post partum period
Transition period for woman and new born and family physiologically and psychologically (birth of placenta to 6 weeks)
Puerperium
the time from the delivery of the placenta through approximately the first 6 weeks after the delivery
Involution of the uterus
contraction of muscle fibers; catabolism; regeneration of uterine epithelium.
Lochia
Vaginal discharge after childbirth
Ruba
Occurs right after child birth lasting 3-4 days bright red dark red with small clots similar to a period flow
Serosa
Lasts 3-10 days after child birth pinkish brown consistency with a lighter flow
Alba
Lasts 10-14 days after child birth Whitish yellow consistency little to no blood
Urinary System Adaptations
Increase Glomular filtration rate increased renal flow
Voiding sensation is affected by
1.Perennial laceration
2. Hematomas
3. decreased bladder Tone
4. Generalized swelling and bruising of perineum and tissues surrounding the meatus
What are some causes of Post Party Diuresis ?
1. Large amount of Iv fluid given during labor
2. decreased Antidiuretic effect of oxytocin
3. Build up and retention of extra fluids during pregnancy
4. Decreased production of Aldosterone
What is Postpartum diuresis ?
Excessive production of urine after child birth .
Lactation Hormones
progesterone, estrogen , prolactin
The New born sucking on breast stimulates the pituitary gland to release
prolactin / oxytocin
how is breast engorgement Relieved ?
frequent emptying warm showers cold compress between feedings
Normal Lactating breast should
Be soft and the mother should be comfortable
Engorgement
Painful swelling of breast tissue as a result of rapid increase in milk production and venous congestion causing interstitial tissue edema; impaired milk flow results in accumulation of milk in breasts; most often occurs between the third and fifth postpartum days
ovulation postpartum
interplay of hormones estrogen prolactin oxytocin
Non lactating women get menstrual cycle
7-9 weeks after birth
Breast feeding frequency and duration last
2-18 months
Factors influencing attachment
-environmental circumstances-newborn health-quality of nursing care
mood disorders
-baby blues-post-partum depression-post-partum psychosis
Risk Factors for Postpartum Infection
-Operative procedure (forceps, cesarean birth, vacuum extraction)
-History of diabetes, including gestational-onset diabetes
-Prolonged labor (more than 24 hours)
-Use of indwelling urinary catheter
-Anemia (hemoglobin <10.5 mg/dL)
-Multiple vaginal examinations during labor
-Prolonged rupture of membranes (>24 hours)
-Manual extraction of placenta
-Compromised immune system (HIV-positive)
Risk Factors for Postpartum Hemorrhage
• Precipitous labor (less than 3 hours)
• Uterine atony
• Placenta previa or abruptio placenta
• Labor induction or augmentation
• Operative procedures (vacuum extraction, forceps, cesarean birth)
• Retained placental fragments
• Prolonged third stage of labor (more than 30 minutes)
• Multiparity, more than three births closely spaced
• Uterine overdistention (large infant, twins, hydramnios)
POST PARTUM DANGER SIGNS
• Fever >100.4°F (38°C)
• Foul-smelling lochia or an unexpected change in color or amount
• Large blood clots or bleeding that saturates a peripad in an hour
• Severe headaches
• Visual changes, such as blurred vision or spots
• Calf pain with dorsiflexion of the foot
• Swelling, redness, or discharge at the episiotomy, epidural, or abdominal sites
• Dysuria, burning, or incomplete emptying of the bladder
• Shortness of breath or difficulty breathing without exertion
• Depression or extreme mood swings
baby blues
a mild postpartum mood disorder that goes away on its own lasts 4-5 days resolve 10 days
postpartum depression
a mood disorder characterized by feelings of sadness and the loss of pleasure in normal activities that can occur shortly after giving birth Lasting longer
post partum depression may lead to
poor bonding alienation from loved ones violent thoughts and actions
Carboprost
treats postpartum uterine Hemorrhage works by contracting the uterus
REVA ROBINS THREE PHASES
taking in phase taking hold phase letting go phase
Taking in phase
-Time immediately after birth when the client needs others to meet her needs and relives the birth process first 24 hrs (range 1-2 days)
-Woman is passive – prefers nurse doing care and making decisions
Taking hold phase
-Second phase characterized by dependent and independent maternal behavior (lasts 10 days to several weeks)
-strong interest in caring for baby
-insecurity if ability to care for baby
Letting go phase
-reestablishes relationships with other people
-accepts role of motherhood not fantasy
Four stages of becoming a mother
Commitment, attachment to unborn baby, preparation for delivery and motherhood during pregnancyAcquaintance/attachment to infant, learning to care for infant, and physical restoration 2 to 6 weeks postbirthMoving toward a new normalAchievement of a maternal identity through redefining self to incorporate motherhood (around 4 months)
3 Stages of Role Development
ExpectationsRealityTransition to mastery
Engrossment: Partner Psychological Adaptation
strong attachment to baby increased self esteem visual awareness perception that the new born is perfect
Risk Factors for Postpartum Infection
Operative procedure (forceps, cesarean birth, vacuum extraction)
• History of diabetes, including gestational-onset diabetes
• Prolonged labor (more than 24 hours)
• Use of indwelling urinary catheter
• Anemia (hemoglobin <10.5 mg/dL)
• Multiple vaginal examinations during labor
• Prolonged rupture of membranes (>24 hours)
• Manual extraction of placenta
• Compromised immune system (HIV-positive)
Risk Factors for Postpartum Hemorrhage
• Precipitous labor (less than 3 hours)
• Uterine atony
• Placenta previa or abruptio placenta
• Labor induction or augmentation
• Operative procedures (vacuum extraction, forceps, cesarean birth)
• Retained placental fragments
• Prolonged third stage of labor (more than 30 minutes)
• Multiparity, more than three births closely spaced
• Uterine overdistention (large infant, twins, hydramnios)
POST PARTUM DANGER SIGNS
• Fever >100.4°F (38°C)
• Foul-smelling lochia or an unexpected change in color or amount
• Large blood clots or bleeding that saturates a peripad in an hour
• Severe headaches
• Visual changes, such as blurred vision or spots
• Calf pain with dorsiflexion of the foot
• Swelling, redness, or discharge at the episiotomy, epidural, or abdominal sites
• Dysuria, burning, or incomplete emptying of the bladder
• Shortness of breath or difficulty breathing without exertion
• Depression or extreme mood swings
BUBBLE – EE
Breast
Uterus
Bladder
Bowel
Lochia
Episiotomy/Perineum/
Epidural
Extremities
Emotional Status
POSTPARTUM ASSESSMENT
-During the first hour: every 15 minutes
-During the second hour: every 30 minutes
-During the first 24 hours: every 4 hours
-After 24 hours: every 8 hours
INVOLUTION
Uterus should be midline and firm
If boggy or off to side –
1)massage till firm,
2)express any clots
3)empty bladder
Encourage breastfeeding
NURSING INTERVENTIONS (involution)
Labor and Pregnancy History
Bladder status
Anesthesia
Involution is enhanced by:
Uncomplicated labor and birth
Complete expulsion of placenta or membranes,
Breastfeeding
Early ambulation
LOCHIA
-Uterus rids itself of debris remaining after birth through discharge called lochia
-Each day the amount of lochia should be less and lighter in color
-Women who have had a c/section have less lochia
-Continues for approximately 4-8 weeks post birth
Lochia changes:
Bright red at birth
Rubra – dark red
Serosa – pink
Alba – white
Clear
If blood collects and forms clots within uterus, fundus arises and becomes boggy (uterine atony)
LOCHIA SHOULD NOT
¡Have a foul odor
¡Have large clots
¡Saturate a pad in less than ½ hour
AFTERPAINS
-Contractions that occur after birth
-May be increased in pregnancies where uterus was -overdistended
-More increased in multiparas
-Afterpains are usually stronger during breastfeeding
-Pain should be assessed with other vital signs
-Provide comfort measures
-Consider premedicating
-Check for other reasons for pain
CERVIX AND VAGINA
-Cervix returns to prepregnant state by 6 weeks post partum
-Internal os closes by 2 weeks postpartum
-External os has permanent changed appearance
PERINEUM
Ask to woman to turn to side with her back towards you
Gently lift the upper buttock and inspect the perineum
Look for :
Ecchymosis
Hematoma
Erythema
Edema
Intactness of skin edges or sutures
Drainage
Bleeding
Odor
using sitz bath
-Close clamp on tubing before filling bag with water
-Fill sitz bath basin and plastic bag with room-temperature water
-Place the filled basin on the toilet with the seat raised and the overflow opening facing toward the back of the toilet.
-Hang the filled plastic bag on a hook close to the toilet or an IV pole.
-Attach the tubing to the opening on the basin.
-Sit on the basin positioned on the toilet seat and release the clamp to allow warm water to irrigate the perineum.
-Remain sitting on the basin for approximately 15 to 20 minutes.
-Stand up and pat the perineum area dry. Apply a clean peripad.
-Tip the basin to remove any remaining water and flush the toilet.
-Wash the basin with warm water and soap, and dry it in the sink.
-Store basin and tubing in a clean, dry area until the next use.
-Wash hands with soap and water
Epiostomy care
-Kegel exercises. These exercises strengthen the muscles in the pelvic area. To do Kegel exercises, squeeze the muscles that you use to stop yourself from passing urine (peeing). Hold the muscles tight for 10 seconds and then release. Try to do this at least 10 times in a row, three times a day.
-Put a cold pack on your perineum. Use ice wrapped in a towel.
