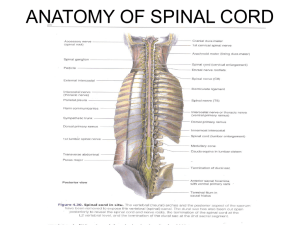
SPINAL DISORDERS
advertisement

SPINAL DISORDERS Disc Disease and Degenerative Disease of the Spine Epidemiology of low back and log pain: Low back pain with or without radicular leg pain affects up to 85% of individuals at some point in their lives. In a given year it has been estimated that between 10%-15% of the population have back and/or leg pain. Sciatica is thought to affect about 2% of the population and about 12% of people with back pain. Age is an important factor in determining the likelihood of back symptoms with peak incidence in the 35- 55 age range. There is no difference in the incidence of back symptoms between men and women. However there are significant differences in the incidence of back symptoms according to race (white> black > other), education (elementary or none > high school > college) and region of the country (West >South and Midwest > Northeast). In the United States, back pain is the leading cause of activity limitation for people younger than 45 years. It is the second most common cause of physician visits, the fifth most common reason for hospitalization and the third ranked reason for a surgical procedure. One percent of the U.S. population is permanently disabled with back pain and at any given time another 1% is temporarily disabled. Each year there are an estimated 400,000+ compensable back "injuries" in the U.S. A number of occupational risk factors have been studied. The relationship between occupation and back symptoms is complex and affected by a variety of confounding factors, e.g. reporting bias influenced by the insurance and Worker's Compensation systems. Several studies have shown an increased risk of low back pain and disc prolapse (HNP) for occupations associated with heavy physical work. Exposure to vibration may increase the frequency of low back pain as seen in truck drivers, machinery operators and individuals who drive automobiles extensively. Psychological work factors are also known to affect the frequency of back symptoms. Monotony, work dissatisfaction, and poor relationships with coworkers are all associated with higher rates of back pain and work incapacity. Individual risk factors have also been carefully studied. The effect of age has already been mentioned. Although gender. differences are not observed in the frequency of low back symptoms, males undergo surgery for disc herniation about 1.5-3 times as often as females. Spinal deformity, such as scoliosis and kyphosis, and leg length differences do not have a predictable predisposition to low back pain. There is also no strong association between body habitus and low back pain or sciatica. Some studies have demonstrated an association between tallness and low back symptoms. Surprisingly a similar finding for obesity has not been uniformly observed. An association between smoking and HNP and low back pain has been noted by several investigators. Numerous other individual risk factors have been examined although clear-cut relationships have not been forthcoming. Spinal Disorders Cervical and Thoracic Disorders: Most large epidemiological surveys lump cervical and thoracic pain with lumbosacraI symptoms, making it difficult to ascertain the relative incidence of these complaints. In one study, neck problems accounted for 7% of work absences related to "back" pain; thoracic problems accounted for only 0.2%. There may be a slightly greater frequency of cervical disc herniation observed in men as compared to women. The C5-6 and C6-7 discs are the most commonly affected. Increased risk for neck pain has been found to be associated with frequent lifting, cigarette smoking and frequent diving from a board, Driving, operating vibrating machinery, frequent head turning and several other plausible risk factors have not proven to be statistically significant. Thoracic spine pain is less common than pain localized to the cervical or lumbar regions. Symptomatic thoracic disc herniation is every more infrequent. Because complaints referable to Lite thoracic region are relatively uncommon especially in the context of 'back strain' or 'lumbago', and because certain disorders, such as metastatic tumors, may have a predilection for this region, the clinician should he suspicious of nondegenerative causes in looking for the etiology of thoracic pain (see section on spinal tumors). Historical background: Although the treatment of spinal disorders was discussed in the Edwin Smith papyrus and the writings of Hippocrates, surgery for these ailments was not generally undertaken until the latter part of the nineteenth century. The first successful laminectomy was probably performed by Paul of Aegina in the 7th century A.D., but this feat was not repeated until 1829 by Alban Smith of Danville, Kentucky. Elective spinal surgery required the development of anesthesia, aseptic techniques, improved instruments and, with the discovery of X-rays in 1895, improved diagnostic methods. Walter Dandy developed air myelography in 1918 at the Johns Hopkins Hospital. The difficulties in properly performing this procedure limited its widespread use in the spine, although pneumoencephalography became an important procedure for intracranial imaging. Sicard introduced iodinated contrast myelography in 1920, allowing the relatively accurate diagnosis of intraspinal pathology. Subsequent evolution in contrast agents from lipid soluble to water soluble to non-ionic water soluble agents has greatly enhanced the accuracy and safety of this diagnostic procedure, which remains as the "gold standard" in intraspinal imaging. Computed tomography (CT) was first used to image the brain in1972. Several years elapsed before high-quality spinal images were routine. The development of magnetic resonance imaging (MRI) soon followed with the first head scan being produced on May 18,1979 in Nottingham, England. Spinal imaging became available within two years and is rapidly becoming the imaging modality of choice for most spinal disorders. The syndrome of sciatica has been recognized since ancient times but the association of sciatic pain with lumbar disc herniation was not made until the twentieth century. Several descriptions of traumatic disc herniations existed in the pathological literature of the late 1800's and in the surgical literature of the early 1900's, but disc herniation was not linked with the genesis of sciatic pain. In 1929, Walter Dandy published two cases of sciatic pain associated with herniated disc fragments which responded to surgical discectomy. Unfortunately, the importance of this paper went largely unrecognized. During those years pathological specimens from what would now be called discectomy procedures were frequently interpreted as "chondromas". In 1934. Mixter and Barr published a paper describing their observations regarding the role of lumbar disc herniation as a common etiology of sciatic pain This revolutionized medical thinking at the time, ushering in a greater interest