A Case of a 71-year-old woman is admitted due to fever and productive cough
advertisement

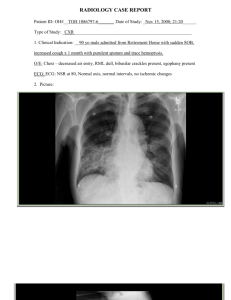
SANJAY SINGHANIA FEVER AND PRODUCTIVE COUGH CHIEF COMPLAINT GENERAL DATA Patient X is a 71-year-old female, retired corporate attorney, currently residing in New Haven came to Yale Emergency Department due to fever and productive cough HISTORY OF PRESENT ILLNESS 4 days PTA patient noted the onset of cough. Initially nonproductive, then became productive with yellowish sputum and was associated with left sided chest pain. 2 days PTA she noted feeling chills and had a temperature of 38.9°C. The fever, cough and chest pain continued over the next 48 hrs. which prompt her to seek consult to Yale Emergency Department. She denied hemoptysis, weight loss, sore throat, sinusitis, back pain, diarrhea, rash, joint pain or headaches. PAST MEDICAL HISTORY She has a history of congestive heart failure related to ischemic heart disease that has been controlled with Lasix, an ACE- inhibitor, and Lopressor. PERSONAL SOCIAL HISTORY Patient X is a retired corporate attorney and lives alone in New Haven. She is a former smoker but quit 3 months ago when her husband died of lung cancer. She denies alcohol use, recent travel, domestic pets or any risk factors for HIV exposure. PERTINENT FINDINGS IN MEDICAL HISTORY PERTINENT FINDINGS PERTINENT (+) 71 years old Female 38.9 C Fever Productive cough Yellow sputum chills Left sided chest pain history of congestive heart failure related to ischemic heart disease that has been controlled with Lasix Former smoker Husband died of lung ca PERTINENT (-) She denied hemoptysis, weight loss, sore throat, sinusitis, back pain, diarrhea, rash, joint pain or headaches. She denies alcohol use, recent travel, domestic pets or any risk factors for HIV exposure PHYSICAL EXAMINATION PHYSICAL EXAMINATION PHYSICAL EXAMINATION GENERAL SURVEY VITAL SIGNS SKIN HEENT PERTINENT POSITIVE (+) PERTINENT NEGATIVE (-) • Thin • in mild respiratory distress • Temperature: 38.9°C • RR: 28 cycles per min • PR: 120 beats per min. • BP: 128/84 mmHg • O2 saturation: is 89% on room air • Decrease turgor • TMs mildly red • oropharynx is mildly red • sinuses nontender • no middle ear fluid • oropharynx no exudate. PHYSICAL EXAMINATION PHYSICAL EXAMINATION CHEST AND LUNGS PERTINENT POSITIVE (+) PERTINENT NEGATIVE (-) • remarkable for splinting to • Right chest is clear the left side on deep inspiration • dullness to percussion ≈ 1/4 way up on left side • decreased breath sounds at left base • egophony and bronchial breath sounds are evident as one listens more superiorly on the left side. The right chest is clear. COR - RRR without murmurs or rubs. PHYSICAL EXAMINATION PHYSICAL EXAMINATION CARDIOVASCULAR ABDOMEN NEURO PERTINENT POSITIVE (+) PERTINENT NEGATIVE (-) • COR - RRR without murmurs or rubs. • soft, nontender without hepatosplenomegaly • nonfocal PERTINENT FINDINGS PERTINENT (+) • HCO3: 29 (NV: 22 to 28 mEq/L) • Glu: 150 (NV:70 to 99 mg/dL) • WBC:18.0 (NV:(4.5 to 11.0 × 109/L) • 41 lymphs (NV: 20-40%) • Sputum Gram’s stain: a few PMN, many epithelial cells, and scattered Gram positive and Gram negative cocci and rods are seen • size/left lower lobe infiltrate is present that obscures the left heart border PERTINENT (-) • • • • • • • • • Na: 143(NV:135-145 mEq/L) K: 4.2 (NV:3.6-5.2 mmol/L) Cl: 100 (NV: 96-106 mEq/L) Cr: 1.0 (NV: 0.59 to 1.04 mg/dL) Hb: 13.8(NV:12.1 to 15.1 g/dL) Hct :39.8(NV:36% to 48%) 54 segmenters (NV:40-60%) 5 bands (NV:0-5%) platelets 255K (NV:150,000 to 450,000) • EKG: NSR/normal rate, intervals and no ischemic changes • CXR: Normal heart size • UA: clear/1.020/1+ protein/no cells or casts Differential Diagnosis 01 Lobar Pneumonia 02 03 Acute Bronchitis 03 Pulmonary Edema Secondary to CHF 04 Pulmonary Tuberculosis Comparison of Signs and Symptoms Disease Productive cough Fever and Chills Yellow sputum Tachypnea Tachycardia Peripheral O2 desaturation Lobar Pneumonia + + + (early stage) + + + Acute Bronchitis + + + + + + Pulmonary Edema Secondary to CHF + + + + + + Pulmonary Tuberculosis + + + + + + Comparison of Signs and Symptoms Disease Chest Pain Dullness to percussion Decreased skin turgor Splinting to the left side on deep inspiration Decreased breath sound at left base Lobar Pneumonia + + + + + Acute Bronchitis + - + + + Pulmonary Edema Secondary to CHF + + + + + Pulmonary Tuberculosis + + + + + P R I M A RY I M P R E S S I O N TYPICALCOMMUNITY ACQUIRED PNEUMONIA SECONDARY TO CONGESTIVE HEART FAILURE HOW WE ARRIVED IN OUR DIAGNOSIS HOW WE ARRIVED IN OUR PRIMARY IMPRESSION? 