-Sit on a pillow or a donut-shaped cushion.
-Soak in a warm bath.
BLOOD VALUES
-Decreased blood volume and cardiac output
-B/P returns to pre- pregnancy by 6 weeks pp
-White blood cell count often elevated after birth for first 4 to 6 days
Activation of clotting factors predispose to thrombus formation – hemostatic system reaches nonpregnant state in 2to 3 weeks postpartum
-Risk of thromboembolism lasts 6 weeks
EXTREMITIES
Pregnancy is a hypercoagulable state
-Increased risk of venous thromboembolism ( VTE)
-Pulmonary Embolism ( PE)
-Deep Vein Thrombosis ( DVT
Factors that Increase Risk of Clot Formation
1.Stasis
2.Altered Coagulation
3.Localized Vascular damage
EXTREMITIES risk factors
•Anemia
•Diabetes mellitus
•Cigarette smoking
•Obesity
•Preeclampsia
•Hypertension
•Severe varicose veins
•Pregnancy
•Multiple pregnancies
•Cardiovascular disease
•Sickle cell disease
•Postpartum hemorrhage
•Oral contraceptive use
•Cesarean birth
•Severe infection
•Previous thromboembolic disease
•Multiparity
•Bed rest or immobility for 4 days or more
•Maternal age older than 35
URINARY ISSUES
-Difficulty feeling sensation to void
-Perineal lacerations
-Swelling and bruising
-Hematomas
-Decreased bladder tone
-Urinary system usually returns to normal by 6 weeks postpartum
BLADDER
-Patient may void up to 3,000 ml a day from 12 hours after birth for several days
-Single void may be 500 ml or more
-Important to check for full bladder
-Monitor for s/s of UTI
-Assess for bowel sound, flatus, undistended abdomen
GASTROINTESTINAL SYSTEM
•May have decreased bowel tones for several days
•Decreased peristalsis
•Constipation
•Fear of having a bowel movement
•May not have spontaneous BM for 1-3 days after birth
•Assess for bowel sound, flatus, undistended abdomen
Vital Signs
•TEMPERATURE
• May be elevated to 100.4 because of dehydration or epidural first 24 hours
• Should return to normal after 24 hours
•PULSE
• 60-80 bpm after birth normal 1st week
•RESPIRATIONS
• WNL – 12- 20
•B/P
• Should be in patient’s normal range
MUSCULOSKELETAL SYSTEM
-Joints return to normal by 6 to 8 weeks postpartum
-Diastasis recti responds to exercise
INTEGUMENTARY SYSTEM
•Linea nigra, melasma, areola darkening fade
•Hair loss
•Striae gravidarum fade to silver
•Diaphoresis
RESPIRATORY SYSTEM
•Diaphragm returns to normal position
•Abdominal organs resume their nonpregnant position
•Returns to normal prepregnant state 1 to 3 weeks
ENDOCRINE
•Estrogen and Progesterone changes with delivery of placenta
•Non Breastfeeding Estrogen increases 2 weeks postpartum
•Prolactin levels decline within 2 weeks for the woman who is not breastfeeding, but remain elevated for the lactating woman
BREAST EXAM
•Checks breasts for symmetry
•Engorgement
•Erythema
•Check Nipples
•Filling, Full, Engorged
•Colostrum, Foremilk
LACTATION
•Lactation is the secretion of milk by the breasts. It is thought to be brought about by the interaction of progesterone, estrogen, prolactin, and oxytocin.
•Breast milk typically appears within 4 to 5 days after childbirth.
•First 2 days postpartum breast soft non tender
TEACHING FOR BREASTFEEDING
•Select a quiet corner or room where you won’t be disturbed.
•Use a rocking chair to soothe both you and your infant.
•Take long, slow deep breaths to relax before nursing.
•Drink water while breastfeeding to replenish body fluids.
•Listen to soothing music while breastfeeding.
•Cuddle and caress the infant while feeding.
•Set out extra cloth diapers within reach to use as burping cloths.
•Allow sufficient time to enjoy each other in an unhurried atmosphere.
•Involve other family members in all aspects of the infant’s care from the start.
•Contact a local La Leche League or a nursing mothers’ group for continued guidance and support
BREASTFEEDING POSITIONS
•Cradle hold position: The mother’s arm cradles the baby close to the breast with their abdomens against each other and supports the baby’s head and neck with the mother’s other hand supporting the breast.
•Cross- cradle hold position: Similar to the cradle hold, but the baby is supported with the mother’s opposite arm
•Football/clutch hold position: (cesarean, large breast, small/premature, or mum with twins) Potion baby at your side in a semi sitting position facing mom with baby’s legs under mum’s arm. Use pillow to bring the baby up to the level of your nipple.
•Side lying position: (middle of night) Position baby on your side facing you, tummy to tummy. mouth in line with nipple.
BREASTMILK SAFETY
1.Wash your hands before expressing milk or handling breast milk.
2.Find a quiet, clean place to express milk if returned to workplace. Use clean containers to store expressed milk. Use sealed and chilled milk within 24 hours.
3.Discard any milk that has been refrigerated for more than 24 hours.
4.Use any frozen expressed milk within 3 months.
5.Do not use microwave ovens to warm chilled milk.
6.Discard any used milk; never refreeze it.
TYPES OF FORMULAS
•Cow milk protein based formulas: This formula contains cows milk that has been altered to resemble to breast milk. The formula has a lot of nutrients within it that is easier for babies to digest. The only downfall however is some babies are allergic to protein in now milk so that would require a different type of formula such as protein or soy milk etc.
•Soy Based Formulas: This formula contains protein found in soybeans. This is especially great for babies who wish to exclude animal proteins in his/her diet. It is a great option for babies who intolerant and/or allergic to cow milk formula and lactose which is a natural carbohydrate found in cow milk.
•Protein Hydrolysate Formulas: This formula contains protein that has been broken down (hydrolyzed) into tiny sizes than are those in cow milk and soybean formula. Protein hydrolysate formula are meant for babies who have a protein allergy.
ENGORGEMENT
•Heat or Cold
•Cabbage Leaf Compress
•Breast Massage
•Hand expression of milk
•Anti-inflammatory medication
NON BREASTFEEDING
•Wear a supportive snug bra 24 hours daily
•May take 5-7 for milk to be suppressed
•Take mild analgesics
•Don’t stimulate breasts
•Drink fluids
•Reduce salt intake
•Ice packs inside bra - change q 30
MASTITIS
•Infection or inflammation
•Lactating or engorged breasts
•Management
• Heat
• Rest
• Empty Breast
Antibiotics as needed
OVULATION AND RETURN OF MENSTRUATION
•Nonlactating women, menstruation may resume as early as 7 to 9 weeks after giving birth, but the majority take up to 3 months
•Lactating women, menstruation return depends on frequency of breastfeeding and length of time
•Ovulation can return before menstruation
SEXUAL ACTIVITY
•Sleep deprivation, vaginal dryness, and lack of time together may impact resumption of sexual activity
•Usually sexual intercourse is resumed once episiotomy has healed and bright red lochia has stopped (about 3 to 6 weeks)
•Breastfeeding mother may have leakage of milk from nipples with sexual arousal
•Contraceptive choices
• Barrier with spermicide
• Combined Oral Contraceptives should not be used until 6 weeks pp and until lactation is established
Factors associated with the health care facility or birthing unit can also hinder attachment
These include:
•Separation of infant and parents immediately after birth and for long periods during the day.
•Policies that discourage unwrapping and exploring the infant.
•Intensive care environment, restrictive visiting policies.
•Staff indifference or lack of support for parent’s caretaking attempts and abilities.
PP exercise
•Abdominal Breathing
•Head Lift
•Modified Sit-Ups
•Double Knee Roll
•Pelvic Tilt
RH IMMUNE GLOBULIN
•For prevention of Rh Isoimmunization
•If mother is Rh negative she receives an IM injection of Rhogam at 28 weeks gestation
• and
•If mother is Rh negative and has a spontaneous birth, abortion ( Spontaneous or Operative, Bleeding in Preganancy, Ectopic, Trauma, External Version, Amniocentisis, Chorionic Villus Sampling , Placenta Previa or Abruption she receives an IM injection of Rhogam within 72 hours of event to prevent sensitization of the mother
•The standard dose of RhoGAM is 300 mcg given intramuscularly,
RH ISOIMMUNIZATION
•If Rh sensitization occurs fetus can develop Hydrops
• Fetalis
• Fetal Edema
• CHF
• Jaundice ( icterus gravis)
• Neurological Damage ( Kernicterus)
Erthroblastosis Fetalsis ( severe hemolytic syndrome)
ENCOURAGE REST
•Nap when the infant is sleeping
•Reduce participation in outside activities, and limit the number of visitors
•Determine the infant’s sleep–wake cycles and attempt to increase wakeful periods during the day so the baby sleeps for longer periods at night.
•Eat a balanced diet to promote healing and to increase energy levels.
•Share household tasks to conserve energy.
•Ask the partner or other family members to provide infant care during the night periodically so that mothers can get an uninterrupted night of sleep if they are not breastfeeding.
