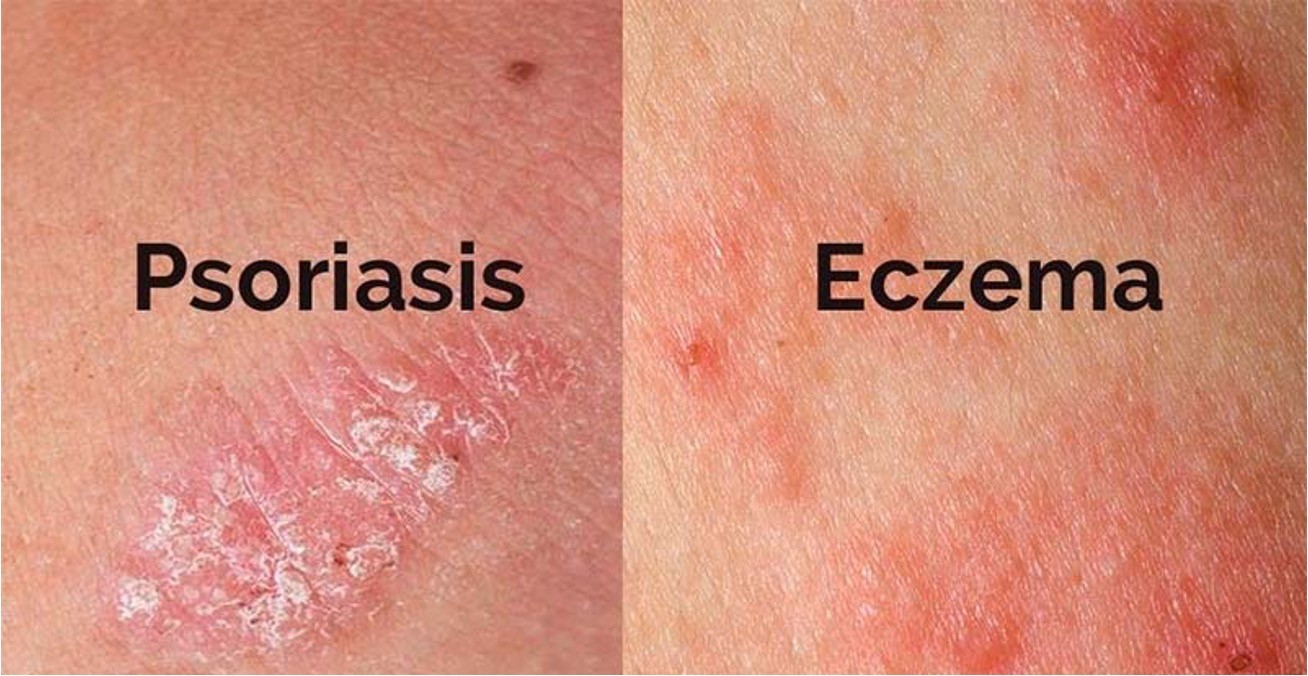
atopic dermatitis - eczema; dry, itchy patches
Chronic inflammatory skin disorders not from hypersensitivity
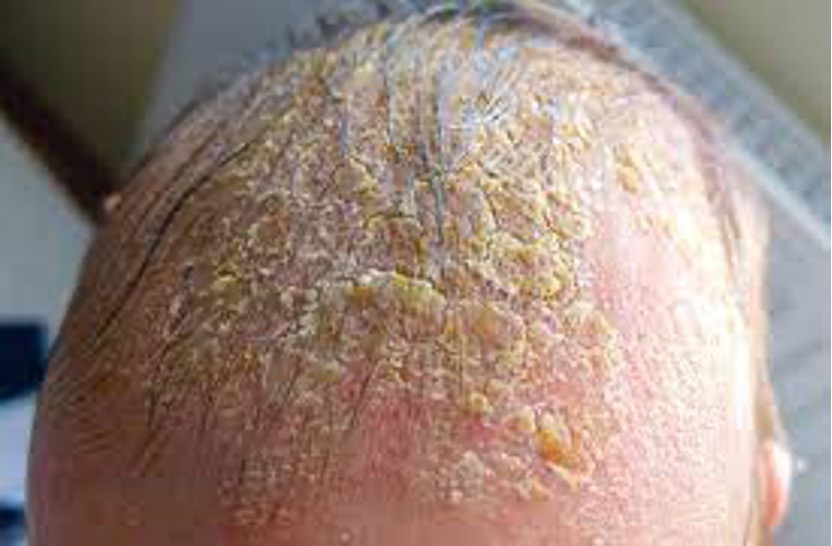
-Seborrhea-chronic inflammatory dermatitis that may occur on the skin or scalp; excess oil accumulation; cradle cap.
-Psoriasis-chronic inflammatory skin disease with periods of remission and exacerbation; build up of scaley red lesions that may burn or itch
Prevention and management of diaper rash
-change diapers frequently
-avoid harsh soaps, baby wipes with fragrance/preservatives
-allow child to go diaper less for periods of time
-blow dry rash area (we don't want it wet)
Contact dermatitis
Causes
-Antigenic substance exposure
-Allergy to nickel or cobalt in clothing, hardware, or dyes
-Exposure to highly allergenic plants: poison ivy, oak, and sumac
Complications
-Secondary bacterial skin infection
-Lichenification (thick and leathery) or hyperpigmentation
Risk Factors for CA-MRSA
-Turf burns
-Towel sharing
-Participation in team sports
-Attendance at day care or outdoor camps
Causes of Urticaria(hives)
-Foods
-Drugs
-Animal stings
-Infections
-Environmental stimuli
-Stress
Injuries
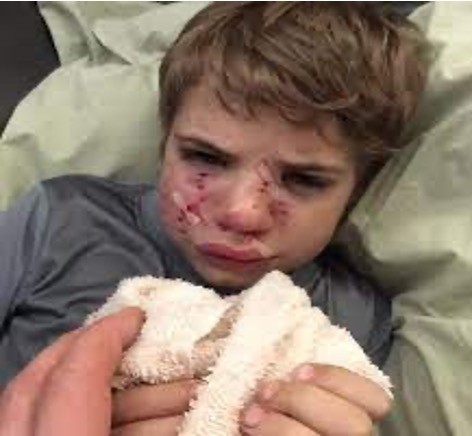
-Pressure ulcers
-Minor injuries
-Burns
-Sunburn
-Cold injury- frost-bite; 1st-4th degree;
-Animal bites – dog bites most frequent; cat bite most infection; hand and face common site; rabies, tetanus
-Insect stings and bites-Hymenoptera class of insects sting; bacterial infection can follow, anaphylaxis
Nursing Interventions for Children with Extensive Burns
-Promoting oxygenation and ventilation
-Restoring and maintaining fluid volume
-Preventing hypothermia
-Cleansing the burn
-Preventing infection
-Managing pain with atraumatic care
-Treating infected burns
-Providing burn rehabilitation
Common Medications
-Antibiotics (topical, systemic)
-Corticosteroids (topical)
-Antifungals (topical, systemic)
-Topical immune modulators (moderate to severe atopic dermatitis)
-Antihistamines
-Isotretinoin (cystic or severe acne)
-Coal tar preparations (psoriasis, atopic dermatitis)
-Silver sulfadiazine 1% (burns)
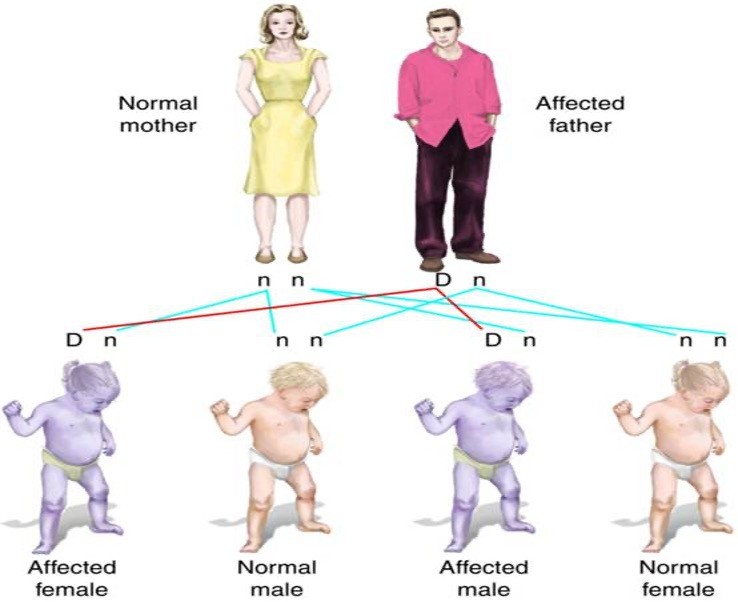
Autosomal dominant inheritance pattern
50% chance of child having affected genes
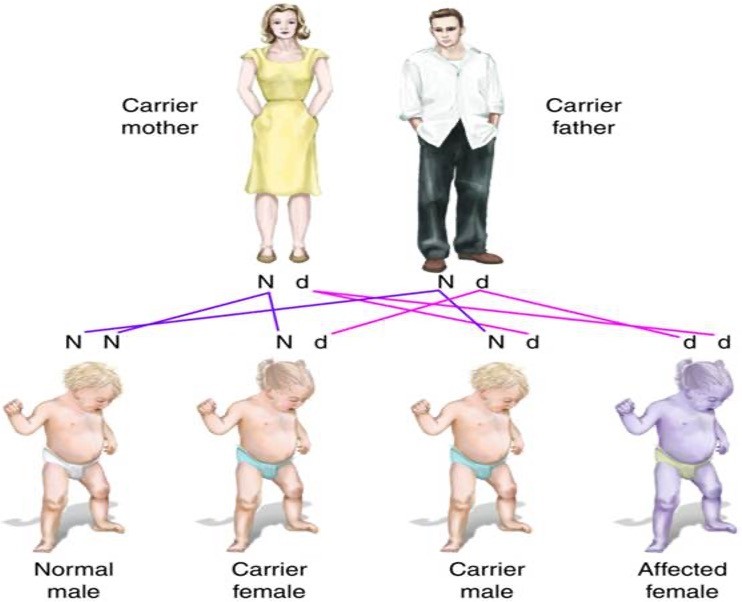
Autosomal recessive inheritance pattern
25% chance of having child affected
Significant Findings in Medical History of a Child with a Genetic Disorder
•Maternal age older than 35 years or paternal age older than 50
•Repeated premature births, breech delivery - Congenital hip dysplasia
•Abnormalities found on ultrasound or in prenatal blood screening tests
•Amniotic fluid abnormalities
•Multiple births
•Exposure to medications and known teratogens
•Decreased fetal movement
Recommend Genetic counseling - allows families the opportunity to prepare for special needs of an unborn child and to consider options for current and future pregnancies
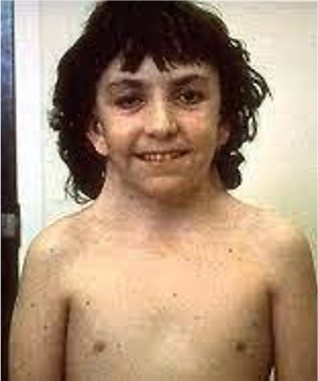
Neurofibromatosis (autosomal dominant)
type 1 most common (von Recklinghausen disease) tumors grow on nerves; skin changes, bone deformties; progressive disease; diagnosis = two or more clinical signs including – 2 or more neurofibromas, tumor on optic nerve, more than 6 café-au-lait spots(brown spot) > 5 mm diameter à high level of suspicion; treament is supportive
Huntington disease (autosomal dominant)
rare; usually presents in 30-40’s; progressive breakdown of nerve cells in brain; muscle problems, abnormal eye movements, impaired gait
Achondroplasia (autosomal dominant)

most common type of short-limbed dwarfism; can also be a mutation; short limbs, large head, average trunk; 4 ft 1in – 4ft 4in; sleep apnea, ear infections, spinal stenosis
Marfan syndrome (autosomal dominant)
affects connective tissue effects the heart, eyes, blood vessels, and bones; tall and thin with long arms, legs, fingers, and toes; treatment includes medications to keep blood pressure low, eyeglasses or contact lenses, and surgery.
