Check for Assessment
-Health hx
-physical exam (least - most invasive)
-Inspection and observation
-color- icteric(yellow/ jaundice)
-Hydration- absence of tears (dehydration
-Abdomen size and shape- protuberant- ascites, fluid, gas, tumor; depressed- high and. obstruction or dehydration (inspection, auscultation, percussion, papatation)
-Mental status- lethargy
Auscultation
-Auscultate all four quadrants
-Nurse can determine absence of bowel sounds after 5 minutes period (can be difficult with infants/children)
Hyperactive bowel sounds
Can be noted in children with diarrhea or gastroenteritis
Hypoactive or absent bowel sounds
Can signify an obstructive process
-Immediately report hypoactive or absent findings to physician
Percussion
-Can reveal normal finding of dullness or flatness along the right costal margin and 1 to 3 cm below costal margin of liver
-area above symphysis pubis may be dull in young children with full bladders (normal finding)
-Percussion of remainder abdomen should reveal tympany
What to know about pediatric patients?
increased risk of hemorrhage
Premature infants have greater risk of bleeds because of more capillaries
Head size
Size in infant/young children is larger than body
Head continues to grow until 5 years of age
Nervous system
complete but immature at birth
Health History
Prematurity, difficult birth, infection during pregnancy, genetic disorders, seizure disorders, headaches, nausea, vomiting, changes in gait, visual disturbances, recent trauma, lethargy, poor feeding, increased irritability, fever,
Inspection and Observation
Level of consciousness
vital signs
head, face, neck
cranial nerve function
motor function
reflexes
sensory function
Increased ICP
Level of consciousness
Alertness and ability to respond to stimuli and show verbal or motor response
-5 states
-Full consciousness
-confusion: disoriented, responds inappropriately to questions
-Obtunded: limited responses and falls asleep if not stimulated
-Coma: not arousable
Head, Face , Neck
size and shape of head, asymmetry, head circumference
Cranial nerve function
Dolls eyes maneuver (turn head right, eyes should look left
Nystagmus: static
Sunset eyes
Sensory Function
Distinguish between light touch, pain, vibration, heat and cold
Scoring
-Less than or equal to 12 suggests severe head injury
-Score less than 8 suggests need for intubation and ventilation
-Score less than or equal to 6 suggests need for intracranial pressure monitoring
(The higher the score, the better/ the lower the score means lower level of consciousness)
Pediatric Glasgow Coma Scale
Eye test
Cranial nerves
-olfactory
-optic
-trigeminal
-facial
-acoustic
-glossopharyngeal
-accessory
-hypoglossal
Changes in motor function
Abnormal posturing due to brain injury
Decorticate- extremities flexed
Decerebrate- extremities extended and pronated (on stomach)
Palpation and auscultation for neurologic disorder
Palpitation of newborn or infant skulls and fontanels (feeling inflammation or depression)
Bruits (whooshing sound)- vibrations resulting from turbulence in intracranial vessels (abnormal)
Increased ICP
sign of neurologic disorder
Possible causes
-head trauma
-birth trauma
-hydrocephalus
-infection
-brain tumors
Early signs of ICP
headache
projectile vomiting
visual changes
dizziness
decreasing HR and respirations
changes in pupil reactions
sunset eyes
changes in LOC
seizures
bulging fontanel and increasing head circumference
Late signs of ICP
Decreased LOC
Depressed motor, sensory
responses
bradycardia
irregular respirations
cheyne- stokes respirations
decerebrate/decorticate postures
fixed and dilated pupils
Types of neural structural defects
Neural tube defects
Microcephaly
Arnold-Chiari malformation
Hydrocephalus
Intracranial Arteriovenous malformation: AVM
Craniosynostosis
Positional Plagiocephaly
Neural tube defects
Occurs 1st few weeks of embryonic life
ex. spina bifida, myelomeningocele, meningocele, anencephaly
Drugs, malnutrition, chemicals, and genetics
Microcephaly
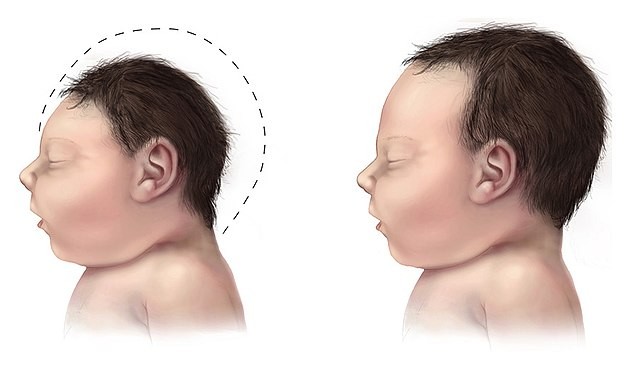
HC3 standard deviations below the mean for age and the sex of the child
Can be congenital (genetic) or acquired (malnutrition, perinatal infection, anoxia)
Arnold-Chiari malformation
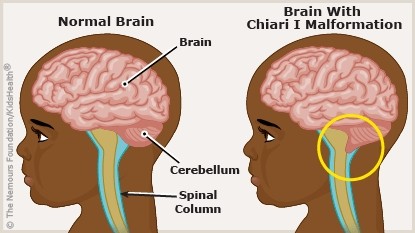
Downward displacement of cerebral structures
Cerebellum, medulla oblongata, and the 4th ventricle are displaced into the cervical canal causing obstruction to CSF flow and resulting in Hydrocephalus
Hydrocephalus
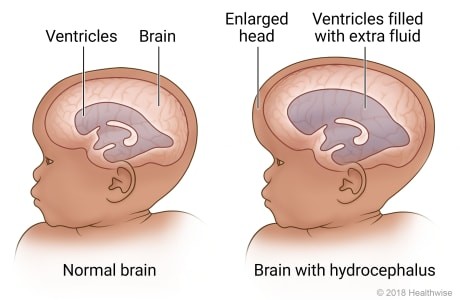
