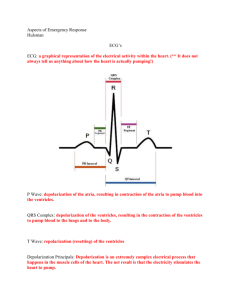
heart anatomy & arrhythmias
advertisement

OVERVIEW OF THE HEART ANATOMY And ARRHYTHMIAS Presented by Linda and Livia www.vancouverhearthealth.com ANATOMY The size of a fist Weighs between 250 and 350 grams It has 4 chambers Two superior chambers called Atria Right Atrium (RA) and Left Atrium (LA) Two inferior chambers called Ventricles Right Ventricle (RV) and Left Ventricle (LV) Sulci define the boundaries of the 4 chambers Coronary sulcus separates the atria from the ventricles Interventricular sulcus separates the left and right ventricles Sulci contain major arteries and veins for heart circulation The heart has 3 layers: Pericardium – tough membranous sac that encloses and protects the heart (outermost layer of the heart) A thin layer of clear pericardial fluid inside the pericardium lubricates the external surface of the heart as it beats Inflammation of the pericardium - Pericarditis Myocardium – thickest layer of the heart made of pure muscle and it gets damaged during a heart attack. It is responsible for contraction and relaxation of the atria and ventricles. Epicardium – covers the outside of the myocardium. It is a thin layer made of connective tissue and fat. Endocardium – innermost thin layer of tissue that lines the heart's chambers and valves. The cardiac conduction system is located in this layer of the Overview of Valves and Blood Flow Heart Chambers, Valves, and Blood Flow The heart is a two pump system The right side of the heart collects blood from the periphery and pumps it through the lungs – called Pulmonary circuit The left side of the heart collects blood from the lungs and pumps it throughout the body – called Systemic circuit The left ventricle pumps the blood against the greater resistance to the body (more muscular) The right ventricle pumps the blood a relative short distance through the pulmonary circuit (less muscular) Valves The heart has 4 valves Atrioventricular valves: Tricuspid valve – controls the blood flow from RA to RV Bicuspid valve – controls the blood flow from LA to LV These valves prevent the retrograde blood flow during ventricular contraction Semilunar valves: Pulmonary valve – lies between the RV and the pulmonary artery Aortic valve – lies between the LV and the aorta The cusps of the semilunar valves prevent the back-flow of blood from the arteries to the ventricles Blood Flow Venous blood flows into the RA via the superior and inferior vena cava, coronary sinus, and anterior cardiac veins The RA free wall contracts, and blood flow moves through the tricuspid valve into the RV The RV free wall contracts, the tricuspid valve closes, and blood flows through the pulmonary valve into the pulmonary artery and the branches of that system Blood ultimately reaches the alveolar capillaries, where gas exchange occurs Blood flows back to the LA via the pulmonary veins The LA free wall contracts, and blood flows through the bicuspid valve and into the LV The LV free wall contracts, the bicuspid valve closes, and blood flows through the aortic valve into the aorta and its branches, where it is distributed to the coronary circulation and the systemic circulation Heart Blood Supply Only the endocardium gets direct blood supply The myocardium is too thick to permit adequate diffusion of nutrients and oxygen to the cardiac muscle cells and epicardium Coronary arteries originate from the aortic sinus at the base of the aorta Left coronary artery (LCA) Right coronary artery (RCA) LCA goes towards the left side of the heart before branching into Left anterior descending (LAD) coronary artery Circumflex artery (CxA) The LAD artery supplies blood to the interventricular septum and anterior walls of both ventricles The CxA branches toward the left margin of the heart in the coronary sulcus and supplies blood to the laterodorsal walls of the LA and LV Both the LAD and CxA curve around the left ventricular wall and supply small branches that interconnect with the RCA The RCA supplies blood to the right side of the heart as it follows the AV (atrio-ventricular) groove It then curves to the back of the heart giving off a posterior interventricular artery (posterior descending artery - PDA) The RCA and PDA have numerous branches that supply blood to the anterior, posterior, and lateral surfaces of the RV and to the RA After circulating through the coronary artery system and the myocardial capillaries, it is collected by the cardiac veins The blood then travels a path similar to that of the coronary arteries but in the opposite direction On the posterior side of the heart, the cardiac veins form an enlarged vessel → coronary sinus, which empties the blood into the RA The smaller anterior cardiac veins also empty directly into the RA Conduction System of the Heart Cardiac muscle has intrinsic properties → no need for neural stimulation Cardiac cells interconnect end to end and form intercalated discs these discs allow electrical impulses to spread from cell to cell and cause the myocardium to act as a single unit Components