in the lumbar disc as a source of back and leg pain and in the surgical treatment of such disorders. Surgery for back and leg pain in association with nerve root compression has become one of the most commonly performed operative procedures. This enthusiastic and generally successful treatment of sciatica secondary to lumbar disc herniation resulted in a preoccupation with the. disc as a source of back pain by physician and the public alike. It is worth remembering, however, that disc herniation accounts for a small percentage of radiating leg pains and an even smaller proportion of back pain. Incidental herniations are not rare and may be observed in up to 25%-30% of myelograms or MRIs. Bulging discs, in which there is a diffuse bulging of the annulus into the spinal canal, are oven more common and are less likely to produce sciatica. The current management of patients with degenerative spine disease and low back pain involves physicians and allied health personnel from numerous disciplines including family practice, internal medicine, neurosurgery, physical medicine arid rehabilitation, orthopedics, neurology; psychiatry, anesthesiology, physical therapy, social work, orthotics and chiropractic. The number of proposed interventions for this group of patients is mindboggling. Many widely prescribed treatments have no evidence for efficacy. Other efficacious treatments, which may benefit subsets of patients, are indiscriminately applied. Clearly, the optimal management of these conditions requires a broad-based understanding of the pathophysiology of these disorders, astute clinical skills, and an unbiased appreciation of effective therapeutic interventions. Disc pathophysiology: The intervertebral disc consists of three parts: the annulus fibrous, the nucleus pulposus, and the cartilaginous endplates. The annulus, which forms the peripheral aspect of the disc, consists of collagenous fibers arranged in concentric layers. The fibers are oriented at a 30 degree angle to the horizontal and are embedded in an amorphous ground substance of proteoglycans and water. The nucleus also consists of these same components, although the amount of collagen is considerably less and the amount of proteoglycans is greater than the annulus. The annular fibers attach to the end plates and have dense attachment via Sharpey’s fibers to the periphery of the vertebrae above and below. The cartilaginous end plates consist of hyaline cartilage and provide an avenue for diffusion of nutrients from the bone of the vertebral bodies into the disc. Pathological evidence of degenerative changes within the disc is apparent beginning in the third decade. Fissures develop in the annulus and progress and enlarge throughout life. These fissures may extend in a radial direction completely through the annulus. Concurrent changes within the nucleus include a loss of water content, and necrosis of nuclear fibers and fibrosis. These pathological events significantly alter the biomechanical properties of the disc and therefore the spinal motion segment as a whole (the motion segment consists of two adjacent vertebral bodies and the associated ligaments and disc). These changes may then predispose to disc herniation or bulging, facet arthropathy and osteophyte formation as well as ligamentous laxity and “segmental instability". The mechanisms producing a disc herniation are not well understood. Attempts to produce herniated discs in cadaver spines by application of various loads have not been generally successful. Most acute loading conditions produce endplate fractures rather than posterolateral disc herniations. These finding suggest that most disc herniations are not the result of a single, acute traumatic event. Numerous structures in the region of the disc are innervated by nociceptive afferent nerves. These include the anterior and posterior longitudinal ligaments, the periosteum, vascular adventitia, the dura, and the posterior aspects of the annulus. The development of back pain in association with disc herniation may be the result of stimulation of these nerve endings. The nerve root is invested with its own nociceptor system, the nervi nervorum. It is presumed that the radicular pain associated with HNP is the result of stimulating these fibers. The neurological manifestations of nerve root compression (reflex inhibition, paresthesias, sensory loss and motor weakness) likely result from either direct compression by the disc fragment or from stretching the root between the herniation and the fibrous attachments of the root at the foramen. It is unclear whether disc herniation per se is a painful condition. The finding of incidental HNP on up to 30% of myelograms or MRIs would tend to support the view that the disc herniation itself is not the source of pain. On the other hand, some patients with radicular pain and HNP do give a prior history of low back pain which then evolved into a typical sciatic distribution. This may present pain arising from the disruption of the disc without root impingement. The degenerative processes occurring in the disc also impacts on the osseous elements. There is good evidence that disc degeneration leads to facet degeneration with the occasional subsequent development of facet hypertrophy, acquired spinal stenosis, ligament hypertrophy, synovial changes, “segmental instability” and the clinical syndromes associated with these changes. CLINICAL EVALUATION Low Back Disorders: T he clinical assessment of patients with degenerative spine disease must be heavily weighted toward the history. Pain is frequently the chief complaint and must be well-characterized. A complete description of the pain is critical including its location, quality, severity, onset and duration., Factors which aggravate or relieve the pain must be elicited as well as any associated symptoms. Some impressions regarding the impact that the pain is having on the patient in terms of work and leisure activities, sleep, mood and interpersonal interactions should are obtained. If the patient perceives the symptoms as the result of injury, the circumstances surrounding this event roust be documented. It is well known that extraneous factors, such as Workmen's Compensation, litigation and disability issues have a major impact on the response to treatment; therefore, they must be accounted for. The patient must be questioned regarding neurological symptoms, such as weakness or gait difficulties, clumsiness or bowel or bladder complaints. The patient should be questioned about numbness, tingling or other sensory changes. The distribution and character of these changes should be understood. The temporal course of the patient's symptoms is important as is a description of previous diagnostic and therapeutic attempts and the results. The past medical history should be elicited, both to evaluate for predisposing or associated conditions, as well as to determine the patient's fitness for various therapies (e.g. surgery). Because psychosocial