presumptive changes of pregnancy
•Amenorrhea
•Nausea and vomiting
•Fatigue
•Urinary frequency
•Breast changes
•Quickening- “first fetal movement”(could be imaginative or gastric)
Quickening
first fetal movement- noticed 16-20 weeks
Probable changes of pregnancy
•Goodell’s and Chadwick’s(blueish color of cervix)and Hegar sign
•Enlargement of the abdomen
•Braxton Hicks contractions- practice contractions(16 weeks)
•Uterine soufflé- swish sound during ultrasound- blooding pumping
•Skin pigmentation changes
•Pregnancy tests
Nageles Rule for pregnancy dating
Begin with the first day of last missed period, subtract 3 months and add 7 days and add 1 year
positive changes of pregnancy
•Fetal heartbeat
•Fetal movement
•Visualization of the fetus
Prior to pregnancy
dietary folic acid
Weight gain recommendations
◦Underweight: 28 to 40 lb
◦Normal weight: 25 to 35 lb
◦Overweight: 15 to 25 lb
◦Obese: Approximately 11 to 20 lb
◦Twins – 46-62 lb for normal pre-pregnancy weight – adjusted according to BMI
Pattern of weight gain
◦First trimester: 2.2 – 4.4 lbs.
◦Second and third trimester: About 1 lb. weekly
◦Twins: Second and third trimesters: 1.5 lbs per week
◦Dieting during pregnancy can result in maternal ketosis
Obesity in Pregnancy
Increased risk of:
◦Gestational diabetes
◦Preeclampsia
◦Induction of labor
◦Cesarean birth
◦Anesthesia complications
◦Venous thrombosis
◦Postpartum hemorrhage
◦Endometritis
◦Fetal anomalies
◦Macrosomia
◦Birth injury
◦Stillbirth
Pregnancy nutritional concerns
◦Calories in second and third trimester
◦Protein increases 25 g daily ( 46 non pregnant + 25 )
◦Water – 3 L daily
◦Caffeine concerns
◦Mercury in fish
◦Artificial Sweeteners
◦Listeria
Vegetarian Diets During Pregnancy
◦There are different types of vegetarian diets
◦Lacto-ovo vegetarians: Dairy and egg products
◦Lacto-vegetarians: Dairy products but no eggs
◦Vegans: No foods from animal sources
◦Most vegans need additional supplementation – vitamins B12, D, and calcium
If the placenta attaches over the cervix what is this called ?
placenta previa
What is the mother at risk for if the placenta covers the cervix ?
-Hemorrhage -C- Section/ baby will not be able to pass through the cervix
Lightening
dropping of baby
Common lab tests for 1st prenatal visit
Complete blood count (CBC)
Blood typing
rubella titer
hepatitis B
HIV testing
STI screening
cervical smears
1st trimester
1-13 weeks
2nd trimester
12-27/28 weeks
3rd trimester
28 weeks 38-42
What are some risk factors for adverse pregnancy outcomes?
diabetes
folic acid deficiency
hepatitis B
HIV/AIDS
Obesity
STIs
smoking
alcohol
What is a non invasive method to monitor the fetus and when can it be done?
Fetal movement counts (kick counts)
from week 28-38
encourage mom to lay on side
encourage mom to eat
Ultrasound
images produced by sound waves to check for possible birth defects
what does an ultrasound assess?
-to estimate gestational age, fetal weight, and growth
-location of placenta and amniotic fluid volume
-accompanying invasive procedures
Doppler blood flow studies
-Intiated at 15 weeks
-measures blood flow changes in maternal and fetal circulation
-assessment of placental function
-if ratio is elevated may indicate baby not growing well
-looks at sys/dias of heart
Why is the doppler blood flow study initiated?
If mother has diabetes or baby is not growing well
What is aminocentesis?
A procedure to obtain amniotic fluid
Allows testing of amniotic fluid
Why is Aminocentesis done?
This test can provide information about genetic disorders and fetal maturity
What are some negatives to having Amniocentesis done?
Hemorrhage
Amniotic fluid embolism
Loss of pregnancy
Rh isoimmunization
Can hurt the fetus
Infection
Cause bleeding
Rupture placenta
Cramping
What does Amniocentesis procedure look like?
Large needled going into amniotic cavity
What is Chorionic villus sampling?
Catheter is used to withdraw a sample of placental tissue to test for chromosomal abnormalities. Test done after 10-13 weeks.
What are the complications of Chorionic villus sampling?
Increased risk of injury to fetus
Inability to detect neural tube defects
Risk of failure to obtain placental tissue
risk of contamination of specimen
risk of leakage of amniotic fluid
risk of intrauterine infection
risk of Rh isoimmunization
What is Alpha-fetoprotein?
Checks the baby's risk of birth defects and genetic disorders, such as high levels for neural tube defects or low levels for Down syndrome. It is done at 15 to 22 weeks gestation.
Nonstress Test
used to assess fetal status using an electronic fetal monitor
If baby moves and heart rate increases-healthy baby
If baby heart rate goes down- unhealthy
Fetal kick counts
Provides reassurance of fetal well being(movement 10 x an hour)
Reactive non-stress test
FHR acceleration of 15 bpm for 15 seconds in response to fetal movement after 32 weeks
for less than 32 weeks 10 bpm for 10 seconds is acceptable
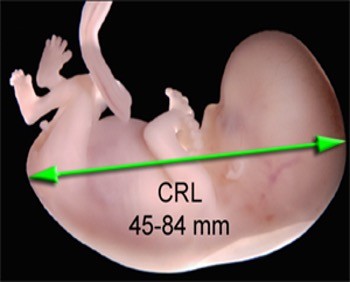
What is crown rump?
Measurement of baby form crown of the head to the buttock shows if the pregnancy is dated correctly
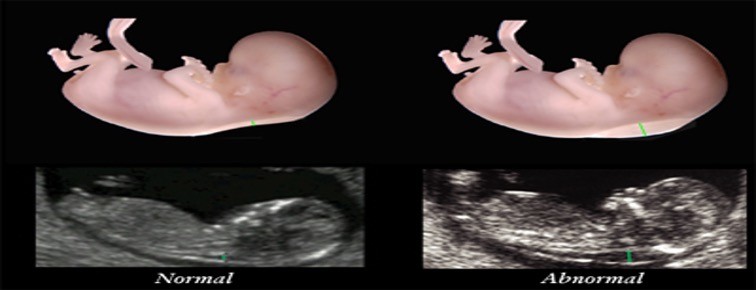
Fetal Nuchal Translucency
An intravaginal ultrasound that measures fluid collection in the subcutaneous space between the skin and the cervical spine of the fetus
What is fetal nuchal translucency used for ?
-Trisomy 21 -looks to see if there is to much fluid -if there is to much fluid further genetic testing is needed
What are the blood test assessments to measure two hormones?
BHCGPAPP-A this is complete the screening for chromosomal abnormalties
When is amniocentesis recommended?
Age 35 and older family history of genetic defects blood test or ultra sound hinting at defects
When is a Non-stress test (NST) done ?
can be done out patient can be done if the mother is past her due date can be done if there is a medical problem
reactive/nonreactive
Nursing interventions if fetus is not moving
lay on left side give sweets wait 30 min give the baby time baby may be sleep they are tiny humans
Contraction Stress Test
Given contraction to see how the baby would tolerate labor- would not be done during preterm stage or mother getting a C-section
Enables identification of fetal risk for asphyxia
Fetal monitor is used
Fetal heart rate response to contractions is noted
Healthy fetus usually tolerates contractions
Positive Contraction Stress Test
Placenta is not working well because baby is not reacting well to contractions(heart rate decelerates)
Biophysical profile ultra sound 5 parameters
- Fetal breathing - Fetal movements body and limbs -Fetal Tone( extension, flextion) - amniotic fluid volume - reactive fetal HR with Reactive NST
RH + baby RH - mother
MOM NEEDS ROHGAM
28 weeks pregnant
RH Negative mother after amniocentesis
MUST GET RHOGAM WITHIN 72 HOURS
Risk if there is not enough amniotic fluid present during ultrasound ?
