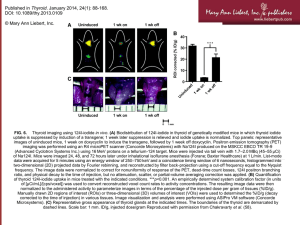
THYROID - Caangay.com

THYROID
James Taclin C. Banez, M.D., FPSGS, FPCS
•
•
•
•
ANATOMY:
Location / Parts
Arteries / Venous drainage
Nerve Supply
•
•
Sympathetic ( cervical ganglion )
Parasympathetis ( vagus )
Histology:
• Thyroid follicle ( thyroglobulin )
• C cells ( neuroectoderm – 4 th and 5 th ultimo brachial bodies ).
•
•
PHYSIOLOGY:
1.
2.
3.
4.
Synthesis & secrets thyroid hormone (thyroid follicle)
Iodide uptake
Oxidation of iodide to iodine
•
Organification (thyroxiniodine) MIT / DIT
Coupling of inactive iodotyrosine T4 /T3
Stored ----> released by protease / peptidase
Calcium Level
• Calcitonin (C cell)
3.
4.
1.
2.
5.
6.
Evaluation of Thyroid Diseases
Clinical history and physical examination
Serum T3 & T4,
TSH
determination
Thyroid scan
Thyroid ultrasound
CT scan / MRI
FNAC
A.
2.
3.
1.
HYPERTHYROIDISM
(Thyrotoxicosis)
With increase thyroid hormone secretion
Grave’s disease
Toxic nodular goiter
Toxic thyroid adenoma
B.
1.
With out increased thyroid hormone secretion
Sub-acute thyroiditis
2.
3.
Functioning metastatic thyroid cancer
Struma ovarii
HYPERTHYROIDISM
•
•
•
•
GRAVE’S Disease (Diffuse Thyroid Goiter)
Most common form of thyrotoxicosis
Autoimmune
Female > male; most prevalent 20-40 y/o
Thyroid stimulating antibody
(immunoglobulin) directed at the TSH receptor or the thyroid follicular cells.
•
•
LATS (long acting thyroid stimulating antibody)
TRAb (thyroid receptor antibody)
HYPERTHYROIDISM
•
GRAVE’S Disease (Diffuse Thyroid Goiter)
Manifestations:
•
Signs/symptoms of thyrotoxicosis:
•
•
• heat intolerance sweating weight loss, muscle wasting
•
•
•
•
•
•
•
• tachycardia/atrial fibrillation fine tremors easy fatigability hypoactive tendon reflexes amenorrhea decrease fertility easy fatigability, agitation and excitability diarrhea
•
•
HYPERTHYROIDISM
GRAVE’S Disease (Diffuse Thyroid Goiter)
Triad:
•
•
• diffuse goiter thyrotoxicosis exopthalmos
Other:
• hair loss
•
•
• pretibial myxedema gynecomastia splenomegally
HYPERTHYROIDISM
•
GRAVE’S Disease:
•
Exopthalmos:
Due to increase retro-bulbar tissue:
•
•
•
Spasm of the upper eyelid, revealing the sclera above the corneoscleral limbus
(Dalrymple’s sign)
Lid lag (von graefes sign)
External ophthalmoplegia
(inability to move the eyeball)
•
•
Supra and infraorbital swelling
Congestion and edema of the conjunctiva and sclera (chemosis) -
---> ulceration
Progression --> damage of optic nerve --> decreases visual acuity and impairment of color vision
( malignant exopthalmos ) not corrected surgically --> blindness
•
•
•
HYPERTHYROIDISM
Diagnosis:
•
•
•
Autonomous thyroid function
Low TSH
Elevated T3 / T4
Thyroid scan ---> diffuse elevated iodine uptake
•
•
Treatment:
1.
2.
3.
Choices:
Antithyroid drugs
Radioactive iodine therapy
Surgery
1.
Choice depends on:
Age
2.
3.
4.
5.
Severity of the disease
Size of the gland
Coexistent pathology (Ophthalmoplegia)
Other factors: a.
b.
Patient’s preference
Pregnancy
3.
1.
2.
HYPERTHYROIDISM
Antithyroid Drugs:
Propyl thiouracil (PTU)
Methimazole (Tapazole)
= 100-300mg TID
= 10-20 TID then OD
Carbimazole = 40mg OD
•
•
• a.
c.
b.