factors are so influential in this patient population, a social history should also be obtained. The physical assessment emphasizes the musculoskeletal, neurological and peripheral vascular examinations. Lumbar radiculopathy: Pain which radiates from the hip or low lumbar region into the leg is commonly presumed to be the result of lumbar nerve root irritation and/or compression. The most common cause of lumbar nerve root compression is disc herniation. Other observed causes include compression by a hypertrophic facet joint, ligamentum flavum hypertrophy in association with stenosis of the lateral spinal canal, and intraspinal synovial cysts. Less frequently, spinal roots may be compressed by tumors or other masses. When the pain radiates down the posterior thigh and posterolateral calf approximating the distribution of the. sciatic nerve, it may be properly referred to as "sciatica", although this term predates the modern understanding that most sciatic pain is of radicular origin. Posterior thigh pain which does not extend below the knee may frequently be seen in patients without nerve root compression. This sort of referred pain can occur with sacroiliac joint inflammation, myofascial pain syndromes, facet syndromes and a number of other conditions. Pain which radiates into the anterior thigh may result from upper lumbar (L1, 2 ,3 and occasionally L4) root involvement. Other diagnoses such as meralgia paresthetica, femoral mononeuropathy (especially in diabetics), muscular strains and hip disease should be considered. Patients with true radiculopathy will often note an exacerbation of pain with cough, sneeze or Valsalva's. Also pain of radicular origin is frequently relieved by flexion of the knee (e. g. lying supine with the knee resting over a pillow). Physical findings in patients with lumbar radiculopathy may include motor loss, dermatomal sensory findings or reflex changes alone with nerve root tension signs i.e., positive straight leg raising (SLR) test. The femoral stretch test may be positive in patients with upper lumbar radiculopathy (see Table 1). Lumbar spinal stenosis: Lumbar spinal stenosis frequently presents as neurogenic spinal claudication. In this syndrome, patients describe pain involving the buttocks, thighs and legs which is brought on by ambulation and decreased by rest. These symptoms must be differentiated from true vascular claudication caused by occlusive arterial disease of the distal aorta or more peripheral arteries. Neurogenic claudication arises from ischemia of the cauda equina brought on by increased metabolic demand in the setting of tight stenosis of the spinal canal. Differential points between these two syndromes include the presence of normal peripheral pulses, and normal skin color and temperature in neurogenic patients. Patients with neurogenic symptoms also often describe relief of symptoms with the adoption of a flexed posture (e.g. will have greater exercise tolerance on a bicycle or when walking behind a shopping cart). Patients with lumbar stenosis may also describe low back pain and radicular symptoms in combination with or instead of, classic claudication. The neurological examination in patients with spinal stenosis is frequently normal. Occasionally, walking the patient to bring out the symptoms of claudication will yield positive findings on sensory or reflex testing. Straight leg raise is typically negative. Pain is occasionally elicited with lumbar extension. TABLE 1 Root Pain Pattern L2 Anterior thigh L3 Anterior thigh L4 Lateral thigh L5 Posterior lateral thigh; lateral calf Motor Symptoms Iliopsoas Sensory Symptoms Inguinal Reflex Change Iliopsoas; Quadriceps Quadriceps Anterior-lateral Thigh Anterior-lateral Calf Lateral calf; dorsum foot; great toe Knee Jerk Dorsiflexors; extensor hallucis longus None Knee jerk None S1 Posterior thigh; lateral calf; lateral foot Gastroc Lateral foot Ankle jerk Cervical and thoracic disorders: Degenerative conditions of the cervical spine are less frequent than those of the lumbar spine. Cervical disc herniation and cervical spinal stenosis are the most commonly seen conditions. Thoracic disc herniations account for less than 1% of disc herniations in the spine. Thoracic disc disease: Thoracic disc hernintion.is commonly an incidental finding on MR scans. Symptomatic thoracic disc herniation produces pain, sensory loss or weakness (myelopathy). Pain may be radicular -- following the course of an intercostal nerve -- or it may be spinal. Sensory findings in this context are usually consistent with an incomplete ventral or lateral cord lesion (e:g. a Brown Sequard pattern ). A sensory level is usually not present except with severe myelopathy. Motor findings are those of a spastic paraparesis (weakness, hyperreflexia, clonus, hypertonus, Babinskis). Cervical radiculopathy: Root compression in the cervical spine produces characteristic symptoms analogous to those in the lumbar region (Table 2). The numbering of cervical roots is such that a given root exits above its like-numbered vertebral body. Thus a C6 root will exit the C5-6 foramen and will be compressed by a herniation of the C5-6 disc. Although disc herniation is the most common cause of cervical radicular symptoms, foraminal stenosis as a result of osteophytes may produce an identical syndrome. Cervical radiculopathy is frequently first noted upon awakening without an identifiable precipitation event. The question of a cardiac source of pain is often raised when the radiculopathy is left-sided. Neck pain and pain with neck movements are important differentiating factors. The pain of cervical radiculopathy is often brought on with axial neck compression associated with lateral flexion to the symptomatic side (Spurling’s sign) or by downward traction of the involved arm with lateral neck flexion to the opposite side. Conversely, many patients report relief of symptoms by abducting their shoulder and placing their hand on their head. Cervical myelopathy: Symptoms resulting from compression of the cervical spinal cord are most commonly caused by disc herniations or spinal stenosis. The latter may occur as a result of a congenitally narrow cervical spinal canal but is usually associated with spondylotic changes (osteophytes, disc bulged, facet and ligament hypertrophy). Infrequently spinal canal narrowing is produced by ossification of the posterior longitudinal ligament (OPLL). The radiographic changes consistent with spondylosis are common after age 40 and demonstrate increasing incidence with increasing age. The measurement of spinal canal diameter on lateral radiographs taken at 3 feet tube-to-plate distance can be used to predict probable spinal cord impingement. The average A-P diameter in the mid and lower cervical spine in 17mm-18mm. Measurement less than 11mm are consistent with significant spinal cord impingement. The spinal cord may be compressed even when larger spinal cord diameters are noted because soft tissue, such as disc or