imbalance in the production and absorption of the CSF; obstruction to the flow of CSF
-increased head size
-loss of developmental milestones
-changes in personality in older children
MAY REQUIRE SURGICAL INTERVENTION TO RELIEVE PRESSURE WITH A VENTRICULAR SHUNT
Intracranial Arteriovenous malformation: AVM
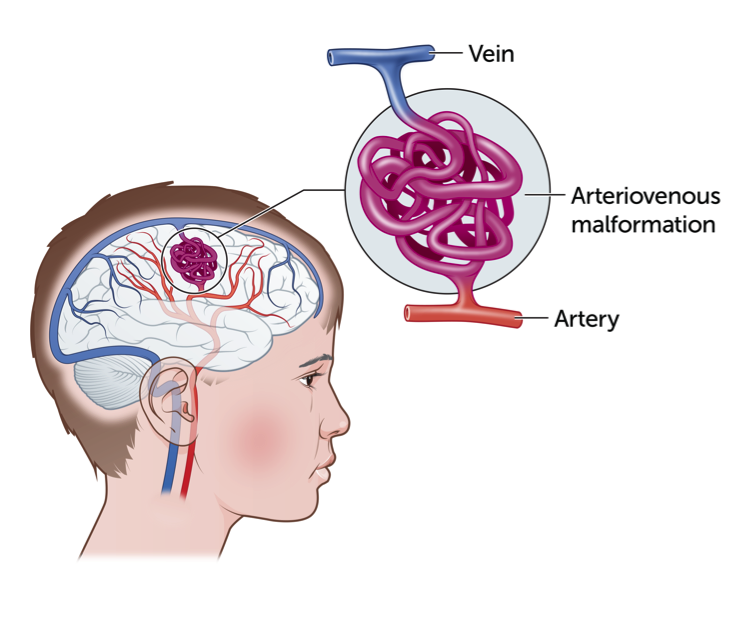
Irregular. connected and poorly formed blood vessels; can cause bleeding, seizures
Craniosynostosis
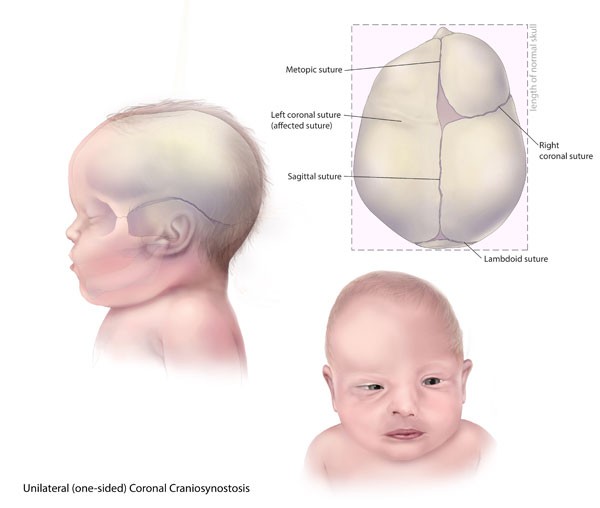
Premature closure of the sutures
Positional Plagiocephaly
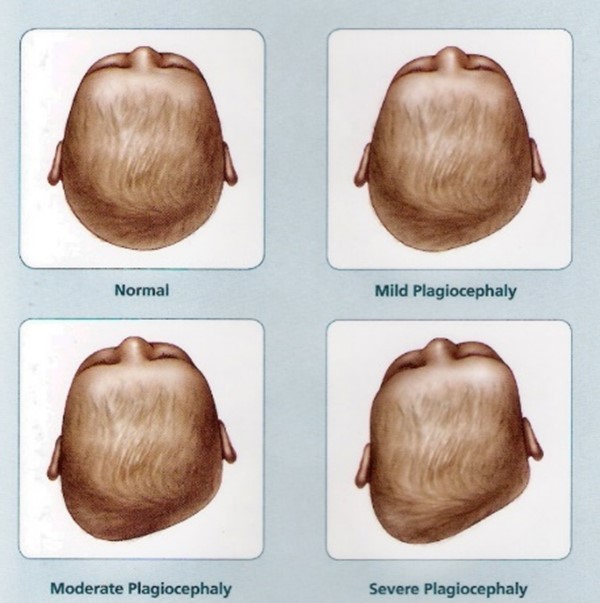
Asymmetry of head without fused sutures
Shunt
hollow tube surgically placed in brain to drain cerebrospinal fluid and redirect it to another location in the body where it can be reabsorbed
Signs and symptoms of shunt infection
-elevated vital signs
-poor feeding
-vomiting
-decreased responsiveness
-seizure activity
-signs of local inflammation along the shunt tract
Types of Seizure
Infantile spasms: spasm seen in infancy 3-12 m
Absence: uncommon before 5 years old, staring, twitching
Tonic: stiffening of muscles, arms legs, back
Clonic: muscle will spasm, jerk and then relax
Tonic-clonic: combination of above
Myoclonic: sudden brief muscle jerks that involve entire body or one part (may lose consciousness )
Atonic: drop seizures, sudden loss of muscle tone, may lose consciousness
Focal seizure without impairment of consciousness: tonic clonic movements, sensory autonomic, psychic symptoms
Focal seizure with impaired consciousness: automatisms and complex purposeful movements
status epileptics: neurologic emergency, lasting more than 5 min/ 2 or more within 5 min
Febrile seizure
Febrile Seizures
Most common type, seen in children less than 5
Associated with 102.2F temperature or higher
Benign
Bacterial Meningitis
Infection of meninges
Serious illness that can lead to brain damage, nerve damage, deafness, stroke and even death
-Causes inflammation, swelling, purulent exudates, tissue damage to brain. Can occur secondary to sinus or ear infection
-MEDICAL EMERGENCY
-May rest in muscles in back, neck and legs spasm and contract (neck pain, bulging fontanel)
-Positive(bad) kerning and Brudzinski signs: indicate irritation of meninges
Inspect child for rash
Kernig's sign
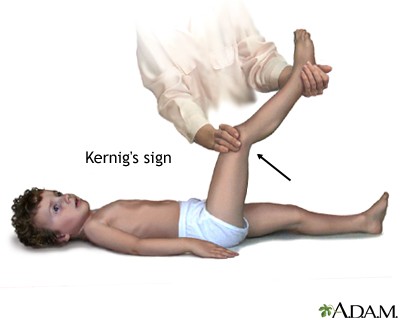
supine patient, with hips and knees flexed, extend the leg passively. The test is positive if leg extension causes pain
Brudzinski's sign
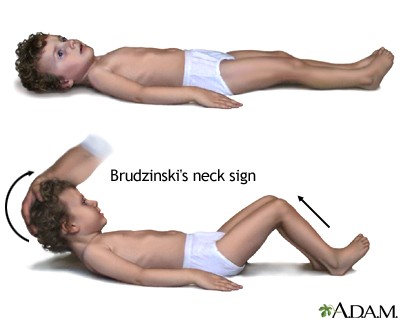
is positive when passive forward flexion of neck causes the patient to involuntarily raise his knees or hips in flexion
Spinal tab/ LP
-Laying on side, knees to chest
-leaning forward, legs flexed
Medications to treat
Antibiotics
Anticonvulsants
Bensodiazepines
Analgesics
Osmotic diuretics
Corticosteriods
Positional alterations
Internal tibial torsion: Lower extremities have bowed appearance
Genuine Valgum: knock knees; knees touch and ankles are significantly separated; resolves by 7-8 y/o
in-toeing: normal finding; feet remain flexible and passively move to midline
Pes planus: (flat feet) noted in infants when they begin to walk; arch develops as they grow
Fractures
rule out possibility of abuse
Casts
Immobilize bone that's injured or deseased
serves to hold the bone in reduction (preventing deformity as it heals)
keeps bones aligned
reduce pain and allow child increased mobility
Type of casts
Short arm cast (forearm)
Long arm cast (full arm)
Shoulder spica cast (one shoulder and down waist)
Long leg cast (full cast)
Short leg cast (calf)
Long leg hip spica cast (chest to both full legs)
One and a half hip spica cast (hip to one full leg and half of other)
Abduction boots (full legs)
Traction
method of immobilization
External fixation
-Used for complicated fractures, especially open fractures with soft tissue damage
-A series of pins or wires are inserted into bone and then attached to an external frame
-INFECTION
Spina Bifida Occulta (can't be seen)
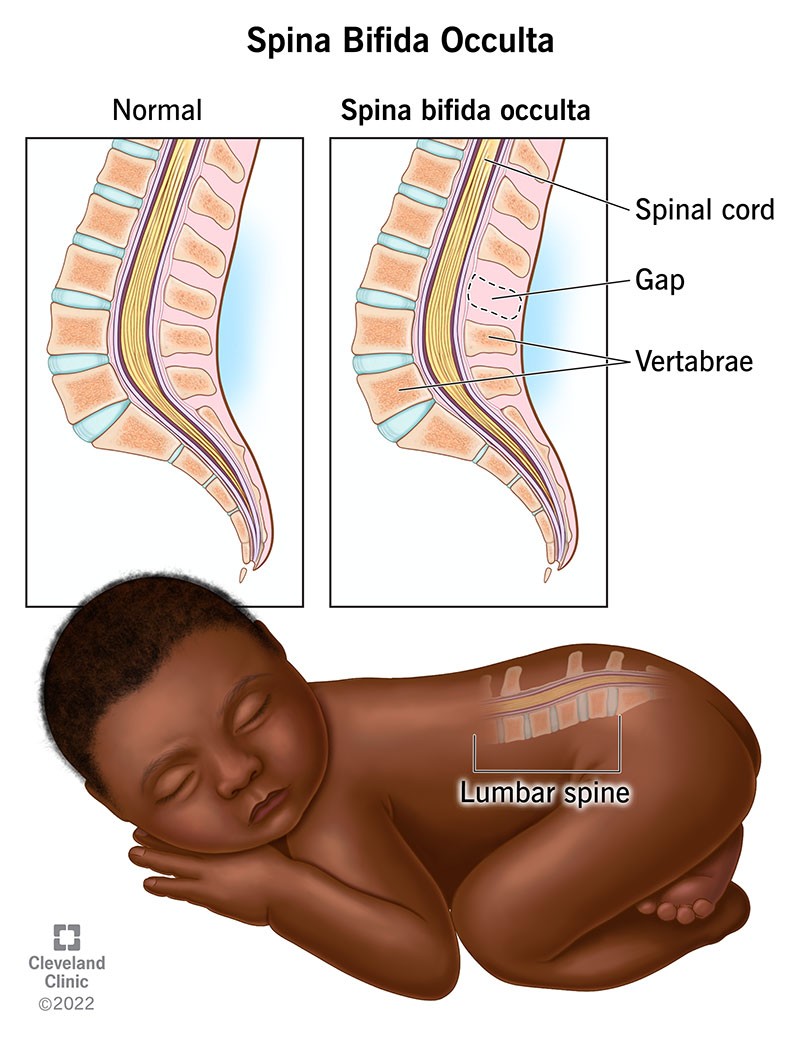
-defect of vertebral bodies without protrusion of spinal cord or meninges
-not visible externally and in most cases no adverse effects
-need no immediate medical intervention
-complications are rare, abnormalities of spinal cord
-dimpling or tats of hair in lumbosacral area- MRI
Neural tube defects
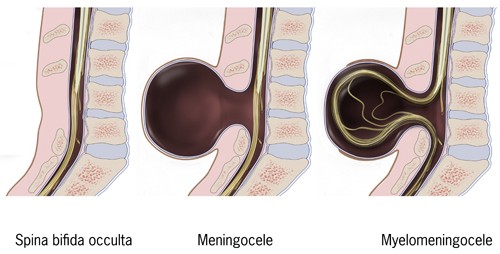
spina bifida cystica- meningocele and myelomeningocele
Meningocele- meninges herniate through a defect in the vertebrae
visible external sac protruding from spinal area: care to prevent rupture of sac
Treatment included surgical correction of lesion
