Nageles Rule for pregnancy dating
Begin with the first day of last missed period, subtract 3 months and add 7 days and add 1 year
Common lab tests for 1st prenatal visit
Complete blood count (CBC)
Blood typing
rubella titer
hepatitis B
HIV testing
STI screening
cervical smears
1st trimester
1-13 weeks
2nd trimester
12-27/28 weeks
3rd trimester
28 weeks 38-42
What is the fundal height at 20 weeks?
by the bellybutton
What are some risk factors for adverse pregnancy outcomes?
diabetes
folic acid deficiency
hepatitis B
HIV/AIDS
Obesity
STIs
smoking
alcohol
A pregnant patient is complaining about urinary frequency or incontinence. What therapeutic advice can the nurse give?
Try pelvic floor exercises to increase control over leakage
empty bladder when you first feel full sensation
avoid caffeinated drinks
reduce fluid intake after dinner to reduce nighttime urination
A pregnant patient is complaining of constant nausea and vomitting. What should the nurse suggest?
avoid an empty stomach at all times
eat dry crackers/toast before arising
avoid brushing teeth right after eating to avoid gag reflex
drink fluids between meals rather than with them
avoid greasy foods
What is a non invasive method to monitor the fetus and when can it be done?
Fetal movement counts (kick counts)
from week 28-38
encourage mom to lay on side
encourage mom to eat
Ultrasound
images produced by sound waves to check for possible birth defects
Quickening
noticed 16-20 weeks
what does an ultrasound assess?
to estimate gestational age, fetal weight, and growth
location of placenta and amniotic fluid volume
accompanying invasive procedures
Doppler blood flow studies
Intiated at 15 weeks
measures blood flow changes in maternal and fetal circulation
assessment of placental function
if ratio is elevated may indicate baby not growing well
looks at sys/dias of heart
Why is the doppler blood flow study initiated?
If mother has diabetes or baby is not growing well
What is aminocentesis?
A procedure to obtain amniotic fluid
Allows testing of amniotic fluid
Why is Aminocentesis done?
This test can provide information about genetic disorders and fetal maturity
What are some negatives to having Amniocentesis done?
Hemorrhage
Amniotic fluid embolism
Loss of pregnancy
Rh isoimmunization
Can hurt the fetus
Infection
Cause bleeding
Rupture placenta
Cramping
What does Amniocentesis procedure look like?
Large needled going into amniotic cavity
What is Chorionic villus sampling?
Catheter is used to withdraw a sample of placental tissue to test for chromosomal abnormalities. Test done after 10-13 weeks.
What are the complications of Chorionic villus sampling?
Increased risk of injury to fetus
Inability to detect neural tube defects
Risk of failure to obtain placental tissue
risk of contamination of specimen
risk of leakage of amniotic fluid
risk of intrauterine infection
risk of Rh isoimmunization
What is Alpha-fetoprotein?
Checks the baby's risk of birth defects and genetic disorders, such as high levels for neural tube defects or low levels for Down syndrome. It is done at 15 to 22 weeks gestation.
Nonstress Test
used to assess fetal status using an electronic fetal monitor
If baby moves and heart rate increases-healthy baby
If baby heart rate goes down- unhealthy
Fetal kick counts
Provides reassurance of fetal well being(movement 10 x an hour)
Reactive non-stress test
FHR acceleration of 15 bpm for 15 seconds in response to fetal movement after 32 weeks
for less than 32 weeks 10 bpm for 10 seconds is acceptable
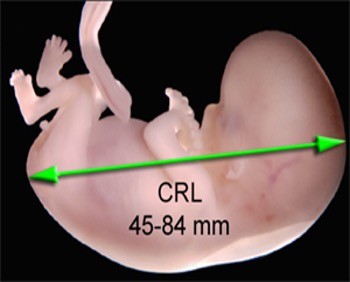
What is crown rump?
Measurement of baby form crown of the head to the buttock shows if the pregnancy is dated correctly
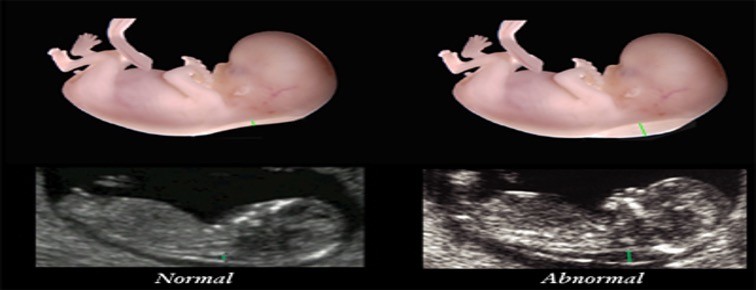
Fetal Nuchal Translucency
An intravaginal ultrasound that measures fluid collection in the subcutaneous space between the skin and the cervical spine of the fetus
What is fetal nuchal translucency used for ?