Osteogenesis imperfecta type 1 (autosomal dominant)
brittle bone
Complications of Neurofibromatosis
•Headaches
•Hydrocephalus
•Scoliosis
•Cardiac defects, hypertension, seizures
•Vision and hearing loss
•Neurocognitive deficits
•Higher risk for neoplasms
Cystic fibrosis (Autosomal Recessive)
affects the cells that produce mucus, sweat, and digestive juices. It causes these fluids to become thick and sticky. They then plug up tubes, ducts, and passageways.
Phenylketonuria (Autosomal Recessive)
amino acid called phenylalanine to build up in the body; untreated phenylketonuria can lead to brain damage, intellectual disabilities, behavioral symptoms, or seizures; Treatment includes a strict diet with limited protein
Tay–Sachs (Autosomal Recessive)
destroys nerve cells in the brain and spinal cord; typically found in people with certain ancestry, such as Eastern European Jews; A fatty substance in the brain destroys nerve cells; Symptoms of slowed development usually appear around six months of age. Symptoms progress until they lead to death, often around age four; There is no cure
Hemophilia
prolonged bleeding due to insufficent clotting factors; hemophilia A, associated with a low level of factor 8 (factor VIII
Color blindness (red/green [most common], blue/green)
reduced ability to distinguish between certain colors.
Duchenne muscular dystrophy
progressive muscular weakness, typically in boys; no cure, but steroids may control symptoms
(The way they get up- gawar sign)
Trisomy 21 (Down Syndrome)
Cause
•Presence of all or part of an extra 21st chromosome
Characteristics
•Some degree of intellectual disability
•Characteristic facial features
•Other health problems (e.g., cardiac defects, visual and hearing impairment, intestinal malformations, and an increased susceptibility to infections)
Health Guidelines for Children with Down Syndrome #1
•Have your child evaluated by a pediatric cardiologist, including an echocardiogram
•Take your child for routine vision and hearing tests. By 6 months have your child seen by a pediatric ophthalmologist
•Make sure your child gets regular medical care, including recommended immunizations and a thyroid test at 6 and 12 months and then yearly
•Have your child follow a regular diet and exercise routine
•Make sure the child gets a cervical radiograph between 3 and 5 years of age to screen for atlantoaxial instability (C1 and C2).
Recommend genetic counseling
oMultidisciplinary care
Physical Characteristics of Turner Syndrome
•Loss of all or part of an X chromosome
•Webbed neck
•Low posterior hairline
•Wide-spaced nipples
•Edema of the hands and feet
•Amenorrhea
•No development of secondary sex characteristics
•Sterility
•Perceptual and social skill difficulties
Physical Characteristics of Klinefelter Syndrome
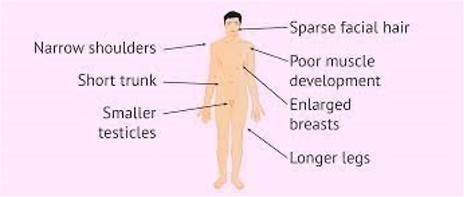
•One or more extra X chromosome; affects males
•Decreased facial hair
•Gynecomastia
•Decreased pubic hair
•Hypogonadism
•Underdeveloped testes,
•Taller than average by 5 years of age, with long legs and a short torso
•Cognitive impairments of varying degree: motor delay, speech or language difficulties, attention deficits, and learning disabilities
Clinical manifestations Associated with Fragile X Syndrome
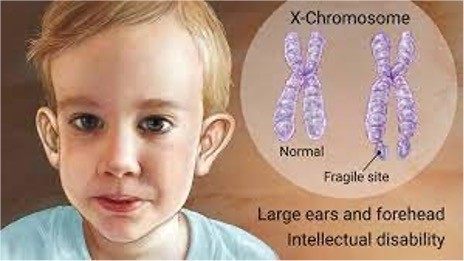
•Most common inherited cause of intellectual disability; can affect males and females but females typically have milder symptoms
•Minor dysmorphic features
•Developmental delay/Intellectual impairment
•Behavior problems:
•Attention deficits
•Hand flapping and biting
•Hyperactivity
•Shyness and social isolation
•Low self-esteem
•Gaze aversion
Nutritional deficiency
Iron deficiency, folic acid deficiency, pernicious anemia (deficiency in B12)
Toxin exposure
-lead poisoning
toxic effect on bone marrow, interferes with synthesis of heme- precursor to hgb
Aplastic anemia
failure of bone marrow to produce cells- acquired as an adverse reaction to medication (chemo, anticonvulsants).