Myelomeningocele- most severe
spinal cord often ends at the point of defect, resulting in absent motor and sensory function
long term complications pf paralysis, orthopedic deformities, and bladder and bowel incontinence
accompanying hydrocephalus
Nursing management of myelomeningocele
Preventing infection
Promoting urinary elimination
Promoting bowel elimination
Promoting adequate nutrition
Preventing latex allergic reaction
Maintain skin integrityEducating and support child and family
Chest Wall Deformities
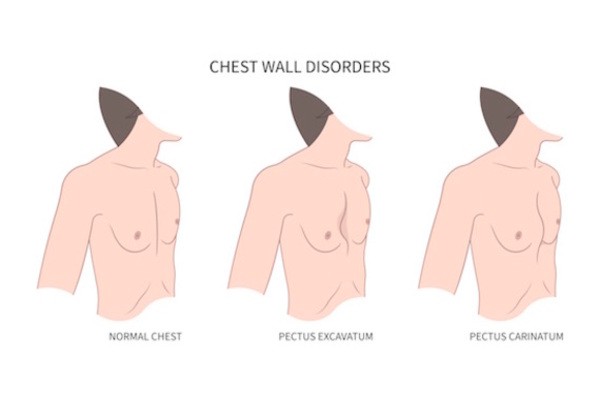
Pectus excavatum: funnel shaped chest, depression that sinks inward is apparent at diploid process, progresses with growth. When pectus more pronounced, cardiac and pulmonary compression occurs
Pectus carinatum: protuberance of the chest wall, accounts for only 5 to 15% of anterior chest wall deformities
Limb deficiencies
absence of limb
Amniotic bands
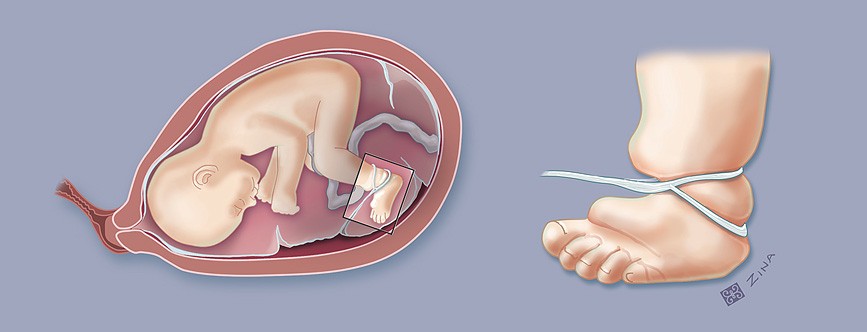
wrapping of limp and causes no blood flow
Polydactyly
Presence of extra digits on hand or foot
-involves digits at border of hand or foot, can occur by any central digit
-note if there is bone present
-possible surgical
Syndactyly
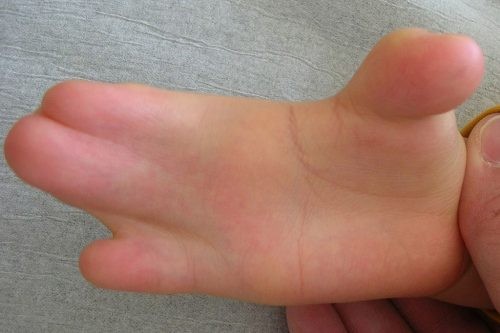
Webbing of fingers and toes
Metatarsus Adductus
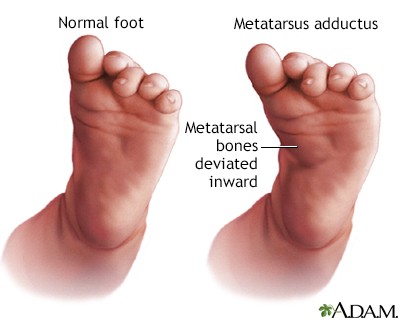
Medal deviation of forefoot
-occurs most commonly in utero
-observation
-stretching
-serial casting
surgery-rarely
congenital club foot
Talipes varus (inversion of heel)
talipes equinus (plantar flexion of foot; heal raised and would not strike ground in standing position)
Foot resembles the head of a golf club
Cerebral Palsy
Caused by damage or abnormal development in parts of brain that control movement
-Some children with CP will have cognitive issues
-Symptoms include exaggerated reflexes, floppy or rigid limbs, and involuntary motions
Complication: mental impairments, seizures, growth problems, impaired vision/hearing, abnormal sensation and hydrocephalus
Ataxia: lack of coordination of muscle movements during voluntary movements such as walking or picking up objects
Osteogenesis Imperfecta
sclera may have blue, purple or gray tint
results in low bone mass, increased fragility of bones, connective -tissue problems such as hyper mobility, instability of joints
-fractures
goal is to decrease fractures and maintain mobility
Hip Dysplasia
asymmetric gluteal, thigh, labial folds
Torticollis
-painless muscular condition
-may result in utero positioning or difficult birth
-preferential turning head to one side while lying supine (flatten head one side)
-results from tightness of sternocleidomastiod muscle
-plagiocephaply
Tibia Vara (Blount disease)
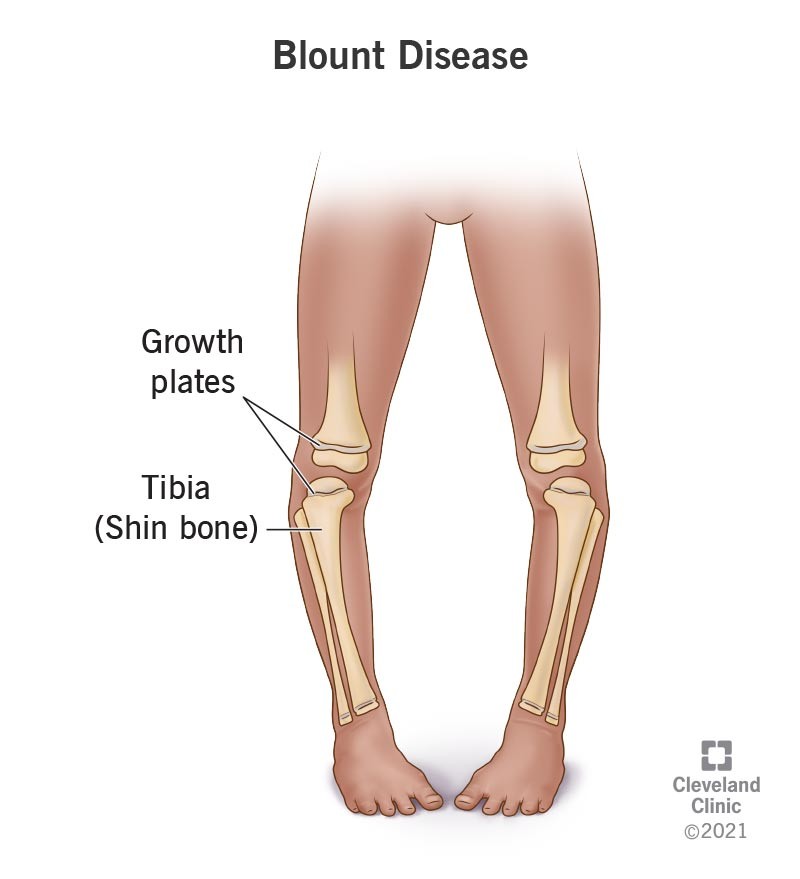
normal physiologic bowing or gene vacuum becomes more pronounced in the child with tibia vara
-occurs in early walkers, associated with obesity
-If left untreated, growth plate of upper tibia ceases bone production
-assymetric growth at knee
Muscular dystrophy
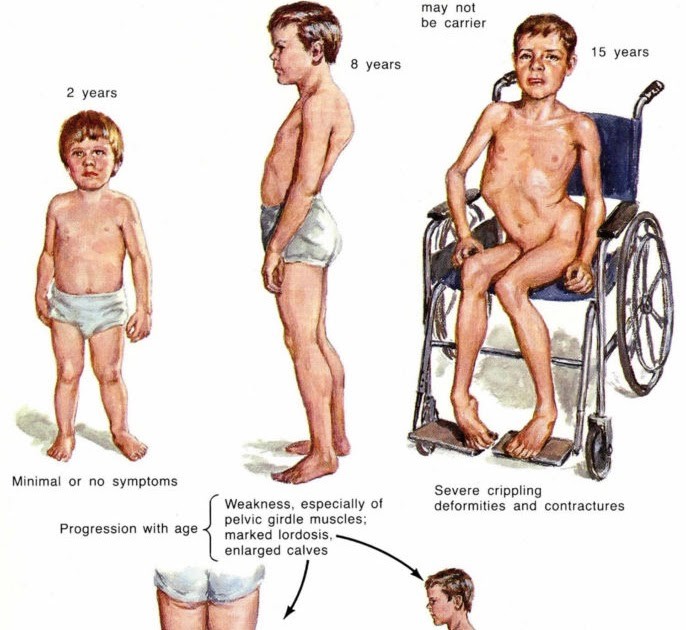
Duchaunee
inherited genetic disorder
progress muscle weakness and wasting
no cure, steroids may slow
Hall mark sign: Gowers sign- difficult to stand up from floor
Rickets
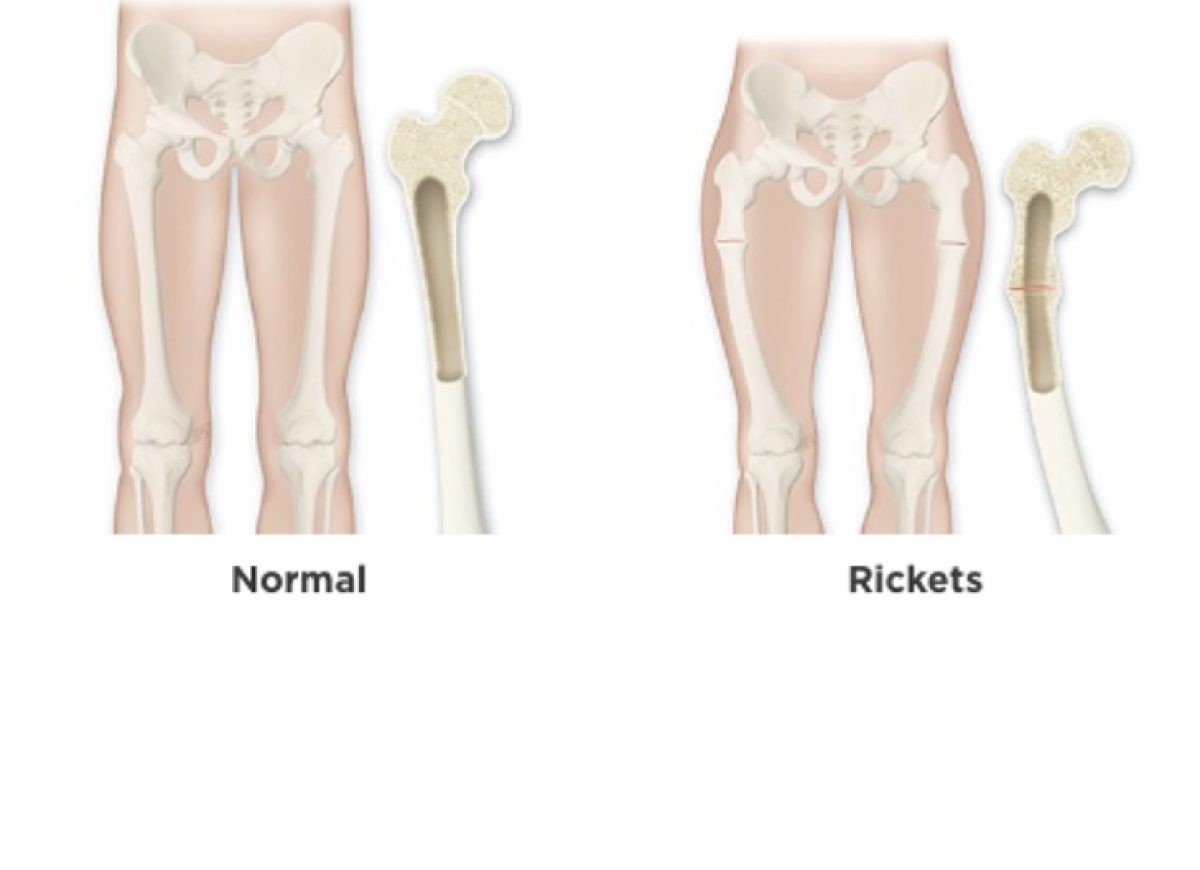
-Softening or weakening of the bones
-Childhood rickets may occur as a result of nutritional deficiencies such as inadequate consumption of calcium or vitamin D or limited exposure to sunlight (required for adequate production of vitamin D).
Rickets caused by vitamin D deficiency is a preventable condition
Scoliosis
Lateral curvature of the spine greater than 10 degrees
-May be congenital, associated with other disorders, or acquired
-Assess: auscultate heart and lung sounds to make sure there is no compromise
-Management
Braces (multiple types based on severity)Surgical repair for severe cases - for curve greater than 45 degreesEncourage compliance if bracedPost-op careBody image
Slipped capital femoral epiphysis
Femoral head dislocates from the neck and shaft of femur at the level of the epiphyseal plate
-left hip is more often affected-Chronic SCFE may lead to shortening of the affected leg and thigh atrophy
Transient synovitis of hip
-Also termed toxic synovitis
-The exact cause is unclear, but it is thought to be associated with recent or active infection, trauma, or allergic hypersensitivity
-It is a self-limiting disease and most cases resolve within a week, but it may last as long as 3 to 6 weeks.
Signs and symptoms of spinal cord injury
-Emergency
-Immobilization
-Prevention!