•Review the family’s daily routine, and try to “cluster” activities to conserve energy and promote res
Newborn vital signs
Respiration: 30-60 (avg 40)
Temp-Rectal: 90-99.5
Axillary: 97.6-98.6
HR: 110-160
BP-Systolic: 60-80
Diastolic: 40-50
Respiratory adaptions to birth
◦Initiation of respirations: adjusting from a fluid filled intrauterine environment to gaseous extrauterine environment
◦Role of surfactant: surface tension redacting lipoprotein that prevents alveolar collapse
◦Respirations: 30-60 breaths per minute; irregular, shallow, unlabored; short periods of apnea (<15 secs); symmetrical chest movements
Cardiovascular changes (fetal to neonate)
1.Increased aortic pressure and decreased venous pressure
2.Increased systemic pressure and decreased pulmonary artery pressure
3.Closure of foramen ovale
4.Closure of the ductus arteriousus
5.Closure of ductus venous
Characteristics of Cardiac Function
◦Blood Pressure:
◦varies with birth weight, gestational age, & changes in blood volume
◦average mean is 5 to 55 mm Hg, full term 3 kg newborn. (70/45 to 50/30 mm Hg)
◦Crying may elevate both systolic & diastolic blood pressure
◦Heart Murmurs: 90% of murmurs are transient, not abnormalities
◦Caused by turbulent blood flow through: narrow opening, across an abnormal valve, stenosed valve
◦Atrial or ventricle septal defect (ASD or VSD)
◦Some serious murmurs not recognized for a few weeks until patent ductus arteriosus closes
Renal system changes
◦Limited ability to concentrate urine until about 3 months of age (urine has a low specific gravity)
◦6-8 voids a day is normal
◦Low glomerular filtration rate and limited excretion and conservation capability: affect newborn’s ability to excrete salt, water loads, and drugs
G I changes
◦Intestines sterile at birth
◦Capacity of newborn stomach varies
◦Newborns prone to regurgitation, vomiting, reflux
◦Meconium formed during fetal life
◦Term newborns pass meconium first 24-48 hours after birth
◦Thick , tarry black or dark green
Immune System changes
◦Activates after birth
◦Immature – so s/s of infection may be subtle
◦Fever is not reliable indication of infection
◦Hypothermia or irregular temperature status more reliable sign of infection!!!
◦Infants active passive acquired immunity in utero from mothers response to illness or immunization
Hepatic changes
◦At birth infant as iron stores for 4-6 months
◦At birth infants is cut off from maternal glucose
Newborn stools
◦Meconium, then transitional stool, then milk stool
◦Breast-fed newborns: yellow-gold, loose, stringy to pasty, sour smelling
◦Formula-fed newborns: yellow, yellow-green, loose, pasty, or formed, unpleasant order
Neutral Thermal Environment-Newborn
◦Infant stressed by change from warm, moist environment of uterus to dry, drafty environment of delivery room and nursery
◦Neutral thermal environment needed to prevent need for increased oxygen and calories
Heat loss for newborns
◦Thin skin; with the blood vessels close to the surface
◦Lack of shivering ability; limited reserve of metabolic substrates (glucose, glycogen, fat)
◦Limited use of voluntary muscle activity
◦Large body surface area relative to body weight
◦Lack of subcutaneous fat; little ability to conserve heat by changing position
THERMOREGULATION
◦Dry immediately with warmed blankets beginning with the head
◦ Skin to skin contact with mother or partner
◦Radiant warmer
◦Stocking cap
◦ Heat regulation is second most critical to the newborn’s survival
◦Hypothermia is a common and dangerous problem
Mechanisms of heat exchange
◦Conduction: transfer of heat from object to object when the two objects are in direct contact with each other
◦Convection: flow of heat from body surface to cooler surrounding air or air circulating over a body surface/ also from drafts
◦Evaporation(most common): loss of heat when liquid is converted to a vapor
◦Radiation: loss of body heat to cooler solid surfaces in proximity but not in direct contact (cold weight)
Consequences of Cold Stress
◦Increased Metabolic Use of Calories
• Failure to gain weight or weight loss
◦Increased Oxygen Consumption
• May lead to hypoxia, acidosis and respiratory distress
◦Rapid Depletion of Glycogen
• Resulting in hypoglycemia
If allowed to continue the baby may develop shock and disseminated intravascular coagulation (DIC) leading ultimately to death.
Behavioral patterns of newborns
First period of reactivity
•Birth to 30 minutes to 2hours after birth
•Newborn is alert, moving, may appear hungry
Period of decreased responsiveness
•30-120mins old
•Period of sleep or decreased activity
Second period of reactivity
•2-8hrs old
•Newborn awakens and shows an interest in stimuli
PRIORITIES OF CARE OF THE NEWBORN
•Establish and maintain an airway and respirations
•Provide warmth and prevent hypothermia
•Provide a safe environment and routine preventive measures
•Promote maternal-infant attachment
Initial newborn assessment
•Apgar scores
•Length/ Weight
•Vital signs
•Physical maturity
Neuromuscular maturity
Signs indicating a problem during Assessment
•Signs indicating a problem
•Nasal flaring, chest retractions
•Grunting on exhalation, labored breathing
•Generalized cyanosis, flaccid body posture
•Abnormal breath sounds, abnormal respiratory rates
•Abnormal heart rates, abnormal newborn size
Newborn Classification Neonatal Mortality Risk Chart
•Preterm: <36.6 (completed) weeks
•Late preterm: 34–36.6 weeks (common respiratory problems)
•Term: 38–41 (completed) weeks
•Postterm: >42 weeks
•Large-for-gestational-age (LGA) (larger than expected)
•Appropriate-for-gestational-age (AGA)
•Small-for-gestational-age (SGA)
Apgar scoring system
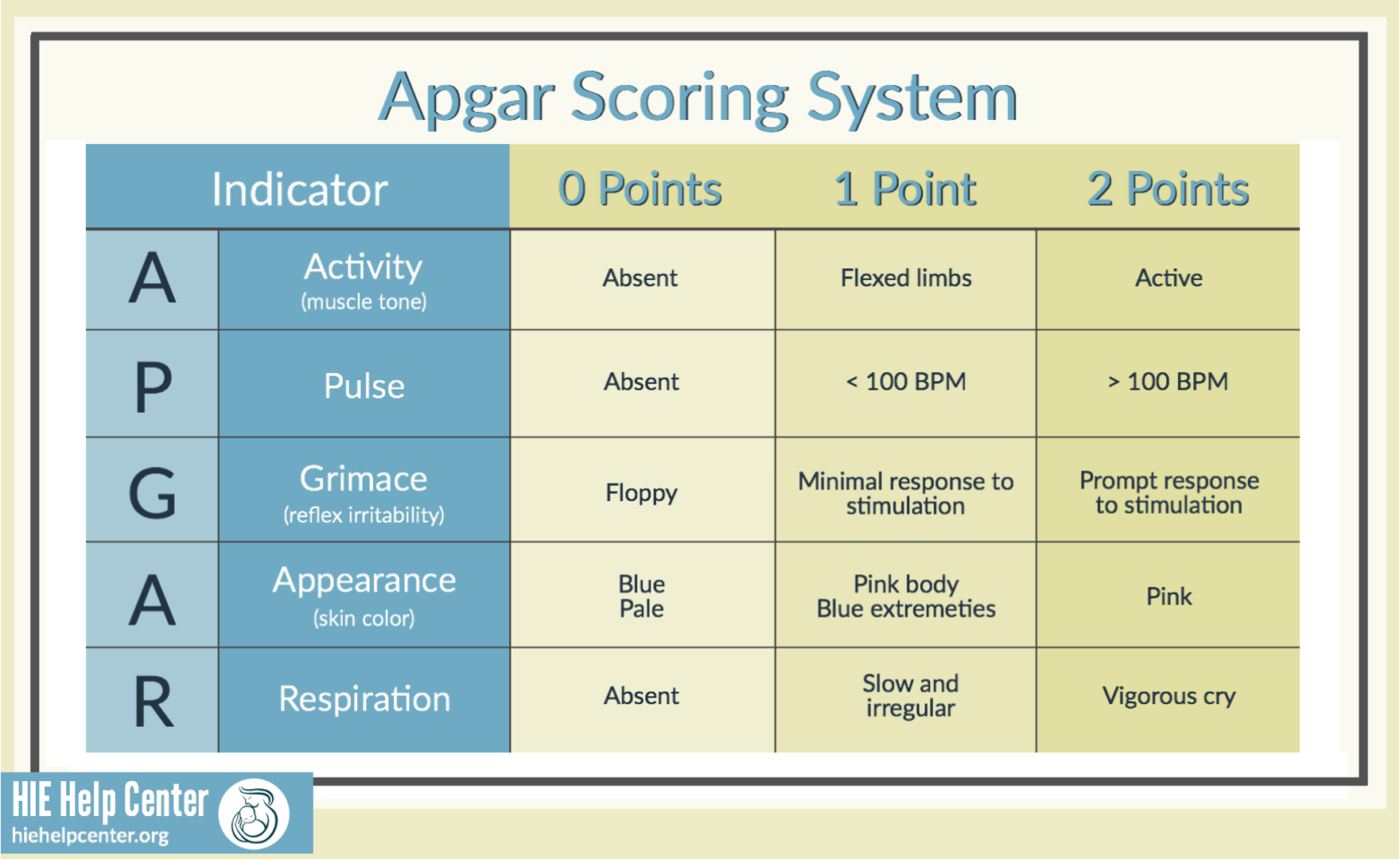
Activity
Pulse
Grimace
Appearance
Respiration
(do 1st and 5th minute of life)
8-10 = an uncompromised or distress free
4-7 = moderately compromised or asphyxiated
0-3 = severely compromised or asphyxiated
Less than 7- do it again in 10 minutes
Nurse’s Responsibility (newborn)
•Initiate Neonatal Resuscitation if necessary
•Assign Apgar score ( if pediatrician not present)
•ID bracelets for baby & mother
•Footprints of baby & mother’s finger print
•Vital signs of baby (30 minutes X4)
•Assist with skin/skin & breastfeeding
•Administer Vitamin K (IM)
•Apply antibiotic eye ointment (or drops)
•Physical assessment of newborn (abbreviated version)
–Size & contours of head, including fontanels, relationship to body
–Assess breathing for flaring of nares, grunting or retractions of chest
–Posture & tone of body
–Symmetry of face, including eyes, ears, nose,
–Arms & legs equal in length, digits on hands & feet.