-rare congenital bone marrow failure (fanconi anemia- autosomal recessive )
Hemolytic anemia
sickle cell anemia, thalassemia
Food high in iron
-red meat
-tuna & salmon
-eggs
-tofu
-leafy green veggies
-dried beans, peas and fruit
-enriched grains
-iron fortified breakfast cereals
Nursing assessment for aplastic anemia
History
Exposure to myelosuppressive medications or radiation therapy
Detailed family, environmental, and infectious disease history
Epistaxis, gingival oozing, or increased bleeding with menstruation
Headache, fatigue
Physical examination
Ecchymoses
Petechiae or purpura
Oral ulcerations
Tachycardia
Tachypnea
Complications of lead poisoning
Lower levels-Behavioral problems-Learning difficulties
Higher levels (requires chelation treatment)-Encephalopathy-Seizures-Brain damage
Types of Hemoglobinopathies
Thalassemia - inherited blood disorder that causes less hemoglobin; anemia; can be mild to severe
Sickle cell disease (SCD)- inherited, most common in autosomal recessive, African, Mediterranean, middle eastern, and Indian descent, hemoglobin SS disease is most common (crescent shaped blood cells)
Types of SCD:
Hemoglobin Ss (Hbss)
Hb "S" gene (abnormal form of hemoglobin) from each parent → sickle cell anemia;
More of the Hb is abnormal
more severe form of the disease
Hemoglobin SC (HbSC) - less severe form
one HbS gene and one HbC gene (another abnormal type)
Sickle cell trait-
Only have HbS from one parent
Symptoms of sickle cell disease
-Anemia
-Pain/sickle cell crisis
-acute chest syndrome
-stroke
-jaundice
-splenic pooling
-priapism
Treatment for Sickle cell disease
-pain medication
-hydration
-blood transfusions
-vaccinations
-folic acid for anemia
-eye exams to assess retinopathy
-Hydroxyurea- medication that may reduce frequency of pain crisis and ACS; makes RBC less likely to turn into sickle shape
-Bone marrow transplant- for children with severe complications
Thalassemia
alpha-thalassemia -severity depends on number of gene mutations you inherit; ; synthesis of the a chain of the hemoglobin protein is affected
beta-thalassemia- severity depends on part of the hemoglobin molecule is affected. the B-globulin chain in hemoglobin synthesis is reduced or entirely absent; severe hemolytic anemia and chronic hypoxia
Thalassemia minor (also called B-thalassemia trait): leads to mild microcytic anemia; often no treatment is required.
Thalassemia intermedia: child requires blood transfusions to maintain adequate quality of life.Thalassemia major: to survive the child requires ongoing medical attention, blood transfusions, and iron removal; Cooley's Anemia
Left untreated, B-thalassemia major is fatal by age 5 years, but use of blood transfusions and chelation therapy increases life expectancy of these children
Hemosiderosis
Excessive supply of iron; accumulation in tissues
Result of rapid hemolysis of RBCs, decrease in hemoglobin production, increased absorption of dietary iron in response to the severely anemic state.
excess iron is deposited in the body's tissues, causing bronze pigmentation of the skin, bony changes, and altered organ function, particularly in the cardiac system, splenomegaly, endocrine abnormalities, osteoporosis, liver and gallbladder disease, and leg ulcers.
Thalassemia management
PRBC transfusions(blood transfusion) as prescribed to maintain an adequate level of hemoglobin for oxygen delivery to the tissues
-Excess iron is removed by chelation therapy. Administer the chelating agent deferoxamine with the transfusion.
Deferoxamine binds to the iron and allows it to be removed through the stool or urine. Oral deferasirox may also be prescribed.
Glucose-6-Phosphate Dehydrogenase
Deficiency
G6PD -an enzyme that helps RBC's work properly is insufficient or abnormal; X-linked recessive
causes red blood cells to break down (hemolysis) in response to certain medications, infections, or other stressors.
Triggers that may result in oxidative stress and hemolysis-
• bacterial or viral illness
exposure to certain substances such as medications (e.g., sulfonamides, sulfones, malaria-fighting drugs [such as quinine], or methylene blue [for treating urinary tract infections]), naphthalene (an agent in mothballs), or fava beans.
• Tea colored urine, splenomegaly
* Administer 02; improve one trigger or illness is removed
clotting disorders
-Idiopathic thrombocytopenia purpura (ITP)
-Henoch-Schonlein purpura
-Disseminated intravascular coagulation (DIC)
-Factor deficiencies
-Hemophilia A (factor VIII deficiency)
-von Willebrand disease
Idiopathic Thrombocytopenia Purpura
Immune response following viral infection that destroy platelets
-Normal platelet count -150,000 to 450,000 platelets per microliter of blood
-Petechiae:Pinpoint hemorrhages occurring on the body that do not blanch to pressure,
-Purpura:Larger purplish areas of hemorrhage in which blood collects under the tissues; complication = bleeding into organs and intracranial pressure - although both rare
* Platelet counts below 10,000/mm3, corticosteroids may be administered for 2 to 3 weeks
• Single dose of intravenous immunoglobulin (IVIG) may be used as an adjunct
-Platelet transfusions are not indicated unless life-threatening bleeding is present.
-Refer the child for follow-up care with a pediatric hematologist.
-Usually, self-limiting
Henoch-Schönlein Purpura
Mostly male children
Associated with viral or bacterial illness- often respiratory
Vasculitis with immunoglobulin A (IgA) -dominant immune deposits affecting small vessels in the skin, gut, and kidney
Benign in most children and resolves with no issues
nephrotic syndrome may occur as a result of renal injury, and those children may have
hypertension.
Pulmonary, cardiac, and neurologic complications can also occur.
Treatment with corticosteroids, such as prednisone, may be helpful in children with severe joint or GI manifestations
Disseminated Intravascular Coagulation
Complex condition leads to activation of coagulation
Usually occurs in critically ill childrenSeptic shock, endotoxins, viruses, tissue necrosis, cancer treatments
Deficiencies of coagulation and anticoagulation pathways occur
Hemorrhage and organ tissue damage result and can be irreversible if not recognized and treated immediately.