Can cause fetal Heart deceleration
Percutaneous umbilical blood sampling
Usually for specific circumstances
-to do a blood transfusion
-take blood out
It goes through umbilical cord
Routine Assessments
weight and blood pressure (vital signs)
urine testing for protein, glucose, ketones and nitrites
Fundal height measurement to asses fetal growth
Edema
Blood tests
assessment for quickening (fetal movement)
assessment of fetal heart rate- 110-160
Danger signs of pregnancy 1st trimester
spotting/ bleeding (miscarriage)
painful urination (infection)
severe vomiting (hyperemesis gravidarum)
fever higher than 100 (infection)
lower abdominal pain with dizziness and shoulder pain (indicative of ruptured or ectopic pregnancy)
Danger signs of pregnancy 2nd trimester
regular uterine contractions (preterm labor)
pain in calf, increased foot flexion (DVT)
sudden gush or leakage of fluid from vagina(pre labor rupture of membranes)
absence of fetal movement for more than 12 hours (possible fetal distress or demise)
Danger of 3rd trimester
-sudden weight gain; periorbital or facial edema, severe upper abdominal pain; headache with visual changes (indicative of gestational hypertension and/or preeclampsia
-decrease in fetal daily movement for more than 24 hours (possible demise)
Onset of labor
-Uterine stretch -Oxytocin increases -Increased prostaglandins -Progesterone withdrawal
Five P's of Labor
Passage way ( birth canal ) Passenger ( Fetus ) , powers (contractions) , position( maternal ) , and psychological response
Stage 1 of labor and delivery
Stage 1 is considered true labor and consists of 3 phases Latnet 0-6cmactive 6-8cmTransition phase 8-10cm SHORTEST STAGE MONITOR FETAL HR
1s stage of labor -(LATENT PHASE )
0-6 cm moms relaxed contractions every 5-10 min Lonest stage of labor
1st stage : Active Phase
6-8 cm dilated contractions every 2-5 min
1st stage Transition Phase
8-10 cm mom is ready to push
Stage 2 labor
10 cm moms fully effaced Birth of the baby encourage mom to bear down when pushing
Stage 3 of labor and delivery
birth of placenta within 30 min Never pull umblicusduring this phase there is an increased risk of infection if placenta isn't fully removed PITOCIN
( Prevents hemmorage )
Signs of hemmorrage
Decreased blood pressure Increased Heart Rate
stage 4 of labor and delivery
1-4 hours after delivery assess : mom assess : Temerature not over 100.4 assess Hemmorage
Placenta Seperation signs
uterus rises upward umblicus lenghtens sudden trickle of blood uterus changes to globular PLACENTA SEPERATION HAPPENS IN THE 3rd stage
FUNDUS
Should be firm midlineleveled with umblicus check the fundus and massage it until it is firm if it is soft ( boggy )
assessment
3 x eveyr 5 min
Fundus abnormality
displaced above umblicus one sided = bladder distention
Methergine medication
medication that treats excessive bleeding after childbirth cannot be given if mom has preeclamisia or HTN
Fern test
High estrogens in amniotic fluid cause crystallization of the salts ; crystals appear as a blade of fern
what does Tocodynamometer meausure ?
external fetal monitoring records the frequency and duration of the contractions placed on fundus
what does transducer meausre ?
Fetal Heart tones bottom
Why would IUPC be used ?
cant pick up mothers contractions * obese patients * Oliohydramus * baby Heart rate decreases CERVIX MUST BE OPEN 2 CM water needs to be broken
Leopold's Maneuvers determine
Engage fetus in uteri position of baby presentation lie
Labor induction medication
cytotec amisaprostale cervidil - thins cervix pitocin oxytocin
Abrution placenta
Placenta separates off wall before the baby is born if this happens baby will not receive oxygen or nutrients emergency c section Cause : HTN TRAUMA
Bishop score
Pre labor scoring that helps predict success of induction
High bishop score
Favorable for induction 8-9
Low bishop score indicates
High risk for c- section cervadil medication cytotec
AROM / SROM ( Spontaneous rupture of membranes )
Gush of fluid trickle Pooling in vagina ( SROM) PH greater than 5 ( ninrazine paper) turns blue or green alkaline ph greater than 6.5
What three methods do nurses use to assess frequency duration and intensity of contraction?
Palpation External fetal monitoring (tocotransducer)Internal Fetal Monitoring ( IUPC )
Systemic analgesia
Morphine
Meperidine
Butorphanol
Nalbuphine (decreases nausea and vomiting)
Fentanyl (hypotension/ respiratory depression)
Hydroxyzine (reduces anxiety)
Epidural
regional block
used for labor and cesarean births
patient receive 500 to 1000 ml of normal saline
Oxygen
left lateral position
T8 to T10 of spinal cord
Epidural Opioids
Fentanyl
Sudentanil
Ropivacaine
Morphine
V C
E H
A O
L P
Variable deceleration- Cord compression
Early decelaration- Head compression
Acceleration- OKAY!
Late deceleration- Placental insufficiency
Aminoinfusion
prevents additional cord compression
room temperature saline into uterus with catheter
Tocolytics
Medication to relax uterus
Improves blood flow to uterus decreasing/stopping contractions
ex Terbutaline
used for preterm to stop labor
L
I
O
N
Left lateral side (turn)
Iv fluids
Oxygen
Notify provider
M
I
N
E
Maternal positioning
Identify labor progress
No intervention
Execute intervention
Uterine Resuscitation Steps
1. Change maternal position ex: if on her back turn to left side
2. Provide supplemental oxygen if indicated
3. Give IV bolus for late decelerations or Amnioinfusion for variable decelerations
4. Correct maternal blood pressure: did she just get an epidural?
5. Reduce uterine activity
Alter second stage pushing efforts
Adverse effects of epidural
•Maternal Hypotension
•Bladder Distention
•Prolonged Second Stage
•Catheter Migration
•Cesarean Birth
•Maternal Fever
•Nausea/Vomiting and Pruritus from Epidural Opioids
•Respiratory Depression up to 24 hours
Threatened Abortion
Spotting, cramping, closed cervix, bleeding unto 24-48hrs, may resolve or pregnancy loss
Treatment: Conservative supportive treatment
Possible reduction in activity in conjunction with nutritious diet and adequate hydration
Inevitable abortion
Moderate to severe bleeding cramping, abdominal pain(contractions), cervical dilatation, if rupture of membranes may need DC or DE
Treatment: Vacuum curettage if products of conception are not passed to reduce risk of excessive bleeding and infection
Prostaglandin analogs such as misoprostol to empty uterus of retained tissue (only used if fragments are not completely passed)
Incomplete abortion (passage of some of the products of conception)
Intense abdominal cramping
Heavy vaginal bleeding
Cervical dilation
Treatment: Client stabilization
Evacuation of uterus via D&C or prostaglandin analog
Complete abortion (passage of all products of conception)
History of vaginal bleeding and abdominal pain
Passage of tissue with subsequent decrease in pain and significant decrease in vaginal bleeding
Treatment: No medical or surgical intervention necessary
Follow-up appointment to discuss family planning
Missed abortion (nonviable embryo retained in utero for at least 6 weeks)
Absent uterine contractions
Irregular spotting
Possible progression to inevitable abortion
Treatment: Evacuation of uterus (if inevitable abortion does not occur): suction curettage during first trimester, dilation and evacuation during second trimester
Induction of labor with intravaginal PGE2 suppository to empty uterus without surgical intervention
Recurrent abortion
History of three or more consecutive spontaneous abortions
Not carrying the pregnancy to viability or term
Treatment:Evacuation of uterus (if inevitable abortion does not occur): suction curettage during first trimester, dilation and evacuation during second trimester
Induction of labor with intravaginal PGE2 suppository to empty uterus without surgical intervention
Identification and treatment of underlying cause (possible causes such as genetic or chromosomal abnormalities, reproductive tract abnormalities, chronic diseases or immunologic problems)
Cervical cerclage in second trimester if incom
Management for types of abortion
Ultrasound
•Lab work: pregnancy test, H&H, CBC, T/X
•Bed rest
•Abstinence from sex
•IV / Transfusion
•D & C - Dilation and curettage
•If beyond 12 weeks: induction of labor by oxytocin and Prostaglandins may be used.
•Emotional support and bereavement care
•RhoGAM if Rh negative
Ectopic pregnancy signs and symptoms
•Progressive Abdominal pain
•Delayed menses
•Abnormal vaginal bleeding
•If rupture has occurred may experience referred shoulder pain
diagnose: ultrasound, low hcg, progesterone
Risk factors for Ectopic pregnancy
Tubal surgery
•Sexually transmitted infections
PID
•Previous ectopic pregnancy
•IUD use
•Progestin-only contraceptive
•Pharmacologic treatment of infertility
•Endometriosis
•Assisted reproductive technologies
Ectopic pregnancy treatment
Methotrexate ( folic acid antagonist) Dissolves Pregnancy Given IM
•Must be unruptured, less than 3.5-4cm size or less
•Woman must be in stable condition, no blood , kidney or liver disease
•Surgery-salpingostomy to preserve tube or removal of tube salpingotomy
Cervical Insufficiency
-Premature dilatation of the cervix which leads to 2nd trimester loss around 20 weeks
-Painless dilatation
-Can be diagnosed with transvaginal ultrasounds and speculum examinations
Incompetent Cervix
•Premature dilatation of the cervix
•Associated with repeated second trimester spontaneous abortions
•Painless, bloodless 2nd trimester abortion
•Minimal uterine contractions until late
•Considered an anomaly (uterine/cervical)
•Intrauterine pressure increases
•Internal cervical os dilates and membranes may protrude and rupture
•Spontaneous effacement and dilatation may occur
Placenta Previa
Symptoms
•Painless, quiet onset bright red bleeding
•Bleeding may be intermittent or continuous
•Uterus soft, palpable
•Presenting part is high and deviated to one side
•Associated with preeclampsia
Management of Placenta Previa
Expectant Management
-Observation and bed rest/pelvic rest if less than 36 week gestation, normal FHR and mild bleeding that resolves
-No vaginal or rectal exam
-NST/BP once or twice weekly
-Assess bleeding
-Potential emergency
Active Management
-If past 36 weeks gestation – can deliver
-If excessive or continued bleeding can deliver at any gestational age
Placenta Abruptio
Premature separation of normally implanted placenta from uterine wall
•Drug use; Cocaine
Symptoms
•Dark venous blood
•Abdomen rigid, hard
•Severe pain
•Sudden onset
placenta previa Management
No Vaginal Exams!!