Inhibits the organic binding of iodine and coupling of iodotyrosine
PTU can also lower conversion of T4 to T3; it can also decrease thyroid autoantibody levels
Disadvantage of these drugs.
Crosses the placenta --> inhibits fetal thyroid function
Excreted in breast milk
Side effects: a.
b.
c.
d.
e.
f.
Skin rashes
Fever
Peripheral neuritis
Polyarteritis
Granulocytopenia (reversible)
Agranulocytosis / aplastic anemia (poor prognosis)
•
HYPERTHYROIDISM
Beta blockers (propranolol) – to alleviate peripheral adrenergic effects
•
Advised medical management
•
Small diffusely enlarge gland or larger glands that decreases in size due to antithyroid drugs
•
Toxic nodule goiters or large diffuse glands or hyperthyroidism when drug was discontinued -
--> thyroidectomy / radioactive iodine
HYPERTHYROIDISM
Radioactive Iodine Therapy:
Advantages:
•
•
Avoidance of surgery (no injury to nerve / parathyroid gland)
Reduce cost & ease of treatment
Disadvantages:
•
Lifelong thyroxin replacement therapy
•
•
•
Slower correction of hyperthyroidism
Higher relapse rate
Adverse effect of ophthalmopathy
Suitable treatment:
•
Small or moderate size goiter
•
•
Relapse after medical and surgical therapy
Antithyroid drug and surgery are contraindicated
Contraindicated:
•
•
•
•
Pregnant / breast feeding
Ophthalmopathy (progression of eye signs)
Isolated nodular goiter or toxic nodular goiter
Young age (children/adolescence ----> Infertility / carcinoma
HYPERTHYROIDISM
Radioactive Iodine Therapy:
Pt. is placed in euthyroid state with anti-thyroid drugs. Then discontinue the drugs for 2-3 wks before RAI tx is started (
I 131 sodium iodide
)
Complication of RAI tx:
1.
Exacerbations of thyrotoxicosis with arrhythmia
2.
3.
4.
5.
6.
Overt thyroid storm
Hypothyroidism
Risk of fetal damage
Worsening of eye sign
Hyperparathyroidism
HYPERTHYROIDISM
Thyroid Surgery:
Indicated to:
1.
2.
3.
4.
5.
Young patient
With Grave ophthalmopathy
Pregnant
With suspicious thyroid nodule in Grave’s gland
Large nodular toxic goiter w/ low level of radioactive iodine uptake.
Placed patient to euthyroid state prior to thyroid surgery:
1.
2.
3.
Antithyroid drugs
Lugol’s iodine solution (3 drops BID)
Propranolol
Thyroidectomy:
1.
2.
3.
Bilateral subtotal thyroidectomy
Total lobectomy & subtotal lobectomy contra-lateral (Hartley-Dunhill)
Total thyroidectomy
Advantages over RAI:
1.
2.
3.
Immediate cure of the disease
Low incidence of hypothyroidism
Potential removal of coexisting thyroid carcinoma
Disadvantages:
1.
2.
3.
Complication ---> nerve injury (1%) and hypoparathyroidism (13% transient/ 1% permanent).
Hematoma
Hypertrophic scar formation
•
HYPERTHYROIDISM
Recurrent thyrotoxicosis after surgery--->
RAI
Treatment of Exopthalmos:
1.
2.
3.
4.
5.
Tape eyelids at night
Wear eyeglasses
Steroid eye drop / systemic steroid (60mg prednisone OD) alleviate chemosis.
Lateral tarsorrhaphy to oppose eyelids
Radio-orbital radiation or orbital decompression
HYPERTHYROIDISM
Toxic Nodular Goiter (Plummers’ disease):
•
No extrathyroidal manifestation
•
•
Milder than Grave’s disease
Treatment:
•
•
Propranolol
Thyroidectomy (lobectomy with isthmectomy)
Toxic adenoma:
•
Solitary toxic nodule (Follicular) tumor
•
Thyrotoxicosis is uncommon unless it is 3 cm in size or more.
Thyroid storm:
•
•
•
•
Life threatening
1.
Precipitated by:
Infection (pharyngitis / pneumonitis)
2.
Iodine 131 treatment
•
Prophylactic treatment: --- Surgery in euthyroid state
1.
Treatment:
Fluid replacement
2.
3.
