Oral health in pre-school children with asthma
advertisement

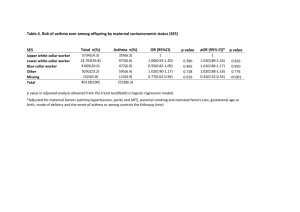
Oral health in pre-school children with asthma MALIN STENSSON1,4, LILL-KARI WENDT1,2, GÖRAN KOCH1, GÖRAN OLDAEUS3 & DOWEN BIRKHED4 1 Department of Paediatric Dentistry, The Institute for Postgraduate Dental Education, Jönköping, 2Department of Natural Science and Biomedicine, School of Health Sciences, Jönköping University, Jönköping, 3Paediatric Department, County Hospital, Ryhov, Jönköping, 4Department of Cariology, Institute of Odontology, Sahlgrenska Academy at Göteborg University, Sweden Correspondence to: Malin Stensson, Department of Paediatric Dentistry The Institute for Postgraduate Dental Education, Box 1030, SE-551 11 Jönköping, Sweden E-mail: malin.stensson@lj.se Declaration of interest This study has no conflict of interest. 2 Objective. The aim of the present study was to investigate oral health and its determinants in 3- and 6-year-old children with asthma. Methods and Subjects. Caries and gingivitis were examined in 127 asthmatic (all children with asthma in a selected area and born during a specific time period) and 117 matched, healthy control children.The parents were interviewed regarding various oral health-related factors. Results. The mean dfs (± standard deviation) in the 3-year-olds with asthma was 1.4 ± 3.2 compared with 0.5 ± 1.2 in the controls (P < 0.05). The corresponding figures for the 6-yearolds were 2.5 ± 3.9 and 1.8 ± 2.8. The 3-year-old asthmatic children had more gingival bleeding than healthy controls (P < 0.05). There were no significant differences in gingivitis in the 6-year-olds. Asthmatic children reported higher consumption of sugar-containing drinks and were more frequently mouthbreathers than healthy children (P < 0.05). In 3-year-old children with asthma and immigrant background, the mean dfs was higher compared with immigrant children in the control group (P < 0.01). Conclusion. The results indicate that pre-school children with asthma have higher caries prevalence than healthy children. The factors discriminating for caries in asthmatic children are higher intake of sugary drinks, mouthbreathing and immigrant background. 3 Introduction Asthma is one of the most common chronic medical conditions in childhood and it has steadily increased during the last two decades [1, 2]. The prevalence of asthma in the world displays large variations. The International Study of Asthma and Allergies in Childhood [ISAAC] shows that the highest rates are found in Australia, Peru, New Zealand, Singapore and the United Kingdom while the lowest are in Albania and Russia [3]. In reports from the Swedish Council on Technology Assessment in Health Care (SBU), about 20% of children under 2 years of age and about 10% of schoolchildren are affected by asthma symptoms [4]. Before puberty, the disease is more common in boys than in girls, whereas the gender incidence is equal after puberty [5]. In spite of the increasing prevalence of asthma only a limited number of studies have investigated oral health in pre-school children during the last 20 years and the results are somewhat conflicting. Some authors have reported a correlation between childhood asthma and dental caries in pre-school children [6-13], while others have found no such connection [14-16]. Eloot et al. [17] found that neither the length of the disease period in 3 to17-year-old children with asthma nor the medication or the severity of the asthma disease had a significant effect on the risk of developing caries or gingivitis. In studies by Ryberg et al. [12, 13], however, it was shown that asthmatic children who medicated with 2 agonists had a decreased saliva secretion rate and increased levels of lactobacilli and mutans streptococci, in addition to more caries lesions, compared with healthy children. Mc Derra et al. [8] found that 4- to 10-year-old children with asthma had more plaque, gingivitis and calculus compared with healthy controls. The lack of consensus in earlier studies of pre-school children could perhaps be attributed to differences in asthma severity or asthma medication, small samples or inconsistent age groups. 