Introduction to Blood transfusion Competencies
advertisement

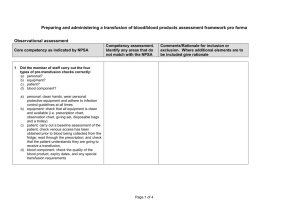
Introduction to Blood Transfusion Competencies Blood transfusion is a complex multi-step process involving personnel from diverse background with different levels of knowledge and understanding. In order to properly and safely accomplish their role in transfusion each individual needs to be trained to the appropriate level. This will very according to the particular task they need to perform as part of the process. Regardless of professional background the essential common element remains correct patient identification (ID) at every stage. A requirement of compliance with the Blood Safety and Quality Regulations 20051, which became UK law on 8th February 2005 is that all staff receive formal, documented training in blood transfusion practice for distribution and traceability of blood and blood components and in Adverse Event Reporting. The information in these competencies has been formally risk assessed against the competencies developed by the National Patient Safety Agency (NPSA) within their Safer practice Notice (14) Right Patient, Right Blood2 which states: “Formal assessment of the relevant competencies is required for nurses, midwives, medical staff, phlebotomists, healthcare, assistants, porters, operating department practitioners and other staff involved in blood transfusion process.” The risk assessment confirms that these materials are fit for the purpose as stated above. Further information can be obtained from: Specialist Practitioner of Transfusion 023 80 798910 Bleep 2463 Diana.agacy-cowell@suht.swest.nhs.uk. The appropriate knowledge and competencies can be found in:• • • understanding required to underpin these SUHT Blood Transfusion Policy Trust Infection Control Policy NMC Code of Professional Conduct Additional References: 1. The Blood safety and Quality Regulations 2005 SI 2005/50 2. National Patient Safety Agency (NPSA) Safer Practice Notice, Right Patient, Right Blood. http://www.npsa.nhs.uk/health/display?contentld=5298 3. NHS Knowledge and Skills Framework (KSF) October 2004 4. British Committee for Standards in Haematology (BCSH). The administration of blood and blood components and the management of transfused patients. Transfusion Medicine, 1999, 9, 227-238 5. www.transfusionguidelines.com Disclaimer The competency assessment is designed for use and deemed fit for purpose in its current format. The authors are not responsible for any subsequent local modifications. When using the competency assessment package it is the responsibility of the assessor to ensure that the documents are current and in date. The authors are not responsible for use of the training package or competency assessments by unauthorised persons. The record of competency relates to performance at the time of assessment and does not guarantee future performance. Blood Transfusion competency is linked to the Individual Learning Log. Once a member of staff has been deemed competent a record of the evidence of competence must be entered into the Individual Learning Log and reviewed at their annual appraisal or development review (for medical staff the appropriate process for their grade). Page 2 of 26 Blood Transfusion key facts When taking a sample, verbally check patient’s ID handwrite the bottle at the bedside copying the patient’s details from the patient’s wristband. Blood Transfusion Laboratory staff will reject all samples that are incorrectly labelled, illegible or have pre-printed addressograph labels! Before collecting or sending for a blood component carry out the pre-collection checklist: • Blood component is prescribed. • If patient requires pre-medication to avoid a reaction. • Is the venous access patent? • Do the baseline observations. 4 points of patient identification is required to collect blood components; Forename, surname, date of birth (DoB) and Hospital/NHS number. If the unit is being collected by ward staff use check the patient’s Transfusion Record (peach coloured) to the patient’s wristband and use Transfusion Record to collect the unit. If the request for collection is to the Portering Dept. again all 4 points of patient identification Blood should only be stored in the blood fridge, never in a domestic or drug fridge. Remember that you must fill in the laboratory register when removing red cells from a blood bank fridge. Put the date and time of removal and your initials along side the unit number you are collecting. Red cells can be returned to the blood bank fridge within 30mins, the return must be recorded on the laboratory register. Red cells should only be removed from the blood bank fridge if it is going to be used immediately. Blood is precious and it is expensive, a donor has taken the time to give blood, we should ensure that it is not wasted. All blood components should be transported in the ‘Blood in Transit’ bags provided or in blood boxes. When administering a transfusion, the checking procedure should be carried out by two qualified persons but separately (Individual checking). Patients should be transfused in an area they can readily be observed, ensure you give them a call bell. The