–Any visual abnormalities
–Obtain height & weight of newborn
Normal Newborn Appearance
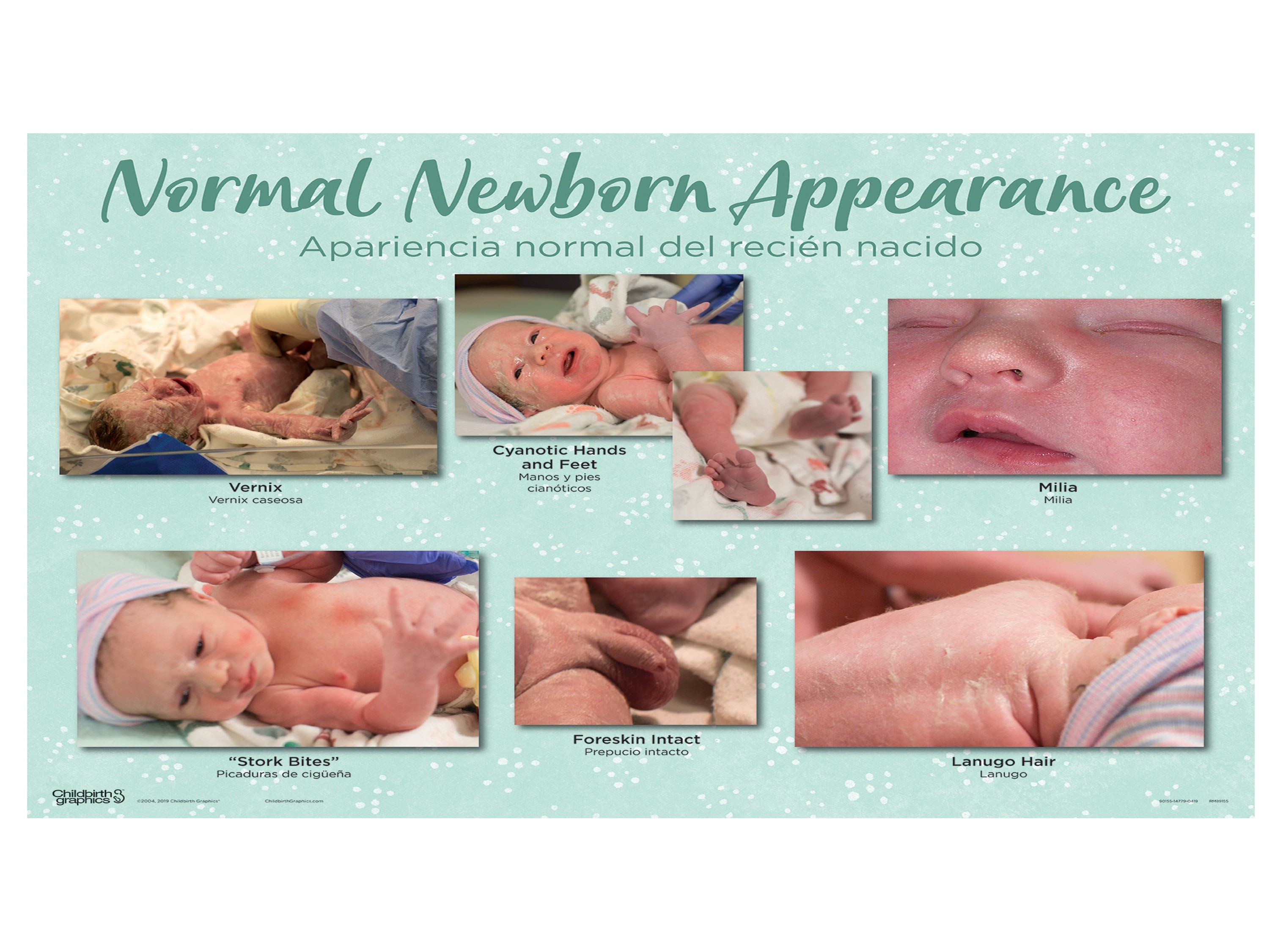
Vernix- protection when baby in utero (not every baby)
Cyanotic hand and feet
Milia- little sebaceous glands
Stork Bites
Foreskin intact
Lanugo hair
Mongolian spots
Erythema toxicum
Harlequin sign
Nevus flammeus
Nevus vasculosus
what do Mongolian spits look like?
Brown spots
What does Erythema toxicum look like?
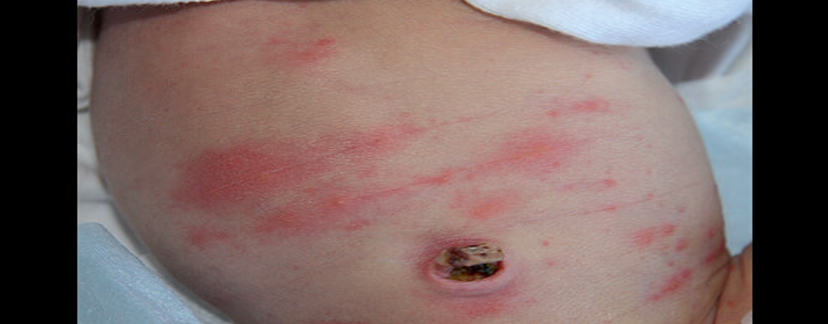
Benign
Its the skins way reacting to new environment
Variations in head size and shape newborn
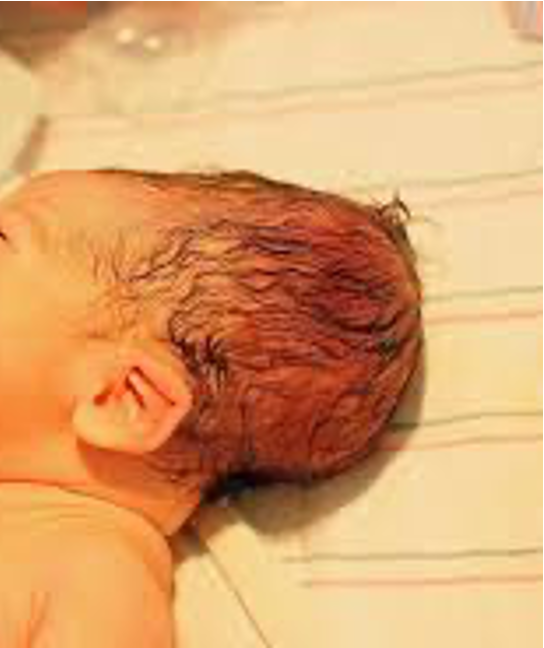
Variations
•Molding
•Caput succedaneum
•Cephalohematoma
Abnormalities
•Microcephaly
•Macrocephaly
•Large, small or closed fontanelles
Fontanelles
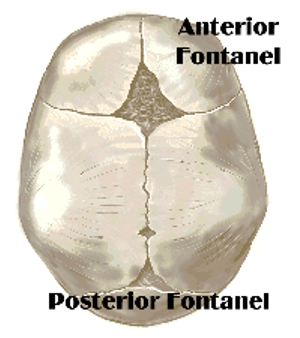
Anterior –
Diamond shaped
Closes at 12-18 months of age
Posterior
Triangular – may be difficult
To palpate in the newborn
Closed by the end of the 2nd month
What is caput Succedaneum?
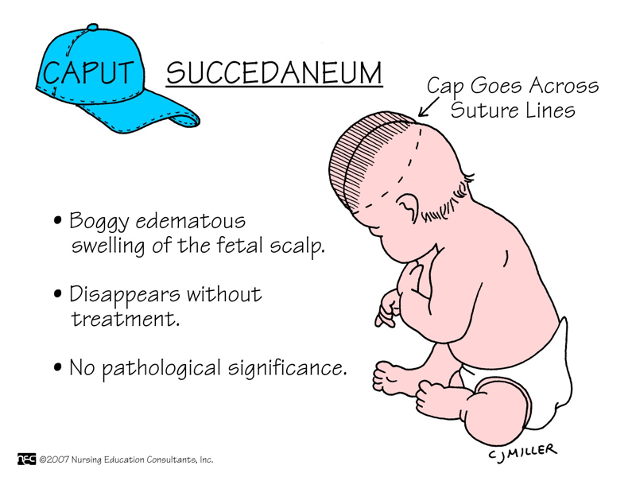
Boggy edematous swelling of fetal scalp(disappears w/o treatment)
No pathological treatment
soft-pits
Crosses the suture line (fluid/edema)
What is cephalohematoma?
