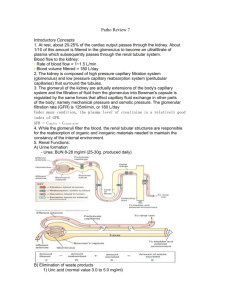
GFR 3 processes involved in Urine formation 1.Glomerular filtration 2.Tubular reabsorption 3.Tubular secretion GFR The amount of the glomerular filtrate formed by all the nephrons of both the kidneys in a one minute is called GFR In the average human adult, the GFR is about 125 ml / min. or 180 L / day Filtration fraction – the fraction of the renal plasma which becomes the filtrate Filtration fraction = GFR / RPF Dr. Ashok Solanki Basic Mechanisms of Urine Formation GLOMERULAR FILTRATE: fluid that filters through the glomeruli into Bowman's capsule =PLASMA – PROTEINS(plasma proteins, plasma proteins binded substances & substances with a MW > 8nm). GLOMERULAR FILTRATION RATE(GFR): The quantity of glomerular filtrate formed in all nephrons of both kidneys / min. - normal value: 125ml/min or 180 Liters/day. GLOMERULAR FILTRATION BARRIER Glomerular Capillary - The capillary endothelium is perforated by thousands of small holes called fenestrae - Although the fenestrations are relatively large, endothelial cells are richly endowed with fixed negative charges that obstruct the passage of plasma proteins. - The basement membrane consists of a meshwork of collagen and proteoglycan fibrillae that have large spaces through which large amounts of water and small solutes can filter. - The basement membrane effectively prevents filtration of plasma proteins because of strong negative electrical charges associated with the proteoglycans. Glomerular Capillary - The final part of the membrane is a layer of epithelial cells that line the outer surface of the glomerulus. - These cells are not continuous but have long foot like processes (podocytes) that encircle the outer surface of the capillaries. - The foot processes are separated by gaps called slit pores through which the glomerular filtrate moves. - The epithelial cells also have negative charges, provide additional restriction to filtration of plasma proteins. Glomerular Filtration • Ultrafiltration of plasma in the glomerulus Governed by 2 major factors: 1. Filtration coefficient (Kf) 2. Pressure gradient/ Starling forces (hydrostatic and osmotic pressure gradients) Mechanism of Glomerular Filtration Filtration coefficient 1. Capillary permeability 2. Size of the capillary bed Capillary permeability Filtration depends on the size and shape of the molecules and the electric charge they carry. 1. Molecular size: Neutral substances with molecular diameter of less than 4nm are easily filtered and substances with diameter with more than 8nm are not filtered 2. shape: the elongated particles with large molecular weight can pass easily, whereas globular particles of same molecular weight cannot pass through 3. Electrostatic charge: particles with positive charge are easily filtered than the negatively charged particles. SIZE OF THE CAPILLARY BED The surface area for filtration of the capillary bed depends on the size of messengial cells. The contractility of messengial cells decreases the area for filtration and relaxation of messengial cells increases the area for filtration. The factors that alter messengial cell activity are Factors that produce contraction of messengial cells Norepinephrin, endothelins, PDGF, Histamine, Thromboxane A2, The factors that produce relaxation of messengial cells Dopamine, ANP, Camp, Bradykinin, Nitric oxide GFR - GFR is determined by - (1) the balance of hydrostatic and colloid osmotic forces acting across the capillary membrane and (2) the capillary filtration coefficient (Kf), the product of the permeability and filtering surface area of the capillaries. - - - In the average adult human, the GFR is about 125 ml/min, or 180 L/day. The fraction of the renal plasma flow that is filtered (the filtration fraction) averages about 0.2; this means that about 20 per cent of the plasma flowing through the kidney is filtered Filtration fraction = GFR/Renal plasma flow Pressure Gradient Determinants of the GFR - The GFR is determined by - (1) the sum of the hydrostatic and colloid osmotic forces across the glomerular membrane, which gives the net filtration pressure, - (2) the glomerular capillary filtration coefficient, Kf. - GFR = Kf X Net filtration pressure - The net filtration pressure represents the sum of the hydrostatic and colloid osmotic forces that either favor or oppose filtration across the glomerular capillaries Determinants of the GFR - (1) hydrostatic pressure inside the glomerular capillaries (glomerular hydrostatic pressure, PG), which promotes filtration; - (2) the hydrostatic pressure in Bowman’s capsule (PB) outside the capillaries, which