1. Patient experienced the following signs and symptoms: • • • • • • • • Fever chills Yellow sputum Productive cough Tachypnea with pleuritic chest pain remarkable for splinting to the left side on deep inspiration Dullness on percussion Decreased breath sounds *Reference: Htun, T. P., Sun, Y., Chua, H. L., & Pang, J. (2019). Clinical features for diagnosis of pneumonia among adults in primary care setting: A systematic and meta-review. Scientific reports, 9(1), 7600. https://doi.org/10.1038/s41598-019-44145-y HOW WE ARRIVED IN OUR PRIMARY IMPRESSION? 2. Patient X has a History of Congestive Heart failure Chronic heart failure patients has an increased risk of pneumonia due to alveoli flooding and reduced microbial clearance. A study by Mor and Thompson suggest that patients with chronic heart failure, in particular those using loop diuretics, have markedly increased risk of hospitalization with pneumonia. *Reference: Mor A, Thomsen RW, Ulrichsen SP, Sørensen HT. Chronic heart failure and risk of hospitalization with pneumonia: a population-based study. Eur J Intern Med. 2013 Jun;24(4):349-53. doi: 10.1016/j.ejim.2013.02.013. Epub 2013 Mar 17. PMID: 23510659 RISK FACTORS RISK FACTORS • Patient X is a former smoker The risk of ex-smokers was similar to current smokers, about 2.14 to 1. According to the study of American College of Chest Physician-The number of cigarettes smoked per day and the life-time pack-years showed a positive dose-response relationship, with a significant trend in pneumonia. *Reference: Mor A, Thomsen RW, Ulrichsen SP, Sørensen HT. Chronic heart failure and risk of hospitalization with pneumonia: a population-based study. Eur J Intern Med. 2013 Jun;24(4):349-53. doi: 10.1016/j.ejim.2013.02.013. Epub 2013 Mar 17. PMID: 23510659 RISK FACTORS • Patient X is 71 years old Age is one of the primary risk factors for pneumococcal pneumonia, and even healthy adults 65 years or older are at increased risk for pneumococcal disease. Our immune systems naturally weaken with age, it's harder for our bodies to fight off infections and diseases like pneumococcal pneumonia — even for healthy adults. *Reference: Stupka, J. E., Mortensen, E. M., Anzueto, A., & Restrepo, M. I. (2009). Communityacquired pneumonia in elderly patients. Aging health, 5(6), 763–774. https://doi.org/10.2217/ahe.09.74 RISK FACTORS • Patient X has a History of Congestive Heart failure Chronic heart failure patients has an increased of pneumonia due to alveoli flooding and reduced microbial clearance. A study by Mor and Thompson suggest that patients with chronic heart failure, in particular those using loop diuretics, have markedly increased risk of hospitalization with pneumonia. *Reference: Mor A, Thomsen RW, Ulrichsen SP, Sørensen HT. Chronic heart failure and risk of hospitalization with pneumonia: a population-based study. Eur J Intern Med. 2013 Jun;24(4):349-53. doi: 10.1016/j.ejim.2013.02.013. Epub 2013 Mar 17. PMID: 23510659 WHAT IS THE ETIOLOGIC AGENT? Streptococcus pneumoniae Streptococcus pneumoniae • • • • • • Gram-positive α-hemolytic Lancet-shaped diplococcus Bile soluble Optochin sensitive Catalase-negative but produces hydrogen peroxide. • Can cause a range of different illnesses including sinusitis, otitis media, pneumonia, bacteraemia, osteomyelitis, septic arthritis and meningitis • frequent colonizer of the human nasopharynx with a colonization rate of 27–65% • Most common etiologic agent on Typical Community Acquired cough Figure 1. Shows Streptococcus pneumoniae under the microscope 27 OTHER ETIOLOGIC AGENTS EPIDEMIOLOGY PNEUMONIA IS COMMON AND SERIOUS • 150.7 million new cases worldwide in 2020 • 2nd leading cause of hospitalization worldwide ~20% of patients with pneumonia require hospitalization • 6th leading cause of death in the world ~10% of patients with pneumonia die Variations in rates of disease: • • More common in men More common in African Americans compared to Caucasians and Asians • More common in children and older adults (overall rate for 18-49 yo is ~5 per 1000 overall rate for >65 yo is 75 per 1000 ) Figure 2. Worldwide disability adjusted life year (DALY) of pneumococcal pneumonia. Global distribution of pneumococcal pneumonia on a log10 scale of the 2016 DALY per 100,000 pneumococcal pneumonia data obtained from Institute for Health Metrics and Evaluation Figure 3. Global distribution of lower respiratory infections over time. This figure depicts how the burden for four major lower respiratory infections changes over time in response to the introduction of antibiotic treatments and vaccine implementation. Disability adjusted life year (DALY) data obtained from Institute for