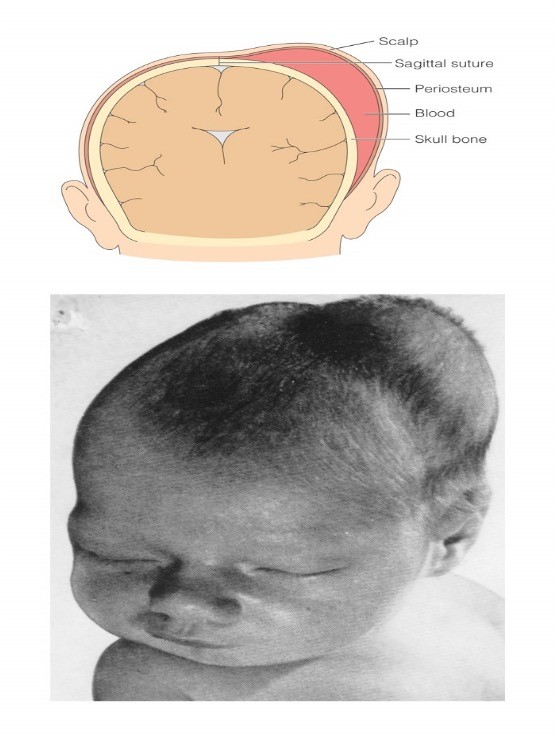
No treatment required
disappears within 6-8 weeks-months
soft-elastic
On one side of the suture line (positive blood)
Newborn reflexes

•Sucking: (non-nutritive sucking on lips)
•Rooting: baby turns head to side of mouth or cheek that is touched, may open mouth (4 months)
•Palmer Grasping
•Moro: lifting arms up & letting go: arms up fingers, spread out, (6 months)
•Startle
•Tonic neck: fencer position, head is turned to one side, extremities straighten on that side & flex on the opposite side (3 months)
•Babinski: gently stroke sole of foot, fanning out and extension of toes
•Stepping reflex: puts one step down in front of other, (4-8 weeks)
•Blink, Gag & Sneeze are protective reflexes
•
Common concerns
•Transient tachypnea of the newborn
(Baby breathing fast/ will go away but will still need to monitor
Starts 4-6 hrs after birth)
•Physiologic jaundice (hyperbilirubinemia)
•Hypoglycemia
TRANSIENT TACHYPNEA OF THE NEWBORN
•Usually results from excess fluid in lungs
•Infant breathes normally at birth but develops symptoms of respiratory distress by 4 to 6 hours of age
•Clinically can resemble RDS
•May be seen cesarean-birth newborns
•Usually resolves over 24 – 72 hours
Nursing interventions for transient tachypnea
•Providing oxygen
•Ensuring warmth
•Observing respiratory status frequently
•Allowing time for pulmonary capillaries and the lymphatics to remove the remaining fluid
Meconium Aspiration Syndrome
•A cause of respiratory failure in term and post-term infants
•Intrauterine distress can cause passage of meconium into the amniotic fluid before birth
•Factors that promote the passage in utero include placental insufficiency, maternal hypertension, preeclampsia, fetal hypoxia, transient umbilical compression, oligohydramnios, and maternal drug abuse, especially of tobacco and cocaine
• Occurs when the newborn inhales particulate meconium mixed with amniotic fluid into the lungs while still in utero or on taking the first breath after birth
•Severe MAS can lead to persistent pulmonary hypertension and death
What Causes Newborn Jaundice
UNCONJUGATED BILIRUBIN
Indirect bilirubin is fat soluble and
not easily excreted by the GI Tract or
kidneys – accumulated in
blood and is deposited in the skin,
sclera and mucus membranes
CONJUGATED BILIRUBIN
Direct bilirubin – easily excreted
Maternal Risk Factors for Neonatal Jaundice
•Blood type ABO or Rh incompatibility – Mother’s blood type is O and fetal is A,B or AB – The infant is not born anemic, hemolysis of the blood begins with birth when blood and antibodies are exchanged as the placenta separates – red blood cells are destroyed
•Breastfeeding
•Drugs : Diazepam, Oxytocin
•Ethnicity: Asian, Native American
Maternal illness : Gestational Diabetes
Nursing interventions for physiologic jaundice
•Begins after 24hours of age
•Frequent breast or formula feeding
•Phototherapy
•Monitor hydration status, stools, skin color
Pathological jaundice (before 24hrs/ SERIOUS)
Nursing Interventions to Decrease Incidence of Hyperbilirubenemia
•
•Maintain newborn skin temperature at 97.8 degrees
•Monitor stool for frequency and characteristics
•Encourage early feedings
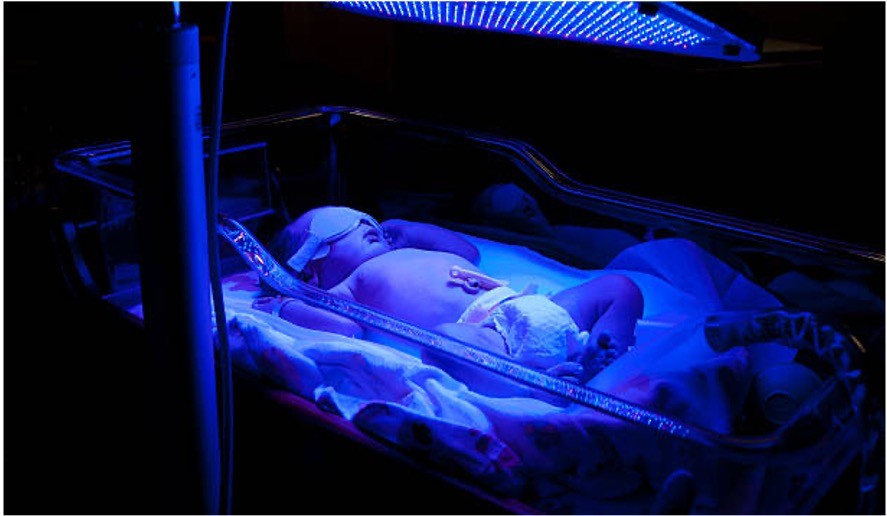
Care for newborn receiving phototherapy:
•Monitor body temp
•Document stools
•Document wet diapers
•Turn frequently
•Observe skin integrity
•Provide eye protection
•Encourage parents to participate
REDUCING BILIRUBIN LEVELSPhototherapy
• Place the newborn under the lights or on the fiberoptic blanket
•Expose as much skin as possible
•Cover the newborn’s genitals and shield the eyes
• Turn the newborn every 2 hours
•Remove the newborn from the lights only for feedings.
•Maintain a neutral thermal environment
•Assess the newborn’s temperature every 3 to 4 hours as indicated.
•Monitor fluid intake and output
•Monitor stool for consistency and frequency. Unconjugated bilirubin excreted in the feces will produce a greenish appearance, and typically stools are loose
•Monitor serum bilirubin levels
Long-Term Complications for the Infant with Fetal Alcohol Syndrome
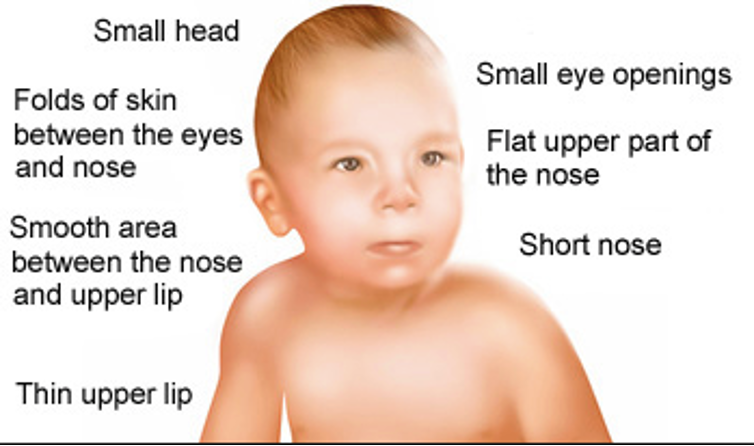
–Delay in oral feeding development
–Central nervous system (CNS) dysfunctions most common
–Impulsivity, cognitive impairment, speech and language abnormalities
–Learning disabilities indicative of CNS involvement
Nursing interventions for Hypoglycemia
•Plasma glucose concentration less than 45mg/dL in the first 72hrs of life
•Rapid acting glucose source
•Dextrose gel
•Breastfeeding
•Formula feeding
•Monitor for symptoms
(When baby in utero and getting glucose from mother, baby makes insulin)
Selected screening for newborns
•Phenylketonuria (PKU)
•Congenital hypothyroidism
•Galactosemia
•Sickle cell anemia
•Hearing (universal screening)
NEWBORN SCREENING
•Should be done in first 24-48 hours of life but NOT before 24 hours –
•Should be done after infant has been breast/formula fed
•Puncture of newborn’s warmed heal
•Blood is collected on filter paper completely filing the circles
Cord care
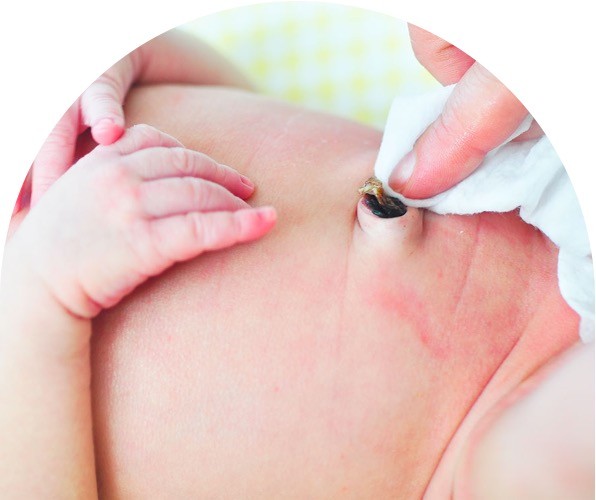
•Remove clamp after 24hrs, will get blk by 2nd/3rd day
•By day 7-10 it will fall off
•Fold diaper below it
•Never pull on it
•No bath until it falls off and heal
What is a Circumcision? What are the side effects?
a surgical procedure in which the prepuce, an epithelial layer, covering tip of penis is removed
–Permit exposure of glands for easier cleaning
–Not performed on premature or compromised infant
–Local and oral pain relief medications are used
•Side effects:
–Infection
–Hemorrhage
–Pain, restlessness
–Difficulty in voiding
–Damage to urethra, stenosis may develop.