•Daily CBC
•Fetal well-being tests – NST
•Monitor for Contractions
•Monitor Bleeding amount
•Monitor for PROM
•Medication - Celestone
HYPEREMESIS GRAVIDARUM
intractable vomiting during pregnancy, leading to weight loss and volume depletion, resulting in ketonuria and/or ketonemia.
Hyperemesis gravid arum management
-Conservative management in the home is the first line of treatment
-Hospitalization may be necessary to reverse the effects of severe nausea and vomiting
-fluid replacement with normal saline
-NPO for 24 – 36 hours
-Antiemetics may be administered rectally or intravenously
Preeclampsia
It is defined as an increase in blood pressure after 20 weeks gestation accompanied by proteinuria.
(edema, headache, blurry vision, dizziness muscle twitching, swollen face/hands/feet,high BP, abdominal pain, )
Preeclampsia achieve safe outcome
Fetal movement record
Nonstress test (NST)
Ultrasonography every 3 to 4 weeks for serial determination of growth.
Biophysical profile
Amniocentesis to determine fetal lung maturity.
Doppler Velocimetry beginning at 30 to 32 weeks to screen for fetal compromise
Eclampsia(SEIZURE)
-Maintain patent airway and safety during convulsion
-Magnesium sulfate (To control seizures and will continue postpartum)
(headache, seizure, visual disturbances, generalized edema)
-Auscultate lungs to r/o pulmonary edema
-Strict Input and Output (Place foley with urimeter)
-Monitor for placental abruption/ bleeding/rigid abdomen
-Left lateral (To prevent aspiration of vomitus)
-Side rails elevated (To prevent falls)
-Plan for Delivery (IOL vs Cesarean section)
-Seizures can still occur first 48 hours postpartum
Deep tendon reflexes
2+ (normal)
Magnesium Sulfate
Administer calcium gluconate IV if toxicity occurs
-respiratory depression (10 breaths)
-0 deep tendon reflex
HELLP
•Category of gestational hypertension that involves changes in blood components and liver function, as well as, a complication of severe preeclampsia
•H: hemolysis
•EL: elevated liver enzymes
•LP: low platelets
•Patient complains of pain, most commonly in the right upper quadrant, epigastric area, or lower chest.
Effects of HELLP Syndrome on Mom and Baby
•DIC
•Abruptio placentae
•Acute renal failure
•BABY:
•Insufficient blood flow
•Intrauterine growth restriction
•Death
•Increased risk of fetal hypoxia during labor
•Thrombocytopenia
•Leukopenia
What medication matures the babies lungs ? also used in preterm labor
Bethametasone
What is your main concern for Hyperemisis
DEHYDRATION * everything Hypo
What signs will you see of HELLP syndrome
~pale ~Anemic ~bleeding around Iv~black and blue bruises RT UPPER QUADRANT PAIN
What important things should you look out for for terbutaline ?
Causes heart to beat really fats if her hr is high hold the medication if someone has cardiac problems precaution.Helps slow labor down always monitor blood pressure if heart rate is 120 over hold the medicine.decreases potassium
What can cause cervical insufficiency ?
~Repeated pregnancy loss ~Abortions ~Trauma to cervix
Causes of Postpartum hemorrhage
Tone
-Overdistention of uterus
-uterine infection
Tissue
-products of conception (incomplete placenta at birth)
-retained blood clots
Trauma
-lacerations
uterine inversion
Thrombom
-preexisting conditions
-traction on umbilical cord
PPH medications
Pitocin
Carboprost
methergine
misoprostol
oxytocin
How to help PPH
Fundal massage
evaluate bladder
bimanual compression
low level suction
Puerperium
the time from the delivery of the placenta through approximately the first 6 weeks after the delivery
Involution of the uterus
contraction of muscle fibers; catabolism; regeneration of uterine epithelium.
Lochia
Vaginal discharge after childbirth
Ruba
Occurs right after child birth lasting 3-4 days bright red dark red with small clots similar to a period flow
Serosa
Lasts 3-10 days after child birth pinkish brown consistency with a lighter flow
Alba
Lasts 10-14 days after child birth Whitish yellow consistency little to no blood
Voiding sensation is affected by
1.Perennial laceration
2. Hematomas
3. decreased bladder Tone
4. Generalized swelling and bruising of perineum and tissues surrounding the meatus
What are some causes of Post Partum Diuresis ?
1. Large amount of Iv fluid given during labor
2. decreased Antidiuretic effect of oxytocin
3. Build up and retention of extra fluids during pregnancy
4. Decreased production of Aldosterone
What is Postpartum diuresis ?
Excessive production of urine after child birth .
Lactation Hormones
progesterone, estrogen , prolactin
The New born sucking on breast stimulates the pituitary gland to release
prolactin / oxytocin
how is breast engorgement Relieved ?
frequent emptying warm showers cold compress between feedings
Engorgement
Painful swelling of breast tissue as a result of rapid increase in milk production and venous congestion causing interstitial tissue edema; impaired milk flow results in accumulation of milk in breasts; most often occurs between the third and fifth postpartum days
Non lactating women get menstrual cycle
7-9 weeks after birth
Breast feeding frequency and duration last
2-18 months
mood disorders
-baby blues
-post-partum depression
-post-partum psychosis
Risk Factors for Postpartum Infection
-Operative procedure (forceps, cesarean birth, vacuum extraction)
-History of diabetes, including gestational-onset diabetes
-Prolonged labor (more than 24 hours)
-Use of indwelling urinary catheter
-Anemia (hemoglobin <10.5 mg/dL)
-Multiple vaginal examinations during labor
-Prolonged rupture of membranes (>24 hours)
-Manual extraction of placenta
-Compromised immune system (HIV-positive)
Risk Factors for Postpartum Hemorrhage
• Precipitous labor (less than 3 hours)
• Uterine atony
• Placenta previa or abruptio placenta
• Labor induction or augmentation
• Operative procedures (vacuum extraction, forceps, cesarean birth)
• Retained placental fragments
• Prolonged third stage of labor (more than 30 minutes)
• Multiparity, more than three births closely spaced
• Uterine overdistention (large infant, twins, hydramnios)
POST PARTUM DANGER SIGNS
• Fever >100.4°F (38°C)
• Foul-smelling lochia or an unexpected change in color or amount
• Large blood clots or bleeding that saturates a peripad in an hour
• Severe headaches
• Visual changes, such as blurred vision or spots
• Calf pain with dorsiflexion of the foot
• Swelling, redness, or discharge at the episiotomy, epidural, or abdominal sites
• Dysuria, burning, or incomplete emptying of the bladder
• Shortness of breath or difficulty breathing without exertion
• Depression or extreme mood swings
baby blues
a mild postpartum mood disorder that goes away on its own lasts 4-5 days resolve 10 days
postpartum depression
a mood disorder characterized by feelings of sadness and the loss of pleasure in normal activities that can occur shortly after giving birth Lasting longer
post partum depression may lead to
poor bonding alienation from loved ones violent thoughts and actions
Carboprost
treats postpartum uterine Hemorrhage works by contracting the uterus
Taking in phase
-Time immediately after birth when the client needs others to meet her needs and relives the birth process first 24 hrs (range 1-2 days)
-Woman is passive – prefers nurse doing care and making decisions
Taking hold phase
-Second phase characterized by dependent and independent maternal behavior (lasts 10 days to several weeks)
-strong interest in caring for baby
-insecurity if ability to care for baby
Letting go phase
-reestablishes relationships with other people
-accepts role of motherhood not fantasy
BUBBLE – EE
Breast
Uterus
Bladder
Bowel
Lochia
Episiotomy/Perineum/
Epidural
Extremities
Emotional Status
INVOLUTION
Uterus should be midline and firm
If boggy or off to side –
1)massage till firm,
2)express any clots
3)empty bladder
Encourage breastfeeding
NURSING INTERVENTIONS (involution)
Labor and Pregnancy History
Bladder status
Anesthesia
Involution is enhanced by:
Uncomplicated labor and birth
Complete expulsion of placenta or membranes,
Breastfeeding
Early ambulation
LOCHIA SHOULD NOT
¡Have a foul odor
¡Have large clots
¡Saturate a pad in less than ½ hour
AFTERPAINS
-Contractions that occur after birth
-May be increased in pregnancies where uterus was -overdistended
-More increased in multiparas
-Afterpains are usually stronger during breastfeeding
-Pain should be assessed with other vital signs
-Provide comfort measures
-Consider premedicating
-Check for other reasons for pain
EXTREMITIES
Pregnancy is a hypercoagulable state
-Increased risk of venous thromboembolism ( VTE)
-Pulmonary Embolism ( PE)
-Deep Vein Thrombosis ( DVT
Factors that Increase Risk of Clot Formation
1.Stasis
2.Altered Coagulation
3.Localized Vascular damage
EXTREMITIES risk factors
•Anemia
•Diabetes mellitus
•Cigarette smoking
•Obesity
•Preeclampsia
•Hypertension
•Severe varicose veins
•Pregnancy
•Multiple pregnancies
•Cardiovascular disease
•Sickle cell disease
•Postpartum hemorrhage
•Oral contraceptive use
•Cesarean birth
•Severe infection
•Previous thromboembolic disease
•Multiparity
•Bed rest or immobility for 4 days or more
•Maternal age older than 35
LACTATION
•Lactation is the secretion of milk by the breasts. It is thought to be brought about by the interaction of progesterone, estrogen, prolactin, and oxytocin.