ligamentum, may encroach on the spinal canal. Varying patterns of clinical signs and symptoms may be noted. Their relative frequencies are seen in Table 3. TABLE 2 Findings in Cervical Radiculopathy Disc Level Percent Cervical Discs Root C4-5 C5-6 20% C6-7 70% C7-T1 C5 C6 C7 C8 Reflex Pectoral Triceps Finger Jerk Motor Symptoms Deltoid (Biceps) Shoulder Biceps; Brachioradialis Biceps; Brachioradialis Radial Forearm; Thumb, Index Triceps; Wrist Extensors Dorsal Forearms; Middle Finger Hand Intrinsics Sensory Symptoms Ulnar Hand, Forearm Cervical myelopathy is frequently of insidious onset and is usually progressive. Acute worsening is occasionally seen as are periods of static symptoms lasting months or even years. Patients commonly describe symptoms of numbness or weakness of the hands, citing difficulty manipulating small objects. Proximal lower extremity weakness is often noted as is stiffness (spasticity). Patients may be aware of clumsiness of their gait and a tendency to fall. Overt sphincter disturbance is uncommon but urinary urgency is often reported. Amyotrophic lateral sclerosis (ALS) is an important differential consideration in some cases. Table 3: Findings in Cervical Myelopathy FINDINGS Pure Myelopathy Myelopathy + Radiculopathy Hyperreflexia Babinski Sensory Level Posterior Column Dermatomal Arm Arm Weakness Paraparesis Hemiparesis Quadriparesis Brown-Sequard Muscle Atrophy Fasciculations PERCENT 59% 41% 87% 54% 41% 39% 33% 31% 18% 18% 10% 10% 10% 10% Radiological Evaluation: The radiologic evaluation of degenerative disease of the spine must be individualized. Extensive and expensive study is generally not indicated in patients who are not surgical candidates. The types of evaluation that may be performed include plain radiographs, dynamic radiograms (e.g. flexion-extension films), CT scanning (with or without intrathecal contrast), myelography, an MR scanning. Radio nuclide bone scanning is occasionally helpful. Other ancillary tests such as discography are rarely performed and their value may be questioned. Plain radiographs: The role of plain films in the evaluation of degenerative spine disease is somewhat limited. Nonetheless they are a useful screening tool to rule out bony destruction as seen with neoplasm or infection, and to visualize deformities, fractures or subluxation. Hyper mobility on flexion-extension films may be associated with pain or neurological symptoms. Vertebral movement of more than 4mm to 5mm in the lumbar region or more than 3mm in the cervical region should be considered abnormal. CT scan: CT is often useful in the evaluation of a variety of disorders. It provides excellent visualization of bony detail. Disc material can often be differentiated from the thecal sac on plain CT of the lumbar spine. This test is less expensive than MR scanning or myelography, but is less likely to be diagnostic in most cases. In cases of far lateral disc herniation, CT is superior to myelography. A major disadvantage of CT scanning is visualization in only the axial plane. In spinal degenerative disease, CT has the advantages of excellent bony detail. It is noninvasive, and can be done as an outpatient procedure. It has a faster scanning time as compared to MR scanning. It is less expensive than MR scanning. It visualizes paraspinal soft tissue. It is often adequate for making a diagnosis. Table 4 Advantages to CT in-Spinal Degenerative Disease Excellent bony detail Noninvasive, outpatient procedure Faster scanning time .vs MR Inexpensive Visualizes paraspinal soft tissue Often adequate for diagnosis Myelography: Myelography is currently performed in conjunction with CT scanning. This study remains as the gold standard for evaluation of most degenerative conditions of the spine. It is, however, are invasive test but it can be done on an outpatient basis. Some morbidity is to be expected (most commonly "post myelogram headache" seen in roughly 10%). Myelography may provide a more "dynamic" sense of the pathology in that films can be obtained after changes in position (e.g. a myelographi (block in cervical stenosis may allow passage of contrast with changes in neck position). Root impingement, especially in the cervical spine, is probably more clearly demonstrated on myelography than on MR scanning. MR scan: Magnetic resonance imaging will be the first imaging study obtained for the evaluation of most patients presenting with hack or neck pain or radiculopathy. MR scanning will be diagnostic in most instances as it provides excellent anatomic resolution and allows visualization in multiple planes. Contrast enhancement with gadolinium is very helpful in distinguishing scar from recurrent disc in the previously-operated patient. Disadvantages to MR scanning are the relatively long scanning times which may not he tolerated by patients in severe pain or who are claustrophobic, the expense, the high level of operator skill required to produce consistently excellent image and the inability to scan patients with certain implants (cardiac pacemakers, ferromagnetic aneurysm clips etc.) Bony detail is also not as well demonstrated on MR as with CT. TREATMENT Lumbar Disc Herniation: Most (80%+) patients with acute lumbar radiculopathy will improve without surgery, therefore a trial of nonoperative therapy is appropriate with the primary goal of palliating painful symptoms until resolution occurs. Generally if symptoms are severe, a few (2-3) days of bed rest are appropriate. Longer regimens are not clearly more beneficial. Analgesics are usually required. Nonsteroidal anti-inflammatory drugs (NSAIDS) may be prescribed for this purpose. Occasionally narcotic (codeine, oxycodone) or propoxyphene are necessary for adequate pain control. So-called muscle relaxants are probably of limited value, although their sedating effect may help patients comply with bed rest. A number of therapeutic modalities have been proposed for the treatment of back pain and radiculopathy, most with tenuous evidence of efficacy. These include physical therapy, spinal manipulation, acupuncture, TENS and traction. The duration of non-operative treatment must be individualized, but generally, a period of 4-6 weeks is considered appropriate before surgery is contemplated. Clearly the presence of a neurological deficit alters these considerations. The development of a cauda equine syndrome (urinary retention, perineal numbness, bilateral motor deficits, sphincter paresis) is an indication for emergent surgery. Table 5 Indications for surgery in lumbar herniated nucleus pulposus (HNP) Failure of nonsurgical management Cauda equina syndrome Acute or progressive motor deficit Severe pain not responding to analgesics (rare): Lumbar spinal stenosis: Patients with neurogenic claudication secondary to spinal stenosis should be given a trial of nonoperative management because symptom severity may wax and wane, and patients may achieve a tolerable level of symptoms without surgery. NSAIDS, rest and physiotherapy are all appropriate