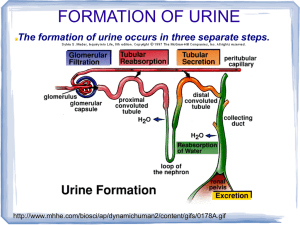
lOMoARcPSD|2619780 Practical exam revision Systems Physiology (Deakin University) StuDocu is not sponsored or endorsed by any college or university Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 PRACTICAL ONE: Blood, heart and ECG Haematocrit normal values: Female: 42%, Males 45%. Normal blood composition: Haematocrit ~42-45%, Buffy coat (leukocytes and platelets) <1%, Plasma 55-58%. Less Haematocrit: possibly due to dilution of blood or blood vessels being lysed, resulting in less haematocrit. Lack of visible leukocytes: visible leukocytes cannot be seen without staining. With staining, the nuclei in the leukocytes can be easily observed. Neutrophils: engulf and destroy bacteria intracellularly. Eosinophils: an increase in eosinophils that are circulating is associated with allergic conditions. Basophils: synthesise histamine and heparin. Monocytes: emigrate from blood, enlarge and become macrophages. Serve 3 main functions in the immune system; phagocytosis, antigen presentation and cytokine production. Lymphocytes: give immune defence against specifically programmed targets. B-lymphocytes: produce anti-bodies. T-lymphocytes: provide cell-mediated immunity by destroying their specific target cells. Left ventricle: Right ventricle: - Has the bicuspid/mitral valve - Wall is thick - Pumps oxygenated blood to the body and tissues - Has the tricuspid valve - Thinner wall than left ventricle - Pumps deoxygenated blood to the lungs P-wave: Atrial depolarisation. P-R interval: AV nodal delay. QRS complex: Repolarisation. T-wave: Ventricular repolarisation. S-T segment: Ventricles are completely depolarised and the cardiac contractile cells are undergoing the plateau phase of action potential before they repolarise. Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Q-T segment: Ventricular action is complete and the ventricles are contracting and emptying. T-P segment: Ventricles are at resting and are refilling. Label waves on ECG trace: Calculate heart rate from ECG trace with a labelled time axis: Count the small (1mm) squares between two QRS complexes. The ECG paper runs at 25 mm/sec through the ECG printer; therefore: Cardiac output: = (heart rate X stroke volume) First heart sound: the closure of the AV valve. Second heart sound: closure of the semilunar valves. Antigens: large, complex molecule that triggers a specific immune response against itself when it gains entry to the body. Antibody: immunoglobulin produced by a specific activated B lymphocyte against are particular antigen; binds with the specific antigen against which it is produced and promotes the antigenic invader’s destruction by augmenting non-specific immune responses already initiated against the antigen. Blood Type Antigens on erythrocytes Antibodies in plasma A A Anti-B B B Anti-A AB A and B No antibodies O No antigens Both anti-A and anti-B Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Rhesus positive: have the Rh factor and can receive rhesus negative and rhesus positive blood. Rhesus negative: lack the Rh factor. Anti-Rh antibodies are only produced by Rhnegative individuals, and therefore can only receive rhesus negative blood. Cardiac muscle under microscope: Major features of mammalian heart: double circulatory system, 2 circuits (pulmonary and systemic) Functions of major features: heart pumping blood to lungs and rest of body simultaneously, Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 PRACTICAL TWO: Blood vessels and Blood pressure. Ductus venous, foramen ovale, ductus arteriosis: name of the foetal shunt that distributes blood from the umbilical vein to the inferior vena cava. Bypasses the lungs. Vessels on arterial side of circulation: - Thick layer of smooth muscle - Small lumen - Thick layer of connective tissue Vessels on venous side of circulation: - Thin layer of smooth muscle - Large lumen (may appear flat) - Thin layer of connective tissue Diastolic pressure (DP): pressure in the arteries when the heart rests between beats. Systolic pressure (SP): when the heart beats, it contract sand pushes blood through the arteries to the rest of the body. The force creates pressure on the arteries – known as the systolic blood pressure. Pulse pressure (PP): = SP - DP Mean arterial pressure (MAP): = DP + (1/3 PP) List and describe the blood vessels that branch off the main vessels leaving the heart: coronary arteries branch from the aorta, surrounding the outer surface of the heart like the crown. They diverge into capillaries where the heart muscle is supplied with oxygen before converging again into the coronary veins to take the deoxygenated blood back to the atrium, where the blood will re-oxygenated through the pulmonary circuit. Coronary arteries are the arteries that supply blood to the heart muscle. A blood vessel’s main function is to transport blood around the body, they also play a role in controlling blood pressure. Effects of gravity on blood pressure: HYPOTENSION: gravity reduces the rate of blood return from the body veins below the heart back to the heart, thus reducing stroke volume and cardiac output. Gravity affects blood pressure via hydrostatic forces (e.g., during standing), and valves in veins, breathing, and pumping from contraction of skeletal muscles also influence blood pressure in veins. How first and second heart sounds are produced: FIRST SOUND: closure of AV valves. It is caused by the sudden block of reverse blood flow due to closure of the atrioventricular valves, i.e. tricuspid and mitral (bicuspid), at the beginning of ventricular contraction, or systole. Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 SECOND SOUND: closure of semilunar valves. It is caused by the sudden block of reversing blood flow due to closure of the semilunar valves (the aortic valve and pulmonary valve) at the end of ventricular systole and the beginning of ventricular diastole. Location and function of ductus venous: hunts a portion of the left umbilical vein blood flow directly to the inferior vena cava. Thus, it allows oxygenated blood from the placenta to bypass the liver. Location and function of ductus arteriosus: is a blood vessel connecting the pulmonary artery to the proximal descending aorta. It allows most of the blood from the right ventricle to bypass the foetus's fluid-filled non-functioning lungs. Location and function of foramen ovale: allows blood to enter the left atrium from the right atrium. It is one of two foetal cardiac shunts, the other being the ductus arteriosus (which allows blood that still escapes to the right ventricle to bypass the pulmonary circulation). Label a histological section of umbilical cord: Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Foetal circulatory system: Adult mammal circulatory system: Blood flow in microcirculation: arterioles, capillaries, and venules are collectively referred to as the microcirculation as they are only visible through a microscope. Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Aorta: largest artery and carries blood from the heart to the body. Blood is forced into the aorta from the left ventricle of the heart. Arteries: carry blood away from the heart to other organs. They can vary in size. The largest arteries have special elastic fibres in their walls. This helps to complement the work of the heart, by squeezing blood along when heart muscle relaxes. Arterioles: smallest arteries in the body. They deliver blood to capillaries. Arterioles are also capable of constricting or dilating and, by doing this, they control how much blood enters the capillaries. Capillaries: tiny vessels that connect arterioles to venules. They have very thin walls which allow nutrients from the blood to pass into the body tissues. Waste products from body tissues can also pass into the capillaries. Venules: Groups of capillaries within a tissue reunite to form small veins called venules. Venules collect blood from capillaries and drain into veins. Veins: Veins are the blood vessels that carry blood back to the heart. They may contain valves which stop blood flowing away from the heart. How blood pressure is measured using a sphygmomanometer: Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 PRACTICAL THREE: Renal Physiology Normal ranges of urine components: COMPONENT NORMAL RANGE BLOOD Negative BILIRUBIN Negative UROBILINOGEN 0.1-1 KETONE Negative PROTEIN NITRITE Negative Weak GLUCOSE Negative pH 5.0 SPECIFIC GRAVITY ~1.000 LEUKOCYTES Negative Control group: as time increased, the volume of urine decreased whereas the volume of sodium remained relatively constantly as no water or sodium was ingested. Water group: as the time increased, the volume of urine also increased whilst the volume of sodium decreased due to the large intake of water. The concentration of aldosterone and vasopressin would be lower than in the control group due to the increased intake of water. Sodium group: as the time increased, the volume of urine decreased and the volume of sodium increased due to the increased intake of sodium and water. The concentration of aldosterone and vasopressin would be higher than in the control group dues to the increased intake of sodium alongside water. Changes in levels of aldosterone and vasopressin: be due to ensure that proper fluid homeostasis and blood pressure are maintained. Renal cortex: Renal medulla: - Outermost layer of kidney - Consists of glomeruli + the proximal and distal tubules - Where ultrafiltration occurs - Erythropoietin production - Middle/inner layer of kidney - Consists of collecting tubules, Henle’s loop, vasa rectae, venulae rectae and the medullary capillary plexus + nephrons - Responsible for maintaining salt and water balance of blood - Consists of renal pyramids - Reabsorption of water Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Importance of differences: differences between the cortex and medulla are important to ensure that both reabsorption + filtration independently and continually. Renin-angiotensin-aldosterone (RAAS): plays an important role in blood volume regulation and systemic vascular resistance which together influence cardiac output and atrial pressure. Renin is primarily released by the kidneys, stimulating the formation of angiotensin in blood and tissues, which in turn stimulates the release of aldosterone from the adrenal cortex. Renin: a proteolytic enzyme that is released