Treat underlying issue -ex. infection → antibiotics
Hemophilia
group of X-linked recessive disorders that result in deficiency in one of the coagulation factors in the blood
transmitted by carrier mothers to their sons, so usually only males are affected by hemophilia
coagulation factors in the blood are essential for clot formation either spontaneously or from an injury, and when factors are absent bleeding will be difficult to stop
The most common= hemophilia A - deficiency of factor VIII
Prevent bleeding
Helmets, avoid contact sports, medical alert bracelet
Von Willebrand Disease
Mild bleeding disorder
• genetically transmitted bleeding disorder that may affect both genders and all races
deficiency in von Willebrand factor (vWF)
serves two functions:bind with factor VIII, protecting it from breakdownserve as the "glue" that attaches platelets to the site of injury
Cancer in Children
-The most common childhood cancers in order of frequency-
-Leukemia, CNS tumors, lymphoma, neuroblastoma (adrenal glands), rhabdomyosarcoma (muscles), Wilms tumor (kidney), bone tumors, and retinoblastoma
Warning signs of cancer-
-most often related to changes in blood cell production; changes in blood cell production may result in fatigue, pallor, frequent or severe infection, or easy bruising
-a result of compression, infiltration, or obstruction caused by the tumor; infiltration, obstruction, or compression by a tumor may result in bone or abdominal pain, swelling, unusual discharge
Function of:
1. Erythrocytes/RBC’s
2. Thrombocytes/Platelets
3. Leukocytes/WBC
1. carry oxygen throughout body
2. clotting
3. fight infection
Low erythrocyte/rbc- anemia(pica, pale, tired)
Low platelets- prolonged bleeding
types of immunity
Passive
-Antibodies received from an external source (mother to baby, IVIG)
Cellular
-Antibodies produced by native T-cell lymphocytes (thymus)
Humoral
-Antibodies produced by native B-cell lymphocytes (bone marrow)
Assessments for Wiskott-Aldrich
Syndrome
History of petechiae
• Bloody diarrhea or bleeding episode in the first 6 months of life
History of hematemesis or intracranial or conjunctival hemorrhages
Eczema
Laboratory findings of low IgM concentration, elevated IgA and IgE concentrations, and normal IgG concentrations
Ten Warning Signs of Primary
Immunodeficiency
Four or more new episodes of acute otitis media in 1 year
Two or more episodes of severe sinusitis
Treatment with antibiotics for 2 months or longer with little effect
Two or more episodes of pneumonia in 1 year
Failure to thrive in the infant
Recurrent deep skin or organ abscesses
Persistent oral thrush or skin candidiasis after 1 year of age
History of infections requiring IV antibiotics to clear
Two or more serious infections such as sepsis
Family history of primary immunodeficiency
Signs and Symptoms of HIV Infection in
Children
-Failure to thrive
-Recurrent bacterial infections
-Opportunistic infections
-Chronic or recurrent diarrhea
-Recurrent or persistent fever
-Developmental delay
-Prolonged candidiasis
food allergies
-dairy (cows milk)
-eggs
-penuts
-tree nuts
-fish and shellfish
-wheat
-soy
PRIMARY IMMUNODEFICIENCIES
Wiskott-Aldrich Syndrome/ Deficiency -X-linked genetic disorder; defective gene that results in immunodeficiency, eczema, and thrombocytopenia, autoimmune hemolytic anemia, neutropenia, skin or cerebral vasculitis, arthritis, inflammatory bowel disease, and renal disease
Severe Combined Immune Deficiency (SCID) - X-linked or autosomal recessive disorder; it can occur in girls or boys. SCID is
characterized by absent T-cell and B-cell function.
Nursing Assessment of Severe Combined
Immune Deficiency (SCID)
-Chronic diarrhea
-Failure to thrive
-History of severe infections early in infancy
-Persistent thrush
-Adventitious sounds related to pneumonia
-Lab findings of very low levels of immunoglobulins
Goals of Nursing Care of the Child with HIV
Infection or Other Chronic Immune Disorder
-Avoiding infection
-How can we avoid infection?
-Promoting compliance with the medication regimen
-Promoting nutrition
-Providing pain management and comfort measures
-Educating the child and caregivers
-Providing ongoing psychosocial support
Common Laboratory and Diagnostic Tests
for Systemic Lupus Erythematosus (SLE)
-SLE definition: chronic multisystem autoimmune disorder with periods of exacerbation and remissions; inflammatory response
Laboratory testing includes:
-CBC (decreased Hgb, Hct)
-Platelet count (decreased)
-WBC (decreased)
Treatment and support - treating the inflammation; NSAIDs, corticosteroids, antimalarials (can reduce autoantibodies), dialysis if in renal failure
(molar/butterfly rash (erythema on cheeks))
Pituitary Disorders
Growth hormone deficiency
Precocious puberty
Delayed puberty
Diabetes insipidus
Syndrome of inappropriate antidiuretic hormone secretion
Growth Hormone deficiency
-hypopituitarism or dwarfism, is characterized by poor growth and short stature
-result of the failure of the anterior pituitary or hypothalamic stimulation on the pituitary to produce sufficient GH.
-lack of GH impairs the body’s ability to metabolize protein, fat, and carbohydrates.
-injury to, or destruction of, the anterior pituitary gland or hypothalamus; tumor, trauma, infection
-genetic syndrome, such as Prader–Willi syndrome or Turner syndrome, or the result of a genetic mutation or deletion
Goal = 3 to 5 in in linear growth in the first year of treatment Treatment stops when the epiphyseal growth plates fuse
Precocious Puberty
-Development of sexual characteristics before the usual age of pubertal onset ->secondary sex characteristics develop in girls before the age of 8 years and in boys younger than 9 years
-more common in females, majority of the time the cause is unknown in females
-premature activation of the hypothalamic–pituitary–gonadal system
-Short stature if untreated ->premature closure of growth plates
-Must determine the cause; GnRH analog to halt or reverse growth and development
Delayed Puberty
-delayed secondary sexual development
-Girls -if the breasts have not developed by age 12
-boys when no testicular enlargement or scrotal changes have occurred by age 14
-constitutional delay- most common cause, hereditary pattern of growth and development (or a “late bloomer”)
-Therapeutic management involves administering testosterone (males) or estradiol-conjugated estrogen; usually necessary for only a short time to get puberty started
Central Diabetes Insipidus (dehydrated)
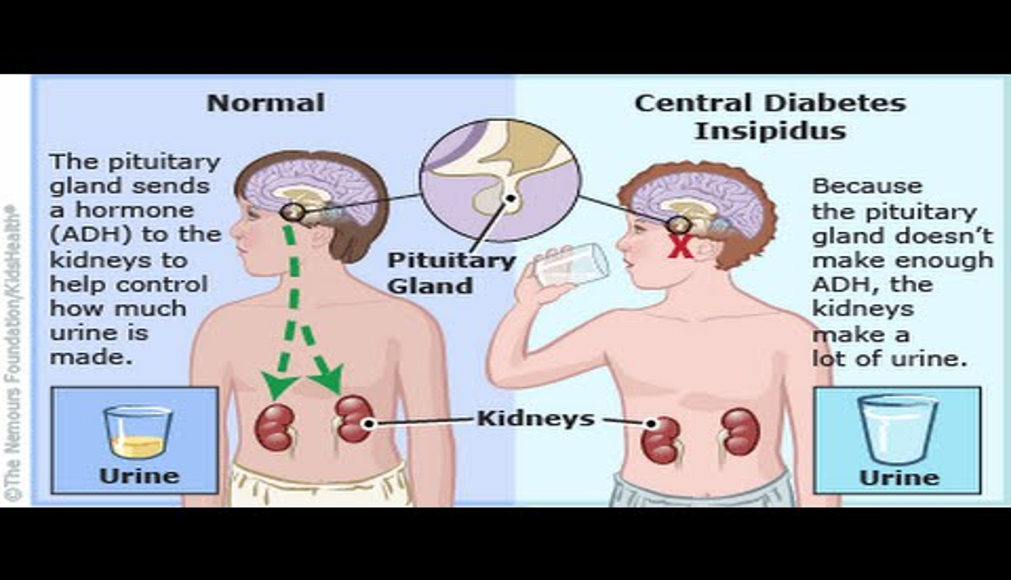
HYPERNATREMIA
•Body produces high urinary output and does not retain water in the correct amount
-low levels Antidiuretic hormone (ADH) aka Vasopressin
-ADH is made in hypothalamus and stored in the kidney
-Damage to pituitary gland, tumor, head injury, illness
•Symptoms –
-Polyuria and polydipsia
-Kidney loses massive amounts of water and retains sodium in the serum
•Treatment
-replacement of ADH/vasopressin à Desmopressin (brand name -DDAVP); can be taken oral or nasal
-low sodium and low protein
-remove tumor if present
Syndrome of Inappropriate Antidiuretic Hormone (SIADH)- over hydrated
Too much ADH- HYPONATREMIA
-Causes water retention(low urinary output), decreased serum sodium due to hemodilution, and extracellular fluid volume expansion.
-Caused by CNS infections such as meningitis, head trauma, brain tumors, intracranial surgery, and certain medications such as analgesics, barbiturates, or chemotherapy.