-Inability to move or feel extremities
-Numbness
-Tingling
-Weakness
-Loss of voluntary movement below the level of the lesion
-Inability to breathe, if injury is at a high cervical vertebra
Sprains
Twisting or turning motion of affected body part
tendons and ligaments stretch excessively and may tear slightly
-Want inflammation (body doing what it needs)
MEAT:
-Movement
-Exercise
-Analgesics
-Treatment
Nursemaid's elbow
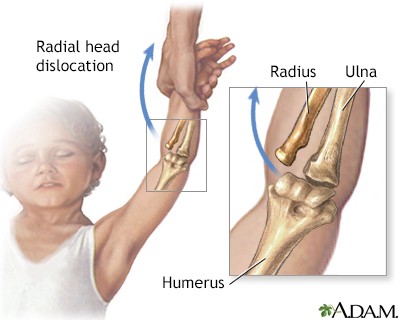
occurs when radius slips out of place from where it normally attaches to the elbow joint
-immediate pain
-refusal or inability to move arm
A 6-month-old infant is admitted with a diagnosis of bacterial meningitis. Which room is appropriate for this infant?
a. room with a 12-month-old infant who has a urinary tract infection
b. room with an 8-month-old infant with failure to thrive
c. private room near the nurses’ station
d. multibed room with other infants who have bacterial meningitis
c. private room near the nurses' station
The nurse is caring for a 6-year-old child who has a history of febrile seizures and is admitted with a temperature of 102.2°F (39°C). What is the nurse's highest priority?
a. Institute safety precautions.
b. Offer age-appropriate activities.
c. Provide family teaching related to the child's history.
d. Encourage the child to do his or her own self-care.
a. Institute safety precautions
. A nurse is preparing a presentation for a group of expectant parents about neural tube defects and prevention. Which would the nurse emphasize?
a. smoking cessation
b. aerobic exercise
c. increased calcium intake
d. folic acid supplementation
d. folic acid supplementation
What finding is consistent with increased intracranial pressure (ICP) in an infant?
a. Emotional lability
b. Increased appetite
c. Narcolepsy
d. Bulging fontanels (fontanelles)
d. Bulging fontanels (fontanelles)
During the physical assessment of a 2½-month-old infant, the nurse suspects the child may have hydrocephalus. Which sign or symptom was observed?
a. Dramatic increase in head circumference
b. Pupil of one eye dilated and reactive
c. Vertical nystagmus
d. Posterior fontanel (fontanelle) is closed
a. Dramatic increase in head circumference
The nurse is observing an infant who may have acute bacterial meningitis. Which finding might the nurse look for?
a. Flat fontanel (fontanelle)
b. Irritability, fever, and vomiting
c. Jaundice, drowsiness, and refusal to eat
d. Negative Kernig sign
b. Irritability, fever, and vomiting
A pregnant client asks if there is any danger to the development of her fetus in the first few weeks of her pregnancy. How should the nurse respond?
a. “As long as you were taking good care of your health before becoming pregnant, your fetus should be fine during the first few weeks of pregnancy.”
b. “Bones begin to harden in the first 5 to 6 weeks of pregnancy, so vitamin D consumption is particularly important.”
c. “During the first 3 to 4 weeks of pregnancy, brain and spinal cord development occur and are affected by nutrition, drugs, infection, or trauma.”
d. “The respiratory system matures during this time, so good prenatal care during the first weeks of pregnancy is very important.”
c. “During the first 3 to 4 weeks of pregnancy, brain and spinal cord development occur and are affected by nutrition, drugs, infection, or trauma.”
A 4-year-old child is brought to the emergency department after being in a motor vehicle accident. The child experienced head trauma in the accident. When assessing the child, which will be the first change noted in the presence of increasing intercranial pressure?
a. change in level of consciousness
b. reduction in heart rate
c. increase in heart rate
d. decline in respiratory rate
a. change in level of consciousness
What information is most correct regarding the nervous system of the child?
a. The child's nervous system is fully developed at birth.
b. As the child grows, the gross and fine motor skills increase.
c. The child has underdeveloped fine motor skills and well-developed gross motor skills.
d. The child has underdeveloped gross motor skills and well-developed fine motor skills.
b. As the child grows, the gross and fine motor skills increase.
A nurse is assessing a 3-year-old child for possible bacterial meningitis. Which sign would indicate irritation of the meninges?
a. Positive Kernig sign
b. Negative Brudzinski sign
c. Positive Chadwick sign
d. Negative Kernig sign
a. Positive Kernig sign
Preterm infants have more fragile capillaries in the periventricular area than term infants. This put these infants at risk for which problem?
a. moderate closed-head injury
b. early closure of the fontanels (fontanelles)
c. congenital hydrocephalus
d. intracranial hemorrhaging
d. intracranial hemorrhaging
A nurse is talking with the parents of a child who has had a febrile seizure. The nurse would integrate an understanding of what information into the discussion?
a. The child's risk for cognitive problems is greatly increased.
b. Structural damage occurs with febrile seizure.
c. The child's risk for epilepsy is now increased.
d. Febrile seizures are benign in nature.
d. Febrile seizures are benign in nature.
A nurse is applying a cast to a 12-year-old boy with a simple fracture of the radius in the arm. What is most important for the nurse to do when she has finished applying the cast?
a. Assess the fingers for warmth, pain, and function
b. Apply a tube of stockinette over the cast
c. Cut a window in the cast over the wrist
d. X-ray the cast to make sure the bones are aligned properly
a. Assess the fingers for warmth, pain, and function
A nurse has provided care to several children during their well-child visits. The nurse has assessed each child’s neurologic status. Which assessment finding indicates a problem requiring intervention?
a. a 2-month-old infant who reaches for a rattle several times before connecting with it
b. a 10-month-old infant who is able to ambulate with assistance
c. a 2-year-old toddler who can walk up the steps one at a time
d. a 4-year-old preschool-age child who consistently walks on tiptoes
d. a 4-year-old preschool-age child who consistently walks on tiptoes
The nurse is educating a group of caregivers about fractures seen in children. One of the caregivers states, “I have heard that if a bone breaks it can cause permanent damage and stop the growth of the bone.” This statement is accurate if the break occurs in the:
a. humerus.
b. joint.
c. xiphoid process.
d. epiphyseal plate.
d. epiphyseal plate.
The nurse is caring for a 14-year-old client in traction prior to surgery. The client has been in the hospital for 2 weeks and will require an additional 10 days in the hospital following surgery. The client states, "I feel isolated and I am refusing any more treatment." Which response by the nurse is most appropriate?
a. “I know it is boring here, but the best place for you to remain immobile is the hospital.”
b. "I will see if you can have friends come spend a few nights with you.”
c. “Let's come up with things for you to do and see if your friends can come visit.”
d. “If you refuse further treatment, your condition will only get worse.”
c. “Let's come up with things for you to do and see if your friends can come visit.”
The nurse receives a report on a child admitted with severe muscular dystrophy. The nurse suspects the child has been diagnosed with the most severe form of the disease, known as:
a. Duchenne.
b. facioscapulohumeral.
c. limb-girdle.
d. myotonia.
a. Duchenne.
A nurse is providing instructions for home cast care. Which response by the parent indicates a need for further teaching?
a. “We must avoid causing depressions in the cast.”
b. “Pale, cool, or blue skin coloration is to be expected.”
c. “The casted arm must be kept still.”
d. “We need be aware of odor or drainage from the cast.”
b. “Pale, cool, or blue skin coloration is to be expected.”
An infant has been born and diagnosed with a meningocele. Which action will the nurse incorporate into each contact with this infant?
a. inspection of the cystic sac on the child’s back for leakage
b. auscultation for bowel sounds
c. listening for a shrill cry
d. careful supine positioning
a. inspection of the cystic sac on the child’s back for leakage
The pediatric nurse practitioner (PNP) records "positive Gowers' sign" after finishing the assessment of a young boy. How will the student nurse reading the PNP's note interpret this?
a. The boy has a large tan skin lesion on his torso.
b. Severe lordosis is evident in the lumbar spine.
c. The head is held tilted with limited side-to-side motion.
d. The boy rises from the floor by walking his hands up his legs.
d. The boy rises from the floor by walking his hands up his legs.
The parents of a infant born with an abnormality on the back are told by the neonatologist that their child has a myelomeningocele. They ask the nurse what exactly that means. Which would be the nurse's best reply?
a. "It is a herniation through the skin of the back of your child with both the spinal cord and nerve roots involved."
b. "The contents of the sac you see only has fluid in it and should cause the child no problem."
c. "Your child's defect involves only the nerves to the bladder and bowel and can be easily repaired."
d. "The sac is a very small cyst and should resolve within the first year of life."
a. "It is a herniation through the skin of the back of your child with both the spinal cord and nerve roots involved."
What information would the nurse include in the preoperative plan of care for an infant with myelomeningocele?
a. positioning supine with a pillow under the buttocks
b. covering the sac with saline-soaked nonadhesive gauze
c. wrapping the infant snugly in a blanket
d. applying a diaper to prevent fecal soiling of the sac
b. covering the sac with saline-soaked nonadhesive gauze
The nurse is assessing the neuromusculoskeletal system of a newborn. What is an abnormal assessment finding?
a. sluggish deep tendon reflexes
b. full range of motion in extremities
c. absence of hypotonia
d. lack of purposeful muscular control
a. sluggish deep tendon reflexes
An 8-year-old girl was diagnosed with a closed fracture of the radius at approximately 2 p.m. The fracture was reduced in the emergency department and her arm placed in a cast. At 11 p.m. her mother brings her back to the emergency department due to unrelenting pain that has not been relieved by the prescribed opioids. Which action would be the priority?
a. Notifying the doctor immediately
b. Applying ice
c. Elevating the arm
d. Giving additional pain medication as ordered
a. Notifying the doctor immediately
When developing the plan of care for a child with cerebral palsy, which treatment would the nurse expect as least likely?