early in the management of these patients. Surgical decompression is reserved for those individuals with refractory symptoms. Serious neurological deficits are very unusual in this disorder. Operative treatment consists of relieving spinal canal and individual nerve root compression by means of bony removal. Hypertrophic facets and ligamentum flavum are removed along with any impinging disc material. This is most. frequently accomplished via a laminectomy although various modifications have been described, consisting of removal of lesser amounts of bone (laminotomies) Spinal segment instability is both a preoperative and a postoperative consideration and may be an indication for concomitant spinal fusion in a subset of these cases. Thoracic disc herniation: Operation in thoracic disc herniation is most often indicated for neurological deficits (myelopathy). The approach is either through a thoracotomy which allows a very ventral trajectory to the disc approaching the problem .away from the neural elements; or through a paramedian approach which does not enter .the chest cavity. This latter approach is more useful when the disc fragment is laterally situated in the canal. Both of these approaches are considerably more difficult than the surgery for lumbar disc herniation and are associated with greater risks of morbidity. Cervical disc herniation: As in lumbar radiculopathy, most patients with arm pain from a cervical disc will recover spontaneously. Initial treatment should consist of rest (avoidance of activities which exacerbate symptoms), NSAIDS, cervical traction (home cervical traction 7-10 pounds for 15-20 min TID), and when pain has improved, physical therapy. Narcotic analgesics and ‘muscle relaxants,’ may be necessary when symptoms are severe. Upper extremity motor weakness, if moderate or severe, is an indication to abandon nonoperative therapy and consider surgery. Patients who present with signs and symptoms of spinal cord compression should be considered for early surgery. There are two main surgical approaches to deal with cervical disc herniation; either an anterior operation or a posterior approach. Each technique has its advantages and indications. The posterior approach is well suited to lateral disc herniations, especially if there are concurrent lesions at more than one level. The anterior interbody approach is best for central disc herniations with spinal cord compression, but it is also a very effective means for treating radiculopathy secondary to a disc herniation. Cervical stenosis: Surgery is generally indicated for treatment of progressive myelopathy resulting from spinal canal stenosis. Several different operative approaches are available for different circumstances. The nature of the compression must be carefully evaluated preoperatively. When the cord is compressed ventrally, consideration should be given to an anterior approach. Stenosis is usually most marked adjacent to the disc spaces because of ventral oseophytes (“bars”) so that decompression at the disc space may be sufficient. In some cases, greater bone removal is required usually in the form of a “trough corpectomy” where a slot of bone is removed spanning the necessary number of spinal segments. In this situation, the spine is fused usually with a strut graft and sometimes with internal fixation such as a cervical plate. In some cases, especially with a congenitally-narrow spinal canal, a posterior decompression is the appropriate operation, and is achieved by multilevel laminectomy or by “laminoplasty” in which the laminar arches are cut but then reattached in a way to provide a roomier spinal canal while maintaining the posterior elements. The result from cervical decompression for myelopathy are sometimes disappointing. Patients occasionally progress in spite of an apparently adequate decompressive operation. The cause for this is unclear although contributing factors might be some degree of minor instability or selection of the wrong surgical approach. It is estimated that 70%-80% of patients are improved by surgery, although there may be a falloff in good results as patients are followed over time. Spasticity, if pronounced preoperatively, may continue to be a problem postoperatively. Baclofen may be indicated in these cases to try to reduce the increased muscle tone. SPINAL TUMORS A variety of tumors affect the spine, spinal cord, nerve roots, and associated structures. From a clinical and anatomical standpoint, these lesions may be classified as spinal (or vertebral), epidural, intradural extramedullary, and intradural intramedullary. Although some tumors overlap these various compartments, thinking about spinal tumors in this way is relevant both from the perspective of developing a differential diagnosis, and in terms of planning further evaluation and treatment. Spinal column and epidural tumors: Tumors involving the vertebral column and adjacent epidural space include metastatic lesions from a variety of sources, primary tumors of bone and cartilage, tumor, of lymphocytic origins (e.g. plasmacytoma, myeloma, lymphoma), vascular elements (hemangioma), nerve sheath (e.g. schwannoma), and other lesions such as chordoma, eosinophilic granuloma, meningioma, etc. Metastatic tumors: The spine is the most common site for osseous metastasis. When one considers that: approximately one million new cases of cancer are diagnosed annually, approximately two-thirds of cancer patients eventually develop metastatic disease, and skeletal metastasis ranks third after metastasis to the lung and liver, it is apparent that metastasis will be the most common form of spinal neoplasm. The most common solid tumors to secondarily involve the spine are: breast, prostate, and renal carcinomas, which account for nearly 80% of vertebral metastases. Tumors of unknown primary account for about 5%-10% of cases. Metastases of hematopoietic neoplasms account for about 4%-10% of most series. The incidence of spinal metastases appears to increase in a rostrocaudal direction and probably is a function of the volume of cancellous bone within the vertebrae which also increases rostrocaudally. When the level of involvement for symptomatic lesions is considered, however, thoracic levels appear more common. Undoubtedly, this is because the thoracic spinal canal, being smaller, is more readily compromised and cord compression is more likely to ensue. Approximately one-third of vertebral metastases are asymptomatic. The vertebral body is the most common site of involvement, although the pedicles, transverse processes and posterior elements maybe involved. Solely epidural tumor without bony involvement is occasionally noted. Multiple sites of involvement in the spine are often seen. Non-contiguous multiple metastases are seen in at least 15% of patients. Metastatic disease producers symptoms by several mechanisms. Bony destruction with fracture or distortion of periosteum and ligaments produces localized pain. Collapse produces