-Trisomy 21 -looks to see if there is to much fluid -if there is to much fluid further genetic testing is needed
What are the blood test assessments to measure two hormones?
BHCGPAPP-A this is complete the screening for chromosomal abnormalties
When is amniocentesis recommended?
Age 35 and older family history of genetic defects blood test or ultra sound hinting at defects
Normal baby heart rate
110-160
When is a Non-stress test (NST) done ?
can be done out patient can be done if the mother is past her due date can be done if there is a medical problem
reactive/nonreactive
Nursing interventions if fetus is not moving
lay on left side give sweets wait 30 min give the baby time baby may be sleep they are tiny humans
Contraction Stress Test
Given contraction to see how the baby would tolerate labor- would not be done during preterm stage or mother getting a C-section
Enables identification of fetal risk for asphyxia
Fetal monitor is used
Fetal heart rate response to contractions is noted
Healthy fetus usually tolerates contractions
Positive Contraction Stress Test
Placenta is not working well because baby is not reacting well to contractions(heart rate decelerates)
Biophysical profile ultra sound 5 parameters
- Fetal breathing - Fetal movements body and limbs -Fetal Tone( extension, flextion) - amniotic fluid volume - reactive fetal HR with Reactive NST
RH + baby RH - mother
MOM NEEDS ROHGAM
When is Rhogam given to RH - mother
28 wees pregnant
RH Negative mother after amniocentesis
MUST GET RHOGAM WITHIN 72 HOURS
Nursing education after amniocentesis
its done under ultrasound guidance may expirence cramping pressure after
Risk if there is not enough amniotic fluid present during ultrasound ?
Can cause fetal Heart deceleration
Percutaneous umbilical blood sampling
Usually for specific circumstances
-to do a blood transfusion
-take blood out
It goes through umbilical cord
If the placenta attaches over the cervix what is this called ?
Placenta previa
What is the mother at risk for if the placenta covers the cervix ?
-Hemorrhage -C- Section/ baby will not be able to pass through the cervix
Prenatal visits
Up to 28 weeks: every 4 weeks
29-36 weeks: every 2 weeks
37 weeks to birth: every weeks
Routine Assessments
weight and blood pressure (vital signs)
urine testing for protein, glucose, ketones and nitrites
Fundal height measurement to asses fetal growth
Edema
Blood tests
assessment for quickening (fetal movement)
assessment of fetal heart rate- 110-160
Lightening
dropping of baby
Fundal height at 16 weeks
below belly button
Fundal height at 26 weeks
like 2 cm above the belly button
Danger signs of pregnancy 1st trimester
spotting/ bleeding (miscarriage)
painful urination (infection)
severe vomiting (hyperemesis gravidarum)
fever higher than 100 (infection)
lower abdominal pain with dizziness and shoulder pain (indicative of ruptured or ectopic pregnancy)
Danger signs of pregnancy 2nd trimester
regular uterine contractions (preterm labor)
pain in calf, increased foot flexion (DVT)
sudden gush or leakage of fluid from vagina(pre labor rupture of membranes)
absence of fetal movement for more than 12 hours (possible fetal distress or demise)
Danger of 3rd trimester
-sudden weight gain; periorbital or facial edema, severe upper abdominal pain; headache with visual changes (indicative of gestational hypertension and/or preeclampsia
-decrease in fetal daily movement for more than 24 hours (possible demise)
A patient is experiencing extreme fatigue. As the nurse what can you tell her?
Attempt to get a full nights sleep without interruptions
Eat a healthy balanced diet
Schedule a nap in the early afternoon daily
when feeling tired, pause, and rest
A patient is experiencing extreme backache. As the nurse what can you tell her?
Avoid standing or sitting in one position for long periods
Apply heating pad (low setting) to the small back
Support lower back with pillows when sitting
Use proper body mechanics for lighting anything
Avoid excessive bending, lifting, walking without rest periods
Wear supportive low heeled shoes: avoid heels
Stand with shoulders back to maintain posture
A patient is experiencing extreme leg cramps. As the nurse what can you tell her?
Elevate legs above heart level throughout day
If you catch cramp, straighten both legs and flex feet toward body
Ask health care provider about taking calcium supplements
Stocking to promote better circulation (compression socks)
A patient is experiencing hemorrhoids . As the nurse what can you tell her?