blood must be checked at the bedside. Firstly check the patient’s ID verbally, check special requirements e.g. Irradiated, CMV negative. Check 14 digit donor number on NHSBT label to 14 digit donor number on unit identity label, these should be the same. Check the patient’s wristband, to the patient information printed on the unit identity tag. If these are correct the transfusion can proceed. The observations for a transfusion are as follows: • • • Baseline: Temp, pulse, blood pressure and respiratory rate Repeat at 15mins from start of transfusion End of the unit. Page 3 of 26 Red cells should be transfused over 2hours, unless the patient is a high risk of circulatory overload. If the patient has a minor reaction, e.g. rash or pyrexia less than 1.5 degrees above the baseline. Stop! The transfusion check it’s the correct blood, if it is treat symptoms. If the symptoms subside or do not get any worse recommence transfusion but at a slower rate, increase observations. Document in patients notes. If the patient’s temperature continues to rise after giving paracetamol, treat as a severe reaction. Stop! transfusion, Airway, Breathing, Circulation, send the unit of blood and giving set to the lab, collect urine sample, blood cultures (if patient gets a temperature) a cross-match sample, FBC sample, chemistry sample, coagulation sample and clotted sample. See page 5 for further information. ALWAYS REMEMBER, TRANSFUSION ERRORS ARE THE BIGGEST RISK TO PATIENTS. Page 4 of 26 Assessment Verification Personal Staff Details Name: Ward/Dept Job title: Band/Grade: Personal Staff Record Competence task Date sent for verification Key Skill Guidance Date Certified as competent If a tick is place under your grade you may need to take the corresponding competency task on the left. Renewal date Porter CS/ HCSW StN DR RN/ RM/ Th P ANAE Organising the receipt of blood/blood products Collecting blood/blood products Preparing to administer blood/blood products to patients and administering a transfusion of blood/ Blood products. Obtaining a venous blood sample. Quick Guide Staff Grade Min competency requirement key Porter Porter Student Nurse Registered Nurse/ Registered Midwives/ /Theatre practitioner StN Clinical Support Worker or Health Care Support Worker Doctor RN/Th P Anaesthetist Staff Grade Min competency requirement key CS /HCSW DR ANAE Mandatory Training Attendance Record Date Attended Update Due Date Page 5 of 26 Authorizing Signature Core blood competencies assessment framework Assessment criteria for organising the receipt of blood/blood products for transfusion This framework is for assessing staff’s ability to organise the receipt of blood/blood products for transfusion. Staff should be assessed after they have attended a local training course on this core task. Further information and training materials can be found at: www.npsa.nhs.uk This framework was developed by the National Patient Safety Agency (NPSA) to assess the core blood transfusion competence, BDS17 Organise the receipt of blood/blood products for transfusion. This workforce competence is linked to the Knowledge and Skills Framework dimensions developed by Skills for Health. The dimensions are Communication, Health and Safety, and Health and Well-being. How to use this competence assessment framework The framework should be completed whilst observing a member of staff organising the receipt of blood/blood products for transfusion. It is available from the local blood transfusion lead in every trust and is part of the NPSA’s Right patient, right blood initiative. Please note that when the competence assessment framework is used to evaluate the competence of porters, they do not have responsibility for verbal patient identification, and this aspect of the assessment is not applicable to them. It is important that the assessor informs the patient that the member of staff’s skills are being assessed as part of a three-yearly process. Page 6 of 26 Organising the receipt of blood/blood products for transfusion assessment framework pro forma Name of member of staff: Name of assessor: Job title/Band: Job title: Date of assessment: Observational assessment Core competency 1 Please put a tick or cross to show whether or not the member of staff completed the task Notes for assessors Confirm that the blood/blood product for transfusion is ready for collection Give a tick or cross for each point separately 2a Patient identification check Did the member of staff ask the patient to state their: a. Full name? b. Date of birth? Did the member of staff check: c. the detail provided with the information on the Transfusion Record (TR) d. match the information provided by the patient to information on the wristband or other attached identifier. Page 7 of 26 2b Patient identification check With an unconscious patient or those unable to verbally comply, did the member of staff check: a. the details on the wristband or other attached identifier were correct? b. the minimum dataset information of: • full name? • date of birth? • hospital number or other identification number? 