deformity. Spinal instability may be associated with pain or deficits. Neurological deficits and radicular pain occur because of direct compression by tumor or by partially destroyed vertebral elements. The most common symptom of vertebral metastasis is pain, which occurs as the presenting complaint in up to 95% of patients. Pain may result from bony destruction causing stimulation of nociceptors in periosteum and ligaments, or it may be the result of neural compression (particularly the spinal roots), causing a radiating pain. Finally, patients my occasionally experience generalized pain in the lower extremities below the lesion, perhaps as a results of spinal cord compression (possibly due to spinothalamic tract involvement). The pain of vertebral metastasis may be associated with movement and weight-bearing much like other causes of spinal pain. However, pain during recumbence, particularly that which awakens the patient from sleep, should raise the question of spinal tumor. Motor weakness is the most common finding on neurological examination in patients presenting with vertebral metastasis. The pattern of neurological deficit is, of course, dependent on the level of spinal involvement. Lesions above T10 (spinal cord level) will generally produce a spastic paraparesis (or in the cervical region, quadriparesis) with the findings of weakness, hyperreflexia, and extensor plantar responses. Lesions at the level of the conus medullaris and cauda equina will give rise to a flaccid paresis which, if longstanding, is associated muscle atrophy and a flaccid bladder. Lesions laterally located in the canal in the cervical region may initially affect the ipsilateral arm and leg. Autonomic dysfunction may be seen with lesions in the upper thoracic or cervical regions. Sphincter disturbances usually occur late in the course of neurological deterioration. The exception is for lesions arising at the conus medullaris where bowel and bladder disturbance may be apparent earlier. Sensory loss is also frequently observed and with high grade lesions a "sensory level" may be determined. With incomplete deficits, the sensory level may not correlate with the vertebral level of involvement and may suggest a level of involvement more caudal than it actually is. Partial lesions may also produce sensory loss primarily of spinothalamic (ventral and lateral) or dorsal column (dorsal) modalities. Asymmetrical involvement is frequently seen. Diagnostic evaluation: Plain radiographs are generally the first modality used to evaluate patients suspected of having a spinal tumor. They are, however, fairly insensitive measures of neoplastic involvement and normal radiographs do not rule out a spinal tumor. Inability to visualize a pedicle on an AP film is a common radiographic sign of metastatic disease. Vertebral collapse or lytic changes should be looked for as well as increases in paraspinal soft tissue shadows. Osteoblastic changes are suggestive of specific primary tumors: prostate and breast are commonly blastic. Bladder, thyroid, carcinoid tumors, or testicular cancer may also have blastic metastases. Radionuclide bone scans are sensitive but non-specific for metastatic bone disease. Technetium scans may be positive weeks or even months before radiographic changes are detectable. False negative scans may occur when the metastatic process is growing rapidly without bony reaction. Examples of tumors associated with false negative scans include: renal or lung carcinoma, multiple myeloma, lymphoma, leukemia, and Ewing’s sarcoma. Computed tomography (CT) is both sensitive and relatively specific for metastasis with bony destruction. Limitations included poor visualization of the contents of the spinal canal, lack of multiplanar imaging and difficulty imaging large areas of the spine. Combining CT with myelography will eliminate many of these problems. Myelography may be disadvantageous for several reasons: it is invasive, neurological deterioration may occur after a myelogram performed below a complete spinal block (presumably as a result of CSF pressure differentials), and evaluation of patients with a complete block may require both a lumbar and lateral C1-2 puncture. Magnetic resonance imaging (MR scanning) has become the imaging modality of choice for many clinical situations in which the differential diagnosis of spinal tumor has been raised. MR provides considerable spatial resolution, allowing the localization of lesions to the appropriate spinal compartment. Additionally, the nature of the lesion may be suggested by signal characteristics on T1, T2 and proton density (PD) weighted images as well as by uptake of gadolinium enhancement. Changes in bone marrow signal characteristics are frequently a sensitive indicator of metastatic vertebral involvement. MR is particularly useful for the diagnosis of intramedullary tumors and cysts. Relative disadvantages to MR imaging in the diagnosis of spinal tumors include the longer imaging times which may not be well tolerated by patients who are acutely ill or in severe pain. Bony detail is less well seen on MR than CT. The quality of imaging on MR is also more operator-dependent than some other modalities so that inexperienced personnel (e.g. at night) may not generate studies of the usual quality. Occasionally small or cystic lesions in the subarachnoid space will be missed on sagittal MR scans, so complete multiplaner imaging should be done. These few concerns notwithstanding, MR scanning is generally the first imaging study that should be done in a patient with signs and symptoms compatible with cord, nerve root or cauda equina compression. Laboratory evaluation: Few laboratory studies are specifically helpful in the diagnostic evaluation of a patient suspected of having a spinal tumor. Routine laboratory evaluation, including CBC, platelets, serum electrolytes and glucose, liver function tests calcium, magnesium, albumin and urinalysis will be useful in evaluating a patient’s general status. PT, PTT and possibly a bleeding time are appropriate if surgery or invasive procedures are contemplated. In a patient suspected of having a plasma cell dyscrasia, urine for Bence-Jones proteins and serum protein electrophoresis may be helpful in suggesting a diagnosis. PSA testing may allow diagnosis of prostate carcinoma. Occult blood on urinalysis should raise the question of renal cell Ca. Lumbar puncture is rarely helpful although CSF protein levels may be elevated and, in the setting of a complete block, the closing pressure drops rapidly. It should be remembered, however, that lumbar puncture may precipitate neurological worsening. Metastatic workup Common sense should be employed when performing a search for the primary tumor (or other metastases) in patients with possible spinal metastasis. Remember that up to 10% of spinal metastases have unknown primary tumors even after autopsy study. If surgery appears to be indicated in any case, extensive testing beforehand may add little. Assuming