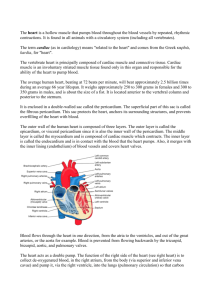
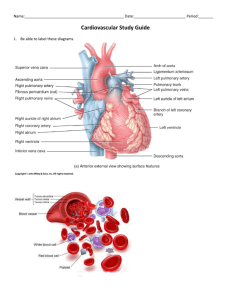
Pericardium and Heart
advertisement

Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 1 of 9 Pericardium and Heart I. II. Introduction A hand out of Trivia, History, Etc, of the Heart was provided. This is not testable material, so it won’t be in the scribe. Last week’s mystery radiograph was of a pneumothorax—identifiable because of the increased radio lucency. Pericardium (200) A. General 1. Fibroserous sac enclosing the heart and the roots of the great vessels 2. Restricts excessive heart movement 3. Serves as a lubricated container in which the different parts of the heart can contract 4. Lies in the middle mediastinum (middle plate), posterior to the sternum, from 2nd to 6th costal cartilage 5. Composed of fibrous and serous pericardium 6. Pericardial sac is fairly thin unless there’s longstanding pericarditis. B. Fibrous Pericardium (200, 201, 180, 203) 1. Strong fibrous outer layer of pericardium 2. Firmly attached below to central tendon of diaphragm 3. Fuses with outer coat of great blood vessels – Aorta – Pulmonary trunk – Superior and inferior venae cavae – Pulmonary veins C. Serous Pericardium (203) 1. Contains parietal—outside layer—and visceral layers 2. Parietal layer: Lines the fibrous pericardium, reflects around roots of great vessels, becomes continuous with the visceral layer 3. Visceral layer – Closely adhered to the heart—it gets on the 3 great vessels and goes to the heart. – Also called the epicardium – Fat is underneath the epicardium and on top of the myocardium (muscle) 4. Serous implies that it can secrete fluid D. Pericardial cavity 1. Slit-like space between the parietal and visceral layers 2. Contains a small film of serous (tissue) fluid called pericardial fluid 3. This fluid acts as a lubricant to facilitate movement of the heart in normal situations E. Pericardial Sinuses (203) 1. Oblique sinus - a recess on the posterior surface of the heart formed by the serous pericardium reflected around the large veins. It is bounded by veins. Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 2 of 9 2. Transverse sinus – posterior surface of heart, short passage between the reflection of serous pericardium around the aorta and pulmonary trunk and the reflection around the large veins Very important surgically. A clamp can be used here to stop blood flow through the pulmonary artery and the aorta. F. How many blood vessels penetrate the pericardial sac? A total of 8. III. Layers of Heart Wall (209) Outer surface of the heart is a fat depot. Amount of fat is often related to obesity of patient. A. Epicardium 1. Visceral layer of the serous pericardium 2. Often very fatty B. Myocardium 1. Composed mainly of cardiac muscle 2. Layer of contraction, forms bulk of heart C. Endocardium 1. Sheet of endothelium ( squamous epithelium) 2. Lines the heart chambers, covers the valves 3. Continuous with endothelium of blood vessels 4. Lines EVERYTHING inside the heart. IV. Heart Surface (201, 202) Calling these surfaces is a bit of a misnomer because the hearts we’ll look at are conical shaped. The surfaces appear on a heart that’s been embalmed and had time to flatten out. A. Surfaces 1. Sternocostal (anterior) surface – Formed mainly by right atrium and right ventricle, left border formed by left ventricle 2. Diaphragmatic surface – Formed by right and left ventricles, also the inferior surface of the right atrium 3. Base of the heart (posterior surface) – Formed mainly by the left atrium where the four pulmonary veins emerge – Heart does not rest on its base; it rests on the diaphragmatic surface 4. Apex of the heart – Formed by the left ventricle – Directed downward, forward, and to the left – At level of 5th left intercostal space, 3 1/2 inches from the midline (apex heart beat) B. Surface Features (201, 202) Blood vessels are found in the sulci. Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 3 of 9 1. Atrioventricular groove – Also called the coronary sulcus – Groove at the junction of the atria and ventricles – Contains right and left coronary arteries, coronary sinus 2. Anterior interventricular groove(sulcus) – Furrow between the right and left ventricles on the sternocostal surface – Contains anterior interventricular artery (left anterior descending artery, LAD) 3. Posterior interventricular groove ( sulcus ) – Between ventricles on diaphragmatic surface – Contains posterior interventricular branch of right coronary artery (posterior descending artery) C. Borders of the Heart 1. Important when examining radiographs 2. Right border > right atrium 3. Left border > left auricle and below by the left ventricle 4. Lower border > formed mainly by the right ventricle, also part of the right atrium and the apex by the left ventricle Note that: Most of the right side is the right atrium. The right ventricle is the predominant chamber seen in this view. The left border is the aortic knob, trachea, pulmonary artery, left atrium, and left ventricle. V. Chambers of the Heart A. Right Atrium (208) 1. Derived embryologically from sinus venosus 2. Sulcus terminalis , crista terminalis (SA node landmark) 3. Pectinate muscle (is the roughened part) 4. Openings – Superior vena cava—the SA node, pacemaker, lies just inside here – Inferior vena cava – Coronary sinus – Right atrioventricular orifice (regulated by tricuspid valve) 5. Interatrial septum Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 4 of 9 6. Fossa ovalis - a shallow depression, which is the site of the foramen ovale in the fetus – The floor of the fossa represents the persistent septum primum from the embryo heart 7. Right auricle 8. Site of atrioventricular (AV) node - found in the lower part of the interatrial septum just above septal cusp of tricuspid valve B. Right Ventricle (208) 1. Much thicker walls than atrium 2. Trabeculae carneae—meaty ridges – Papillary muscles—contract • Chordae tendineae - connect muscle to valve cusps; keep tricuspid valve from going into the wrong ventricle. You hear a hear murmur if the valve does not completely close. – Moderator band—conducts intrinsic nerve fibers to the right ventricular wall 3. Tricuspid valve (right atrioventricular valve) – Consists of three cusps formed by a fold of endocardium – Closes on contraction (like a parachute) 4. Pulmonary valve – Between right ventricle and pulmonary trunk – three semilunar cusps, open at contraction 5. Interventricular septum 6. Conus arteriosus ( infundimulum—hollowed out space ) is the opening of the pulmonary trunk C. Left Atrium (209)—larger chamber Note that the atrium and auricle are DIFFERENT 1. Similar to right atrium 2. Left auricle—smaller chamber 3. Pectinate muscle 4. Opening of pulmonary veins 5. Left atrioventricular orifice (regulated by the mitral or bicuspid valve). Mitral valve disease would be the most common type in the bodies we’re looking at. 6. Walls are 3x thicker than the right ventricle. If they’re greater than that (like 7:1 or 10:1), then it’s pathologic. 7. Left intraventricular bp is 6x higher 8. Trabeculae carnea , papillary m., and chordae tendineae 9. Left atrioventricular valve ( mitral or bicuspid valve) – Two cusps 10. Aortic valve – Contains three cusps, bulge to form aortic sinus – Two cusps contain openings to coronary arteries Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 5 of 9 11. The esophagus travels through the thorax to the abdomen and touches the left atrium. If there’s swelling in either the esophagus or the left atrium, there can be problems. VI. Pathway -Blood through Heart • Heart is actually two pumps side-by-side – Each pump serving a different circuit A. Right side of heart - pulmonary circuit 1. Oxygen-poor blood (CO2-rich) returning from the body enters the right atrium and passes passively into the right ventricle 2. then pumped to the lungs via the pulmonary trunk and pulmonary arteries (deoxygenated blood) 3. O2-poor (CO2-rich) blood in pulmonary arteries and O2-rich (CO2-poor) blood in pulmonary veins exact opposite of systemic circulation B. Left side of heart - systemic circuit 1. Freshly oxygenated blood enters the left atrium (from the lungs) then passes into the