KendallWilliams_202_20130625190844
advertisement

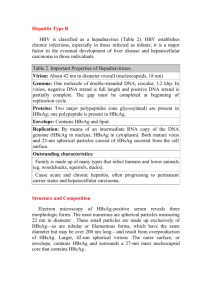
Management of Chronic Hepatitis B in the Antenatal Clinic- a Retrospective Review at The Wollongong Hospital. Background: Vertical transmission of hepatitis B virus is the main cause of chronic hepatitis B. Recent evidence suggests a role of maternal treatment in late pregnancy in addition to standard passive and immuno-prophylaxis in women with high viral load (HBV DNA >106 IU/mL) to further reduce the risk of mother to child transmission. Objectives: To assess the burden of chronic hepatitis B and how this is managed in our local antenatal population, with a particular view to whether maternal treatment could be incorporated into our local practices. Method: A retrospective single centre study of antenatal records over a 5 year period. After appropriate ethics approval, the Antenatal Department data bank was reviewed for all deliveries at The Wollongong Hospital between 2008 and 2012. Data collected included maternal demographics, HBsAg status at booking visit and HBeAg status where recorded, as well as neonatal date and time of birth, Apgar scores, administration of hepatitis B immunoglobulin (HBIG) and birth dose of monovalent hepatitis B vaccine. Hospital electronic medical records were then reviewed to confirm or clarify HBsAG status. Gastroenterology Department electronic records were searched for evidence of follow-up of women identified as HBsAg positive during their pregnancy. Results: There were 11,955 deliveries by 9494 women at The Wollongong Hospital between 2008 and 2012. HBsAg screening occurred in 99.6% pregnancies. HBsAg was positive in 35 pregnancies (28 women) giving a prevalence of 0.29%. A majority of these women were born in high endemic areas. HBeAg was checked in 32/35 cases, with 21 positive results. HBV DNA levels were checked in 5 cases but were not required to be recorded on the antenatal booking data sheet. 34/35 (97%) infants to HBsAg positive mothers received HBIG within 12hrs of birth and all received birth dose of monovalent hepatitis B vaccine. It is unclear if these infants receive the subsequent 3 doses of hepatitis B vaccine or have confirmed hepatitis B immunity as follow-up was by primary care physician. 11,362 (95%) infants received the birth dose of HB vaccine prior to discharge from hospital. Of 28 HBsAg positive women, 11 were seen in our gastroenterology department by either a hepatology nurse or a gastroenterologist, and only 7 were seen during a pregnancy. Conclusion: Although we have a low prevalence and excellent screening and immuno-prophylaxis rates, our current practices do not adequately identify high risk patients and would not facilitate maternal treatment in late pregnancy. New local policies should be considered.