CIRCUMCISION musts
•Infant should be at least 12 hours old or older
•Infant has received standard vitamin K prophylaxis
•Infant has voided normally at least once since birth
•Infant has not eaten for at least an hour prior to the procedure
•Written parental consent has been obtained
•Correct identification of the infant brought to the procedure room
Care OF THE CIRCUMCISION
•Assess for bleeding every 30 minutes for at least 2 hours.
•Document the first voiding to evaluate for urinary obstruction or edema.
•Squeeze soapy water over the area daily and then rinse with warm water. Pat dry.
•Apply a small amount of petroleum jelly with every diaper change if the Plastibell was used; clean with mild soap and water if other techniques were used.
•Fasten the diaper loosely over the penis and avoiding placing the newborn on his abdomen to prevent friction.
•Do not remove yellow exudate from penis
newborn period: breastfeeding
Concerns
sore nipples
Engorgement
Mastitis
L: how well infant latches onto the breast
A: amount of audible swallowing
T: nipple type
C: level of comfort
H: Amount of help mother needs
Miscarriage Signs and symptoms
Vaginal bleeding
uterine cramping
Backache
Decreasing HCG levels
Threatened Abortion
Spotting, cramping, closed cervix, bleeding unto 24-48hrs, may resolve or pregnancy loss
Treatment: Conservative supportive treatment
Possible reduction in activity in conjunction with nutritious diet and adequate hydration
Inevitable abortion
Moderate to severe bleeding cramping, abdominal pain(contractions), cervical dilatation, if rupture of membranes may need DC or DE
Treatment: Vacuum curettage if products of conception are not passed to reduce risk of excessive bleeding and infection
Prostaglandin analogs such as misoprostol to empty uterus of retained tissue (only used if fragments are not completely passed)
Incomplete abortion (passage of some of the products of conception)
Intense abdominal cramping
Heavy vaginal bleeding
Cervical dilation
Treatment: Client stabilization
Evacuation of uterus via D&C or prostaglandin analog
Complete abortion (passage of all products of conception)
History of vaginal bleeding and abdominal pain
Passage of tissue with subsequent decrease in pain and significant decrease in vaginal bleeding
Treatment: No medical or surgical intervention necessary
Follow-up appointment to discuss family planning
Missed abortion (nonviable embryo retained in utero for at least 6 weeks)
Absent uterine contractions
Irregular spotting
Possible progression to inevitable abortion
Treatment: Evacuation of uterus (if inevitable abortion does not occur): suction curettage during first trimester, dilation and evacuation during second trimester
Induction of labor with intravaginal PGE2 suppository to empty uterus without surgical intervention
Recurrent abortion
History of three or more consecutive spontaneous abortions
Not carrying the pregnancy to viability or term
Treatment:Evacuation of uterus (if inevitable abortion does not occur): suction curettage during first trimester, dilation and evacuation during second trimester
Induction of labor with intravaginal PGE2 suppository to empty uterus without surgical intervention
Identification and treatment of underlying cause (possible causes such as genetic or chromosomal abnormalities, reproductive tract abnormalities, chronic diseases or immunologic problems)
Cervical cerclage in second trimester if incom
Management for types of abortion
•Ultrasound
•Lab work: pregnancy test, H&H, CBC, T/X
•Bed rest
•Abstinence from sex
•IV / Transfusion
•D & C - Dilation and curettage
•If beyond 12 weeks: induction of labor by oxytocin and Prostaglandins may be used.
•Emotional support and bereavement care
•RhoGAM if Rh negative
Ectopic pregnancy signs and symptoms
•Progressive Abdominal pain
•Delayed menses
•Abnormal vaginal bleeding
•If rupture has occurred may experience referred shoulder pain
diagnose: ultrasound, low hcg, progesterone
Risk factors for Ectopic pregnancy
•Tubal surgery
•Sexually transmitted infections
PID
•Previous ectopic pregnancy
•IUD use
•Progestin-only contraceptive
•Pharmacologic treatment of infertility
•Endometriosis
•Assisted reproductive technologies
Ectopic pregnancy treatment
•Methotrexate ( folic acid antagonist) Dissolves Pregnancy Given IM
•Must be unruptured, less than 3.5-4cm size or less and unruptured
•HcG level lower than 5,000ml/U/m.
•Woman must be in stable condition, no blood , kidney or liver disease
•Woman monitored outpatient
•If does not fit criteria
•Surgery-salpingostomy to preserve tube or removal of tube salpingotomy
Hydatidiform mole (molar pregnancy)

Type of gestational trophoblastic disease
Benign proliferative growth of the placental trophoblast in which the chorionic villi develop into edematous, cystic, avascular transparent vesicles that hang in a grapelike cluster
Types
Complete: no embryonic or fetal parts
Partial: often have embryonic or fetal parts and an amniotic sac
Hydatidiform mole (molar pregnancy) Treatment
Suction evacuation and curettage of uterus
Early evacuation decreases complications
Uterine stimulation avoided
Careful follow-up for
Complications:
Anemia
Hyperthyroidism
Infection
DIC
Ovarian cysts
Trophoblastic embolization of the lung (CPR emergency)
Cervical Insufficiency
-Premature dilatation of the cervix which leads to 2nd trimester loss around 20 weeks
-Painless dilatation
-Can be diagnosed with transvaginal ultrasounds and speculum examinations
Incompetent Cervix
•Premature dilatation of the cervix
•Associated with repeated second trimester spontaneous abortions
•Painless, bloodless 2nd trimester abortion
•Minimal uterine contractions until late
•Considered an anomaly (uterine/cervical)
•Intrauterine pressure increases
•Internal cervical os dilates and membranes may protrude and rupture
•Spontaneous effacement and dilatation may occur
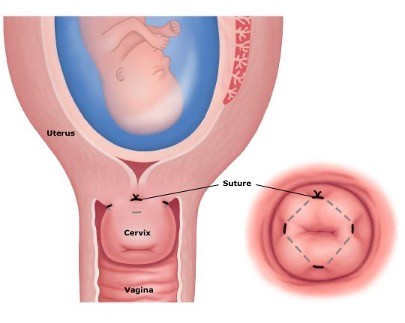
Cerclage
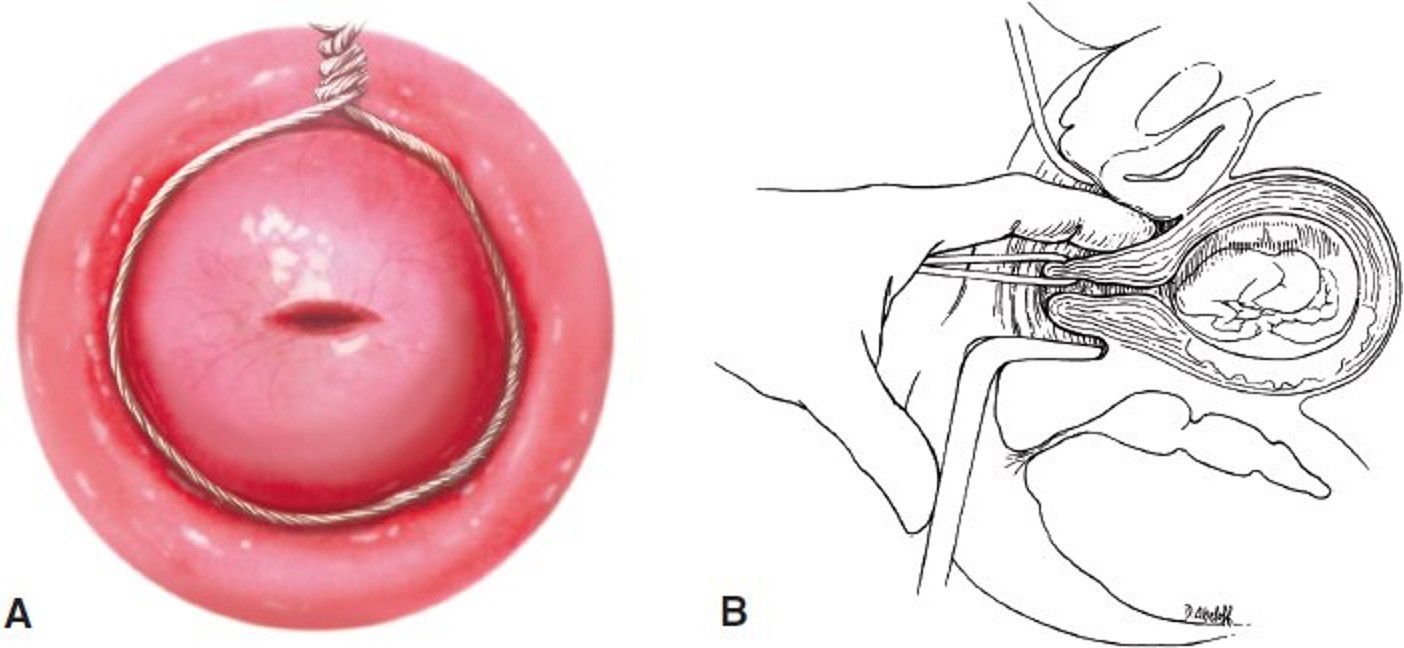
Cerclage Procedures:
-McDonald procedure a purse-string technique is placed high up in the cervix and then tied closed. (12,3,6,9 and tied at 12 o’clock)
-Shirodkar procedure places a submucosal band at the level of the internal os.