4 The aim of the present investigation was therefore to study oral health and its determinants in one group of 3-year-old children and one group of 6-year-old children with asthma, with special reference to asthma, severity, period of exposure to medication and mouthbreathing. Subjects and methods The study was approved by the Ethic committee at Linköping University, and informed consent was given by the parents or care-givers before the children were examined. Participants Children with asthma were selected from the Department of Paediatrics at the County Hospital, Ryhov, Jönköping, and from three child welfare centres in the Municipality of Jönköping, Sweden. The participants comprised all the 3-year-old children (n = 70) with asthma, born between April 2001 and January 2002, and all the 6-year-old children (n = 70), born between April 1998 and April 1999. Furthermore, two age- and gender-matched control groups were randomly selected from the County Council’s register of persons residing in the Municipality of Jönköping. The control group consisted of 3-year-olds (n = 70) and 6-year-olds (n = 70) without a diagnosis of asthma (status were confirmed by the parents). The age of the children at the time of the dental examinations was 3-year (±2 months). and 6-year (±2 mounts). Four children in the 3-year-old asthma group and 8 in the 3-year-old control group dropped out of the study. The corresponding figures for the 6-year-olds were 8 and 14 respectively. Moving out of the area or unwillingness to participate were the main reasons for dropouts in both age groups. Of the 6-year-olds, one child in the control group was being treated at a specialist clinic of paediatric dentistry and was therefore excluded. Two 6-year-old children (one with asthma and one control) were excluded because of other chronic diseases. The final 5 group of 3-year-olds with asthma therefore comprised 66 children, while 61 of the 6-year-old children were asthmatics. The corresponding figures for the control groups were 62 and 55 respectively. The girl/boy ratio in the asthma groups was 16/50 among the 3-year-olds and 23/38 among the 6-year-olds. The corresponding figures for the control groups were 13/49 and 25/30 respectively. Preventive programmes Children and adolescents living in the County of Jönköpings take part in a basic dental preventive programme starting at 1 year of age. The parents of the children are informed about preventive measures and are recommended to brush their children’s teeth with fluoridated toothpaste twice a day. Furthermore, individually intensified preventive programmes are designed for children with special needs, such as a high caries risk or mental or physical disabilities. Classification of children with asthma The asthmatic children were divided into four groups by a senior paediatrician, according to the classification of severity in the Swedish guidelines on the management of asthma, Swedish Paediatric Society, Section of Paediatric Allergy, as follows: Mild: 3-year-olds (n = 49), 6-year-olds (n = 43)- “Exacerbations are rare and symptoms at night uncommon ( once a month). No use of inhaled steroids and only intermittent use of short-acting 2 agonists”. Moderate: 3-year-olds (n = 13), 6-year-olds (n = 15)“Exacerbations are more frequent and symptoms at night more common (2-3 times a month). Periodic use of inhaled steroids in low to moderate doses (≤ 400 g/day) in combination with short-acting 2 agonists”. Severe: 3-year-olds (n = 3), 6-year-olds (n = 3)- 6 “Exacerbations weekly and regular use of inhaled steroids 100-400 g/day and in combination with long-acting 2 agonists or leukotriene receptor antagonists”. Very severe: 3year-olds (n = 1), 6-year-olds (n = 0)-“Exacerbations weekly and symptoms every day. Regular use of inhaled steroids 400-800 g/day in combination with long-acting 2 agonist or leukotriene receptor antagonists”. According to the length of exposure time to the asthma drugs, the children were divided into two groups: a) children with exposure for ≤ 2 years and b) children with exposure for > 2 years. According to the regularity of inhaled steroid medication, the children were divided into two groups: a) intermittent use in periods ≥ 1 time/day and b) regular use daily ≥ 1 time/day. Methods Clinical examination All the children were examined by one of the authors (MS) at the children’s ordinary Public Dental Service (PDS) clinics (n = 10). Before the start of the study, the examiner was calibrated to an experienced dentist in terms of diagnostic criteria. Each examination took 3045 minutes and was performed with a mirror, probe and under optimal light conditions. Caries. Both initial and manifest caries lesions were diagnosed on all surfaces in the 3year-olds. In order to avoid interference with exfoliated teeth, initial and manifest caries were only diagnosed on primary molars and canines in 6-year-olds. Clinically visible initial caries was defined as “a demineralised surface with a chalky appearance”. Clinically visible manifest caries was registered according to the criteria formulated by Koch [18] and defined as “the minimal level that could be verified as cavities by gentle probing which, on probing in fissures, caused the probe to get stuck at slight pressure”. 