a. skeletal traction
b. physical therapy
c. orthotics
d. occupational therapy
a. skeletal traction
Risk Factors for Respiratory Disorders
•Prematurity
•Chronic illness (diabetes, sickle cell anemia, cystic fibrosis, congenital heart disease, chronic lung disease)
•Developmental disorders (cerebral palsy)
•Passive exposure to cigarette smoke
•Immune deficiency
•Crowded living conditions or lower socioeconomic status
•Daycare attendance
Nursing Assessment for Child with Respiratory Distress
•Health history – PMH, FH, Hx present illness, immunization hx, exposure to smoke
•Atopy –genetic tendency to asthma, allergic rhinitis, atopic dermatitis
•Physical exam
•Inspection and observation
•Palpation
•Percussion
•Auscultation
Inspection and Observation
•Anxiety and restlessness
•Color: pallor, cyanosis
•Hydration status
•Clubbing
•Breath sounds
•Rate and depth of respirations: tachypnea
•Respiratory effort
•Nose and oral cavity
•Cough and other airway noises: stridor
Adventitious Breath Sounds
•Wheezing
•High-pitched sound usually heard on inspiration; sometimes on expiration
•May occur with obstruction in lower trachea or bronchioles
•May occur in asthma or viral infections
•Rales
•Crackling sounds heard when alveoli become fluid filled
•May occur with pneumonia
Common Medical Treatments for respiratory
•Oxygen
•High humidity
•Suctioning
•Chest physiotherapy and postural drainage
•Saline gargles or lavage
•Mucolytic agents
•Chest tubes
•Bronchoscopy
Acute respiratory Infectious Disorders
•Common cold – viral URI or nasopharyngitis; e.g., Respiratory syncytial virus (RSV);
•Sinusitis – bacterial; acute or chronic
•Influenza – viral infection; ‘the flu’; bacterial infections may follow
•Pharyngitis, tonsillitis– often viral
•Laryngitis – inflammation of larynx
•Croup syndromes – parainfluenza main cause; inspiratory stridor; worse at night
•Pneumonia and bronchitis
•Infectious mononucleosis –caused by Epstein-Barr virus; ‘kissing disease’, often in adolescence; spleen rupture, Guillain-Barre syndrome; meningitis
Signs and Symptoms of Bronchiolitis (RSV)
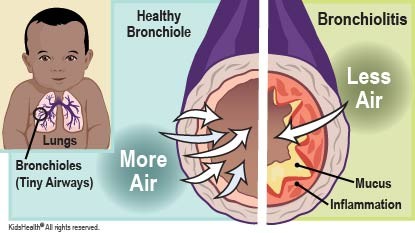
•Onset of illness with a clear runny nose(sometimes profuse)
•Pharyngitis
•Low-grade fever
•Development of cough 1 to 3 days into the illness, followed by a wheeze shortly thereafter
Poor feeding
Epiglottitis
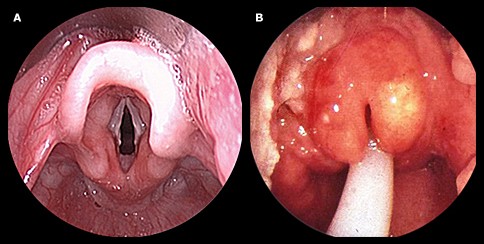
•The epiglottis — a small cartilage "lid" that covers the trachea — wells. Epiglottitis can be deadly
•Severe sore throat
•Difficulty swallowing
•Stridor
•DO NOT
•Attempt to visualize the throat - laryngospasm
•Leave the child unattended
•Place the child in a supine position
•DO
•Provide 100% oxygen in the least invasive manner
•Ensure tracheostomy tray and emergency equipment readily available
Chronic Respiratory Disorders
•Allergic rhinitis – associated with asthma and atopic dermatitis
•Asthma –chronic inflammatory airway disorder
•Chronic lung disease infants who had RSD and require O2 past 28 days
•Cystic fibrosis – disruption of chloride - gets trapped in cells = mucous thick, sticky. Lungs- increased infection & inflammation; pancreas – prevents nutrients from being absorbed
•Apnea – absence of breathing for more than 20 seconds; may be accompanied by bradycardia
•Central – unrelated to another cause
•Occur with other illnesses
•Apnea of prematurity – precursor to SIDS; caffeine - theophylline
Cystic Fibrosis
•Autosomal recessive disorder
•Cystic fibrosis transmembrane conductance regulator (CFTR) mutation results in problems in exocrine glands
•Excess thick, tenacious mucus lining airways causing decreased resistance to infection and air trapping
•Decreased pancreatic enzymes and hypersecretion of gastric acids
Cystic Fibrosis—Laboratory and Diagnostic Tests
•Sweat chloride test: considered suspicious if the level of chloride in collected sweat is above 50 mEq/L and diagnostic if the level is above 60 mEq/L
•Pulse oximetry: oxygen saturation might be decreased, particularly during a pulmonary exacerbation
•Chest radiograph: might reveal hyperinflation, bronchial wall thickening, atelectasis, or infiltration
•Pulmonary function tests: might reveal a decrease in forced vital capacity and forced expiratory volume, with increases in residual volume
Cystic Fibrosis Treatment
•Chest physiotherapy (multiple times daily)
•Inhaled dornase alfa (pulmonary enzyme)
•Inhaled antibiotics for exacerbation
•Pancreatic enzyme supplementation
•ADEK vitamin supplementation
•Well-balanced, high-calorie, high-protein diet
Risk Factors for Tuberculosis
•TB – highly contagious, droplet precautions;
•HIV infection
•Immigration or travel to endemic countries
•Exposure at home to HIV-infected or homeless persons, illicit drug users, persons recently incarcerated, migrant farm workers, or nursing home residents
Asthma
•Chronic inflammatory airway disorder- most common chronic illness of childhood
•Airway hyperresponsiveness
•Airway edema
•Mucus production
•Results in airway obstruction that might be partially or completely reversed
•Incidence & severity increasing -environment
Signs of asthma in infants
Coughing
wheezing
nasal flaring
exaggerated belly breathing
fatigue
shortness of breath
Asthma Management
•Rescue medicine: short-acting bronchodilators - albuterol
•Maintenance medicines
•Leukotriene modifiers-decrease the body's production of the leukotrienes (inflammatory chemicals) that worsen both asthma and allergic reactions (singular)
•Inhaled corticosteroids – flovent, Pulmicort
•Long-acting bronchodilators - serevent
Lab and Diagnostic Tests for Asthma
•Pulse oximetry: oxygen saturation may be decreased significantly or normal during a mild exacerbation.
•Chest radiograph: usually reveals hyperinflation.
•Blood gases: might show carbon dioxide retention and hypoxemia.
•Pulmonary function tests (PFTs): can be very useful in determining the degree of disease but are not useful during an acute attack. Children as young as 5 or 6 years might be able to comply with spirometry.
•Peak expiratory flow rate (PEFR): is decreased during an exacerbation.
•Allergy testing: skin test or RAST can determine allergic triggers for the asthmatic child.
Nursing Care Post-tonsillectomy
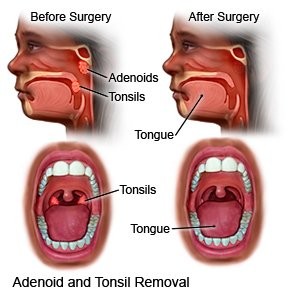
•Promoting airway clearance: place child in side-lying or prone position
•Maintaining fluid volume
•Discourage coughing
•Encourage fluids; avoid citrus, brown, or red fluids
•Relieving pain: ice collar and analgesics with or without narcotics
**Frequent swallowing may indicate bleeding**
Acute Noninfectious Respiratory Disorders
•Epistaxis – bloody nose
•Foreign body aspiration
•solid or liquid substance inhaled in reparatory tract
•Small objects smaller than diameter of their airway
•Items smaller than Toilet paper roll
•Acute respiratory distress syndrome – may follow another illness or insult
•Pneumothorax – collection of air in pleural space
•Needle aspiration or chest tube
Tracheostomy

•Artificial opening in the airway
•Plastic tracheostomy tube is in place to form a patent airway
•Relieve airway obstruction.
•Used in child who requires chronic mechanical ventilation
•Facilitates secretion removal, reduces work of breathing, and increases the child’s comfort.
Interventions to Minimize Psychosocial Impact of Chronic Respiratory Conditions
•Promoting child’s self-esteem through education and support
•Allowing school-age child to take control of management of the disease
•Promoting family coping through education and encouragement
•Providing culturally sensitive education and interventions
•Consider developmental age
Cardiovascular Changes in Childhood
Heart Rate (HR)
Faster in infancy (90–160 bpm), decreases as the child ages
Blood Pressure (BP)
Lower in infancy (~80–55 mm Hg), increases as the child ages
HR and BP reach adult levels by adolescence
Congenital Heart Disease
Structural anomalies that are present at birth
Acquired Heart Disease
▪Disorders that occur after birth (heart failure, most common reason for admission)
Cyanotic Heart Disease
right to left
allow oxygen rich blood and oxygen poor blood to mix
-cyanosis: bluish tint of skin, lips, and nail beds
ex. Tetralogy of Fallot.
Transposition of the great vessels.
Total anomalous pulmonary venous return.
Truncus arteriosus.
Tricuspid valve abnormalities.
Pulmonary atresia.
Hypoplastic left heart syndrome.
Acyanotic Heart Disease
left to right
asymptomatic(bluish tint may appear during activities when baby needs more oxygen such as crying or feeding
ex Ventricular septal defect (VSD).
Atrial septal defect (ASD).
Atrioventricular septal defect.
Patent ductus arteriosus (PDA).
Pulmonary valve stenosis.
Aortic valve stenosis.
Coarctation of the aorta.
