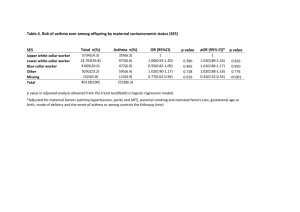
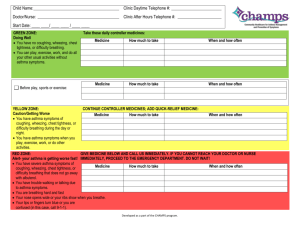
PMHx: Asthma
advertisement

What is asthma? Asthma is an inflammatory disease of the airway. As a result of this inflammation, the airways become blocked or narrowed because of swelling, muscular contractions and mucous production. These effects are usually temporary, but they cause shortness of breath, breathing trouble and other symptoms. If an asthma attack is severe, a person may need emergency treatment to restore normal breathing. More than 15 million people in the United States have asthma. This health problem is the reason for nearly half-a-million hospital stays each year. People with asthma can be of any race, age or sex. Its treatment costs billions of dollars each year. Despite the far-reaching effects of asthma, much remains to be learned about what causes it and how to prevent it. Although asthma can cause severe health problems, in most cases treatment can control it and allow a person to live a normal and active life. What are the major classes of asthma medications? There are seven major classes of asthma medications: steroidal anti-inflammatories, non-steroidal anti-inflammatories, beta-agonists, xanthines. anticholinergics, leukotriene receptor antagonists, and anti-allergics. The first two categories of drug treat the underlying inflammation of the lung. All steroidal anti-inflammatories are glucocorticosteroids, which are entirely different from the anabolic steroids that have become notorious for their abuse by athletes. There are many different corticosteroids available for the treatment of asthma, almost all available via inhaler to reduce the amount of side effects The non-steroidal antiinflammatories currently available are nedocromil sodium and cromolyn sodium, though cromolyn sodium is perhaps more properly known as a mast cell stabilizer, since it blocks both the release of histamine and inflammatory mediators, which means that although it blocks the inflammatory response, it cannot reverse inflammation once it has taken place. For this reason, I have classed it as an anti-allergic since it is mostly commonly taken for asthma that has a strong allergy component. The second two classes of asthma medications, beta-agonists and xanthines, are both bronchodilators, meaning that they relax the muscles lining the airways, allowing the airways to expand to their normal size. Beta-agonists are chemically related to adrenalin, but are specifically tailored to be more effective on the muscles of the lung while having little effect on the muscles in the heart. They are usually taken in inhaled form, and all but one (salmeterol) are short-acting. Theophylline, the major xanthine, is chemically related to caffeine, since caffeine is also a xanthine derivative, and is present in tea. Theophylline is taken orally, often in a sustained-action form Because its therapeutic range is close to its toxic range, asthmatics taking theophylline should have their blood levels monitored to ensure that their blood concentrations of theophylline lie within the therapeutic range There are some asthmatics, however, who cannot tolerate even very low doses of theophylline. Anticholinergics, the fourth class of medication, work by blocking the contraction of the underlying smooth muscle of the bronchi. Although used to treat asthma in Canada, the anticholinergic ipratropium bromide (Atrovent) has not approved by the US Food and Drug Administration for the treatment of asthma, but is used for the treatment of COPD. (It is interesting to note, however, that in the April 1982 issue of The FDA Drug Bulletin, the FDA states that "the FD&C Act does not, however, limit the manner in which a physician may use an approved drug. Once a product has been approved for marketing, a physician may prescribe it for uses or in treatment regimens or patient populations that are not included in a approved labeling." The FD&C Act is the Food, Drug, and Cosmetic Act.) The newest class of asthma medications is leukotriene receptor antagonists. My information as to how they work is sketchy, but as I understand it, the leukotriene receptor starts off the inflammator response of the immune system when it detects an allergen, so presumably an antagonist would block the receptor from responding to the presence of an allergen. Zeneca Pharmaceuticals has just now announced that its new leukotriene receptor antagonist, zafirlukast (Accolate), has been approved by the FDA (the US Food and Drug Administration) and will be available in November of .Abbott Laboratories now produces a second drug in this class: zileuton (Zyflo). The last class, the anti-allergics, has been included because the two anti-allergic drugs, cromolyn sodium and ketotifen, are commonly taken for the prevention of allergic asthma. Cromolyn sodium is a mast cell stabilizer -- it blocks the release of histamine from mast cells, which acts to prevent asthma flares since histamine is a very strong bronchoconstrictor. However, it isn't considered an antihistamine because it cannot prevent the effects of histamine once the histamine has been released from the cell. Similarly, it blocks the release of inflammatory mediators from the mast cell, and so prevents the inflammatory response, although it cannot reverse inflammation once the mediators have been released. Ketotifen fumarate (Zaditen), a non-sedating antihistamine used mostly for the treatment of pediatric allergic asthma, is not currently available in the United States. Management of Respiratory Failure: Patients who continue to worsen despite maximum treatment can have sudden respiratory arrest and death. It is not optimal to wait until the patient is nearly moribund from CO2 narcosis to take control of the airway. Rather, if active airway intervention is inevitable, it is preferable to make this decision early in the presentation. This should not be cause to take this procedure lightly in the asthmatic patient. Those asthmatics that require intubation have a significant rate of morbidity and mortality. Other Complications of Acute Asthma Exacerbation: Supraventricular tachydysrhythmias are common during an asthma exacerbation for multiple reasons. The combination of adrenergic stimulating agents, anticholinergics, hypoxia, electrolyte imbalances, and acidosis all add up to make the patient a high risk for dysrhythmias. Sinus tachycardia is the most common rhythm and is usually well tolerated by the patient. Unfortunately, there are a variety of other rhythms that can be more dangerous and will not be tolerated by the already stressed individual. Patients who develop these dysrhythmias tend to be older. When these dysrhythmias develop is incumbent upon the emergency medicine physician to be able to treat them in a logical manner. Paroxysmal atrial tachycardia