7 Oral hygiene. Gingival inflammation was diagnosed as “bleeding” or “no bleeding” after gentle probing according to Löe and Silness [19] in all primary tooth surfaces in 3-year-olds (80 surfaces) and in all primary molars and canines in 6-year-olds (60 surfaces). Plaque was measured after drying the teeth with air as “visible” or “no visible” plaque, according to Silness and Löe [20]. Plaque was registered buccally on primary upper incisors in the 3-yearolds (4 surfaces) and in all surfaces in primary molars and canines in the 6-year-olds (60 surfaces). Radiographic examination Two posterior bitewings were taken in 6-year-olds with a special film holder (Kwik-bite Trollhätteplast, Trollhättan, Sweden). Initial proximal caries was defined as “a caries lesion in the enamel that has not reached the enamel-dentine junction or a lesion that reaches or penetrates the enamel-dentine junction but does not appear to extend into the dentine”. Manifest proximal caries was defined as “a caries lesion that clearly extends into the dentine”. The bitewings were analysed by two of the authors by using a viewing box and binoculars according to Mattsson [21]. One of the examiners was not aware of the group to which the child belonged. In the event of disagreement the findings from the radiographs were discussed until consensus was reached. Saliva sampling A paraffin-stimulated whole saliva sample was collected in the 6-year-olds. The sample was shaken on a mechanical mixer for 30 sec and serial diluted in 0.05 M phosphate buffer (pH 7.3). 25-µl portions were plated in duplicate on mitis salivarius with bacitracin (MSB) agar for the growth of mutans streptococci and in Rogosa Selective Lactobacilli (SL) agar for the growth of lactobacilli. The Rogosa SL agar plates were incubated aerobically at 37°C for 3 8 days. The MSB agar plates were incubated in candle jars at 37°C for 2 days. The number of colony forming units (CFU) of mutans streptococci was counted on the MSB agar and identified by their characteristic colony morphology. All CFU in Rogosa SL agar were considered to be lactobacilli. The number of CFU was transformed to logarithms before the statistical analysis. The buffer capacity of saliva was estimated by using the Dentobuff Strip test (Orion Diagnostica, Espoo, Finland), according to the manufacturer’s instructions. Interview In connection with the clinical examination, a semi-structured interview was performed. The parent/caregiver of the child was interviewed about prior and current medication, mode of administration and duration of asthma medication, immigrant background (defined as at least one parent born outside the Nordic countries), tooth-brushing habits, use of fluorides, mouthbreathing during the last year and dietary habits (drinking during the night and number of daily intakes of caries-risk products). The intake frequency of each risk product was registered according to Wendt and Birkhed [22] and each risk product was assigned “points” corresponding to its regularity: 7 points indicate once a day, 1 point once a week and so on. The sum of the points for each child was then divided by seven to calculate the average number of intakes of caries-risk products per day. Statistical analysis The data were analysed using the Statistical Package for the Social Sciences, SPSS 13.0 software program (SPSS Inc., Chicago, IL, USA). After the computation of univariate statistics, bivariate analyses explored the association of asthma status and caries experience, while chi-square tests were used to test the association with categorical dependent variables. Mann-Whitney U tests were used for continuous dependent variables. Univariate and multiple 9 logistic regression analyses were performed to explore the effects on caries of dietary habits, presence of plaque, bleeding on probing (gingivitis), mouthbreathing, immigrant status, period of exposure to medication, regular use of asthma drugs and severity of the disease. The level of significance was set at P < 0.05. Results Caries The results are shown in Table 1. There was a general trend for asthmatic children to have somewhat higher caries prevalence than children without asthma, but it was only significant for the 3-year-olds. The caries data relating to children who dropped out of the study were collected from records from the children’s ordinary PDS-clinics and revealed that 75% of the 3-year-olds were caries free, which is in accordance with the children participating in the study 71% of the 3-year-olds in the asthmatic group and 81% of the 3-year-olds in the control group were caries free. The corresponding figures for the 6-year-olds were 66%, 51% and 