Try to establish regular time for bowel movement
Avoid constipation and straining during defecation
Prevent straining by drinking plenty of fluids and eating fiber rich foods and exercise daily
Use warm site baths and cool witch hazel compresses
A patient is experiencing constipation. As the nurse what can you tell her?
Increase intake foods high in fiber and drink at least 8 glasses of fluid
Ingest prunes or prune juice (natural laxative )
Consume warm liquids
Exercise each day to promote movement
Reduce amount of cheese consumed
A patient is experiencing heartburn/indigestion. As the nurse what can you tell her?
Avoid spicy or greasy foods
Sleep on several pillows so that head is elevated 30 degrees
Avoid laying down 3 hours after meals
take antacids sparingly
Onset of labor
-Uterine stretch -Oxytocin increases -Increased prostaglandins -Progesterone withdrawal
fetal presentation
occpital bone (O) Chin (M)Buttocks (S)Scapula ( A)
Premonitory signs of labor
- Cervical changes- Lightening- Increased energy level ( Nesting )- "Bloody show"- Braxton Hicks contractions- Spontaneous rupture of membranes( water breaks )
true labor
Patient will have a cervical change !! Contactions increase in duration , intensity , and frequency Pain that starts in your back-and radiates to belly bloody show spontaneous rupture
False Labor
irregular contractions, discomfort is abdominal, contractions decrease with either rest or activity, NO CERVIX CHANGE !
Five P's of Labor
Passage way ( birth canal ) Passenger ( Fetus ) , powers (contractions) , position( maternal ) , and psychological response
Passageway
Make sure the mothers Pelvis can accommodate for the Fetus
Passageway: Pelvic Shape
*Gynecoid( preferable )-Android( male shaped not favorable ) *Anthropod (usually adaquate)-Platypelloid ( Not favaroble )
passageway soft tissues
Cervix pelvic floor muscles vagina
passenger
Fetal skullFetal attitudeFetal lieFetal presentationFetal positionFetal stationFetal engagement
fetal presentation
Brow & Face makes birthing process very difficult
Effacement
thinning of the cervixcervix pulls back 0/ 50/100
Fetal station
Baby location baby presentation in the pelvis
Powers
contractions - frequency , duration , intensity
Maternal Physiological response to labor
Increased heart rate , Increased cardiac out put , increased blood pressure ( during contractions )Decreased GI NPO Decreased glucose NPO
Fetal Physiological response
Decrease in fetal oxygen Fetal heart rate accelerations and decelerations
Stages of Labor
Stages 1-4 stage 1 ( contractions get to 10 cm ) stage 2 ( delivery of baby goal push out baby ) stage 3 placenta delivery stage 4 ( postpartum recovery do not make pt bleed )
Stage 1 of labor and delivery
Stage 1 is considered true labor and consists of 3 phases Latnet 0-6cmactive 6-8cmTransition phase 8-10cm SHORTEST STAGE MONITOR FETAL HR
1s stage of labor -(LATENT PHASE )
0-6 cm moms relaxed contractions every 5-10 min Lonest stage of labor
1st stage : Active Phase
6-8 cm dilated contractions every 2-5 min
1st stage Transition Phase
8-10 cm mom is ready to push
Stage 2 labor
10 cm moms fully effaced Birth of the baby encourage mom to bear down when pushing
Stage 3 of labor and delivery
birth of placenta within 30 min Never pull umblicusduring this phase there is an increased risk of infection if placenta isn't fully removed PITOCIN ( Prevents hemmorage )
Signs of hemmorrage
Decreased blood pressure Increased Heart Rate
stage 4 of labor and delivery
1-4 hours after delivery assess : mom assess : Temerature not over 100.4 assess Hemmorage
Placenta Seperation signs
uterus rises upward umblicus lenghtens sudden trickle of blood uterus changes to globular PLACENTA SEPERATION HAPPENS IN THE 3rd TRIMESTER
FUNDUS
Should be
firm midlineleveled with umblicus check the fundus and massage it until it is firm if it is soft ( boggy )
fundus assessment
3 x eveyr 5 min
Fundus abnormality
displaced above umblicus one sided = bladder distention
Methergine medication
Methylergonovine is a medication that treats excessive bleeding after childbirth cannot be given if mom has preeclamisia or HTN
Cardinal Movements
"Every Day Fine Infants Enter Ready (Eager) and Excited"Engagement, descent, flexion, internal rotation, extension, restitution (external rotation), expulsion
Fetal Lie
Vertex- normal
Breech- butt legs up
Shoulder
Fetal position
LOP- Left Occiput posterior (back to back)
LOT- Left Occiput transverse
LOA- Left Occiput Anterior (facing front)
ROP- Right Occiput posterior
ROT- Right Occiput transverse
ROA- Right Occiput Anterior
Birthing positions
recumbent position
left lateral sims
squatting
semi fowlers
sitting
hand and knees
Psychosocial considerations
understanding and preparing for childbirth
support from others
present emotional status
beliefs and values
Physiological changes during birth
-increased cardiac output
-increased heart rate
-increased blood pressure during uterine contractions
-increased WBC
-increased respiratory rate
-increase in temperature
-decreased GI motility and absorption
-decreased blood glucose level
Fetal side of placenta
Schultze presentation- shiny and smooth
(s for shiny)
Maternal side of placenta
Duncan presentation- rough and irregular
(D for dirty)
Can cause excessive bleeding
Fern test
High estrogens in amniotic fluid cause crystallization of the salts ; crystals appear as a blade of fern
what does Tocodynamometer meausure ?