may be treated with an agent such as verapamil (the usual contraindications apply) as it acts at the AV node and also has weak bronchodilating properties. As always, a patient with an unstable tachdysrhythmia should be cardioverted. Adenosine, normally the drug of choice for supraventricular tachycardias, should be avoided if possible as it may worsen bronchoconstriction. Beta blockers should be avoided due to the risk of worsening bronchospasm. Multifocal tachycardia is best treated by dealing with the underlying pulmonary problem. Try to find metabolic abnormalities such as hypokalemia, hypomagnesemia, hypoxia, and theophylline toxicity and correct them. Beta- agonist therapy may have to be held temporarily while rate control with an agent such as verapamil is attempted. If the blood pressure is stable, magnesium can probably be given to these patients. Atrial Fibrillation with rapid ventricular response can be treated with synchronized cardioversion if unstable. Otherwise digoxin and calcium channel blockers may be effective. Finally, ventricular dysrhythmias can develop and should be treated as normal. The addition of rapid IV push of magnesium should be considered early as it appears to be beneficial in ventricular tachycardia associated with asthma. Assessment and Management Plan A diagnosis of asthma is indicated based on the patient's hisotry of recurrent cough, wheezing and shortness of breath since childhood. The presence of wheezing during physical examination and the reversible airway obstruction documented on spirometry co nfirm the diagnosis. The high eosinophil count, high Ig E level and positive results of her allergy testing point toward an allergic origin for her asthma. The management plan is directed at improving asthma control through more effective use of medications and removal of environmental allergens. At present she is using high doses of inhaled bronchodilators, but is not using inhaled corticosteroids adequate ly. Several possible aggravating factors are present in the environment: a work place where she may be exposed to textile byproducts known to trigger asthma problems, and could explain why her asthma is worse at theend of the week; tobacco smoke at ho me; pets at home (dogs and cats). Her medication regimen should include an inhaled corticosteroid (Beclomethasone), initially 4 puffs 4 times per day until symptoms are stabilized. Later she may lower her dose to a 3 times/day regimen. She will continue to use Ventolin (albuterol) on a prn basis, keeping a diary of how much medicine she is using. The medication regimen should be kept as simple as possible to reduce the cost of medications. The patient is at high risk of diabetes in view of her Mexican-American origin, family history of diabetes in her mother, obesity and a borderline high blood glucose value. Patient Counselling and Education 1) The concept of asthma as a chronic inflammatory problem which requires continuous anti-inflammatory medication, even during symptom-free periods. Need for anti-inflammatory medication. The anti-inflammatory medication example inhaled corticosteroid (Beclomethasone). Because of her fear of "steroids," the following points will be emphasized: the need for regular use of anti-inflamm atory medications, the advantage of using inhaled vs. systemic steroids, and the difference between corticosteroids and anabolic steroids, the different actions of inhaled corticosteroids and inhaled bronchodilators and the need to use beclomethasone regularly in order for it to be effective. 2) The use of metered dose inhalers (MDIs). She will be trained in the correct use of inhalers. A spacer will be used, since it facilitates the MDI technique. 3) Identification of environmental triggers. The patient will be trained to keep a diary and measure her peak flow rates twice a day in order to establish a pattern between her symptoms, flow rates and invironmental circumstances. Since the patient completed three years of high school, her literacy level is not a serious barrier to learning to keep the diary. 4) Her risk of diabetes. The importance of weight control through proper dietary habits and exercise will be reviewed. What medications should asthmatics be careful about taking? Aspirin can trigger an asthma attack in approximately one in five asthmatics. This is especially common in those asthmatics who also have nasal polyps. As acetominophen (Tylenol), also known as paracetamol overseas, doesn't have this effect, it may be used as an alternative for anyone who suspects that they might have aspirin sensitivity. Cough medicines should also be treated with caution. In general, suppressing a productive cough (one which is bringing up mucus) is not a good idea, since the mucus can obstruct the airways and also irritate them further. Also, in Asthma: Stop Suffering, Start Living, the authors caution that prescription cough suppressants (including those with codeine) are potentially dangerous for asthmatics. They may make you sleepy and reduce your breathing effort. They may also dry out your secretions, making mucus harder to raise." Antihistamines, however, should not pose a problem for most asthmatics, in spite of many warning labels. In Children with Asthma, , "Most asthma experts see no problems with using antihistamines between or during asthmatics . . . Theoretically these drugs might dry up the mucus in the windpipes, thus making it harder to cough it up, but this has never been proved." Asthmatics taking theophylline should be careful when taking any of the following medications: the ulcer medications cimetidine (Tagamet) and troleandomycin (TAO), beta-blocker drugs such as propranolol, and the antibiotics erythromycin and ciprofloxacin. These medications may increase the concentration of theophylline in the bloodstream, possibly even to the toxic level . People taking theophylline should be alert for signs of possible toxicity such as rapid or irregular heartrate, nervousness, or nausea, when taking these medications. In fact, asthmatics taking theophylline should check with their physician before taking any OTC medication, as the list of drugs, including antihistamines, which affect theophylline levels is almost endless. Beta-blockers, usually taken for hypertension, can pose problems even for those asthmatics not taking theophylline. Beta-blockers work by blocking the hormone adrenalin, but as adrenalin and other adrenergic drugs help keep airways dilated, the use of beta-blockers may aggravate asthma symptoms. children taking oral or injected corticosteroids may be at increased risk of complications from chicken pox. Children taking inhaled corticosteroids are not at this increased risk, according to the pamphlet, since the system concentrations of the medication are so small. . Case study I Patient detail. The patient is a 68-year-old History of Present Illness: with a history of left ankle and calf swelling over the last 2 months, who was evaluated by an outside physician who did a duplex scan as an outpatient and found that the patient had a deep vein thrombosis of the left lower extremity. The patient was admitted for heparinization and coumadinization. Past Medical History Asthma, previously on steroids for approximately 15 years. 