-Abdominal Cerclage: band is placed around cervix through abdomen.
Cerclage NURSING MANGEMENT
•Monitor for signs of preterm labor
•Monitor for backache
•Monitor for increase in vaginal discharge
•Monitor of ruptured membranes
•Education
Placenta Previa
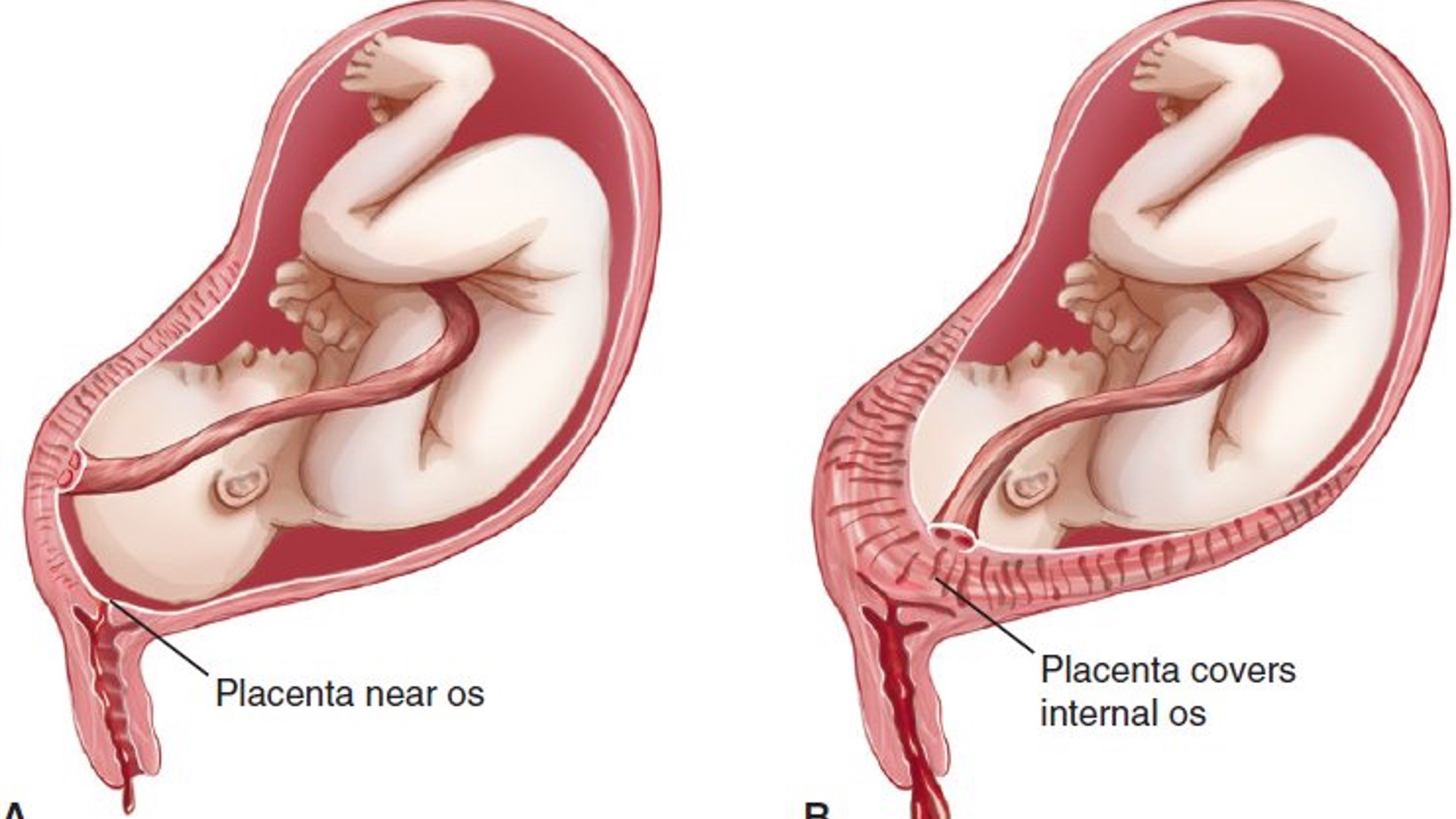
•Placenta implantation in the lower uterine segment
Predisposing Factors:
•Prior uterine scar
•Multiple pregnancies/gestation
•Prior history of placenta previa
Symptoms
•Painless, quiet onset bright red bleeding
•Bleeding may be intermittent or continuous
•Uterus soft, palpable
•Presenting part is high and deviated to one side
•Associated with preeclampsia
Management of Placenta Previa
Expectant Management
-Observation and bed rest/pelvic rest if less than 36 week gestation, normal FHR and mild bleeding that resolves
-No vaginal or rectal exam
-NST/BP once or twice weekly
-Assess bleeding
-Potential emergency
Active Management
-If past 36 weeks gestation – can deliver
-If excessive or continued bleeding can deliver at any gestational age
Placenta Abruptio
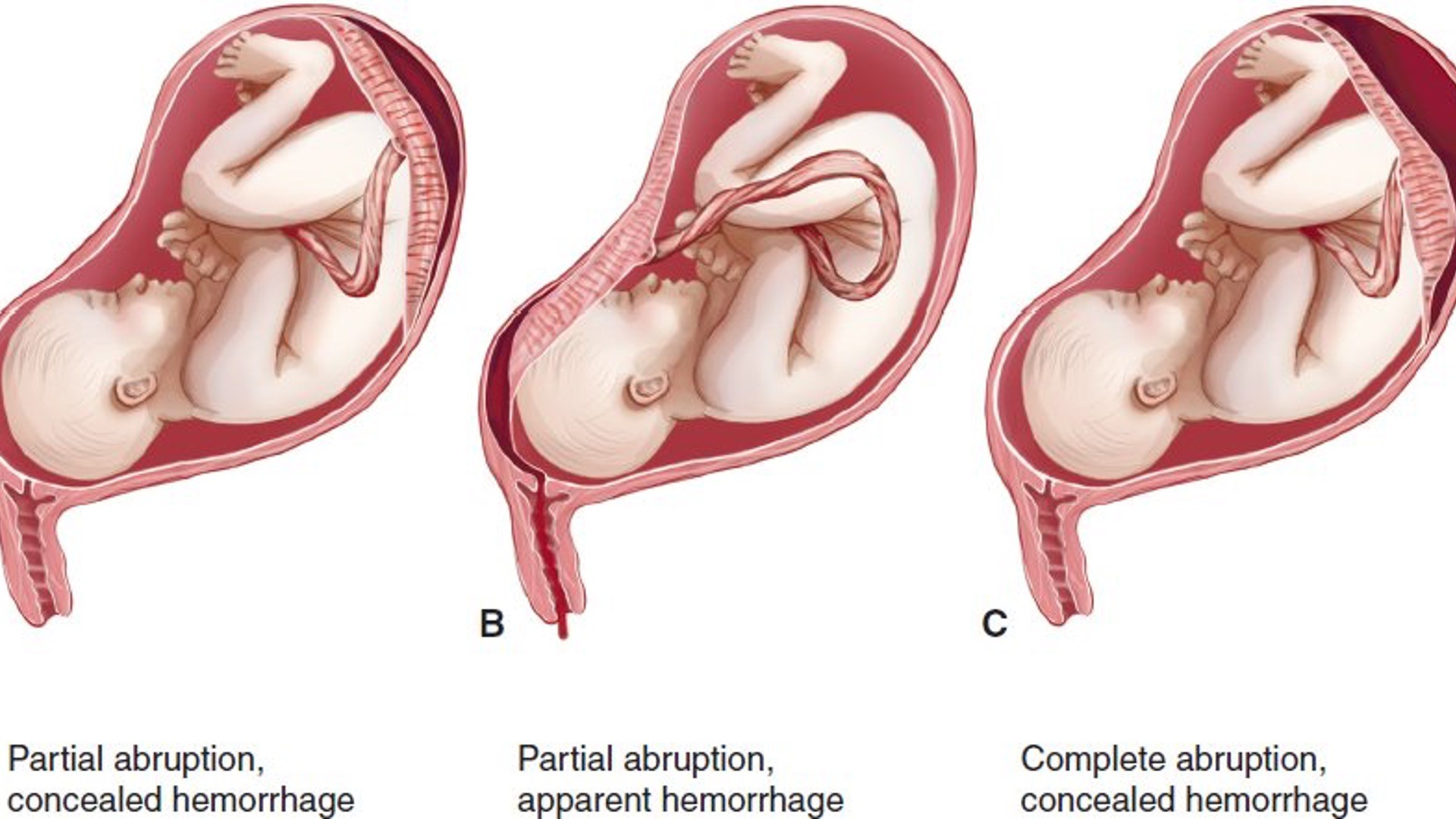
•Premature separation of normally implanted placenta from uterine wall
•Associated Factors:
•Drug use; Cocaine
•Hypertension
•Trauma
•Hydramnios
Symptoms
•Dark venous blood
•Abdomen rigid, hard
•Severe pain
•Sudden onset
placenta previa Management
•No Vaginal Exams!!