•Breast milk typically appears within 4 to 5 days after childbirth.
•First 2 days postpartum breast soft non tender
BREASTFEEDING POSITIONS
•Cradle hold position: The mother’s arm cradles the baby close to the breast with their abdomens against each other and supports the baby’s head and neck with the mother’s other hand supporting the breast.
•Cross- cradle hold position: Similar to the cradle hold, but the baby is supported with the mother’s opposite arm
•Football/clutch hold position: (cesarean, large breast, small/premature, or mum with twins) Potion baby at your side in a semi sitting position facing mom with baby’s legs under mum’s arm. Use pillow to bring the baby up to the level of your nipple.
•Side lying position: (middle of night) Position baby on your side facing you, tummy to tummy. mouth in line with nipple.
BREASTMILK SAFETY
1.Wash your hands before expressing milk or handling breast milk.
2.Find a quiet, clean place to express milk if returned to workplace. Use clean containers to store expressed milk. Use sealed and chilled milk within 24 hours.
3.Discard any milk that has been refrigerated for more than 24 hours.
4.Use any frozen expressed milk within 3 months.
5.Do not use microwave ovens to warm chilled milk.
6.Discard any used milk; never refreeze it.
TYPES OF FORMULAS
•Cow milk protein based formulas: This formula contains cows milk that has been altered to resemble to breast milk. The formula has a lot of nutrients within it that is easier for babies to digest. The only downfall however is some babies are allergic to protein in now milk so that would require a different type of formula such as protein or soy milk etc.
•Soy Based Formulas: This formula contains protein found in soybeans. This is especially great for babies who wish to exclude animal proteins in his/her diet. It is a great option for babies who intolerant and/or allergic to cow milk formula and lactose which is a natural carbohydrate found in cow milk.
•Protein Hydrolysate Formulas: This formula contains protein that has been broken down (hydrolyzed) into tiny sizes than are those in cow milk and soybean formula. Protein hydrolysate formula are meant for babies who have a protein allergy.
ENGORGEMENT
•Heat or Cold
•Cabbage Leaf Compress
•Breast Massage
•Hand expression of milk
•Anti-inflammatory medication
NON BREASTFEEDING
•Wear a supportive snug bra 24 hours daily
•May take 5-7 for milk to be suppressed
•Take mild analgesics
•Don’t stimulate breasts
•Drink fluids
•Reduce salt intake
•Ice packs inside bra - change q 30
MASTITIS
•Infection or inflammation
•Lactating or engorged breasts
•Management
• Heat
• Rest
• Empty Breast
Antibiotics as needed
RH IMMUNE GLOBULIN
For prevention of Rh Isoimmunization
•If mother is Rh negative she receives an IM injection of Rhogam at 28 weeks gestation
• and
•If mother is Rh negative and has a spontaneous birth, abortion ( Spontaneous or Operative, Bleeding in Preganancy, Ectopic, Trauma, External Version, Amniocentisis, Chorionic Villus Sampling , Placenta Previa or Abruption she receives an IM injection of Rhogam within 72 hours of event to prevent sensitization of the mother
•The standard dose of RhoGAM is 300 mcg given intramuscularly,
RH ISOIMMUNIZATION
•If Rh sensitization occurs fetus can develop Hydrops
• Fetalis
• Fetal Edema
• CHF
• Jaundice ( icterus gravis)
• Neurological Damage ( Kernicterus)
Erthroblastosis Fetalsis ( severe hemolytic syndrome)
Newborn vital signs
Respiration: 30-60 (avg 40)
Temp-Rectal: 90-99.5
Axillary: 97.6-98.6
HR: 110-160
BP-Systolic: 60-80
Diastolic: 40-50
Respiratory adaptions to birth
◦Initiation of respirations: adjusting from a fluid filled intrauterine environment to gaseous extrauterine environment
◦Role of surfactant: surface tension redacting lipoprotein that prevents alveolar collapse
◦Respirations: 30-60 breaths per minute; irregular, shallow, unlabored; short periods of apnea (<15 secs); symmetrical chest movements
Cardiovascular changes (fetal to neonate)
1.Increased aortic pressure and decreased venous pressure
2.Increased systemic pressure and decreased pulmonary artery pressure
3.Closure of foramen ovale
4.Closure of the ductus arteriousus
5.Closure of ductus venous
Characteristics of Cardiac Function NB
◦Blood Pressure:
◦varies with birth weight, gestational age, & changes in blood volume
◦average mean is 5 to 55 mm Hg, full term 3 kg newborn. (70/45 to 50/30 mm Hg)
◦Crying may elevate both systolic & diastolic blood pressure
◦Heart Murmurs: 90% of murmurs are transient, not abnormalities
◦Caused by turbulent blood flow through: narrow opening, across an abnormal valve, stenosed valve
◦Atrial or ventricle septal defect (ASD or VSD)
◦Some serious murmurs not recognized for a few weeks until patent ductus arteriosus closes
Renal system changes NB
◦Limited ability to concentrate urine until about 3 months of age (urine has a low specific gravity)
◦6-8 voids a day is normal
◦Low glomerular filtration rate and limited excretion and conservation capability: affect newborn’s ability to excrete salt, water loads, and drugs
G I changes NB
◦Intestines sterile at birth
◦Capacity of newborn stomach varies
◦Newborns prone to regurgitation, vomiting, reflux
◦Meconium formed during fetal life
◦Term newborns pass meconium first 24-48 hours after birth
◦Thick , tarry black or dark green
Immune System changes NB
◦Activates after birth
◦Immature – so s/s of infection may be subtle
◦Fever is not reliable indication of infection
◦Hypothermia or irregular temperature status more reliable sign of infection!!!
◦Infants active passive acquired immunity in utero from mothers response to illness or immunization
Hepatic changes NB
◦At birth infant as iron stores for 4-6 months
◦At birth infants is cut off from maternal glucose
Newborn stools
◦Meconium, then transitional stool, then milk stool
◦Breast-fed newborns: yellow-gold, loose, stringy to pasty, sour smelling
◦Formula-fed newborns: yellow, yellow-green, loose, pasty, or formed, unpleasant order
Neutral Thermal Environment-Newborn
◦Infant stressed by change from warm, moist environment of uterus to dry, drafty environment of delivery room and nursery
◦Neutral thermal environment needed to prevent need for increased oxygen and calories
Heat loss for newborns
◦Thin skin; with the blood vessels close to the surface
◦Lack of shivering ability; limited reserve of metabolic substrates (glucose, glycogen, fat)
◦Limited use of voluntary muscle activity
◦Large body surface area relative to body weight
◦Lack of subcutaneous fat; little ability to conserve heat by changing position
THERMOREGULATION NB
◦Dry immediately with warmed blankets beginning with the head
◦ Skin to skin contact with mother or partner
◦Radiant warmer
◦Stocking cap
◦ Heat regulation is second most critical to the newborn’s survival
◦Hypothermia is a common and dangerous problem
Mechanisms of heat exchange NB
◦Conduction: transfer of heat from object to object when the two objects are in direct contact with each other
◦Convection: flow of heat from body surface to cooler surrounding airor air circulating over a body surface/ also from drafts
◦Evaporation(most common): loss of heat when liquid is converted to a vapor
◦Radiation: loss of body heat to cooler solid surfaces in proximity but not in direct contact (cold weight)
Consequences of Cold Stress NB
◦Increased Metabolic Use of Calories
• Failure to gain weight or weight loss
◦Increased Oxygen Consumption
• May lead to hypoxia, acidosis and respiratory distress
◦Rapid Depletion of Glycogen
• Resulting in hypoglycemia
If allowed to continue the baby may develop shock and disseminated intravascular coagulation (DIC) leading ultimately to death.