-May be caused by excessive treatment of DI
Therapeutic management -correcting the underlying disorder, fluid restriction, and intravenous sodium chloride administration to correct hyponatremia and increase serum osmolality
Hyperthyroidism symptoms
Rare in children
excessive T3,T4
TSH low
Treated with destruction of thyroid gland
Symptoms
-diarrhea
-bulging eyes
-tachycardia
-weight loss
-amenorrhea
-localized edema
-always hot
Hypothyroidism symptoms
can be congenital or acquired
-Certain populations at risk (Downs, maternal hypothyroidism)
-Decreased thyroid hormones
Decreased T3, T4
TSH usually elevated
Lifelong thyroid supplementation
Symptoms
-lethargy
-dry skin
-constipation
- always cold
-facial edema
-brittle nails/hair
-weight gain
bradycardia
Acquired Hypothyroidism
•Hashimoto
•antibodies develop against the thyroid gland, causing the gland to become inflamed, infiltrated, and progressively destroyed
•Management involves oral sodium L-thyroxine, Synthroid
Symptoms-
•goiter -enlargement of the thyroid gland
•Deep tendon reflexes may be sluggish and the face, eyes, and hands may be edematous
•thinning or coarse hair, muscle hypertrophy with muscle weakness, and signs of delayed or precocious puberty.
•Diagnostic evaluation involves serum thyroid function studies
Hyperthyroidism
•Hyperfunction of the thyroid gland, excessive levels of circulating thyroid hormones
•Uncommon in children, 5 times more in girls than boys
•increased rate of growth; weight loss despite an excellent appetite; hyperactivity
•Usually develop a goiter
•Congenital hyperthyroidism -neonatal thyrotoxicosis - occurs in infants of mothers with Graves disease- life threatening, self-limiting disorder lasting 2 to 4 months
•Therapeutic management –decrease thyroid hormone levels. Current treatment involves antithyroid medication, radioactive iodine therapy, and subtotal thyroidectomy. First-line treatment involves methimazole (MTZ, Tapazole) - blocks the production of T3 and T4
Signs of Thyroid Storm
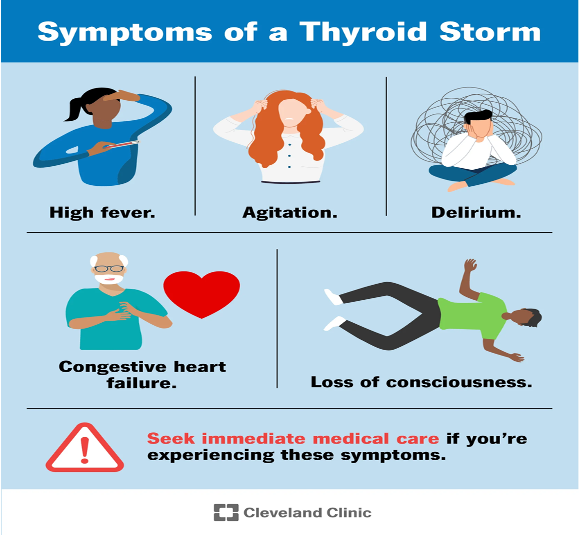
Acute, life-threatening, hypermetabolic state severely elevated Thyroid Hormone
-Graves disease, neonatal graves, thyroid nodules
Symptoms:
•Sudden onset of severe restlessness and irritability
•Fever
•Diaphoresis
•Severe tachycardia
Treatment:
•antithyroid medications, potassium iodide, beta blockers, and steroids.
Congenital adrenal hyperplasia
-adrenal glands don’t produce enough cortisol, adrenal gland enlarges to compensate
-Males=enlarged penis, puberty by 2-3; females = ambiguous genitalia(can't tell if boy or girl), fertility issues
-Treatment = hormone replacement, steroids
Cushing syndrome
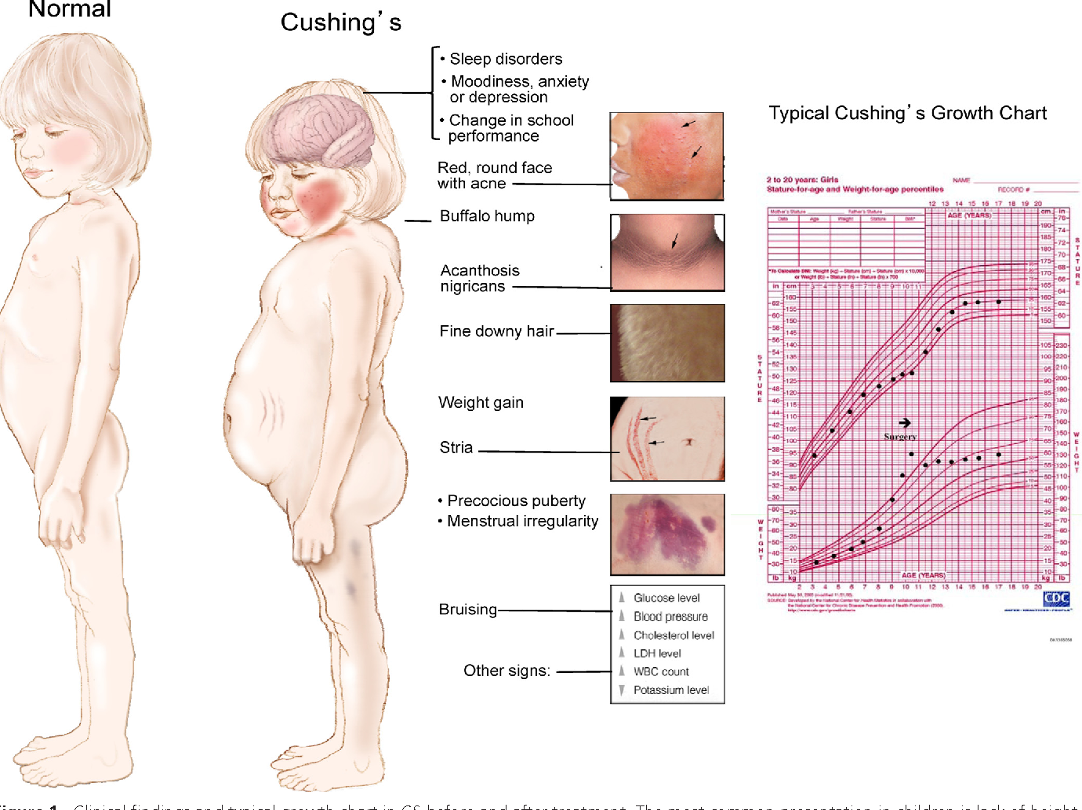
condition from high cortisol levels; caused by use of steroids or overproduction by adrenal glands
-red round face
-hunch back(buffalo hump)
-carry fat in stomach (bulging0
Addison disease
adrenal insufficiency – weakness, fatigue, fragile and thin skin
Polycystic Ovary Syndrome
testosterone production by the ovaries and adrenal cells is excessive, causing hirsutism, balding, acne, increased muscle mass, and decreased breast size.
Role of Insulin
-A hormone made by the islet cells of the pancreas
-Controls the amount of sugar in the blood by moving it into the cells, where it can be used by the body for energy.
Diabetes Type 1
autoimmune disorder
-Destruction of beta cells of pancreas ->inadequate insulin secretion ->hyperglycemia
-Kidneys try to lower blood glucose ->glycosuria and polyuria
-Protein and fat are used for energy -> buildup of ketones and acidosis
Diabetes Type 2
Pancreas produces insulin but:
-Body is resistant to insulin or there is inadequate insulin produced
-Overtime, insulin production decreases
DKA
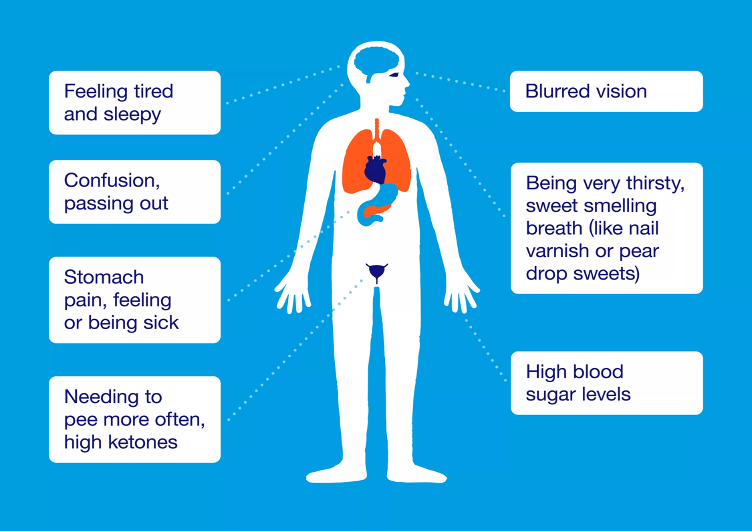
Body is using fat instead of glucose for energy)
-producing excess blood acids -ketones
-If unrecognized or not treated, DKA – fat catabolism develops
Symptoms:
-anorexia, nausea and vomiting, lethargy, stupor, altered level of consciousness, confusion, decreased skin turgor, abdominal pain, Kussmaul respirations (deep, rapid, labored) and air hunger, fruity (sweet-smelling) or acetone breath odor, presence of ketones in urine and blood, tachycardia, and, if left untreated,.