2. Polycystic kidney and liver disease. 3. Coronary artery disease with a mid right coronary artery occlusion, status post PTCA 3 years ago. 4. Rectal carcinoma resulting in resection with colostomy in January of 1993; no chemotherapy or radiation postoperatively. 5. Hypertension since 1965. 6. History of lower extremity edema for approximately one year. Physical Exam The patient was normotensive, with a pulse of 80, respirations 12, and afebrile. His exam was totally unremarkable, except for mild hepatomegaly. The left kidney was palpable, an intact colostomy, and a midabdominal scar. Extremities were unremarkable, except for a palpable cord over the left lateral malleolus. Neurologically, the patient was nonfocal. Lab Data CBC on admission with a white count 6,000, hematocrit 46.3. PT 9.7, PTT 32. Blood gas on room air with a pH 7.40, pO2 87, pCO2 31, bicarbonate 19, 97% saturated. Urinalysis was negative. Pertinent labs besides the above-mentioned, the patient had a duplex Doppler on the 17th done that revealed a common femoral, profundus femoral, and superficial femoral thrombosis. Hospital Course The patient was admitted and started on heparin therapy for a DVT. The patient's other evaluation for hypercoagulable state included thyroid function tests that were normal, an ANA that was negative, and a sedimentation rate that was 33. The patient's liver function tests were also normal, and urinalysis was negative for proteinuria. The patient was continued on heparin, and a VQ scan was ordered secondary to the patient's known underlying lung disease; this was obtained merely as a baseline in case the patient developed any respiratory symptoms following hospitalization or in the subsequent months. The patient was maintained on heparin with the PTT goal of 50-75. This he tolerated with no difficulty, and his hematocrit remained stable throughout his hospitalization. Coumadin was started on the first hospital day, and the patient reached therapeutic with an INR of 2.5 by the 4th hospital day. The heparin was maintained for the full hospital course, and was discontinued just prior to discharge. The patient during hospitalization had variable blood pressures, and required an addition of Lisinopril with spotting with Clonidine 0.1 mg p.o. q.6h. as needed for systolic hypertension. The patient through out his hospital stay had no complications related to his heparinization, nor developed any shortness of breath, chest pain, or tachycardia. Clinical History Patient with history of asthma and deep venous thromboses. Findings There is heterogeneous perfusion to both lungs. However, no segmental perfusion defects are identified. Central deposition of radioaerosol is seen on the ventilation scan. This may be secondary to asthma vs. poor inspiratory effort during the scan. These findings make interpretation of the ventilation scan difficult. Conclusions Baseline perfusion lung scan demonstrates heterogeneous blood flow to both lungs, secondary to underlying pulmonary disease vs. possible old pulmonary emboli. No segmental ventilation/perfusion mismatches are noted to suggest a significant pulmonary embolus. Discharge Diagnosis: Left lower extremity deep vein thrombosis. Chronic obstructive pulmonary disease. Polycystic kidney and liver disease, Coronary artery disease. Status post rectal carcinoma with colostomy. Hypertension, History of lower extremity edema. Case study II Patient study A 16-year-old boy with severe asthma presents with worsening exertional dyspnea, chest pain, and an abnormal chest radiograph. History of Present Illness The patient is a 16-year-old boy with a history of severe asthma and hypothyroidism who developed increased exertional dyspnea 5 months prior to admission (PTA). Montelukast sodium, 10 mg, was added with some improvement in symptoms and an increase in FEV1 by 14%. The patient was also taking fluticasone propionate, 220 µg twice daily, salmeterol xinafoate, 50 µ g twice daily, albuterol sulfate as needed, intranasal triamcinolone acetonide, 220µ g daily, loratidine, 10 mg daily, and levothyroxine sodium, 75 µg daily. Six weeks PTA he developed flu-like symptoms with low grade fever, nonproductive cough, nausea, and chest pain. A chest radiograph showed diffuse alveolar-interstitial infiltrates. A complete blood count was normal without eosinophilia, and cold agglutinins were negative. He was treated with a course of oral erythromycin with minimal improvement in pulmonary symptoms. A repeat chest radiograph taken 3 weeks later showed no improvement. The patient then developed oral candidiasis and streptococcal pharyngitis and was treated with oral fluconazole and amoxicillin-clavulanate potassium with resolution of both. Chest pain worsened and the patient was admitted to the hospital. Past Medical History The patient had multiple admissions for status asthmaticus starting at age 18 months. He required intubation and mechanical ventilation for status asthmaticus at age 3. He was steroid-dependent until 2 years PTA (age 14) when his asthma symptoms stabilized after he started taking inhaled fluticasone and salmeterol. He was then able to be taken off oral steroids. He suffered growth delay related to the chronic use of steroids. In addition to asthma, he also had chronic sinusitis which required surgery at age 6, and hypothyroidism. Diagnostic evaluation in the past included a negative sweat test, normal barium swallow, and positive skin tests to Aspergillus, trees, weeds, and ragweed extracts. The patient is in the 10th grade and is a nonsmoker. He is not sexually active and has received no blood transfusions in the past. There were two dogs in the home but no birds. The patient had traveled to Ohio 6 months PTA for vacation. Physical Examination On examination, the patient appeared small-statured and was in no acute distress. The temperature was 37.6° C, heart rate was 70 beats per minute, and respirations were 16 breaths/minute. Pulse oximetry on room air was 96%. Oral examination did not reveal any evidence of oral candidiasis and the posterior pharynx was clear. The trachea was midline with no cervical adenopathy. Lung examination revealed good air exchange with occasional dry inspiratory crackles heard at both bases and over the right anterior chest. Cardiac examination was normal. The extremities were without clubbing, cyanosis, or edema. Hospital Course The patient