4.
5.
6.
7.
8.
Antithyroid drug
Beta blocker
Lugol’s iodine solution
Hydrocortisone
Cooling blanket
Sedation
Extreme cases ----> peritoneal dialysis or hemofiltration to lowe T4&T3
Avoid ASPIRIN ---> increases free thyroid hormone levels
B.
A.
Causes:
HYPOTHYROIDISM
1.
2.
3.
4.
5.
Primary:
•
Autoimmune thyroiditis
Hashimotos thyroiditis
•
•
•
•
•
•
•
•
•
Primary myxedema
Iatrogenic
Thyroidectomy
Iodine 131 tx
Antithyroid drugs
Congenital (Cretinism)
Thyroid dysgenesis
Dyshormonogenesis
Inflammatory
Subacute thyroiditis
Riedels thyroiditis
Metabolism
Iodine deficiency
1.
2.
Secondary:
Hypopituitarism
Hypothalamic hypothyroidism
Peripheral resistance to thyroid hormone
3.
Treatment:
L-thyroxine (50-100ug)
A.
•
•
•
•
•
•
THYROIDITIS
Acute Suppurative Thyroiditis
Uncommon
Associated with URTI
Staphylococcuc, Streptococcus and Pneumococci
E. Coli
Sx: - acute thyroid pain
- dysphagia
- fever
Dx: - FNA ----> smear and CS
Tx: - IV antibiotics / drain (abscess)
B.
1.
THYROIDITIS
Nonsuppurative Thyroiditis:
•
•
•
Hashimotos disease (Autoimmune lymphocytic thyroiditis)
Most common form of chronic lymphocytic thyroiditis
Autoimmune disease:
•
Antithyroglobulin / antimicrosomal antibodies
10 x more in females; 30 – 60y/o
•
•
•
•
•
•
Familial; 50% in first degree relatives
Predisposing factors:
1.
2.
3.
Down syndrome
Familial Alzheimer’s disease
Turner syndrome
Can co-exist with papillary CA
S/Sx: - Tightness in the throat (most common)
- Painless, nontender enlargement of gland
Dx: - Increase TSH, decrease T3 & T4
- (+) Anti-thyroid antibodies
- FNA ---> rule out CA (confirmatory)
Tx: - Medical if w/o compression ---->
- Surgical: thyroid hormone
1. Obstructive
2. Cosmetically unacceptable
3. Thyroid carcinoma coexist
B.
THYROIDITIS
2.
Nonsuppurative Thyroiditis:
•
•
•
•
•
•
Subacute Thyroiditis (De Quervans
Thyroiditis / Giant Cell Thyroiditis)
Exact cause unknown
Female 5x more the males
20 – 40 y/o
S/Sx: - Tender enlargement of the gland
Dx:
- Fever, malaise w/ unilateral or bilateral thyroid pain
- FNA
Tx:
- ESR (increase)
- Neutrophilia
- NSAIDS
- Prednisone
B.
3.
THYROIDITIS
Nonsuppurative Thyroiditis:
•
•
•
•
Riedels’ Thyroiditis:
Marked dense invasive fibrosis that may involve surrounding structures
Can cause hypoparathyroidism
Unknown cause ( maybe part of fibrosclerosis – retroperitoneum, mediastinum, lacrimal gland and bile duct)
S/Sx: - Compression symptoms
- Hoarseness - dyspnea
- stridor - dysphagia
•
Tx: - Tamoxifen
- Steroid
- Isthmectomy – to relieve compression symptom
- Thyroxine replacement
•
GOITER
1.
2.
3.
Enlargement of the thyroid gland in a euthyroid pt inflammation:
not associated
with neoplasm or
•
•
•
Familial:
Inherited enzymatic defect (dyshormonogenesis)
Autosomal recessive
Hypothyroidism / euthyroid
•
Endemic:
Iodine deficiency
•
Sporadic:
No definite cause, excludes goiter caused by thyroiditis and neoplasm as well as endemic goiter
GOITER
Pathology:
•
•
•
May be diffusely enlarged and smooth, or enlarged markedly nodular
Nodules are filled w/ gelatinous, colloid rich material and scattered between areas of normal thyroid tissues
With areas of degeneration, hemorrhage and calcification.
GOITER
•
•
S/Sx:
1.
2.
3.
4.
5.