Diabetic Ketoacidosis - DKA management
•blood glucose monitoring
•Hemoglobin A1C – shows blood glucose control over previous 3 months
• daily injections of insulin and/or administration of oral hypoglycemic medications
• a realistic and well-balanced diet
•an exercise program
•self-management and decision-making skills.
Insulin Type
Rapid acting- 15 min
Short acting- 30 min-1hr
Intermediate acting- 2-4 hrs
Long acting- 2-4hrs
Complications of Diabetes Mellitus
Damage to nerves and vessels d/t prolonged exposure to high blood glucose levels
•Failure to grow
•Delayed sexual maturation(erection)
•Poor wound healing
•Recurrent infections (especially of the skin)
•Retinopathy
•Neuropathy
•Vascular complications
•Nephropathy
•Cerebrovascular disease
•Peripheral vascular disease
•Cardiovascular disease
The nurse is caring for a child diagnosed with juvenile diabetes. Which of the following medical treatments would be appropriate for this child?
a. Surgery
b. Irradiation
c. Radioactive iodine
d. Glucose monitoring
d. Glucose monitoring. Glucose monitoring is an intervention appropriate for managing diabetes.
The nurse is caring for a child with diabetes insipidus. Which of the following clinical manifestations would be expected for this child?
a. Urine specific gravity greater than 1.005
b. Serum osmolality greater than 300 mOsm/kg
c. Increased urine osmolality
d. Hyponatremia
b. Serum osmolality greater than 300 mOsm/kg. Serum osmolality greater than 300 mOsm/kg is a clinical manifestation of diabetes insipidus.
The parents of a child with a bleeding disorder ask the nurse about appropriate activities and sports that they should encourage the child to participate in. What activity would be the safest for the nurse to suggest?
Soccer
Gymnastics
Rugby
Swimming
Swimming
A nurse is administering a blood transfusion to a child. About 35 minutes after beginning the transfusion, the child develops pruritus(itching) and urticaria(hives). Some wheezing is noted. Which action would the nurse take first?
Discontinue the transfusion.
Obtain a blood culture.
Give an iron-chelating agent.
Ask the health care provide for a prescription for a diuretic.
Discontinue the transfusion.
A nurse is giving instructions to the father of a boy who is receiving chemotherapy (including methotrexate) regarding how best to care for the boy during this period of treatment. What should the nurse mention to him?
Keep him away from people with known infections
Give him aspirin to help manage pain
Be sure that the boy receives only live-virus vaccines
Give the boy folic acid supplements
Keep him away from people with known infections
The nurse is preparing to post a sign above the crib of an infant with a Wilms tumor. Which statement should the nurse post?
"Do not palpate abdomen."
"No intramuscular injections."
"No milk or milk products allowed."
"No blood sampling in lower extremities."
"Do not palpate abdomen."
A child receiving chemotherapy wants to have a large birthday party and invite all the classmates. When the parent asks the nurse about this, how should the nurse respond?
"That will be a good way to cheer your child up!"
"It is better to avoid large groups right now."
"What about taking your child to a movie instead?"
"We can have the party here in the hospital play room."
"It is better to avoid large groups right now."
The nurse is instructing the parents of a child with sickle cell anemia on safety precautions. What should the nurse emphasize during this teaching?
Suggest the child participate in sports activities without restriction.
Treat upper respiratory infections with over-the-counter medication.
Ensure a consistent and daily intake of adequate fluids to prevent dehydration.
Remind parents that the child should avoid immunizations to prevent the introduction of bacteria into the body.
Ensure a consistent and daily intake of adequate fluids to prevent dehydration.
A 12-year-old child is suspected of having Hodgkin lymphoma. When preparing the child and family for diagnostic testing, which test would the nurse describe as being used to confirm the diagnosis?
24-hour urine test
lymph node biopsy
chest computed tomography
liver function tests
lymph node biopsy
The nurse is assessing children in an ambulatory clinic. Which child would be most likely to have iron-deficiency anemia?
A 3-month-old infant who is totally breastfed
A 15-year-old adolescent who has heavy menstrual periods
An 8-year-old child who carries lunch to school
A 7-month-old infant who has started table food
A 15-year-old adolescent who has heavy menstrual periods
A child allergic to insect stings presents to the school nurse stating, "A bee stung me on the playground." Which action by the nurse is priority?
Notify the client's caregivers and primary health care provider
Assess the client's airway and breathing rate
Administer epinephrine subcutaneously to the client
Locate the stinger and remove it with tweezers
Assess the client's airway and breathing rate
The nurse is reviewing the health records of an 18-year-old with Guillain-Barré syndrome (GBS). The nurse anticipates finding what information in the client's health history?
an upper respiratory viral infection
a history of drug use
a serious automobile accident
a recent orthopedic injury
an upper respiratory viral infection
The parents are concerned their child with atopic dermatitis is having an allergic reaction to diphenhydramine because the child became “sleepy and has a dry throat” after receiving the medication. Which education provided to the parents by the nurse is most important?
“Children with eczema are more likely to have a medication allergy.”
“Your child is exhibiting signs and symptoms of an allergic reaction.”
“Side effects, such as drowsiness and dryness, do not indicate an allergy.”
“Toxic amounts of diphenhydramine can cause this response in children.”
“Side effects, such as drowsiness and dryness, do not indicate an allergy.”
The nurse in the emergency department is examining an 18-month-old child who recently received a first dose of penicillin. The nurse notes lip edema, urticaria, stridor, and tachycardia. Which action will the nurse take next?
Begin cardiopulmonary resuscitation (CPR).
Administer epinephrine.
Obtain intravenous (IV) access.
Gather tracheal intubation equipment.
Administer epinephrine.
Food allergies have become more and more common in the last few decades. What are some common food allergies of childhood? Select all that apply.
Eggs
Peanuts
Cheerios
Milk
Apples
eggs
penuts
milk
The nurse is assisting with skin testing for allergies in a pediatric client. What will the nurse do to ensure the results are accurate?
Be certain the child has not received an antihistamine in the past 8 hours
Read the test results within 40 minutes of administration.
Inject the allergens into the muscle of the child's forearm.
Apply a topical diphenhydramine cream to the site following each injection.
Be certain the child has not received an antihistamine in the past 8 hours
The nurse is speaking with the parent of a child who has experienced an allergic reaction to peanuts. Which statement by the parent would indicate a need for further education?
“If my child’s tongue or lips start to itch, my child may be having an anaphylactic reaction.”
“If my child has shortness of breath, my child may be having a symptom of anaphylaxis.”
“If my child has gastrointestinal upset, my child is not having anaphylactic shock.”
“If my child has high blood pressure and low heart rates, my child is not having an anaphylactic reaction.”
“If my child has gastrointestinal upset, my child is not having anaphylactic shock.”