3 Blood transfusion collection document: Transfusion Record for ward staff/Porter task sheet Did the member of staff check the TR to the patient’s wristband? Describe which points need to be exactly the same: a) the patient’s full name? b) date of birth? c) hospital or other identification number? d) Instruct person collecting to initial, date and time lab register? . 4 Did the member of staff identify an appropriate person to collect the blood/blood products for transfusion and ensure: a) there was clear communication about which blood/blood products to collect? b) there was clear communication about which patient the blood/blood products is for? (Porter collection) c) there was verbal confirmation on where the blood/blood product should be collected from? d) there was verbal instruction on the procedure to be carried out at the collection point? 5 Receipt of blood/blood products Did the member of staff respond promptly to the delivery of blood/blood products by: a) checking that the details on the delivered blood/blood products match the Transfusion Record b) ensuring that receipt of the blood was documented with their signature, time and date of receipt? (Porter delivery) All of the above must be achieved to pass the assessment Page 8 of 26 Knowledge assessment Does the member of staff know and understand the importance of: Using open-ended questions for patient identification? Why information on the; • Porter task sheet • TR must be complete? The potential risks in the blood component collection process? Why information should be cross-checked against the blood compatibility form attached to the blood component at the point of collection? Page 9 of 26 Assessment Record for the receipt of Blood components/products Assessor comments Candidates comments Assessor signature Date Print Name Candidate signature Date Print Name Having undertaken the above competency assessment the candidate achieved a: PASS REFERRAL Please circle the appropriate action If referred date for re-assessment Page 10 of 26 Core blood competencies assessment framework Assessment criteria for collecting blood/blood products for transfusion This framework is for assessing staff’s ability to collect blood/blood products for transfusion. Staff should be assessed after they have attended a local training course on this core task. Further information and training materials can be found at: www.npsa.nhs.uk This framework was developed by the National Patient Safety Agency (NPSA) to assess the core blood transfusion competency, BDS18 Collect blood/blood products for transfusion. This workforce competence is linked to the Knowledge and Skills Framework dimensions developed by Skills for Health (2004). Core 5 Quality Level 1; Indicators: a, b, c, d, e EF3 Transport and logistics Level 1; Indicators: a, b, c, d, e How to use this competence assessment framework The framework should be completed whilst observing a member of staff who is collecting blood/blood products for transfusion. It is available from the local blood transfusion lead in every trust and is part of the NPSA’s Right patient, right blood initiative. It is important that the assessor informs the patient that the member of staff’s skills are being assessed as part of a three-yearly process. Page 11 of 26 Collecting blood/blood products for transfusion assessment framework pro forma Name of member of staff: Name of assessor: Job title/Band: Job title: Date of assessment: Observational assessment Core competency Please put a tick or a cross to show whether or not the member of staff completed the task 1 Did the member of staff demonstrate effective use of health and safety measures by: a) washing their hands or using alcohol gel b) using personal protective equipment? c) adhering to other infection control procedures? 2 Documentation taken to the issue fridge or BT laboratory – Transfusion record/porter task sheet – contains required identifiers • • • • Forename Surname DOB Hospital no/NHS no. 3 Match details on the written/typed documentation with the patient information on the issue bank register and compatibility label attached to unit. 4 Full documentation is completed to include • Date of removal • Time of removal • Signature & initial 5 Take units immediately to the clinical area and according to local transport requirements. Page 12 of 26 Notes for assessors Give a tick or cross for each point separately. 6 Hand unit to appropriate member of staff a) Obtain a record of receipt to include the date, time and signature of member of staff b) (where an electronic tracking system is in place) demonstrating that they know how to maintain a secure ID throughout and showing this by scanning in and out correctly? 