of the Conduction System: Sinoatrial node (SA node) Atrioventricular node (AV node) AV bundle (Bundle of His) Right and Left bundle branches Purkinje Fibers The electrical impulse starts at the SA node (intrinsic pacemaker) The cells depolarize spontaneously at 60 to 80 beats per minute at rest Electrical activity goes rapidly to AV node via internodal pathways through both atria Depolarization spreads more slowly across atria. Conduction slows through AV node to allow the atria to contract and fill the ventricles Depolarization moves rapidly through ventricular conducting system to the apex of the heart Depolarization wave spreads upward from the Sympathetic nerves and hormones (neropinephrine and epinephrine) stimulate the atria and ventricles of the heart to beat faster → chronotropic effect and more forcefully → inotropic effect Parasympathetic nerves control the atria and slow the heart rate ECG changes during electrical events in the heart The SA node initiates a depolarization wave at regular intervals in the atria which is represented by a P wave on an ECG The P wave represents both depolarization and contraction of atria When the wave of atrial depolarization enters the AV node, depolarization slows producing a brief pause – time it takes for the blood to enter the ventricles Depolarization conducts rapidly through the Bundle of His and its subdivisions and into Purkinje fibers Depolarization of the ventricular myocardium records as a QRX complex The horizontal segment of baseline that follows the QRS complex is the ST segment ST segment is horizontal, flat, and most importantly, it is normally level with other areas of the baseline If the ST segment is elevated or depressed beyond the normal baseline level, this is usually a sign of serious pathology that may indicate imminent problems ST segment represents the initial phase of ventricular repolarization The final T wave represents the final “rapid” phase of ventricular repolarization What Is Arrhythmia? Abnormal rhythm of the heart It can feel like a temporary pause and be so brief that it doesn't change your overall heart rate Or it can cause the heart rate to be too slow or too fast What are the signs of Arrhythmia? If brief it can have almost no symptoms → it can feel like a skipped heart beat that you barely notice Or it can feel like a fluttering in the chest or neck If it lasts long enough the heart may not be able to pump enough blood to the body → it can cause tiredness and light-headedness, or the person may pass out Tachycardia can lead to decreased cardiac out (heart is not able to pump blood effectively) → can lead to shortness of breath, chest pain, light-headedness or loss of consciousness. In severe cases it can cause heart attack and death. Different Types of Arrhythmias Pacemaker of the heart → SA node → initiates depolarization of the myocardium Beats at its own inherent rate of 60 bpm to 100 bpm Bradycardia → slow heart rate < 60 bpm Common in athletes → ↑ stroke volume, ↓ heart rate Increased vagal stimulation → release of hormones that slow down the heart rate Patients who receive drugs to slow down the heart rate Individuals who have disease of the sinus node Symptoms: tiredness, dizziness, light-headedness or fainting Treatment: electronic pacemaker Types of Bradycardias: Sick Sinus Syndrome: “malfunction” in the SA node → it fires too slowly due to increasing age or disease some medications can slow your heartbeat Solution: treatment with medication or with an electronic pacemaker Heart Block: Interruption of the electrical signal to the lower chambers of the heart It may develop as a side effect of certain heart medications It may be idiopathic in nature Or may be due to other forms of circulatory diseases: coronary artery disease cardiomyopathy rheumatic heart disease uncontrolled or untreated high blood pressure primary conduction system disease Complete AV block (3rd degree block) is usually due to a complication of a heart attack, but may the result of a heart surgery or infections of the heart muscle Symptoms: Llight-headedness, fatigue, or fainting Diagnosis: By ECG Treatment: Implanting an electronic pacemaker Tachycardia → fast heart rate → > 100 bpm Causes: stimulation of the heart by sympathetic nerves increased body temperature or toxic conditions of the heart Factors that affect SNS stimulation of the heart: blood loss that results in a shock or semishock weakening of the myocardium Supraventricular Tachycardia (above the ventricle) rapid heartbeat in the atria or AV node Atrial flutter Atrial fibrilation Paroxysmal supraventricular tachycardia Wolf-Parkinson-White Syndrome Atrial Flutter → 250 to 350 atrial depolarization per minute Due to back-to-back identical atrial depolarization waves Usually not life threatening Can cause chest pain, faintness, or others more serious problems Atrial Fibrillation → multiple foci discharge rapidly at 350-450/min Very common dysrhythmia Results in ↓ cardiac output Usually not life threatening Causes light-headedness or palpitations It increases the risk