Health Metrics and Evaluation EPIDEMIOLOGY • Spread via air-borne droplets from a cough or sneeze. • Outbreaks usually occur in close communities • Incubation period: 1-3 days • Susceptibility of population: immunity after infection is short and unsteady, no cross-immune PATHOGENESIS CLEARANCE vs. COLONIZATION Microbes constantly enter airways but many factors prevent colonization: • mucous entrapment • ciliary clearance • immune surveillance • intact epithelial barrier • secreted factors such as: ‒ secretory IgA ‒ surfactant proteins (SP-a, SP-d) ‒ defensins Disrupting or overwhelming these defense mechanisms can allow microbes to colonize the lungs, resulting in PNEUMONIA Effects and patterns of microbial colonization: where and how inflammati o n appe ars can be informativ e Alveolar Interstitial • In alveolar lumen • Purulent exudate of RBCs and PMNs • Mostly in alveolar wall • Mononuclear WBCs • Fibrinous exudate Lobar pneumonia • lobar distribution • “typical” CAP • S. pneumo, H. flu. Bronchopneumonia Atypical pneumonia • patchy distribution • aspiration, intubation, bronchiectasis • Staph, enterics, Pseudomonas • diffuse infiltrate w/ perihilar concentration • Mycoplasma, Chlamydophila, Legionella • Respiratory viruses, e.g. influenza 35 COMMUNITY ACQUIRED PNEUMONIA • Infection of the pulmonary parenchyma acquired from exposure in the community • Classically divided into “typical” and “atypical” syndromes: I. “Typical” CAP: • presents with “typical” severe, acute infection • infectious agent (usually S. pneumo or H. flu) is culturable/ identifiable • responsive to cell-wall active antibiotics II. “Atypical” CAP: • presentation is usually sub-acute • causative pathogens are difficult to culture/identify by standard methods • not responsive to penicillins CLINICAL MANIFESTATION Describe the physical findings in the chest and what they indicate? • Splinting to the left side on deep inspiration: Splinting is a reduce in inspiratory effort through shallow breathing to lessen the sharp pain felt with inspiration • Dullness to percussion indicates denser tissue, such as zones of effusion or consolidation. Once an abnormality is detected, percussion can be used around the area of interest to define the extent of the abnormality. Normal areas of dullness are those overlying the liver and spleen at the anterior bases of the lungs • Decrease breath sounds at left base or decreased sounds can mean: Air or fluid in or around the lungs (such as pneumonia, heart failure, and pleural effusion) Increased thickness of the chest wall. Over-inflation of a part of the lungs Describe the physical findings in the chest and what they indicate? • Egophony is increased resonance of voice sounds heard when auscultating the lungs. When spoken voices are auscultated over the chest, a nasal quality is imparted to the sound which resembles the bleating of a goat. • Bronchial breath sounds are tubular, hollow sounds which are heard when auscultating over the large airways (e.g. second and third intercostal spaces). They will be louder and higher-pitched than vesicular breath sounds 42 TYPICAL CAP PRESENTATION History • sudden onset of fever and cough Physical signs and symptoms • • • • • • fever tachycardia tachypnea productive cough with purulent sputum and possible hemoptysis pallor and cyanosis localized: − dullness to percussion − decreased breath sounds − crackles , ronchi , egophony (“E” -to-”A” change) Investigations • • • CXR showing lobar consolidation CBC showing leukocytosis w/ left shift Sputum sample contains neutrophils, RBCs; Gram stain may be positive depending on organism COMPLICATIONS COMPLICATIONS Don’t SLAP HER: • Septicemia • Lung abscess • ARDS • Para-pneumonic effusion • Hypotension • Empyema • Respiratory failure/Renal failure WORK UP/LABS 46 ROUTINE LABORATORY TEST The following laboratory tests may not be useful for diagnostic purposes but are useful for classifying illness severity and site-of-care/admission decisions: • Serum electrolyte panel (sodium, potassium, bicarbonate, blood urea nitrogen [BUN], creatinine, glucose) • Arterial blood gas (ABG) determination (serum pH, arterial oxygen saturation, arterial partial pressure of oxygen and carbon dioxide) – Hypoxia and respiratory acidosis may be present. • Venous blood gas determination (central venous oxygen saturation) • Complete blood cell (CBC) count with differential • Serum free cortisol value • Serum lactate level 47 BLOOD CULTURE • Blood cultures should be obtained before the administration of antibiotics. These cultures require 24 hours (minimum) to incubate. When blood cultures are positive, they