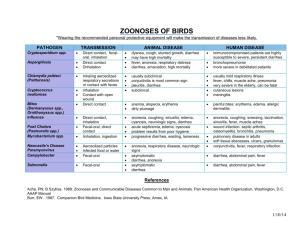
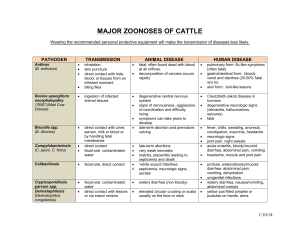
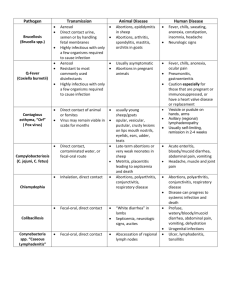
Gastrointestinal Tract
advertisement
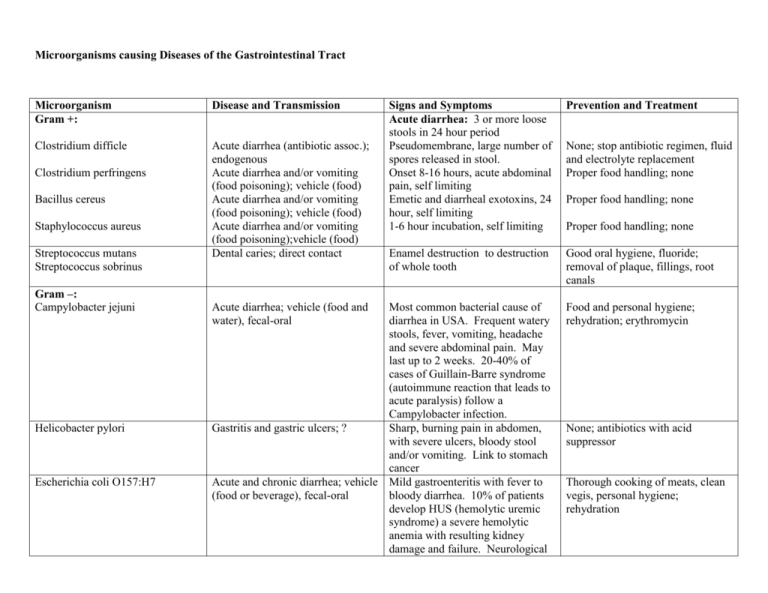
Microorganisms causing Diseases of the Gastrointestinal Tract Microorganism Gram +: Disease and Transmission Clostridium difficle Acute diarrhea (antibiotic assoc.); endogenous Acute diarrhea and/or vomiting (food poisoning); vehicle (food) Acute diarrhea and/or vomiting (food poisoning); vehicle (food) Acute diarrhea and/or vomiting (food poisoning);vehicle (food) Dental caries; direct contact Clostridium perfringens Bacillus cereus Staphylococcus aureus Streptococcus mutans Streptococcus sobrinus Gram –: Campylobacter jejuni Helicobacter pylori Escherichia coli O157:H7 Acute diarrhea; vehicle (food and water), fecal-oral Signs and Symptoms Acute diarrhea: 3 or more loose stools in 24 hour period Pseudomembrane, large number of spores released in stool. Onset 8-16 hours, acute abdominal pain, self limiting Emetic and diarrheal exotoxins, 24 hour, self limiting 1-6 hour incubation, self limiting Prevention and Treatment Enamel destruction to destruction of whole tooth Good oral hygiene, fluoride; removal of plaque, fillings, root canals Most common bacterial cause of diarrhea in USA. Frequent watery stools, fever, vomiting, headache and severe abdominal pain. May last up to 2 weeks. 20-40% of cases of Guillain-Barre syndrome (autoimmune reaction that leads to acute paralysis) follow a Campylobacter infection. Gastritis and gastric ulcers; ? Sharp, burning pain in abdomen, with severe ulcers, bloody stool and/or vomiting. Link to stomach cancer Acute and chronic diarrhea; vehicle Mild gastroenteritis with fever to (food or beverage), fecal-oral bloody diarrhea. 10% of patients develop HUS (hemolytic uremic syndrome) a severe hemolytic anemia with resulting kidney damage and failure. Neurological None; stop antibiotic regimen, fluid and electrolyte replacement Proper food handling; none Proper food handling; none Proper food handling; none Food and personal hygiene; rehydration; erythromycin None; antibiotics with acid suppressor Thorough cooking of meats, clean vegis, personal hygiene; rehydration Salmonella Acute diarrhea; vehicle (food or beverage, fecal-oral Shigella Acute diarrhea; fecal-oral, direct contact Vibrio cholerae Acute diarrhea; vehicle (water and some foods), fecal-oral DNA viruses: Hepatitis B virus RNA viruses: Hepatitis A virus Hepatitis C virus Hepatitis E virus Paramyxovirus symptoms-blindness, seizure and stroke are more likely in children under the age of 5 and the elderly. Enteric fever or gastroenteritis. High fever and septicemia in severe cases. Generally mild with vomiting, non-bloody diarrhea, cramping. Last 2-5 days. Shiga toxin leads to dysentery (frequent bloody stools, abdominal pain and tenesmus-the constant urge to defecate Vomiting, copious watery feces. “rice water stool”-filled with mucus, nonodorous. Severe fluid and electrolyte loss leads to hypovolemic shock and mortality is 55% without treatment. Takes a very large inoculums to cause disease however. Food and personal hygiene; rehydration Food and personal hygiene; rehydration Water