Asymptomatic usually
Pressure symptoms usually
Dysphagia
Dyspnea
Paralysis of recurrent laryngeal nerve
Sudden pain associated with rapid enlargement of the gland ---> hemorrhage into a colloid nodule or cyst
Superior mesenteric syndrome due retro-sternal extension causing facial flushing that is accentuated by raising his arm above the head (Pemberton’s sign).
GOITER
Dx:
•
•
FNAC ---> specially if one nodule predominates, or painful or has recently enlarged. To rule out CA
TSH, T3 & T4 ---> usually normal
---> pts > 60y/o w/ long standing multinodular goiters (>17yrs) develops thyrotoxicosis
(Plummer’s dse). Low TSH w/ increased T3 but normal T4
(T3 toxicosis)
Tx:
•
•
•
•
No tx for euthyroid, small, diffuse goiter
Thyroxine ---> for large diffuse goiter; to depress TSH stimulation and reduce hyperplasia
Iodine ---> for endemic goiter
Surgery:
1.
Cosmetically acceptable
2.
3.
Compression symptoms
Suspicion for malignancy
Solitary or Dominant Thyroid Nodule
•
Most are benign (colloid nodule/adenomas)
Physician should:
1.
2.
Perform an accurate clinical assessment
Appreciate the risk factors for thyroid carcinoma
3.
Which pts would benefit from surgery
Risk factors for thyroid CA:
1.
Low-dose radiation to head & neck (<2000 rad)
2.
3.
4.
a.
b.
c.
d.
e.
- >2000rads causes destruction of thyroid gld.
- tends to be papillary type, multi-focal w/ higher incidence of LN metastases.
Family hx of thyroid CA
Medullary CA – inherited as an autosomal dominanat trait
Papillary CA – 6% familial dse.
Age
- thyroid nodule in children and elderly are more likely to be malignant.
Signs
Rapid enlargement of an old or new nodule
Symptoms of local invasion or compression symptoms
Consistency: Hard, gritty or fixed to surrounding structures
Palpable cervical lymphadenopathy
A cyst larger than 4 cm malignancy in diameter or in ultrasound is complex has 15% incidence of
Solitary or Dominant Thyroid Nodule
Work up for Thyroid nodule:
1.
FNAC – procedure of choice
•
• benign malignant -
65%
5% false (+) - 1% false (-) - 5%
Suspicious 15%
Non-diagnostic 15%
Limitation of FNAC:
1.
Follicular or Hurtle cell neoplasm (needs vascular and capsular invasion)
2.
Hx of head and neck radiation and family hx of thyroid CA usually has multifocal lesions.
If FNAC encountered a cyst ---> drain completely 75% is curative; if cyst persist after 3 attempts ---> unilateral lobectomy
Solitary or Dominant Thyroid Nodule
Work up for Thyroid nodule:
2.
3.
•
•
•
•
Thyroid ultrasonography:
Use to a) follow up the size of suspected benign nodules diagnosed by FNAC b) to detect presence of non-palpable nodules to locate and differentiate it for cyst or solid
MRI / CT scan:
For large retro-sternal extension
For recurrent or persistent thyroid tumor and to differentiate recurrence from postoperative fibrosis
Detect the presence of invasion, sign of CA.
Solitary or Dominant Thyroid Nodule
Work up for Thyroid nodule:
4.
•
Thyroid isotope imaging:
Check the function and locate small lesions
•
•
Cold -----------> 10 – 25% malignant
Hot -----------> 1% malignant
5.
b.
c.
a.
Laboratory:
•
Thyroid function test:
Not useful in assessing thyroid nodule d.
•
•
•
Serum thyroglobulin level:
To detect presence of metastatic lesions
Check completion of thyroidectomy
Not used in medullary and anaplastic thyroid CA
•
Serum calcitonin:
Follow up in medullary CA
RET oncogens (+) pt should have 24 hrs urine determination of VMA, metanephrine and cathecolamine to rule out a coexisting pheochromocytoma (for medullary CA)
Solitary or Dominant Thyroid Nodule
Approach for Thyroid Nodule
•
MALIGNANT THYROID
1.
90 – 95% are differentiated tumor w/ follicular origin
Papillary thyroid adenocarcinoma
2.
3.
Follicular adenocarcinoma
Hurtle cell carcinoma
•
1.
6% arise from parafollicular cells:
Medullary carcinoma of thyroid
•
1.