56% respectively. Oral hygiene and dietary habits Data are shown in Table 2. There was no significant difference when it came to the frequency of tooth brushing between asthmatic and non-asthmatic children and all the children used fluoridated dentifrice. Mouthbreathing The results are shown in Table 2. There was a general trend for asthmatic children to have a somewhat higher prevalence of mouthbreathing than children without asthma, although it was not significant for 6-year-olds. In 3-year-olds with asthma and frequent mouthbreathing, the mean dfs was 3.1 ± 5.0 compared with 0.8 ± 1.9 in asthmatic children without mouthbreathing 10 (P < 0.05). At 6 years of age, there was no significant difference in caries prevalence between mouthbreathers and non-mouthbreathers. Immigrant status The results are shown in Table 2. Immigrant children with asthma had a mean dfs of 2.0 ± 2.8 compared with 0.3 ± 0.7 for children in the control group with an immigrant background (P < 0.01). In 6-year-old immigrants with asthma, the mean dfs was 3.5 ± 5.3 compared with 0.4 ± 0.8 in immigrants in the control group (P = 0.1). Salivary and microbiological factors One 6-year-old child in the asthma group and 7 in the control group did not cooperate with the saliva sampling. Of the remaining 108 children, no mutans streptococci or lactobacilli were detected in about 60% of the children the same results in both groups. The mean numbers (log CFU/ml) of mutans streptococci were 4.66 ± 0.71 in the asthma group and 4.73 ± 1.61 in the control group. The corresponding figures for lactobacilli were 3.60 ± 0.97 and 3.87 ± 1.78 respectively. The distribution of buffer capacity classes according to Dentobuff was about the same in the two groups: only 1 child in the asthma group and 3 in the control group displayed a low buffering capacity. None of the differences relating to the microbiological and salivary factors was statistically significant. Medication The most common mode of administering the asthma drugs was by inhalation using a metered dose inhaler in both age groups. Inhalation using a dry powder inhaler occurred more frequently in the 6-year-olds than in the 3-year-olds. The mean dfs was 2.6 ± 5.5 for 3-yearold children who medicated regularly with steroids (n = 22) compared with 1.2 ± 1.9 for 3- 11 year-olds who medicated intermittently (n = 40). Among the 6-year-olds, the corresponding figures were 3.0 ± 5.0 (n = 29) compared to 2.0 ± 3.0 (n = 32). None of the differences were statistically significant. The mean period of exposure of asthma medication was 21 months for the 3-year-olds and 40 months for the 6-year-old children. There was no statistically significant difference in mean dfs in children who had medicated for more than 2 years compared with children who had medicated for 2 years or less. Severity of the disease In the 3-year-old children with mild asthma (n = 49), the mean dfs was 1.1 ± 2.1 compared with 5.5 ± 9.7 in children with severe/very severe asthma (n = 4). The corresponding figures for 6-year-olds were 2.4 ± 3.4 (n = 43) and 3.7 ± 6.4 (n = 3), respectively. The differences were not statistically significant. Multiple logistic regression analyse The results of the multiple logistic regression analyses for different outcome variables in the asthma groups are presented in Table 3. Variables that indicated an increased risk of caries development in 3-year-olds with asthma were sugary drinks more than once a day, presence of plaque, mouthbreathing and immigrant background. In the stepwise logistic regressions analyse for 6-year-olds with asthma, the presence of plaque was the only variable that indicated an increased risk of caries development. In a similar analysis performed for children in the control groups, no independent variable showed an increased risk of caries development. 12 Discussion The relationship between the asthmatic condition and caries prevalence in pre-school children is difficult to examine. The asthma disease, its severity and the medication often fluctuate over time according to the seasons. Furthermore, the start of the asthmatic disease is difficult to assess. Despite this, the present study has revealed a difference in caries prevalence in asthmatic and non-asthmatic pre-school children, even though it was not significant for 6year-olds. The difference between the two age groups, 3 and 6 years of age, might be due to the fact that the group of asthmatic 3-year-olds is more homogeneous in terms of the onset of the disease than the group of asthmatic 6-year-olds. One of the strengths of the present study is that, unlike most other studies [7-9, 11] conducted in pre-school children with asthma, this study comprised all the children