the patient's clinical condition allows, studies to look for the most common primary sites is appropriate. Chest and spine radiographs, breast examination and possibly mammography, rectal examination, stool guaiac and evaluation of the appropriate laboratory studies (above) is a reasonable battery of tests. More extensive evaluation can be undertaken in specific situations. Treatment: Treatment of metastatic involvement of the spine must be individualized with special attention to the issues of spinal stability, pain, neurological deficit, and duration and rate of evolution of symptoms. It may be useful to subdivide patients into three groups for treatment based on the severity of neurological findings: Group 1: Signs/symptoms of new or progressive cord Compression. These patients are at high risk for rapid deterioration and require immediate evaluation. Group 2: Radicular signs/symptoms or mild stable signs of cord compression. These patients generally should be admitted and evaluated within 24 hours. Group 3: Pain in the absence of neurological signs or symptoms. These patients may be evaluated over several days usually as an outpatient. Steroids: There is little doubt that corticosteroids are beneficial in the management of patients with neoplastic spinal cord compression. Some controversy surrounds the optimal dose in this context. Some clinicians advocate large doses (e.g. 100mg Spinal Disorders dexamethasone bolus followed by 25mg qid for several days for acute spinal cord compression). Others cite steroid-related complications, such as infections, hyperglycemia, intestinal perforation arid mental status changes as reasons to use more moderate doses. Conclusive data are lacking. For short-term use in neurologicallycompromised patients (Group 1), the risks of high doses appear small, but definitive treatment must be initiated expeditiously. Smaller doses (4mg-10mg dexamethasone qid) are appropriate in Group 2 or 3 patients during evaluation. Radiation Therapy (R;T): An extensive literature documents the beneficial effects of radiation therapy for a large number of solid tumors causing cord compression. Approximately 1/3-1/2 of treated patients improve and are able to walk at the completion of therapy. Half of these patients maintain this ability at one year. Pain relief is noted in about 50%. Response to therapy is related to radiation sensitivity of the tumor and initial neurological grade. A typical treatment involves 200cGy per day to total of 3000eGy3500cGy, although treatment is individualized with respect to fractionation, fields and dose. Some tumors involving the spine are particularly radiation-sensitive or tend to be treated first by radiation alone or radiation and chemotherapy after biopsy to confirm diagnosis. Examples include: Ewing's sarcoma, primary lymphoma, and solitary plasmacytoma. Surgical Treatment- Surgical management of spine lesions has undergone Considerable evolution in the last two decades. The two most significant areas of development are: the proliferation and popularization of various approaches to the spine, notably anterior and anterolateral approaches, and the advances in internal fixation technology for reduction and stabilization of the spine. Additionally, improved imaging has aided preoperative planning and has resulted in earlier diagnosis. Laminectomy is no longer the primary procedure performed for neoplastic spinal cord compression. Surgery is indicated for the treatment/evaluation of suspected spinal metastasis in the following circumstances: (1) To obtain a diagnosis (e.g. unknown primary) (2) When there is associated spinal instability or deformity secondary to neoplastic vertebral destruction (3) When neurological deficits progress during or after a course of irradiation (4) When cord compression is the result of bone in the spinal canal (5) In certain radio-resistant tumors (e.g. renal cell carcinoma) (6) When rapid progression to severe neurological deficit has occurred and patient can be operated on soon after onset (<.24 hours) The surgical approach must be tailored to the specific problem. Metastatic cord compression is usually ventral anti thus requires an anterior or anterolateral decompression. This may require a thoracotomy or extraperitonal exposure. Decompression generally must be followed by reconstruction/stabilization. This is most often accomplished with rods or plates affixed to the spine by means of hooks, screws or wires. A large variety of implants are currently available for instrumenting the spine, many having originally been devised for the treatment of scoliosis or fracture. Most such implants are made of titanium, which is quite strong and resistant to fatigue fracture. Titanium is more expensive than stainless steel, but introduces fewer artifacts on CT and MR scans. PRIMARY BONE TUMORS Aneurysmal bone cyst (ABC): This is not truly a neoplasm. It affects children and young adults. Fifteen percent of ABCs are spinal and generally involve the laminar arch and posterior elements (60%). They may be associated with osteoblastoma or other tumors. They may involve adjacent vertebrae. The treatment of choice is surgical excision, as they may recur after curettage. Osteod Osteoma: This is a benign, bone forming tumor. Ten percent are spinal. They have a predilection for the posterior spinal elements. By definition; they are less than 1.5 cm in diameter (see osteoblastoma). Classically they present with localized pain which is dramatically relieved by aspirin. The lack of an aspirin response (seen in approximately two-thirds), does not rule out this lesion. A bone scan is the most sensitive study. The lesion will be seen on CT often as a “target” of dense bone surrounded by a halo of resorption. The. treatment is surgical excision. Osteoblastoma: This is a benign, bone forming tumor (<1 % of all bone tumors). Histologically, it is identical to osteoid osteoma but characterized by growth (>1.5 cm). More than 40% involve the spine. A plain film demonstrates expansion of cortical bone. The treatment is surgical excision if possible. Curettage and-bone grafting may yield satisfactory results but recurrence can occur. The recurrence rate with initial total gross removal is approximately 10%. Hemangioma: These are benign vascular lesions generally involving the vertebral body. They are found incidentally on approximately 10% of spinal MR scans and are rarely symptomatic. A minority are associated with pain or neurological symptoms. Plain radiographs typically demonstrate a classic "corduroy cloth" appearance with thickened trabeculation of the involved body. The treatment must be individualized. It may include radiation, surgery and embolization. The latter may be an adjunct to surgical excision or radiation but is not presently useful as definitive therapy alone. Giant cell tumors: They are often slow-growing but may be locally aggressive. They most commonly involve the vertebral body. Recurrence is common with partial