1% poorly differentiated
Anaplastic thyroid carcinoma
MALIGNANT THYROID
Oncogene associated w/ Thyroid carcinoma:
1.
2.
3.
4.
•
•
RET oncogene:
Seen in papillary and medullary thyroid CA
Located in chromosome 10
•
TRK – A:
Chromosome 1
•
Mutated ras oncogenes:
Follicular thyroid carcinoma , thyroid adenoma and multinodular goiter
•
Mutated p53 gene:
Anaplastic thyroid carcinoma
MALIGNANT THYROID
Papillary Thyroid Carcinoma:
•
•
•
•
•
•
•
Most common (80%)
Predominant thyroid CA in children (75%)
Usually due to radiation exposure of the neck (85-90%)
Multi-focal (30-88%); has LN spread (para-tracheal & cervical LN).
Can invade trachea, esophagus and recurrent laryngeal nerve; late hematogenous spread.
Mixed tumor (papillary & follicular): variant of papillary CA, but classified as papillary for it biologically acts as papillary CA.
Orphan Annie Nuclei:
•
•
Characteristic cellular feature
Abundant cytoplasm, crowded nuclei and intra-nuclear cytoplasmic inclusion
•
2.
3.
MALIGNANT THYROID
Papillary Thyroid Carcinoma:
3 forms of papillary CA (based on size and extent):
1.
Minimal or occult / micro carcinoma
•
•
1 cm or less, no capsular invasion
Non-palpable and usually an incidental finding intra-op or autopsy
•
•
•
•
•
Recurrence rate ----> 7%
Mortality ------------> 0.5%
Intra-thyroidal Tumors:
> 1cm and confined to the thyroid gland
(-) extra thyroidal invasion
Extra-thyroidal Tumors:
Locally advanced with invasion through the thyroid capsule into adjacent structures.
All types can be associated w/ LN metastases and intrathyroidal blood vessel invasion or occasionally metastases
MALIGNANT THYROID
Papillary Thyroid Carcinoma:
S/Sx:
•
•
•
•
Euthyroid, slow growing painless mass
Signs of local invasions:
•
•
Dysphagia
Dyspnea
•
Hoarseness of voice
Palpable cervical LN more apparent than primary lesion
(lateral aberrant thyroid)
Uncommon distant metastases (lung metastases in children)
Diagnosis:
•
•
FNAC (specific and sensitive for papillary, medullary and anaplastic)
CT/MRI in pts w/ extensive local or sub-sternal extension
MALIGNANT THYROID
Papillary Thyroid Carcinoma:
•
1.
2.
3.
4.
Prognostic indicators: (85% 10yrs survival)
AGES scale:
A- age G- grade E- extent S- size
MACIS scale:
M- metastases A- age C- completeness of resection
S- size I- extra thyroidal invasion
AMES
TNM
Distant metastases
(bone): most significant prognostic indicator overall
MALIGNANT THYROID
•
•
•
•
Papillary Thyroid Carcinoma: (SURGERY)
Lobectomy with isthmectomy acceptable for minimal papillary thyroid CA
Total thyroidectomy (near total) if:
1.
Size: if tumor > 3cm
2.
3.
4.
2.
3.
4.
Age: male > 40y/o female > 50y/o
Angioinvasion
Distant metastases
Thyroidectomy w/ modified radical neck dissection :
•
•
If with clinically palpable cervical lymphadenopathy
Not done for prophylaxis
Reasons for total thyroidectomy:
1.
85% is multifocal
To decrease incidence of anaplasia in any residual tissue
Facilitate the diagnosis of unsuspected metastatic disease by RAI scanning or treatment
Greater sensitivity of blood thyroglobulin level to predict recurrent or persistent of the disease.
•
•
•
•
•
•
•
•
MALIGNANT THYROID
Follicular Thyroid Carcinoma:
1.
2.
10%; Female > Male (3:1), mean age= 50y/o
More frequent in Iodine deficiency area
Vascular invasion & hematogenous spread is more common (bone, lung and liver).
Types:
Minimally invasive tumor:
•
•
Invasion into but not through the tumor capsule
Previously called atypical adenoma
Invasive tumors (capsular/vascular)
1% thyrotoxic
Dx / Tx:
•
FNAC not helpful ----> lobectomy and isthmectomy (frozen section) ----> (+) total thyroidectomy ----> iodine 131 to detect distant metastases and for ablation.