was admitted and started on intravenous azithromycin. Mycoplasma titers, both IgG and IgM levels, were elevated. The sedimentation rate was 77 mm/hour and cold agglutinins were now positive at 1.25 Fungal antibody titers were negative. Total IgE was 72 U/mL (0 to 93). Angiotensin-converting enzyme level was 22 IU (14 to 78) and Legionella titers were negative. The patient's chest pain improved, but a repeat chest radiograph showed no change in pulmonary infiltrates. High resolution CT scan of the chest showed a widespread pattern of air space disease involving the upper lobes, lower lobes, and lingula. There was mild pretracheal, right hilar, and mediastinal lymphadenopathy with lymph nodes measuring up to 2 cm in size Bronchoscopy with bronchoalveolar lavage (BAL) and transbronchial biopsy were performed. It was noted on bronchoscopy that there was a copious amount of tan mucus in the airways. Differential Diagnosis The patient's presentation suggests a subacute illness superimposed on a more chronic pulmonary disease process. The subacute illness could be of an infectious etiology such as mycoplasma pneumonia, given the rise in cold agglutinins, elevated mycoplasma titers, and partial clinical improvement after treatment with a macrolide antibiotic. Convalescent mycoplasma titers were not obtained, which would have helped diagnose acute mycoplasma disease. The clinical symptoms predate by months and it would be unlikely for mycoplasma infection to account for the entire clinical process. The recent travel to Ohio suggests possible histoplasmosis, which is endemic in the Ohio valley. Clinical manifestations can include cough, fever, malaise, and an abnormal chest radiograph with fibronodular infiltrates and hilar adenopathy. Patients with chronic pulmonary histoplasmosis can have more of a gradual onset of symptoms over weeks to months, as this patient did. Serologic tests in appropriate clinical settings are considered diagnostic. Definitive diagnosis requires identification of the organism by culture or on biopsy. Allergic bronchopulmonary aspergillosis (ABPA) should be considered in any asthmatic patient with pulmonary infiltrates. A diagnosis of ABPA requires the patient to have asthma, positive immediate skin test to Aspergillus mold, elevated total IgE level greater than 1000 ng/mL, elevated IgE and IgG specific to Aspergillus compared with control values, and positive precipitans to Aspergillus. Other supportive evidence includes central bronchiectasis, peripheral eosinophilia, a sputum culture positive for Aspergillus, and cough productive of mucus plugs or casts. The current patient had a positive skin test to Aspergillus but a low IgE level. He had not recently received systemic corticosteroids, which can lower the IgE level. The high resolution CT scan of the chest did not show any bronchiectasis and had more diffuse infiltrates, making the diagnosis of ABPA less likely. Bronchiolitis obliterans with organizing pneumonia (BOOP) can occur after exposure to certain medications, radiation, or viral infections, or it can be idiopathic. The patient's flu-like symptoms could have represented a viral syndrome with BOOP as a resulting sequela. Open lung biopsy would be needed to make a definitive diagnosis. Alveolar proteinosis is a lung disease with accumulation of proteinaceous material in the alveolar lung space. Patients can present with exertional dyspnea and an abnormal chest radiograph. Definitive diagnosis depends on demonstrating periodic acid-Shiff (PAS)-positive staining of the proteinaceous material either from BAL or lung biopsy. Sarcoidosis is a multisystem disease characterized by the accumulation of noncaseating granulomas with predilection for the lung. Patients can be asymptomatic. Acute or subacute sarcoidosis can present with constitutional symptoms such as fever, cough, chest discomfort, malaise, anorexia, and weight loss. Laboratory abnormalities can include an elevated sedimentation rate and elevated angiotensin-converting enzyme level. Chest radiograph can range from showing bilateral hilar adenopathy to diffuse parenchymal disease. Transbronchial biopsy would help delineate the diagnosis. Hypersensitivity pneumonitis (HP) is an allergic lung disease resulting from inhalational exposure to antigen. Acute, subacute, and chronic forms of HP can occur depending on the timing and amount of exposure to antigen. Patients with chronic hypersensitivity pneumonitis can present with cough, dyspnea, weight loss, malaise, and pulmonary infiltrates from exposure to small amounts of antigen over a prolonged period of time. Although the time course of chronic HP is consistent with the patient's clinical scenario, there was no identifiable antigen in the history, such as bird exposure, in this patient. Obtaining a hypersensitivity panel that some commercial labs offer would be of little help in making the diagnosis because a result of positive precipitans to an antigen would only indicate exposure, not disease. Pathology The cytologic smears of BAL fluid revealed copious amounts of finely granular, eosinophilic, acellular material. The amorphous material was highlighted with PAS stain with and without diastase digestion. Silver stain, to rule out the possibility of Pneumocystis carinii infection, was negative. Gram stain and acid-fast stains were also negative for microorganisms. The transbronchial biopsy contained alveolar spaces filled with the same eosinophilic, granular, amorphous debris seen in the BAL specimen There was no associated inflammatory or neoplastic infiltrate identified in the biopsy material. These findings were consistent with pulmonary alveolar proteinosis. Followup The patient was referred to a large tertiary center to have large volume lavage. He tolerated bilateral lung lavage under general anesthesia. He had an improvement in the pulmonary infiltrates but not complete resolution. He also clinically improved with a decrease in exertional dyspnea. DISCUSSION Alveolar proteinosis is a rare pulmonary disease of unknown etiology, and has been reported in infants, children, and adults. Alveolar proteinosis has also been reported in patients with cancer (lymphoma, leukemia, breast cancer), human immune deficiency virus (HIV), Pneumocystis carinii pneumonia, pericardial disease, inflammatory bowel disease, and prune belly syndrome. 4,5 Patients with alveolar proteinosis develop progressive dyspnea because of accumulation of surfactant-like proteins in the alveolar space leading to a decrease in gas exchange. Surfactant is a lipid-rich protein mixture that lines the alveoli and reduces surface tension. A disruption in surfactant homeostasis leading to a defect in surfactant clearance has been proposed as a possible mechanism for the disease. Mutant mice that were deficient in GM-CSF developed pulmonary disease characteristic of alveolar proteinosis in humans with increased concentrations of surfactant proteins in the alveolar space. When the genetic defect was corrected by supplying the gene for GM-CSF to the respiratory epithelium, the alveolar proteinosis resolved. 