into the circulation primarily by the kidneys. Its release is stimulated by: 1. sympathetic nerve activation (acting through β1-adrenoceptors) 2. renal artery hypotension (caused by systemic hypotension or renal artery stenosis) 3. decreased sodium delivery to the distal tubules of the kidney. Aldosterone: the adrenocortical hormone that stimulates Na + reabsorption and K+ secretion by the distal and collecting tubules of the kidney’s nephron during urine formation. Angiotensin II: part of the RAAS hormonal pathway and is important in regulating the body’s salt balance. Potent vasoconstriction. Vasopressin: primarily involved in maintaining water balance by regulating the amount of water the kidneys retain for the body during water formation. A hormone secreted by the hypothalamus, then stored and released from the posterior pituitary. It increases the permeability of the distal and collecting tubules of the kidneys to water and promotes arteriolar vasoconstriction (also known as ADH). Anatomical and histological features of a kidney: Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Label nephron: Processes carried out by nephrons: responsible for removing waste products from blood and maintaining water, salt and pH balance in the body. This vital job results in the formation of urine. Filtration: the mass movement of water and solutes from plasma to the renal tubule that occurs in the renal corpuscle. Reabsorption: the net movement of interstitial fluid into the capillary. Secretion: release to a cell’s exterior, on appropriate stimulation, of substances produced by the cell. Role of salt and water balance in kidney: The kidneys maintain our body's water balance by controlling the water concentration of blood plasma. The kidneys also control salt levels and the excretion of urea. Water that is not put back into the blood is excreted in our urine. Our bodies take in water from food and drinks. We even get some water when we respire by burning glucose to release energy. We lose water in sweat, faeces, urine and when we breathe out (on a cold day you can see this water as it condenses into vapour). For the cells of our body to work properly, it is important that their water content is maintained at the correct level. This means our body must maintain a balance between the water we take in and the water we lose. Altering levels of salt and water balance: A high salt intake has been shown to increase the amount of protein in the urine which is a major risk factor for the decline of kidney function. There is also increasing evidence that a high salt intake may increase deterioration of kidney disease in people already suffering from kidney problems. Afferent Arteriole: The afferent arteriole receives blood rich in oxygen from the renal artery. This blood is transported to the glomerulus of the nephron where it is pressure filtered. Glomerulus: The glomerulus (Latin glomus=ball) is a knotted up capillary that contains small pores. The plasma of the blood and the small molecules contained in Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 plasma are pressure filtered into the Bowman's capsule. Large blood proteins and formed elements like blood cells and platlets are too big to be pressure filtered and remain in the arteriole. Efferent Arteriole: The efferent arteriole is smaller in diameter than the afferent arteriole and increases the pressure in the glomerulus aiding pressure filtration. The blood entering the efferent arteriole is thicker, as plasma has entered the tubule, but still contains oxygen that is moved on to the peritubular network to provide for the metabolic needs of the tubule. Bowman's Capsule: The filtrate produced in the glomerulus is collected in a bulblike start to the nephron called the glomerular capsule or Bowman's capsule (named for British surgeon Sir William Bowman). The plasma and its' dissolved molecules are transported from the Bowman's capsule into the lumen or inside of the nephron. Proximal Convoluted Tubule: At this point in the nephron, the filtrate from the blood contains both waste molecules like urea and useful molecules like amino acids, glucose, and salt. The filtering process in the glomerulus is not selective (except by size) so the proximal convoluted tubule works to actively transport nutrients (glucose, amino acids, and salts) back into the blood capillaries so they are not lost in the urine. The tubule has a brush border with many villi to increase the surface area for this process of selective reabsorption. The cells of the tubule also contain many mitochondria that produce the ATP required for the large amount of active transport taking place throughout the length of the tubule. Loop of Henle: The Loop of Henle dips down into the hypertonic environment of the kidney medulla and is responsible for the reabsorption of water from the filtrate. Water is drawn out of the descending limb of the loop, by osmosis, into the hypertonic medulla of the kidney. This water can then move into the capillary network and back into circulation to maintain blood volume. The ascending limb of the loop is impermeable to water and removes salt into the medulla of the kidney adding to the hypertonicity. Distal