Types of Therapy
-behavioral therapy
-play therapy
-cognitive-behaviorla therapy
-dialectical behavioral therapy
-family therapy
-group therapy
-milieu therapy
-individual therapy
-hypnosis
Behavior Management Techniques
•Set limits and hold child responsible for behavior
•Do not argue, bargain, or negotiate about the limits set
•Provide consistent caregivers and establish a daily routine
•Use a low-pitched voice and remain calm
•Redirect the child’s attention when needed
•Ignore inappropriate behaviors
•Praise the child’s self-control efforts
•Use restraints only when necessary
Autism Spectrum Disorder
-Onset in infancy or early childhood
-Spectrum of autism disorder ranges from mild to severe
-From intellectually disabled normal to high intelligence levels
Warning signs
-Does not imitate
-Lack of interest in joint attention
-Eye contact abnormalities
-Delayed language development
-Failure to develop symbolic-imaginative play
-Losing language or social skills at any age (Volkmar, 2019)
Attention-Deficit/Hyperactivity Disorder
Most common neurodevelopmental disorder of childhood
-Disruption in learning ability, socialization, and compliance, -> high demands on the child, parents, teachers, and community
Often have a comorbidity
-such as oppositional defiant disorder
-conduct disorder
-anxiety disorder
-depression
-less severe developmental disorder
-auditory processing disorder
-learning or reading disabilities
Diagnosis of Attention-Deficit/Hyperactivity Disorder
•Careless mistakes on schoolwork
•Doesn’t listen
•Doesn’t follow through
•Doesn’t complete tasks
•Doesn’t understand instructions
•Poorly organized
•Avoids, dislikes, or fails to engage in activities requiring mental effort
•Loses things needed for task completion
Anorexia nervosa
low body weight, fear of gaining weight, distorted body image
-characterized by dramatic weight loss as a result of decreased food intake and sharply increased physical exercise
Bulimia
distortion of body image, bouts of extreme overeating followed by purging, fasting, over-exercising
-refers to a cycle of normal food intake, followed by binge eating and then purging; callouses, redness on knuckles
Pica
craving & chewing substances with no nutritional value
Complications of Anorexia Nervosa and Bulimia
-Fluid and electrolyte imbalance
-Decreased blood volume
-Cardiac arrhythmias
-Esophagitis
-Rupture of the esophagus or stomach
-Tooth loss
-Menstrual problems
-Mortality rate may be as high as 18%
Risk Factors for Suicide
•Previous suicide attempt
•Change in school performance, sleep, or appetite
•Loss of interest in formerly favorite social or school activities
•Feelings of hopelessness or depression
•Statements about thoughts of suicide
•Giving away belongings
•Having a plan for suicide or self-harm!!!
Types of Anxiety Disorders
•Generalized anxiety disorder (GAD) -unrealistic concerns over past behavior, future events, and personal competence.
•Social phobia -persistent fear of speaking or eating in front of others, using public restrooms, or speaking to authorities
•Selective mutism -persistent failure to speak in social situations
•Obsessive-compulsive disorder (OCD) - compulsions the child performs to reduce anxiety about obsessions
•Posttraumatic stress disorder (PTSD) -occurs after a child experiences a traumatic event, later experiencing physiologic arousal when a stimulus triggers memories of the event.
Therapeutic Management of Anxiety Disorders
-Pharmacologic agents and psychological therapies
-Anxiolytics or antidepressants are the most common pharmacologic approaches
-Cognitive-behavioral therapy; individual, family, or group psychotherapy; and other behavioral interventions such as relaxation techniques
Child maltreatment
associated with the development of anxiety and depressive disorders, suicidal ideation and attempts, and alcohol and drug use
Physical abuse
injuries that are intentionally inflicted
Sexual abuse
oinvolvement of the child in any activity meant to provide sexual gratification to an adult.
Neglect
failure to provide a child with appropriate food, clothing, shelter, medical care, and schooling
Warning Signs of Medical Child Abuse
•Child with one or more illnesses that do not respond to treatment or that follow a puzzling course; a similar history in sibling
•Symptoms that do not make sense or that disappear when the perpetrator is removed or not present; the symptoms are witnessed only by the caregiver
•Physical and laboratory findings that do not fit with the reported history
•Repeated hospitalizations failing to produce a medical diagnosis, transfers to other hospitals, discharges against medical advice
•Parent who refuse to accept that the diagnosis is not medical
The nurse caring for a child with autism coaches the child to change reactions by replacing automatic negative thought patterns with alternative ones. What treatment is the nurse employing?
a. Behavioral therapy
b. Play therapy
c. Milieu therapy
d. Cognitive therapy
d. Cognitive therapy. Cognitive therapy involves coaching the child to change reactions by replacing automatic negative thought patterns with alternative ones.
Is the following statement true or false?
The nurse caring for a child with bulimia explains to the parents that bulimia refers to a cycle of normal food intake, followed by binge-eating and then purging.
True. Bulimia refers to a cycle of normal food intake, followed by binge-eating and then purging.
What is the most common type of child abuse reported in the healthcare setting?
A) Physical abuse
B) Emotional abuse
C) Sexual abuse
D) Neglect
D) Neglect
Which of the following is NOT a common indicator of physical abuse in a child?
A) Unexplained bruises in various stages of healing
B) Burns or scalds in unusual patterns
C) Frequent absences from school without explanation
D) Fecal soiling
C) Frequent absences from school without explanation
As a nurse, what is your responsibility when you suspect child abuse or neglect?
A) Discuss your concerns with the child's family to get their perspective
B) Document your suspicions in the patient's medical record and take no further action
C) Report your suspicions to the appropriate authorities as mandated by law
D) Ignore your suspicions unless there is clear evidence of abuse
C) Report your suspicions to the appropriate authorities as mandated by law
Which of the following statements about mandated reporting of child abuse is TRUE?
A) Mandated reporters are only required to report abuse if they witness it firsthand.
B) Mandated reporters can choose not to report abuse if they believe it was unintentional.
C) Mandated reporters can face legal consequences for failing to report suspected abuse.
D) Mandated reporters are required to confront the suspected abuser before reporting.
C) Mandated reporters can face legal consequences for failing to report suspected abuse.
Which of the following statements about interviewing a child who may have experienced abuse is FALSE?
A) It is important to interview the child alone, without the presence of their caregiver.
B) Closed-ended questions should be used to guide the conversation and gather specific information.
C) Leading questions should be avoided to prevent influencing the child's responses.
D) It is acceptable to promise the child confidentiality to encourage them to disclose abuse.
D) It is acceptable to promise the child confidentiality to encourage them to disclose abuse.
Risks Factors for Respiratory Arrest in Children versus Adults
•Smaller airways than adults
•Underdeveloped immune systems
•Lack motor coordination to save self after falling into water
•Susceptible to choking on food and small objects
•Higher risk for sudden infant death syndrome
Nursing Management of a Child with a Pediatric Emergency
•Maintaining a patent airway
•Providing supplemental oxygen
•Assisting ventilation
•Monitoring for changes in status
•Offering support and education to the child and family
RAPID CARDIOPULMONARY ASSESSMENT
Airway Evaluation and Management – patency(clear), secretions, obstructions
Breathing Evaluation and Management – look, listen, feel; resp distress 100% O2 and begin ventilation, may need intubation
Circulation Evaluation and Management - HR, pulses skin color and temperature, (BP), cardiac rhythm,and level of consciousness; brachial artery in infant
AVPU
•Alert
•Responsive to Voice
•Responds to Pain
•Unresponsive
Using Automated External Defibrillation
AHA has recommended that an AED can be used for children who are older than age 1 year who have no pulse and have suffered a sudden, witnessed collapse- arrhythmia often cause
Compression to infant
Two fingers placed one finger breadth below nipple line
One person CPR
-30 Compressions to 2 breaths
Two person CPR
-15 compression to 2 breaths
Compression to child
Heal of hand pressing on sternum at nipple line (adult position for larger child)
One person CPR
-30 compressions to 2 breaths
Two person CPR
-15 compressions to 2 breaths
Jaw Thrust technique
if cervical spine injury suspected
DO NOT US HEAD TILT-CHIN LIFT
Forms of Vascular Access
-Peripheral IV route
-Central IV route
-Saphenous vein cutdown
-Intraosseous access (anterior tibia preferred)
ABCs of Life Support
Primary Survey
-Airway
-Breathing
-Circulation
Secondary Survey
-Disability
-Exposure
Neurologic Assessment of a Child with a Pediatric Emergency
•Evaluate level of awareness (sensorium) in an older child
•Evaluate interest in environment in an infant
•Evaluate the child’s head
•Assess the eyes
•Evaluate the child’s face
•Evaluate spontaneous movement of extremities
•May use Pediatric Glasgow Coma Scale
Shock
•Life threatening condition brought on by sudden drop in blood flow through the body
Signs and symptoms:
•Pallor
•Hypotension
•arrythmias
•Respiratory distress
•Delayed capillary refill
•Weak distal pulses
Septic shock – severe infection leads to cardiac dysfunction
Hypovolemic shock– blood loss
Common Types of Emergencies in Children
•Respiratory arrest
•Shock
•Cardiac arrhythmias and arrest – brady, tachy, asystole
•Near drowning – 3rd leading cause of preventable death
•Poisoning – suspect toxic ingestion if sudden deterioration
Traumatic injury - leading cause of death in children and adolescents is unintentional injuries
Respiratory Patterns
Tachypnea
•Increased respiratory rate
Hypoventilation
•Decrease in depth and rate of respiration
Periodic breathing
•Regular breathing with occasional short pauses
Increased work of breathing
•Use of intracostal muscles or presence of retractions
Tachyarrhythmia- beat 100 min or more
Compensated SVT-hr 220
Uncompensated SVT- hr 220
Ventricular tachycardia- normal to 220
Causes of Sudden Cardiac Arrest in Children
•Electrolyte abnormalities
•Toxic drug ingestion
•History of a serious primary congenital or acquired cardiac defect
•Potentially lethal arrhythmias, such as prolonged QT syndrome
•Hyper- or hypotrophic cardiomyopathy
•Traumatic cardiac injury or a sharp blow to the chest, known as commotio cordis
Laboratory and Diagnostic Tests When Assessing Respiratory Status
Arterial or capillary blood gases
•Measures the amount of oxygen, carbon dioxide in blood. It also checks the acidity or pH level.