6 Further aerosolized GM-CSF in GM-CSF-deficient mice with alveolar proteinosis also corrected the disease with a decrease in surfactant in the lungs. Lastly, a patient with alveolar proteinosis was treated with subcutaneous injections of GM-CSF with clinical improvement in symptoms. After discontinuation of the GM-CSF, symptoms worsened and again improved with restarting GM-CSF. Current treatment for alveolar proteinosis consists of mechanical removal of the protein by large volume, whole lung lavage under general anesthesia. Other therapies such as the use of trypsin in lung lavage and oral corticosteroids have been used. 9 Future studies on the role of bone marrow transplantation or the use of GM-CSF in humans is needed. CONCLUSION In summary, we believe that this is the first reported case of alveolar proteinosis in a child with asthma. The case had many complicating factors, including possible super-infection with mycoplasma in a young asthmatic with underlying alveolar proteinoisis. Given the diagnosis of asthma, clinicians were biased to consider conditions in which asthma is an underlying criterion, ie, Churg-Strauss vasculitis. This case emphasizes the need for a broad differential diagnosis when evaluating patients with alveolar lung disease as well as the value of bronchoscopy with clinical-pathologic correlation to arrive at the correct diagnosis. . Case study III patient detail A 16 year old man, Case history with a history of asthma that had needed hospital admission on several occasions, present history was referred to the intensive care unit with a diagnosis of acute severe asthma. Seven weeks earlier he had sustained a head injury in a road traffic accident and had been mechanically ventilated through an oral tracheal tube for 84 hours at another hospital. Subsequently he had been transferred to a neurological rehabilitation unit. Two days after admission he complained of exertional dyspnoea and wheeze. Although treatment with bronchodilators was started, his symptoms worsened progressively over the next two weeks, and he became acutely dyspnoeic at rest. He was transferred to an acute medical ward but continued to deteriorate despite receiving nebulised bronchodilators, intravenous hydrocortisone, aminophylline, and antibiotics. He became exhausted within 24 hours and was thus referred to our intensive care unit for further management. Sing and symptom complained of exertional dyspnoea and wheeze On admission he was in extremis and had tachypnoea , a virtually silent chest, and hypercarbia Physical examination (respiratory rate 30/min), (partial pressure of carbon dioxide 9.3 kPa) arterial blood gas analysis treatment treatment with bronchodilators receiving nebulised bronchodilators, intravenous hydrocortisone, aminophylline, and antibiotics. We decided to intubate and ventilate him. After intravenous induction of anaesthesia, laryngoscopy was performed, with a good view of a normal glottis, Case study IV Patient detail A 37 y/o black female Case history : with a history of asthma, present history presents to the ER with tachypnea, and acute singe and symptom shortness of breath with audible wheezing. coughing up small amounts of white sputum physical examenation HR 110, RR 40 with signs of accessory muscle use. Ausculation revealed decreased breath sounds with inspiratory and expiratory wheezing and pt was SaO2 was 93% on room air. An arterial blood gas(ABG) was ordered with the following results: pH 7.5, PaCO2 27, PaO2 75. Treatment Patient has taken her prescribed medications of Cromolyn Sodium and Ventolin An aerosol treatment was ordered and given with 0.5 cc Ventolin with 3.0 cc normal saline in a small volume nebulizer for 10minutes. Peak flows done before and after the treatment were 125/250 and ausculation revealed loud expiratory wheezing and better airflow. 20 minutes later a second treatment was given with the above meds. Peak flows before and after showed improvements of 230/360 and on ausculation there was clearing of breath sounds and much improved airflow. RR was 24 at this time and HR 108. Symptoms resolved and patient was given prescription for inhaled steroids to be used with current home meds. Case study V Patient detail A 20 year-old woman started work as an animal house technician, dealing mainly with rodents. She was given minimal training on commencement of exposure. Singe and symptoms A few months later she developed symptoms of runny glazed and gritty eyes (conjunctivitis), stuffy, itchy and runny nose (rhinitis). She also had wheeze, tight chestedness, and shortness of breath (asthma) which improved on spells away from work. She noticed that when she was scratched by the rodents her skin very quickly developed raised red patches (urticaria). Treatment Her general practitioner prescribed treatment with bronchodilators, producing slight improvement but her symptoms persisted. Complication After about one year in employment she experienced an episode of angio-oedema and had serious difficulty with breathing. She was seen in a hospital casualty department, follow up treatment with adrenaline and hydrocortisone. However no specific action in relation to her job was considered. After this episode she did not return to that work, and eventually resigned her employment. Arguably, from a medical standpoint the problem was solved. The work related nature of her symptoms had been demonstrated, at least circumstantially; she would no longer work in the animal house and her symptoms would be expected to resolve. Case study VI Patient detail Beth Brown is a 32-year-old, Past history first visit to emergency room two weeks ago for a severe asthma attack where she received nebulized albuterol treatments and was started on inhaled steroids , bothered by exercise induced asthma only when she runs. Prior to her move, her only medications were oral contraceptive pills, an albuterol inhaler, which she used before she would exercise, and Seldane 60 mg used when seasonal allergic symptoms would bother her. Since moving to NC, she has been wheezing on a regular basis, She uses her beclomethasone inhaler, 3 puffs 3 times a day; albuterol inhaler, 2 puffs QID. She admits to being noncompliant with her medications except during periods when she is substantially affected by asthma symptoms. Singe and symptom Three days before she went to the ER she developed symptoms of rhinorrhea, nasal congestion, and itchy eyes. She has a history of seasonal allergic rhinitis and had taken Seldane 60 mg BID in the past. Physical examenation PE