left ventricle 2. Then pumped into the aorta and transported via smaller systemic arteries to the body tissues where gas and nutrients are exchanged across capillary walls C. Pathway Pulmonary Circuit Systemic Circuit Right Atrium Left Atrium Right Ventricle Left Ventricle Pulmonary Trunk Pulmonary Arteries Capillary beds of Lungs Pulmonary Veins (to left atrium) Aorta Systemic Arteries Capillary beds of Body Tissue Systemic Veins/Venae Cavae (back to right atrium) VII. Heart Sounds (210) • During each heart cycle, 2 distinguishable sounds can be heard by auscultation Checked by Dr. John Leppi • Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 6 of 9 Described as “ lub - dup ” A. First Sound: lub 1. First sound, low-pitched and longer duration, occurs as the heart contracts and the AV valves close 2. Signifies the onset of systole (contraction) when ventricular pressure rises above atrial pressure 3. Associated with the palpable apex heart beat and arterial pulse B. Second Sound: dup 1. The second sound, shorter and higher-pitched, is caused by the sharp closure of the semilunar valves 2. Signify the onset of diastole (dilation or relaxation) C. Auscultation of the Heart Valve Note that these are not the anatomic sites of blood flow. They are the location where it’s easiest to pick up the sound. 1. Tricuspid - right side (also left) of the lower medial end of the body of the sternum, about 5th intercostal space—inferior margin of the sternum on left or right, side isn’t standard 2. Mitral - 5th left intercostal space, 3 1/2” from midline, at heart apex beat 3. Pulmonary - medial end of second left intercostal space (next to sternum) 4. Aortic - medial end of the second right intercostal space (next to sternum) Note that the pulmonary and aortic are opposite each other. VIII. Conducting System of the Heart (213) 1. Impulse causes the atria to contract first, followed by the contraction of both ventricles 2. Sino - atrial (SA) node - is site where heart muscle contraction is initiated, often called the pacemaker of heart • It is located at the upper part of the sulcus terminalis near opening of sup. vena cava into the right atrium 3. Ventricles fill by passive blood flow from the atria, and when almost full, atrial systole occurs (SA node) 4. Wave of contraction in the atria commences around the openings of large veins and “milks” blood toward the ventricles 5. Cardiac impulse now reaches the atrio -ventricular (AV) node • Atrioventricular (AV) node is located in the lower part of the atrial septum just above the attachment of the septal cusps of tricuspid valve 6. Impulses continue to the papillary muscles via the atrioventricular bundle (Bundle of His) 7. Impulse then travels to the right and left bundle branches (going to their respective ventricles) with fibers of the Purkinje plexus 8. Papillary muscles contract first, and take up the slack of the chordae tendinae 9. Next, the ventricles contract which closes the AV valves 10. The cardiac impulse traveling through the terminal bundle branches and their Purkinje fibers, ensures almost simultaneous contraction of the ventricles Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 7 of 9 IX. Nerve Supply of Heart (214) • Very difficult to dissect. • Innervated by sympathetic and parasympathetic fibers of autonomic nervous system via cardiac plexuses A. Sympathetic 1. Cervical and thoracic sympathetic cardiac n. from sympathetic trunk 2. Postganglionic fibers terminate at SA and AV nodes, cardiac m. fibers, and coronary arteries 3. Activation results in cardiac acceleration, increased force of contraction, dilation of coronary arteries 4. Some of the sympathetic fibers carry visceral afferents with them, so the body thinks things are happening on the outside of the body, when in reality, the problem with an organ inside. On the left, the intercostals brachial nerve is responsible for the ‘surface’ pain felt with heart attacks. B. Parasympathetic 1. Vagal cardiac n. from vagus (X) nerve 2. Postganglionic fibers terminate on SA and AV node, and the coronary arteries 3. Activation results in a