Pulse oximetry
Chest radiograph
•Alterations in normal anatomy or lung expansion
•Evidence of pneumonia, tumor, or foreign body
AHA Chain of Survival- Child
1.Prevention of cardiac arrest and injuries
2.Early CPR
3.Early access to emergency response system
4.Early advanced care (pediatric advanced life support [PALS])
5.Integrated post–cardiac arrest care
NALOXONE
Narcan
Opioid overdose treatment
Nasal spray
DOPE Mnemonic for Intubation Troubleshooting
Displacement
•Tracheal tube is displaced from the trachea
Obstruction
•Tracheal tube is obstructed (e.g., with a mucous plug)
Pneumothorax
Equipment failure
•Disconnected oxygen supply
•Leak in the ventilator circuit
•Loss of power
Drugs Administered Through Tracheal Tubes
“LEAN”
-L: lidocaine
-E: epinephrine
-A: atropine
-N: naloxone
The nurse assisting a child in respiratory distress inserts the rubber connecting tube of an inflatable silicone mask blindly into the airway to form a seal. What method of resuscitation is being performed by the nurse?
a. Anesthesia bag
b. Flow-inflating ventilation system
c. Bag-valve-mask device
d. Laryngeal mask airway
d. Laryngeal mask airway. Using this method, the nurse inserts the rubber connecting tube of an inflatable silicone mask blindly into the airway to form a seal.
Is the following statement true or false?
The nurse accessing a vein to manage a child while CPR is in progress uses the recommended route, the saphenous vein.
False. The femoral route is best for obtaining central venous access while CPR is in progress.
The nurse is caring for a child with respiratory distress who is being treated with narcotics for pain related to leukemia. For what condition should the nurse monitor in this child?
a. Hyperventilation
b. Hypoventilation
c. Tachypnea
d. Periodic breathing
b. Hypoventilation. A child who is being treated with narcotics for pain related to leukemia should be monitored for hypoventilation.
Infancy Erikson stage
Basic trust versus mistrust.
Toodler Erickson stage
autonomy versus shame and doubt
· Learning to do for themselves
· Independence
preschool age Erickson stage
Initiative versus guilt
· Pride in accomplishments; guilt when not capable
School age erickson stage
Industry versus inferiority
· Interested how things are made
· Success on personal/ social tasks
· Outside activities
· Peers
· Learning
Adolescence Erickson stage
identity versus identity confusion
· Focus on body changes, importance of peer culture become primary
Newborn
Weight
Double weight by 4-5 months (6 months)
Triple weight by 12 months
(grow rapidly first 6 months)-lenght increased by 50% by 12 months
Anterior fontanelle-12-18 months
Posterior fontanelle-2 months
Common developmental concerns
o Colic- constant crying
o Spitting up
o Thumb sucking, pacifiers
o Teething
Primitive reflexes
present at birth
Protective reflexes
develop as soon as primitive reflexes disappear
Newborn vitals
Resp- 30-60 newborn (20-30 12 monthly)
Pulse- 120-40 newborn (100 1 year old)
BP- 60/40 (newborn) (110/5 12 month old)
Gross motor(CEPHALOCAUDAL) Infant
- 1 month- lifts and turns head when prone, head lag
- 2 months- raises head and chest
- 3 months- raises head 45 degrees in prone, slight head lag
- 4 months- lifts head and looks around, rolls from prone to supine
- 5 months- rolls supine to prone and back, sits upright w/ support
- 6 months- tripod sits
- 7 months- sits alone with use of hands
- 8 months- sits unsupported
- 9 months- crawls, abdomen off floor
- 10 months- pulls to stand, cruises
- 12 months- sits from standing, may walk independently
Fine motor (PROXIMODISTAL) Infant
- 1 month- fists clenched, involuntary hand movement
- 3 months- hold hand in front of face, hands open
- 4 months- bats at object
- 5 months- grasps rattle
- 6 months- releases object in hand to take another
- 7 months- transfers object from hand to another
- 8 months- gross pincer grasp
- 9 months- bangs objects together
- 10 months- fine pincer grasp, puts objects into containers and takes out
- 12 months- feeds self with cup/spoon, mark paper, pokes with index
Stranger anxiety
- Become clingy when approached by strangers
- Begins around 8 months
Toddler
Respiratory rate 24-40 (decreased)
Blood pressure increases
Parallel play- play alongside another child
Developmental concerns
o Negativism- saying no
o Temper tantrums
o Sibling rivalry
o Toilet teaching
Cephalocaudal toddler
-Initial walking with “toddler gait
- Later includes running, climbing, jumping, pulling toy, throwing ball, tricycle
Proximodistal toddler
-Holding and pinching to managing utensils, holding crayon, work a puzzle, use touch screen
preschooler
·Motor skills development
o 3 years- climb well, runs easily, up and down stairs, bend over without falling
o 4 years- throws ball, kicks ball, catches bounced ball, hops on one foot, stands on one foot for 5 seconds, alternates feet using stairs, moves forward/backwards with agility
o 5 years- stands on one foot for 10 seconds, swings/climbs, skips(maybe), somersaults, learn to skate/ swim
·Fine motor skills
o 3 years- undresses self, builds tower (9-10 cubes), holds pencil, screws/unscrews lids, turn book pages
o 4 years- uses scissors, capital letters, draws circles/squares, learning diamond, draws a person figure with 2-4 parts, laces shoes
o 5 years- draws 6 person parts, dresses/undresses without help, learning to tie laces, fork, spoon, cares for toileting needs
preeschooler Conti
3 years- Vocabulary-200 words
5 years- vocab 2100 words
Developmental issues
o Lying
o Sex education
o Masturbation
School age child
· 6-12 years old
Gross motor skill
o Encourage physical activity
o Coordination, balance rhythm improves
o Ride bike, jump rope, dance, sports, skating, swimming
Fine motor skill
o Hand usage improves
o Eye-hand coordination and balance improve
o Write, print words, sew, build models
o Take pride in activities
o Vocabulary expands to 8000 to 14000
o Self-esteem development
o Body image
o School age fears
Adolescence
Puberty
o Girls 9-10
o Boys 10-11
Developmental concerns
-Changes in body image
- Peer groups
- Violence
- Suicide
- Homicide
- Substance use
Developmental concerns
- Changes in body image
- Peer groups
- Violence
- Suicide
- Homicide
- Substance use