•Daily CBC
•Fetal well-being tests – NST
•Monitor for Contractions
•Monitor Bleeding amount
•Monitor for PROM
•Medication - Celestone
Management of Placental Abruption
Expectant
-Dependent on amount of blood loss and fetal maturation
-Between 20-34 weeks if both stable can use expectant management
-Close monitoring for bleeding, IUGR, fetal well being
Active
-If term or bleeding moderate to severe
-May need immediate delivery
-Needs at least one large ore IV line
-Vaginal birth preferred if possible
PLACENTA ACCRETA
•Retained Placenta due to partial separation, entrapment or abnormal adherence of the placenta to the uterine wall
•Must be removed after delivery to prevent infection and hemorrhage
•Hysterectomy is done if uncontrollable bleeding occurs
•Nursing care includes vital signs, post-up care and emotional support
HYPEREMESIS GRAVIDARUM
-Severe form of N & V
-Persistent
-Begins before 9 weeks gestation
-Risk factors for hyperemesis include
Previous pregnancy complicated by hyperemesis,
Molar pregnancies,
History of Helicobacter pylori infection, multiple gestation,
Prepregnancy history of genitourinary disorders, and/or clinical hyperthyroid
Prepregnancy psychiatric diagnosis
medications:
Promethazine (Phenergan)
Pyridoxine and doxylamine (Diclegis)
Ondansetron (Zofran)
Hypertension
-Chronic hypertension: Hypertension exists prior to pregnancy or that develops before 20 weeks’ gestation
-Gestational hypertension: A new-onset blood pressure elevation (140/90 mm Hg) identified after 20 weeks’ gestation without proteinuria; blood pressure returns to normal by 12 weeks’ postpartum
-Preeclampsia/eclampsia and HELLP: Most common hypertensive disorder of pregnancy, which develops with proteinuria after 20 weeks’ gestation
-Chronic hypertension with superimposed preeclampsia: develops after 20 weeks’ gestation and occurs in approximately 25% of pregnant women with increased maternal and fetal morbidity rates)
Preeclampsia
-It is defined as an increase in blood pressure after 20 weeks gestation accompanied by proteinuria.
-The signs and symptoms can develop for the first time after 20 weeks
Fetal movement record
Nonstress test (NST)
Ultrasonography every 3 to 4 weeks for serial determination of growth.
Biophysical profile
Amniocentesis to determine fetal lung maturity.
Doppler Velocimetry beginning at 30 to 32 weeks to screen for fetal compromise
(edema, headache, muscle twitching, swollen face/hands/feet,high BP, abdominal pain, )
Eclampsia(SEIZURE)
-Maintain patent airway and safety during convulsion
-Magnesium sulfate (To control seizures and will continue postpartum)
(headache, seizure, visual disturbances, generalized edema)
-Auscultate lungs to r/o pulmonary edema
-Strict Input and Output (Place foley with urimeter)
-Monitor for placental abruption/ bleeding/rigid abdomen
-Left lateral (To prevent aspiration of vomitus)
-Side rails elevated (To prevent falls)
-Plan for Delivery (IOL vs Cesarean section)
-Seizures can still occur first 48 hours postpartum
Magnesium Sulfate
Loading Dose ( 4-6 gm over 15-30 min)
Maintenance Dose – 40 gm/1000ml LR ( 1-2 gm/hr)
Serum Magnesium Therapeutic Level- 4-7 mEg/L
Serial Magnesium Level q 6 hours
Administer calcium gluconate IV if toxicity occurs
Medications Used with Preeclampsia and Eclampsia
Magnesium sulfate
Hydralazine hydrochloride (Apresoline)
Labetalol hydrochloride (Normodyne)
Nifedipine (Procardia)
Sodium nitroprusside (Nitropress)
Furosemide (Lasix)
HELLP
•Category of gestational hypertension that involves changes in blood components and liver function, as well as, a complication of severe preeclampsia
•H: hemolysis
•EL: elevated liver enzymes
•LP: low platelets
•Patient complains of pain, most commonly in the right upper quadrant, epigastric area, or lower chest.
Effects of HELLP Syndrome on Mom and Baby
•DIC
•Abruptio placentae
•Acute renal failure
•BABY:
•Insufficient blood flow
•Intrauterine growth restriction
•Death
•Increased risk of fetal hypoxia during labor
•Thrombocytopenia
•Leukopenia
Polyhydramnios
•Excessive amount of amniotic fluid, more than 2L
•Accompanies neural tube defects such as spina bifida and anencephaly
•Can lead to ineffective contractions (dystocia) and failure of uterus to contract after birth
What are some medications that stop preterm labor ?
Tocolysis Nifedipine ( Procardia )magnesium sulfate Terbutaline
What medication matures the babies lungs ? also used in preterm labor
Bethametasone
Magnesium Sulfate for preterm labor
prevent seizures muscle relaxant and neuro protective
Symptoms of magnesium toxicity
FLUSHING / HEADACHE/ DIZZY Depressed DTRRESPIRATORY DEPRESSION
What do you teach patients when they have a cerclage procedure
look out for signs and symptoms of labor ~leakage of fluid ~ contractions ~ pelvic pains
A new mother comes into the ED with Placenta abruption. After the successful delivery of her baby she notices the 24 hour newborn is pooping blood what should the nurse do ?
Inform the mother that this is normal the baby might of swallowed blood in utero
What is your main concern for Hyperemisis
DEHYDRATION * everything Hypo
What signs will you see of HELP syndrome
~pale ~Anemic ~bleeding around Iv~black and blue bruises RT UPPER QUADRANT PAIN
When is the Glucose challenge test done ? ( done on every pregnant mother)
Done at 24-28 weeks Gestation
What important things should you look out for for terbutaline ?
Causes heart to beat really fats if her hr is high hold the medication if someone has cardiac problems precaution.Helps slow labor down always monitor blood pressure if heart rate is 120 over hold the medicine.decreases potassium
What can cause cervical insufficiency ?
~Repeated pregnancy loss ~Abortions ~Trauma to cervix
What is a sign of cervical insufficiency ?
cervix will be dilating and shortening before 37 weeks
What is Hyperemisis?
Excessive vomiting
What medication is used for Hyperemissis?
Zofran
Causes of Postpartum hemorrhage
Tone
-Overdistention of uterus
-uterine infection
Tissue
-products of conception (incomplete placenta at birth)
-retained blood clots
Trauma
-lacerations
uterine inversion
Thrombom
-preexisting conditions
-traction on umbilical cord
PPH medications
Pitocin
Carboprost
methergine
misoprostol
oxytocin
How to help PPH
Fundal massage
evaluate bladder
bimanual compression
low level suction
Subinvolution
incomplete involution of uterus after birth
•Failure of uterus to return to normal size after pregnancy – lochia rubra of greater than 2 weeks duration suggests subinvolution
Caused by:
•Retained placental fragments
•Distended bladder
•Uterine myoma
•Infection
Infection
•Puerperal/Postpartum/Endometritis
Mastitis
•Risk Factors
Prolonged ROM
Prolonged labor
Fetal scalp electrode or IUPC
BV or Chlamydia infection
Vacuum or forceps use
Manual removal of placenta
Episiotomy of laceration
Compromised health status or DM
Endometritis
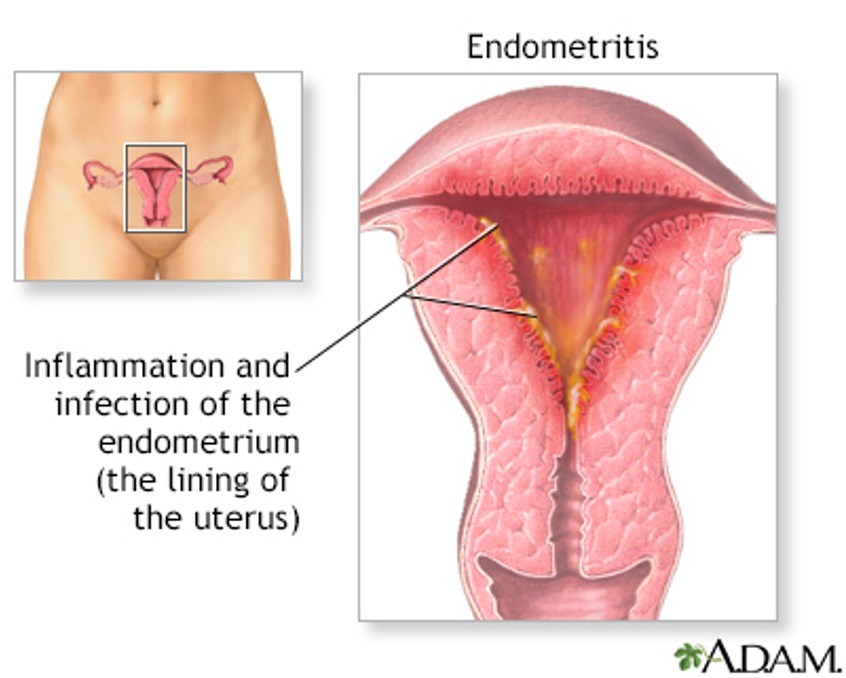
•Most common with labor then c-section
•Bacteria from the vagina, bowel and perineum invade the uterus
•S/S start within 1-2 days of delivery; fever, tachycardia, uterine tenderness
•Antibiotics needed