7 RETURNING BLOOD COMPONENTS • • • Date of return Time of return Signature & Initial All of the above must be achieved to pass the assessment Page 13 of 26 Knowledge assessment Did the candidate demonstrate an understand of the importance of the following points: Right blood – Right patient Action to take if blood is not in the fridge. Following correct transport procedures Leaving blood unattended Following correct procedure for return of blood and components Transfer to satellite fridge ( if not observed) Page 14 of 26 Assessment Record collecting of Blood components/products Assessor comments Candidates comments Assessor signature Date Print Name Candidate signature Date Print Name Having undertaken the above competency assessment the candidate achieved a: PASS REFERRAL Please circle the appropriate action If referred date for re-assessment Page 15 of 26 Core blood competencies assessment framework Assessment criteria for preparing to administer blood/blood products to patients and administering a transfusion of blood/blood products This framework is for assessing staff’s ability to prepare and administer blood/blood products to a patient. Staff should be assessed after they have attended a local training course on this core task. Further information and training materials can be found at: www.npsa.nhs.uk This framework was developed by the National Patient Safety Agency (NPSA) to assess the core blood transfusion competencies, BDS19 Prepare to administer blood/blood products to patients and BDS20 Administer a transfusion of blood/blood products. This workforce competence is linked to the Knowledge and Skills Framework dimensions developed by Skills for Health. The dimensions are Communication, Health and Safety, and Health and Well-being. Core 5 Quality Level 1; Indicators: a, b, c, d, e HWB7 Interventions and treatments Level 1; Indicators: a, b, c, d, e How to use this competence assessment framework The framework should be completed whilst observing a member of staff who is involved in preparing and administering blood and/or blood products. It is available from the local blood transfusion lead in every trust and is part of the NPSA’s Right patient, right blood initiative. It is important that the assessor informs the patient that the member of staff’s skills are being assessed as part of a three-yearly process. Page 16 of 26 Preparing and administering a transfusion of blood/blood products assessment framework pro forma Name of member of staff: Name of assessor: Job title/Band: Job title: Date of assessment: Observational assessment Core competency Please put a tick or cross to show whether or not the member of staff completed the task Did the member of staff carry out the four types of pre-transfusion checks correctly: 1 a) b) c) d) personal? equipment? patient? blood component? a) personal: clean hands, wear personal protective equipment and adhere to infection control guidelines at all times b) equipment: check that all equipment is clean and available (i.e. Transfusion Record, giving set, disposable bags and a trolley) c) patient: prior to blood being collected from the fridge; carry out a baseline assessment of the patient; check venous access has been obtained; read through the prescription; and check that the patient understands they are going to receive a transfusion, d) blood component: check the quality of the blood product, expiry dates, and any special transfusion requirements Page 17 of 26 Notes for assessors Give a tick or cross for each point separately. 2 Patient identification for the conscious patient Did the member of staff ask the patient to state their: a) full name? b) date of birth? Did the member of staff check: c) the details on the wristband or other attached identifier were correct? 3 Patient identification for unconscious patients or patients unable to verbally respond: Did the member of staff check: a) the details on the wristband or other attached identifier: full name? date of birth? hospital number? b) To the information on the blood or blood product? 4 Did the member of staff record the patient’s vital signs? a) b) c) d) 5 blood pressure? temperature? pulse rate? resp rate? Administering the blood transfusion Did the member of staff ensure that the blood transfusion was: a) completed within four hours of it leaving the fridge, OR b) within 30 minutes for platelets & Fresh Frozen Plasma? Did the member of staff c) record the patient’s vital signs prior to starting the transfusion? d) monitor the patient’s vital signs 15 minutes after starting the transfusion? e) dispose of equipment safely? f) monitor the patient’s vital signs on completion of the blood transfusion? Page 18 of 26 6 Documentation Did the member of staff record the following information in the patient’s notes: a) date? b) start time? c) stop time of the transfusion? Did the member of staff: d) complete the traceability documentation in accordance with national law? All of the above must be achieved to pass the assessment Knowledge assessment Does the member of staff know and understand the importance of: Using open-ended questions for patient identification? The timescales for administering blood and/or blood product safely after it had been collected from the fridge? Correct procedure if unconscious patient or unable to give verbal identification? The risks associated with checking the blood compatibility form against the blood product instead of the information on the wristband? Monitoring the patient’s vital signs throughout the transfusion process? Page 19 of 26 Assessment Record for Administration of Blood and Blood Components Assessor comments Candidate comments Assessor signature Date Print Name Candidate signature Date Print Name Having undertaken the above competency assessment the candidate achieved a: PASS REFERRAL Please circle the appropriate action If referred date for re-assessment Page 20 of 26 Core blood competencies assessment framework Assessment criteria for obtaining a venous blood sample This framework is for assessing staff’s ability to obtain a venous blood sample. Staff should be assessed after they have attended a local training course on this core task. Further information and training materials can be found at: www.npsa.nhs.uk This framework was developed by the National Patient Safety Agency (NPSA) to assess the core blood transfusion competence, Obtain a venous blood sample. This workforce competence is linked to the Knowledge and Skills Framework dimensions developed by Skills for Health. The dimensions are Communication, Health and Safety, and Health and Well-being. Core 5 Quality Level 1; Indicators: a, b, c, d, e HWB6 Assessment and treatment planning Level 1; Indicators: a, b, c, d, e HWB8 Biomedical investigation and intervention Level 1: Indicators: b, e How to use this competence assessment framework The framework should be completed whilst observing a member of staff obtaining a venous blood sample. It is available from the local blood transfusion lead in every trust and is part of the NPSA’s Right patient, right blood initiative. It is important that the assessor informs the patient that the member of staff’s skills are being assessed as part of a three-yearly process. Page 21 of 26 Obtaining a venous blood sample assessment framework pro forma Name of member of staff: Name of assessor: Job title/band: Job title: Date of assessment: Observational assessment Core competency Please put a tick or a cross to show whether or not the member of staff completed the task 1 Did the member of staff check for each of the following on the request form: Notes for assessors Give a tick or cross for each point separately a) full name? b) date of birth? c) hospital number? Did the member of staff: d) sign and write their contact details to show who had taken the sample? e) print their name to show who had taken the blood sample? . 2 Did the member of staff bleed only one patient at a time? 3a Patient identification for conscious patient Did the member of staff ask the patient to state their: a) full name? b) date of birth? Did the member of staff check: c) details on the wristband or other attached identifier? d) The information on the wristband against that on the request card? Page 22 of 26 Give a tick or cross for each point. 3b Patient identification for unconscious patient or patient unable to verbally respond Did the member of staff check details on the wristband or other attached identifier? a) full name? b) date of birth? c) hospital number? Did the member of staff check the information on the wristband with the transfusion request card and to at least another patient document e.g. Prescription Drug Transfusion Record? Can the member of staff describe the trust’s policy for identifying unconscious patients? 4 Personal checks Did the member of staff wash their hands? Did the member of staff use personal protective equipment? 5 Taking the venous blood sample Did the member of staff: a) prepare the skin properly? b) use the tourniquet (disposable) appropriately? c) minimise discomfort for the patient? d) take blood appropriately if a transfusion is being carried out alongside other sampling procedures? e) monitor the patient’s responses? f) remove needles using an appropriate technique? g) apply a dressing at the end of the procedure? If the last two questions are not applicable to the patient from whom the sample has been taken, can the member of staff say what they would do in these circumstances? Page 23 of 26 6 Labelling the venous blood sample Did the member of staff label the venous blood sample as soon as it was taken before leaving the patient’s side? Does the label include the following information: a) full name? b) date of birth? c) hospital number? d) gender? e) date? f) the member of staff’s signature and contact details? 7 Packaging and documentation Did the member of staff take the blood sample to the correct collection point? If the sample was urgent were the appropriate steps followed as per Blood Transfusion policy Did the member of staff record the following information in the patient’s notes: a) why the sample had been taken? b) when the sample was taken? c) who took the sample? All of the above must be achieved to pass the assessment Page 24 of 26 Knowledge assessment Does the member of staff know and understand the importance of: using open-ended questions for identifying patients? not using pre-labelling bottles? correct procedure if patient is unconscious or unable to give verbal identification? the risks created if more than one patient is bled at a time? correct action to take if the information identifying a patient is missing? Page 25 of 26 Assessment Record for obtaining a venous blood sample Assessor comments Candidates comments Assessor signature Date Print Name Candidate signature Date Print Name Having undertaken the above competency assessment the candidate achieved a: PASS REFERRAL Please circle the appropriate action If referred date for re-assessment Page 26 of 26