of stroke Symptoms of Atrial fibrillation: Irregular and fast heart beat Heart palpitations and rapid thumping in the chest Chest discomfort, chest pain or pressure Shortness of breath, particularly with exertion or anxiety Fatigue Dizziness, sweating, or nausea Light-headedness or fainting Causes of Atrial fibrillation: In most cases idiopathic in nature Age High blood pressure Infection or inflammation of the heart Valvular heart disease Ischemic heart disease Cardiomyopathy Conduction system disease Overactive thyroid Pulmonary embolism Hypoxia Holiday heart syndrome Treatment of Atrial fibrillation Blood thinners to decrease the risk of stroke Rhythm control therapy: medication to prevent atrial fibrillation from occurring electrical cardioversion ablation maze procedure Rate control therapy: medication to slow down the heart rate: Digitalis Calcium channel blockers (diltiazem and verapamil) Beta-blockers Treatment of Atrial fibrillation Blood thinners to decrease the risk of stroke Rhythm control therapy: medication to prevent atrial fibrillation from occurring electrical cardioversion ablation maze procedure Rate control therapy: medication to slow down the heart rate: Digitalis Calcium channel blockers (diltiazem and verapamil) Beta-blockers Paroxysmal supraventricular tachycardia → 140-250/minute Involves atria or AV node Usually occurs in young, healthy people May be distressing and can cause weakness during the paroxysm Rarely life threatening Can occur with digitalis toxicity and WolfParkinson-White Syndrome The following increases your chance for PSVT: Alcohol use Caffeine use Illicit drug use Smoking Symptoms: Anxiety Chest tightness Palpitations and rapid pulse Shortness of breath Dizziness and fainting Treatment: Valsalva maneuver Cough while sitting with your upper body bent forward Splashing ice water on face Ablation Cardioversion Medications Pacemaker Wolf-Parkinson-White syndrome Ventricular Arrhythmias Premature Ventricular Contractions Ventricular Tachycardia Ventricular Fibrillation Long QT syndrome Premature ventricular contractions → a site in the ventricle fires before the next wave of depolarization from the sinus node reaches the ventricle These are bizarre looking complexes Relatively benign → often occurs in healthy hearts during rest and exercise → occasional PVC's Causes: cigarettes, excessive coffee intake, lack of sleep, various mild toxic states, and emotional irritability Many PVC's may be markers of underlying cardiac disease such as infarcted or ischemic areas of the heart and can develop into lethal ventricular fibrillation Ventricular tachycardia → three or more consecutive ventricular beats at 100 bpm or faster Non-sustained ventricular tachycardia lasts less than 30 seconds Sustained ventricular tachycardia lasts more than 30 seconds Wide QRS complex, AV dissociation A serious condition → occurs due to considerable ischemic damage that is present in the ventricles → initiates the lethal condition of ventricular fibrillation Treatment: ICD, ablation, medications - quinidine Ventricular fibrillation → 250-350/minute Serious of all cardiac arrhythmias If not stopped within 1 to 3 minutes it is fatal It's not a coordinate contraction of all the ventricular muscle at once The ventricular chambers neither enlarge nor contract but remain in an indeterminate stage of partial contraction → loss of consciousness within 4 to 5 seconds due to lack of blood flow to the brain Causes: Sudden electrical shock of the heart Ischemia of the heart muscle Treatment: CPR Defibrillation Long QT syndrome Normal QT interval is less than half of the R-to-R interval at normal rates Usually hereditary due to mutations of sodium or potassium channel genes Acquired forms include hypomagnesemia, hypokalemia, or hypocalcemia, or excess amounts of antiarrhythmic drugs such as quinidine or some antibiotics Symptoms: no major symptoms present fainting and ventricular arrhythmias due to exercise, intense emotions, or when startled by a noise Treatment: magnesium sulfate for acute LQTS beta blockers, or ICD for long term LQTS Long QT syndrome Delayed repolarization of ventricular muscle can lead to ventricular arrhythmia called Torsades de pointes → if unresolved, it can lead to a deadly arrhythmia What to do if you think you have an undiagnosed Arrhythmia? Check your heart rate and blood pressure on regular basis Check your family history Screening → looking for disease before there are symptoms Seek medical help → your family doctor Your doctor will review your medical history including a physical exam He/she may send you for further testing including: An electrocardiogram (ECG) Exercise electrocardiogram (Stress test) Holter monitor How is Arrhythmia Treated? Life-style changes Avoiding stress, cutting out alcohol and caffeine, eating healthy diet, being more physically active Medications Digitalis/digoxin, beta blockers, calcium channel blockers Surgery or other non-surgical techniques Ablation Cardioversion therapy Implantable pacemaker Ventricular resection or remodeling THE END