Behavioral patterns of newborns
First period of reactivity
•Birth to 30 minutes to 2hours after birth
•Newborn is alert, moving, may appear hungry
Period of decreased responsiveness
•30-120mins old
•Period of sleep or decreased activity
Second period of reactivity
•2-8hrs old
•Newborn awakens and shows an interest in stimuli
PRIORITIES OF CARE OF THE NEWBORN
•Establish and maintain an airway and respirations
•Provide warmth and prevent hypothermia
•Provide a safe environment and routine preventive measures
•Promote maternal-infant attachment
Initial newborn assessment
•Apgar scores
•Length/ Weight
•Vital signs
•Physical maturity
Neuromuscular maturity
Signs indicating a problem during NB Assessment
•Signs indicating a problem
•Nasal flaring, chest retractions
•Grunting on exhalation, labored breathing
•Generalized cyanosis, flaccid body posture
•Abnormal breath sounds, abnormal respiratory rates
•Abnormal heart rates, abnormal newborn size
Apgar scoring system
Activity
Pulse
Grimace
Appearance
Respiration
(do 1st and 5th minute of life)
8-10 = an uncompromised or distress free
4-7 = moderately compromised or asphyxiated
0-3 = severely compromised or asphyxiated
Less than 7- do it again in 10 minutes
Nurse’s Responsibility (newborn)
•Initiate Neonatal Resuscitation if necessary
•Assign Apgar score ( if pediatrician not present)
•ID bracelets for baby & mother
•Footprints of baby & mother’s finger print
•Vital signs of baby (30 minutes X4)
•Assist with skin/skin & breastfeeding
•Administer Vitamin K (IM)
•Apply antibiotic eye ointment (or drops)
•Physical assessment of newborn (abbreviated version)
–Size & contours of head, including fontanels, relationship to body
–Assess breathing for flaring of nares, grunting or retractions of chest
–Posture & tone of body
–Symmetry of face, including eyes, ears, nose,
–Arms & legs equal in length, digits on hands & feet.
–Any visual abnormalities
–Obtain height & weight of newborn
Normal Newborn Appearance
Vernix- protection when baby in utero (not every baby)
Cyanotic hand and feet
Milia- little sebaceous glands
Stork Bites
Foreskin intact
Lanugo hair
Mongolian spots
Erythema toxicum
Harlequin sign
Nevus flammeus
Nevus vasculosus
what do Mongolian spits look like?
blue-gray spots
What does Erythema toxicum look like?
Red streaks
Benign
Its the skins way reacting to new environment
Variations in head size and shape newborn
Variations
•Molding
•Caput succedaneum
•Cephalohematoma
Abnormalities
•Microcephaly
•Macrocephaly
•Large, small or closed fontanelles
Fontanelles
Anterior –
Diamond shaped
Closes at 12-18 months of age
Posterior
Triangular – may be difficult
To palpate in the newborn
Closed by the end of the 2nd month
What is caput Succedaneum?
Boggy edematous swelling of fetal scalp(disappears w/o treatment)
No pathological treatment
soft-pits
Crosses the suture line (fluid/edema)
What is cephalohematoma?
Boggy edematous swelling of fetal scalp(disappears w/o treatment)
No pathological treatment
soft-pits
Crosses the suture line (fluid/edema)
What is cephalohematoma?
No treatment required
disappears within 6-8 weeks-months
soft-elastic
On one side of the suture line (positive blood)
Newborn reflexes
•Sucking: (non-nutritive sucking on lips)
•Rooting: baby turns head to side of mouth or cheek that is touched, may open mouth (4 months)
•Palmer Grasping
•Moro: lifting arms up & letting go: arms up fingers, spread out, (6 months)
•Startle
•Tonic neck: fencer position, head is turned to one side, extremities straighten on that side & flex on the opposite side (3 months)
•Babinski: gently stroke sole of foot, fanning out and extension of toes
•Stepping reflex: puts one step down in front of other, (4-8 weeks)
•Blink, Gag & Sneeze are protective reflexes
Common concerns NB
•Transient tachypnea of the newborn
(Baby breathing fast/ will go away but will still need to monitor
Starts 4-6 hrs after birth)
•Physiologic jaundice (hyperbilirubinemia)
•Hypoglycemia
TRANSIENT TACHYPNEA OF THE NEWBORN
•Usually results from excess fluid in lungs
•Infant breathes normally at birth but develops symptoms of respiratory distress by 4 to 6 hours of age
•Clinically can resemble RDS
•May be seen cesarean-birth newborns
•Usually resolves over 24 – 72 hours
Nursing interventions for transient tachypnea
•Providing oxygen
•Ensuring warmth
•Observing respiratory status frequently
•Allowing time for pulmonary capillaries and the lymphatics to remove the remaining fluid
Meconium Aspiration Syndrome
•A cause of respiratory failure in term and post-term infants
•Intrauterine distress can cause passage of meconium into the amniotic fluid before birth
•Factors that promote the passage in utero include placental insufficiency, maternal hypertension, preeclampsia, fetal hypoxia, transient umbilical compression, oligohydramnios, and maternal drug abuse, especially of tobacco and cocaine
• Occurs when the newborn inhales particulate meconium mixed with amniotic fluid into the lungs while still in utero or on taking the first breath after birth
•Severe MAS can lead to persistent pulmonary hypertension and death
What Causes Newborn Jaundice
UNCONJUGATED BILIRUBIN
Indirect bilirubin is fat soluble and
not easily excreted by the GI Tract or
kidneys – accumulated in
blood and is deposited in the skin,
sclera and mucus membranes
CONJUGATED BILIRUBIN
Direct bilirubin – easily excreted
Maternal Risk Factors for Neonatal Jaundice
•Blood type ABO or Rh incompatibility – Mother’s blood type is O and fetal is A,B or AB – The infant is not born anemic, hemolysis of the blood begins with birth when blood and antibodies are exchanged as the placenta separates – red blood cells are destroyed
•Breastfeeding
•Drugs : Diazepam, Oxytocin
•Ethnicity: Asian, Native American
Maternal illness : Gestational Diabetes
Nursing interventions for physiologic jaundice
•Begins after 24hours of age
•Frequent breast or formula feeding
•Phototherapy
•Monitor hydration status, stools, skin color
Pathological jaundice (before 24hrs/ SERIOUS)
Nursing Interventions to Decrease Incidence of Hyperbilirubenemia
•Maintain newborn skin temperature at 97.8 degrees
•Monitor stool for frequency and characteristics
•Encourage early feedings
Care for newborn receiving phototherapy:
•Monitor body temp
•Document stools
•Document wet diapers
•Turn frequently
•Observe skin integrity
•Provide eye protection
•Encourage parents to participate
REDUCING BILIRUBIN LEVELSPhototherapy
• Place the newborn under the lights or on the fiberoptic blanket
•Expose as much skin as possible
•Cover the newborn’s genitals and shield the eyes
• Turn the newborn every 2 hours
•Remove the newborn from the lights only for feedings.
•Maintain a neutral thermal environment
•Assess the newborn’s temperature every 3 to 4 hours as indicated.
•Monitor fluid intake and output
•Monitor stool for consistency and frequency. Unconjugated bilirubin excreted in the feces will produce a greenish appearance, and typically stools are loose
•Monitor serum bilirubin levels
Long-Term Complications for the Infant with Fetal Alcohol Syndrome
–Delay in oral feeding development
–Central nervous system (CNS) dysfunctions most common
–Impulsivity, cognitive impairment, speech and language abnormalities
–Learning disabilities indicative of CNS involvement
Nursing interventions for Hypoglycemia
Plasma glucose concentration less than 45mg/dL in the first 72hrs of life
•Rapid acting glucose source
•Dextrose gel
•Breastfeeding
•Formula feeding
•Monitor for symptoms
(When baby in utero and getting glucose from mother, baby makes insulin)
Selected screening for newborns
•Phenylketonuria (PKU)
•Congenital hypothyroidism
•Galactosemia
•Sickle cell anemia
•Hearing (universal screening)
NEWBORN SCREENING
•Should be done in first 24-48 hours of life but NOT before 24 hours –
•Should be done after infant has been breast/formula fed
•Puncture of newborn’s warmed heal
•Blood is collected on filter paper completely filing the circles
Cord care
•Remove clamp after 24hrs, will get blk by 2nd/3rd day
•By day 7-10 it will fall off
•Fold diaper below it
•Never pull on it
•No bath until it falls off and heal
What is a Circumcision? What are the side effects?
a surgical procedure in which the prepuce, an epithelial layer, covering tip of penis is removed
–Permit exposure of glands for easier cleaning
–Not performed on premature or compromised infant
–Local and oral pain relief medications are used
•Side effects:
–Infection
–Hemorrhage
–Pain, restlessness
–Difficulty in voiding
–Damage to urethra, stenosis may develop.
CIRCUMCISION musts
•Infant should be at least 12 hours old or older
•Infant has received standard vitamin K prophylaxis
•Infant has voided normally at least once since birth
•Infant has not eaten for at least an hour prior to the procedure
•Written parental consent has been obtained
•Correct identification of the infant brought to the procedure room
Care OF THE CIRCUMCISION
•Assess for bleeding every 30 minutes for at least 2 hours.
•Document the first voiding to evaluate for urinary obstruction or edema.
•Squeeze soapy water over the area daily and then rinse with warm water. Pat dry.
•Apply a small amount of petroleum jelly with every diaper change if the Plastibell was used; clean with mild soap and water if other techniques were used.
•Fasten the diaper loosely over the penis and avoiding placing the newborn on his abdomen to prevent friction.
•Do not remove yellow exudate from penis
newborn period: breastfeeding
Concerns
sore nipples
Engorgement
Mastitis
L: how well infant latches onto the breast
A: amount of audible swallowing
T: nipple type
C: level of comfort
H: Amount of help mother needs
Miscarriage Signs and symptoms
Vaginal bleeding
uterine cramping
Backache
Decreasing HCG levels
Cerclage
Cerclage Procedures:
-McDonald procedure a purse-string technique is placed high up in the cervix and then tied closed. (12,3,6,9 and tied at 12 o’clock)
-Shirodkar procedure places a submucosal band at the level of the internal os.