opposes filtration; - (3) the colloid osmotic pressure of the glomerular capillary plasma proteins (µG), which opposes filtration; and - (4) the colloid osmotic pressure of the proteins in Bowman’s capsule (µB), which promotes filtration. Determinants of the GFR - (Under normal conditions, the concentration of protein in the glomerular filtrate is so low that the colloid osmotic pressure of the Bowman’s capsule fluid is considered to be zero.) - The GFR can therefore be expressed as - GFR = Kf X (PG – PB – µG + µB) Net filtration pressure • Forces favoring filtration (mm Hg) glomerular hydrostatic pressure - Pgc 60 bowmen’s capsule colloid osmotic pressure – πbc 0 • Forces opposing filtration (mm Hg ) bowmen’s capsule hdrostatic pressure - Pbc 18 glomerular capillary colloid osmotic pressure – πgc 32 Net filtration pressure = 60 – 18 – 32 = +10 mmof Hg Dr. Ashok Solanki Determinants of the GFR - Increased Bowman’s Pressure Decreases GFR Capsule Hydrostatic - In certain pathological states associated with obstruction of the urinary tract, Bowman’s capsule pressure can increase markedly - serious reduction of GFR. - Precipitation of calcium or uric acid may lead to “stones” that lodge in the urinary tract, often in the ureter, thereby obstructing outflow of the urinary tract and raising Bowman’s capsule pressure. GLOMERULARHYDROSTATIC PRESSURE (PGC) • the determinant of GFR most subject to physiological control • Factors that influence PG - arterial pressure (effect is buffered by autoregulation) - afferent arteriolar resistance - efferent arteriolar resistance Effect of Afferent and Efferent Arteriolar Constriction on Glomerular Pressure R a Blood Flow R a P P Blood Flow G GF R GFR + Renal Blood F R e Δ 𝑄 𝑃 𝑅 = Re G GF R GFR + Renal Blood F Determinants of the GFR - Increased Glomerular Capillary Colloid Osmotic Pressure Decreases GFR - As blood passes from the afferent arteriole through the glomerular capillaries to the efferent arterioles, - the plasma protein concentration increases about 20 % - (1) the arterial plasma colloid osmotic pressure and - (2) the fraction of plasma filtered by the glomerular capillaries (filtration fraction). - Increasing the arterial plasma colloid osmotic pressure raises the glomerular capillary colloid osmotic pressure decreases GFR. Determinants of the GFR - Increased Glomerular Capillary Osmotic Pressure Decreases GFR Colloid - Increasing the filtration fraction also concentrates the plasma proteins and raises the glomerular colloid osmotic pressure - a greater rate of blood flow into the glomerulus tends to increase GFR, and a lower rate of blood flow into the glomerulus tends to decrease GFR. Determinants of the GFR - Increased Glomerular Pressure Increases GFR Capillary Hydrostatic - Increased arterial pressure tends to raise glomerular hydrostatic pressure and so increases GFR. - Increased resistance of afferent arterioles reduces glomerular hydrostatic pressure and decreases GFR. - dilation of the afferent arterioles increases both glomerular hydrostatic pressure and GFR Determinants of the GFR - Increased Glomerular Pressure Increases GFR Capillary Hydrostatic - Constriction of the efferent arterioles increases the resistance to outflow from the glomerular capillaries. - This raises the glomerular hydrostatic pressure, and as long as the increase in efferent resistance does not reduce renal blood flow too much, GFR increases slightly Determinants of the GFR - Increased Glomerular Capillary Hydrostatic Pressure Increases GFR - Efferent arteriolar constriction reduces renal blood flow - the filtration fraction and glomerular colloid osmotic pressure increase - So, if the constriction of efferent arterioles is severe, the rise in colloid osmotic pressure exceeds the increase in glomerular capillary hydrostatic pressure caused by efferent arteriolar constriction. - When this occurs, the net force for filtration actually decreases, causing a reduction in GFR. Determinants of the GFR - Increased Glomerular Pressure Increases GFR Capillary Hydrostatic - constriction of afferent arterioles reduces GFR. - the effect of efferent arteriolar constriction depends on the severity of the constriction; - moderate efferent constriction raises GFR, - severe efferent constriction reduces GFR. Factors affecting GFR GFR is influenced by factors that alter renal blood flow, Pressure gradients, glomerular capillary permeability and surface area for filtration 1. Change in renal blood flow: 2. Glomerular capillary hydrostatic pressure 3. Bowmans capsule hydrostatic pressure 4. Glomerular capillary oncotic pressure 5. Glomerular capillary permeability 6. Effective filtration surface area 7. Size, shape and electric charge Conditions that alter GFR 1. 