Today, BP: 144/82 Wt: 125 Ht. 5'5", T 99.6 RR19, HR 96 PEFR: 280 TM’s: slightly retracted Nose: swollen turbinates with yellowish discharge, Pharynx4 erythematous Neck: submandibular tenderness, Lungs, audible wheezes in expiration, with popping noises in bases, Abdomen:. The next week, who is breathless. She has been taking her medications as prescribed but developed worsening symptoms of asthma including server wheezing and coughing. . By the time she makes it to the emergency room she appears in moderate distress, actively using her accessory muscles to breathe Her peak flow is measured at 50 L/minute. Her vital signs are 150/92, (18 mm paradox) HR 122, RR=40, T. 100.6. An arterial blood gas is obtained and is reported as pH 7.46, pO2=64 mmHg, pCO2=35. She is placed on supplemental oxygen therapy at 5L/minute and is given an albuterol treatment fter 3 nebulized treatments, her blood gasses are as follows: HR 140, BP 190 90,Temp=100.6, RR 36 02 saturation on 5L, 91t. She is very fatigued and you decide to admit her to the hospital. After three days, Beth has significantly improved and is back to her baseline. She is ready for discharge from the hospital. You review her therapies and make recommendations about changes in her outpatient regimen Case study VII Patient detail is a 17 year old black male. He was seen last at a medical center for c/o headache, sore throat, cough and congestion. He is diagnosed with a viral URI. He was last hospitalized in. He is seen at the medical center often for problems related to his asthma. has also been diagnosed with asthma GERD. History of Present Illness (HPI) Asthma GERD and his mother both state that he was diagnosed with asthma at 11 years of age. He has had recurring severe problems and multiple hospitalizations due to his asthma. He.. His asthma appears to be worse at night and is aggravated by house dust mites and weather changes. Past Medical History (PMH) was diagnosed with asthma at 11 years of age. After being diagnosed, he had allergy testing done. It was found at that time that he was allergic to 9 varieties of grass pollen, pigweed pollen, and white oak tree pollen and house dust mites. He began to take allergy shots until he developed problems from the shots asthma is so severe that he was singe and symptoms was in the ICU in October of 1998. He was noted as having wheezing, tachypnea and retractions. He was placed on a continuous albuteral nebulizer in the ED. At the time of this hospitalization was noted as having chronic chest pain and had a right bundle branch block noted on EKG.has had the following surgeries: fundoplication, tonsillectomy, adenodectomy and PE tubes. He had no known drug allergies., it appeared that the severity and frequency of his asthma attacks had improved until August of 1998, when he began occurring at least 2-3 times a week. His attacks usually occur at nighttime. c/o shortness of breath with exertion, specifically while climbing stairs, was seen by a neurologist for headaches and was diagnosed with migraines. Current Medications Volmaz 1 Tab. at bedtime Pulmicort 2 puffs BID (twice a day) TheoDur 600mg at bedtime Tilade 2 puffs BID with the inspieases Singulair 10 my daily Flonase or Beconase as needed Prilosec 40mg daily Albuteral as needed (usually required at least twice a day) Nortriptyline 25mg as needed for headaches Claritin 10mg daily Family History is the oldest of four boys. All four boys have been diagnosed with asthma at varying degrees from mild to severe. His mother and her sister have both been diagnosed with asthma Physical Exam) Weight: 242 lbs. 110 kg Height: 6' 3" BP: 110/70 Temp: 97.6 Pulse: 84 Physical Exam (PE) Weight: 272 lb BP: 126/76 Temp: 97.6 C/O headache, sore throat, congestion and cough. He does not have any problems with his asthma. His peak flows are in the 450 range. A lot of nasal congestion, sneezing and coughing. Hypersensitivity skin prick test have a 3+ response to the histamine and a negative response to the saline. He had a large 4 +reaction to both species of dust mite and a minimal 2+ response to cat dander. He had a negative response to dog dander, mold spores and pollen of all grasses, trees and weeds. Case study VIII Patient detail A 37 y/o black female Case history : with a history of asthma, present history presents to the ER with tachypnea, and acute singe and symptom shortness of breath with audible wheezing. coughing up small amounts of white sputum physical examenation revealed the following: HR 110, RR 40 with signs of accessory muscle use. Ausculation revealed decreased breath sounds with inspiratory and expiratory wheezing and pt was . SaO2 was 93% on room air. An arterial blood gas(ABG) was ordered with the following results: pH 7.5, PaCO2 27, PaO2 75. Treatment Patient has taken her prescribed medications of Cromolyn Sodium and Ventolin An aerosol treatment was ordered and given with 0.5 cc Ventolin with 3.0 cc normal saline in a small volume nebulizer for 10minutes. Peak flows done before and after the treatment were 125/250 and ausculation revealed loud expiratory wheezing and better airflow. 20 minutes later a second treatment was given with the above meds. Peak flows before and after showed improvements of 230/360 and on ausculation there was clearing of breath sounds and much improved airflow. RR was 24 at this time and HR 108. Symptoms resolved and patient was given prescription for inhaled steroids to be used with current home meds. Case study IX Patient detail This is a 52 year old black male brought by EMS with an asthma exacerbation. Singe and symptom Pt notes worsening shortness of breath for 2 days not responding to nebs. Not responding to MDI at home. No fever/chills. No cough. One albuterol neb given in field with little to no change. Never intubated, several previous hospitalizations, but none in the last 6 months. No long term steroid use. PMHx: Asthma PSHx: Appy Meds: MDIs Cardiac Risks: None. Exam significant for: Decreased breath sounds with little air movement throughout. Positive accessory muscle use. Positive prolonged expiratory phase. Minimal wheezing heard. Cardiac: Tachycardic but regular. No JVD, tracheal deviation, or leg edema. No unilateral leg swelling. The remainder of the exam is essentially normal. ECG: Sinus tachycardia with no acute changes. CXR: No infiltrate or pneumothorax. ED Course: The patient receives two nebulizations and steroids with no response to therapy. He remains tachycardic, diaphoretic, and severely short of breath. An ABG is drawn and shows the following results: Gas on 100%: 7.25/203/53/23. 2nd ED course continued: The patient has received three albuterol nebulizations, steroids and has made no progress. His chest is quiet with little air movement appears and will. His pulse oximeter is reading 94 %on a 100% non-rebreather. 