Prognosis:
1.
2.
3.
4.
5.
6.
Age over 50y/o
> 4cm size
Higher tumor grade
Marked vascular invasion
Marked extra-thyroidal invasion
Distant metastasis
Mortality: 40 % ----> 10 yrs
MALIGNANT THYROID
HURTLE CELL THYROID TUMOR:
•
•
•
3 – 5%, intermediate, uni-focal
Male : Female (2:1), spread by lymphatics
Derived from oxyphilic cells of the thyroid gld.
•
•
Possess TSH receptors and produces thyroglobulin
Only 10% takes up iodine hence localize distant metastasis thallium scan is used to
•
Often multifocal and bilateral
Dx: FNAC ----> 20% malignant
Tx: - total thyroidectomy for RAI ablation usually fails
- mod radical neck dissection if with palpable cervical LN
- Thyroid suppression is suggested
Prognosis: 60% ------> 5yr survival
MALIGNANT THYROID
•
•
•
•
•
MEDULLARY THYROID CARCINOMA:
5-7%; Aggressive tumor; 50-60y/o
Arise from parafollicular or C cells of the thyroid
(neuroectodermal-ultimobrachial bodies 4 th &5 th branchial pouches.
Secrets calcitonin (95%); 85% secrets carcinoembryonic antigen
(CEA)
Sporadic 90%
• unifocal, usually 45y/o
• worse prognosis
Familial 10%
•
•
•
Associated with:
•
•
MEN IIA or Sipples’ syndrome (MTC, hyperplastic parathyroid and pheochromocytoma
MEN IIB (MTC, pheochromocytoma, ganglioneuromatosis and Marfan,s syndrome)
Multifocal, usually 35 y/o
Better prognosis
MALIGNANT THYROID
•
•
•
MEDULLARY THYROID CARCINOMA:
Does not concentrate Iodine 131, localized distal metastasis.
Thallium scan is used to
Spread:
•
•
•
Lymphatics (neck and superior mediastinum)
Blood ---> liver, bone (osteoblastic) and lung
Local invasion
Can secrets:
•
•
•
•
•
•
Calcitonin
Histamine
Serotinin (causes diarrhea)
ACTH 2-4% causing Cushing syndrome
CEA
Prostaglandin E2 and F2 alpha
Dx:
•
Hx ‘ PE; serum calcitonin, CEA, FNAC, Serum calcium
MALIGNANT THYROID
Tx:
•
•
•
Total thyroidectomy
Radiotherapy and chemotherapy ---> failure
•
MRND is done for:
Palpable cervical LN
•
•
•
1.
2.
•
>2cm tumor for 60% nodal metastasis
Tumor debulking in cases of metastatic and local recurrence should be done to ameliorate symptoms of flushing and diarrhea and help to decrease the risk of death.
All pt should be screen for pheochromocytoma (MEN II) w/c shoud be resected first.
Selective removal of the parathyroid shd be done if preoperatively has hypercalcemia.
Follow up: - serum calcium / CEA level
Prognosis:
Localize -------> 80% 10 year survival
(+) LN --------> 45% 10 year survival
Best ------------> Worst prognosis
Familial non-MEN MTC -----> MEN IIA ----> Sporadic cases ------> MEN IIB
MALIGNANT THYROID
Anaplastic Thyroid Carcinoma:
•
1 – 3% most aggressive, few survive > 6 months
•
•
•
Most arise from previous differentiated thyroid CA
Low incident could be due to low iodine deficiency
70 – 80 y/o
Treatment:
•
Radiotherapy ----> doxorubicin ----> debulking thyroidectomy ----> completion with radiotherapy and chemotherapy
MALIGNANT THYROID
LYMPHOMA:
•
•
•
•
•
1 – 5% non-Hodgkin B cell
Usually develops in pts w/ chronic lymphocytic thyroiditis (Hashimotos thyroiditis)
S/Sx similar with anaplastic CA, compression symptoms is the most common
Tx: Chemotherapy
•
•
Cyclophosphamide
Doxorubicin
•
Vincristine
•
Prednison
Radiotherapy
Surgery: - done for diagnosis and to alleviate compression symptoms
80% survival if confined to the gland; 40% it had spread
•
Metastatic Carcinoma:
Rare; hypernephroma is the most common primary site
T h a n k y o u