external fetal monitoring records the frequency and duration of the contractions placed on fundus
what does transducer meausre ?
Fetal Heart tones bottom
Why would IUPC be used ?
* cant pick up mothers contractions * obese patients * Oliohydramus * baby Heart rate decreases CERVIX MUST BE OPEN 2 CM water needs to be broken
Leopold's Maneuvers determine
Engage fetus in uteri position of baby presentation lie
What stage of labor is episiotomy done ?
stage 2
What do you need to know when the water breaks ?
* spontaneous * artificial * odor * should be clear * should not have meconium ( color if baby has BM )
why cant patients eat before labor ?
Gi system slows down no food risk for aspiration in case of emergency c-section
whats the biggest concern if your water breaks before labor starts ?
Infection labor will be induced
Labor induction medication
cytotec amisaprostale cervidil - thins cervix pitocin oxytosin
High Risk factors during labor?
- Diabetes-prolapse chord -Breech baby -meconium in the fluid
Abrution placenta
Placenta separates off wall before the baby is born if this happens baby will not receive oxygen or nutrients emergency c section Cause : HTN TRAUMA
Bishop score
Pre labor scoring that helps predict success of induction
If a mother comes into the ED and says water broke what do you do first ?
CHECK THE FETAL HEART RATE
Low bishop score indicates
High risk for c- sectioncervadil medication cytotec
where can you feel contractions ?
top of the Fundus
High bishop score
Favorable for induction 8-9
AROM / SROM ( Spontaneous rupture of membranes )
Gush of fluid trickle Pooling in vagina ( SROM) PH greater than 5 ( ninrazine paper) turns dark blue dark green
what color does Nitrazine paper turn ?
turns blue or green alkaline ph greater than 6.5
What three methods do nurses use to assess frequency duration and intensity of contraction?
Palpation External fetal monitoring (tocotransducer)Internal Fetal Monitoring ( IUPC )
Nursing interventions for 4th stage
ice to perineum PRN
perineal care- peri bottle
monitor for return of sensation of regional anethesia
monitor PPH and Urinary retention
analgesia PRN
food and fluids
parent infant interaction
Non pharmacologic pain management
relaxation/visualization
acupressure/tough/massage/effleurage
ambulation/position changes
hypnobirthing
breathing
application of heat or cold
Systemic analgesia
Morphine
Meperidine
Butorphanol
Nalbuphine (decreases nausea and vomiting)
Fentanyl (hypotension/ respiratory depression)
Hydroxyzine (reduces anxiety)
Epidural
regional block
used for labor and cesarean births
patient receive 500 to 1000 ml of normal saline
T8 to T10 of spinal cord
Epidural Opioids
Fentanyl
Sudentanil
Ropivacaine
Morphine
V C
E H
A O
L P
Variable deceleration- Cord compression
Early decelaration- Head compression
Acceleration- OKAY!
Late deceleration- Placental insufficiency
Aminoinfusion
prevents additional cord compression
room temperature saline into uterus with catheter
Tocolytics
Medication to relax uterus
Improves blood flow to uterus decreasing/stopping contractions
L
I
O
N
Left lateral side (turn)
Iv fluids
Oxygen
Notify provider
M
I
N
E
Maternal positioning
Identify labor progress
No intervention
Execute intervention
Fetal Bradycardia
hypoxia
hypothermia
maternal hypotension
prolonged umbilical cord compression
Fetal Tachycardia
prematurity
hypoxia
maternal dehydration
maternal hyperthyroidism