3rd.ED course continued: The patient has had a modified rapid sequence intubation done and is now on a ventilator. The patient is tachycardic, but suddenly develops a heart rate of 170-200. The blood pressure is stable at 130/85. Discussion: Asthma is one of the most common respiratory diseases, with an incidence of more than 5% of the total population in industrialized countries. The prevalence and severity of asthma appear to be increasing in these countries, and there has been an increase in the death rate. This trend is disturbing since treatment modalities were thought to have been improving. majority of patients with this disease are easily managed in the outpatient setting, any patient with asthma has the potential to develop status asthmaticus. Status is defined as asthma that is severe at its onset or progresses rapidly despite standard therapy. Without successful management it may progress to ventilatory failure and death. Case study X Patient detailes A 27 year-old Hispanic female, born and raised in McAllen, Texas, was referred to a pulmonologist because of severe asthma. She works (since her marriage) as a cleaning clerk in a textile factory, does not smoke, but is exposed to environmental tobacco smoke because her husband and in-laws, with whom she lives, smoke. There are a cat and two dogs where she lives. Family history She has a sister with asthma and hay fever. Both parents are alive and her mother suffers from diabetes. Her asthma symptoms began during childhood and were controlled with Marex, an over-the-counter combination of a bronchodilator and antihistamine used to treat asthma. She never had to be hospitalized, but required frequent visits to the ER for asthma exacerbations Symptom of the asthma Five years prior to this visit her asthma relapsed, with symptoms including chest pressure, cough, shortness of breath and wheezing. She is unable to identify any triggers for her asthma exacerbations. However, her symptoms are worse at the end of the week. Before the asthma exacerbations she frequently develops itching and increased secretions in her eyes and nose. Her asthma symptoms have become progressively worse. She now has symptoms every day and night, and over the past year Drug treatment she has received several courses of oral prednisone to control asthma exacerbations. She is afraid of cortisone side effects, and would rather not use that medication. She was also prescribed inhaled beclomethasone (Beclovent), albuterol (Ventolin), and theophylline (Slobid). During the past six months she has had seven ER visits for asthma exacerbations, and has missed 21 days at work. She uses two to three canisters of Ventolin per month. She describes no medicine allergies and has never been allergy tested. Physical Exam: The physical examination revealed a slightly obese Latin American female in mild respiratory distress. She is normocephalic, pupils are symmetrical and reactive, conjunctiva are hyperemic. Nasal mucosa are edematous, pink, with increased clear secretions. No polyps. Pharynx is slightly hyperemic without exudates. Neck is unremarkable. Chest is symmetrical. Auscultation shows diffuse expiratory wheezes in both lung fields without crackles or ronchi. Heart rate is 100 and reg ular. No murmurs. Rest of physical exam is within normal limits. Laboratory: CBC:Hb 13.2, Ht 43, WBCs 10500--Neut 64%, Lymphs 20%, Eos 6% SMA 15 BUN 18 Creatinine 0.7 Glucose 103 Uric Acid 3.1 Cholesterol 234 Triglycerides 106 Calcium 9.3 Phosphorus 2.8 Total Protein 6.7 Albumin 4.1 Glob 2.5 Total Bilirrubin 0.9 Alk Phos. 69 ALT 21 AST 33 LDH 256 Ig E Level: 790 CXR: Normal Spirometry: FVC is 85% or predicted FEV1 is 65% of predicted. FEV1/FVC ratio is 67%. Improvement in FEV1 after inhaled albuterol: 22%. Allergy testing revealed allergies to dust mites, cats, dogs, and grass. Case study XI Patient detail Mary was an a thin, athletic 11 year-old child with chronic asthma. Her asthma had started a five months old, and had been severe for the next two and a half years. Patint history She was a forceps delivery. She was never breastfed, and was put on soy formula at birth. Solid food was introduced at 4 months. She had had chickenpox twice, once at four months and again at age 9 . She had had fever and irritability after a DPT shot. She had had one wart on her elbow. Her 19 year-old sister had developed asthma after Mary. Singe and symptom Mary's asthma had continued since infancy and now was of particular concern because she played sports. She was a very competitive swimmer and soccer player. Whenever she would get a cold, it went into asthma. Her lungs would tighten up and she would develop loud, squeaky wheezing. The wheezing was worse on inspiration. Attacks were induced by viral illnesses, pollen or exercise. She was very reactive to grasses, mold, wool and rabbit dander. Her asthma was very definitely worse from being exposed to cold, damp air. Her typical pattern was to get a runny nose or ear infection which would proceed to a cough, sore throat and wheezing. Treatment Then she would be treated with prednisone or antibiotics, which would relieve the symptoms for a while. . Case Study XII Patient detail A 19-year-old female (height 5'6", weight 125 lbs) presents with symptoms of cough and breathlessness which at times is not related to specific events or activities. Singe and symptom The patient who seeks medical consultation because of shortness of breath,dyspnea difficult breathing, fatigue and so forth is usually subjected to a series of questions, a physical examination, chest x-ray, spirometry, a methacholine challenge is often ordered. The symptoms of chest tightness, breathlessness, etc., produced by the reactive airways disease, and produced during testing in patients with the disease are in part due to the hyperinflation that accompanies the bronchospasm. A positive test by traditional pulmonary function testing is regarded as a 20% change from baseline measurement of the FEV1. In some situations, there may be no change in the FEV1 as demonstrated in the following case study. The testing reveals a significant increase in thoracic gas volume, residual volume and total capacity with methacholine challenge. Airway resistance increased and conductance decreased similarly, and all values returned to baseline with the inhalation of bronchodilator therapy, while the FEV1 from spirometry did not show any signs of reduction when challenged. Treatment The patient was started on bronchodilator therapy which resulted in improvement in symptoms. Case study VIII Patient detail C.G. is a 43 yo white woman Medical history in May, 1997, experienced lip swelling that lasted for a few hours and regressed spontaneously. Two days later, immediately after swimming, she developed diffuse, itchy hives that disappeared in less than 24 hours. Since she continued to experience hives intermittently. Her initial pulmonary function test in Feb of 1996 revealed an FVC of 76% and a FEV1 of 70 .