correlate well with the microbiologic agent causing the pneumonia. Figure 4.S. pneumoniae colonies with a surrounding green zone of alpha-hemolysis (black arrow) on a BAP 48 LABORATORY TECHNIQUES • Flow chart for identification and characterization of a S.pneumoniae isola te 49 SPUTUM EVALUATION • Sputum Gram stain and culture should be performed before initiating antibiotic therapy (if a good-quality, contaminant-sparse specimen containing < 10 squamous epithelial cells per low-power field can be obtained). The white blood cell (WBC) count should be more than 25 per low-power field in nonimmunosuppressed patients. Figure.S. pneumoniae in sputum specimens 50 CHEST RADIOGRAPH • Chest radiography is considered the standard method for diagnosing the presence of pneumonia, that is, the presence of an infiltrate is required for the diagnosis. However, it must be noted that the accuracy of plain chest radiography for detecting pneumonia decreases depending on the setting of infection Figure. A chest X-ray of a patient who have bacterial pneumonia 51 CHEST ULTRASONOGRAPHY • Ultrasonography (US) is useful in evaluating suspected parapneumonic effusions. US can identify septations within the fluid collection that may not be visible on CT scans. US also has great utility for directing needle placement for pleural fluid aspiration (throacentesis) at the patient's bedside. Figure. Chest Ultrasonography showing lung consolidation of a patient who have pneumonia MANAGEMENT APPROACH TO PATIENT X Figure 5. A concept map showing the approach to a 71 year old female who came in due to fever and productive cough Should the patient be hospitalized or could she be treated as an outpatient? • Yes, the patient should be hospitalized and monitored since patient is categorized under moderate-risk community acquired pneumonia until signs of improvement is manifested. When should antibiotics be initiated for the empiric treatment of communityacquired pneumonia (CAP)? • Antibiotics, the mainstay for the treatment of pneumonia, should be initiated as soon as a diagnosis of CAP is made. Patient X is under moderate-risk community acquired pneumonia • Clinical Features of patients with CAP according to risk categories EMPIRIC THERAPY B: For patients with moderate risk CAP What initial antibiotics are recommended for the empiric treatment of moderate-risk community-acquired pneumonia? • For moderate-risk CAP, a combination of an IV nonantipseudomonal β-lactam (BLIC, cephalosporin) with either an extended macrolide or a respiratory fluoroquinolone is recommended as initial antimicrobial treatment. When should de-escalation of empiric antibiotic therapy be done? • De-escalation of initial empiric broad-spectrum antibiotic or combination parenteral therapy to a single narrow spectrum parenteral or oral agent based on available laboratory data is recommended once the patient is clinically improving, is hemodynamically stable and has a functioning gastrointestinal tract. SIGNS OF IMPROVEMENT • In the absence of any unstable coexisting illness or other life threatening complication, the patient may be discharged once clinically stable and oral therapy is initiated • A repeat chest radiograph prior to hospital discharge is not needed in a patient who is clinically improving • A repeat chest radiograph is recommended during a follow-up visit, approximately 4 to 6 weeks after hospital discharge to establish a new radiographic baseline and to exclude the possibility of malignancy associated with CAP, particularly in older smokers REASONS ON LACK OF RESPONSE OF PATIENTS TO EMPIRIC THERAPY • The following are the reasons why patients have lack of response to empiric therapy Recommended Hospital discharge criteria PREVENTION PREVENTION • Get the flu vaccine each year. People can develop bacterial pneumonia after a case of the flu. You can reduce this risk by getting the yearly flu shot. • Get the pneumococcal vaccine. This helps prevent pneumonia caused by pneumococcal bacteria. • Practice good hygiene. Wash your hands frequently with soap and water or an alcohol-based hand sanitizer. • Don’t smoke. Smoking damages your lungs and makes it harder for your body to defend itself from germs and disease. If you smoke, talk to your family doctor about quitting as soon as possible. • Practice a healthy lifestyle. Eat a balanced diet full of fruits and vegetables. Exercise regularly. Get plenty of sleep. These things help your immune system stay strong. • Avoid sick people. Being around people who are sick increases your risk of catching what they have. Thank You Stay safe and God speed DOC! SANJAY SINGHANIA