-Abdominal Cerclage: band is placed around cervix through abdomen.
Cerclage NURSING MANGEMENT
•Monitor for signs of preterm labor
•Monitor for backache
•Monitor for increase in vaginal discharge
•Monitor of ruptured membranes
•Education
A new mother comes into the ED with Placenta abruption. After the successful delivery of her baby she notices the 24 hour newborn is pooping blood what should the nurse do ?
Inform the mother that this is normal the baby might of swallowed blood in utero
What can cause cervical insufficiency ?
~Repeated pregnancy loss ~Abortions ~Trauma to cervix
What is a sign of cervical insufficiency ?
cervix will be dilating and shortening before 37 weeks
Subinvolution
incomplete involution of uterus after birth
•Failure of uterus to return to normal size after pregnancy – lochia rubra of greater than 2 weeks duration suggests subinvolution
Caused by:
•Retained placental fragments
•Distended bladder
•Uterine myoma
•Infection
Infection
•Puerperal/Postpartum/Endometritis
Mastitis
•Risk Factors
Prolonged ROM
Prolonged labor
Fetal scalp electrode or IUPC
BV or Chlamydia infection
Vacuum or forceps use
Manual removal of placenta
Episiotomy of laceration
Compromised health status or DM
Endometritis
•Most common with labor then c-section
•Bacteria from the vagina, bowel and perineum invade the uterus
•S/S start within 1-2 days of delivery; fever, tachycardia, uterine tenderness
•Antibiotics needed
Complications of Diabetes
Without treatment high levels of glucose can accumulate in the blood and damage organs, including blood vessels, eyes, and kidneys
Some individuals with diabetes need daily insulin injections to prevent these complications
Glucose and Insulin
•When the body cells lack insulin, it is unable to use the foods eaten for energy
•Glucose builds up in the blood stream
•Without available glucose for energy, the body will break down stored fats for fuel and energy
•A byproduct of the breakdown of fats—ketones will begin to circulate
•Large amounts of ketones can cause coma and death
Diabetes Mellitus
Glucose crosses the placenta, Insulin does not
-At 10 weeks maternal glucose levels rise fetal glucose levels are increased resulting in increased fetal insulin secretion
-Insulin requirement may double or quadruple by the end of pregnancy
-Renal threshold for glucose decreases
-Increased risk of ketoacidosis
-Nephropathy and retinopathy may develop
-After the placenta is delivered insulin requirements decrease
How Pregnancy Affects Diabetes
•During the first trimester, less insulin may be needed because less food may be eaten
•After the third month, more insulin is needed because the placenta produces substances that weaken insulin
Diabetes and the Fetus
•Fetus has a continuous need for nutrients
•This produces a stress on the maternal system with a constant drain of glucose and amino acids potentially leading to hypoglycemia and ketoacidosis
•If the mother’s blood sugar becomes too high or too low, development of the fetus may be affected
•Research has proven that strict regulation of maternal glucose levels is essential to optimal perinatal outcome
MATERNAL RISKS (GD)
Polyhydramnios
Hyperglycemia
Preeclampsia
Increased risk for cesarean delivery
FETAL RISKS (GD)
Macrosomia
Heart defects
Spina bifida
Increased risk of miscarriage and stillbirth
Birth injuries
GESTATIONAL DIABETES AND EFFECTS ON THE FETUS
Babies of all diabetic women are at increased risk of health problems arising during the newborn period
1.Respiratory distress
2.Hypoglycemia
3.Low calcium levels
4.Hyperbilirubinemia; jaundice
Risks of Gestational Diabetes
•Women older than age 25 years
•Obesity
•Insulin resistance
•Polycystic ovary syndrome
•History of pregnancy-related diabetes mellitus
•History of a large for gestational age infant, hydramnios
•Stillbirth, miscarriage, or an infant with congenital anomalies during a previous pregnancy
•Family history of type 2 diabetes (first-degree relative)
•Ethnicity
Glucose Challenge Test
•All pregnant women should be screened for gestational diabetes
•Screen between the 24th and 28th week of pregnancy
•Take a blood sample one hour after consuming a drink containing 50 grams of glucose
Screening for Gestational Diabetes
•Results of blood sugar >130-140 mg/dL requires follow up with a 3 hour oral glucose tolerance test (OGTT)
•Involves drawing samples 1, 2, and 3 hours after drinking 100 grams of glucose
ORAL GLUCOSE TOLERANCE TEST
The diagnosis of GDM is made when two values or more of the threshold are above the norm.
According to the American Diabetes Association (ADA) (2010), the normal plasma values are:
FBS less than 95mg/dL
1hr less than 180mg/dL
2hr less than 155mg/dL
3hr less than 140 mg/dL
TREATMENT FOR GESTATIONAL DIABETES
•Once gestational diabetes is diagnosed, most women can control their blood sugar levels with diet; about 10% require insulin injections
•After delivery, blood sugar levels should return to normal
•Fetal surveillance
•Women with gestational diabetes are at increased risk of developing diabetes in the future and of developing gestational diabetes in any later pregnancy
•Requires the addition of oral medications and/or insulin, depending on the blood glucose levels.
Fetal Surveillance
•Ultrasounds
•NST
•Amniocentesis
Psychosocial support GDM
•Education re: hypo and hyperglycemia
•Must see their doctor more often
•Follow a carefully prescribed diet
•Monitor blood sugar levels
•These necessary steps may lead to increased stress levels
•Support group
Labor and Postpartum Management GDM
•Primary goal is is to control maternal glucose levels in labor to prevent neonatal hypoglycemia
•Maternal glucose levels are measured regularly
•Labor patients receiving insulin usually receive insulin on a sliding scale
•IV insulin is discontinued after the delivery of the placenta
•Gestational Diabetics usually has normal glucose values by 24 hours postpartum
•Gestational Diabetics are retested at 6 weeks postpartum
Infant of the diabetic mother
Asphyxia
Birth injury because of large size:
Shoulder dystocia: brachial plexus nerve injuries, facial paralysis, intracranial hemorrhage, fractured clavicle
Congenital anomalies
Respiratory distress
Hypoglycemia
Classic IDM(INFANT OF DIABETIC MOTHER)
•Macrosomatic
•Excess adipose tissue
•Cherubic round face
•Hypotonic extremities
•Reddened Appearance
•Difficulty feeding
Symptoms of hypoglycemia
•Jitteriness
•Twitching of the extremities
•Apnea
•Hypotonia
•Tachypnea
•Seizures
Risk Factors for Preterm Labor
Multiple Gestation
Cervical Incompetence
Polyhydraminos
Uterine anomaly
Fetal abnormality
Febrile Illness
UTI/Pylonephritis
Previous history of
Uterine irritability
History of cervical surgery
Age < 18 or > 35
Low socioeconomic status
Cigarette smoking
Substance abuse
STI
Anemia
IUD
Prevention of Preterm Labor (PTL)
•Teaching
Recognize Symptoms of PTL
Bed Rest
Empty bladder
Pelvic rest
Palpate for contractions
Drink water
Treatment of Preterm Labor
•IV Hydration
Tocolytics
Nifedipine ( Procardia ) administered orally or sublingual few maternal side effects hypotension, tachycardia, facial flushing and headache
Magnesium Sulfate
Terbutaline
Terbutaline ( Brethine)
Side Effects – Tachycardia Headache/Hypotension/Increased blood glucose/pulmonary edema
Use Terbutaline with caution in women with diabetes mellitus and thyroid dysfunction
Monitor B/P and pulse if pulse is > 120 bpm hold
medication
May need EKG prior to or with continued doses
Initially given as sq and changed to PO maintenance when
contractions have subsided
Chorioamnionitis
•Bacterial infection in the amniotic cavity
•Most commonly occurs after rupture of membranes
•Diagnosed by symptoms fever, maternal/fetal tachycardia, uterine tenderness, foul smelling amniotic fluid
•Treated with broad spectrum antibiotics
Group B Streptococcal Infection
•Bacterial infection
•Found in lower GI or GU tracts
•Transmitted to fetus in utero or during childbirth
•Associated with poor pregnancy outcomes
•Results from vertical transmission from the birth canal of the infected mother to the infant during birth
Treated in labor (penicillin G or vancomycin)
Group B Streptococcal Infection Risk Factors
Preterm Labor
Maternal Intrapartum Fever
Prolonged Rupture of Membranes
Previous Birth of Infected Infant
GBS bacteriuria in current pregnancy
Group B Streptococcal Infection to know
•All pregnant women should be screened at 35-37 weeks gestation with vaginal/rectal swab
•Women who are GBS carriers should receive antibiotic with labor and/or ROM
( In urine = high colonization) they do not need to have vaginal/rectal swab done at 35-37 weeks
• If woman has had a child with GBS disease she should receive prophylaxis in labor ( no culture)
External Cephalic Version
-Turning the fetus from breech to vertex
-Done Externally
-Success Rate 51% - 65%
35-36 weeks (turn baby if breech, give terbutaline- uterine relaxation)
External Cephalic Version before
-Reactive Non Stress Test prior
-Fetus cannot be engaged in pelvis
-IV
Terbutaline
-Ultrasound
-valid blood type and screen sample
stop procedure if:
-severe maternal pain
-fetal bradycardia
External Cephalic version contraindications
-Bleeding in the 3rd Trimester
-Multiple gestation (twins)
-Oliohydramnios
-Uteroplacental insufficiency
-Nuchal Cord
-Previous C/S
Cervical Ripening
Softening and effacing of cervix
Prostaglandins
•Cervidil
•Misoprostol (Cytotec)
•Used for PP hemorrhage
•Contraindicated for previous
•cesarean birth
Inserted in vagina, left in for 12 hrs
-monitor them for every 2 hours
Cervical ripening nursing management
•Providers administer medication
•Support and inform patient
•Continuous EFM
•Monitor for hyper stimulation
Induction and Augmentation
•Cervical ripening is the process of effecting physical softening and distensibility of the cervix in preparation for labor and birth.
