Wave 6 Quality Improvement Charter
advertisement

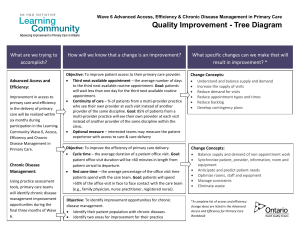
Wave 6 Quality Improvement Charter: Advanced Access, Efficiency and Chronic Disease Management in Primary Care “Advanced access has dramatically improved my patients’ ability to see me at the starting point of their health problem. Only having to wait one day has decreased their stress, as well as the stress of me and my staff” ~Dr. Paul Cano, Physician, Smithville Family Health Team “[This HQO] initiative has revolutionized the way we do business.” ~Susan Ouellet, Administrator, Greenstone Family Health Team “Diving deep into understanding your practice provides great opportunities for improvement. I used the 5 P's and specifically one of the 5 P's (patients) to make dramatic shifts in how I care for patients with complex health needs -- and in doing so have seen a 50% reduction in 3NA.” ~Dr. Jamie Read, Physician, Sherbourne Family Health Team What are we trying to accomplish? According to Health Quality Ontario’s 2012 Quality Monitor, “only half of sicker adults could see a doctor or nurse the same or next day when they were unwell, compared to 79% in the United Kingdom.”1 Patient delays in seeing their primary provider results in “patient dissatisfaction, contributes to staff dissatisfaction, and may lead to worsening clinical outcomes.” 2 Delays are also expensive: There is a cost in maintaining the wait list and triaging patient requests for appointments; The no-show or fail-to-show rate increases the longer the patient has to wait for their appointment; There is a risk that patients waiting for an appointment will arrive to their office visit with a more costly clinical condition;3 and Patients use the emergency department to access medical care that they could have received from their primary care provider (Canadian Triage Acuity Level (CTAS) 4 or 5). “Almost one in two Ontarians felt they could have been treated by their primary care provider if care had been available the last time they went to the hospital or Emergency Department.” 4 Findings in the 2012 Quality Monitor demonstrate some positive signs of improvement when it comes to chronic disease management (CDM) related to complications and the use of recommended medications. There remain many opportunities for improvement to ensure people routinely receive all of the evidence-based best practices in CDM.5 2 The Project AIM: Improvement in access to primary care and efficiency in the delivery of primary care will be realized within six months during participation in the Learning Community Wave 6 Advanced Access, Efficiency and Chronic Disease Management in Primary Care. Using practice assessment tools, primary care teams will identify chronic disease management improvement opportunities during the final three months of Wave 6. The online Advanced Access and Efficiency for Primary Care Road Map will guide you through the improvement process. Teams will apply changes to their practice to improve office efficiency and better match their supply of appointments with patient demand for appointments to achieve advanced access. The core principle of advanced access is that patients calling to schedule a physician visit are offered an appointment with their primary care provider on the same day or a day of the patient’s choosing.6 After working to improve access and efficiency, you will be guided through an assessment of your management of patients with chronic disease in order to identify where improvements can make a difference to the quality of care you are able to provide. The online Chronic Disease Management Road Map will guide you through the assessment, diagnosis and quality improvement plan development. How will we know that a change is an improvement? The following four measures will be tracked to monitor whether the changes are resulting in improvements. The tracking will occur throughout the nine months during which practices participate in Wave 6 Advanced Access , Efficiency and Chronic Disease Management in Primary Care (March 2013 to December 2013), and continue for another three months (January 2014 to the end of March 2014) to demonstrate sustainability of improvement efforts made during the Wave. Access and Efficiency: 1. Third next available appointment – Patients will wait less than one day for the third next available routine appointment. This sentinel measure is used to measure the number of days a patient has to wait to get a routine appointment. “The third appointment is featured because the first and second available appointments may reflect openings created by patients cancelling appointments and thus does not accurately measure true accessibility.” 7 2. Continuity of care – 85% of patients from a multi-provider practice will see their own provider at each visit instead of another provider of the same discipline within the clinic. 3. Cycle time – Patient office visit duration will be <60 minutes in length from patient arrival to departure. 4. Red zone time – Patients will spend >50% of the office visit in face to face contact with the care team (e.g., family physician, nurse practitioner, registered nurse). Teams are encouraged to use their data to guide their change efforts. In the early stages of the initiative, completing the panel size equation, tracking daily appointment demand and supply and activity rates will assist the practice team to inform their change decisions. Third next available appointment and future open capacity are helpful measures to monitor on an ongoing basis to sustain the improvements and identify when and where additional changes may be needed. Wave 6 Charter Health Quality Ontario 3 Chronic Disease Management: Teams will be assessing and identifying improvement opportunities for chronic disease management. At the end of the three months (September 2013 to December 2013) focusing on chronic disease management, assessment and diagnosis, teams will be able to: Identify their patient population with chronic diseases; and Identify two areas for improvement for their practice. Patient Experience: Teams will also be encouraged to guide their change efforts with information about the patient experience. Capturing, understanding, and utilizing the patient experience with access to care, care delivery and the management of chronic disease can create incredible opportunity for the team to gain insights, as well as identify opportunities for improvement, and ultimately engage patients in co-design to improve the patient and care team experience. 8 Teams participating in Wave 6 Advanced Access, Efficiency and Chronic Disease Management in Primary Care will be able to track an optional measure(s) to capture the patient experience. What changes can we make that will lead to improvement? Change concepts are general approaches that have been found to be useful in making an improvement. There are a number of change concepts reported in the literature and experienced by teams that will lead to improvement. From these change concepts, practices will develop more specific ideas for change that they want to test. These specific change ideas may include processes and tools that are new, or that have been tested and implemented with demonstrated effectiveness in other environments.9 A list of change concepts a team can further develop and test are listed in the document Advanced Access and Efficiency for Primary Care Workbook. 1 Health Quality Ontario (2012). Quality Monitor. Toronto: Ontario, p.4. Murray, M. (2000). Modernising the NHS – Patient Care: Access. BMJ, Vol. 320, p.1594. 3 Ibid., p.1594. 4 Health Quality Ontario (2011). Quality Monitor. Toronto: Ontario, p.80. 5 Health Quality Ontario (2012). Quality Monitor. Toronto: Ontario, p.10. 6 Murray, M., & Berwick, D. (2003). Advanced Access: Reducing Waiting and Delays in Primary Care. JAMA, Volume 289(8), p.1035. 7 Ibid., p.1038. 8 Baxter, H., Mugglestone, M., & Maher, L. (2009). The EBD Approach – Experience Based Design Concepts and Case Studies. NHS Institute for Innovation and Improvement. New Audience Ltd: West Midlands, UK. 9 Langley, G.J., Moen, R.D., Nolan, K.M., Nolan, T.W., Norman, C.L., Provost, L.P. (2009). The Improvement Guide. 2nd Ed. Jossey-Bass: San Francisco, California, USA. 2 Wave 6 Charter Health Quality Ontario