Congentital Heart Disease risk factors
▪Premature infants have a higher rate
▪Most common chromosome defects associated with CHD are trisomy 21 (Down syndrome) and Turner syndrome
▪Complications of CHD include heart failure, hypoxemia, growth retardation, developmental delay, and pulmonary vascular disease. Children with severe anomalies frequently experience failure to thrive
Tetralogy of Fallot (TOF) - Decreased Pulmonary Blood Flow
Cyanotic
▪Decrease O2 to lungs, decrease O2 of blood returning to left atrium and lungs, increase pressure in right ventricle. Mixing of blood, poorly oxygenated blood in systemic circulation leading to cyanosis
▪Usually diagnosed in first few weeks due to presence of murmur
▪Surgical intervention is usually required during the first year of life
▪Becomes worse within first dew days of life when ductus arteriosus closes
TOF
Signs and Symptoms:
▪Color changes with feeding, activity, crying
▪Hyper-cyanotic spells can progress to anoxia
▪In older children, bending at knees, squatting (increases systemic vascular resistance and improves pulmonary blood flow)
Atrial Septal Defect
Acyanotic
▪Poor feeding, difficulty growing
Diagnostic Tests for Cardiovascular Disorders
▪Pulse oximetry
▪Electrocardiogram (ECG) and Holter monitoring
▪Echocardiogram-
▪Chest radiograph- x ray
▪Exercise stress testing
▪Laboratory tests including
▪CBC
▪BMP
▪C-reactive protein (CRP)
▪Erythrocyte sedimentation rate (ESR)
▪Arteriogram and cardiac catheterization
Heart Failure
•Nursing Management
•Promoting oxygenation
•Supporting cardiac function
•Providing adequate nutrition
•Promoting rest
Cardiomyopathy
•Risk factors:
•Congenital heart defect
•Genetic disorders
•Inflammatory or infectious processes
•Posttransplant or postoperatively after cardiac surgery
•Hypertension
•Duchenne and Becker muscular dystrophy
Kawasaki Disease
•Acute systemic vasculitis – inflammation of blood vessels -mostly occurring in 6 mo – 5 yr
•Signs and symptoms include:
•High fever for 5 days (unresponsive to antibiotics)
•Chills
•Headache
•Malaise
•Extreme irritability
•Distinctive rashes (strawberry tongue, palmar erythema)
•Desquamation(peeling) of perineum, fingers and toes
•Vomiting
•Diarrhea
•Abdominal and joint pain
•Treatment: IV immunoglobulin and aspirin
Signs of a Cardiac Disorder
•Cyanosis
•Irregular heart rate
•Edema
•Clubbing of fingertips
•Fever
•Retractions or increased work of breathing
•Prominence of precordial chest wall
•Visible, engorged, or abnormal pulsations
•Abdominal distention
Characteristics of Heart Murmurs
Location
duration
quality
variation in sound with position
intensity
Focus of Nursing Care for Child With a Cardiac Disorder
•Improving oxygenation
•Promoting adequate nutrition
•Assisting the child and family with coping
•Providing postoperative nursing care
•Preventing infection
•Providing child and family education
Hypospadias
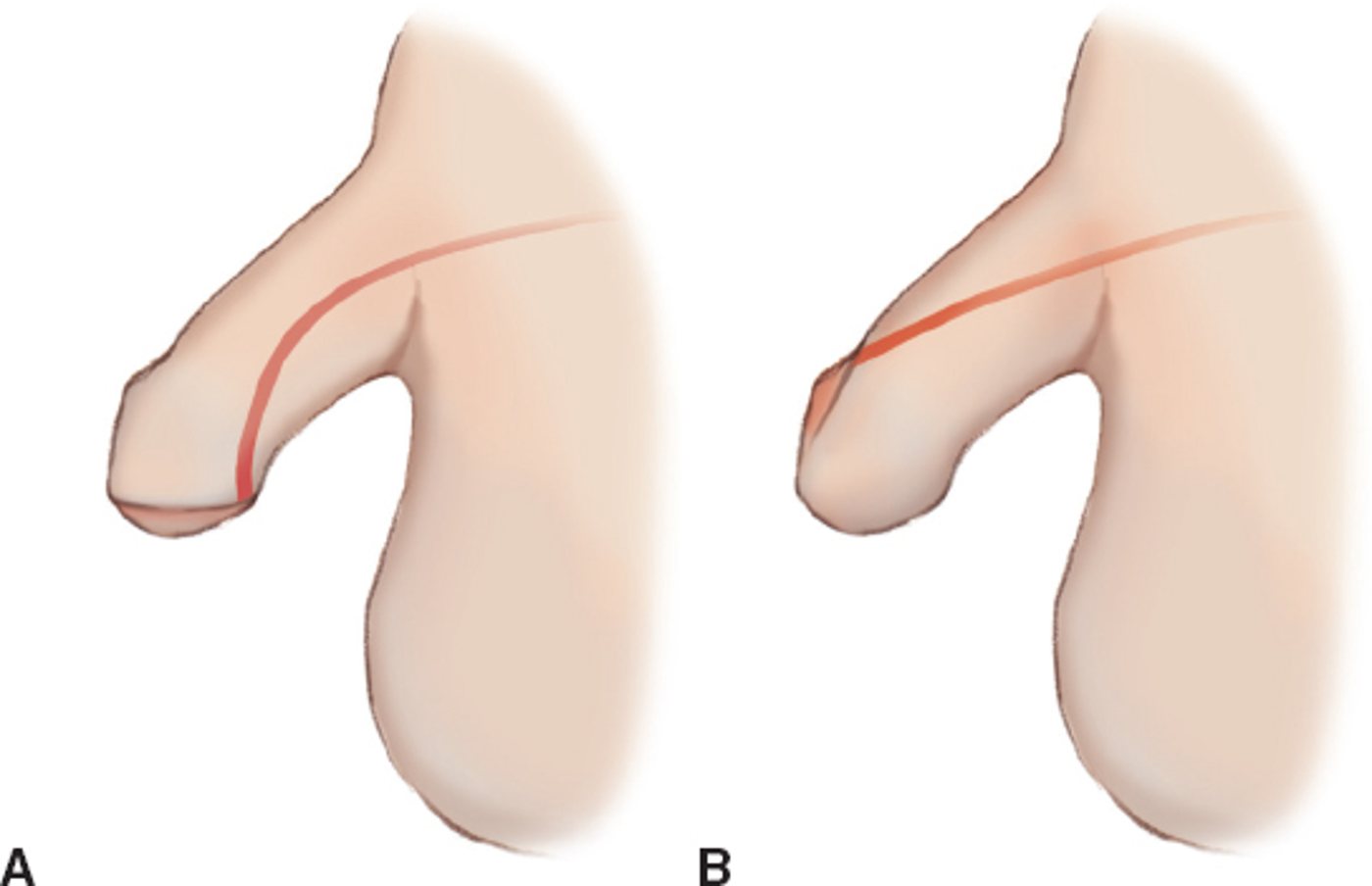
defect in which the opening is on the ventral surface of the penis rather than at the end of the penis; •usually repaired 6 mo. – 1 year
Epispadias
urethral defect in which the opening is on the dorsal surface of the penis; usually repaired 6 mo. – 1 year
Obstructive uropathy
obstruction at any level along the upper or lower urinary tract
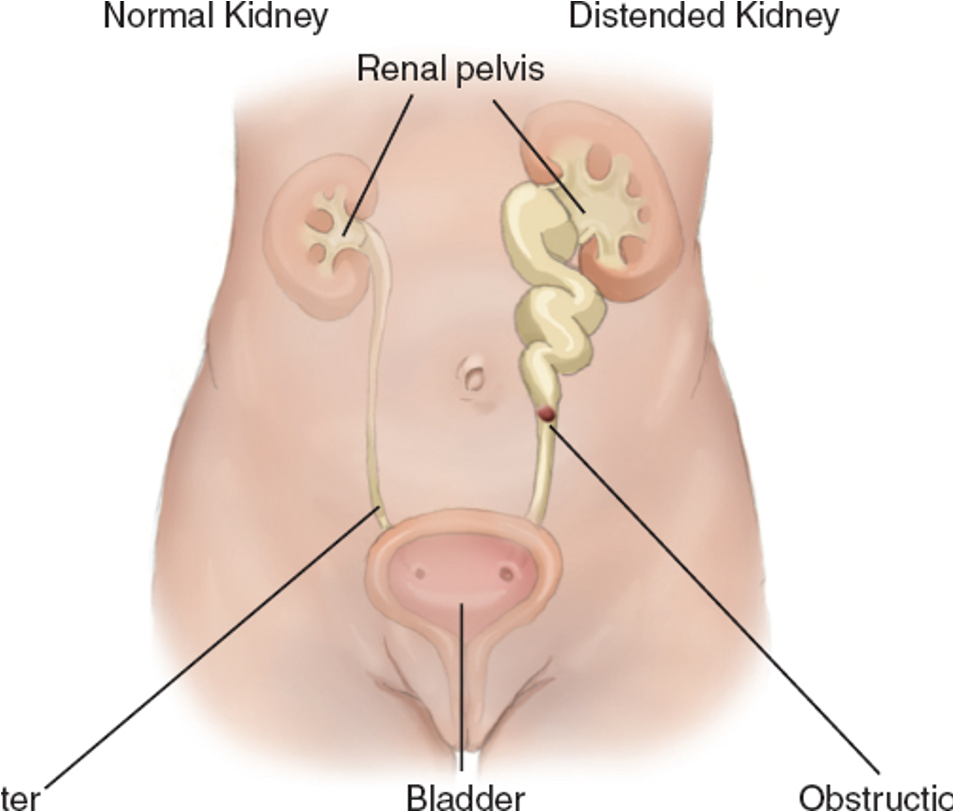
Hydronephrosis
excess fluid in a kidney due to a backup of urine. Can be caused by blockage in ureter, infection, tumor. Complications of hydronephrosis include renal insufficiency, hypertension, and eventually renal failure
Vesicoureteral reflux
urine from the bladder flows back up the ureters; If reflux occurs when the urine is infected, the kidney is exposed to bacteria and pyelonephritis may result
Urinary tract infection
occurs most often because of bacteria ascending to the bladder via the urethra; E.coli most common cause
Enuresis
continued incontinence of urine past the age of toilet training; Nocturnal enuresis generally subsides by 6 years of age; if it does not, further investigation and treatment may be warranted; DM, sickle cell, UTI (regression)
Nephrotic syndrome
damage to small blood vessels in the kidney cause an abnormal loss of protein in the urine – proteinuria, facial edema, proteinuria, hypoalbuminemia and hypercholesterolemia, ascites
Acute glomerulonephritis /Acute poststreptococcal glomerulonephritis (APSGN)
condition in which immune processes injure the glomeruli. Immune mechanisms cause inflammation, which results in altered glomerular structure and function in both kidneys
Hemolytic uremic syndrome
Typical HUS features an antecedent diarrheal illness; defined by three features—hemolytic anemia, thrombocytopenia, and acute renal failure
Renal failure (acute and chronic)
condition in which the kidneys cannot concentrate urine, conserve electrolytes, or excrete waste products. As in adults, renal failure in children may occur as an acute or chronic condition (transplant/ dialysis)
Definitions Related to Enuresis
Primary enuresis: enuresis in the child who has never achieved voluntary bladder control.
• Secondary enuresis: urinary incontinence in the child who previously demonstrated bladder control over a period of at least 3 to 6 consecutive months.
• Diurnal enuresis: daytime loss of urinary control.
• Nocturnal enuresis: nighttime bedwetting.