•Induction of labor is the stimulation of uterine contractions before the spontaneous onset of labor for the purpose of accomplishing vaginal birth.
•Augmentation of labor is the stimulation of ineffective uterine contractions after the spontaneous onset of labor to manage labor dystocia.
Methods of Induction
•Stripping membranes
•Amniotomy
•Pitocin infusion
•Complementary Methods
•Sexual intercourse
•Nipple stimulation
•Herbs
Mechanical dilators
Indications for Induction of Labor
•Abruptio placentae (depends on extent of abruption and absence of maternal fetal compromise)
•Chorioamnionitis
•Fetal demise
• Gestational hypertension
• Preeclampsia
• Eclampsia
•Premature rupture of membranes
• Postterm pregnancy
• Some maternal medical conditions
• Fetal compromise (e.g. IUGR)
Oxytocin
•IV piggyback infusion
•Baseline vitals
•Reassuring tracing
•Continuous EFM
•RN increases or decreases Pitocin
•Discontinue Pitocin if needed
Oxytocin: Nursing Responsibilities
•Titrate oxytocin according to maternal & fetal response:
• Decrease dosage or discontinue medication when contractions are too frequent.
•Discontinue medication if abnormal or indeterminate FHR patterns occur.
• Increase dosage when uterine activity and labor progress are inadequate.
•Baseline Vitals
•Continuous EFM
Operative Vaginal Delivery
Forceps
•Outlet Forceps
•Low Forceps
•Midforceps
Vacuum
•Apply suction cup
Negative pressure
Forceps
•Use of specialized instrument with two curved blades to assist birth of the fetal head
Vacuum
•No more than 600 mmHg
•Three pop offs
•Total 20 minutes
Vacuum nursing management
-Keep patient and partner informed
-Continuous EFM
-Examine infant after birth
Vacuum-Assisted Birth:PotentialNeonatal Risks
•Scalp lacerations
• Cephalohematoma
• Subgaleal hemorrhage
• Intracranial swelling
• Hyperbilirubinemia
• Retinal hemorrhage
Cesarean Birth
•Oldest surgical procedure
Rate rising
•Repeats due to risk of uterine rupture
Request for C/S for first time mothers
Never less than 39 weeks
Vaginal Birth AfterCesarean Birth (VBAC)
•Trial of labor following previous cesarean birth (TOLAC)
• Requires evaluation of potential maternal, fetal, and neonatal risks and benefits
•Successful VBAC associated with less morbidity than cesarean birth
•Alternative to repeat cesarean
Contraindications to VBAC
•Previous classical or T-shaped uterine incision or other transfundal uterine surgery
•Previous uterine rupture
•Medical or obstetric problem that precludes vaginal delivery
• Two prior uterine scars and no vaginal deliveries
VBAC Risks If Uterine Rupture Occurs
-Hemorrhage
-Uterine scar separation
-Hysterectomy
-Surgical injuries
-Infant death
-Neurologic complications
VBAC Nursing management
•Continuous EFM
•IV access
•Support
•Comfort measures
•Keep family informed
Encouragement
Amniotomy
•Artificial rupture of membranes (AROM)
•Shortens labor
•Augments labor
•Internal monitoring
Assessment of amniotic fluid
AROM Nursing Management
•Use of amnihook by provider
•Tears membranes
•Explain procedure to patient
•FHR assessed before and after
• Assess amniotic fluid
•Monitor temperature and perform q2h
Heart Disease
•Pregnancy increased
•Cardiac output
•Heart rate
•Blood volume
Heart disease Nursing Management
•Assess the stress of pregnancy on the heart’s functioning
•Limitation of activity
•Monitor for signs of impending cardiac failure
•Health teaching
Causes of Persistent OP Fetal Positioning
•Poor quality contractions
•Abnormal flexion of head
•Inadequate maternal pushing efforts – usually due to regional anesthesia
•Large fetus
Cord Prolapse
EMERGENCY UMBILICAL CORD COMPLICATION
-water breaks before baby is at birth canal
-umbilical cord comes before baby (cord high risk for compression)
-Emergency c-section
Cord prolapse diagnosis
-appearance of loop of umbilical cord
-pulsation of cord on v/e
-suspect in unexplained fetal distress
-variable deceleration
-prolonged bradycardia
Nursing Care in Prolapsed Umbilical Cord
•Assess for nonreassuring fetal status
•If a loop of cord is discovered, the examiner’s gloved fingers must remain in vagina to provide firm pressure on fetal head until physician or CNM arrives
•Oxygen via face mask
•Monitor FHR to determine whether cord compression is adequately relieved
•Woman assumes knee-chest position or bed is adjusted to Trendelenburg position
•Transport to the delivery or operating room in this position
Shoulder Dystocia
HELPERR
Call for Help
Evaluate for Epiostomy
Legs: McRoberts Maneuber
External Pressure-suprapubic
Enter: rotational maneuvers
Remove the posterior arm
Roll the patient to her hands and knees
Management of shoulder dystocia
BECALM
Breathe, do not push; lower head of bed
Elevate legs into McRoberts
Call for help- nurses, anethesiologists
Apply suprapubic pressure- downward & lateral
Enlarge vaginal opening with episiotomy
Maneuvers
Birth Weight Variations
■AGA: about 80% of newborns; normal height, weight, head circumference, body mass index
■SGA: weight <2500g (5lbs, 8oz) at term or below the 10th percentile
■LGA: weight >90th percentile; weight >4000g (8lbs, 13oz) at term
■Low Birth Weight (LBW): weighing <2500g or 5.5lb
■Very Low Birth Weight (VLBW): weighing <1500g or 3.5lb
■Extremely Low Birth Weight (ELBW): weighing <1000g or 2.3lb
SGA
■Conditions affecting fetal growth
–<28wks leading to overall growth restriction
–>28wks, intrauterine malnutrition
■IUGR for some SGA newborns (asymmetric vs symmetric)
■Contributing factors (Box 23.1)
SGA Newborns
■Head is larger than body
■Wasted appearance of extremities; lose dry skin
■Reduced subcutaneous fat stores
■Decreased amount of breast tissue
■Scaphoid abdomen (Sunken)
■Wide skull sutures
■Poor muscle tone over buttocks and cheeks
■Thin umbilical cord
■Perinatal asphyxia
■Difficulty with thermoregulation
■Hypoglycemia
■Polycythemia
■Meconium aspiration
■Hyperbilirubinemia
■Birth trauma
SGA: Nursing Management
■Weight, length and head circumference measurements
■Serial blood glucose monitoring
■Vital signs monitoring
■Early and frequent oral feeding; IV infusion of dextrose 10%
■Monitoring for signs and symptoms
■Anticipatory guidance
LGA
■Maternal diabetes mellitus or glucose intolerance
■Multiparty
■Prior history of a macrocosmic infant
■Post dated gestation
■Maternal obesity
■Male fetus
■Genetics
LGA Newborns
■Large body, plump, full face
■Proportional increase in body size
■Poor motor skills
■Difficulty regulating behavioral states
■Birth trauma
■Hypoglycemia
■Polycythemia
■Hyperbilirubinemia
LGA: Nursing Management
■Vital sign monitoring
■Blood glucose level monitoring
■Initiation of oral feedings with IV glucose, supplementation as needed
■Continued monitoring for signs and symptoms of polycythemia and hypoglycemia
■Hydration
■Phototherapy for increased bilirubin
Gestational Ages
•Preterm: born before 37 weeks
•Late preterm: 34-36.6 weeks
•Term: 37-39.9 weeks
•Post dates: 40-41.6 weeks
•Post term: past 42 weeks
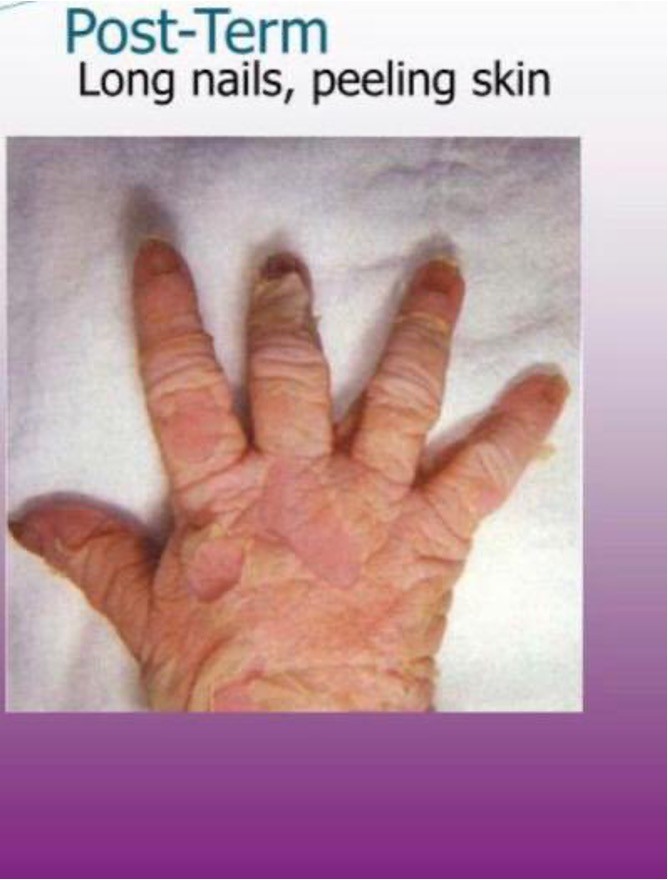
Post-term Baby
■Inability if placenta to provide adequate oxygen and nutrients to fetus after 42 weeks