2. 3. 4. 5. 6. 7. 8. EXERCISE PREGNANCY POSTURE SLEEP WEATHER GENDER AGE FOOD INTAKE Regulation of GFR Myogenic mechanism Intrinsic mechanism Extrinsic mechanism Tubuloglomerular feedback Neural mechanism Hormonal mechanism Physiologic Control of GFR and - Sympathetic NervRouBsFSystem Activation Decreases GFR - Strong activation of the renal sympathetic nerves can constrict the renal arterioles and decrease renal blood flow and GFR - Norepinephrine, Epinephrine and Endothelin Constrict Renal Blood Vessels and Decrease GFR Physiologic Control of GFR and - Angiotensin II ConstrR icB ts F Efferent Arterioles - raise glomerular hydrostatic pressure while reducing renal blood flow - helps prevent decreases in glomerular hydrostatic pressure and GFR - Endothelial-Derived Nitric Oxide Decreases Renal Vascular Resistance and Increases GFR - Prostaglandins and Bradykinin Tend to Increase GFR Autoregulation of GFR and - Feedback mechanR isB msF intrinsic to the kidneys normally keep the renal blood flow and GFR relatively constant, despite marked changes in arterial blood pressure. - Role of Tubuloglomerular Autoregulation of GFR Feedback in - Decreased Macula Densa Sodium Chloride Causes Dilation of Afferent Arterioles and Increased Renin Release Autoregulatio n Despite changes in mean arterial blood pressure (from 80 to 180 mm Hg), renal blood flow is kept at a relatively constant level, a process known as autoregulation Myogenic mechanism BP Stretching of blood vessels (afferent arteriole smooth muscle) Opening of cationic channels Depolarization Opening of voltage-dependent calcium channels Calcium influx Increased intracellular calcium vasoconstriction Myogenic Autoregulation - the ability of individual blood vessels to stretching during increased arterial pressure. resist - Arterioles respond to increased wall tension or wall stretch by contraction of the vascular smooth muscle. - Stretch of the vascular wall allows increased movement of calcium ions from the ECF into the cells, causing them to contract - This contraction prevents overdistension of the vessel and raises vascular resistance - prevent excessive increases in RBF and GFR when arterial pressure increases. GFR/RBF autoregula tion Myoge nic mechani sm Tubuloglome rular feedback mechanism MYOGENI C MECHANI SM INCREASE ARTERIAL PRESSUR E AFFERENT ARTERIOLES STRETCHE S VASCULAR SMOOTH MUSCLE CONTRACTS ARTERIOL E RESISTAN CE TUBULOGLOMERULAR FEEDBACK MECHANISM JG MECHANI FEEDBAC SM K INCREASED ARTERIAL PRESSURE INCREASE PG INCREASE GFR - INCREASE TUBULAR FLOW Increase Macula Densa stimulation Increase AFFERENT arteriole resistance INCREASE GFR INCREASE NaCl Macula densa Increase uptake - through 1-Na-1-K- 2Cl symporter Increase production of ATP and adenosine ATP and adenosine binds to their specific receptors Increase intracellular calcium ion Increase Afferent arteriole JG FEEDBAC K MECHANIS M HORMONES THAT INFLUENCE GFR AND RBF Stimulus Vasoconstric tor Angiotensin II Endothelin Vasodilator PGE Nitric oxide ECFV Stretch, Ang II, Epi, Bradykinin ECFV, Shear stress, Ang II Shear stress, ACh, Histamine Effect on GFR Effect of RBF •Clearance is a general concept that describes the rate at which substances are removed (cleared) from the plasma. Clearance Technique Renal clearance of a substance is the volume of plasma completely cleared of a substance per min. C = Us x V Cs x Ps = s Ps Us x V Wher Cs = clearance of substance S e: (mL/min) Ps = plasma conc. of substance S (mg/mL) Us = urine conc. of Use of clearance to measure GFR For a substance that is freely filtered, but not reabsorbed or secreted (inulin, 125 Iiothalamate, ~creatinine), renal clearance is equal to GFR amount filtered = amount excreted GFR x Pin = Uin GFR x Pi = V n Uin x V Calculation of GFR: Pinulin = 1.0 mg / 100ml Uinulin = 125 mg/100 ml Urine flow rate = 1.0 ml/min GFR = Cinulin = Uin x 125 x 1.0 = 125 GFR ml/min =V 1.0 Creatinine clearance U x GFR = C cr r P PVC = r Creatinine, endogenously released into plasma by skeletal muscle, is used to measure GFR Not as accurate as inulin amount excreted > amount filtered Reasonably accurate measurement of GFR Clearance Methods - The rates at which different substances are “cleared” from the plasma provide a useful way of quantitating the effectiveness with which the kidneys excrete various substances. - The renal clearance of a substance is the volume of plasma that is completely cleared of the substance by the kidneys per unit time - renal clearance of