Convoluted Tubule: The Distal Convoluted Tubule is the site of tubular secretion. This process involves the active transport of materials from the blood directly into the tubule. Examples of molecules that are secreted by the distal convoluted tubule are creatinine, drugs like penicillin, and hydrogen ions. Tubular secretion of hydrogen ions along with the reabsorption of bicarbonate ions (a biological buffer) acts as a mechanism to control blood pH. Peritubular Capillary Network: The Peritubular Capillary Network acts as the blood supply to the nephron. The capillaries provide the nephron with glucose and oxygen to help with ATP production needed for active transport. The nutrients and water that are reabsorbed by the nephron are taken up by the capillary network surrounding the tubules and carried back to the renal vein and the body. Collecting Duct: The collecting duct receives filtrate from several nephrons. The collecting duct will remove varying amount of additional water from the filtrate depending on the hydration state of the individual. This results in a wide range of urine, from very dilute (lots of water remains) to very concentrated (most of the water Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 was reabsorbed). The amount of water reabsorbed is controlled by a hormone called ADH and is the topic of a future lesson. Once in the pelvis of the kidney the filtrate (now urine) contains substances that were pressure filtered and never reabsorbed such as urea, excess salt, water and other substances that were secreted from the blood such as hydrogen ions, drugs, or creatinine. Formation of urine: For the production of urine, the kidneys do not simply pick waste products out of the bloodstream and send them along for final disposal. The kidneys' 2 million or more nephrons (about a million in each kidney) form urine by three precisely regulated processes: filtration, reabsorption, and secretion. Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 PRACTICAL FOUR: Respiratory Physiology Barometric pressure: 760mmHg Water vapour pressure: 21.1PH20 Inspiratory reserve volume (IRV): extra volume of air that can be maximally inspired over and above the typical tidal resting volume (3000mL) Inspiratory capacity (IC): maximum volume of air that can be inspired at the end of a normal quiet expiration = IRV + TV (3500mL) Expiratory reserve volume (ERV): the extra volume of air that can be actively expired by maximally contracting the expiratory muscles beyonf that normally passively expired at the end of a typical resting tidal volume. (1000mL) Residual volume: the minimum volume of air remaining in the lungs even after maximal expiration. (1200mL) Functional residual capacity (FRC): the volume of air in the lungs at the end of a normal passive expiration = ERV + RV (2200mL) Vital capacity (VC): the maximum volume of air that can be moved out during a single breathe following a maximal inspiration. Subject inspires normally and expires maximaly = IRV + TV + ERV (4500mL) Total lung capacity (TLC): the maximum volume of air that lungs can hold = VC + RV (5700mL) Respiratory rate: = number of breaths / minutes (12 breaths/min) Total volume: = final reading - initial reading Pulmonary ventilation: = total L / minutes (6000mL/min) Tidal volume: volume of air entering or leaving the lungs during a single breath = total L / number of breaths (500mL) Alveolar ventilation: (tidal volume – dead space) X respiratory rate (4200mL/min) Dead space ventilation: dead space X ventilation rate (150mL) FEV1: forced expiratory volume in 1 second - volume of air that can be expelled from maximum inspiration in the first second. FEV1 is usually 80% of VC (normally 80% of the air that can be forcibly expired from maximally inflated lungs can be expired in 1 second). FVC: forced vital capacity - volume of air that can be forcibly expelled from the lung from the maximum inspiration to the maximum expiration. Downloaded by Tenai Amber (tenhae@hotmail.com) lOMoARcPSD|2619780 Why abnormal volumes may be bad: Effects of different gas mixtures on breath holding: Purpose of conversion factors: measurements have been taken in ATPS conditions but need to be in BTPS conditions to ensure physiological accuracy. Conversion factors ensure that the value can be compared regardless of altitude or location of the laboratory in the world. Hyperventilation conditions: holding their breath the longest under these conditions due to the large elimination of carbon dioxide from the body resulting in a perceived increased uptake of oxygen to saturate haemoglobin. ATPS: measured at ambient temperature, pressure, saturated with water vapor (e.g. expired gas, which has cooled down): ambient temperature and pressure, saturated. BTPS: in respiratory physiology lung volumes and flows are standardized to barometric pressure at sea level, body temperature, saturated with water vapor: body temperature and pressure, saturated. STPD: oxygen consumption and carbon dioxide delivery are standardized to standard temperature (0 ºC), barometric pressure at sea level (101.3 kPa) and dry gas: standard temperature and pressure, dry. Downloaded by Tenai Amber (tenhae@hotmail.com)