■Dry, cracked, wrinkled in; possibly Meconium stained
■Long, thin extremities; long nails; creases over entire soles of feet
■Wide-eyed, alert expression
■Abundant hair on scalp
■Thin umbilical cord
■Limited vernix and lanugo
Post-term Newborn
■Perinatal asphyxia
■Hypoglycemia
■Hypothermia
■Polycythemia
Meconium aspiration
■Blood glucose level monitoring
■Initiation of feedings Iv dextrose 10%
■Prevention of heat loss
■Evaluation for polycythemia
■Parental support
Preterm Newborn
■Etiology
–Infections/inflammation
–Maternal/fetal distress
–Bleeding
–Stretching
■Body system immaturity; increased risk for complications
–Respiratory system
–Cardiovascular system
–GI system
–Renal system
–Immune system
Central nervous system
Preterm Newborn: Common Characteristics
■Weight <5.5lb
■Scrawny appearance
■Poor muscle tone
■Minimal subcutaneous fat
■Undescended testes
■Plentiful lanugo
■Poorly formed ear pinna
■Fused eyelids
■Soft spongy skull bones
■Matted scalp hair
■Absent to few screamed in soles and palms
■Minimal scrotal rugae; prominent labia and clitoris
■Thin transparent skin
■Abundant vernix
Preterm Newborn
■Hypothermia
■Hypoglycemia
■Hyperbilirubinemia
■Problems related to immaturity of body systems
■Oxygenation
■Thermal regulation
■Nutrition and fluid balance
■Infection prevention
■Stimulation
■Pain management
■Provide developmental care
■Parental support
■Discharge preparation
Dealing with Perinatal Loss
•Any pregnancy loss and/or neonatal death put to 1 month of age
•A profound experience for the family
•Avoidance is a common reaction
•Nurses must be aware of personal feelings
•Communicate empathy
Acquired Disorders
•Typically occur at, or soon after, birth
•Problems or conditions experienced by the woman during pregnancy or at birth
•Possibly no identifiable cause for the disorder
Congenital Disorders
•Present at birth; usually due to some type of malformation occurring during the ante-partal period; typically, some problem with inheritance
•Majority with a complex etiology
Acquired Conditions of the Newborn
•Hypoxic-Ischemic Encephalopathy
•Transient tachypnea
•Respiratory distress syndrome
•Meconium aspiration
•Necrotizing enterocolitis (NEC)
•Infants of diabetic mothers
•Birth trauma
•Newborns of perinatal substance abusing mothers
•Hyperbilirubinemia
•Newborn infections
Hypoxic-Ischemic Encephalopathy
•Asphyxia occurs when adequate breathing is not established after birth; insufficient oxygen delivery to meet metabolic demands
Nursing Assessment:
•Risk factors, newborn's color, work of breathing, heart rate, temperature, Apgar scores
Nursing Management:
•Immediate resuscitation, continued observation, neutral thermal environment, blood glucose levels, parental support and education
Respiratory Distress Syndrome
•Lung maturity and lack of alveolar surfactant
Nursing assessment
•Expiratory grunting, nasal flaring, chest wall retractions, see-saw respirations, generalized cyanosis; heart rate >150-180; fine inspiratory crackles, tachypnea (>60), Silverman-Anderson index score
•Chest x-ray: hypoaeration, under expansion, and ground glass pattern
RDS Nursing management
•Supportive care; close monitoring
•Respiratory modalities: ventilation (CPAP, PEEP); exogenous surfactant; oxygen therapy
•Antibiotics for positive cultures; corrections of metabolic acidosis
•Fluids and vasopressors; gavage or IV feedings
•Blood glucose level monitoring
•Clustering of care; prone or side-lying position
•Parental support and education
Necrotizing Enterocolitis (NEC)
•Three pathologic mechanisms: bowel ischemia, bacterial flora, and effect of feeding
Nursing assessment
•Signs and symptoms: abdominal distention and tenderness, bloody stools, feeding intolerance (bilious vomiting), sepsis, lethargy, apnea, shock
•KUB: air in bowel wall; dilated bowel loops
Infants of Diabetic Mothers
•High levels of maternal glucose crossing the placenta, stimulating increased fetal insulin production leading to somatic fetal growth
Nursing assessment
•Full rosy cheeks, ruddy skin color, short neck, buffalo hump, massive shoulder, distended upper abdomen, excessive subcutaneous fat tissue: hypoglycemia, birth trauma
•Hypocalcemia, hypomagnesemia, polycythemia, hyperbilirubinemia
Newborn of Substance-Abusing Mothers
Nursing management
•Comfort promotion; stimuli reduction
•Nutrition
•Prevention of complications
•Parent-newborn interaction
Birth Trauma
•Injuries due to the forces of labor and birth
•Types: fractures, brachial plexus injury, cranial nerve trauma, head trauma (cephalohematoma, caput succedaneum)
Nursing assessment
•Physical and neurological assessment: bruising, bumps, swelling, paralysis, symmetry of structure and function
Myelomeningocele
•The spinal cord often ends at the point of the defect, resulting in absent motor and sensory function beyond that point
•Nursing management: Preventing infection, promoting urinary elimination, promoting bowel elimination, promoting adequate nutrition, preventing latex allergy reactions, maintaining skin integrity, educating and supporting the family
Esophageal Atresia and Tracheoesophageal Fistula
•Lack of normal separation of esophagus and trachea during embryonic development
•Esophageal atresia: congenitally interrupted esophagus
•Tracheoesophageal fistula: abnormal communications between trachea and esophagus
•Nursing assessment
•Hydramnios
•Copious frothy bubbles of mucus and drooling; abdominal distention
•Coughing, choking and cyanosis
•Omphalocele
•Umbilical ring defect with evisceration of abdominal contents into external peritoneal sac
•Gastroschisis
•Herniation of abdominal contents through abdominal wall defect (no peritoneal sac)
Imperforate Anus
•Rectum ending in blind pouch or fistulas between the rectum and perineum
Nursing assessment
•Absence of anal opening, no passage of meconium, signs and symptoms of intestinal obstruction
Nursing management
•Preparation for surgery,
•Postoperative care
Bladder Exstrophy
•Protrusion of bladder onto abdominal wall
•Separation of rectus muscles and symphysis pubis
•Boys also with epispadias
•Initial bladder closer within 48 hours of birth; further reconstruction at age 2-3 years old
REEDA
Redness, Edema, Ecchymosis, Discharge, Approximation
Chlamydia
Azithromycin
⁃ Doxycycline ❌ 🤰🏽
Gonnorhea
Ceftraxone IM ✅🤰🏽
⁃ Ciprofloxacin
⁃ Ievofloxacin
Syphilis
Benzathaine penicillin 1dose
~less then yr
⁃ Benzathaine penicillin 3x ~ more then yr
PID
inpatient- iv antibiotics
- iv fluids
- pain meds
Out patient - cephalosporin w/ doxycycline
HPV
Tricholoroacetic Acid (TCA)
⁃ Podphyllin ❌🤰🏽
⁃ Imiquimod ❌🤰🏽
⁃ Gardadil~ before sexually active (9yrs)
Herpes
Herpes
⁃ Acyclovir
⁃ Valacyclovir (36 weeks)
⁃ Famiclovir
Bacterial Vaginosis
Flagyl- metronidazole
⁃ Cindamycin cream
Trichmoniasis
Flagyl- metronidazole
⁃ Tinidazole
Vulvovaginal Candidiasis
Miconazole
⁃ Terconazol
⁃ Clotrimazol
⁃ Nystatin vaginal cream
When don't you give methergine?
hypertension
What vaccine should not be given during pregnancy?
Rubella (live vaccine)