a substance is calculated from the urinary excretion rate (U X V) of that substance divided by its plasma concentration (P). C =U X V/P Inulin Clearance - If a substance is freely filtered and is not reabsorbed or secreted by the renal tubules, - then the rate at which that substance is excreted in the urine is equal to the filtration rate of the substance by the kidneys - Inulin, a polysaccharide molecule with a molecular weight of about 5200. - Inulin is not produced in the body, is found in the roots of certain plants and must be administered intravenously to a patient to measure GFR. Inulin Clearance - (1) if the clearance rate of the substance equals that of inulin, the substance is only filtered and not reabsorbed or secreted; - (2) if the clearance rate of a substance is less than inulin clearance, the substance must have been reabsorbed by the nephron tubules; and - (3) if the clearance rate of a substance is greater than that of inulin, the substance must be secreted by the nephron tubules. Creatinine Clearance - Creatinine is a by-product of muscle metabolism and is cleared from the body fluids almost entirely by glomerular filtration. - Because measurement of creatinine clearance does not require intravenous infusion into the patient, this method is much more widely used than inulin clearance for estimating GFR clinically. - creatinine clearance is not a perfect marker of GFR because a small amount of it is secreted by the tubules, so that the amount of creatinine excreted slightly exceeds the amount filtered Creatinine Clearance GFR = CCreatinine = Ucreatinine X V / Pcreatinine - If GFR suddenly decreases by 50%, the kidneys will transiently filter and excrete only half as much creatinine, - causing accumulation of creatinine in the body fluids and raising plasma concentration - plasma creatinine concentration is inversely proportional to GFR GLOMERULAR DISEASES - Glomerular diseases include a large and clinically significant group of renal diseases. - Glomerulonephritis (GN) is the term used for diseases that primarily involve the renal glomeruli. - I. Primary glomerulonephritis in which the glomeruli are the predominant site of involvement. - II. Secondary glomerular diseases include certain systemic and hereditary diseases which secondarily affect the glomeruli. GLOMERULAR DISEASES - The clinical presentation of glomerular disease is quite variable but in general four features—proteinuria, hematuria, hypertension and disturbed excretory function - nephritic and nephrotic syndromes; - acute and chronic renal failure; - asymptomatic proteinuria and haematuria ACUTE NEPHRITIC is the acSutYe NonsDet RofOhaMemEaturia, proteinuria, - This hypertension, oedema and oliguria following an infective illness about 10 to 20 days earlier. - 1. The haematuria is generally slight giving the urine smoky appearance and erythrocytes are detectable by microscopy 2. The proteinuria is mild (less than 3 gm per 24 hrs) and is usually non-selective (nephritic range proteinuria). 3. Hypertension is generally mild. 4. Oedema in nephritic syndrome is usually mild and results from sodium and water retention. 5. Oliguria is variable - - NEPHROTIC SYNDROME - it is characterised by findings of massive proteinuria, hypoalbuminaemia, oedema, hyperlipidaemia, lipiduria, and hypercoagulability. - 1. Heavy proteinuria (protein loss of more than 3 gm per 24 hrs) is the chief characteristic of nephrotic syndrome (nephrotic range proteinuria). - A highly-selective proteinuria consists mostly of loss of low molecular weight proteins, while a poorlyselective proteinuria is loss of high molecular weight proteins in the urine. In nephrotic syndrome, proteinuria mostly consists of loss of albumin (molecular weight 66,000) in the urine. - NEPHROTIC SYNDROME - 2. Hypoalbuminaemia is produced primarily consequent to urinary loss of albumin, and partly due to increased renal catabolism and inadequate hepatic synthesis of albumin. - 3. Oedema in nephrotic syndrome appears due to fall in colloid osmotic pressure resulting from hypoalbuminaemia. - 4. Hyperlipidaemia - the liver faced with the stress of massive protein synthesis in response to heavy urinary protein loss, also causes increased synthesis of lipoproteins NEPHROTIC SYNDROME - 5. Lipiduria occurs following hyperlipidaemia due to excessive leakiness of glomerular filtration barrier. - 6. Hypercoagulability – - increased urinary loss of antithrombin III, - hyperfibrinogenaemia from synthesis in the liver, - decreased fibrinolysis, - increased platelet aggregation and - altered levels of protein C and S. increased Thank You…