Nursing Goals for the Child with End‐Stage Renal Disease (ESRD)
•Promoting growth and development
•Removing waste products and maintaining fluid balance via dialysis
•Minimize complications by maintaining adequate fluid and nutrition
•Encouraging psychosocial well-being
•Supporting and educating the family
Labial adhesions
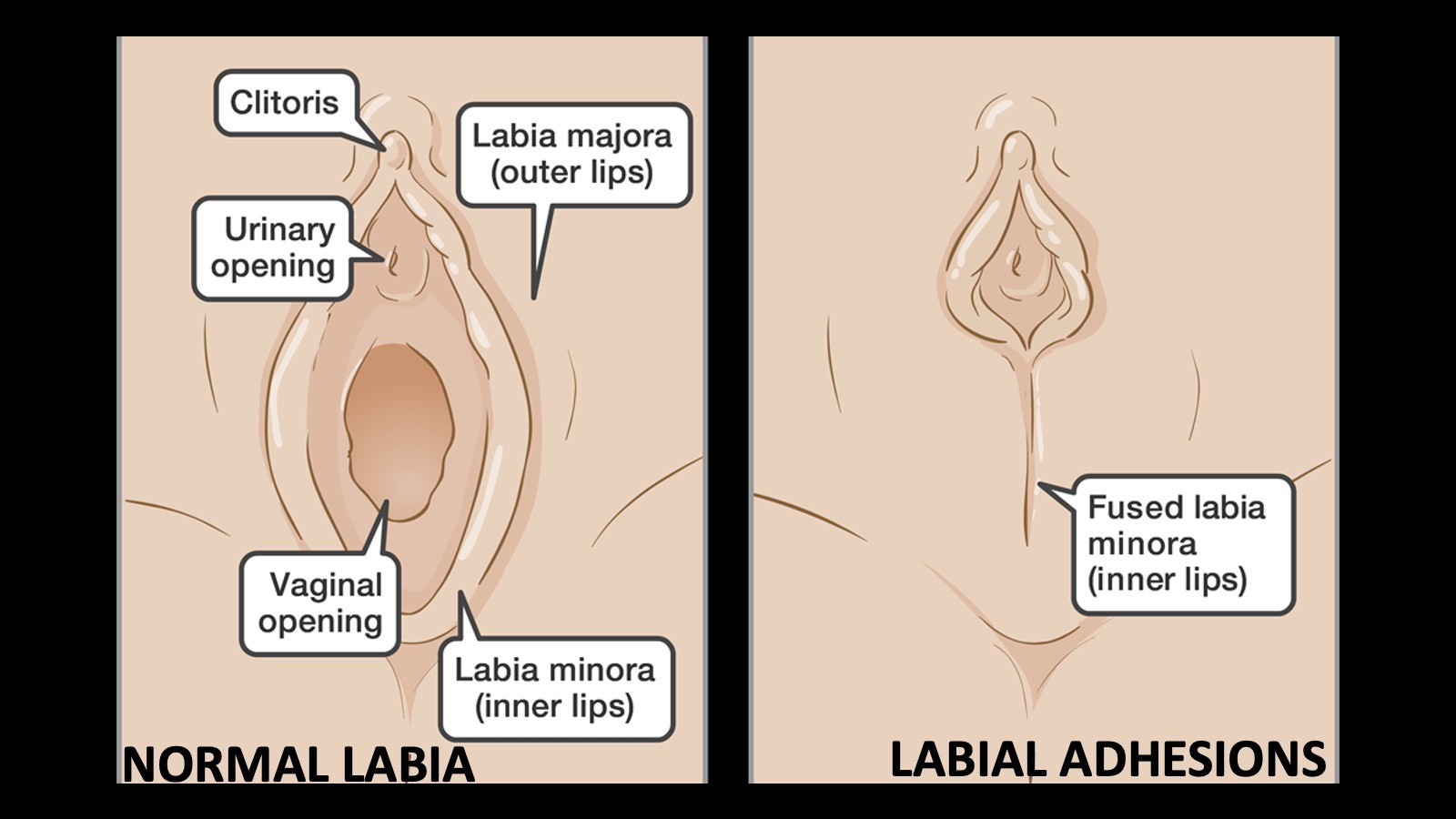
partial or complete adherence of the labia minora (Fig. 43.10). UTI may result from urinary stasis behind the labia; if the adhesions are left untreated, the vaginal orifice may become inaccessible, presenting difficulty with sexual intercourse in the future
Vulvovaginitis
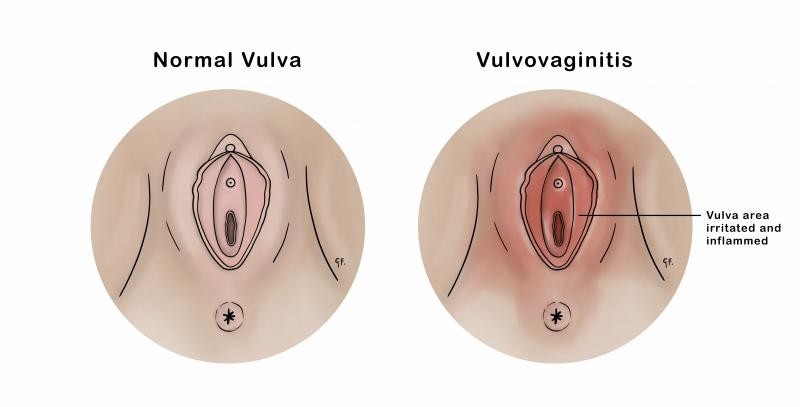
inflammation of the vulva and vagina; hygiene, bacteria, yeast
•Tight clothing may cause a heat rash in the perineal area
•Persistent scratching of the irritated area may result in the complication of superficial skin infection
Phimosis
•inability to retract foreskin (uncircum)
Paraphimosis
•retraction of the phimotic prepuce, which causes a constricting band behind the glans of the penis and results in incarceration if left untreated
Cryptorchidism
•undescended testicles; if not descended-orchiopexy is performed to release the spermatic cord, and the testes are then pulled into the scrotum and tacked into place
Hydrocele
•(fluid in scrotal sac) usually resolves by 1 y/u
Varicocele
•(venous varicosity on spermatic cord) low sperm count, reduced motility
Testicular torsion
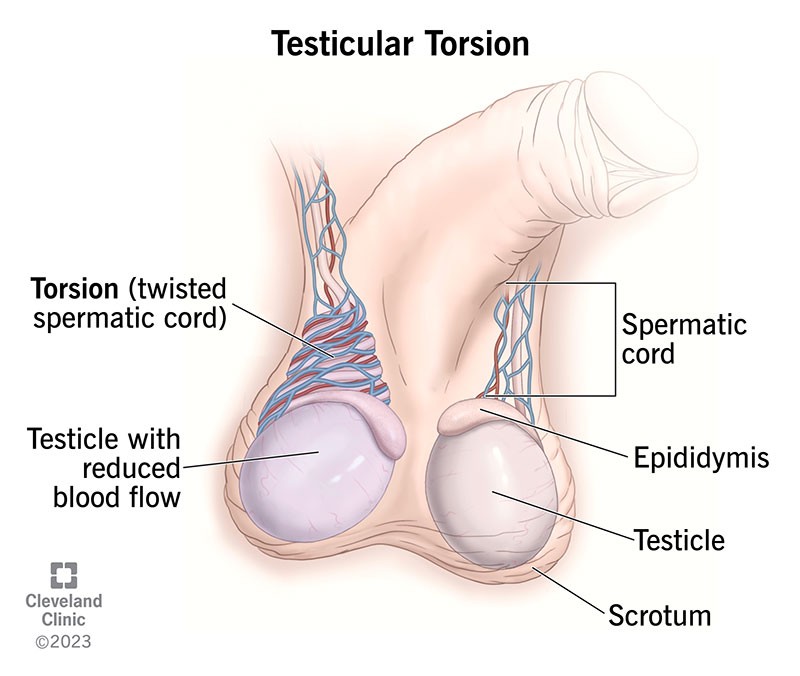
abnormally attached to the scrotum and twisted, medical emergency
•Sudden, severe pain on one side of the scrotum
•Requires immediate surgery because ischemia can result if the torsion is left untreated, leading to infertility
(during puberty)
Epididymitis
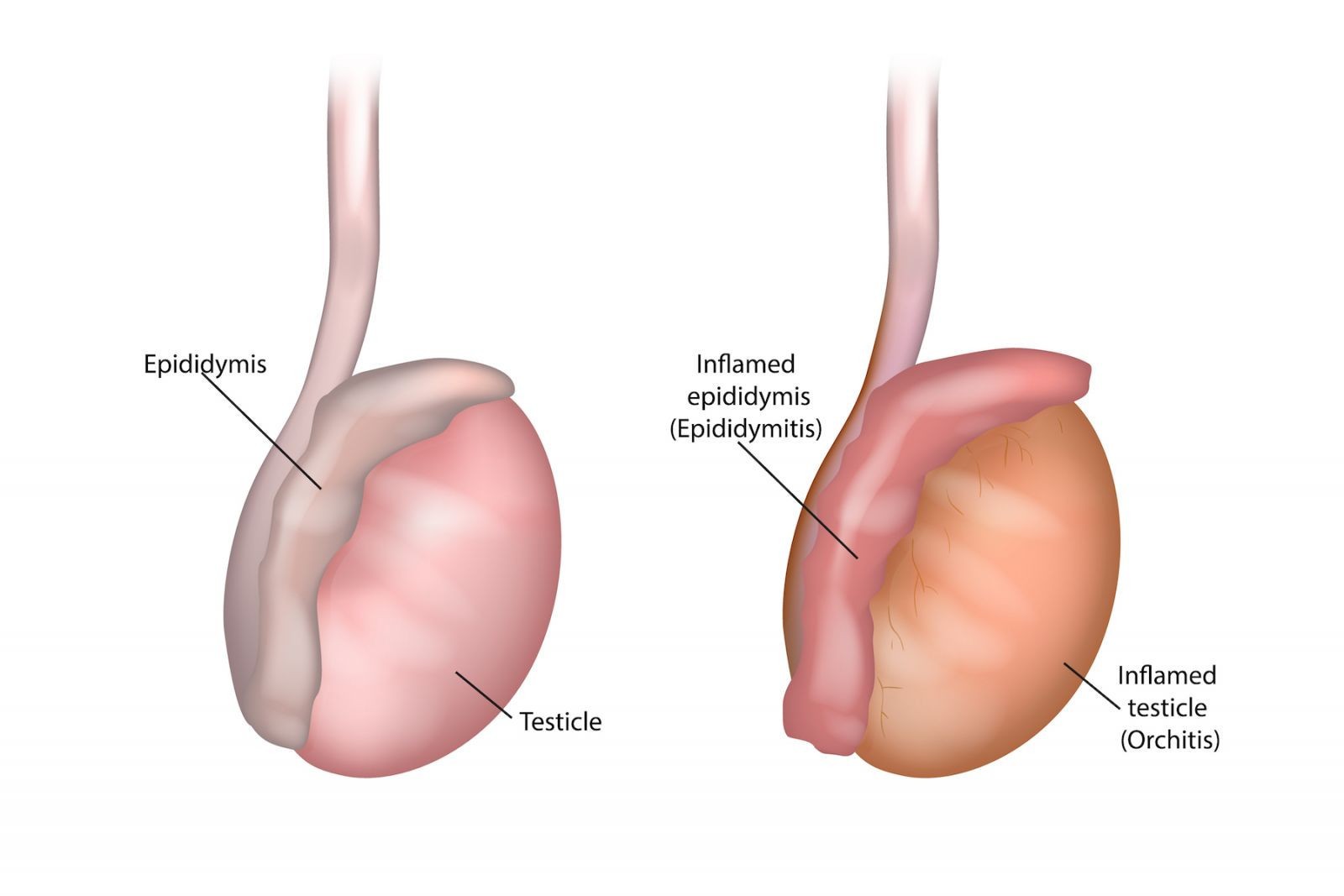
– tube at back of testicle that stores and carries the sperm is inflamed; caused by bacteria; most common causse of pain in scrotum
Signs and Symptoms of Genitourinary Disorders #1
•Burning on urination
•Changes in voiding patterns
•Foul-smelling or dark-colored urine
•Vaginal or urethral discharge
•Genital pain, irritation, or discomfort
•Blood in the urine
•Edema
•Masses in the groin, scrotum, or abdomen
•Flank or abdominal pain; cramps
•Distention in lower abdomen
•Nausea and/or vomiting
•Poor growth; weight gain
•Fever
•Infectious exposure
•Trauma
Common Medical Treatments for Genitourinary Disorders
•Urinary diversion
•Foley catheter
•Ureteral stent
•Nephrostomy tube
•Suprapubic tube
•Vesicostomy
•Appendicovesicostomy
•Bladder augmentation
Dialysis (hemodialysis and peritoneal)
Restoring Fluid and Electrolyte Balance GU
•Monitor vital signs frequently and assess urine specific gravity
•Ensure diet meets required guidelines to support growth
•Maintain strict records of intake and output
•Administer diuretics as ordered
•When urine output is restored, diuresis may be significant
•Monitor for signs of hyperkalemia and hypocalcemia
•Administer packed red blood cell transfusions as ordered
•Dialysis may become necessary
COMMON GI MEDICAL TREATMENTS
•Hydration (oral, enteral, and IV)
•Providing adequate nutrition (oral, enteral, and IV)
•Enemas and bowel preparations
•Ostomies—surgical opening into a digestive organ
•Probiotics—support/replace intestinal microbial flora
•Medications
TENDERNESS WITH PALPATION
Tenderness in the abdomen is not a normal physical finding.