registered as having asthma within the selected geographical areas and the children were all 3 or 6 years of age at time for examination. One limitation, however, is that all participating children came from geographical areas with a high socioeconomic profile and thereby had a lower caries prevalence than a random sample of preschool children from the Municipality of Jönköping [23]. A series of factors could influence the statistical outcome of the present study. One such factor could be the skewed distribution of caries prevalence and another could be the large standard deviation, which results in difficulty obtaining statistically significant differences. However, the present investigation has revealed differences in caries prevalence in children with and without asthma. This is in line with previous studies [7-13], which have shown a correlation between childhood asthma and dental caries. In a study by Wogelius et al [24] comparing children with asthma-drug use with children without asthma-drug use, that ”found no increased risk of dental caries in the deciduous teeth, while in the newly erupted permanent teeth, the risk was increased” .Furthermore, in the present study 9% of the 3-year-old asthmatic children had 6 or more caries lesions, compared with none in the control group, and 13 10% of the 6-year-olds with asthma had more than 9 caries lesions, compared with 2% of the children in the control group (Table 1). This indicates that asthma triggers caries development in asthmatic children. The multiple logistic regression analyse showed that sugary drinks, presence of visible plaque, mouth breathing and immigrant status were more common in 3-year-olds with asthma than in 3-year-olds without asthma. These factors are well-known risk factors for caries development in young pre-school children [25,26]. One reason why none of these risk factors could be identified among non-asthmatic 3-year-olds might be the skewed distribution of caries and that all children came from areas with high socioeconomic profile. In agreement with previous studies [27], mouthbreathing was more prevalent in pre-school children with asthma than in healthy pre-school children. This may explain why 3-year-olds with asthma experienced significantly more bleeding on probing (gingivitis) than pre-school children without asthma and why plaque was more prevalent in both 3- and 6-year-olds with asthma compared with children without asthma. Mouthbreathing could also be an explanation for the frequent consumption of sugar-containing drinks in asthmatic 3-year-olds. It has been suggested that the main reasons for the increased caries prevalence in asthmatic children could be reduced salivary flow and increased levels of mutans streptococci and lactobacilli in saliva [13]. In the present study, no connection between caries prevalence and microbiological factors in 6-year-olds could be demonstrated. In line with a study by Eloot et al. [17], the present study was unable to demonstrate any connection between the severity of the asthma, the period of exposure to medication and caries prevalence. If such a connection is to be assessed, pre-school children with early asthma onset should be followed for a long time. Further longitudinal research is therefore needed to clarify how the severity of the disease and the period of exposure to medication affect the oral health of asthmatic children. 14 To conclude, the main differences between asthmatic children who did and did not develop caries lesions were mouthbreathing, the consumption of sugar-containing drinks and the presence of plaque for the 3-year-olds and the presence of plaque and gingivitis for the 6year-olds. The parents of pre-school children with asthma should therefore be encouraged to brush their children’s teeth carefully twice a day with fluoridated dentifrice and to give their children water to drink when they are thirsty. 15 Bullet points What this paper adds This study shows that pre-school children with asthma have higher caries prevalence than pre-school children without asthma. The results of the study reveal that asthmatic pre-school children with caries had more visible plaque than asthmatic caries-free pre-school children. Why this paper is important to paediatric dentists It points to the importance of developing preventive dental programmes for pre-school children with asthma. It points to the importance of developing collaboration between dental and medical care-givers in relation to children with asthma. Conclusions The results of this investigation show that: Pre-school children with asthma have a higher caries prevalence than healthy children. Asthmatic 3-year-olds with caries consume sugar-containing drinks more frequently than caries-free asthmatic 3-year-olds. Bleeding gingivitis was more prevalent in asthmatic 6-year-olds with caries than in caries-free asthmatic 6-year-olds. Acknowledgements The authors are grateful to all the children and their parents for participating in the study. Many thanks to the staff at the participating PDS-clinics for their valuable assistance. 