reduction in the rate and force of contractions, and constriction of the coronary arteries X. Coronary Arteries (211, 204) A. Right coronary artery - arises from right aortic sinus 1. Branches – Can have quite a bit of variation; at times, the circulation is not balanced – SA nodal branch (off the atrial branch) – Marginal branch – Posterior interventricular branch (artery) 2. Also called the posterior descending artery B. Left coronary artery - arises from left aortic sinus 1. Branches – When dissecting, transect these every ½ inch to look for coronary heart disease. – Circumflex branch – Anterior interventricular branch (artery) • Also called left anterior descending (LAD) artery 2. Many variations occur in the coronary arteries 3. Anastomosis occur between terminal branches XI. Cardiac Veins 1. Coronary sinus 2. Great cardiac vein 3. Middle cardiac vein 4. Small cardiac vein 5. Anterior cardiac veins - drain directly into the right atrium Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 8 of 9 XII. Clinical Considerations A. Pericarditis 1. Inflamation of the pericardium – Might follow bacterial pneumonia – Hinders the production of serous fluid – Roughens the serous membrane surfaces – Beating heart creates a rustling sound as it rubs against the pericardial sac, called pericardial friction rub 2. May lead to painful adhesions in which the layers of the pericardium stick together, impeding heart activity 3. In severe cases, large amounts of inflammatory fluid seep into the pericardial cavity 4. This compresses the heart, limiting its ability to pump blood 5. Condition called cardiac tamponade 6. Treated by inserting needle into the pericardial cavity and draining off the fluid, called pericardiocentesis. The subxyphoid approach can be used: a needle is inserted into the sac at a 45° angle to the surface on the left side. B. Myocardial Ischemia 1. Inadequate blood supply to the myocardium 2. Narrowing of the coronary arteries due to atherosclerosis can cause a condition known as “angina pectoris” 3. Blood supply to myocardium is sufficient at rest, but inadequate when work load increases 4. Severe pain over the middle of the sternum often spreading to one or both arms, the root of the neck and even the jaw 5. Cardiac pain not felt in the heart, but is referred to skin areas (referred pain) supplied by corresponding spinal nerves 6. Supplied by the four intercostal nerves and the intercostobrachial n. (T2) C. Myocardial Infarction (MI) 1. Sudden insufficiency of arterial or venous blood supply can produce an area of necrosis of the myocardium 2. Usually resulting from an occlusion of a coronary artery 3. Complications: most deaths in early hours after MI are due to ventricular fibrillations or cardiac arrest D. Valvular Disease of the Heart 1. Inflammation of a valve can cause the edges of the valve cusp to stick together 2. Later, fibrous thickening occurs, followed by loss of flexibility and shrinkage (normally, edges are thin and flexible) 3. Narrowing ( stenosis ) and valvular incompetence (regurgitation) results 4. Rheumatic fever used to be a common cause of mitral valve stenosis – Caused from nodules formed on the valve cusp, which roughens them, causing irregular blood flow Checked by Dr. John Leppi Cardio #61 Tues, 01/21/03, 11am Dr. John Leppi Jennifer Uxer for Greg Hibbets Page 9 of 9 – Bloods builds up in left atrium and lungs – Producing pulmonary congestion and a strain on the right side of the heart – A murmur is produced as the atria contract and and blood is forced through the narrow mitral orifice just prior to ventricular contraction 5. Stenosis is more common in the pulmonary or aortic valves – Aortic valve stenosis – Edges of the valve are fused together forming a dome with a narrow opening – This causes extra work resulting in hypertrophy of the left ventricle – Produces a heart murmur 6. Aortic valvular incompetence – Results in aortic regurgitation – Produces a heart murmur – Also a collapsing pulse, one with a forcible impulse that immediately collapses • Heart murmurs most often indicate some type of valve problem