Right upper quadrant tenderness could indicate liver enlargement
Right lower quadrant pain, including rebound tenderness (pain upon release of pressure during palpation),can be a warning sign of appendicitis;
COMMON GI LABORATORY AND DIAGNOSTIC TESTS
Abdominal ultrasonography
Barium swallow, small bowel series
Blood work: amylase, electrolytes, lipase, LFTs
Esophageal manometry/ esophageal pH probe
Endoscopy (gastroscopy, colonoscopy)
Hemoccult, stool sample/culture, stool O&P
Hepatobiliary (HIDA) scan
Liver biopsy
Lactose tolerance test, urea breath test
ORAL REHYDRATION THERAPY
Oral rehydration solution (ORS) should contain
75 mmol/L sodium chloride
13.5 g/L glucose
Standard ORS solutions include Pedialyte, Infalyte, and Ricelyte
NOT appropriate for oral rehydration:
Tap water
Milk
Undiluted fruit juice
Soup
Broth
Mild to moderate dehydration: requires 50 to 100 mL/kg of ORS over 4 hours
MEDICATIONS FOR MANAGEMENT OF GASTROINTESTINAL DISORDERS
Histamine-2 blockers, proton pump inhibitors – reduce gastric acid production; GERD
Prokinetics –stimulates GI mobility; GERD, erosive esophagitis
Antibacterial/antibiotics – C diff
Corticosteroids, immunosuppressants –for autoimmune disorders- Crohn's, ulcerative colitis
Stimulants, laxatives – constipation – softens or increases peristalsis
Antidiarrheals and antiemetics – decrease peristalsis, act on CNS to prevent nausea
Anticholinergics – control cramping
Anti-inflammatories – ulcerative colitis
RISK FACTORS FOR DEHYDRATION
Diarrhea
Vomiting
Decreased oral intake
Sustained high fever
Diabetic ketoacidosis – high level of glucose àcause kidney to excrete glucose and water
Extensive burns
Oral candidiasis
yeast infection- painful and stop from eating) and oral lesions
Hypertrophic pyloric(stomach) stenosis
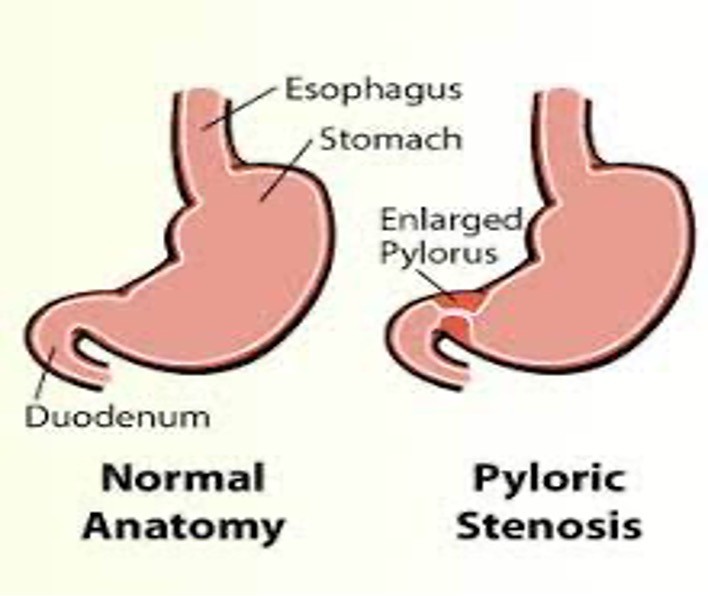
thickening of pyloric muscle; projectile vomiting; 3-6 weeks of life; males > females; **palpable ‘olive’ sized mass RUQ**; pylorectomy(surgery)
Intussusception
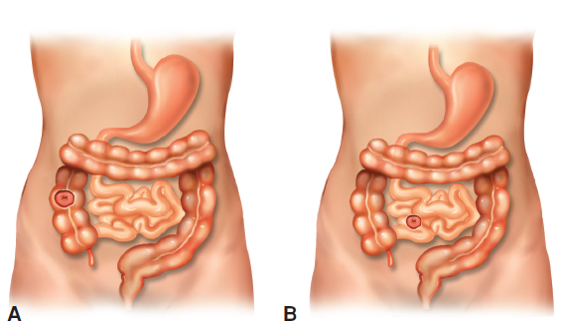
proximal segment of bowel telescopes into more distal section; partial or total bowel obstruction;
currant(red)-jelly stools; sausage shaped mass is hallmark sign
malrotation & volvulus
intestine is abnormally attached and the mesentery narrows, twisting on itself vomiting (yellow-green)
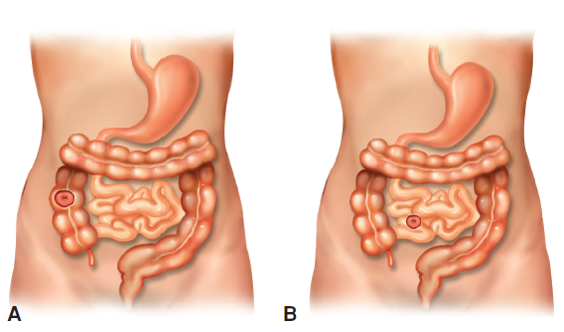
Appendicitis
most common cause of emergent abdominal surgery in children and peaks in prevalence in the second decade of life
Cleft lip and palate
occurs early in pregnancy lip 5-6 weeks, cleft 7-9 weeks; 50% born with cleft lip have cleft palate; may be unilateral (the left side is affected more often) or bilateral (hard to feed/risk for aspiration/surgical procedure but in steps)
Hernias (inguinal and umbilical)
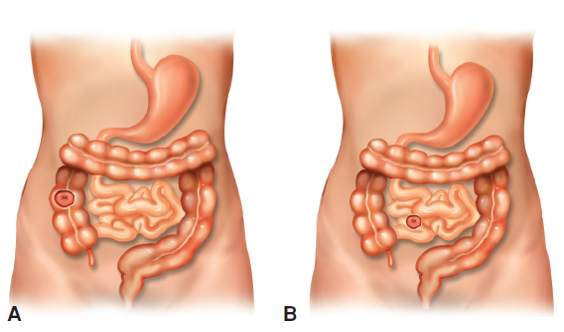
defect during development; abdominal or pelvic viscera to travel through the internal inguinal ring into the inguinal canal. The hernia sacs that develop most often contain bowel in males and fallopian tubes or ovaries in females. Boys are more likely than girls to develop inguinal hernia and premature infants demonstrate an increased incidence overall
ANOMALIES AND COMPLICATIONS ASSOCIATED WITH CLEFT LIP AND PALATE
Anomalies
Heart defects
Ear malformations
Skeletal deformities
Genitourinary abnormality
Complications
Feeding difficulties
Altered dentition
Delayed or altered speech development
Otitis media
Hirschsprung disease
disorder of motility of the intestinal track resulting in obstruction, characterized by failure to pass a stool (meconium) within the first 24 hours of life. This is due to a lack of ganglion cells in the intestine
Short bowel syndrome
clinical syndrome of nutrient malabsorption and excessive intestinal fluid and electrolyte losses that occurs following massive small intestinal loss or surgical resection most common causes of short bowel syndrome are necrotizing enterocolitis, small intestinal atresia, gastroschisis, malrotation with volvulus, and trauma to the small intestine;
Celiac disease
immune disease; gluten causes damage to small intestine; steatorrhea (fatty, bulky, oily stools)
SIGNS AND SYMPTOMS OF CROHN DISEASE AND ULCERATIVE COLITIS
Abdominal cramping
Nighttime symptoms, including waking due to abdominal pain or urge to defecate
Fever
Weight loss
Poor growth
Delayed sexual development
HEPATOBILIARY DISORDERS (liver)
Pancreatitis
Gallbladder disease
Jaundice
Biliary atresia
Hepatitis (multiple types)
Cirrhosis and portal hypertension
Liver transplantation
COLOSTOMY AND ILEOSTOMY
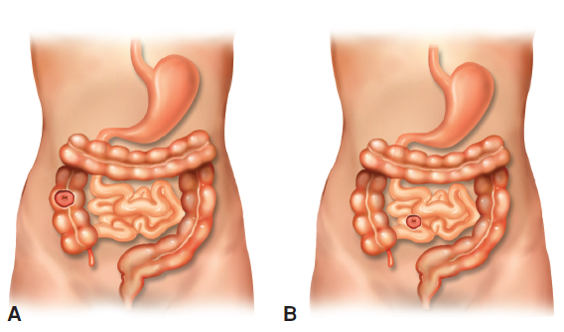
Colostomy- more formed
Ileostomy- watery
BEEFY RED(surrounding skin is good)