16 References 1 Mannino DM, Homa DM, Pertowski CA et al. Surveillance for asthma--United States, 1960-1995. MMWR CDC Surveill Summ. 1998;47: 1-27. 2 Steinbacher DM, Glick M. The dental patient with asthma. An update and oral health considerations. J Am Dent Assoc. 2001;132: 1229-39. 3 The International Study of Asthma and Allergens in Childhood (ISAAC) Steering Committe. Worldwide variations in the prevalence of asthma symptoms: the International Study of Asthma and Allergens in Childhood. 1998. 4 SBU. Treating asthma and COPD. The Swedish Council on Technology Assesment in Health Care. SBU report No 151. 2000. 5 Wright AL, Stern DA, Kauffmann F, Martinez FD. Factors influencing gender differences in the diagnosis and treatment of asthma in childhood: the Tucson Children's Respiratory Study. Pediatr Pulmonol. 2006;41: 318-25. 6 Arnrup K, Lundin SA, Dahllof G. Analysis of paediatric dental services provided at a regional hospital in Sweden. Dental treatment need in medically compromised children referred for dental consultation. Swed Dent J. 1993;17: 255-9. 7 Ersin NK, Gulen F, Eronat N et al. Oral and dental manifestations of young asthmatics related to medication, severity and duration of condition. Pediatr Int. 2006;48: 549-54. 8 McDerra EJ, Pollard MA, Curzon ME. The dental status of asthmatic British school children. Pediatr Dent. 1998;20: 281-7. 9 Milano M. Increased risk for dental caries in asthmatic children. Tex Dent J. 1999;116: 35-42. 10 Milano M, Lee JY, Donovan K, Chen JW. A cross-sectional study of medication-related factors and caries experience in asthmatic children. Pediatr Dent. 2006;28: 415-9. 17 11 Reddy DK, Hegde AM, Munshi AK. Dental caries status of children with bronchial asthma. J Clin Pediatr Dent. 2003;27: 293-5. 12 Ryberg M, Moller C, Ericson T. Effect of beta 2-adrenoceptor agonists on saliva proteins and dental caries in asthmatic children. J Dent Res. 1987;66: 1404-6. 13 Ryberg M, Moller C, Ericson T. Saliva composition and caries development in asthmatic patients treated with beta 2-adrenoceptor agonists: a 4-year follow-up study. Scand J Dent Res. 1991;99: 212-8. 14 Bjerkeborn K, Dahllof G, Hedlin G, Lindell M, Modeer T. Effect of disease severity and pharmacotherapy of asthma on oral health in asthmatic children. Scand J Dent Res. 1987;95: 159-64. 15 Meldrum AM, Thomson WM, Drummond BK, Sears MR. Is asthma a risk factor for dental caries? Finding from a cohort study. Caries Res. 2001;35: 235-9. 16 Shulman JD, Taylor SE, Nunn ME. The association between asthma and dental caries in children and adolescents: A population-based case-control study. Caries Res. 2001;35: 240-6. 17 Eloot AK, Vanobbergen JN, De Baets F, Martens LC. Oral health and habits in children with asthma related to severity and duration of condition. Eur J Paediatr Dent. 2004;5: 210-5. 18 Koch G. Effect of sodium fluoride in dentifrice and mouthwash on incidence of dental caries in schoolchildren. Odont Revy. 1967;18. 19 Loe H, Silness J. Periodontal Disease in Pregnancy. I. Prevalence and Severity. Acta Odontol Scand. 1963;21: 533-51. 20 Silness J, Loe H. Periodontal Disease in Pregnancy. II. Correlation between Oral Hygiene and Periodontal Condtion. Acta Odontol Scand. 1964;22: 121-35. 18 21 Mattsson O. A magnifying viewer for photofluorographic films. Acta Radiol. 1953;39: 412-4. 22 Wendt LK, Birkhed D. Dietary habits related to caries development and immigrant status in infants and toddlers living in Sweden. Acta Odontol Scand. 1995;53: 339-44. 23 Hugoson A, Koch G, Gothberg C et al. Oral health of individuals aged 3-80 years in Jonkoping, Sweden during 30 years (1973-2003). I. Review of findings on dental care habits and knowledge of oral health. Swed Dent J. 2005;29: 125-38. 24 Wogelius P, Poulsen S, Sorensen HT. Use of asthma-drugs and risk of dental caries among 5 to 7 year old Danish children: a cohort study. Community Dent Health. 2004;21: 207-11. 25 Grindefjord M, Dahllof G, Nilsson B, Modeer T, Stepwise prediction of dental caries in children up to 3.5 years of age. Caries Res. 1996;30:256-66. 26 Wendt LK, Hallonsten AL, Koch G, Birkhed D. Analysis of caries-related factors in infants and toddlers living in Sweden. Acta Odontol Scand. 1996;54:131-7. 25 Venetikidou A. Incidence of malocclusion in asthmatic children. J Clin Pediatr Dent. 1993;17: 89-94. 19