%After treatment with an inhaled corticosteroid, her follow-up pulmonary function test in May 1996 revealed an FVC of 89% and FEV1 of 80%. For her asthma management, the patient was prescribed triamcinolone 2 breaths three times a day with a taper totwo times a day. Currently, the patient is using either an albuterol inhaler with good relief and a steroid nasal spray intermittently. Of note, she works in a daycare center and has suffered from several upper respiratory tract viral episodes. Her present peak flow readings at home are 250 to 300 L/min (predicted 480). She presently denies nighttime symptoms, but notes asthma symptoms with cold air exposure, upper respiratory tract infections, sinus infections, tobacco smoke and exercise. She denies seasonal variation in either nasal or chest symptoms. In 1996 the pt. had a sinus CT scan consistent with ethmoid sinusitis and received 6 weeks of cefuroxime and beclomethasone nasal spray. Presently, she denies rhinorrhea, nasal congestion and nasal or ocular pruritis. Allergy profille The patient denies eczema, food, drug, or bee sting hypersensitivity. Past history Hepatitis (A?) as a college student, otherwise unremarkable. Medications are: Pulmicort® 3 breaths BID, albuterol 2 breaths prn, Singulair® 10 mg QD, Flonase® 2 sprays/nostril QD, saline nasal spray prn, Suprax® 200 mg BID, Claritin® 10 mg QD, Atarax® 20 mg QD, doxepin 20 mg QD, Pepcid® 20 mg QD. Famil history Allergic rhinitis and asthma in two siblings. Father had prostate cancer. Enviromntal history The patient is native of New York and has been living in Williamsburg, VA, for the past 15 years. For the past 9 years she lived in a 35 years old house with central air, hardwood floors, no curtains. She uses hypoallergenic encasements for pillows and mattress and has one dog with no access to the bedroom. She denies current or past exposure to chemicals. work history The patient has worked for many years in an office. Social history The patient is married, denies smoking or alcohol use. physical exam RR 20, BP 120/80, P 128, T 97.5. Height 160 cm, Weight 50 Kg. PEFR 300 (62% of predicted). A healthy-looking 43 years old woman. Skin exam showed a overall dry skin with diffuse urticarial lesions on breasts and waist line and few round <1 cm diameter dark red papules. Also noted were many scattered abrasions from scratching especially localized to the lower extremities and ? positive dermatographism. Head and neck exam showed small nasal passages with erythematous nasal mucosa, dry oral mucosa, bilateral fronto-maxillary sinus tenderness. No thyromegaly or neck or axillary lymphoadenomegaly was detected. Heart, lungs, abdomen, extremities and neurological exams were normal. lab finbing Hgb 10.7 g/dl, Hct 32.4%, MCV 77.8; WBC 10,100/mm3 (PMN 81%, L 5%, Eos 7%, tot 300); platelets 573,000/mm3. Sed rate: 75 mm/h. Albumin 3.3 g/dl. Electrolytes: Normal. TSH: 0.8. HBSAg, anti-HBs, anti-HCV: Negative. Anti-ds-DNA, antiRo/La, Sm, nRNP: Negative. IgG, IgM, IgA: Normal. b-tryptase: <1 ng/ml. Case syudy XIV Patient detail M. is a 33 year old white woman . Not married. Does not smoke or drink. Medical history Type I diabetes mellitus since age 8. She developed diabetic nephropathy and hypertension. To relieve end stage renal disease requiring peritoneal dialysis, she had a combined kidney and pancreas transplant 2 years ago. Since recovery from that operation, kidney function has been adequate, blood pressure has been normal and she has not required insulin. She had a diagnosis of diabetic retinopathy and had laser treatments but that has subsided since the transplant. She continues to take immunosuppressive drugs. About one and one-half years ago she developed itchy eyes with redness and noted some swelling about the eyes. She stopped using eye makeup without relief. About one year ago she consulted an allergist, who carried out skin tests, all of which were negative. The allergist prescribed steroid cream to the eyelids, but this accorded only partial relief. She tried several antihistamine eye drops, both with and without vasoconstrictors with at best partial relief. She saw an ophthalmologist who found no changes in vision and advised her that allergies were a likely cause of the problem. She also saw a dermatologist who prescribed tetracycline and antihistamines without benefit. She also complained of occasional sneezing and runny nose that were not related in time to the ocular symptoms. Beconase and Flonase had been tried but not continued because nasal symptoms were minor and these drugs did not help the eye symptoms. Allergy profile She denies hay fever, asthma, urticaria, food or drug hypersensitivity Past history About 3-4 years ago she was diagnosed as hypothyroid and started on synthroid 0.075 mg daily. Thyroid function tests now normal. Since operation, she has been treated with depo- Provera injections every three months and has not had menstrual bleeding. She takes propulsion to prevent heartburn associated with prednisone treatment. Medications are: 1. Azathioprine 50 mg t.i.d. 2. Prograf 3 mg b.i.d. 3. Depo-Provera by injection every 3 mos. 4. K-Dur 40 meq daily. 5. Prednisone 10 mg daily. 6. Procardia-XL 60 mg daily. 7. Propulsid 30 mg daily. 8. Stresstab daily. 9. Synthroid 75 mcg daily. 10 Thiamine 100 mg daily. Family history Her father and a paternal aunt have "thyroid disease". An older sister had diabetes Enviromental history She has lived with her parents in a large city suburb in a 33 year old individual home for the past 30 years. It has warm air gas-fired heat, central air conditioning and wall-to-wall carpeting. She has had a dog for11 years. Work history She works as a temporary clerk and changes job locations frequently. Physical exam .T. 98.0'F. P. 77. B.P. 128/85. Ht. 5'4". Wt. 117 lb. PEFR 98% predicted. She is a young woman who does not appear ill. Examination of the eyes shows swelling of the lids with distinct redness of the margins and mild injection of the conjunctivae. The nasal mucosa and pharynx are normal. There is no enlargement of the thyroid. Heart, lung and abdomen are normal. There is a surgical scar in the right side at the rib margin posteriorly. Extremities and neurological are not remarkable except for slight tremulousness. Lab finding Skin tests to tree, grass and weed pollen, outdoor and indoor molds, dust mites, cat, dog and cockroach were all negative both by puncture test and intraderinal test. Wbe. /5./cu nun. Rbc. 3.81 million/cu mm. HGB 13.0 g/DL. PL 249,000/cu mm. Diff. Ly. 19% ,Mono. 5%. Eo. 1%. Baso. 1%. Neutro. 76%. T4.9.4 mcg/DL. TSH 1.74 MUAL. Thyroglobulin autoantibody, negative, rnicrosomal antibodies, negative.