hygiene; rehydration, tetracycline Chronic liver infection, liver cancer Jaundice, hepatomegaly, ascites, (with hep D), death; Parenteral bleeding in skin and internal (blood), direct (sexual), passage organs, coma through birth canal HBV vaccine, safe sex practices; interferon Infectious hepatitis; fecal-oral Vaccine; immunoglobulins Liver infection; parenteral (blood), direct (body fluids) Enteric hepatitis; fecal-oral Mumps; droplet contact Fever, nausea, anorexia, jaundice, 99% recovery Chronic infection and liver disease, cancer and death Mild except in 20% of pregnancies where fatal Incubation 2-3 weeks, fever, rhinorrhea, myalgia, malaise, parotitis. Viral invasion to testes, ovaries, thyroid, pancreas, meninges, heart and kidney. Avoid exposure; interferon Vaccine; immunoglobulins MMR vaccine; supportive Rotavirus Protozoa: Entamoeba histolytica Giardia lamblia Helminths: nematodes Ascaris lumbricoides Enterobius vermicularis Necator americanus Trichinella Cestodes: Taenia solium Trematodes: Shistosoma mansoni or japonicum Acute diarrhea;fecal-oral, vehicle, fomite Usually complete recovery. Infantile gastroenteritis, 50% of all diarrhea in children. Usually self limiting Chronic diarrhea; vehicle, fecaloral Dysentery Greasy, malodorous stool. Water and personal hygiene; antiprotozoan drugs Intestinal distress; vehicle (soil, fecal-oral). Self-inoculation Most common nematode infection globally. Loeffler’s syndromefever, dry cough, SOB. With high burden, nausea, vomiting, intestinal obstruction. Pinworm. Most common parasitic worm in USA. Perianal itching. Hookworm, second most common nematode infection globally. Chronic anemia, ground itch, Loeffler’s syndrome. 1st symptoms mimic flu with diarrhea, nausea, abdominal pain, fever and sweating. 2nd phase, puffy eyes, intense myalgia and arthralgia, SOC and eosinophilia. Hygiene; antihelminthics Intestinal distress; vehicle (pork), fecal-oral Not many symptoms. Vague pain in abdomen and nausea in some. Presence of eggs and proglottids in stool. Proper cooking of meat, avoid pig feces; antihelminthics Shistosomiasis; vehicle (contaminated water) “swimmer’s itch”, fever, chills, diarrhea and cough. Severehepatoslenomegaly and bladder obstruction Water sanitation; antihelminthics Intestinal distress; vehicle (food and water), self inoculation Intestinal distress; vehicle (soil) Muscle and neurological symptoms; vehicle (food) Oral vaccine; rehydration Hygiene; antihelminthics Sanitation; antihelminthics Proper cooking of meats; antihelminthics and steroids Defenses & Normal Microbiota of CVS and Lymphatics Defenses Oral cavity: IgA, lysozymes, lactoferrin, saliva, tonsils Upper GI: IgA, HCl, GALT Lower GI: IgA, GALT (Peyer’s patches), bile, enteric bacteria Normal Microbiota Streptococcus, Moraxella, Bacteroides,Actinomyces, Treponema, Candida, Entamoeba, Haemophilus Sparsely populated (Helicobacter pylori) Bacteroides, Bifidobacterium, Streptococcus, Clostridium, Lactobacillus, Escherichia, Enterobacter, Candida, Entamoeba, Trichomonas Virulence factors: attachment structures, acid production, urease, effacement, endotoxins, intracellular growth, latency, syncytia, exotoxins, invasiveness, induction of hypersensitivity reaction, antigenic “cloaking”