resection. Radiation induced sarcomas may occur especially with higher doses. The Treatment is complete excision where feasible. Radiation may be appropriate for nonresectable lesions. Eosinophilic granuloma: This is usually a benign condition affecting children usually before age ten. Vertebral lesions constitute 10%-15% of these tumors and most often affect the vertebral body. Vertebral collapse producing a "vertebra planum" may occur. Neurological compromise may result requiring decompression and stabilization. Multiple lesions and poorer prognoses may be noted in Hand-Schuller-Christian disease and LettererSiwe disease. Treatment consists of biopsy, spinal decompression and stabilization, and radiation therapy. Benign cartilage tumor: (Osteochondromas and Enchondromas). Osteochondromas are not true neoplasms. They consist of a cartilage-capped, bony growth, first noted in childhood, arising adjacent to an epiphyseal plate. Although usually solitary, a hereditary form, multiple osteochondromatosis, occurs as an autosomal dominant disorder. Spinal involvement with these lesions is rare. Enchondromas, which are benign intraosseous tumors of hyaline cartilage, generally occur in the hands and feet. Syndromes of multiple enchondromatosis occur but rarely involve the spine. Malignant degeneration of these lesions into chondrosarcoma is not infrequent in these latter syndromes. Chondrosarcoma: This is a malignant tumor of cartilage, second in frequency to osteosarcoma as a primary sarcoma of bone. It occurs more frequently in males. The mean age of occurrence is approximately 40 years. It is most common in the pelvis, femur, scapula and humerus. Fewer than 4% arise in the spine or sacrum. The treatment of choice is complete en bloc excision (which is rarely feasible in the spine). Wide excision is usually performed. Radiation and chemotherapy are of little benefit. Chordoma: These are rare primary malignancies arising from notochordal remnants. They occur in the axial skeleton (clivus 35%, sacrurn 50%, vertebral column 15%). They account for 1%-4% of malignant bone tumors. The male to female ratio is 2:1. They occur in all age groups with peaks after the fifth decade. Radiologically an osteolytic soft tissue mass is usually seen with stippled calcification. The treatment is complete surgical excision. Radiation therapy may have a limited role for palliation because these lesions are not radiosensitive. Osteosarcoma is the most common primary malignant tumor of bone. It represents 20% of osseous tumors with an incidence of 2:1.,000,000. The peak incidence is in the second decade (associated with the growth spurt). 1%-3% arise in the spine. Paget's disease is a predisposing condition in older adults. The treatment is wide excision. Adjuvant chemotherapy and local radiation therapy is usually given. The prognosis is very poor. Other sarcomas and primary malignancies: Other types of sarcomas of the spine are relatively uncommon. These include fibrosarcomas, rhabdomyosarcomas- and tumors arising from other cells of origin. It has been estimated that <1000 cases per year are seen in the U.S. The treatment is generally like that for sarcomas elsewhere, although en bloc excision is rarely feasible. Plasma cell tumors: This tumor is composed of malignant plasma cells. It presents as solitary lesions in 3%. It is most commonly systemic (multiple myeloma). The male to female; ratio is 3:1. - The age of patients is usually <50 years at presentation. The spine is the initial site in 25% -50% of cases. Pain is the most common presentation. A lytic lesion is seen on radiographs. The bone scan may be negative. The treatment is radiation therapy as the primary modality. Surgery is done for stabilization of the spine. Chemotherapy is given for progressive systemic disease. INTRADURAL EXTRAMEDULLARY TUMORS The differential diagnosis of masses in this compartment is considerably different from extradural lesions. Intradural metastasis is uncommon, accounting for only 1%-5% of spinal metastatic disease from systemic malignancies. Occasionally, cerebrospinal spread of CNS neoplasms may result in solid metastases in the spinal compartment. This is perhaps most commonly seen in medulloblastoma, but is also recognized in other tumors, including primitive neuroectodermal tumors (PNET’s), malignant glial neoplasms (glioblastoma, highgrade ependymomas and oligodendrogliomas) and intracranial sarcomatous tumors. The most common tumors in adults in the intradural extramedullary space are meningiomas and benign nerve sheath tumors (schwannomas and neurofibromas). Spinal ependymomas, which are often intramedullary in the spinal cord, may also arise from the filum terminale and appear as extramedullary growths. The myxopapillary variant of ependymoma is commonly seen in this location. Dermoid and epidermoid lesions may be found in the lumbar or lumbosacraf level. Teratomas and lipomas often occur in association with spinal disruption in the lumbosacral region. Nerve sheath tumors, including schwannomas (neurilemmomas) and neurofibromas are the most common intradural extramedullary lesions. They predominate in the lumbar region. There is a slight male preponderance. Roughly 72% are intradural extramedullary, 14% are solely extradural, 13% are "dumbbell" (involving both compartments along an exiting nerve), and 1% are intramedullary. Neurofibromas, and to a lesser extent spinal schwannomas, may be associated with von Recklinghausen's neurofibromatosis (NF-1). In the context of NF-1,malignant degeneration of neurofibromas to neurofibrosarcomas usually occurs. The treatment is surgical excision. Recurrence is uncommon with complete resection Meningiomas are the second most common intraspinal neoplasm. They are most common in the 4th-6th decades. Women are affected 8-10 times more often than men. These lesions generally involve thoracic levels and are often anterior or anterolateral in the canal. They are usually well seen on MR scans and enhance brightly with gadolinium. The treatment is surgical excision. Radiation or chemotherapy are not indicated for these benign lesions. Ependymomas are often considered as intramedullary lesions (see below), but most commonly arise from the filum at the lumbar level. There is a male predominance with presentation usually in the 3rd or 4th decades. Although generally benign in this location, malignant behavior can be seen. The treatment is total excision when possible. Radiation therapy is reserved for malignant or incompletely excised lesions. Dermoids, epidermoids and teratomas are uncommon lesions generally seen in the pediatric age group. They are congenital and are often associated with other anomalies, such as dysraphism, dermal sinus tracts, and cutaneous lesions (such as angiomas and hairy patches or lipomas). Although most common in the lumbosacral area, they may occur throughout the spine. The treatment is surgical excision. Teratomas of the sacrococcygeal region may undergo malignant change.